Abstract
Long-duration spaceflights beyond low-Earth orbit, including missions to the Moon and Mars, pose significant health risks. Although biomedical approaches commonly appear in the literature, considering psychological and social factors alongside physiologic health offers a more holistic approach to astronaut care. Integrating the biopsychosocial (BPS) framework into medical planning addresses complex spaceflight challenges and aids in developing mitigation strategies. This review examined health risks associated with long-duration spaceflight within a BPS framework. Sources included governmental space agencies, academic textbooks, and relevant publications from multiple databases. Considering the National Aeronautics and Space Administration's Human Research Program's 5 main hazards, a conceptual model was developed to highlight the multifactorial BPS effects of spaceflight. In space, astronauts face unique environments and biological adaptations, including fluid shift, plasma volume loss, bone density loss, and muscle atrophy. Noise and the absence of natural light disrupt circadian rhythms, causing sleep disturbances and fatigue, which affect physical and mental health. Studies on crews in isolated and confined extreme environments reveal psychosocial challenges, including impaired mood and cognition, interpersonal tension, and miscommunication. International collaboration in spaceflight introduces differences in communication, problem solving, and social customs due to diverse cultural backgrounds. Upcoming long-distance missions likely will amplify these challenges. This review emphasizes BPS health considerations in long-duration spaceflight. It highlights the interplay among psychological, social, and biological factors, advocating for multidisciplinary teams and a holistic approach to astronaut health and mission planning and the potential added value of BPS perspectives in considering countermeasures.
Keywords
Introduction
Long-duration and long-distance spaceflight missions pose multiple health risks. In space, crew illness or incapacitation has the potential to risk both the entire crew's health and safety and mission success. 1 Healthcare services are limited beyond Earth, with emergency return trips from the Moon being difficult and time-consuming and nearly impossible from Mars. The growing diversity of crews emphasizes the importance of individualized medical considerations, and longer-distance missions prompt the need for less reliance on real-time communication with Earth.
The biopsychosocial (BPS) model
2
offers a holistic framework for health and considers interactions between biological (eg, anatomy, physiology, neurochemistry, and genetics), psychological (eg, cognition, attitudes, and personality), and social factors (eg, culture, education, interpersonal relationships, socioeconomic variables, and companionship3,4). Discrepant to the biomedical model “
The National Aeronautics and Space Administration (NASA) Human Research Program (HRP) outlines 5 main health/performance hazards of human spaceflight: 1) gravity fields, 2) radiation, 3) hostile closed environments, 4) distance from Earth, and 5) isolation and confinement. 13 Addressing these challenges and health needs effectively requires collaborative healthcare expertise. Adopting multidisciplinary team (MDT) care can improve quality of care and health outcomes significantly.14,15 The segregation of teams into biomedical and psychosocial may impede the adoption of a BPS approach to care. 16 Furthermore, the positive impacts of multidisciplinary care in team sciences have been highlighted previously in isolated, confined, and extreme (ICE) environments (eg, space) when reviewing the bidirectional effects of neurobiology on behavior and social dynamics. 17 To optimize care, each MDT member should be grounded in BPS approaches, promoting shared mentality across disciplines. 18 Space agency MDTs, including crewmembers, typically are comprised of individuals with backgrounds in medicine, nursing, physiotherapy, pharmacy, nutrition, psychology, and biomedical engineering.19,20 NASA's Exploration Medical Capability component of the HRP comprises a clinical science team that provides clinical insights to systems engineers to develop the necessary medical technologies for long-duration spaceflight. 21
Space medicine MDTs are well equipped to apply BPS care, but the current literature rarely addresses spaceflight's medical challenges using this approach. To accentuate the importance of embedding BPS approaches into medical planning for long-duration and long-distance spaceflight, a focused initial review of the principal evidence base is warranted. Therefore, this review aims to 1) present the cardinal evidence on health risks related to long-duration and long-distance spaceflight in the context of BPS approaches, 2) explore the interlinking factors that may influence health and performance in space, and 3) present a model that visually represents these elements.
Previous reviews have provided focused insights into the management of astronaut health and performance that contribute to understandings of BPS care. For instance, Landon et al discussed important neurobiological processes that impact behavior and social dynamics in ICE environments. 17 Our paper, however, seeks to provide a broader overview of space medicine that focuses on holistic approaches to astronaut health and performance, adopting the BPS framework. Reviewing current understanding using distinct and overlapping aspects of biological, psychological, and social health factors allows the multifaceted challenges of long-duration spaceflight to be presented in a clear and succinct manner. However, the complexity of space medicine requires careful interpretation to avoid oversimplification of its challenges. Our intention is to present this review as a complementary framework that builds on and can integrate with existing space medicine literature, reviews, and practices, additionally expanding the space medicine capabilities within the United Kingdom and beyond. Acknowledging current efforts to identify MDT research gaps,22,23 this review can be positioned within the broader context of current research and practice that also underscores potentially unconsidered reciprocal BPS health factors for future space medicine research.
Methods
Given the scale of the topic, large heterogeneity of possible sources, disparity of interventions, variability of outcome measures and analyses, and mixed time frames, a narrative review was preferred to a systematic review. 24 The following sources informed the subsequent review: governmental space agency websites (eg, NASA's HRP and Technical Reports Server and evidence and commissioned reports), space medicine academic textbooks, and pertinent publications searched using EBSCO, PubMed, Web of Science, Google Scholar, and King's College London Library.
Search filters included English language from 1950 to 2024. To capture an overview of the topic, search terms included “astronaut” OR “aerospace” OR “astronaut health” OR “aerospace medicine” OR “space medicine” OR “spaceflight” AND “health” OR “medic*” OR “risk” OR “physio*” OR “psycho*” OR “social” OR “biopsycho*.” Where spaceflight-specific research was unavailable/nonexistent, we highlighted understandings from terrestrial population literature to discuss possible relevance to human health in spaceflight.
Discussion
Challenges of Human Spaceflight
Long-duration space missions present many biological, psychological, and social challenges. These begin with preflight training, where astronauts and cosmonauts are exposed to remote and extreme environments and rigorous physical activity. This phase may result in significant psychological stress due to isolation from family, friends, daily routines, and cultural events.
During flight, astronauts are exposed to the unique environment of space, leading to biological adaptations. The experience of living in confinement and managing high-pressure tasks essential for mission success further exacerbates psychological strain. On returning to Earth, astronauts face the effects of physiologic adaptations to space, which become adverse within Earth's gravity. This requires extensive medical testing and physical reconditioning. Demanding post-mission schedules can further contribute to feelings of isolation from family and friends.
Despite stringent medical standards, humans remain susceptible to illness, injury, psychosocial challenges, and medical emergencies in unpredictable and isolated environments. Serious medical events have been predicted to occur once every 2.8 years 25 and elevate with increasing distance beyond low-Earth orbit (LEO). NASA's Human System Risk Board (HSRB) determines the risks and likelihoods of mission scenarios, varying by mission design. High likelihood (>1% per year) of “death or permanently disabling injury to one or more crew” or “severe reduction of performance that results in loss of most mission objectives” during a 3-year mission has been suggested. 26
Upcoming missions such as Artemis, the Lunar Gateway assembly, and human exploration of Mars will extend the boundaries of space travel. These long-duration and long-distance missions require comprehensive strategies to address complex challenges. Prolonged separation from Earth likely will amplify the physiologic, psychological, and social stressors affecting astronauts, highlighting the interplay among these factors.
Biological Challenges
The biological challenges of human spaceflight are closely related to its unique environment, including altered gravity, radiation, remoteness, and the body's physiologic and pathophysiologic responses. Although some changes lead to adaptation to the new environment, others may be maladaptive and pose health risks to astronauts.
Ionizing radiation is a key challenge for human deep-space exploration. While Earth's magnetosphere offers some protection for International Space Station astronauts, those traveling beyond LEO will face increased doses of high-energy radiation. This may cause DNA and cellular damage, carcinogenesis; 27 damage to cardiac tissues and early onset of atherosclerosis; 28 microbiome alterations; 29 neurobehavioral impairments and nervous system damage; 30 skin burns; modifications in bone, muscle, cartilage microarchitecture;31,32 and prodromal symptoms such as nausea and vomiting. However, the health consequences of space radiation are complex, making it challenging to quantify the acute and long-term effects anticipated for astronauts on long-duration missions.
Microgravity is another challenging factor leading to a cephalic fluid shift that increases stroke volume and cardiac output. Although natriuresis and peripheral vasodilation maintain blood pressure during flight, these adaptations may compromise cardiovascular function on return. Astronauts may struggle to stand or readapt to Earth's gravity due to changes in blood volume, peripheral resistance, and sympathetic nerve activity. 33
The cephalic fluid shift also leads to facial edema, which is hypothesized to contribute to changes in intracranial pressure. 34 Changes in facial features and unusual orientation relative to each other may disrupt crewmembers’ ability to recognize nonverbal cues and make communication and social interaction difficult. 35 The nasal blockage due to edema may affect odor and flavor perceptions, potentially leading to decreased food enjoyment, an important factor for crew well-being.
Microgravity also leads to space adaptation syndrome, resulting in nausea, vomiting, dehydration, electrolyte imbalances, and potentially impaired task performance. Additionally, it affects spatial orientation and gaze stabilization, impairing object localization and perceived shape and size. 36 However, the symptoms typically subside on their own with adaptation to the space environment within a few days.
In microgravity, mechanical loading is reduced, causing decreased muscle protein synthesis, increased protein breakdown, and induced bone resorption. This results in bone mineral density (BMD) loss of ∼1% to 2% per month. 37 Elevated carbon dioxide and dietary acids exacerbate bone loss by altering acid buffering, 38 with bone bicarbonate being used as compensation. 39 Loss of BMD results in hypercalcemia and increased calcium excretion, predisposing astronauts to renal stone formation. 40 Microgravity also may alter tendon collagen and cartilage content and impede wound healing. Additionally, it increases spinal column length, reduces thoracic and lumbar curvature, and weakens trunk muscles, increasing the risk of disc injury and back pain on return to Earth. 41 The combination of microgravity and cosmic radiation further enhances bone loss and fracture risk. 42 It is unclear how exposure to the gravity on the Moon or Mars will affect these responses.
Microgravity and spaceflight conditions may suppress the immune system, making astronauts more susceptible to infections. 43 Furthermore, the enclosed spacecraft environment can harbor microbial contaminants, posing health risks to the crew. Microbiome alterations can contribute to chronic inflammation, which predisposes various diseases. Additionally, microgravity, radiation, and stress also have been associated with deleterious effects on oral health 44 and skin, 45 with reports of erythematous, burning, itchy, and sensitive skin during and after flight. 45
Adverse physiologic health risks can trigger psychological consequences. For instance, one cosmonaut's mission terminated early partly due to psychosomatic worries about prostatitis and impotence. 46 Terrestrially, stress, depression, and anxiety concerning functional decline are commonly reported by patients experiencing hospital-associated deconditioning. 47 Anxiety and depression have been negatively associated with BMD.48–50 Discomfort and inability to perform occupational and mission-specific tasks efficiently when exposed to altered gravity may cause further frustration.
The distance from Earth complicates nutritional management in space. Astronauts must receive adequate nutrition to sustain their health and mitigate the physiologic effects of weightlessness. Nutritional deficits may negatively influence neurochemical processes and contribute to pathophysiologic changes of anxiety and depression, potentially resulting in impaired concentration, social interaction, and occupational performance. 17 However, maintaining a balanced diet poses challenges due to limited food choices, storage constraints, and nutrient degradation over time, as well as the appetite-suppressing effect of microgravity.17,51 Furthermore, the selection, storage, and consumption patterns of food items may influence the enjoyment of food due to altered flavor, odor, or appearance. 52 The busy schedule may impact social dynamics surrounding mealtimes in space. 17
Microgravity and the absence of natural light disrupt circadian rhythms and, in combination with operational noise, can lead to sleep disturbances and fatigue. These sleep issues adversely affect all major bodily systems and increase the risk of disease and medical events, even in healthy individuals.53,54 Sleep deprivation also can adversely affect cognitive function, mood, and overall health. These factors may induce stress responses and negatively affect astronauts’ psychological and social well-being. 17 Furthermore, sleep disturbances may increase feelings of loneliness and social withdrawal, 55 which may be exacerbated by long-duration missions. Importantly, loneliness and social isolation have been associated with increased risk of heart disease and stroke. 56
Finally, asthenia, recognized by Roscosmos as a long-duration spaceflight health threat, includes symptoms such as fatigue, nervous exhaustion, sleep disturbances, irritability, and prolonged negative emotions. 57 It is caused by factors such as microgravity deconditioning, radiation exposure, high workloads, and prolonged isolation. Although NASA is aware of the phenomenon, it does not recognize it as a distinct condition due to diagnostic subjectivity and overlap with anxiety, depression, and chronic fatigue syndrome. 58 Nonetheless, these symptoms are important considerations for mission success and crew safety.
Psychological Challenges
Long-duration space missions pose many psychological stressors ranging from confinement and isolation to the demands of living and working in confined, highly controlled environments. 59 Psychological resilience becomes critical in the face of prolonged separation from Earth and is compounded by the inherent risks and uncertainties associated with deep-space exploration. In recent decades, as missions have extended in duration, there has been a growing recognition of the importance of addressing the psychological challenges in spaceflight. 60 Efforts to understand the complexity of human psychological adaptation to the space environment are a result of interdisciplinary perspectives from psychology, neuroscience, and human factors and space medicine, which are embedded in NASA's HRP Human Factors and Behavioral Performance element. The psychosocial impacts of being far from Earth are not well researched in spaceflight itself because previous missions generally have kept Earth visibly large rather than as a distant, small point of light. 61
Group living in confined spaces throughout long-duration missions can cause psychophysiologic stress. Terrestrial analogues for confinement (eg, closed-chamber environments) have inflicted psychoneuroendocrine duress and pathophysiologic symptoms in long-term studies. Findings have included altered biomarkers of stress hormone levels and neurocognitive and immune modulation.62,63 Perceptions of crowdedness and overlapping work schedules have been considered for habitable spacecraft designs. 64
Selye's general adaptation syndrome framework 65 elucidates the interconnectedness of psychological and physiologic responses under the presence of significant stressors. This framework, delineating the stages of alarm, resistance, and exhaustion, provides a structured approach to understanding the adaptive processes brought by the stressors of long-duration spaceflight. Adapting Selye's model to spaceflight, the alarm stage may be initiated by the novel stressors of isolation and confinement, triggering a series of physiologic responses primed for acute stress management. This is followed by the resistance phase, where adaptive mechanisms strive to restore homeostasis amid sustained stressors. Prolonged exposure without effective coping strategies, however, may culminate in the exhaustion phase, depleting the body's reserves and jeopardizing astronaut health. This emphasizes the need for advanced support systems and resilience-building strategies for astronauts on extended missions.
Despite many challenges, long-duration missions in remote environments also may bring positive long-term psychological effects. Individuals who adapt positively may derive benefit by gaining an improvement in mental health as they adjust to the environment as well as more sustained personal growth during the mission, described by the concept of salutogenesis, 66 a theory that suggests that not all stressful experiences inevitably lead to illness; rather, effective management of tension can mitigate negative physiologic and psychological outcomes.
Specifically, a group of individuals facing similar circumstances and challenges may cope with their anxiety and pressure more effectively than others facing them alone, 67 emphasizing the crucial role of social interconnectedness within the BPS approach. When applying this principle, space agencies should continue to develop training sessions and in-flight activities that focus on enhancing interpersonal communication skills 68 as well as harnessing social bonds that foster a sense of purpose and meaning in the mission. Preflight and in-flight activities should encourage the development of a supportive and cohesive team dynamic among astronauts. These considerations can be enabled by embedding BPS approaches in medical and mission planning.
Social Challenges
Spaceflight is an example of a human endeavor that requires effective social cohesiveness and teamwork to ensure safety and mission success. Long-duration exploration–class missions into deep space amplify the social factors that can directly impact mission safety and success as well as impact the psychological and physical conditions of astronauts. Terrestrially, social connectedness and networks have been associated with better health, longevity, and improved physiologic measurements, 69 with positive social connections being a primary determinant of happiness and longevity. 70 Contrastingly, older adult studies from COVID-19 pandemic lockdowns considered the detrimental impact of social isolation.71,72 Furthermore, social connections, or threats to it, can alter sympathetic nervous systems and hypothalamus-pituitary-adrenal axis activity accordingly. 73 ICE environments with small crews limit social relationships, where social monotony is likely to occur over time. 74 The risk of ostracism and subgrouping in ICE environments (eg, from simple disagreements between crew and/or mission control) can be detrimental to team cohesion, creativity, cognition, safety, and psychosomatic health.74,75 However, the extent of stress that an individual will experience remains debatable because some evidence shows either no effect or even positive behavioral effects (eg, improved self-confidence and courage) occurring with exposure to ICE environments. 74
Studies on terrestrial crews and individuals living and working in ICE environments (eg, polar stations, oil rigs, submarines, and space analogues) have highlighted the social challenges faced by those in such environments. These range from social withdrawal to interpersonal tension and hostility toward team performance (eg, poor leadership, miscommunication, and poor teamwork), which can lead to adverse outcomes or failure to achieve the intended mission objectives.73,75
The social factors associated with long-duration spaceflight encompass various aspects of crew interaction, communication, and cooperation, as well as the socioeconomic, socioenvironmental, educational, and cultural backgrounds. Considering these diverse elements among crew members on long-duration space missions is crucial because they will influence social dynamics in the ICE environment of space beyond LEO.
Interpersonal dynamics, social integration, and team performance are heavily influenced by the unique team composition. Bell et al highlighted the importance of identifying team composition variables and configurations associated with performance risks.
75
Differences in sex, personality, communication style, power/distance, and cultural backgrounds among crew members may lead to subgrouping, conflicts, and compromised safety. Subgrouping can occur if some team members have familiarity or shared experiences (eg, training and flights), and newer team members disrupt the social integration, coined the
Another point to consider is restrictions to privacy and intimate partners, which may heighten interpersonal conflicts 3 and psychophysiologic stress. 17 Additionally, the potential for romantic and sexual relationships forming between crew members may affect professional working relationships, impact the wider team and mission, and have politicoeconomic repercussions for the organizations involved. 3 Furthermore, the international collaborative approach to spaceflight brings together astronauts from different national space agencies and consequently diverse cultural backgrounds. This diversity can present challenges in effective teamwork and collaboration, particularly in areas such as communication norms, problem-solving approaches, and social customs.77,78
Communication delays due to distance from the Earth during exploration-class missions pose significant challenges when urgent communication is necessitous between crew and mission control during an emergency. Communication delays with loved ones back on Earth also can compound feelings of isolation and remoteness for crew members. 79 Misinterpretation of text, voice, or video messages and difficulty conveying emotions through communication methods that do not occur in real time can strain relationships, further exacerbating feelings of isolation among crew members. 80 Using a BPS approach provides a holistic framework to incorporate all these social aspects into health and performance elements of mission planning.
Biopsychosocial Model
Health and performance considerations for long-duration and long-distance spaceflight, through the BPS model, are summarized in Figure 1, applying NASA's 5 main hazards of spaceflight. For simplicity of presentation, the link is presented broadly in each BPS component, rather than to each individual health risk, due to the complexity and overlapping influence of each hazard. The initial review and model identify the key BPS health interconnectivities, highlighting the need for further research. In the figure, topics that are predominantly biological, psychological, or social are presented in those parts of the diagrams. However, it is important to remember that application of the BPS approach means considering the psychosocial aspects of all those points just in the biological section as well as those that more obviously overlap with psychological or social domains. The same is true for elements primarily within both psychological and social domains.
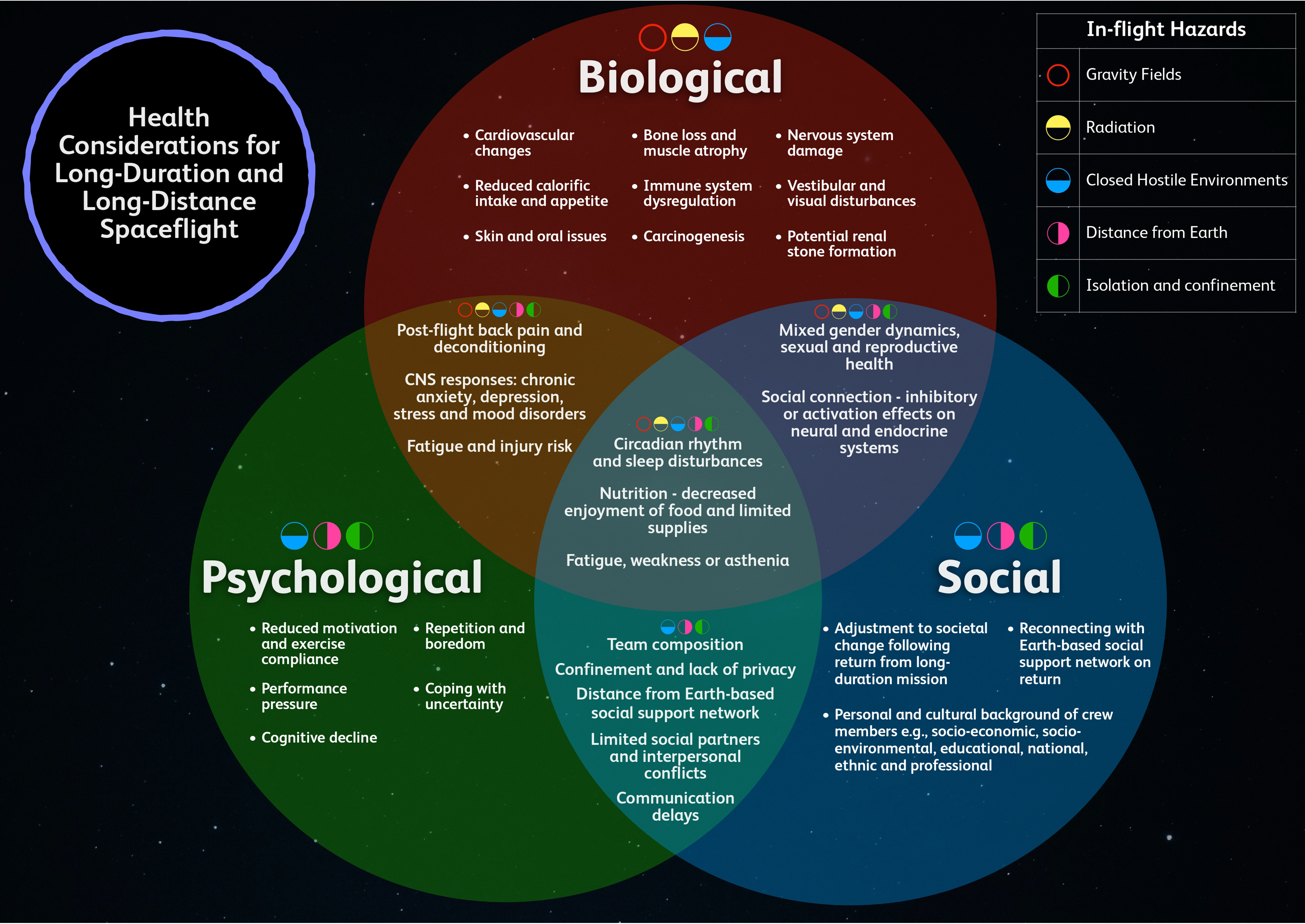
Application of the biopsychosocial model for long-duration and long-distance spaceflight. This presents health and performance considerations for long-duration and long-distance spaceflight through the lens of the biopsychosocial model, which applies NASA's 5 main hazards of spaceflight to the biological, psychological, and social sections. Top right: color-coded key representing NASA's 5 main hazards of spaceflight. CNS: central nervous system.
Space Medicine Planning and Future Considerations
Space medicine planning requires risk assessment, prediction, and concepts of operations and infrastructure to accommodate necessary countermeasures and medical system components, including medical kits and supplies. NASA's Integrated Medical Model (IMM) represents a significant step in quantifying and predicting medical risks associated with space missions by integrating spaceflight and analogue medical data to estimate impacts on crew health and mission success. 81 Employing a probabilistic risk assessment, the IMM anticipates possible medical emergencies and necessary interventions. 82 It includes a database of medical conditions that could occur in space, evaluating incidence, best- or worst-case outcomes, and necessary medical resources.
However, the IMM predominantly features biological conditions, reflecting the extensive data derived from historical space missions that primarily captured physical health issues. As we continue to understand the psychological dimensions of spaceflight and psychosocial considerations of biological disease, incorporating additional considerations could further improve the model and its impact. Stress, cognitive decline, interpersonal conflicts, and homesickness can impact crew performance and mission success significantly. Addressing these challenges alongside physical health risks by including a BPS approach in medical models and associated medical planning or medical concept of operations would ensure a comprehensive approach to astronaut health and performance that enhances overall mission safety and effectiveness. With the further development of an accepted medical condition list 83 tailored for extended missions, there is a clear recognition of the need for vigorous risk-management processes that incorporate elements of spaceflight and extravehicular activities beyond LEO. IMM version 4.0 has introduced functionalities that improve its predictive capabilities under different spaceflight conditions, such as longer and more isolated missions. 84
The Human Factors and Behavioral Performance element of NASA's HRP have adopted a translational approach that aims to address the combined impacts of space radiation, isolation, and altered gravity on the central nervous system and overall well-being of crew members, aiming to enhance crew functionality and long-term health through comprehensive strategies that mitigate these interrelated risks, 85 which is a great example of a holistic BPS approach. Furthermore, biomarkers relating to the central nervous system effects of radiation exposure, stress response, and sleep disturbance are currently being evaluated as possible tools for early detection of adverse cognitive effects. 86
Causal diagramming using directed acrylic graphs (DAGs) has been employed to analyze large datasets, including those from the HSRB, to algorithmically map out causal connections between various stimuli (ie, common spaceflight hazards) and potential impacts on mission-level outcomes. 87 This method has been considered valuable for fostering communication among HSRB stakeholders from different disciplines, supporting an MDT in sharing the same mental model of the situation. Individual DAGs can be used to create risk networks that can be structurally and computationally analyzed to gain insights into countermeasure development and mission preparation. 87 When developing such models, it is important to give emphasis to MDT and BPS factors. Although previous literature supports an MDT approach, 17 our review advocates for giving emphasis to this through a BPS framework, alongside the conventional biological and psychological aspects of medical planning.
Risk mitigation is essential to each mission phase, starting with preflight strategies that involves selection and preparation to ensure medical suitability, psychiatric qualification, psychological suitability, and team and social cohesion. Personalized medicine approaches can optimize selection with high individual specificity.88,89 For example, identifying disease-predisposing genes can exclude candidates, whereas genetic profiles resilient to spaceflight adversities are more desirable. 90
In-flight, countermeasures include exercise and nutrition plans. The European Space Agency has previously adopted an individualized training approach to exercise countermeasures considering fitness levels, personal preferences, and career status. 91 Missions greater than 6 months risk boredom, psychological fatigue, and low motivation to exercise adherence. 92 Strategies to reduce exercise time such as blood flow restriction, neuromuscular electrical stimulation, and whole-body vibration have been proposed and are being explored. 38 Extended-reality modalities may improve enjoyment and motivation for exercise. 93 Other potential extended-reality applications in spaceflight include virtual reality to simulate larger habitable volumes to overcome the stress of crowdedness and confinement, augmented reality for simulated images of Earth settings, virtual reality and artificial intelligence (AI) for social interaction, and simulated social sphere beyond crewmates to combat loneliness or improve team cohesion and for games and entertainment. 93 Continuous well-being monitoring via AI-based voice stress analysis and personalized in-flight interventions using virtual reality, 94 digital self-help resources, 95 and AI-integrated robotic human or animal companions are also options. Additionally, scheduled or themed mealtimes can aid in-flight nutritional management by encouraging organized breaks and enhancing social and cultural cohesion. 17 Postmission countermeasures focus on reconditioning to Earth through comprehensive physiologic rehabilitation, debriefing, social reintegration schemes, and continued psychological support to mitigate long-lasting health effects.96,97
The demographic diversity of spaceflight is expanding in age, sex, and ethnicity. Biological variability is considered within the DAG approach via the “individual factor” node and allows for personalized adaptations to medical planning to occur. 95 Differences in some populations are also relevant considering health disparities and lower socioeconomic status. Psychological resilience and social dimensions also can be impacted by cultural factors, whereas unique needs will be required for physical disabilities. The European Space Agency's Parastronaut Feasibility Project highlights intentions to promote greater inclusion. 98
Despite diversification, significant data gaps exist. NASA astronauts are now more likely to be female, civilian, and older, yet females and ethnic minorities remain underrepresented in research. 99 Although the scope is shifting toward greater diversity, spaceflight-specific data remain scarce and somewhat limit effective DAGs for these populations. To promote diversity, equality, and inclusion within effective BPS care for space travelers, future research must address these gaps. These data can provide input for future DAGs, predictive modeling, and algorithms and personalize medicine with AI. Benefits of this can extend to commercial spaceflight, where the diversity likely will exceed that of current astronauts and include individuals with preexisting medical conditions or disabilities.
As current exploration medical capability investigations aim for a progressive paradigm shift toward Earth-independent medical operations, 100 BPS approaches should be embedded in these efforts. Table 1 represents a selection of countermeasures at different mission phases, identifying their aims and the potential added value of BPS considerations.
Countermeasures for long-duration spaceflight with potential added value of biopsychosocial consideration.
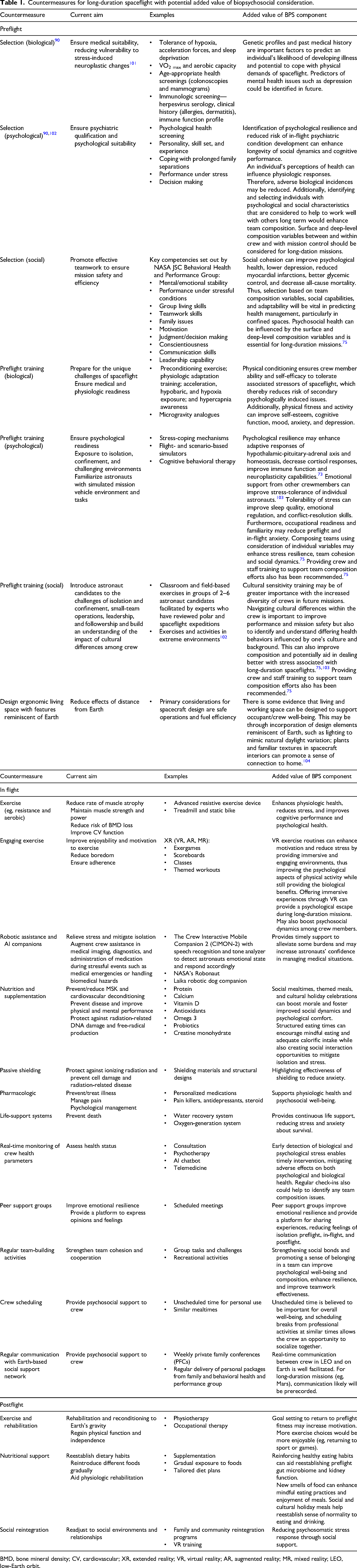
BMD, bone mineral density; CV, cardiovascular; XR, extended reality; VR, virtual reality; AR, augmented reality; MR, mixed reality; LEO, low-Earth orbit.
Conclusions
Adopting a BPS healthcare philosophy provides a holistic approach to long-duration and long-distance spaceflight, beyond medical kit contents, and can shape health and performance systems architecture and concepts of operations. To our knowledge, this review is the first to address space medicine using the BPS framework. Psychological and social factors are antecedents to biological health and vice versa. Countermeasures that reflect BPS elements are likely to enhance their outcomes. Continued inclusion of MDT care in current practices will be integral to its success.
Footnotes
Author Contribution(s)
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
