Abstract
Objectives
Gastrointestinal foreign bodies (FBs) are an important cause of emergency surgical intervention in cats, but little information exists in the literature evaluating the risks and outcomes in this species. The study purpose was to describe cases of feline FBs and compare perioperative factors and outcomes between linear foreign body (LFB) and discrete foreign body (DFB) surgery in cats.
Methods
The medical records from the University of Georgia Veterinary Teaching Hospital were searched for cats that had undergone surgery for FB removal between August 2009 and August 2021. Perioperative data were collected and described. Data were compared between cats with an LFB and cats with a DFB. A binomial probability series was used to estimate the likelihood of postoperative septic peritonitis or mortality in an additional cat in the series.
Results
A total of 56 cats were included in this study; 38 cats had a DFB and 18 had an LFB. No cats developed postoperative septic peritonitis, and all cats survived. The likelihood of postoperative septic peritonitis or mortality in an additional cat was estimated to be <5.2%. Cats with an LFB were found to have a significantly higher body condition score (P = 0.047), albumin (P = 0.025), American Society of Anesthesiologists status (P = 0.027), surgery length (P <0.001) and total cost of visit (P = 0.006) when compared with cats with a DFB. Cats with LFBs were more likely to develop a surgical site infection (SSI; P = 0.007) and be administered postoperative antibiotics (P = 0.017).
Conclusions and relevance
Cats undergoing surgery for gastrointestinal FBs had a low incidence of postoperative complications. Cats with LFBs had longer surgeries and were more likely to develop postoperative SSIs.
Introduction
Gastrointestinal (GI) foreign bodies (FBs) are common in companion animals; however, almost all the recent literature details data from canine populations. In dogs, postoperative dehiscence and septic peritonitis are reported in 1–16% of cases, and overall survival after FB surgery is reported to be 83–99%.1–5 In dogs, the reported preoperative risk factors for septic peritonitis after GI surgery include serum albumin <2.5 mg/dl, preoperative septic peritonitis, an inflammatory leukogram, a linear foreign body (LFB), older age and intraoperative hypotension.6–8 One recent study on chronic FB obstructions found that resection and anastomosis was associated with postoperative dehiscence and septic peritonitis in both dogs and cats. 5 Another study provides information specific to the removal of feline FBs. 1 That study reported a 100% survival rate for cats that underwent FB removal, with no cats developing intestinal dehiscence.
In cats, no studies have identified risk factors for septic peritonitis or death in cats undergoing FB surgery. However, one study from 2017 evaluated the rates of dehiscence and death after full-thickness biopsies of the GI tract in 172 cats. 9 This study found that dehiscence occurred in 2 (1.2%) cats and was significantly associated with hypoalbuminemia. Death occurred in 18/172 (10.5%) cats, with most of these being euthanized (n = 14/172). The reason for euthanasia or death included poor prognosis due to biopsy results, poor recovery postoperatively and dehiscence (n = 2/172). Hypoalbuminemia and neoplastic disease were found to be significantly associated with death.
LFBs occur less frequently than discrete foreign bodies (DFBs) in both dogs and cats. Cats tend to have a higher percentage of LFBs than dogs, with 33–61% of cat FBs being classified as LFBs,1,11–13 compared to 5–26% reported in dogs.1,3,10 In addition, it has also been shown that dogs with LFBs experience higher mortality and a higher rate of postoperative septic peritonitis compared to dogs with a DFB.1,7 In cats, one study on thread and sewing needle GI LFBs showed that approximately 84% of the cats survived; however, cats with preoperative septic peritonitis had a lower survival rate of 50%. 11 As previously noted, survival in dogs after surgery to remove LFBs is lower (80%) when compared to survival rates of dogs diagnosed with DFBs (94%). 1 Similar findings were identified in cats in a study from 2009. In that report, the eight cats with LFBs were found to have a 63% survival rate, while the 16 cats with DFBs were found to have a higher survival rate, with all cats surviving (100%). 1
Although these data guide our understanding of small-animal GI surgery, there are no recent data regarding prognostic indicators and risk factors in cats undergoing GI FB surgery. Therefore, the objectives of the present study were to report outcomes in cats undergoing surgery for removal of GI FBs, identify the perioperative risk factors for intestinal dehiscence and postoperative septic peritonitis in cats, and compare the perioperative course of cats with non-linear DFB versus LFB obstruction. The hypotheses were that cats would have lower occurrence of postoperative intestinal dehiscence compared to historical reports from dogs with similar risk factors for intestinal dehiscence, and cats with LFBs would have a more protracted clinical course than cats with DFBs.
Materials and methods
The medical records from the University of Georgia Veterinary Teaching Hospital from August 2009 to August 2021 were retrospectively evaluated. Cats with a GI FB, confirmed during an abdominal exploratory surgery, were included. Information on the patient’s signalment, admission day and time, clinical signs, duration of clinical signs, preoperative physical exam findings, pre- and postoperative clinical pathology findings, results of diagnostic imaging, anesthetic factors (American Society of Anesthesiologist [ASA] status, anesthetic duration, occurrence of hypotension), surgical factors (surgical duration, surgical procedures [gastrotomy, enterotomy, multiple site surgery], portions of the GI tract affected, linear or discrete foreign material identified, whether a surgery resident or surgery faculty member performed the surgery, and whether the FB could be manipulated into the stomach or the colon), postoperative care (whether a feeding tube was placed, duration of intravenous fluid therapy, medications given, change in body weight in hospital, hours until voluntarily eating), survival to discharge and total cost of the hospital stay were collected from hospital records. After-hours surgeries were defined as surgeries starting between 5 pm and 8 am or occurring on a Saturday or Sunday.
All cats in this study underwent an exploratory lap-arotomy through a ventral midline incision, and the entire abdominal contents were examined. Attempts were made to manipulate the FB to the stomach or colon to facilitate removal. If manipulation was not possible, an enterotomy or resection and anastomosis was performed. All surgeries were performed by either surgery residents (under the supervision of a board-certified surgeon) or a board-certified surgical faculty member.
Data for all cats were tested for normality then described using mean and standard deviation, median and range, or percentages, as appropriate. A binomial probability series was used to estimate the probability of mortality or septic peritonitis in an additional cat using the formula 0.05 = 0.9479^56 and subtracting 1 – 0.9479. Perioperative data from cats with surgically confirmed DFBs and LFBs were compared using a Student’s t-test, Mann–Whitney U-test or Fisher’s exact test. A P value of <0.05 was used to determine statistical significance.
Results
A total of 56 cats were identified for this study. Of these, 71% were male (n = 40) and 29% were female (n = 16), with a mean age of 3.3 ± 3.4 years and weight of 4.4 ± 1.4 kg. The most common breed was the domestic shorthair (n = 40). Other breeds included were the domestic longhair (n = 10), domestic medium hair (n = 5) and Siamese (n = 1). In total, 38 (68%) cats were diagnosed with a DFB and 18 (32%) with an LFB.
The median duration of clinical signs before presentation was 2 days (range 1–14 days). Of the cats, 7 (12%) previously had a FB removed. The most common reported clinical sign was vomiting, in 96% of cats (n = 54). Other common clinical signs included anorexia (n = 45, 80%), lethargy (n = 34, 61%) and diarrhea (n = 4, 7%). Other less commonly reported clinical signs included lameness (n = 1, 2%), coughing (n = 1, 2%), hairballs (n = 2, 4%), hiding (n = 2, 4%) and changes in urination behavior (n = 2, 4%). Pain on abdominal palpation was present in 43% of cats (n = 24), and 12% of cats (n = 7) had a palpable mass or object in the abdomen.
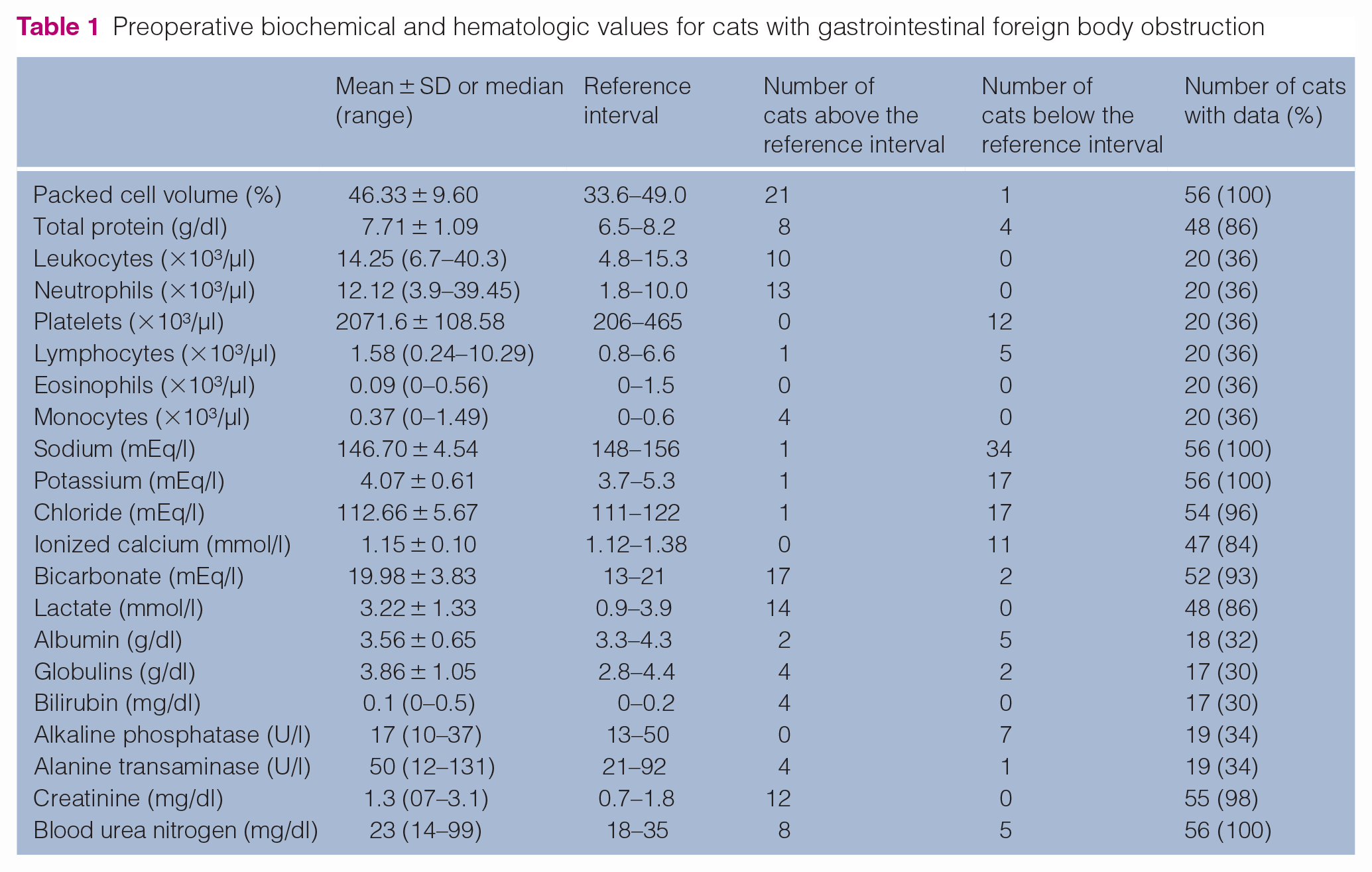
Table 1 lists preoperative biochemical and hematologic values for cats with GI FB obstruction. Of the 53 cats with electrolyte data available at admission (Table 1), hyponatremia was the most common abnormality identified (n = 34, 61%). In total, 17 (32%) cats were hypochloremic and hypokalemic; 14 (30%) cats were hyperlactatemic; 23 cats had complete blood counts performed; 21 cats had relative erythrocytosis. Multiple cats had an inflammatory leukogram (n = 8) with band neutrophils, or a stress leukogram (n = 5) characterized by neutrophilia and lymphopenia. Otherwise, no significant changes in bloodwork were reported.
Preoperative biochemical and hematologic values for cats with gastrointestinal foreign body obstruction
The most common method used for the diagnosis of FB obstruction was the combination of abdominal radiography and an abdominal ultrasound examination (n = 30, 54%). A total of 22 (40%) cats had only radiographs performed, and 3 (5%) cats had only an ultrasound performed.
After-hours surgery was performed in 35 (67%) cats. In total, 18 (31%) cats had a FB present in multiple parts of their GI tract. This was more common in cats with LFBs (n = 16/18 cats with LFBs, 89%) than cats with DFBs (n = 2/38 cats with DFBs, 5%). Because cats frequently had multiple locations within the gastrointestinal tract for a foreign body, there were 90 total recorded locations for foreign bodies; of these, the most common location for an FB was the jejunum (n = 40/90, 44%), followed by the duodenum (n = 21, 24%), stomach (n = 20, 22%), ileum (n = 6, 7%) and colon (n = 3, 3%). A total of 16 (29%) FBs were manipulated to the stomach and removed with a gastrotomy, while 6 (11%) FBs were manipulated into the colon and removed without an intestinal incision.
Multiple incisions were required to remove FBs in 12 (21%) cats. Of the cats that required multiple incisions, nine had LFBs and three had DFBs. Of the three cats with DFBs that required multiple incisions, two were found to have multiple FB obstructions, while one required a GI biopsy that had been planned before surgery. A gastrotomy was performed in 34 (60%) cats, and an enterotomy was performed 27 (44% of incisions) times in this population of cats. Four cats (7%) required more than one enterotomy, while 12 (21%) cats required a gastrotomy and at least one enterotomy. Resection and anastomosis was performed in three (5%) cats. Cats with FBs manipulated into the colon (n = 6) had no intestinal incision. An omental patch was placed in 22 (41%) cats. The most common location for LFBs to be anchored was the pylorus (n = 10, 56%), followed by the jejunum (n = 5, 28%) and the tongue (n = 3, 16%).
Table 2 details significantly different perioperative factors between cats with DFBs and LFBs. Cats with LFBs had a significantly higher body condition score, higher ASA status, longer duration of surgery, longer duration of postoperative fluid therapy, increased use of maropitant (Cerenia; Zoetis) postoperatively, higher total visit cost, increased likelihood of developing a surgical site infection (SSI) and received postoperative antibiotics more commonly than cats with DFBs. One cat was administered antibiotics without a documented SSI due to a fever of unknown origin; the remainder were administered antibiotics to treat SSIs.
Significantly different perioperative factors between cats with DFB and LFB
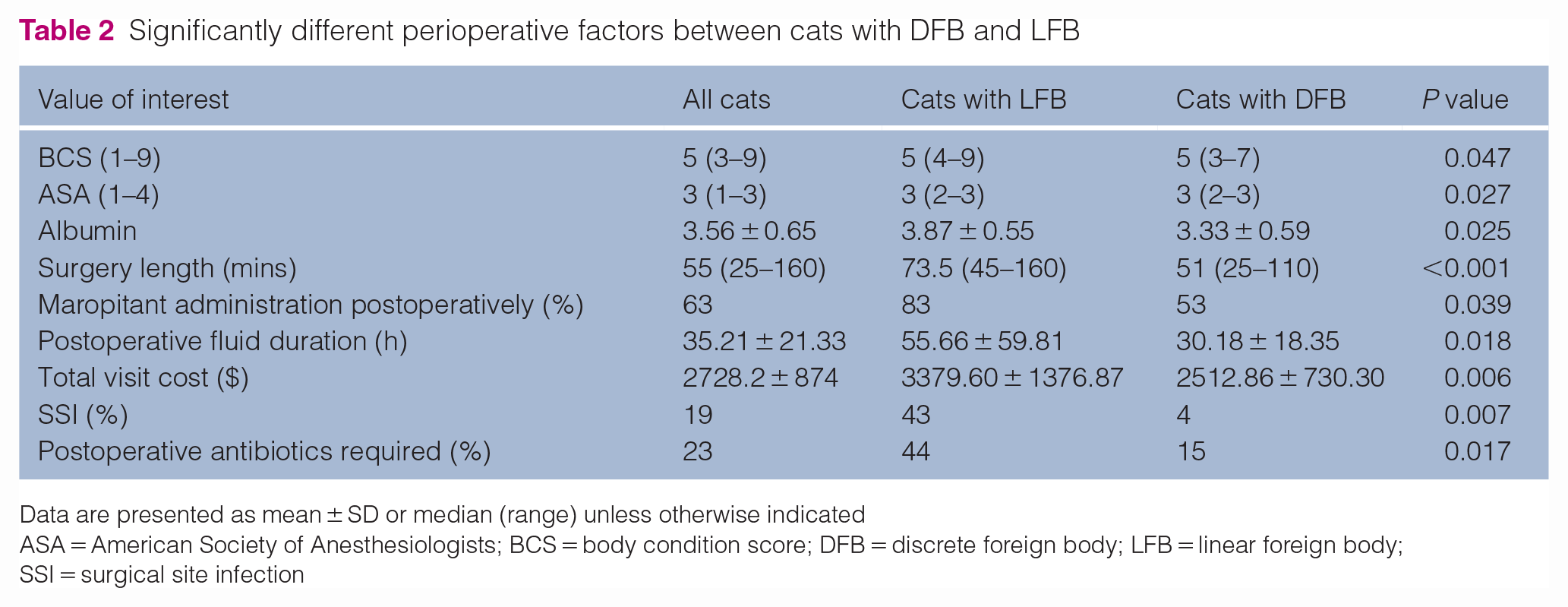
Data are presented as mean ± SD or median (range) unless otherwise indicated
ASA = American Society of Anesthesiologists; BCS = body condition score; DFB = discrete foreign body; LFB = linear foreign body; SSI = surgical site infection
There was no GI dehiscence in the cats in this study, so no cats developed septic peritonitis. All cats survived and were discharged from the hospital. Using the binomial probability series, an additional cat would have an estimated <5.2% chance of either septic peritonitis or death.
Discussion
The data presented here show that the cats in this study undergoing surgery for treatment of GI FB had an excellent prognosis with a low incidence of postoperative septic peritonitis and a high probability of survival. The hypothesis that cats would have a lower occurrence of postoperative intestinal dehiscence than historical reports in dogs was also accepted. The risk factors for intestinal dehiscence in cats could not be evaluated due to no cats in this report experiencing postoperative septic peritonitis. The hypothesis that cats with LFBs would have a more protracted clinical course than cats with DFBs was accepted, as cats with LFBs had longer surgeries, longer hospitalizations, were more likely to develop SSIs and had greater overall total visit costs.
A previous study evaluated the survival rate of both dogs and cats that underwent surgical removal of GI FBs. In that study, cats that had a DFB had a survival rate of 100% (16/16), while cats with an LFB had a survival rate of 63% (5/8) (1). This contrasts with the canine population of the same study, with a reported 94% (145/154) survival in dogs with DFBs and 80% (24/30) in dogs with LFBs. 1
Despite sparse recent literature specific to feline GI surgery, a few studies have reported on outcomes after full-thickness intestinal biopsy. Outcomes after full-thickness intestinal biopsies in cats were evaluated in multiple studies, and these procedures were found to have a low risk of dehiscence.9,14 However, hypoalbuminemia and the presence of neoplastic disease did significantly increase the risk of death or dehiscence.9,15 These studies may not represent normal GI healing given the neoplastic or inflammatory cell infiltrate and older population, so the outcomes are not entirely comparable to cats with FB obstruction.
LFBs were diagnosed in 31% of cats in this study, which is a similar percentage to a previous report in cats. 1 However, the classic presentation of a string anchored under the tongue was uncommon and only present in 17% of cats with LFBs. In this population of cats, the pylorus was the most common anchor point, noted in 44% of cats. With this information, clinicians should not rule out an LFB if a string under the tongue is not present, as this was found to be uncommon in this population of cats.
Cats with LFBs were also found to have had higher ASA statuses, potentially because they were more dehydrated and painful, making them more critical patients. Cats with LFBs also had significantly higher albumin than cats with DFBs, which was likely due to preoperative dehydration, which is similar to results from a recent paper on chronic FB obstructions in cats and dogs. 5 Cats with LFBs also had a longer surgery duration, likely due to the need for multiple GI incisions. Similar results are reported in dogs with LFB obstructions. 10 Cats with LFBs required more intensive postoperative care, as evidenced by a longer duration of postoperative intravenous fluids and a higher percentage of cats being administered maropitant. The reason for this is unclear but is suspected to be related to a higher degree of postoperative ileus because of more diffuse intestinal injury in cats with LFBs. Similar findings have been reported in dogs with LFBs. One study showed that dogs with LFBs were more likely to show clinical signs, require more surgical procedures for repair, have intestinal necrosis and perforation, be hospitalized longer and have greater hospitalization costs.5,10 Cats with LFBs also developed a high percentage of SSIs (43%), treatment of which may have further increased the hospitalization time. The cause for this increased infection percentage is unclear but may relate to a longer duration of surgery, increased risk of contamination from multiple GI incisions or a greater risk for incisional contamination during manipulation of long, contaminated, linear material.
As with any retrospective data evaluated over a long period, there are limitations related to the ability to accurately collect data from the medical records and inconsistent clinical decisions inherent in variation in personnel. Additional limitations could include clinicians’ perceptions of postoperative LFBs being at a higher risk for dehiscence, leading to hospitalizing cats with LFBs for longer and providing more intensive care. In addition, all procedures were performed in a single referral hospital and may not be reflective of FB exploratory laparotomies in general practice.
Conclusions
Cats undergoing surgery for FB removal have a good prognosis with a low risk of developing postoperative septic peritonitis or death. Cats with LFBs may require more intensive surgical therapy and postoperative care.
Footnotes
Author note
This paper was presented at the ACVS 2022 Surgery Summit.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The work described in this manuscript involved the use of non-experimental (owned or unowned) animals. Established internationally recognized high standards (‘best practice’) of veterinary clinical care for the individual patient were always followed and/or this work involved the use of cadavers. Ethical approval from a committee was therefore not specifically required for publication in JFMS. Although not required, where ethical approval was still obtained, it is stated in the manuscript.
Informed consent
Informed consent (verbal or written) was obtained from the owner or legal custodian of all animal(s) described in this work (experimental or non-experimental animals, including cadavers) for all procedure(s) undertaken (prospective or retrospective studies). No animals or people are identifiable within this publication, and therefore additional informed consent for publication was not required.
