Abstract
Introduction:
Snake envenomation is relatively uncommon in New York State (NYS) but remains clinically relevant. The incidence and characteristics of snakebite and envenomation in NYS from 2000 to 2010 have been reported. This study sought to evaluate the incidence of snakebites in NYS from 2011 to 2022 and to describe recent patterns in terms of geography, time trends, and clinical characteristics.
Methods:
This is a retrospective observational study of snakebites reported to NYS poison control centers from January 2011 to December 2022. Data from the National Poison Data System were analyzed for demographics, geographic location, treatment, and medical outcome. Density maps were constructed to illustrate frequency across NYS counties, and a time-series plot was generated to demonstrate trends over time of snakebite reports.
Results:
From 2011 to 2022, 564 snakebites were reported; 112 (19.9%) venomous snakes, 245 (43.4%) nonvenomous, and 207 (36.7%) unknown. Many cases were classified as minor outcomes (69.3%), and 6.6% of victims received antivenom. Both venomous and nonvenomous bites were common in more populous counties and correlated with known indigenous snake populations. Time-trend analysis showed a gradual nonlinear decrease in total number of snakebites reported over the study period.
Conclusions:
snakebites reported to NYS poison control centers have decreased over the last 12 y but remain a risk to the NYS population. Public education surrounding prevention strategies and standardized approaches to seeking medical care and clinical management of snakebite injuries remain an important area for research and public health. These data help inform clinical management and guide antidote stocking at healthcare facilities.
Introduction
The United States harbors ∼120 different species of snakes, of which ∼20 species have been identified to be venomous. 1 Nearly all of these indigenous venomous snakes belong to the pit viper family (subfamily of vipers), also called Crotalinae.1,2 Snakes in this subfamily include Crotalus (eastern diamondback, western diamondback, and timber rattlesnakes), Sistrurus (massasauga and pigmy rattlesnakes), and Agkistrodon (copperhead and cottonmouth) snakes. 1 A much smaller population of snakes belongs to the family Elapidae, genus Micurus (coral snakes) and Micruroides euryxanthus (Sonoran [Arizona] coral snake). 1 Apart from these indigenous snakes, there are nonnative venomous snakes residing in zoos or in the hands of animal collectors which, despite their infrequency, remain clinically relevant due to the therapeutic dilemmas they pose in the circumstance of an envemenomation.1,3,4
snakebite injuries are a greater public health concern in Africa, Asia, Latin America, and Australia because the incidence of morbidity and mortality there is far greater than in North America and Europe. 5 The incidence of snakebites in the United States, on average, ranges from 6000 to 8300 bites per year, with approximately one third to one half of these being venomous snakebites based on published and National Poison Data System (NPDS) data.1,3,6–8 The United States has no mandatory central reporting system for snake envenomations, and many go unreported.1,2,6
Despite the low incidence and low mortality risk, snakebite injuries in the United States remain a clinically important disease entity due to the potential for morbidity and healthcare expenses. 3 North American pit viper envenomation, which accounts for most of the venomous snakebites in the United States, can produce a range of toxicity. Depending on the snake species and degree of envenomation, patients may develop local tissue injury and swelling, hematologic toxicity with coagulopathy and thrombocytopenia, and, in severe cases, systemic toxicity with shock and multiorgan failure. Some North American species also can cause neurotoxicity with fasciculations and muscle paralysis.1,5,6,9,10 Despite low mortality rates (101 fatal bites were reported in the United States between 1989 and 2018), medical management may require critical care unit admission, and recovery time may be prolonged.3,10,11
The incidence of snakebite envenomation in the United States is well documented in the western and southern states, where venomous snakebites are more common.9,10,12,13 However, epidemiologic data for New York State (NYS) regarding envenomation from snakes is sparse, with only 1 study reporting the incidence between 2000 and 2010. 2 As NYS undergoes climate and demographic changes, the incidence and range of various endemic species important to human health have been expanding in the region, leading to increased morbidity.9,10 Furthermore, the rising degree of deforestation has altered the population density. 3 With these changes, we sought to evaluate the distribution and burden of snakebite injuries in NYS from 2011 to 2022.
Methods
Study Design and Setting
This retrospective observational study was conducted on all snakebite cases reported to the 2 regional poison control centers (PCCs) in NYS through the NPDS between January 1, 2011 and December 31, 2022. The NPDS collects and reports on standardized, deidentified data on humans or animals exposed to a large spectrum of products, including bacterial, viral, venom, foreign body, chemical agent, and commercial or drug products. 14
Study Participants
Data from NYS PCCs were queried for all snakebite injuries using the NPDS classification of “unintentional bite/sting” for snakebites and human exposure cases within the above-mentioned timeframe. Cases were reviewed for inclusion, and only cases that originated in NYS and were reported to an NYS PCC were included. Cases were coded as reported in the NPDS for type of snakebite as venomous, nonvenomous, or unknown. If a bite was categorized as unknown but the patient was coded as having received antivenom as treatment, those bites were recategorized as venomous for the purposes of this study. This study was approved with exempt status by the coordinating center's research subjects review board.
Outcomes
The primary outcome was to describe the overall number of snakebites occurring in NYS during the study timeframe and describe geographic location, treatment, and medical outcomes. Secondary outcomes were to evaluate the frequency across NYS counties and assess trends of snakebite reports over time.
Data Collection
Specific data related to this study included patient demographics (eg, age and gender), year of incident report, county of incident report, coded snake species, exposure site or specific setting in which the snakebite occurred, where the patient was managed, treatment received (including antivenom), coded medical outcome, and disposition. Treatment with antivenom occurred at the discretion of the bedside clinician or clinical toxicologist on call for the PCC using PCC management guidelines, and data were only collected as received or not in the NPDS. Minor, moderate, and major medical outcomes were coded as defined by America’s Poison Centers’ NPDS coding manual. 15 Data were extracted by 1 investigator using a standardized data collection form and data dictionary.
Statistical Analysis
Descriptive analyses using frequency tables were employed to describe cases. In addition, a stratified analysis of all the variables by type of snakebite injury (venomous vs nonvenomous vs unknown) were performed to compare demographics, exposure, and clinical characteristics across the different types of snakebites. Density maps were generated to illustrate the distribution of total snakebites and snakebites per capita and to compare the distribution of venomous vs nonvenomous snakebites across NYS counties. snakebites per capita were calculated by dividing the number of snakes bites in each county by that county's 2016 population (midpoint between 2011 and 2022), with the result expressed as bites per 1 million population. 16 A time-series plot was generated to demonstrate the yearly frequency overall and the different types of snakebites reported from 2011 to 2022. All analyses and figures were produced using SAS, version 9.4 (SAS Inc, Cary, NC).
Results
Geographic Distribution and Time Trends
A total of 564 snakebite cases in humans were reported in NYS between 2011 and 2022, resulting in an average of 47 snakebites per year. Most snakebites were coded as nonvenomous (43.4%), followed by unknown venomous status (36.7%) and venomous (19.9%) (Table 1). Among the 112 snake envenomation cases, >70% were from 2 types of snakes (copperhead 35.7% and rattlesnake 35.7%). The geographic distribution across counties is shown in Figure 1. The largest concentration of all snakebites was in the southeast counties in the greater New York City area (Figure 1A). Large numbers can be noted in Onondaga County in central NY, Monroe County in the Finger Lakes Region, and Erie County in western NY (Figure 1A). However, after addressing the population in each county, it is noted that the largest concentration of snakebites is in Delaware and Sullivan counties in the southeastern part of the state (Figure 1B). Distribution of venomous and nonvenomous snakebites showed a similar spread across NYS (Figure 2).
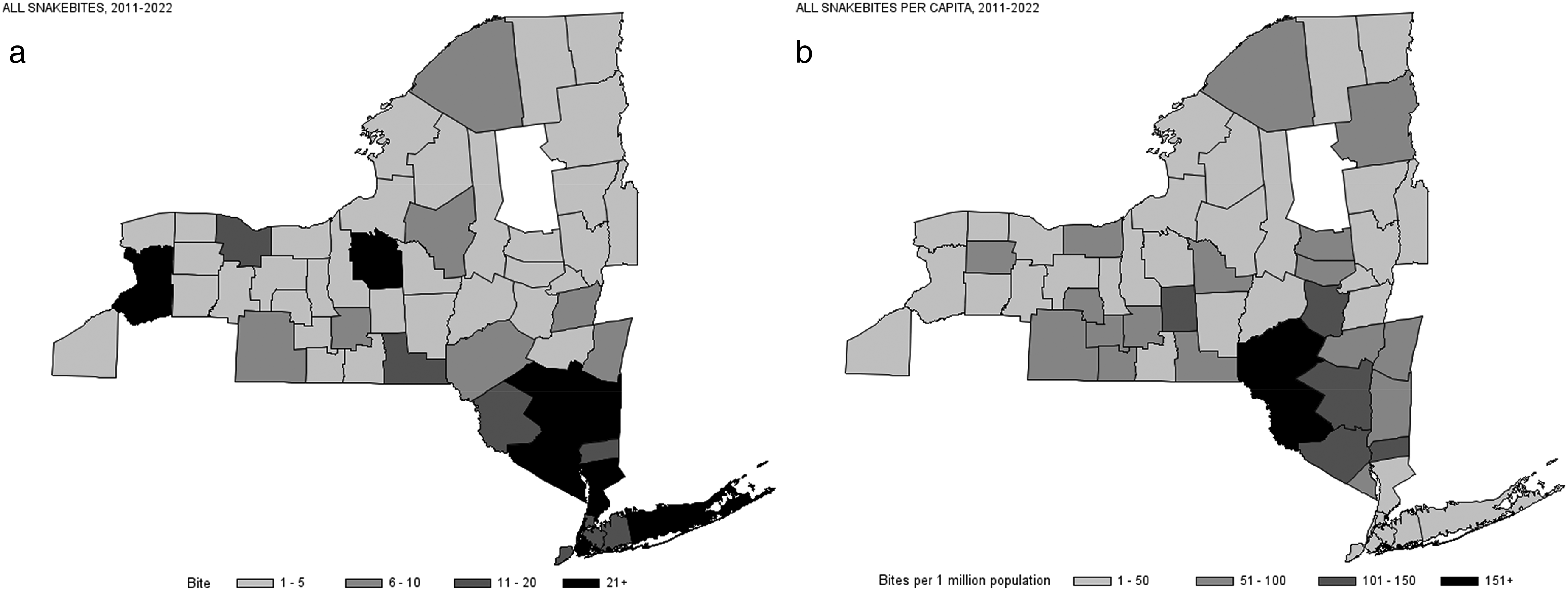
Density Maps of Snakebites Reported to New York State Poison Centers From 2011 to 2022: (a) All Snakebites (Total Count); (b) All Snakebites (Per Capita). a
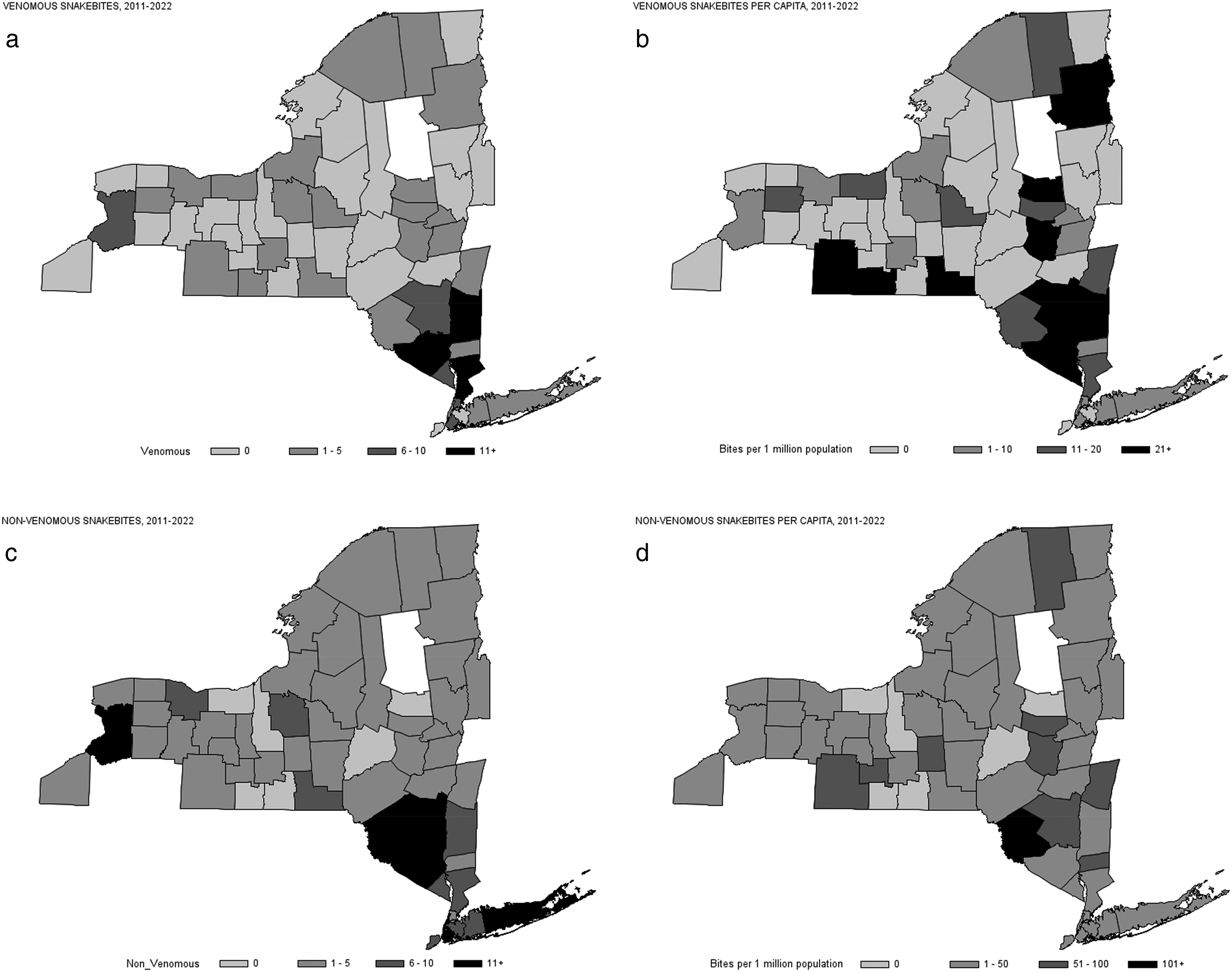
Density Map of Snakebites Reported to New York State Poison Centers From 2011 to 2022 by Snakebite Type: (a) Venomous Snakebites (Total Count); (b) Venomous Snakebites (Per Capita); (c) Nonvenomous Snakebites (Total Count); (d) Nonvenomous Snakebites (Per Capita). a
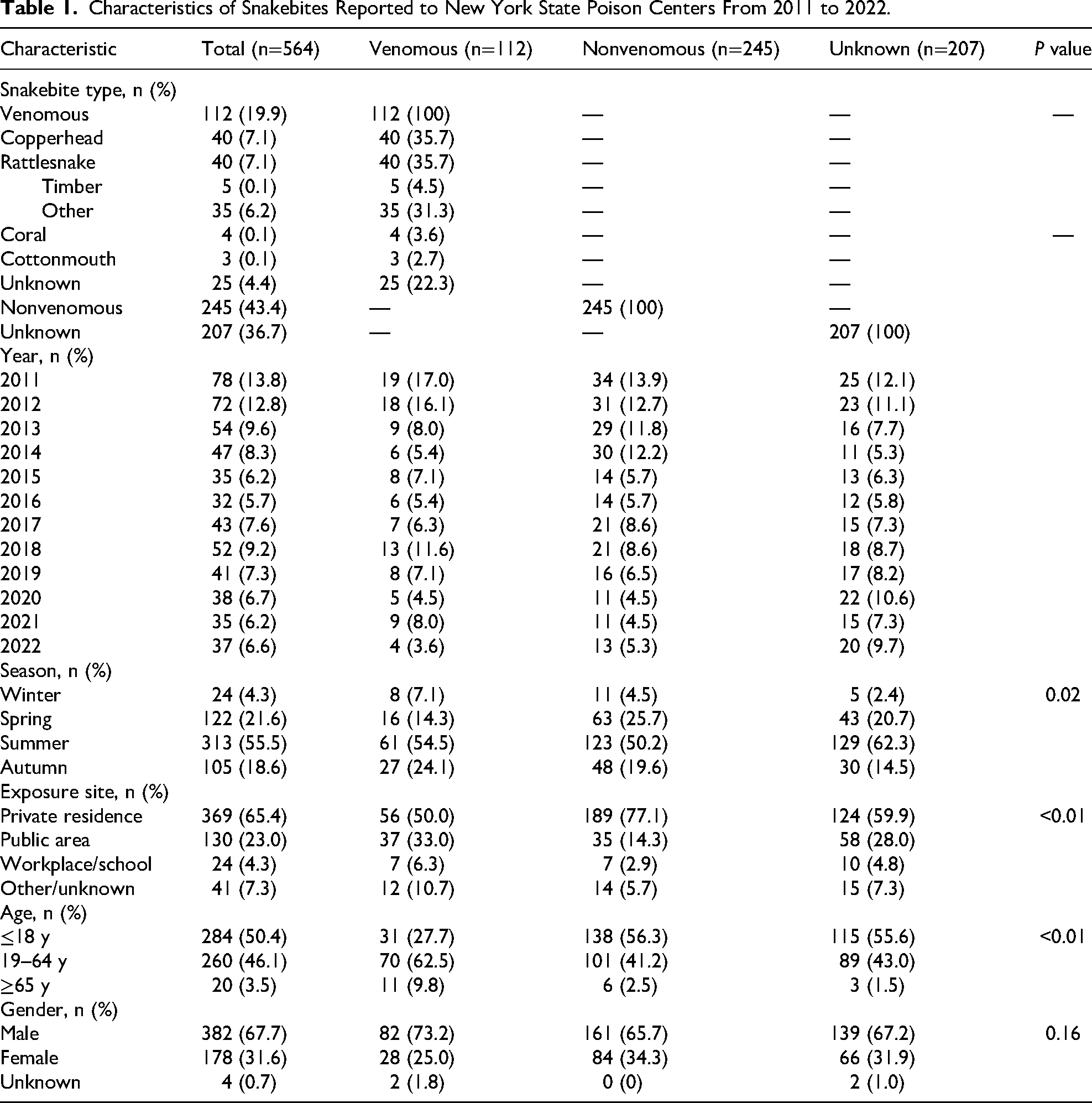
Characteristics of Snakebites Reported to New York State Poison Centers From 2011 to 2022.
The time-trend analysis showed a gradual nonlinear decrease in the total number of snakebites reported over the study period (Table 1, Figure 3). Total snakebites decreased by nearly half from 78 cases reported in 2011 to 37 cases reported in 2022. Similar patterns were seen for venomous (19 vs 4 cases) and nonvenomous snakebites (34 vs 13 cases) in 2011 and 2022, respectively. snakebites of unknown venomous status experienced some variability over the study period but remained relatively stable over time, with 25 and 20 snakebites in 2011 and 2022, respectively.
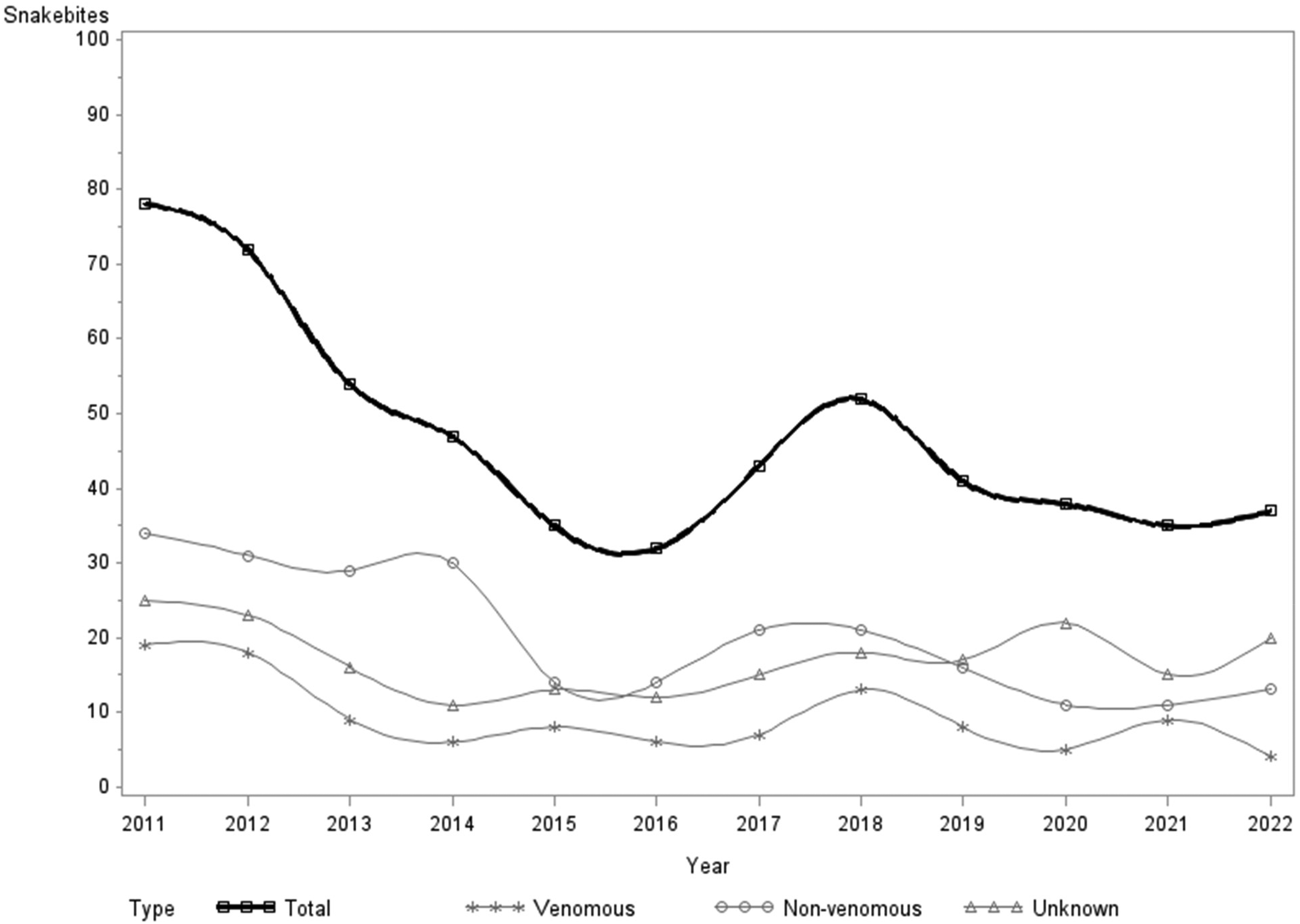
Time-Trend Analysis of Snakebites Reported to New York State Poison Centers From 2011 to 2022 Stratified by Venomous Status.
Demographic Characteristics and Medical Outcomes
In total, half the patients were 18 y of age and less (50.4%), and males were more common than females (67.7% vs 31.6%). Stratified analysis showed the distribution of age (ie, 18 y or less, 19–64 y, or 65 y or older) differed according to type of snakebite (ie, venomous, nonvenomous, or unknown; P<0.01). Complete patient-level characteristics are listed in Table 1.
Most patients were treated and released (47.3%). However, a small percent received management with antivenom (6.6%), antibiotics (6.2%), antihistamines (2.7%), steroids (1.4%), or opioid analgesia (0.7%). Likewise, among patients with a confirmed snakebite who were followed up, most were reported to have a minor (69.3%) or moderate (23.2%) outcome, with only a fraction reporting a major medical outcome (0.6%). Moderate medical outcomes were most common among venomous snakebite patients, and minor outcomes were most frequent among nonvenomous snakebite patients. Of the 2 major medical outcome cases, 1 was following a venomous snakebite and the other of unknown classification. The venomous case had coded symptoms of ecchymosis, edema, dermal irritation, and puncture wound; was admitted to the intensive care unit; and received antivenom and opioid analgesia, and the unknown classification case had coded symptoms of puncture wound and renal failure and required intubation. Treatment strategies and medical outcomes stratified by snakebite type are listed in Table 2.
Treatment and Medical Outcomes of Snakebites Reported to New York State Poison Centers From 2011 to 2022.
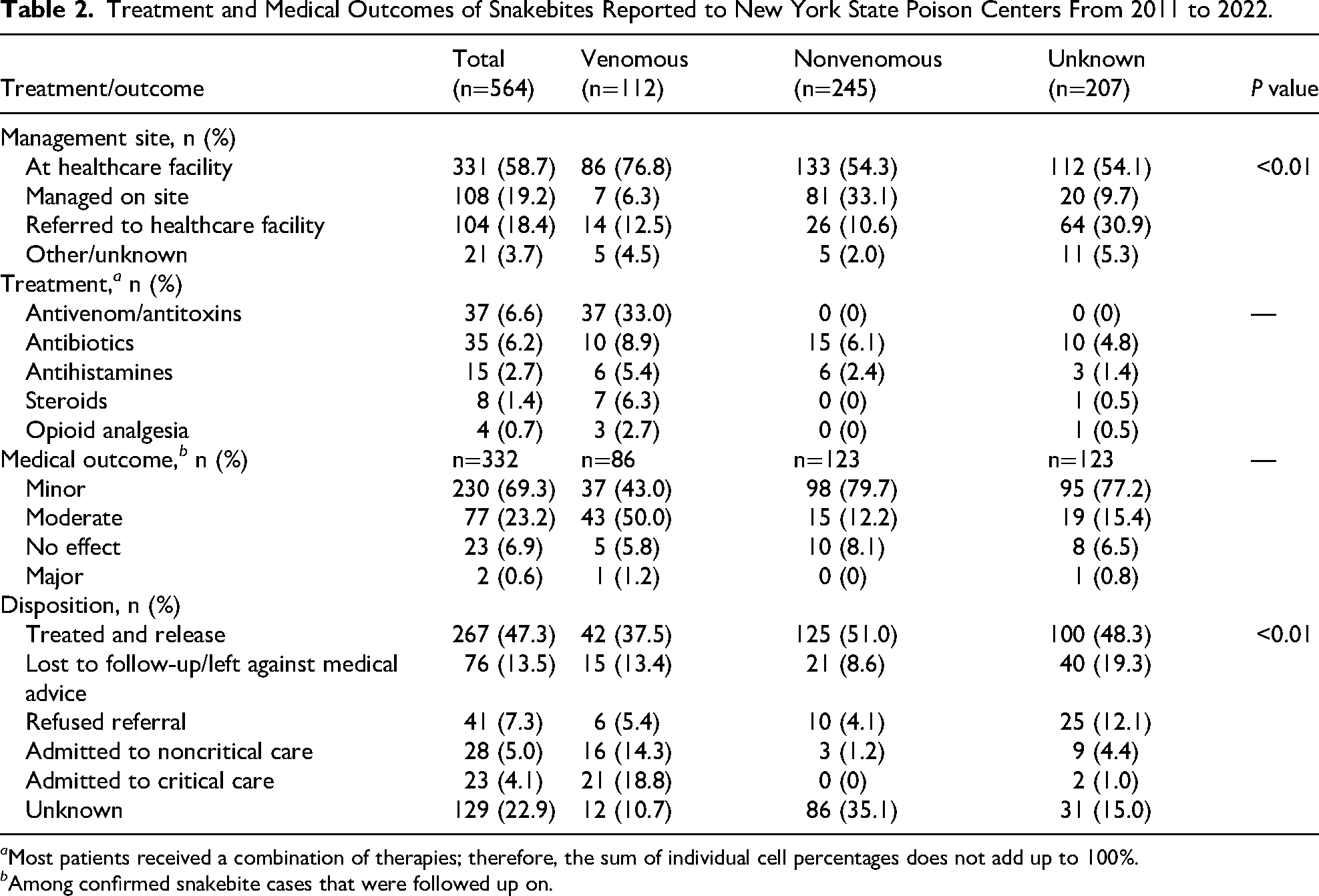
a Most patients received a combination of therapies; therefore, the sum of individual cell percentages does not add up to 100%.
b Among confirmed snakebite cases that were followed up on.
Discussion
snakebites reported to NYS PCCs between 2011 and 2022 averaged 47 per year, with the majority from nonvenomous snakes and occurring in private residences. Most patients were male, 18 y of age and younger, did not require antivenom, and were reported as having a minor outcome. Both venomous and nonvenomous bites were common in more populous counties and correlated with known populations of indigenous snakes. The time-trend analysis showed a gradual nonlinear decrease in the total number of snakebites reported over the study period.
Compared with previous data from 2000 to 2010, our findings showed that the average number of snakebites per year reported to NYS PCCs from 2011–2022 did not appreciably change, 47.3 vs 47 per year, respectively. 2 However, when taking into account NYS population changes over this time, the incidence rate of snakebites reported shows an increase from 2.43 snakebites per 100,000 population between 2001 and 2010 to 2.88 snakebites per 100,000 population between 2011 and 2022.2,16,17 In reviewing the individual calendar years, there is significant annual variability in the number of reported snakebites that likely impacts these averages. Specifically, there was a minor increase in snakebites reported in 2018, but we do not have an adequate hypothesis as to why this occurred. Regardless, our time-trend analysis showed a clear decrease in the number of snakebite cases over the 12-y study period (2011 to 2022) as a whole. The cause for this decrease is unknown but may be attributed to a decline in the snake population in NYS due to habitat destruction, indiscriminate killing, or unregulated collection.18,19 In particular, the eastern massasauga is classified as an endangered species, whereas the timber rattlesnake is classified as a threatened species.18,19 It is also possible that this decline may reflect changes in human behavior or changes in the frequency of layperson calls and clinician reports to the PCC.
There are more nonvenomous snakes (ie, eastern garter snake [Thamnophis sirtalis sirtalis], eastern milk snake [Lampropeltis triangulum], northern water snake [Nerodia sipedon], and eastern rat snake [Pantherophis alleghaniensis]) compared with venomous snakes spread throughout NYS. 20 The distribution of snakebites reported across NYS counties is consistent with the distribution of snake populations and also with areas of larger human population. 21 This is a similar pattern to those observed in the 2000 to 2010 report. 2 Three venomous snakes are indigenous to NYS, all of which are classified as Crotalinae (pit vipers), namely, 1) timber rattlesnake, 2) eastern massasauga, and 3) copperhead.18,20 Of the 3, the timber rattlesnake (Crotalus horridus) is noted to be the most widespread across NYS, with its population predominantly located in the southeastern part of the state and other pockets of population spread throughout the northern part of the state up to Lake George and the western part of the state along the Southern Tier.19,20 The eastern massasauga (Sistrurus catenatus) has populations concentrated in 2 specific wetlands in NYS: 1) northeast of Syracuse (Onondaga County) and 2) west of Rochester (Monroe County and Erie County).18,20 Lastly, the copperhead (Agkistrodon contortrix) is located mainly in the lower Hudson Valley (Orange, Rockland, and Westchester counties), with some scattered population across the Catskill Mountains. 20 Our study showed 112 venomous snakebites, and most fall into the pit viper family of snakes. This follows the same distribution as the habitat locations of indigenous venomous snake species. However, it is also important to note that in our findings, although the timber rattlesnake and copperhead were major contributors, a few cases also reported bites from coral and cottonmouth snakes. These 2 snake species are not indigenous to NYS and were either misidentified or were snakes owned by animal collectors or kept in zoos.1,20 When comparing the proportion of venomous snakebites between 2001 to 2010 and 2011 to 2022, there was an increase from 14.2% (67 of 473) to 19.9% (112 of 564) and a higher average number of venomous snakebites per year (6.7 vs 9.3 cases per year, respectively). 2 This may be attributed to the growing human population in and around the habitats of venomous snakes. 3
Among the confirmed snakebite cases that were followed up, our study showed that most cases were coded as having a minor outcome (69.3%; 230 of 332) after a snakebite, which was a shift from 2001 to 2010, where the majority of patients had a moderate outcome (68%; 204 of 300). 2 Although the criteria for classification have not changed over this timeframe, this is a subjective measure that may have resulted in differences. Regardless, snakebites still pose a significant risk, and clinicians should be aware of how to manage envenomation cases. 22 Most snakebite cases in our sample occurred in private residences, followed by public settings. This presents an opportunity for community education and public health outreach. snakebites occurring in public settings, school/workplaces, and other locations remained stable over the course of the study period. Targeted education on snakebite prevention strategies and emphasizing the importance of seeking medical attention in the event of a snakebite can be tailored for different populations, such as individuals who own pet snakes and individuals who are likely to encounter snakes via recreational outdoor activities.
There are several limitations to our study that need to be considered. Although the NPDS captures robust data on ingestion and envenomation cases, it is likely that there are snakebite cases that were not reported to a PCC. Additionally, the type of snakebite was unknown in 36.7% of all reported cases, potentially underestimating the true incidence of venomous snakebites in NYS. It is also possible that the geographic locations of some snakebites were miscoded. If the location of the occurrence was not specified to the PCC, it is possible that it was coded by default to the county where the PCC is located, potentially inflating the frequency of envenomation in Onondaga County and New York City. Moreover, the NPDS does not have further delineation of snake species captured, and therefore, clinical features were not able to be described within specific species where qualitatively and quantitatively different clinical features from bites were seen. The categorization of minor, moderate, or major medical outcome is limited by the definitions used for the NPDS. 15 Overall, this coding is subjective, and it is possible that the outcome would have been categorized differently if entered by a different reporter. Further, there were missing data on medical outcome (not available in >40% of cases; ∼20% of venomous snakebites were not followed and medical outcome not reported) and occurrence of surgical intervention. Lastly, we did not review the narratives for each patient in the NPDS, which may have provided case details that could have added to the robustness of our data, including clarity on snake species, bites occurring while the snake was in captivity or the wild, and treatment and outcome clarity that may have influenced our results.
Conclusions
snakebites reported to NYS PCCs have decreased in frequency over the last 12 y from 2011 to 2022. Furthermore, there has been a gradual decrease compared with 2000 to 2010. Most cases only reported mild to moderate symptoms, and only a small percent required systemic clinical management. Despite these decreases, snakebites remain a risk to the population of NYS. Public education surrounding prevention strategies and standardized approaches to seeking medical care and clinical management of snakebite injuries remain important areas for research and public health, and these data can help inform clinical management and guide antidote stocking at healthcare facilities.
Footnotes
Acknowledgments
The authors thank David P. Toomey for assistance with conceptualization, methodology, and visualization.
Ethical Considerations
This study was conducted in accordance with the Declaration of Helsinki and was approved by the Institutional Review Board of the University of Rochester (00008043) on February 17, 2023, with the need for written informed consent waived.
Consent to Participate
Informed consent for information published in this article was not obtained because the need for written informed consent was waived by the Institutional Review Board of the University of Rochester (00008043) on February 17, 2023.
Author Contribution(s)
Data Availability
All data generated or analyzed during this study are included in this published article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Previous Presentation
Presented at the American College of Medical Toxicology Annual Scientific Meeting, Washington, DC, April 12–14, 2024.
