Abstract
Study Objectives: To examine the survival rate and differences in fall-related health service use among community-based participants of the Stepping On fall prevention program compared to controls in the year before and three years after program initiation. Study type: Case-control retrospective study using linked ambulance, emergency department, hospital and mortality data. Methods: 39,014 individuals admitted to hospital in New South Wales between 1 July 2005 and 31 March 2016, including 7,964 from the Stepping On program and 31,050 controls, were matched using propensity score analysis. We used competing risk analysis to assess fall-related mortality and described the patterns in acute and fall-related health service use one year pre-program (index) and three years’ post-Stepping On program completion. Results: Overall Stepping On participants had higher health service use in the pre-index program period compared to controls. Three-year post-index showed a trend towards reduced fall-related mortality (hazard ratio 0.84, 95% CI 0.66-1.05), along with plateau in health service use for the Stepping On program participants compared to the control group, whose service use increased over a three-year follow-up time. Conclusions: Patterns of service use suggest Stepping On program benefits are sustained for a short period of time. The greatest improvements were found in the very old group (85+ years) who undertook the program, which could potentially help reduce the unnecessary use of healthcare services for falls and prolong survival. While interpretation of the results ought to be addressed with caution, they suggest the need for ongoing program refreshment to achieve lasting effects.
Introduction
Approximately 34% of Australians aged 65+ years fall annually. 1 Additionally, 50% of older adults (>80 years) experience at least 1 fall each year, 2 of which 30% of these result in medical attention with a proportion leading to disability or death. 3 Falls among older people can have a major impact on the individual, their family, community and health services, due in part to injuries sustained (e.g., lacerations and fractures) and/or ongoing psychological impact (e.g., fear of falling and fear avoidance behaviors that lead to unnecessary restrictions in activity). 4 Falls and fall injury among older people may result in health service use, such as hospital admission, 5 or even admission to residential aged care. 6 Ambulance services are generally their first point of call, of which 75% are transported to the emergency department. 7 Rates of hospitalizations and other healthcare use following falls, particularly injurious falls, continue to rise, 8 with some older adults, particularly those in, residents of aged care facilities, at greater risk. 6 Fall-related health service use by older adults is also associated with high costs. 9
Systematic reviews10,11 provide clear evidence that falls in older people can be prevented with evidence-based programs. Such injuries and related health service use may be reduced by providing appropriately validated preventative intervention programs to reduce the risk of falls. 12 Stepping On is a fall prevention program for community dwelling older adults incorporating behavior change, education and exercise that has been shown to prevent falls13,14 and fall-related healthcare use 15 while enhancing self-efficacy. 13 Stepping On is directed at older adults with good cognition who walk unaided but who identify to be at risk of falls, owing to a previous fall or by expressing a fear of falling. The program consists of 7 weekly 2-hour group sessions conducted in a community setting, led by a trained professional. Each interactive session includes discussions on topics related to falls followed by an exercise session; participants are also provided a home exercise program. Weekly sessions often include a volunteer subject matter expert who discusses topics related to healthy aging and fall prevention, for example, managing medications, home and community safety. 13
Beginning in 2009, the health department of Australia’s most populous state of New South Wales (NSW), began implementing the Stepping On program among adults aged 65+ years to combat the rising rates of fall-related hospitalizations. 8 The project reported herein is part of a series of studies determining the impact of this state-wide rollout of Stepping On on fall-related healthcare utilization among older residents of NSW. Previously, we reported that due to limited reach there was no detectable impact on health service usage for falls across the state-wide older population. 16 However, among community-dwelling program participants (i.e., older adults at risk of falls) it appeared the Stepping On program mitigated fall-related healthcare utilization. The study found that controls increased their health care use while Stepping On participants reduced use 15 such that there were no differences between groups over the long term (1-3 years).
Over the next 50 years the Australian population is expected to double, with the proportion of people aged 65 and over increasing from 15% in 2014 to 23%. The increase in the older population is also predicted to increase health service use and health expenditure for those over 65 years of age. 17 Additionally, increased use of health services, particularly hospitalizations, is common in older adults in the final years of life.17,18 This includes hospitalizations arising from fall-related injuries. 19 Nonetheless, previous research has shown that proactive use of health services by older adults may be associated with better physical functioning and prolonged survival. 20 As such, programs such as Stepping On may be protective against ongoing functional decline and mortality among older adults with previous hospitalization. This study therefore examined the fall-related survival rate and differences in health service use among participants of Stepping On by age categories 60 to 74 (young old), 75 to 84 (old aged) and 85+ (oldest old) with previous hospitalization compared to matched hospital controls over a 3-year period following program participation.
Methods
Data Collection
This study analyzed state-based hospital, emergency department (ED) and ambulance linked administrative data from routinely collected information to determine fall-related health service use. Presentations to hospital (i.e., over-night stay) from a fall sustained outside hospital, with or without an associated injury were extracted from the NSW hospital Admitted Patient Data Collection (APDC), visits to a hospital ED due to a fall were extracted from the NSW Emergency Department Data Collection (EDDC) , and calling an ambulance or being attended by a paramedic due to a fall were extracted from NSW Ambulance’s Computer Aided Dispatch (CAD) and Patient Health Care Record (PHCR)/Electronic Medical Record (EMR) databases, which is a centralized system used for logging and dispatching emergency and patient transport calls and includes documented clinical information collected during patient care episodes f in NSW. Data between 11 June 2005 and 31 March 2016 were used in analyses. The administrative datasets collected information on all public and private patient presentations to any of the mentioned services. The NSW Registry of Births Deaths and Marriages (RBDM) dataset provided information about a participant’s death date; where this was missing, the Australian Bureau of Statistics (ABS) mortality data was used to fill in any missing dates and to determine a participant’s cause of death. Further definition of health service use calculations may be found in Supplemental S1.
Sample Population
Participants who took part in the Stepping On program from 11 June 2009 until 17 February 2015 were included in the study. The Centre for Health Record Linkage (CHeReL) conducted a preliminary matching process to reduce the eligible control pool of hospitalized people (for more information about this first phase of control matching please refer to Supplementary 2 of Paul et al 15 ) and returned a total of 260,909 persons from the APDC to the research team. Controls were residents of the state of NSW, aged 65 years or older who had a hospital admission and who did not have a diagnosis of dementia (ICD10-AM codes “F00-F03,” “F05.1” or “G30-G31”) before the matched Stepping On cases’ date of program enrollment.
Statistical Analysis
Firstly, propensity score analyses were performed to create a matched sample population of Stepping On participants and controls. Propensity score methods are used to estimate the treatment effect in adjusted analyses applied to observational study data when random assignment is not possible. Propensity scores are assigned as the probability that indicates the likelihood of a study participant being enrolled in the Stepping On program conditional on a participant’s measured baseline covariates 21 by controlling for covariates that may determine a participant’s potential probability of having the intervention, allowing study participant groups to have the same distribution of measured baseline characteristics. Furthermore, propensity scores reduce potential confounding and bias in the analysis 22 and allow comparable and representative comparisons between the Stepping On and control groups. 21 Logistic regression models were performed to estimate the predicted probability of being in the Stepping On program.22,23 Participants identified with a higher propensity score have a higher probability of taking part in the Stepping On program, while those with a lower propensity score have a lower probability of taking part in the program. 21 Matching based on sociodemographic variables, hospital information and chronic conditions (Table 1) was performed on a half-year accrual block process with matched controls excluded from the preceding block. Matching using a 1:4 (Stepping On vs controls) optimal matching method and a caliper distance of 0.2 was applied. 24
Descriptive Characteristics of Pre-Index Categorical and Continuous Variables After Matching of Intervention and Control Groups.
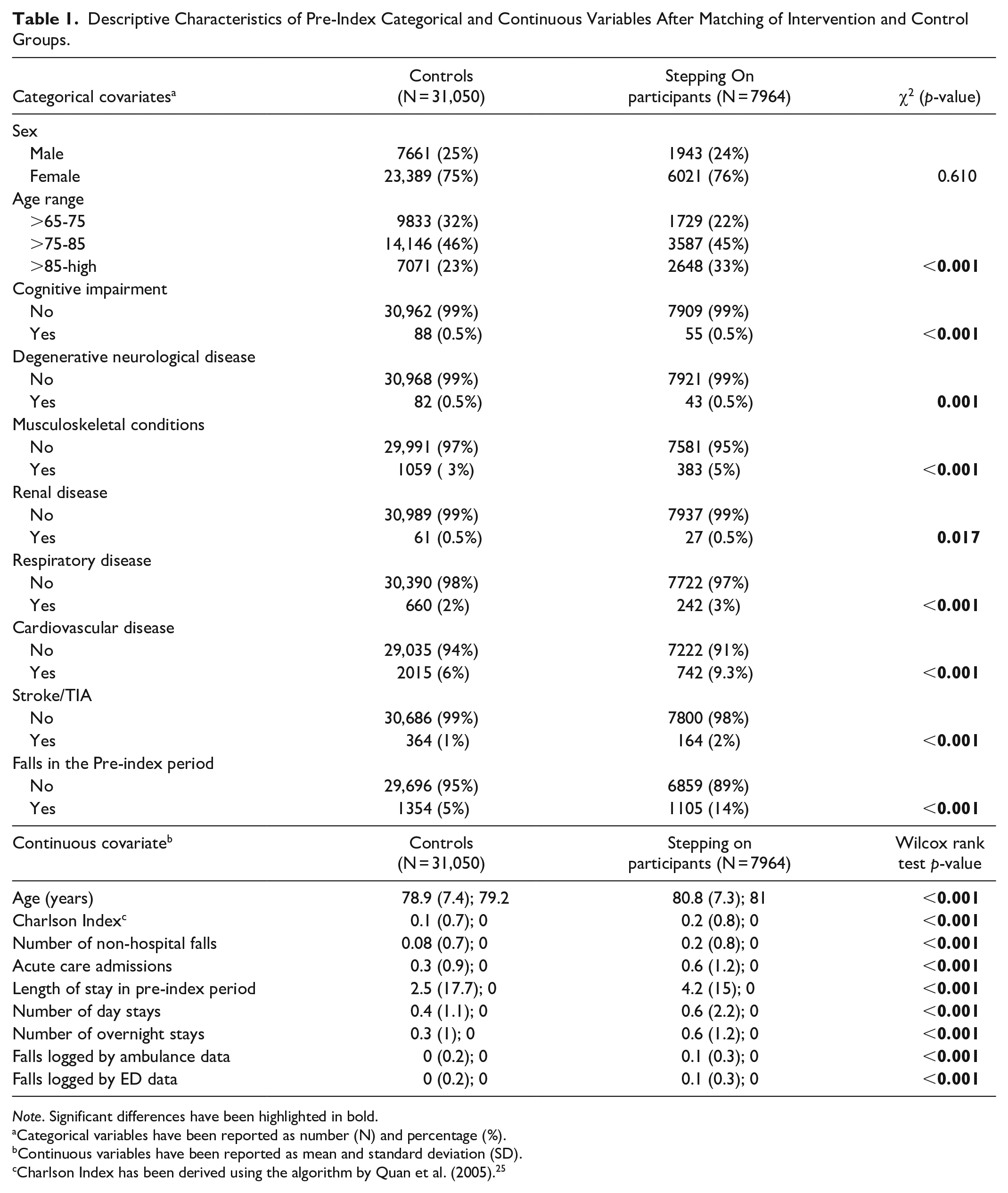
Note. Significant differences have been highlighted in bold.
Categorical variables have been reported as number (N) and percentage (%).
Continuous variables have been reported as mean and standard deviation (SD).
Charlson Index has been derived using the algorithm by Quan et al. (2005). 25
Descriptive statistics for continuous variables reported the mean and standard deviation (SD), except where otherwise indicated. Paired t-tests were used to present bivariate comparisons for continuous variables, while chi-square tests were used for comparisons of categorical data. All p-values < .05 were considered significant.
Number of deaths were specified using the RBDM and ABS datasets. Standardized mortality rates were calculated as the ratio of actual days of follow-up to the end of the 3-year study period or mortality, and the standardized mortality ratio (SMR) as the ratio of actual mortality to expected risk of death. The value of SMR was evaluated by sex and by age range risk groups (young old (<75), old aged (75-84) oldest old (85-94 and 95+ years) ) and included patients’ intervention group (Stepping On and controls). Sex and age specific mortality rates have been expressed per 1000 persons in those sub-groups.
Survival was calculated from the date when participants were discharged from hospital and censored at date of death (using RBDM and ABS mortality data) or end of the study (up to 3-years). Fall-related mortality was defined as death (all-cause) occurring within 30 days of a fall-related injury, as this period captures the majority of deaths directly attributable to the initial trauma and its complications. 26 Fall-related mortality was identified from the ambulance, emergency department, hospital or death data. (see Supplemental S1). We performed Cox’s proportional hazards regression models, adjusting for covariates with standardized differences (>0.1) after propensity scoring; this included sex, age and risk factors (falls in the pre-index period and cardiovascular disease; Table 1), to obtain estimates of relative all-cause mortality (with 95% confidence intervals) and to calculate hazard ratios for all-cause mortality and competing-risk models for fall-related mortality, by comparing Stepping On to controls, using days from hospital discharge as a time scale.24,27
Since the Stepping On program aims to reduce the risk of falls and maintain independence for older frail community members (those aged 75 and over) 28 , health service use was described for the subset of the participants in the old and oldest old age groups (75-84 vs 85+). Patterns of health service use for the subset of Stepping On and control group participants are presented descriptively (i.e., no statistical comparisons were performed) as the number of presentations divided by the total person-years. Rates are then reported per 100 person-years, which was calculated as the number of reported cases for the incident of interest (e.g., hospital stay) during the follow-up time interval divided by the summed person-years of observation during the follow-up time interval. All health service use reported in the graphs have standardized rates by a scaling factor of 100 person-years for ease of comparison between the different subgroups. Time periods have been presented as 12-month pre-index, 1-year post-index, 2nd year post-index, and 3rd year post-index, with index being the start date of Stepping On.
Data were analyzed using the statistical software SAS version 9.4, SAS Institute Incorporated, Cary, NC, USA.
Results
The estimated sample of people who were admitted to hospital included 9909 Stepping On participants (after excluding 403 duplicates) 29 and up to 197,154 potential controls. Of the 271,215 records provided by the CHeREL, 225,051 were eligible for the propensity score estimation, of which 197,154 (95.9%) were controls and 8426 (4.1%) Stepping On participants. On completion of the propensity score matching our sample was reduced to a sample of 39,014 (7964 Stepping On participants compared to 31,050 controls; Figure 1).
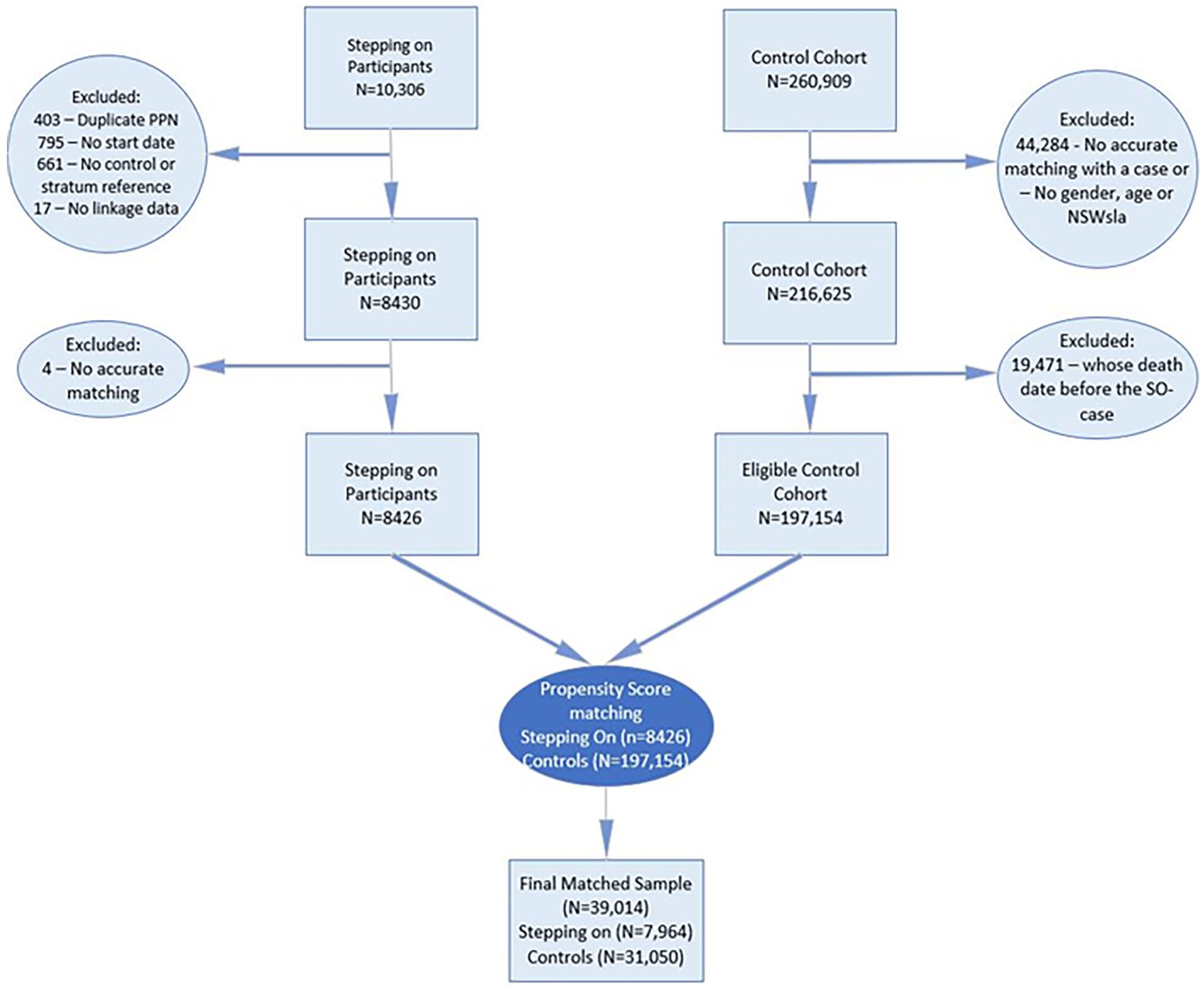
Flowchart of the propensity score matching for Stepping On participants and Controls.
The baseline characteristics of both groups are shown in Table 1. Before propensity score matching, Stepping On and control groups were significantly unbalanced across clinical characteristics, with the Stepping On participants exhibiting more musculoskeletal conditions, falls prior to the index fall-related hospitalization, cardiovascular disease, respiratory risk factors and more use of health services (Table 1). These results suggest that participants in the Stepping On group had a higher comorbidity burden, health service use and falls at pre-index than those in the control group.
Propensity Score Process
Propensity score models aim to control for confounding rather than predicting outcomes, therefore some variable constructs may overlap.30,31 All variables included in the propensity score models are shown in Table 1. After performing propensity score analysis, age, falls in the pre-index period, pre-acute care admissions, number of overnight stays, falls logged with an ambulance and ED visits had standardized differences >0.1 and were added as covariates in the final Cox proportional hazard models. After performing propensity score 1:4 matching (Stepping On: N = 7964, vs Controls: N = 31,050), significant differences between Stepping On and control groups existed except for sex (p-value: .61). The covariates with the greatest differences between Stepping On and control groups were for falls in the pre-index period (14% vs 4%) and a hospital diagnosis of cardiovascular disease (9% vs 7%). Fall related outcomes and age-sex SMR per 1000 population are reported in Supplemental S2.
Fall-Related Death and Health Service Use
Of the 39,014 individuals included in the study across both groups, 7771 (19.9%) had a fall leading to health service use or death in the 3-year follow-up period. In total 3767 (9.7%) of the sample population died, of which 1358 (36%) of all deaths were due to fall-related mortality and the remaining 2409 (64%) were defined as all-cause mortality. The time to all-cause mortality results are presented in Supplemental S3.
In Stepping On participants, standard and competing risk adjusted models were examined for fall-related mortality (Supplemental Table S3). The Stepping On program was found to be associated with decreased hazard ratio (HR: 0.96, 95% CI 0.73, 1.27) and sub-distribution hazards (HR: 0.84, 95% CI 0.66, 1.05) for fall-related mortality but increased hazard for all-cause mortality (HR: 1.03, 95% CI 0.98, 1.09) in the multivariable analyses. However, these results were not statistically significant.
Figure 2 shows the estimated cumulative incidence functions for fall-related mortality with a competing risk of all-cause death for the 4 groups (Control: men and women and Stepping On: men and women). Cumulative risk estimates from Kaplan-Meier estimators produced higher 3-year risk estimates in men than women and higher estimates for those in the control group compared to the Stepping On group. There was a clear separation of the 4 groups: female Stepping On participants had the lowest probability of fall-related mortality, while male controls had the highest probability of fall-related mortality. This pattern was consistent across follow-up, however, the gap increased across the groups after 2-years of follow-up (Figure 2).
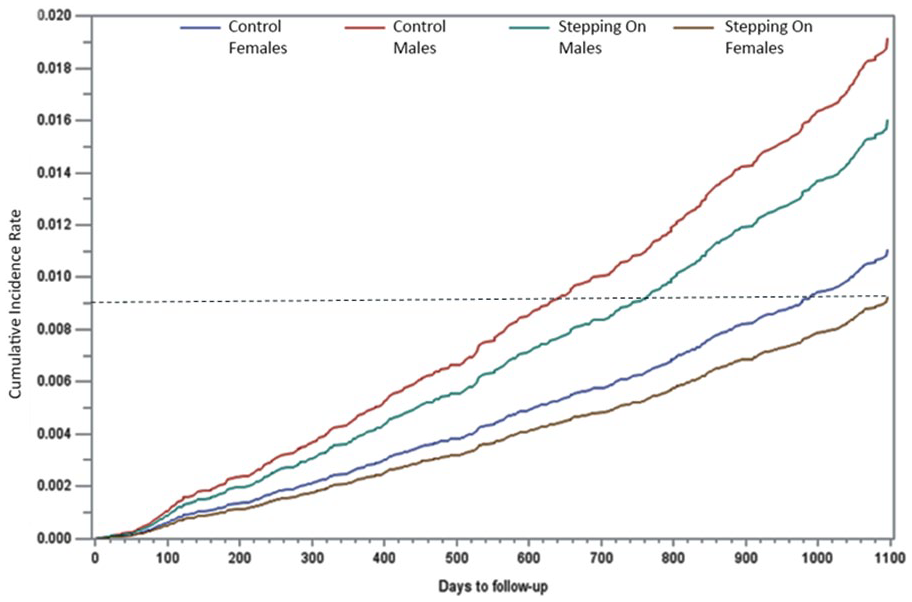
Cumulative Incidence fall-related mortality with competing risk of all-cause death.
Figures 3 and 4 are descriptive, and no inferential statistics were performed. Nonetheless Figure 3 shows the collection of hospital and ED fall-related presentations by age and intervention group per 100 person-years. Stepping On participants had considerably higher rates of fall-related presentations to hospital or the ED at pre-index, however, these rates remained relatively stable over the 3-year follow-up period compared to the control group. Importantly, the majority of fall-related presentations by Stepping On participants aged 85+ years stabilized over time with the exception of any fall-related presentation to the ED, including those who were or were not admitted to hospital. Interestingly, these rates were still lower than those in the control group at 3-year follow-up (Figure 3). Of patients who had experienced a fall-related presentation to hospital or the ED, similar trends in service use were seen between Stepping On and control groups (Figure 3) to those for all health service use (found in the Supplemental S4).
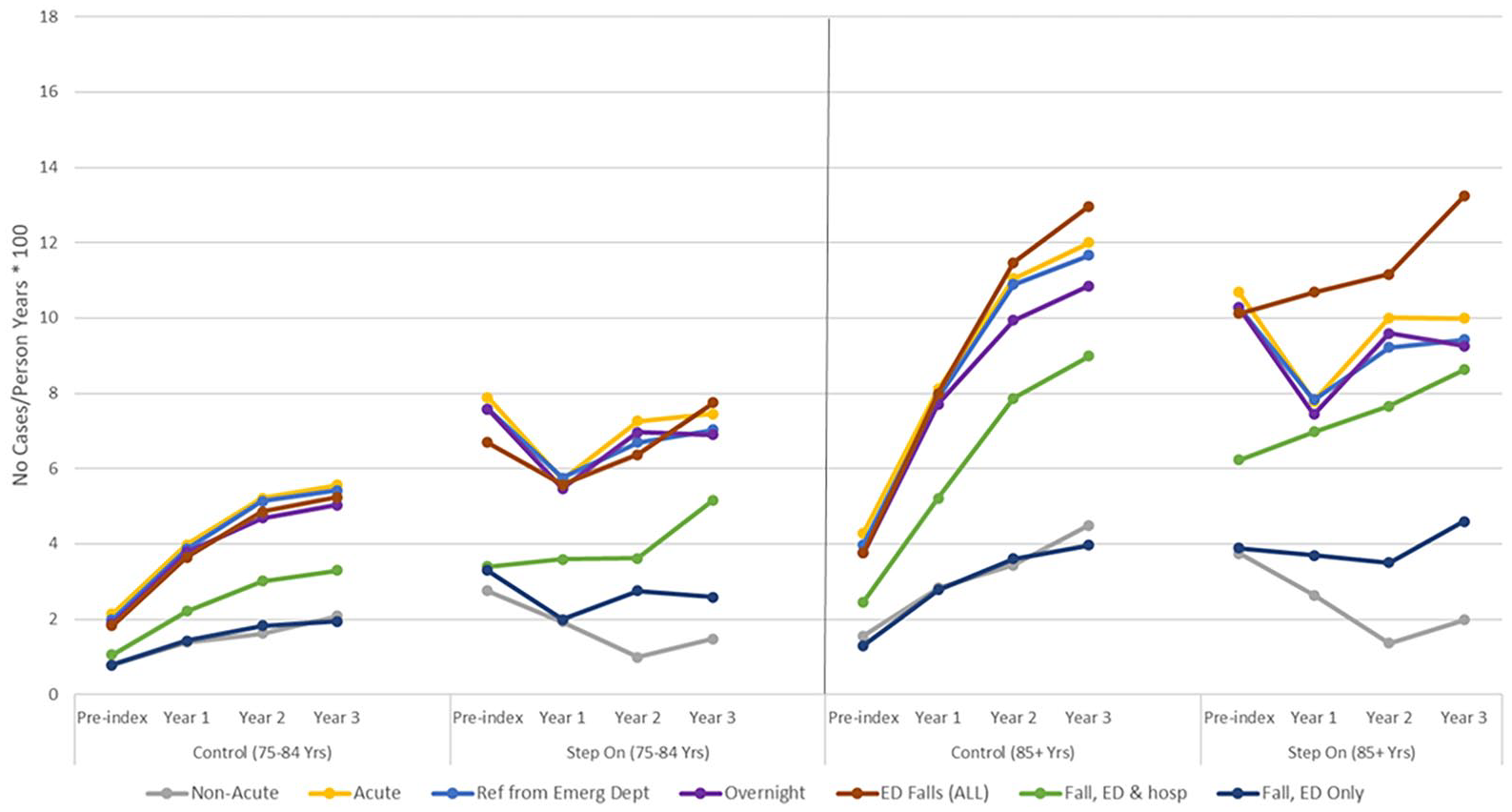
Hospital and ED fall-related presentation by age and intervention group per 100 person-years. Reference from Emergency Department (ED) represents admissions to hospital from the ED ED falls (ALL) represents all presentations to the ED due to a fall. Fall, ED & Hospital represents presentations to the ED due to a fall that resulted in a hospital admission. Fall, ED Only represents presentations to the ED due to a fall, but no hospital admission was required.
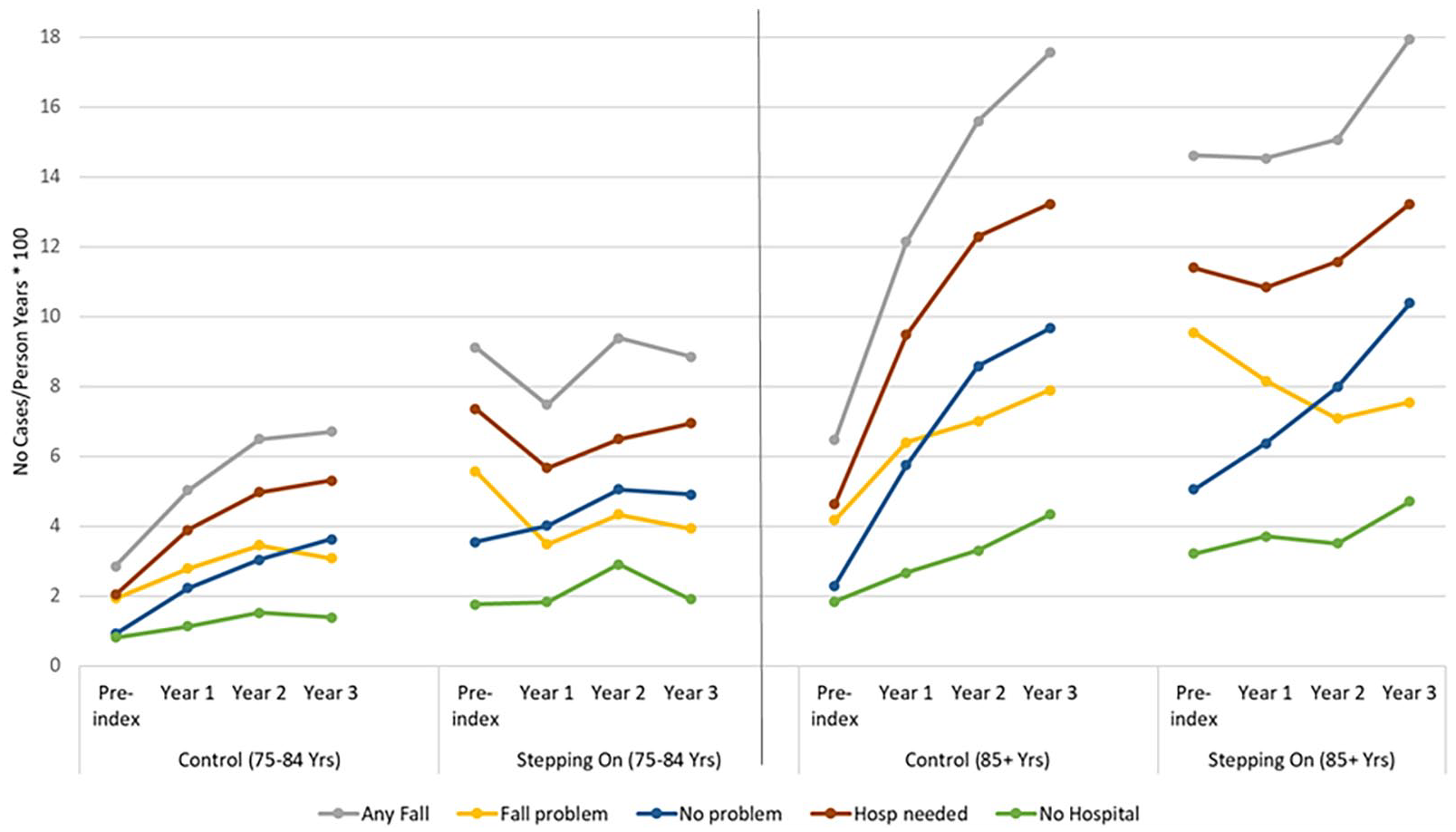
Ambulance fall-related call-outs by age and intervention group per 100 persons per years.
Most fall-related ambulance calls resulted in an ED presentation (Figure 4). Ambulance fall-related presentation to the ED made up the majority of fall-related ambulance callouts for both age groups and intervention groups. When controls versus Stepping On patients were examined, ambulance callouts that resulted in an ED presentation varied by age group. Amongst the 75- to 84-year-olds, increased rates of ambulance call-outs that resulted in an ED presentation between pre-index and 3-year follow-up were seen in the control group (from 2.04 to 5.31 per 100 persons per year). In contrast, rates decreased marginally in the Stepping On group (from 7.36 to 6.95 per 100 persons per year). For participants aged 85+ years, the greatest increase in fall-related presentations between pre-index and 3-year follow-up appeared in the control group compared to the Stepping On group (from 4.63 to 13.23 vs 11.41 to 13.23 per 100 persons per year, respectively). For ambulance call-outs due to a fall, patients in the control group showed similar callouts compared to Stepping On participants at 3-year follow-up (75-84 years: 1.93-3.08 vs 5.58-3.94 per 100 persons per year, 85+ years: 4.17-7.9 vs 9.55-7.55 per 100 persons per year, respectively). Interestingly, patients aged 75-84 and 85+ years in the Stepping On group continued to show a decrease in fall-related ambulance callouts at the 3-year follow-up even if they ceased participating in the program.
Discussion
Falling or fear of falling is one of older adults’ concerns due to restrictions in physical fitness, frailty and increased instability. Community-based exercise programs have been designed to reduce fall risk by helping older adults develop effective strategies to reduce their risk. Many government organizations globally have undertaken initiatives to disseminate exercise programs to support vulnerable adults. Programs such as the Otago Exercise Program, Tai chi: Moving for Better Balance and the Stepping On Program have been developed to directly target falls prevention and have shown to offer positive net benefits .32 -34 We investigated the Stepping On program which has been found to be sustainable, cost-effective and comparable to the other programs33,34 and examined fall-related survival and differences in health services use (for falls and all causes) among Stepping On participants with previous hospitalization and matched hospital controls following program participation. As the individuals included in the study had previous inpatient admissions, the Stepping On participants were a subset of this group. Fall-related mortality was less among Stepping On participants compared to controls, particularly for women aged 75 years and older, and males aged under 85. Across different age subgroups, we found that health service use stabilized in the Stepping On fall prevention program participants over a 3-year period.
Findings from our study revealed that healthcare use can be substantially reduced for older people who undertake an individualized fall prevention program such as Stepping On. These effects were seen for hospital and ED visits for fall-related issues by adults aged 85 years and over. The reduction in health service use following program participation may reflect increased robustness and health, as a previous study found that frailty and falls both reduced up to a year following participation in Stepping On, with many who improved physical function maintaining ongoing exercise. 35 The oldest old participants (85+ years) who were involved in the Stepping On program in the pre-index period were more likely than controls to access health care providers. This was also the case when examining ambulance call-outs for falls. Our study shows that following program participation, Stepping On participants were less likely to call an ambulance due to a fall and showed immediate decline in call-outs needing an ED visit. This impact did not last the 3-year follow-up, however, another study found exercise programs with structured exercises for frequent fallers delivered over a longer duration resulted in significantly lower rates of falls and morbidity at 3-year follow-up. 32 Taken together, these results suggest the need for prolonged and/or possibly frequent “top up” interventions, particularly exercise, to maximize health outcomes and reduce falls among older adults, particularly those with increased health problems.
Falls in older adults with health problems may be under reported by older people who do not inform their family or GPs about the incident. 36 Falls in older adults can result in hospitalizations or more critically in mortality. 37 Sherrington et al found that intervention effectiveness does not show any difference according to age groups 11 and others have investigated the effects of fall prevention programs by gender but findings are equivocal. 38 Our study adds to this literature showing that females compared to males and those in the intervention group compared to the control group, especially when examining fall-related mortality with a competing risk of all-cause death implying benefits of the Stepping On program. Mortality rates for women were lower than those for men, in accordance with previous research39,40 which suggests that different approaches to intervention according to gender may be needed to improve survival among males. 41
The European Union has estimated that fall-related expenditure costs €25 billion each year. 2 Likewise, in the USA, ED visits for falls account for the leading contribution of medical costs each year 3 of which, many older patients end up admitted to hospital and in many cases result in nursing home admissions. 42 As hospitalization in older adults is associated with increasing disability, 43 early provision of exercise addressing known fall risk factors (i.e., balance and leg muscle weakness), even while in hospital, may increase function, reduce disability 44 , and lessen subsequent health service use. Fall risk can be reduced with the implementation of evidence-based fall prevention programs and management by the GP. 2 The Stepping On program has shown consistent results globally (including the USA, Sweden) and has been translated into Spanish to target older adults in the USA who are from linguistically and culturally diverse groups. 45 Our study findings emphasis the benefits of falls prevention programs, showing reduce fall-related health service use in participants undertaking the Stepping On program. Additionally, findings from our study showed in this older cohort with previous hospitalization, Stepping On participation appears to have reduced fall-related mortality, acute care health service use (hospitalizations) in the 85+ year group, and subacute service use (ED and ambulance services) in the 75-84-year group. The impact on hospitalization and ED admission was most considerable in the oldest old (85+ year group) who showed rates that were lower or similar to those of the healthier control groups, even 3 years after program completion. In contrast, the greatest effect on fall-related ambulance use was among old aged patients (75-84 years). Thus, suggesting interventions such as the Stepping On program, if delivered as an early intervention, may provide protective effects and support the reduction of unnecessary health service use 15 as well as prolong survival particularly in males.
Limitations in the Research
This study has some limitations. The study population of hospital controls, who were matched with the Stepping On cohort, may not generalize to all older Australian adults or to those at risk of falls. The researchers used robust propensity score analysis to identify the study populations but were limited to variables available within the administrative databases to perform the matching algorithm. Further, differences between the control and Stepping On groups may exist for which the researchers did not have data, including some socio-demographic information. However, the analysis performed did provided reasonable 1:4 matching of Stepping On participants to controls. Another limitation of our study is the data collection which was provided by administrative routinely collected dataset and not specially targeted for falls issues. Therefore, the results from our study might not be an actual estimate of the proportion of patients with a fall.
Conclusions and Suggestions for Further Research
Regular top-ups of fall prevention programs, such as Stepping On, are needed to decrease mortality in later life for older Australian adults and to help with the reduction of unnecessary use of health care emergency services. Reducing fall-related mortality and health service use among older adults with poorer health may also help to alleviate the added service costs currently facing the health care system. 8 While there has been a call for programs to be scaled up to truly impact health outcomes, 46 less is known about rigorous evaluation methods for scaled up programs. Collaboration between researchers and service deliverers is crucial for evaluation of real-world programs such as the Stepping On program. Additionally, funding sustainability from government bodies to ensure fall prevention programs are ongoing and may be undertaken on a regular annual basis for those most vulnerable is paramount. To maintain the program’s positive effects over time for older individuals, access and availability to routinely participate in an exercise intervention long term needs to be acknowledged. 1
Supplemental Material
sj-docx-1-hhc-10.1177_10848223251345743 – Supplemental material for Evaluation of a Scaled-Up Fall Prevention Community Program in Older Adults With Previous Hospitalization
Supplemental material, sj-docx-1-hhc-10.1177_10848223251345743 for Evaluation of a Scaled-Up Fall Prevention Community Program in Older Adults With Previous Hospitalization by Dolja-Gore Xenia, Paul Serene S., Clemson Lindy, Lord Stephen R., Close Jacqueline C. T., Tiedemann Anne, Harvey Laura and Sherrington Catherine in Home Health Care Management & Practice
Footnotes
Acknowledgements
Open access publishing facilitated by The University of Newcastle, as part of the Sage - The University of Newcastle agreement via the Council of Australian University Librarians.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The authors thank Rob Herbert for his advice on study design and analysis, and NSW Health for its in-kind support and contribution to the NHMRC Partnership Projects grant Widespread implementation of interventions to prevent falls in older people (ID: 1016876). We also acknowledge the support ofthe NSWCentre for Health Record Linkage (CHeReL; ![]() ).
).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
