Abstract
Objective
Vipera berus is the only naturally occurring venomous snake in Poland. Its venom is primarily vasculotoxic and evokes both local and systemic findings. The aim of the study was to review a series of clinical cases of V berus bites occurring in southwest Poland.
Methods
The charts of 26 patients (age range, 16–66 years; mean, 42 years) hospitalized with V berus bites were retrospectively analyzed using a data collection tool. Demographic and clinical data were extracted.
Results
The most common local findings of envenomation were edema of the bitten limb with associated extravasations observed in 24 (92.3%) patients, but in only 1 (3.8%) case did the edema spread to the trunk. In 22 (84.6%) cases edema disappeared within 2 weeks after the bite. Systemic disturbances observed in the patients were: shock (1 case), mild transient hypotension (1 case), prolonged hypotension (3 cases), bronchospasm and laryngeal edema (1 case), diarrhea (1 case), transient supraventricular arrhythmias (2 cases), neutrophilic hyperleukocytosis (2 cases), and thrombocytopenia below 50 000 cells/μL (5 cases). In 16 patients (61.5%) the envenomation was classified as moderate and this type was predominant. Six cases were classified as severe. No fatal case was reported. Treatment included the administration of specific antivenom in 14 cases (in all severe and half of moderate cases) and symptomatic treatment applied in all cases.
Conclusions
Moderate envenomation prevailed among the patients analyzed in the study. Antivenom treatment is primarily necessary in cases of severe (grade 3) and in some cases of moderate (grade 2) envenomation, especially in patients with persistent or recurring hypotension.
Introduction
Vipera berus is the only naturally occurring venomous snake in Poland. Its venom is primarily vasculotoxic and contains hyaluronidase, which facilitates the tissue spread of other venom components such as proteolytic enzymes, toxic polypeptides, amino acids, and a small amount of carbohydrates. 1 Phospholipase A2, one of the most important constituents, detaches arachidonic acid from cell membrane phospholipids and starts an inflammatory cascade. Inflammatory mediators together with vasoactive substances liberated from injured tissues are responsible for vascular damage and increased permeability, which subsequently leads to edema and the extravasation of cellular blood elements.1,2 Because the venom of V berus spreads mainly throughout lymphatic vessels, regional lymphadenitis can be one of the findings. Envenomation has more severe consequences in small children, probably because of the higher dose of venom compared with body weight. 1 ,3,4
V berus bites remain problematic in Poland and concern not only toxicologists, but also the emergency service, pediatricians, and family doctors. Mortality in cases of V berus bites is rare and does not exceed 1%. 3 However, the disease may diminish physical and professional activity for several weeks. Because of the potentially dangerous course of envenomation and possible severe complications, proper management of such bites is very important.
The aim of this retrospective case study was to collect epidemiological and clinical data from patients bitten by V berus. We evaluated signs and symptoms, severity of envenomation, clinical course, treatment, and outcome.
Methods
The medical records of adult patients hospitalized due to V berus bites at the Toxicological Unit of T. Marciniak Hospital in Wroclaw, Poland from 2000 to 2008 were retrospectively analyzed. A data-gathering form was filled out by one medical doctor and reviewed by another. Data collected included: epidemiologic data, local findings, systemic symptoms, laboratory findings, complications, and treatment.
All cases of V berus bites were recorded from the region of Lower Silesia (southwest Poland), which has an area of 19 946.77 km2 and a population of 2 878 410. T. Marciniak Hospital is a major hospital and the only toxicologic referral center for adult patients in this area. All adult patients with moderate and severe V berus bites are hospitalized in this center. Patients were observed in hospital until all swelling was gone. There was no patient follow-up.
Mild cases may be treated in local hospitals. However, each of these cases is generally reported to the referral unit. Eighteen cases of bites were reported to us by telephone from 2000 to 2008. These cases were not included in this analysis due to a lack of detailed medical data from the respective hospitals. However, they were classified as mild by the reporting doctors.
The grading scale of Audebert et al with the modification by Petit was used for clinical evaluation. 3
Children under age 16 from the region of Lower Silesia are treated in another pediatric unit and were not enrolled in this case study.
Because the study is the retrospective analysis of clinical cases, institutional review board approval was unnecessary.
Results
This retrospective case study involved 26 patients (16 men and 10 women; age range, 16–66 years; mean, 42 years). Most often the patients were bitten in the forest (20 cases), more rarely in the countryside (5 cases). One case of viper bite happened in town, in a garden bordering a house. The annual incidence of V berus bites varied widely, from 0 in 2001 to 8 cases each in 2006 and 2008. Moreover, the incidence of V berus bites showed a distinct seasonal pattern, with a higher frequency in late spring and summer; all of the patients were bitten from May to September and 61% of the bites occurred in June and July. All of the patients were bitten during the day, with a peak between 11
In our patients, moderate V berus envenomation predominated (Table 1). At the time of admission to the toxicologic unit, fang marks were observed in all patients, who also reported local pain just after the viper bite. Edema was the next most common manifestation of bites (92.3% of cases), lasting up to 2 weeks in most cases (Table 2). In 16 cases (61.5%) the edema was painful and the patients required treatment with analgesics: 4 cases with tramadol, 1 case with ketoprofen, and 2 cases with metamizol. Paracetamol or tramadol was used in 11 patients (42.3%) who received low-molecular weight heparin (LMWH) as prophylaxis against deep vein thrombosis following lower limb bites. Edema-associated pain usually disappeared or was considerably diminished within 1 week after the bite. Widespread extravasations were always observed together with the edema and usually disappeared just after the edema had subsided (Figure). In 1 case, axillary lymphadenitis developed after a bite on the hand and was accompanied by edema of the whole upper limb.
Clinical gradation of envenomation after viper bite
Duration and range of edema in patients after V berus bites
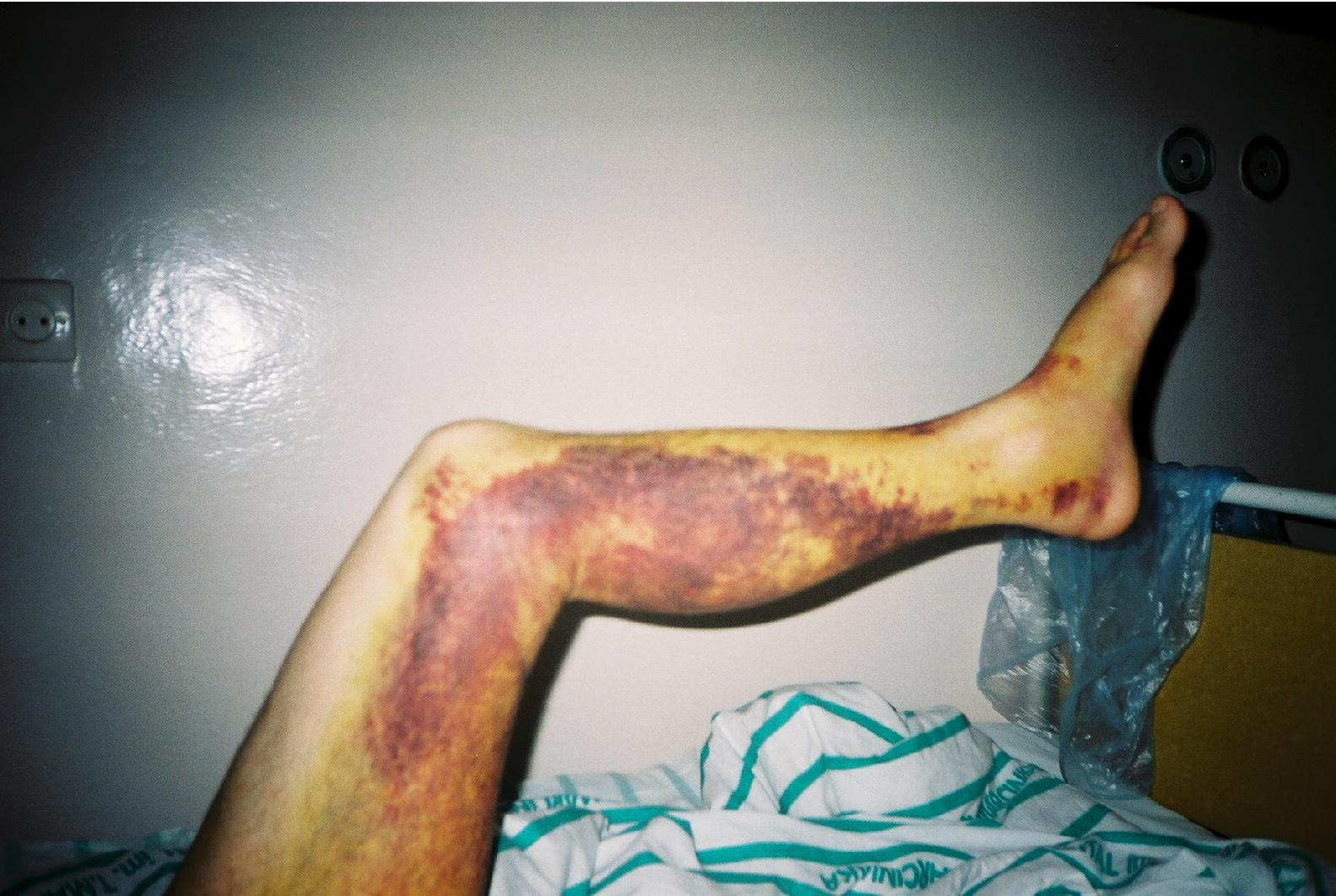
Left lower extremity 16 days after V berus bite to the dorsum of the left foot. Slight edema of the foot and ankle, and widespread ecchymoses of the foot, calf, and thigh are still present.
The most common systemic finding of envenomation was hypotension: mild and transient in 1 case (3.8%) and prolonged without clinical symptoms of inadequate perfusion of vital organs in 3 cases (11.5%) (Table 3). No cases of deep vein thrombosis were recorded. Detailed laboratory findings are presented in Table 4. In 16 cases increased levels of creatine phosphokinase (CPK) and aspartate aminotransferase (AST) normalized within 5 to 7 days. Only 1 patient showed increased activity of these enzymes up to 10 days. In all of our patients, even those with massive edema and ecchymoses, no significant changes in red blood cell morphology were noticed. No electrolyte disturbances or abnormalities in creatinine and urea levels were revealed. In all of the patients, international normalized ratio (INR) values and fibrinogen levels were normal.
Clinical findings of V berus bites depending on grade of envenomation
Laboratory findings in patients with V berus bites
CPK, creatine phosphokinase; AST, aspartate aminotransferase; ALT, alanine aminotransferase.
A case of 36-year-old woman with increased activities of CPK and AST (8249 U/L and 6868 U/L, respectively), which normalized within 10 days of hospitalization.
A case of 56-year-old man with chronic C-type hepatitis; ALT activity did not differ from values before envenomation as obtained from patient's medical history.
Treatment was considered individually with regard to each patient's clinical state and envenomation course (Table 5). Specific antivenom was administered in 14 cases (53.8%), which included all the severe and half of the moderate cases of V berus bites. Antivenom was not used in patients with grade 0 (no envenomation) or grade 1 (minimal) envenomation. Serum sickness was not observed in any patient during hospitalization.
Treatment of V berus bites depending on grade of envenomation
LMWH, low-molecular weight heparin; HAES, hydroxyethly starch.
Because of the potential risk of infection with anaerobes from the viper's teeth, antibiotics (amoxicillin with clavulanic acid) were administered in all cases. Moreover, antitetanus prophylaxis was considered in all patients depending on age and previous vaccination.
In addition to specific treatment with equine antivenom, symptomatic management was undertaken in the patients with generalized symptoms. In those with arterial hypotension, hydroxyethyl starch (HAES) was administered. Apart from HAES, hydrocortisone and dopamine (5 μg/kg/min) were given by intravenous infusion to the patient with shock. The individual with laryngeal edema and bronchospasm received antivenom, an intravenous infusion of theophylline (300 mg), and hydrocortisone (200 mg), which caused the symptoms to subside rapidly. The cardiac dysrhythmias observed in 2 patients on the first day of envenomation were mild and did not require treatment. One patient developed nonbloody diarrhea lasting 5 days and was treated with loperamide. None of the patients required surgery and no fatal envenomation was reported.
Discussion
In this study of 26 patients, the clinical severity of the adder bites ranged from no envenomation to severe. In 22 (84.6%) cases the course of envenomation was classified as moderate or severe (grade 2 and 3). Including the mild cases consulted by telephone, the percentage of moderate and severe cases of envenomation in the investigated region was similar to other reports from European countries (eg, France, Switzerland, Italy) and was estimated as 50%. 3 ,5,6
A symptomless course of V berus bites was noted in only 2 persons (7.7% of cases). In some other reports, this kind of viper bite was observed in up to 30% to 50% of cases. 7 Asymptomatic cases of viper bites may be due to so-called “dry bites,” ie, without venom injection into tissues. Enzyme-linked immunosorbent assay (ELISA) tests for V berus venom identification in patient serum and urine may be helpful in the diagnosis of such cases. 8 However, ELISA tests are better at distinguishing different venoms than detecting envenomation.
The use of antibiotics after a V berus bite is not evidence-based and is more restricted in other countries. 3 All of our patients received antibiotics, as this is routine practice in Poland.
Contrary to some other reports, 3 leg bites were more frequent in our patients than hand bites. LMWH was given in prophylactic doses to individuals with edema of the whole limb (11 cases) as prevention against thrombosis during the longer immobilization of these patients. The efficacy of such therapy is not well established. However, in the cases of true thrombophlebitis higher, therapeutic doses of LMWH are recommended. 3 Because V berus venom does not contain neurotoxins, sedatives may be used in cases of severe anxiety or nervousness. We prefer hydroxyzine because of its additional H1-antihistamine action. In our observation, only 1 patient required an anxiolytic drug on the first day of hospitalization (a 16-year-old girl bitten on the hand).
It is estimated that systemic findings of V berus envenomation appear in 30% to 45% of cases. 4 Besides the generalized findings described in our patients, urticaria, gastrointestinal hemorrhage, paralytic ileus, pancreatitis, transient alanine aminotransferase (ALT) elevation, renal function impairment or insufficiency, fever, disseminated intravascular coagulation (DIC), thromboses, hemoptysis, and anemia due to hemorrhage, hemolysis, and/or blood loss in the swollen limb have been reported. 1 ,3,4 Cardiotoxicity related to V berus bites has been described as nonspecific ST segment changes or second-degree heart block.9,10 Allergic symptoms (eg, laryngeal edema, urticaria, bronchospasm) may also occur after viper bite. 2
In 18 patients (62.9%), increased AST activity was observed, but in only 1 case was concomitant elevation of ALT level noticed. However, increased aminotransferases activity in this patient was not evoked by viper bite but was related to earlier chronic C type hepatitis. On the basis of medical history obtained from the patient's family, similar ALT and AST values were observed a month before envenomation. In the remaining 17 patients (65.4%) with increased AST activity, concomitant elevation of CPK activity was noticed, whereas activity of ALT was within normal range. Thus, in these cases, we relate the elevated enzyme activity to the muscle damage caused by proteolytic properties of viper venom rather than liver injury. Fortunately, muscle damage was not complicated with kidney dysfunction in any case.
Thrombocytopenia caused by V berus bite is of 2 types: (1) benign, probably due to the aggregation of platelets by venom proteins or platelet loss in the swollen limb, and (2) severe, accompanying coagulopathy, with abnormal values of prothrombin time and fibrinogen. 3 Thrombocytopenia below 50 000 cells/μL was noticed in only 5 of our patients. In all of these cases extensive edema and massive extravasations covered the whole lower limb; however, no symptoms of systemic coagulopathy were observed. Therefore, platelet loss in the swollen limb was considered the main reason for thrombocytopenia.
Not all cases of V berus bites require treatment with antivenom. Its use should therefore be considered individually. Antivenom is indicated in all cases of grade 3 and in some cases of grade 2 envenomation with persistent hypotension, impending coagulopathy, or severe thrombocytopenia.3,11 There are also some specific clinical situations in which antivenom should be used, such as bites in regions such as the face, neck, and tongue due to the risk of loss of an airway; bites in small children and in pregnant women (except for dry bite cases); and in cases of extensive or rapidly spreading edema or the presence of systemic findings of toxicity (eg, protracted gastrointestinal symptoms, bleeding, arrhythmias, conduction disorders, ST segment changes on electrocardiography). Treatment with antivenom is also needed in cases with laboratory evidence of envenomation such as hemolysis, coagulopathy, increased serum CPK activity, metabolic acidosis, or pronounced leukocytosis (>20 000/μL). 1 ,3,7,11–14
In our study, 14 patients (53.8%) had bites severe enough to require antivenom. Antivenom against V berus (Antitoxinum vipericum, Biomed, Warsaw, Poland) is produced from horse serum. One ampoule of Antitoxinum vipericum contains 500 units of antivenom. In Poland, this dose is recommended for both adults and children. If necessary, the dose may be repeated after a few hours. 15 In all of our cases, additional injections of Antitoxinum vipericum were not necessary. The antivenom was administrated from 30 minutes to 2 hours after the bite (average, 76 minutes). Antitoxinum vipericum is registered for intramuscular injection, but in life-threatening envenomation or multiple bites the manufacturer suggests intravenous administration. 15 Increasing data suggest that intravenous infusion (over 30–45 minutes) may be the most efficient route of viper antivenom administration since it provides the highest bioavailability of the drug without a higher risk of allergic reactions compared with intramuscular injection. 16 The antivenom must not be injected into the bitten extremity and it should not be administered without immediately available epinephrine. 15 Prior to Antitoxinum vipericum administration, the manufacturer recommends an intracutaneous allergic test by injection of 0.1 mL of antivenom diluted 1:10 with normal saline solution. Flare and/or blister at the site of injection after 10 to 20 minutes may be evidence of an allergy to horse protein. 15 Such a procedure is not accepted by all physicians, and Reid observed in 1976 a low correlation between positive skin test and allergy to foreign protein. 12
“Serum antivenoms” held a bad reputation in the past. They caused many complications and even several deaths from anaphylaxis, especially in cases of repeated administration.
3
However, in patients treated at the Toxicological Unit of T. Marciniak Hospital, no adverse reactions after administration of Antitoxinum vipericum were observed during hospitalization
With V berus bites, pre-hospital management is also important. To limit venom spread in the tissues and its absorption into the systemic circulation, immobilizing the bitten limb is advised; however, such management is not evidence-based.3,14 Making an incision at the site of the bite is not advised because it may facilitate venom absorption into the circulation. Tourniquets and suction have not been shown to be beneficial.3,11 All patients should be transported to the hospital as soon as possible and observed for at least 6 hours, even in the absence of evidence of envenomation, because delayed evolution to a higher grade is always possible. 1 Children deserve special attention because the course of envenomation may be more severe.3,22
This retrospective case study describes signs and symptoms, clinical course and prognosis, and criteria of severity, as well as the treatment of V berus bites. We hope it may serve as a guide in the pre-hospital and hospital management of similar patients, especially in assessing the severity and risks of envenomation and indications for V berus antivenom administration. The major limitations of our study are its retrospective design, the relatively small number of patients included, and the lack of outpatient follow-up. The incidence of clinical findings that may have been present but not recorded in patients' charts are, therefore, underestimated, and late adverse reactions, especially serum sickness, occurring after patients were discharged cannot be assessed.
Conclusions
Moderate envenomation (61.5% of cases) prevailed among the 26 patients hospitalized at the Toxicological Unit of T. Marciniak Hospital in Wroclaw from 2000 to 2008. In 23% of the cases the course of envenomation was severe, but no fatal outcomes were noted. In 53.8% of the cases, specific treatment included equine antivenom (Antitoxinum vipericum). Our observations confirm that antivenom treatment is primarily necessary in cases of severe (grade 3) and in some cases of moderate (grade 2) envenomation, especially in patients with persistent or recurring hypotension.
