Abstract
Practical relevance:
Phosphorus is an essential nutrient required for the normal function of every cell in the body and a deficiency in dietary phosphorus may lead to adverse effects. Conversely, high dietary phosphorus may cause kidney damage in otherwise healthy adult cats, particularly when provided in highly bioavailable forms and when the calcium-to-phosphorus ratio is low. For cats that have chronic kidney disease (CKD), phosphorus is the most important mineral in its pathogenesis and morbidity. As the disease progresses, elevated phosphorus may increase the risk of complications such as soft tissue mineralization, which can lead to a further decrease in renal function. Additionally, the hormones secreted in response to increased circulating phosphorus have harmful effects, such as bone resorption, and can cause cardiovascular pathology. Very low phosphorus diets can also be problematic in cats with early CKD, potentially leading to hypercalcemia.
Clinical challenges:
There is currently a lack of maximum safety limits for dietary phosphorus in accepted nutritional guidelines in North American and Europe, which makes it difficult to assess the safety of some higher phosphorus cat foods. Additionally, information regarding phosphorus bioavailability is unknown for many diets and there are no commercially available tests. Similarly, there is no consensus regarding phosphorus requirement and recommended intake in cats with International Renal Interest Society stage 1-4 CKD despite there being targets for serum phosphorus.
Aims:
This review evaluates dietary phosphorus in healthy cats and cats with renal disease, and describes how newer research is informing evolving clinical approaches in feline nutrition.
Audience:
The article is aimed at general practitioners, internal medicine specialists and veterinary nutritionists.
Evidence base:
Information provided in this article is drawn from the published literature.
Homeostasis and metabolism of this essential nutrient
Phosphorus is an essential nutrient present in all cells and has varied roles in the body. The main store of phosphorus is skeletal tissue. Circulating phosphorus, its excretion and its absorption from the gastrointestinal tract are regulated by several hormones and also impacted by calcium in the diet and circulation. Dietary phosphorus requirements are highest during growth when skeletal development and maturation occur; however, phosphorus remains an essential nutrient throughout life.
Phosphorus homeostasis is maintained by similar mechanisms across mammalian species. These include the regulation of phosphorus absorption in the gastrointestinal tract, filtration and absorption in the kidneys, and shifts in and out of the bone. Phosphorus is absorbed throughout the intestinal tract, although most absorption occurs in the small intestines. Intestinal absorption is mediated by the type IIb sodium phosphate cotransporters Npt2b, which are regulated by phosphorus intake as well as cholecalciferol -the active form of vitamin D. The sites of active intestinal absorption of phosphorus in cats are unknown and cannot be presumed as they appear to vary depending on the species; in rats and humans, for example, the sites of absorption are thought to be primarily the duodenum and jejunum with little absorption in the ileum, whereas phosphorus absorption occurs primarily in the ileum in mice. 12 The kidneys also have an important role in phosphorus regulation where filtered phosphorus may be reabsorbed. Most renal reabsorption occurs in the proximal tubule, where the density of sodium phosphorus cotransporters Npt2a, Npt2c and PiT-2 determines how much phosphorus is reabsorbed. Factors such as dietary phosphorus, calcitriol levels, parathyroid hormone (PTH), fibroblast growth factor-23 (FGF-23), metabolic acidosis and glucocorticoids all impact phosphorous reabsorption.
Effects of CKD
CKD results in disturbances in calcium and phosphorus homeostasis, which can lead to complications such as soft tissue mineralization and progression of CKD. Phosphorus retention may occur because of a decline in renal function and glomerular filtration rate with CKD. Despite the increase in serum phosphorus and the decline in metabolic transformation of vitamin D to cholecalciferol in advanced CKD, the absorption of phosphorus from the intestines is hardly affected, however (as shown in rats). 3 PTH, which is secreted in response to hypocalcemia with or without hyperphosphatemia, leads to the release of calcium stores from the bone and in the long term results in bone remodeling. 4 Elevated serum phosphorus and calcium may result in soft tissue mineralization, which can exacerbate CKD if the kidneys are affected. FGF-23, which is secreted from the bone in response to hyperphosphatemia, has the primary role, in combination with a factor named Klotho, of decreasing the density of sodium phosphorus cotransporters in the kidney, thereby having a phosphaturic effect.

High phosphorus intake and risk of kidney damage in healthy cats
High dietary soluble phosphorus (see 'Dietary phosphorus and its varied bioavailability' box) may induce kidney disease in otherwise healthy adult cats. This may be of higher concern in senior cats, which are at a greater risk of CKD, and so clinicians should especially consider phosphorus intake in this age group. The impact of dietary soluble phosphorus on kidney health in cats has been evaluated in several feeding studies in adult cats:
✜ Two studies documented a reduction in endogenous creatinine clearance as a measure of glomerular function and, in some cases, glucosuria and albuminuria, when healthy adult cats were fed diets supplemented with soluble phosphorus for a total intake of 3.0-3.6 g in 1000 kcal and a calcium:phosphorus of 0.3-0.4.8,13
✜ Ina more recent study, adult cats were fed extruded dry foods with phosphorus exceeding 4.8 g/1000 kcal, with 3.6 g primarily provided by a soluble phosphorus salt, and a calcium:phosphorus of 0.6, for 4 weeks. This resulted in a significant increase in creatinine, a decline in glomerular filtration rate and ultrasonographic abnormalities, including nephrolithiasis. 14
✜ When a different cohort of cats in the same study was fed a diet with 3.6 g of phosphorus per 1000 kcal, with 1.5 g coming from inorganic phosphorus, and a calcium:phosphorus of 0.9, for 28 weeks, this resulted in renal echogenicity changes on ultrasound and nephrolithiasis, with one cat developing an acute uremic crisis leading to euthansia. 14
✜ A further trial included feeding diets with 4 g or 5 g of phosphorus per 1000 kcal, with 1 g provided by inorganic phosphoric salt and a calcium:phosphorus above 1.0, for 30 weeks. 15 Cats in this study maintained good overall health, without evidence of glucosuria or albuminuria, despite a temporary increase in FGF-23 in one of the diet groups.

A low-phosphorus approach to nutritional management of cats with CKD
The clinical benefit of dietary phosphorus reduction in animals with CKD has been well established for many years. One of the first studies to demonstrate this was performed in nephrectomized cats where a diet with reduced phosphorus resulted in fewer pathologic renal changes, such as tissue fibrosis, compared with the higher phosphorus control diet. 16 Dietary phosphorus reduction can bring a decrease, or even normalization, of serum phosphorus and PTH in cats with naturally occurring CKD. 17 In rats, a lower phosphorus diet may also prevent parathyroid hyperplasia and hyperparathyroidism. 18
The benefits of dietary phosphorus reduction in cats with IRIS stage 2 or higher CKD specifically have been known for decades, while data for cats with early kidney disease is only recent and limited (see 'Veterinary therapeutic diets through the renal disease stages' box). Some cats lose weight and muscle mass while being fed low-phosphorus veterinary therapeutic diets, however, which raises the question of whether they are of clinical benefit when cats have a low appetite and are frail.


Veterinary therapeutic diet composition
Veterinary therapeutic diets for cats with kidney disease are typically reduced in phosphorus and sodium, supplemented with B vitamins and long-chain omega-3 fatty acids, and are alkalizing. These diets also have less protein in order to reduce the accumulation of uremic toxins, which result from protein metabolism and are not cleared effectively because of decreased renal filtration. Protein reduction can additionally help mitigate proteinuria when present and prevent the progression of tubular injury. 26
While lower in protein, these diets are often highly digestible, and the provided protein is of high quality, meaning that amino acid composition and ratios approximate the cat's requirement. This allows for maximal utilization of amino acids to minimize endogenous protein catabolism, amino acid oxidation and protein fermentation in the colon. Moreover, the protein amount in these diets usually meets the recommended allowance by the National Research Council (2006) for healthy adult cats, meaning that while veterinary therapeutic renal diets are reduced in protein, they are not considered deficient in protein. 27
Meeting the protein and calorie requirements of cats with renal disease
While veterinary therapeutic diets meet the recommended allowance for protein in a healthy cat, as described earlier, protein requirements for cats with kidney disease are unknown and may be higher due to increased muscle catabolism. Moreover, these requirements may not be met when the energy intake is below a cat's energy requirements due to poor appetite associated with disease, poor diet palatability or food aversion. Therefore, some cats with kidney disease may suffer from an exacerbated decrease in lean body mass following a diet change to a veterinary therapeutic diet (Figure 1). It may then be hard to discern whether the reduction in muscling is due to primary disease, protein malnutrition or insufficient calorie intake. The new diets for cats with early CKD (see 'Veterinary therapeutic diets through the renal disease stages' box) can be a good option for individuals at this stage without the significant proteinuria that would indicate further protein reduction.

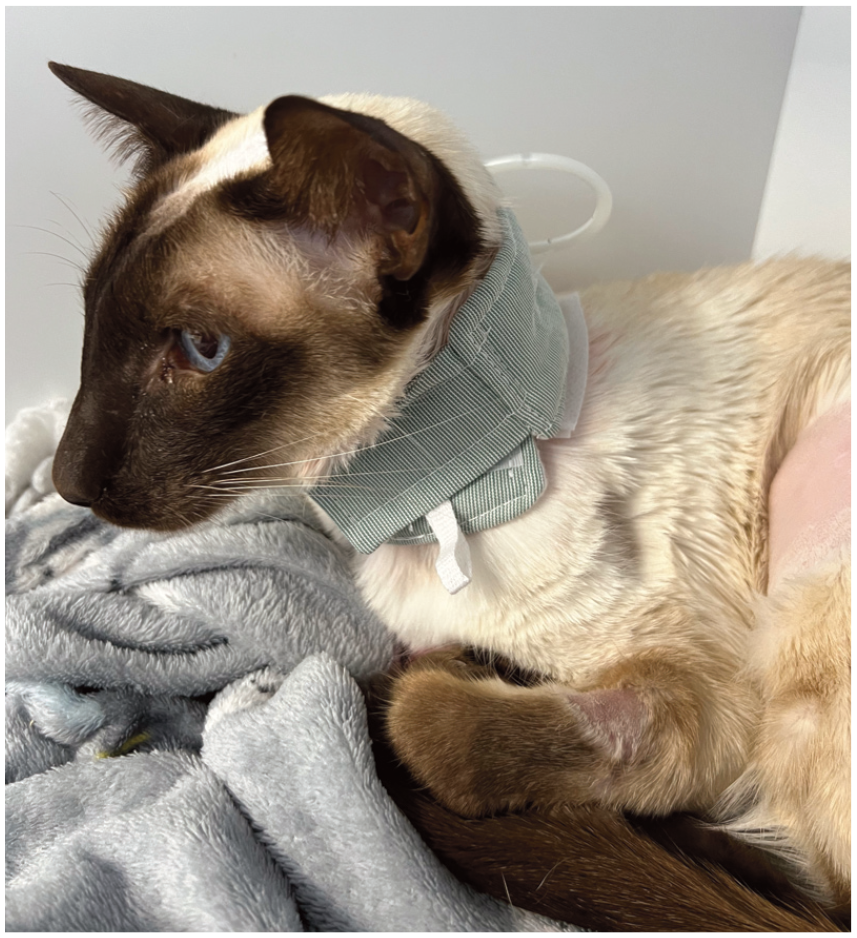
Kidney disease often results in decreased appetite and many cats with advanced disease present with sarcopenia and poor body condition. The dilemma many clinicians therefore face is whether to prescribe a therapeutic veterinary kidney diet and risk poor intake with resultant decreased muscling and body condition, or to opt for an 'over-the-counter' commercial maintenance diet with or without a phosphate binder such as aluminium hydroxide (see 'Veterinary therapeutic diets vs phosphate binders' box). Monitoring serum phosphorus can be a helpful tool (see 'Monitoring serum phosphorus and its metabolism' box). Appetite-enhancing medications and even feeding tubes for assisted enteral feeding may be considered in patients that are reluctant or unable to meet their energy needs with an appropriate diet (Figure 2).

Key Points
✜ Dietary phosphorus intake is a paramount consideration during the management of feline CKD.
✜ While phosphorus is an essential nutrient, decreased kidney function causes a shift in normal phosphorus homeostasis, which promotes disease progression.
✜ New information highlights that excessive soluble/inorganic phosphorus intake in healthy cats may lead to kidney injury and CKD.
✜ Clinicians should consider phosphorus intake, particularly in senior cats and in cats with CKD. An important limitation, however, is that phosphorus solubility and bioavailability are rarely known and no commercial assays are available.
Footnotes
Conflict of interest
The author is a paid consultant for Petco Health and Wellness Company. In addition, the author has previously received a speaking honorarium from Hill's Pet Nutrition and research support from Hill's Pet Nutrition and Royal Canin, a subsidiary of Mars. None of the above impacted the content of this manuscript.
Funding
The author of this commissioned Clinical Spotlight review received an honorarium; as for all JFMS articles, this Clinical Spotlight article went through peer review.
Ethical approval
This work did not involve the use of animals and therefore ethical approval was not specifically required for publication in JFMS.
Informed consent
This work did not involve the use of animals (including cadavers) and therefore informed consent was not required. For any animals or people identifiable within this publication, additional informed consent for publication was obtained.
