Abstract
Toxicokinetic investigations are an essential component of nonclinical toxicology studies and generally rely on bioanalysis of plasma samples, which requires relatively large volumes of blood and, often, additional numbers of animals. Dried blood spot (DBS) analysis can substantially reduce the volume of blood needed and, therefore, presents a particular opportunity for reducing animal use in studies involving small animals; an approach consistent with industry objectives to reduce animal use and refine methods that are minimally invasive and improve animal welfare. Investigations using mice and juvenile rats indicate that implementation of DBS technology can reduce the number of animals used, and data are as good as those derived from whole blood in terms of AUC, drug-concentration-over-time curves, quantitation, accuracy, variability, and precision. These factors, and the improved data quality arising from less reliance on composite data, suggest that DBS analysis should be considered from the early stages of nonclinical development.
Introduction
Dried blood spot (DBS) methodology has been long established for the collection and storage of whole blood on filter paper prior to analysis. The technique was first described in 1913 for the estimation of blood glucose concentration 1 and became established, following the work of Robert Guthrie, in the early 1960s in the development of a cost-effective screening test for new-borns in the detection of phenylketonuria. 2 This initial work and the development of the collection and transportation of blood on filter paper led to the widespread screening of new-borns for the detection of metabolic diseases. Possibilities in DBS are continuing to develop and extend to many reaches of scientific investigation including the measurement of antibodies, 3,4 viruses, 5,6 and indicators of endocrine, immune, reproductive, and metabolic function, as well as measures of nutritional status and infectious disease. 7
In the last few years, further development in production of filter papers specifically designed for the purpose has coincided with increased use of the DBS technique in the field of drug development. Its usefulness has been demonstrated in early stage screening, 8 preclinical development, 9 and the clinical arena for therapeutic drug monitoring and human pharmacokinetic studies. 10 –13 This document focuses on the preclinical applications of DBS analysis, particularly in the determination of exposure, in consideration of the potential to reduce and refine the use of animals in drug development.
The utility of data identifying the relationship between toxicological end points and drug exposure has long been recognized and provides much needed safety data to support clinical dose setting and escalation and is recommended by all regulatory guidelines for nonclinical testing. The International Conference on Harmonisation of Technical Requirements for Registration of Pharmaceuticals for Human Use (ICH) Note for Guidance on Toxicokinetics (ICH S3A) 14 reflects the traditional use of plasma as the biological matrix of choice for toxicokinetic bioanalysis but also mentions that whole blood may be used.
In reality, it is the whole blood analysis that best represents exposure. The historic arguments in favor of plasma over whole blood are largely related to analytical accuracy and difficulties associated with manipulating and subsampling frozen blood. These limitations have led to the predominant use of prepared plasma samples. These samples can often be stored for prolonged periods under appropriate conditions, but the costs associated with plasma processing and frozen storage and shipment are significant. The cost savings of not shipping in this manner during large clinical trials have been estimated to be very substantial. 15 In addition, the preparation of plasma involves an unavoidable reduction in sample volume and the further wastage associated with pipetting steps or other sample handling results in a requirement for relatively high sample volumes, despite the sensitivity of modern analytical methods. While not of particular concern for larger animal species, blood volume limitations can become prohibitive on rodent studies. The maximum blood volume permissible to take from an individual animal (as determined by the size of the animal, the number of time points being investigated, and the blood volume required) is limited and industry guidance is available. 16 As a consequence, rodent exposure data are often derived from composite profiles compiled from multiple animals, which reduce the quality of the data and simultaneously increases the total animal usage, 8,9 associated costs, and quantity of test item required for the nonclinical development package.
Other authors have recently described advances in the use of DBS technology for bioanalysis of pharmaceutical products 17 and, as a result, this alternative biological matrix is being viewed with increasing interest by those involved at all stages of drug development. 15 In DBS bioanalysis, whole blood is spotted onto specially designed filter paper, which promotes even spreading of the blood spot and the potential for increased stability. 18 After drying and shipment/storage at room temperature, a small punch (3 mm) is excised from the DBS and processed via solvent extraction for analysis using liquid chromatography–mass spectrometry (LC-MS/MS). This presents immediate advantages over plasma methods relating to the smaller volume of blood required, no centrifugation for plasma separation, and ambient temperature sample storage and shipment. 2,8,19
Although a substantial amount of work has been performed, demonstrating the use and validity of DBS analysis 7,9,16,19 –24 and the advantages over conventional sampling methods, there has been little practical focus on optimizing the benefits of the smaller blood volume in reducing the number of animals in preclinical studies. It is clearly intuitive that smaller blood volumes should result in the use of fewer animals, indeed the blood volume required for a DBS sample is approximately 10% of that required for traditional plasma analysis but to obtain maximum benefit in this respect requires a new approach to study design and, above all, the method used to obtain the blood samples. There are potential benefits to reduce the number of animals in many different study types, but there are two particular areas where the challenges associated with obtaining sufficient sample volumes are such that the use of DBS sampling could have a major impact. These are studies conducted in mice and juvenile rats.
Typically, due to their physical size and resultant blood volume limitations, blood samples in mice are collected under terminal anesthesia, resulting in just 1 blood sample per animal. Aside from the ethical considerations involved in the use of such large numbers of animals, there is also a significant cost implication. Given the emergent use of transgenic mice in toxicology, the costs of additional animals can become disproportionate. In addition, following the global consensus on the need for pediatric clinical trials to test pediatric pharmaceutical products, legislative and regulatory changes in the clinical environment over the last decade 25 have driven an increase in the conduct of juvenile animal toxicity studies. Most of these studies are conducted in juvenile rats and there is no less imperative to measure drug exposure in these animals than in the adults used in other toxicity studies. The difficulty in obtaining blood samples from juvenile animals is not sufficient justification for omitting these data. 26,27 Not only are there limitations in the total circulating blood volume but, depending on the age of the animals, the standard blood sampling techniques may not be feasible. Overall, this has resulted in the typical use of terminal blood sampling techniques thereby increasing the number of animals required to generate data, which can often be limited to an assessment of proof of absorption in the pre-weaning juvenile. Even by sampling in this manner, in very young animals pooling of samples from different animals is sometimes necessary to provide sufficient plasma volume for bioanalysis. This is not ideal as pooling does not allow assessment of variability or calculation of mean exposure in groups.
The investigations described here set out initially to establish the DBS methodology in our laboratories and compare the results obtained from DBS samples with those from traditionally processed whole blood samples, using a current investigative new drug substance. Subsequently, a series of studies was carried out to identify and optimize blood sampling techniques that could be used in conjunction with DBS analysis when sampling from mice and juvenile rats, including serial sampling from individual animals.
Our investigations indicate that DBS methodology provides data which are as good as whole blood in terms of precision, accuracy, and variation, as well as stability. In addition, our in vivo data demonstrated that our collection methods and DBS analytical method are as good as whole blood analysis, with respect to concentration analysis and maximal and systemic exposure.
All animal work was conducted in compliance with current UK legislation: Animals (Scientific Procedures) Act 1986 and was subject to internal ethical review.
Methods
Mouse DBS Versus Whole Blood Investigation
The initial phase involved comparison of bioanalytical results for a current investigative new drug when analyzed either from DBS samples or directly from whole blood samples. The purpose of this phase was to identify any interference or other effect on the analytical results attributable to the DBS sampling method.
Detection of the analytes was by LC-MS/MS using a previously validated method. The MS was used with an electrospray ion source (ESI) and was employed in positive ion mode using selected reaction monitoring (SRM) of the mass transitions.
Mouse blood for the study was supplied by B & K Universal (Hull, UK) and was collected with EDTA anticoagulant. For preparation of calibration standard and quality control (QC) samples, blood was spiked with the analytes over an appropriate analytical range. For DBS analysis, 40 µL portions of the spiked blood were placed on DMPK type A DBS cards (Whatman, Maidstone, UK).
The test compound and its metabolite were recovered from DBSs by solvent extraction with methanol. Using a manual punch, 3-mm-diameter sections were excised from the DBS and transferred into a polypropylene tube. Methanol, 200 µL, containing internal standard were added and the tubes vortex mixed for 5 minutes. The solvent was transferred to a clean tube and evaporated to dryness under a stream of heated nitrogen at 40°C.
The analytes were recovered from whole blood by protein precipitation. Aliquots of whole blood (20 µL) were dispensed onto a protein precipitation plate positioned on a vacuum manifold, and 200 µL of methanol containing internal standard were added. After vortex mixing the samples briefly, the supernatants were drawn through under vacuum to collection tubes situated within the vacuum manifold. The supernatants were evaporated to dryness under a stream of heated nitrogen at 40°C.
Both extracted DBS and whole blood samples were re-dissolved with 100 µL of 0.1% (volume/volume [v/v]) formic acid–acetonitrile [70:30 (v/v)]) and 5-10 µL were injected into the LC-MS/MS system.
Method validation
Quality control samples at 5 concentrations were analyzed in replicates of 6 on 3 occasions (DBS) and 1 occasion (whole blood), and intrarun and interrun (DBS only) precision and accuracy were determined for the analytical methods. The specificity in each matrix was assessed by analysis of 6 different batches of mouse blood. The DBS samples were stored at room temperature and were further analyzed following storage for 24 hours, 9 days, and 34 days to assess stability. Whole blood samples were stored at approximately 4°C and were reanalyzed following 4 and 5 days storage to determine stability. Reinjection of analytical runs performed during precision and accuracy determination was performed as a means of demonstrating stability of the processed samples. Quality control samples were prepared at 5 times the Upper Limit of Quantification (ULQ) of the method and were diluted into range with the appropriate matrix to determine precision and accuracy of above range samples. Matrix effects were assessed both for the whole blood and DBS extraction procedures. For DBS, a comparison was made between 20 and 40 µL blood spots by analyzing 6 replicate subsamples from a single blood sample spotted onto the card at either volume.
Investigative Study in the Mouse
To investigate and establish a suitable in-life sampling technique for the DBS sample analysis in the mouse, female mice of the Crl: CD-1 (ICR) strain were dosed once with the test compound by oral gavage. Two hours after dosing, a blood sample was taken from each animal by the insertion of a 23-gauge butterfly needle into a lateral tail vein. While still in situ, blood flowing from the distal end of the needle was taken using different sampling techniques and immediately dispensed onto a DBS card within the animal facility. Based on the ease of use and acceptable bioanlytical results, the Microvette 100 EDTA-coated capillary (
To assess the validity of the DBS method, the concentration of the test compound found in DBSs was compared to that in whole blood collected and stored in a conventional manner. For this investigation, following administration of the test compound by oral gavage, the blood samples were taken at 6 time points equivalent to 0.5, 1, 2, 4, 8, and 24 hours after dosing. Blood samples (40 µL) were taken into Microvette 100 capillary tubes and spotted onto DBS cards (Figure 1 ). Immediately following the collection of the DBS sample, a further 0.1 mL blood was collected into an EDTA blood tube and stored refrigerated. The DBS cards were air dried at room temperature for a minimum of 2 hours prior to analysis. As the analysis is performed on a 3-mm-diameter disc punched from the DBS (Figure 1), complete coverage of the blood spot card is not necessary.
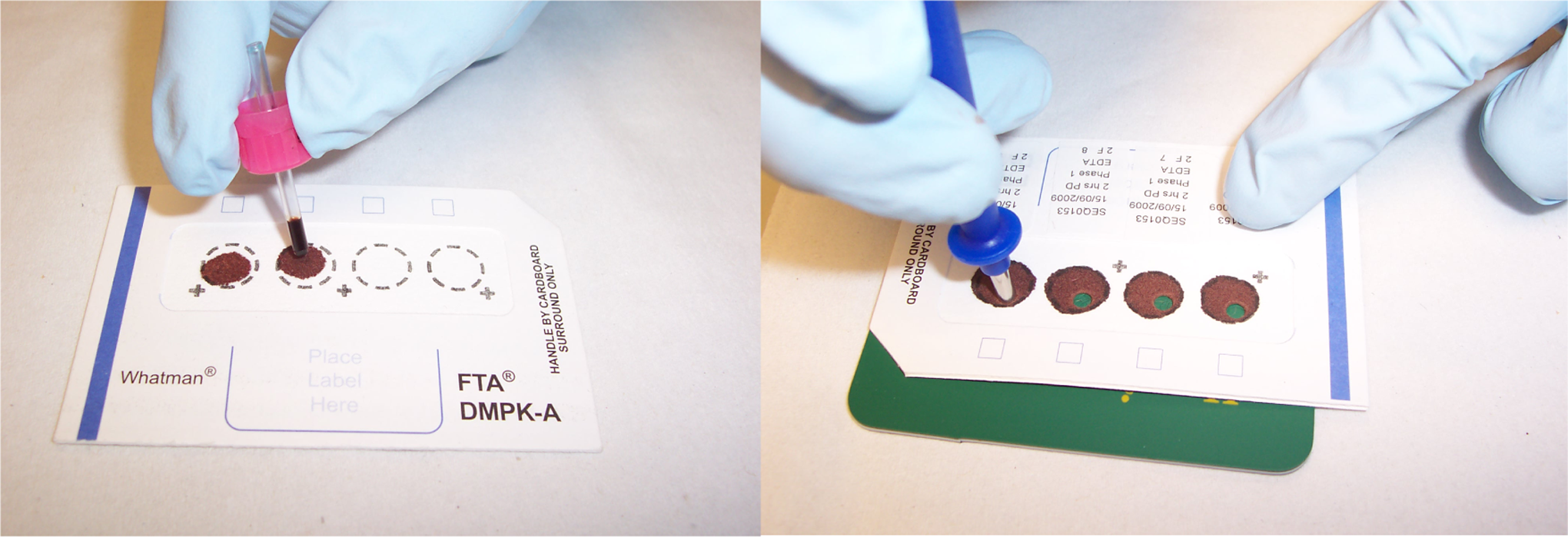
The blood sample (40 µL) is collected into an EDTA capillary tube and immediately dispensed onto a dried blood spot card (left) and allowed to dry for a minimum of 2 hours. Prior to LC-MS/MS analysis, the investigative drug parent and metabolite were isolated by solvent extraction from a 3 mm disc excised from the dried blood spot (right). LC indicates liquid chromatography; MS, mass spectrometry.
The test compound (parent and metabolite) was isolated from mouse whole blood and DBSs by protein precipitation and solvent extraction, respectively, and the processed samples analyzed by LC-MS/MS.
During this investigation, due to the blood volume required for the DBS/whole blood comparison, it was only possible to sample each mouse twice (a total of 5 mice were sampled per time point). However, using the described technique, further in-house work has demonstrated that six 40-µL blood samples can be collected from the same mouse within 24 hours. Depending on the weight of the mouse, and therefore the circulatory blood volume available (equivalent to 72 mL/kg), six 40-µL blood samples taken with subsequent recovery within the widely accepted 15% limit for the maximum blood volume that should be taken from an individual mouse.
DBS Sampling Techniques for Application With the Juvenile Rat
In the absence of any previously established non-terminal blood sampling methods for serial sampling in 7- and 14-day-old Sprague Dawley rat pups, investigations focused on the identification of a non-terminal blood sampling route suitable for DBS technology. Pre-existing blood sampling techniques were considered suitable for DBS analysis in rats ≥21 days old. An initial study first investigated different sampling techniques and the feasibility of taking repeat samples from the same animal.
In order to mimic normal laboratory conditions, pups were dosed by oral gavage with 0.5% carboxymethylcellulose, once daily from day 4 of age. A control group was similarly dosed to act as a comparator, but no blood samples were collected from these animals. On a daily basis, animals were weighed and a detailed clinical examination was conducted to monitor the tolerability of the blood sampling procedure.
Animals were sampled on day 7 and again on day 14 of age using various sampling techniques, taking a single target volume of 20 µL per animal up to 6 time points (pre-dose, 1, 2, 4, 6, and 24 hours) after dosing. Animals were then retained for 3 days after the procedure to monitor any effects of the blood sampling. In consideration of the site of sampling, common adult routes such as sublingual or orbital sinus were avoided in order to prevent any persistent damage to regions which could affect suckling ability and to avoid the use of anesthesia, which was considered undesirable in such small animals. On both day 7 and 14 of age, vessels of the forelimb digits and tail were selected as possible suitable sites in juvenile rats. Within the tail, both the lateral tail vein and dorsal and ventral arteries were assessed using a range of needle gauges, with or without the stimulation of peripheral vasoarterial dilation (using a warming chamber). Animals were restrained manually during the blood sampling procedures.
Following this assessment, the ventral tail artery pricked with a 21-gauge needle produced a sufficient blood volume with minimal injury to the pup. A second investigation was performed to further verify the feasibility of serial sampling using the established blood sampling technique. Given the propensity for juvenile blood to clot, for this investigation a target blood volume of 2 × 10 µL per occasion was implemented to reduce blood extraction time and surface clotting at the sample site. Duplicate blood samples were taken serially from pups on day 7 and again on day 14 of age at least for 6 time points. Samples were collected into an EDTA-coated capillary tube and spotted onto a DBS card. Following a period of drying, the blood spots were examined for their suitability to provide an adequate sample for DBS analysis (an area of card saturated with blood being at least 3 mm diameter). Assessment of whether the blood spot (in either sample) could yield a second viable sample was also made to indicate the possibility of a further reserve sample. Samples were considered unsuitable where the area of blood was not sufficient and, in the case of small samples, where the blood had not saturated through the card. Spots were also considered unsuitable where micro clots were present in the sample, indicating the spot was not homogeneously spread across the card.
Results
Mouse DBS Versus Whole Blood Investigation
Protonated precursor ions, [M+H]+, were observed for each compound in the ESI LC-MS full-scan mass spectra. Fragmentation of the precursor ions yielded common product ions for the parent compound and its metabolite, and these were used in the SRM mass transitions. The internal standard was a structural analogue of the parent compound and yielded similar product ions to the parent.
Precision and accuracy results were within acceptable ranges for the analytes in either whole blood or DBS.
No interference was observed in the chromatograms obtained from samples of blank mouse blood when analyzed as whole blood or DBS, demonstrating the specificity of the method. Adequate analytical signal was obtained at the method Lower Limit of Quantification (LLQ) and demonstrative chromatograms are shown (Figure 2 ). In this case, the chromatograms show the analytes eluting very close together; however, the analytes can be mass resolved since the detection is by MS/MS. The LC-MS/MS procedure has been long established and there is no cross talk (interference) between each mass transition monitored. The response, therefore, for each analyte is unbiased. The closeness of elution of each analyte also means that the analytes enter the ion source in a very similar solvent environment, resulting in similar ionization efficiency for each one.
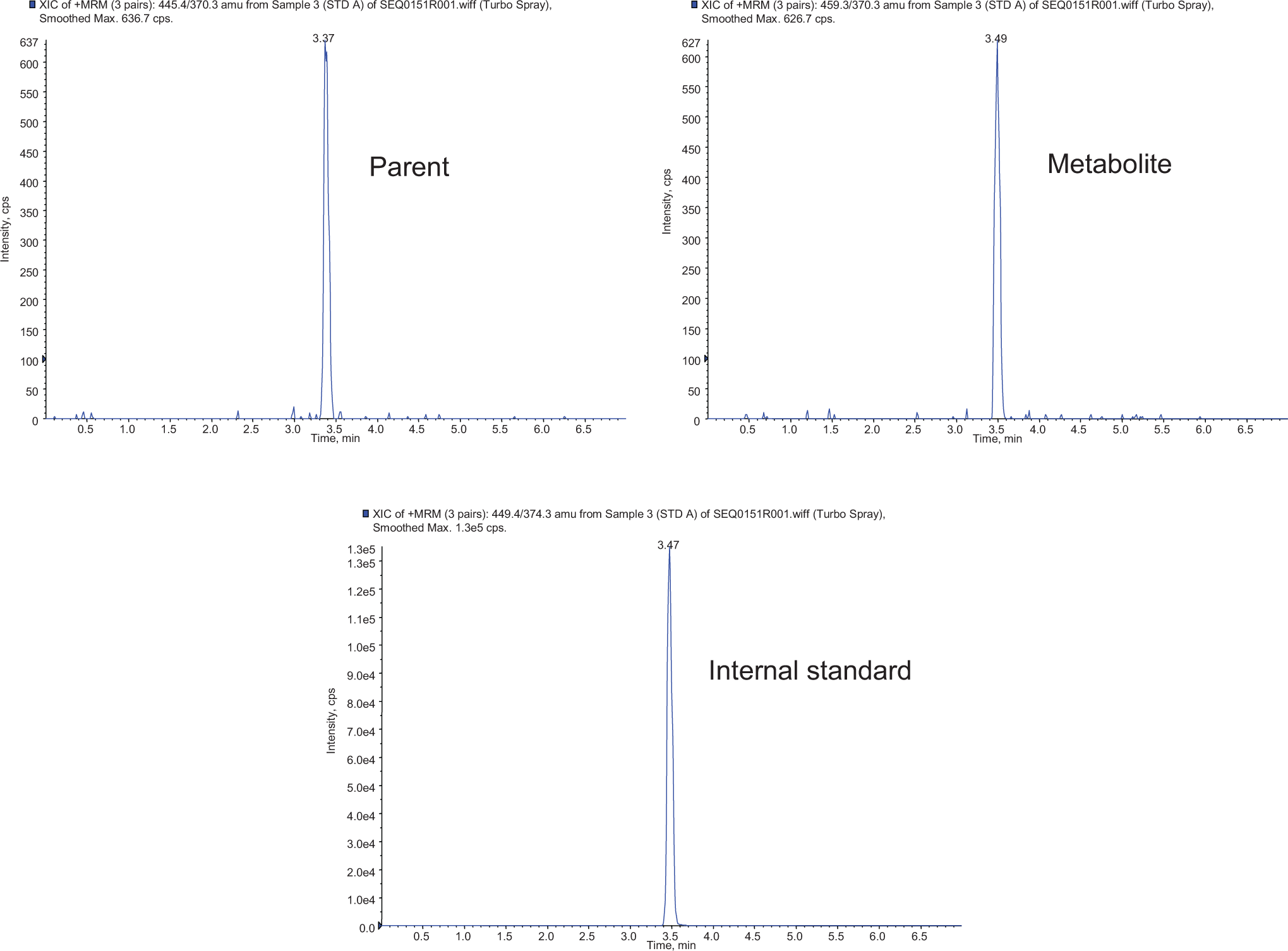
The LC-MS/MS SRM chromatograms of a DBS calibration standard show that an adequate analytical signal was obtained at the method LLQ (10 ng/mL). LC indicates liquid chromatography; MS, mass spectrometry; SRM, selected reaction monitoring; DBS, dried blood spot.
The DBS samples stored at room temperature and the whole blood samples stored at approximately 4°C were found to be stable for up to 34 days and 5 days, respectively; while the processed samples were found to be stable at room temperature for up to 3 days and 12 days, respectively. Matrix effects were found to be <5% for parent and metabolite in DBS, with a maximum value of 6.96% observed for the internal standard (all determined values indicated slight signal enhancement). For whole blood, signal suppression was observed although no greater than 11.45% for parent, metabolite, or internal standard.
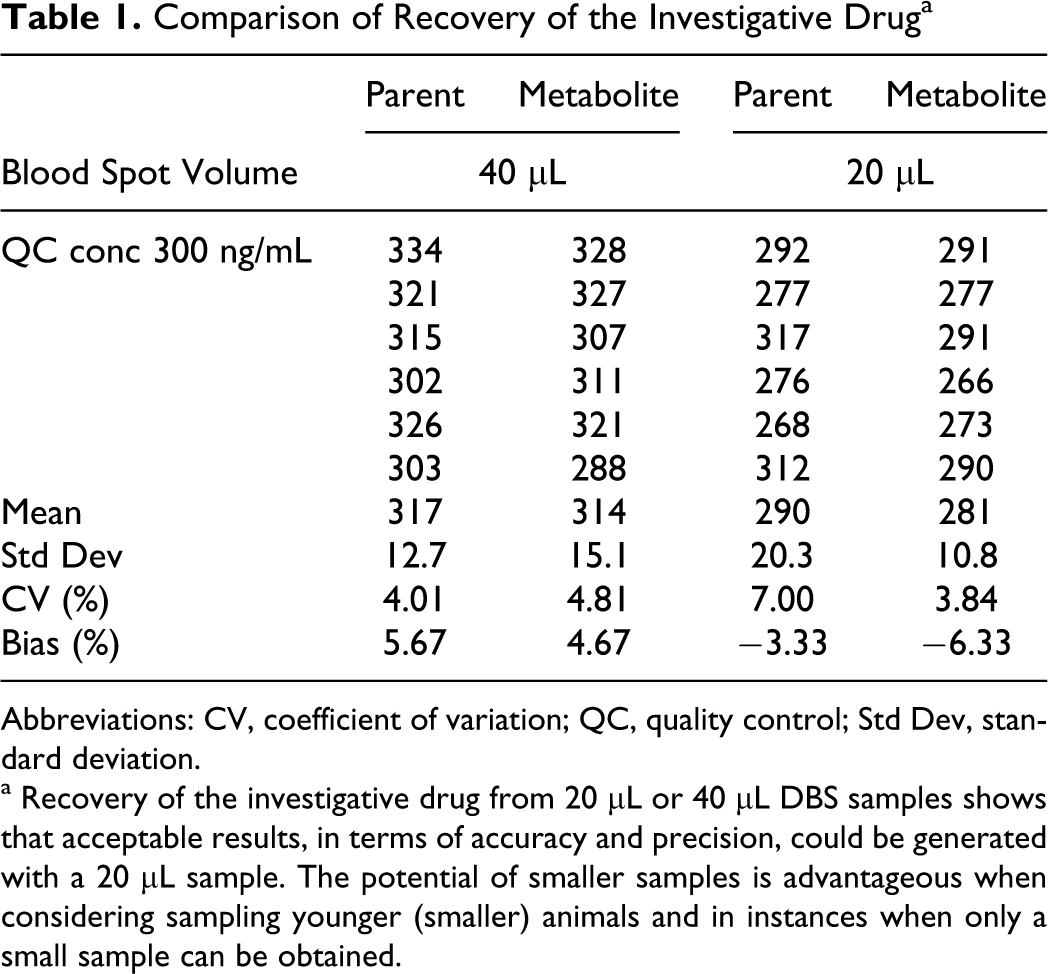
The comparison of 40 and 20 µL DBS yielded maximum intrarun precision values of 4.81% and 7.00%, respectively, for parent and metabolite and concluded that acceptable results, in terms of accuracy and precision, could be generated with a 20 µL sample. The corresponding maximum inaccuracy values observed were 5.67% and −6.33%, respectively (Table 1 ).
Comparison of Recovery of the Investigative Drug a
Abbreviations: CV, coefficient of variation; QC, quality control; Std Dev, standard deviation.
a Recovery of the investigative drug from 20 µL or 40 µL DBS samples shows that acceptable results, in terms of accuracy and precision, could be generated with a 20 µL sample. The potential of smaller samples is advantageous when considering sampling younger (smaller) animals and in instances when only a small sample can be obtained.
Investigative Study in the Mouse
The mouse blood sampling technique enabled samples to be successfully taken for application to DBS cards using a minimally invasive technique. Furthermore, serial sampling was shown to be possible with six 40 µL samples taken from the tail vein of individual mice over 24 hours, without compromising the tail for subsequent sampling.
Following administration of the test compound as a single oral (gavage) dose, ratios of maximal and systemic exposure for both parent and metabolite indicated good concordance between the DBS technique and whole blood analysis (Table 2 and Figure 3 ).
Mean Toxicokinetic Parameters of Parent and Metabolite a
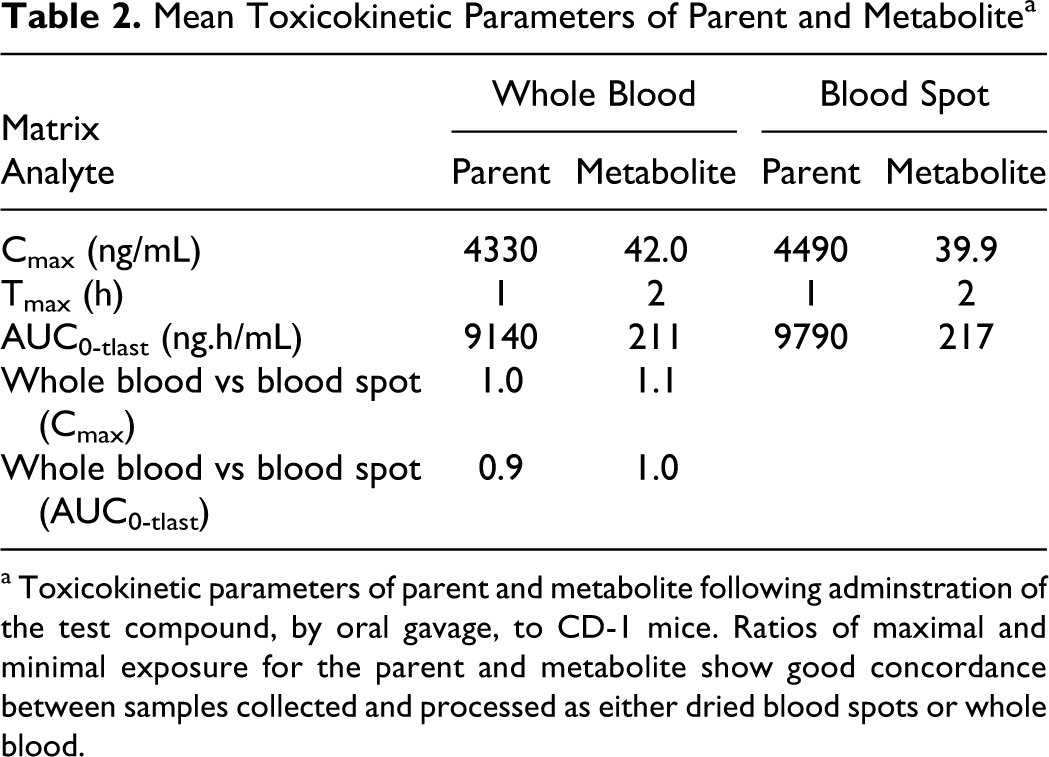
a Toxicokinetic parameters of parent and metabolite following adminstration of the test compound, by oral gavage, to CD-1 mice. Ratios of maximal and minimal exposure for the parent and metabolite show good concordance between samples collected and processed as either dried blood spots or whole blood.
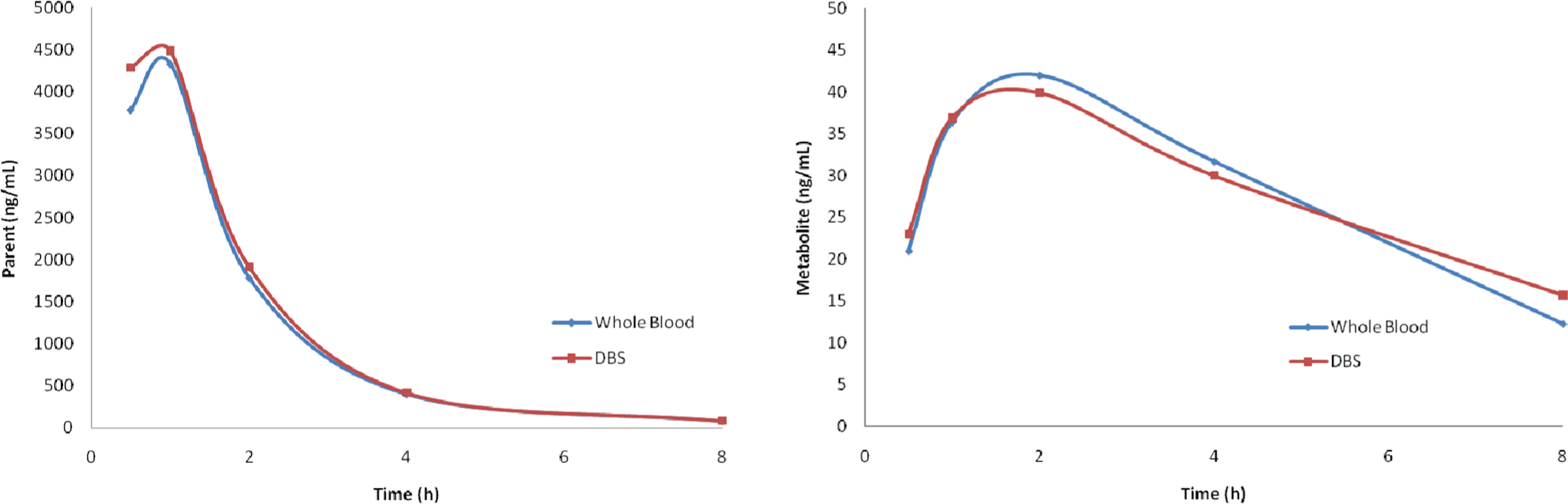
Mean analyte profiles of parent (left) and metabolite (right) following a single dose, by oral gavage, of the test compound to CD-1 mice. Analysis was performed on samples collected and processed as either dried blood spots or whole blood.
DBS Sampling Techniques for Application With the Juvenile Rat
Route identification
Sampling from the superficial toe vessels of the forelimb digits by needle puncture provided inadequate volumes of blood and was associated with significant distress to the animal; the route was therefore considered unsuitable for use at any age.
Due to the physical constraints of the tail vessels, intravenous or intra-arterial in situ positioning of the needle was not possible at any site, with any needle, and only vessel puncture and collection of the surface blood was achievable (after prior sanitization of the puncture location to reduce surface contamination)
The needle gauge was critical in providing a sufficiently large puncture to provide a satisfactory blood volume, while allowing the prompt cessation of blood flow post sampling to prevent excess blood loss. Needles smaller than 21 gauge were explored but found to provide little, if any, blood due to poor flow. This resulted in greater levels of pup discomfort due to restraint and the more frequent formation of micro-blood clots.The ventral tail artery, sampled with a 21-gauge needle, was identified as the superior route on both days 7 and 14 of age due to consistent success in achieving satisfactory blood volume and minimal distress due to rapid blood flow. Stimulation of peripheral arterial dilation was found to be superfluous and no sex difference was identified due to the similarity in physical size at this age.
Serial sampling feasibility
Following satisfactory route identification, pups were sampled at 4 time points on day 7 and 6 time points on day 14 of age. Serial samples indicated that at least 1 blood spot per time point suitable for DBS bioanalysis could be obtained from each pup. There was no associated mortality and, in comparison with controls, there were no differences in pup growth or condition (Figure 4 ). Other than a small puncture point, the tail appeared unaffected.
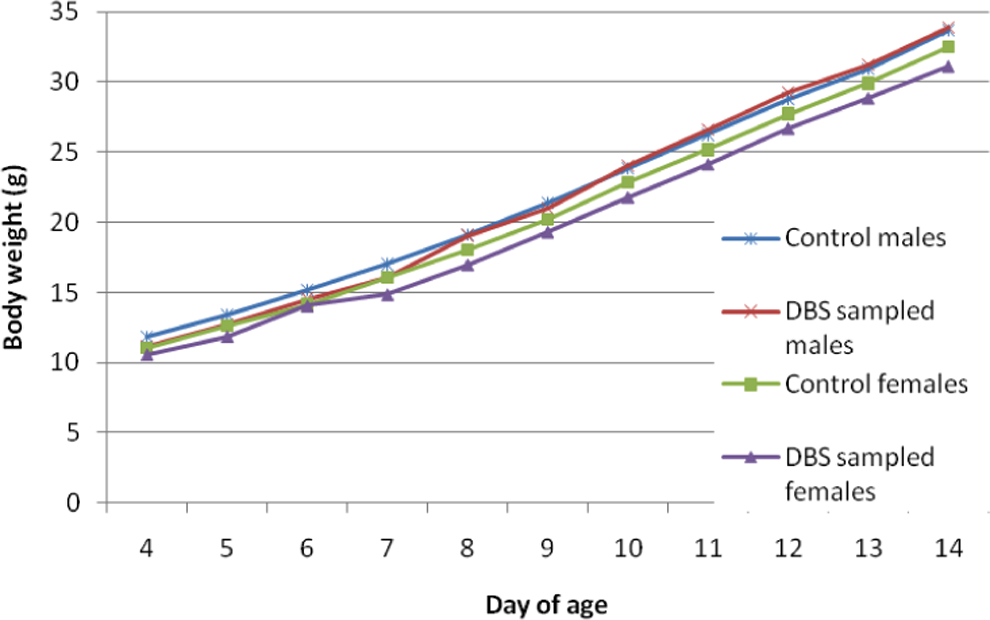
Sprague Dawley rat pups serially sampled by the DBS method on day 7 (4 time points) and again on day 14 (6 time points) show no difference in growth when compared with controls. DBS indicates dried blood spot.
In the majority of cases where a sample could not be obtained or was considered unsuitable, the second sample was viable
It was also noted that a viable blood spot would allow for two 3 mm punches to be taken and hence had the potential for 2 analyses if required. During sampling on both day 7 and day 14, there was no deterioration in the ability to obtain a viable sample from the pups.
Discussion
The bioanalytical comparison of 40 and 20 µL DBS samples demonstrated that a blood sample less than 20 µL would potentially be sufficient for analysis. The potential for this smaller volume is advantageous when considering sampling smaller (younger) animals and in instances where only a small sample can be obtained. Nevertheless, the use of a 40 µL blood volume per sample represents a substantial reduction (in the region of an order of magnitude) when compared with typical plasma methods. This would greatly reduce the number of mice required for toxicokinetic profiling and also allow for serial sampling from individual animals. The need for composite profiles, using results from more than 1 animal, would be removed with resulting improvement in the quality of toxicokinetic data and reduction in the amount of test compound required.
The volume of blood obtained per animal (40 µL) was sufficient, if required, to obtain 4 replicate samples (4 × 3 mm punches from the same blood spot). This enables repeat analysis from the same blood spot and also an opportunity to perform incurred sample reanalysis which has recently become an expectation of the US Food and Drug Administration (FDA) as part of the bioanalytical method validation. 28,29 Although there is no industry standard for a specific blood volume to be used, other laboratories have been adopting a method where a volume of blood is collected into a tube containing anticoagulant and, later, up to 3 samples of approximately 15 to 20 µL per animal are spotted onto a DBS card in a separate laboratory. We, however, have found advantages with taking one 40-µL sample including the ability to spot the sample straight from the animal onto a card, hence eliminating the requirement for additional spotting post collection. We have also found no evidence which would suggest that the homogeneity of a 40 µL blood spot is adversely affected, and data support that variations in subspot sampling are negligible and hence no cause for concern. This is due to the design of the DBS card, which achieves a uniform homogeneous spread of blood across the card. Uniform spot sizes have been previously shown to be highly reproducible. 18,21
Even though the authors’ laboratory has adopted a 40 µL method, it is reasonable to suppose that in some circumstances, for example when the use of automated processing is employed for a high volume of samples, multiple smaller spots large enough for a single punch may be more beneficial. It should, however, also be considered that further work is required from the industry as a whole before any definite conclusions can be made over the ideal size of a blood spot.
Prior to the “live” DBS sampling of any animal, some consideration should be made of factors that have the potential to affect the DBS assay. In particular, the type of DBS card, compound and metabolite stability on the card, different blood spot volume and punch size, and possible hematology effects on the test model (namely hematocrit) should be addressed on a compound-by-compound basis. Research has shown that for certain compounds the punch size, sampling from different locations on the DBS card and variation in the sample volume does not affect assay quantitation accuracy. 20
The investigative study in the mouse demonstrated that reliable results for toxicokinetic evaluation can be obtained from the mouse using the DBS technique. For this investigation, 40 µL blood samples were taken from the tail vein of the mouse after a short period of time in a warming chamber to induce vasodilation. This method of sampling was considered to have minimal impact on the welfare of the animal and overall to be far less invasive than alternative methods. To obtain a blood sample of a suitable size for plasma analysis, the usual sampling route at these laboratories is via orbital sinus puncture, which involves anesthesia, usually without recovery. This technique is, however, a potentially harmful procedure which should only be performed by skilled technicians; ocular damage due to poor technique would necessitate the termination of the animal. In comparison, the tail vein sampling method is relatively less technically challenging and the risk to the animal is minimal. It is acknowledged that other workers have reported alternative sampling routes such as submandibular and sublingual vein sampling in mice, 30 and although these generally require anesthesia, the smaller blood volume required for the DBS technique could also increase the utility of these methods.
The main benefits of DBS sampling in the mouse as part of a preclinical study are the reduction and refinement aspects which can be utilized during any such study where blood sampling is required. The low blood volume required for DBS analysis has the potential to vastly reduce the number of mice on such studies. For example, a bioanalytical method may require plasma derived from a 0.5 mL whole blood sample to assess the toxicokinetics of the test compound. According to the widely applied good practice guidance, 16 this volume would have to be taken as a terminal sample. During a typical 4 week mouse regulatory study with samples being taken at 6 time points on day 1 and during week 4, approximately 240 mice would be required for the satellite (toxicokinetic) groups alone. If DBS sampling was used, where each mouse was sampled 6 times from the tail vein (40 µL), there would be no requirement for anesthesia and all samples could be taken with recovery. The number of mice required for this study could be reduced to 24. To further reduce the number of animals, the small volume of blood required could enable these animals to be incorporated into the main study groups and the need for separate satellite groups could be eliminated altogether.
A well-tolerated and minimally invasive, nonterminal blood sampling method from the ventral tail artery of the juvenile rat has also been demonstrated. This was sufficient to provide serial blood samples (up to 20 µL) suitable for DBS analysis.
Due to the collection of surface blood, the most apparent limitation of this technique is the potential for surface contamination; however, this is minimized by the sanitization of the site prior to sampling and is also common to other sampling techniques. In addition, the limit of detection for the DBS analysis of test item must be sufficient to detect what can often be very low circulating blood levels in juvenile animals. It is felt that this latter consideration requires further validation work with a range of analytes in order to fully assess its impact. It should, however, be considered that solvent extraction can be conducted on multiple card punches to increase signal strength and, therefore, even low circulating blood concentrations may not discount the use of DBS bioanalysis.
The low blood volume required for DBS sampling could result in a drastic reduction in the number of animals required for toxicokinetic evaluation in juvenile toxicity studies, negating the use of terminal or vena cava sampling as is currently customary for pre-weaning juvenile rodent toxicity studies. When compared with the typical numbers routinely required for standard plasma bioanalysis, assuming 1 pre-weaning occasion of 6 time points with a 0.5 mL whole blood volume, up to a 70% reduction in the number of animals could be achieved by the use of DBS bioanalysis (72 animals/sex vs 16 animals/sex).Aside from the clear ethical attraction, decreasing the numbers of animals required also represents a substantial cost-benefit and reduction in the requirement for test compound. Furthermore, due to the repeat sampling feasibility, serial exposure profiling at multiple occasions now becomes a more realistic option for juvenile toxicity studies. This would significantly refine the drug exposure data and allow assessment at critical developmental time periods for key organs.
The main perceived disadvantage of the DBS technique relates to the historical use of plasma analysis. Clearly, plasma and whole blood results are not directly comparable due to the concentration effect of plasma separation and potential binding in the cellular fraction of the sample so it is best to use consistent analysis techniques throughout the drug development program. For programs already underway using plasma analysis, it may not be efficient to change to the DBS method (although potential cost savings in transport and storage of clinical samples should be taken into account). For investigational new drugs embarking on non-clinical studies to support first-in-man trials, serious consideration should be given to developing and validating the bioanalytical methods using DBS.
Possibly the greatest cost saving opportunity lies within the high volume of samples generated during large clinical trials; an area where the pharmaceutical industry is already seeing the advantages of DBS sampling. For such trials, the procedures are simplified due to the ease of sampling (finger prick rather than venous cannula) and the plasma preparation step/frozen storage can be eliminated. For a high volume of samples, one concern from the bioanalyst’s point of view may be the processing of the DBS cards required prior to analysis, particularly taking hole punches from the DBS cards. This has led to a current focus on automated processing where a range of robotic devices can punch out many samples per hour and direct the discs into a 96-well plate for analysis. Initial testing has also explored the possibility of extracting analytes directly from the DBS card, eliminating the hole punching step completely. 31
Following increased demand for DBS analysis as part of initial preclinical development and early toxicokinetic studies, DBS analysis has been used on a variety of different species including the rat and dog. The small volume of blood required for DBS analysis may also prove beneficial over the current sampling method used in the minipig where DBS sampling methods have more recently been investigated at this laboratory. The traditional method of taking blood from a minipig is via the cranial vena cava, which is both stressful to the animal and potentially dangerous. Initial investigations using DBS sampling methods have established that a small volume of blood suitable for DBS analysis can be obtained from the marginal ear vein up to 6 time points on 2 separate occasions 1 week apart. As good samples were obtained on each occasion, DBS sampling seems a favorable alternative for toxicokinetic blood sampling in the minipig.
Concluding Remarks
Overall, it is concluded that the non-terminal mouse and juvenile blood sampling methodology identified by these investigations support the future use of DBS analysis in non-clinical studies for safety assessment representing a superior approach for blood sampling in terms of ethics, cost, and quality of data. It is felt that the use of this technology could revolutionize the attainment of drug exposure data, allowing a more robust and comprehensive assessment.
Other potentially substantial cost benefits in relation to sample processing, storage, and transportation, both in the non-clinical and clinical settings, are such that the use of the DBS technique should perhaps be the default for early stage bioanalytical method development.
Footnotes
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding provided by Sequani Limited, Bromyard Road, Ledbury, HR8 1LH, UK.
The author(s) received no financial support for the research, authorship, and/or publication of this article.
