Abstract
Introduction
Predictive analytics may be a useful adjunct to identify training needs for exploration class medical officers onboard deep space vehicles.
Methods
This study used a preliminary version of NASA's newest medical predictive analytics tool, the Medical Extensible Database Probabilistic Risk Assessment Tool (MEDPRAT), to test the application of predictive analytics to exploration crew medical officer curriculum design for 5 distinct design reference mission (DRM) profiles. Partial and fully treated paradigms were explored. Curriculum elements were identified using a leave-one-out analysis and a threshold of 5% risk increase over the fully treated baseline.
Results
For the partial treatment scenario, among the 5 DRM profiles 4-32 curriculum elements met the 5% RRI increase. For the absolute treatment scenario, among the 5 DRM profiles, 13-126 curriculum elements met the 5% RRI increase. For the partial treatment paradigm, 13 capabilities are present in at least 3 of the 5 DRM profiles, and these elements may constitute a common baseline curriculum. This covers 41% of the skillsets needed for an ISS-like profile, 100% of a late Artemis-like profile, 41% of a Mars mission-like profile, 100% of a Starship orbital-like profile, and 68% of a Starship lunar flyby-like profile.
Conclusions
This proof-of-concept study demonstrated that predictive analytics can rapidly generate generic and mission profile-specific exploration CMO curricula using an evidence-based process driven by optimizing mission risk reduction. This technique may serve as part of a human-machine team approach to medical curriculum planning for future space missions. It has significant potential to improve astronaut health and save time and effort for planners, trainers, and trainees.
Keywords
Introduction
Determining the skill set necessary for a crew medical officer (CMO) supporting deep space missions is a complex task. The number and severity of medical events that will occur are unknown, and in addition to limitations in diagnostic and therapeutic resourcing and ground communication, it is not possible for a small crew to attain the diversity of expertise necessary to safely manage all conceivable medical contingencies. 1 Furthermore, the required knowledge, skills, and abilities (KSA) are likely to change with each mission profile, further complicating the question of what pre-mission training an exploration-class medical trainee (exploration CMO) should receive.2,3
Present-day space medical operations address these limitations by supporting crews in the International Space Station (ISS) with robust real-time telemedical capabilities, timely resupply of consumables, and the option to rapidly evacuate to Earth should medical needs exceed those available onboard the spacecraft. 4 This allows the ISS CMO to prioritize KSA required of routine medical care, managing minor medical concerns, triaging more complex medical complications with the assistance of the Flight Surgeon in mission control, and triaging the need for urgent stabilization and evacuation. 5 However, the sustainability of this paradigm diminishes rapidly beyond low Earth orbit (LEO).2,3,6 Celestial conjunction leading to blackout periods, speed limits of electromagnetic waves, limitations of current communication systems, and shortcomings of near future vehicle propulsion increasingly diminish the capabilities for telemedical support, resupply, and evacuation in medically meaningful timeframes as the distance from Earth grows.7–9 These factors mandate increased reliance on the KSA of the crew and medical system onboard the spacecraft as support from Earth decreases. 2 Thus, the optimal risk reduction strategy combines careful preflight health screening and maintenance with predictive analytics to quantify and qualify the risk of unplanned in-flight medical events. These 2 pillars inform the capabilities required of the medical system and, in turn, the training required by the crewmembers who must operate it.
Until recently, the subject of exploration CMO training has been purely conjectural. Most assessments of the optimal exploration CMO training relied on heuristic estimations based on subject matter expertise and tended to reflect the background of the physician or care provider making the recommendations. 5 For example, a surgeon might be biased toward the importance of surgical capabilities, while an internal medicine specialist might emphasize the importance of medical management.10,11 However, the ideal set of skills will invariably combine capabilities from a legion of terrestrial specialties and vary dramatically depending on the specific mission profile. 12 Fortunately, predictive analytics tools offer an evidence-based alternative that may help identify which capabilities are most likely to improve the chances of a successful mission. Outputs from probabilistic risk assessment tools are generated to provide operational teams with recommendations to consider regarding elements to build into a medical system and important capabilities that may translate to crew medical skills training.
NASA has used predictive analytics models to assess and mitigate the effects of medical risk in space for nearly three decades.2,4,13 The most recent of these, the Medical Extensible Database Probabilistic Risk Assessment Tool (MEDPRAT), drives the medical system design tool suite known as Informing Mission Planning through Analysis of Complex Tradespaces (IMPACT). IMPACT is an evidence-based and data-driven tool suite designed specifically for exploration class missions to predict relevant healthcare outcomes during spaceflight. 13 IMPACT defines a list of mission-relevant medical conditions in terms of the capabilities required for their diagnosis and management. These capabilities represent a broad range of knowledge, skills, and abilities that the medical system will need to support, such as to provide oral antiemetics, obtain intravenous access, or support management decisions for an upper extremity fracture. 14 IMPACT capabilities are comprised of individual resources that allow IMPACT to inform specific medical system elements and optimize those elements for mass, volume, and risk outcomes based on the desired mission parameters.6,14 For example, the capability to provide oral antiemetics may include specific medications, water, and a drink bag.
The capabilities in IMPACT were intended to inform the requirements for spacecraft medical systems based on a customizable, user-defined design reference mission (DRM). 14 However, since the capabilities are based on medical guidelines, they also often reflect the cognitive and procedural diagnostic and management skills required of the provider as well. 6 Since IMPACT uses incidence and outcome data to identify the capabilities with the greatest potential to improve the success of the mission, the list of capabilities offers an opportunity to apply data-driven predictive analytics to the question of medical officer training requirements and recommend a foundation for which to build a CMO curriculum around. The data that drives IMPACT comes from NASA medical records, space analog data, systematic reviews of medical literature, and clinical practice guidelines. These data were collated and curated into the IMPACT evidence library (IMPACT-EL) by subject matter experts, and terrestrial practice guidelines were modified to meet anticipated mission restrictions by clinical experts with extensive space medicine and space medical system design experience. This investigation used a preliminary version of the IMPACT-EL (lockdown 141) to explore this concept.
Methods/Procedures
The data in this paper was drawn from lockdown 141 of NASA's IMPACT – Evidence Library (IMPACT-EL). 15 The preliminary EL included 597 clinical capabilities along with incidence and outcome data for 120 medical conditions of interest for Lunar exploration missions. 16 MEDPRAT, the computational engine for the IMPACT tool suite, was used directly in conjunction with a modified version of the IMPACT-EL to perform the required simulations. This was necessary as MEDPRAT offered the additional flexibility and robustness required by the complexity of this analysis. 17
To estimate the effect of each exploration CMO capability rather than individual resources, a modification to the treatment data was required. MEDPRAT provides a highly malleable feature for defining treatment called “treatment clusters.”
18
Treatment clusters specify the relationships and dependencies between the resources themselves and also enable resources to be designated for the treatment of each condition in IMPACT-EL. For example, consider a capability “abdominal ultrasound” that consists of the following 3 resources:
ultrasound machine ultrasound machine power supply and ultrasound gel
Treatment clusters allow these resources to be assigned as a group to multiple conditions (eg, appendicitis, cholecystitis, and abdominal blunt trauma). The clusters also allow resources to be linked together (absolute), treated individually (partial), or substituted for equivalent alternatives (alternate). “Absolute” indicates that if only the gel is present in the MEDPRAT simulation, the abdominal ultrasound cannot be performed, and a condition requiring this ultrasound will not be treated. “Partial” means that if only the gel is present, 1/3 of the required resources are available, and the required condition will get 1/3 of the benefit resulting from the full abdominal ultrasound capability. The alternate structure allows ultrasound gel to be substituted for an equivalent resource (eg, water in microgravity) should the gel become depleted.18,19
The clinical resource tables (CRTs) in the IMPACT-EL organize data so that each condition is defined by clinical capabilities, and each capability contains the resources and their interdependent relationships.14,18 Capabilities are typically broad skill sets or clinical activities such as “obtain intravenous access,” while resources are discrete items (eg, “20 gauge IV catheter”) built within each capability that enable the performance of the named capability. The hierarchical structure of capabilities superseding resources functions as an organization tool within IMPACT-EL; however, resources are also associated with discrete masses and volumes enabling IMPACT to conduct material trades within the constraints of the spacecraft and determine how a missing resource affects mission medical outcomes.
Since capabilities are more descriptive of the training a clinician would need, the lockdown 141 data was reorganized to remove the resource characteristics (ie, mass and volume information) and force IMPACT to estimate clinical outcomes based on capabilities alone. This allowed the authors to analyze the effect of each capability by comparing the outcome when an individual capability was removed to the outcomes when the full set was available.
For each DRM, 2 different scenarios were considered. The first scenario used absolute treatment clusters so that if any individual capability in the condition treatment cluster was unavailable, the entire condition would remain untreated, and MEDPRAT would report the outcome values associated with the untreated state. In essence, there is no “partial credit” given for having some, but not all, of the capabilities.
The second scenario involved partial treatment clusters and allowed partial credit for whatever percentage of capabilities were available. This meant condition outcomes would fall somewhere between the fully treated and untreated outcome paths, with the exact weighting being a function of the number of resources available. For example, if 5 of 10 required resources are present, MEDPRAT would allow a 50% partial treatment credit and outcomes would be halfway between fully treated and fully untreated values. For this proof-of-concept study, MEDPRAT was configured so that each capability is used exactly once per condition occurrence, and all capabilities are weighted as equally important.
To quantify the relative importance of each capability, a “Leave-One-Out” sensitivity analysis was performed on the availability of each capability for treatment in the simulated mission. In this application, the most important capabilities are defined as the ones whose absence in the medical set results in the largest relative increase in risk. Performing the sensitivity analysis consists of configuring and running a simulation for each capability, where the only variable parameter from one simulation to the next is the specific capability being designated as unavailable in the medical system. In doing this, we could isolate the effect that each capability has on the mission and measure how the risk profile changes with these variations.
This analysis consisted of nearly 6000 unique simulations, one for each combination of 597 capabilities, 2 treatment scenarios (absolute and partial), and 5 DRMs. Scripts were written in the Python programming language to configure the input/setup data for each simulation and to post-process the output data. The simulations were autonomously deployed using a bash script to minimize human-in-the-loop requirements. Each simulation consisted of 300 000 parallelized trials and was run on the NASA Glenn Research Center Human Research Program computer cluster with 156 cores. The total runtime was approximately 150 h.
MEDPRAT and IMPACT-EL report 3 outcome metrics:
Mortality, reported as loss of crew life (or LOCL) Evacuation risk, reported as return to definitive care (or RTDC) Mission-specific disability, reported as task time lost (or TTL)
To simplify the analysis, only TTL was compared across profiles; however, a similar comparison can be performed for any of the outcomes. A clinical relevance threshold was set for determining which capabilities have a “significant” effect on mission outcomes. This threshold depends on the user's preference, and for the purposes of this proof-of-concept analysis, the authors arbitrarily selected a threshold of 5%. Thus, clinically significant capabilities were considered to be those with a minimum of 5% relative risk increase (RRI) over the baseline fully treated state for the target outcome metric. RRI is calculated first by taking the difference between the simulated risk from removing the capability minus the baseline risk and then dividing this by the baseline risk.
Results
For the purposes of this study, “fully treated” refers to a DRM with unlimited medical supplies and no risk of malfunction. Table 1 describes the 5 simulated mission profiles used in this investigation, which were adapted from the NASA Human Systems Risk Board design reference missions. 20
Design reference mission profiles used for the IMPACT simulations and the associated number of curriculum elements returned from the absolute and partial treatment scenario simulations.
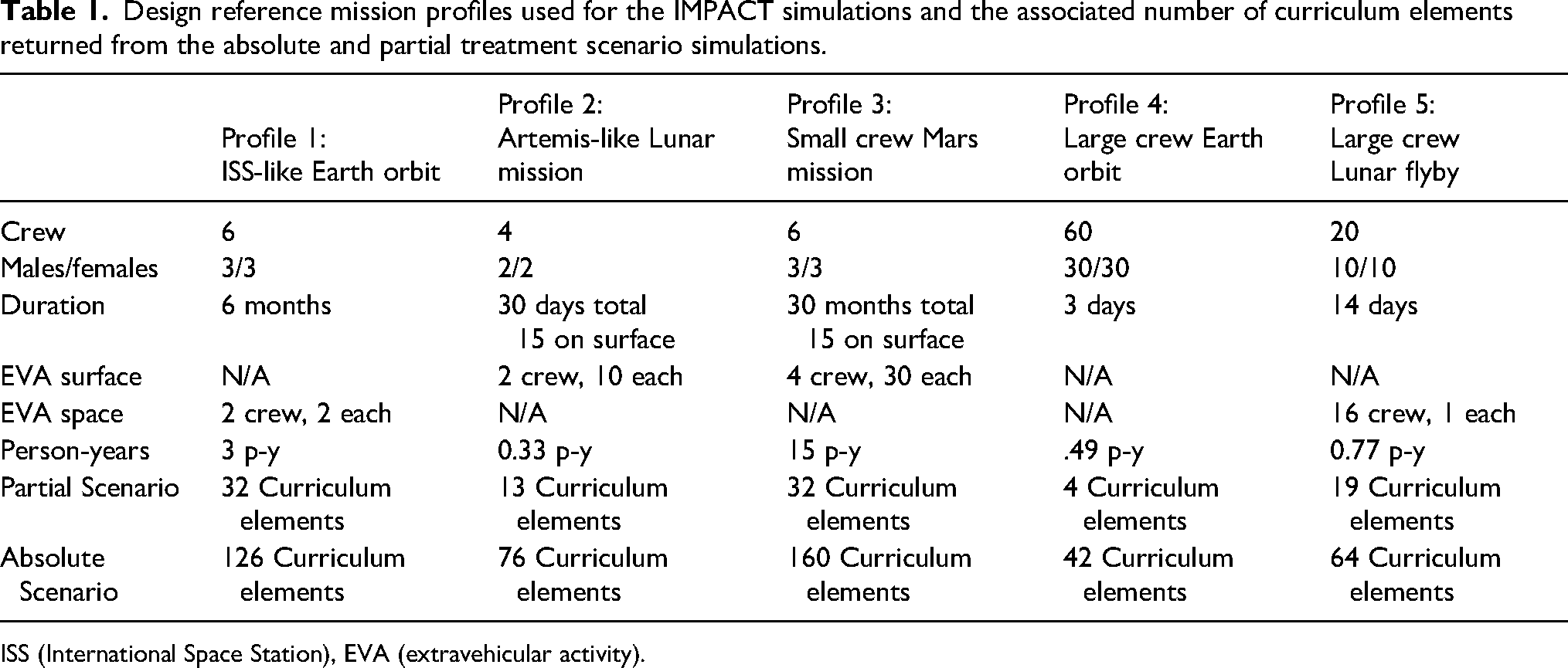
ISS (International Space Station), EVA (extravehicular activity).
The major factor influencing curriculum complexity is the number of person-years in the DRM. This is why the shortest profile has the fewest elements. However, specific mission activities, such as extravehicular activities (EVAs) on the Lunar surface, and the number of male versus female crewmembers also influence the system capabilities.
For the partial treatment scenario, there were 32 curriculum elements meeting the 5% RRI increase for profile 1, 13 elements for profile 2, 32 elements for profile 3, 4 elements for profile 4, and 19 elements for profile 5. For the absolute treatment scenario, there were 126 curriculum elements meeting the 5% RRI increase for profile 1, 76 elements for profile 2, 160 elements for profile 3, 42 elements for profile 4, and 64 elements for profile 5. For the partial treatment paradigm, 13 capabilities are present in at least 3 of the 5 mission profiles, and these elements may constitute a common baseline curriculum. This covers 41% of the skill sets needed for an ISS-like profile, 100% of the late Artemis-like profile, 41% of the Mars mission-like profile, 100% of a Starship orbital-like profile, and 68% of a Starship lunar flyby-like profile. Table 2 presents the common curriculum elements and compares them to the additional skill sets required for each tested profile as well as a curriculum made up of skill sets that appear in all 5 profiles. The common curriculum derived from capabilities that are present in the majority (3 or more) of the profiles is identical to the Artemis-like mission profile (profile 2). The orbital Starship-like profile (profile 4) only included 4 skillsets: collecting a medical history, interpreting a physical exam, performing a primary assessment, and assessing fitness for duty. In this context, the primary assessment refers to the initial assessment of immediate life threats commonly consisting of assessing a patient's circulation, airway, and breathing (CABs).
The capabilities meeting the 5% RRI threshold for the partial treatment paradigm.
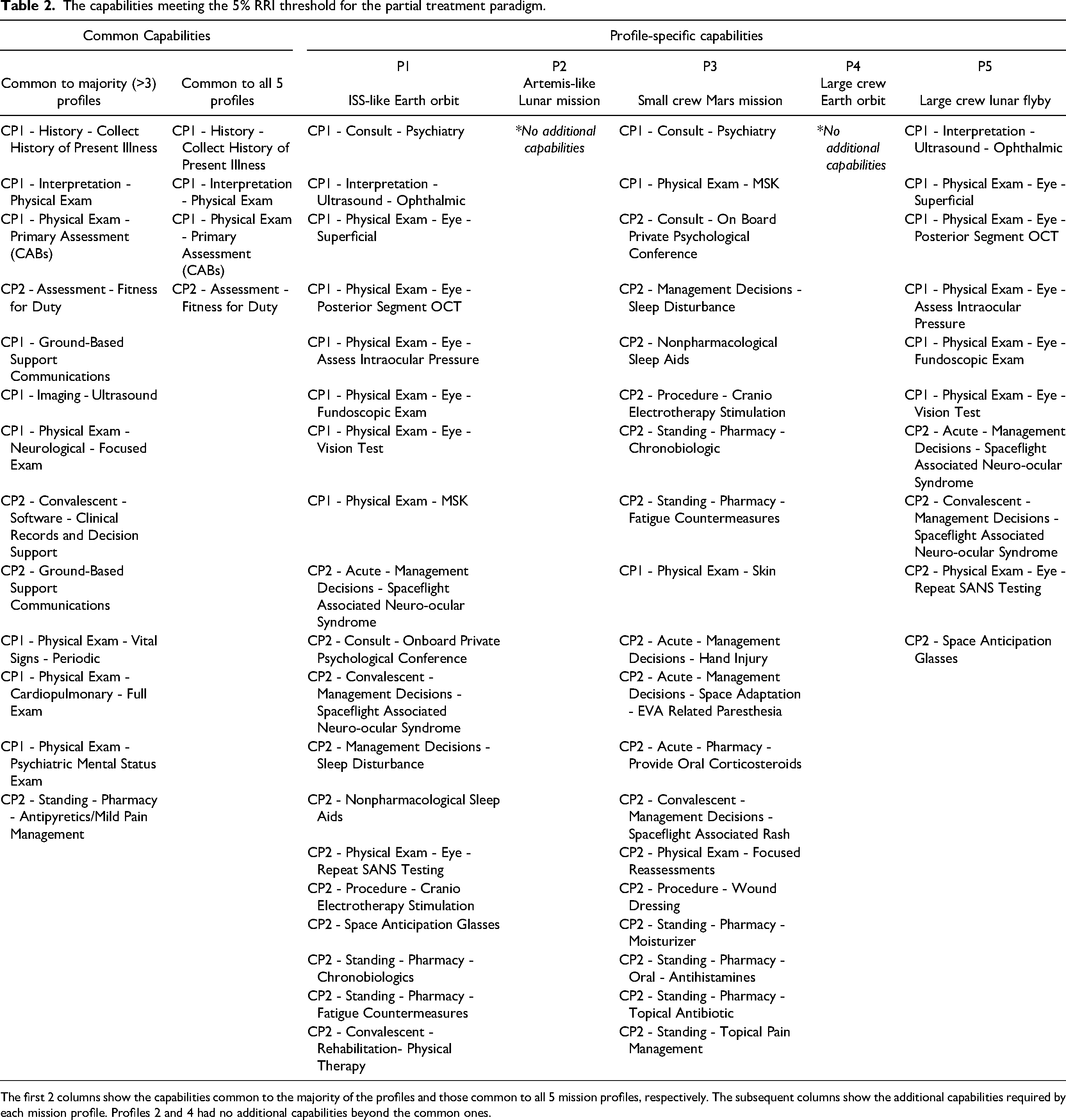
The first 2 columns show the capabilities common to the majority of the profiles and those common to all 5 mission profiles, respectively. The subsequent columns show the additional capabilities required by each mission profile. Profiles 2 and 4 had no additional capabilities beyond the common ones.
For the absolute treatment paradigm, a common curriculum that includes capabilities present in at least 3 of the profiles includes 72 elements. This covers 57% of the skill sets needed for an ISS-like profile, 95% of the late Artemis-like profile, 45% of the Mars mission-like profile, 98% of a Starship orbital-like profile, and 97% of a Starship lunar flyby-like profile. Table 3 presents the common curriculum elements and compares them to the additional skillsets required for each tested profile as well as a curriculum made up of skillsets that appear in all 5 profiles.
The capabilities meeting the 5% RRI threshold for the absolute treatment paradigm.

The first 2 columns show the capabilities common to the majority of the profiles and those common to all 5 mission profiles, respectively. The subsequent columns show the additional capabilities required by each mission profile.
Discussion
This proof-of-concept study demonstrates that predictive analytics tools such as IMPACT can rapidly generate evidence-based, outcomes-driven curricula for exploration CMOs that can be customized for a given DRM. Using this process, we were able to generate 5 distinct evidence-based curricula in less than 1 week, each customized for its specific DRM. It is also likely that the required time can be reduced as the tools and processes are refined through further study.
This probabilistic risk-based curriculum increased in complexity as the DRMs themselves became more complex, indicating that the system performs as expected. Furthermore, there were significantly higher numbers in the absolute treatment paradigm than in the partial treatment paradigm. This is also expected because the absolute paradigm means that a single absent capability renders the condition, requiring it untreated. This means each capability has a relatively greater effect on outcomes, but the overall mission risk is likely to be overestimated.
The partial treatment paradigm has the reverse problem. It is far more tolerant of missing capabilities, so each individual capability contributes relatively less to mission outcomes. This means it is likely to provide a closer approximation of actual mission medical risk because, in most cases, something can still be done for a patient even if a few items are missing. However, for the same reason, it is more likely to include incomplete sets of capabilities. This is why the partial paradigm list includes several assessments for ocular problems but none of the capabilities needed to intervene should a problem be found.
From a curriculum design perspective, it is more important to derive an optimal list of required skill sets than an accurate risk assessment. While the partial paradigm problem of orphan capabilities can likely be mitigated by lowering the RRI threshold, this implies that the absolute paradigm may be better for PRA-based curriculum design.
To date, there have been no deaths and only a handful of evacuations from space. 4 Thus, for pragmatic purposes, the PRA curriculum was optimized for TTL only. A single outcome was chosen due to constraints on processing time, and TTL was selected because medical care in space has historically been rendered to decrease crew downtime. 4 TTL is also likely to be the most comprehensive metric since capabilities that prevent death and evacuation are also likely to reduce task time lost. However, this is also likely to yield a longer list than the other 2 outcomes and may overestimate the training needs for a medical system optimized for a different outcome. A curriculum designed for a single outcome metric may also miss some important capabilities that are rare but more likely to lead to a loss of mission. However, it is sufficient for the proof of concept. Future studies can be run for each metric individually or all metrics as a group to balance the pragmatic with the severe. It is also important to consider that the data used in this study was drawn from a prevalidation and verification (V&V) version of IMPACT. While this is sufficient for a proof-of-concept, the listed capabilities may be more accurate once the V&V process is complete.
Understanding that premission training time is limited, it is difficult to customize crew training for every potential mission that space operators may wish to undertake. Our findings suggest that a more efficient model may entail developing a generic curriculum based on a set of high-level skills common to a variety of different mission profiles. This common curriculum could then be augmented with mission-specific skills, as needed, or modified into something all crew are trained on rather than only the CMO.
The absolute paradigm common curriculum, including capabilities common to at least 3 of the 5 profiles, is one example of how this might work. The curriculum primarily includes medical history, physical exam, ultrasound, and ground consultation skill sets with a few basic interventions such as antiemetics, antitussives, sleep management interventions, and mild pain control. The same is true of the partial paradigm skills list, though it includes fewer capabilities. If a narrower curriculum is desired, mission planners could opt for capabilities common to even more DRMs or simply choose the capabilities for a short-duration mission.
Another potential use for this type of PRA-informed curriculum design is to identify which preexisting terrestrial curricula most closely approximate the skillsets required for the mission. Using the results in this way can help minimize premission planning by informing crew selection based on existing medical backgrounds. For example, using the absolute paradigm curriculum results, the most complicated curriculum is the Mars mission-like profile. This curriculum contains 160 curriculum elements—almost all of which fall into the core competency requirements for emergency medicine and family medicine.21,22 Only a few competencies, such as making management decisions for spaceflight associate neuro-ocular syndrome (SANS), fall outside the competencies for residency-trained family and emergency physicians. Based on these data, it may be more efficient to develop a tailored training program for a family or emergency physician rather than a custom 160-point curriculum for a nonphysician or a physician specialty with less capability overlap. 12
Conclusions
This study demonstrates the successful application of predictive analytics to inform curriculum design and highlights the versatility of the system levers to rapidly generate both generic and tailored training programs on an as-needed basis. When employed as part of a human-machine team for future exploration CMO curriculum designs, PRA can provide objective data to serve as a foundation upon which subject matter experts can then begin to address challenging questions surrounding spaceflight medical risk mitigation that have historically had to rely solely on expert opinion. It may save substantial time and effort for both planning and training and has the potential to improve astronaut health. This will be particularly important as increasing mission numbers, mission complexity, and crew medical complexity begin to tax existing space medicine infrastructure. 2
Footnotes
Acknowledgments
We are eternally grateful to Lynn Boley and the rest of the Exploration Medical Capabilities Element Clinical Science Team.
Author Contribution(s)
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
