Abstract
Fishing is a common recreational activity in the United States, with over 29 million registered fishers. Although not inherently dangerous, commonly seen injuries from fishing include embedded fishhooks and injury from flora and fauna. Emergency department (ED) physicians need a basic understanding of how to treat these less-than-frequent injuries. We present a case report of a patient who presented with a catfish spine lodged in her leg. These spines not only cause puncture wounds but can result in lacerations and venom release as well. Our patient presented 6 hours after the initial injury for spine removal and symptom management. Plain radiographs of the affected extremity demonstrated a 2 cm foreign body consistent with a catfish spine. The wound was expanded, and the spine successfully removed. The patient was discharged on levofloxacin and reported a healing wound without complications nearly 2 weeks after the injury.
Introduction
Fishing in the United States occurs for business and leisure in various bodies of fresh and salt water. Freshwater leisure or sport fishing is common in the United States, with over 29.2 million registered fishers or anglers. 1 Species fished vary widely, with common choices in the Northeastern state of Pennsylvania being the larger “flathead” (Pylodictis olivaris) and smaller “channel” (Ictalurus punctatus) varieties of catfish. These species are sought out for their large size, which can reach upwards of 100 lbs. 2
Channel catfish are social and largely omnivorous. 3 Channel catfish use their sensory whiskers or “barbells” to transmit both touch and taste. 4 These whiskers are located around their mouth. Catfish respond to threats with venom-containing spines in their two pectoral and single dorsal fins. 4 The spines are retracted at rest, but when startled, the catfish binds and locks them in an extended position, causing impaled trauma. 4 The catfish moves its body laterally to make it easier for the spines to enter the victim. The spines contain proteolytic venom glands inside glandular tissue within an integumentary sheath. 4 Once the spine penetrates the skin, the integumentary sheath is damaged, and the venom gland is exposed. 4 This allows toxin release into the wound in which the spine has directly penetrated. The toxin is acidic and causes immediate pain, and it has hemolytic effects that contribute to prolonged bleeding at the site of injury. The pectoral spines blunt with the increasing age of the fish. Therefore, younger fish have sharper spines, which increases their ability to injure fishermen. 5
Prior literature has revealed that catfish have injured fishers and bystanders, most commonly to the hands. 6 Injuries range in severity from minor puncture wounds to fatal penetrating wounds of the thorax or abdomen. 6 Direct trauma can cause immediate mechanical damage, while toxin-mediated damage predominates soon after penetration, followed by infection in the subsequent 2 weeks. Bacterial infection is caused by either skin or water organisms. 7 The type of water involved cannot be used to guide antibiotic coverage. Vibrio, commonly thought of as a saltwater organism, has been isolated from freshwater 8
This case report is unique and contributes to the existing literature in several ways. The patient presented in land-locked southeastern Pennsylvania, where marine injuries are rare presentations in the ED. Additionally, the patient presented approximately 6 hours after the initial injury, placing the patient at increased risk of complications. The anatomical location of the injury prevented the standard use of hot water soaks to inactivate the toxin. Therefore, the decision was made to use a novel approach of lidocaine buffered with sodium bicarb to neutralize the acidic environment. 9 This approach has not been utilized in the literature to the best of our knowledge.
In this case report, we present a case of a patient with a puncture wound in the thigh secondary to freshwater catfish spine penetration and subsequent spine avulsion requiring removal in the ED.
Case Report
A 76-year-old female with hypertension and hyperlipidemia presented to the ED with a foreign body and pain in her left thigh. Prior to presentation, the patient had been fishing and caught a channel catfish. She was subsequently struck in the left lateral thigh upon reeling in the fish. The spine lodged in the patient's leg, causing immediate pain and later edema and erythema. The patient, unsuccessfully, attempted self-removal of the spine. She then presented to an urgent care center where wound irrigation and exploration were performed with another unsuccessful removal attempt. She presented to the ED 6 hours after the initial injury for further evaluation and management.
Her review of systems was negative. She had no fevers, rigors, nausea, vomiting, or paresthesias. Initial vital signs were pulse 61, blood pressure 228/109, respiratory rate 18, temperature 36.7, and pulse oximetry 97% on room air. Her physical exam demonstrated an open wound and a visible foreign body in the left lateral thigh. The wound was erythematous, edematous, and tender to palpation without evidence of purulent drainage or active bleeding from an arterial source. The patient had normal pulses in the foot and full strength with normal range of motion of her hip and knee. Plain radiographs of the femur demonstrated a 2 cm foreign body consistent with a catfish spine (Figure 1); 10 mL of lidocaine 1% without epinephrine, buffered with sodium bicarbonate 8.4% 10:1, was used to anesthetize the area. Utilizing a sterile technique, the wound was extended longitudinally by 0.5 cm on either side. This provided optimal visualization and facilitated the successful removal of the foreign body with Debakey forceps. The wound was irrigated with sterile water, and it was left open to heal by secondary intention (Figure 2). The patient tolerated the procedure well without any immediate complications. The spine was examined and found to be intact; therefore, postprocedure radiographs were not obtained.
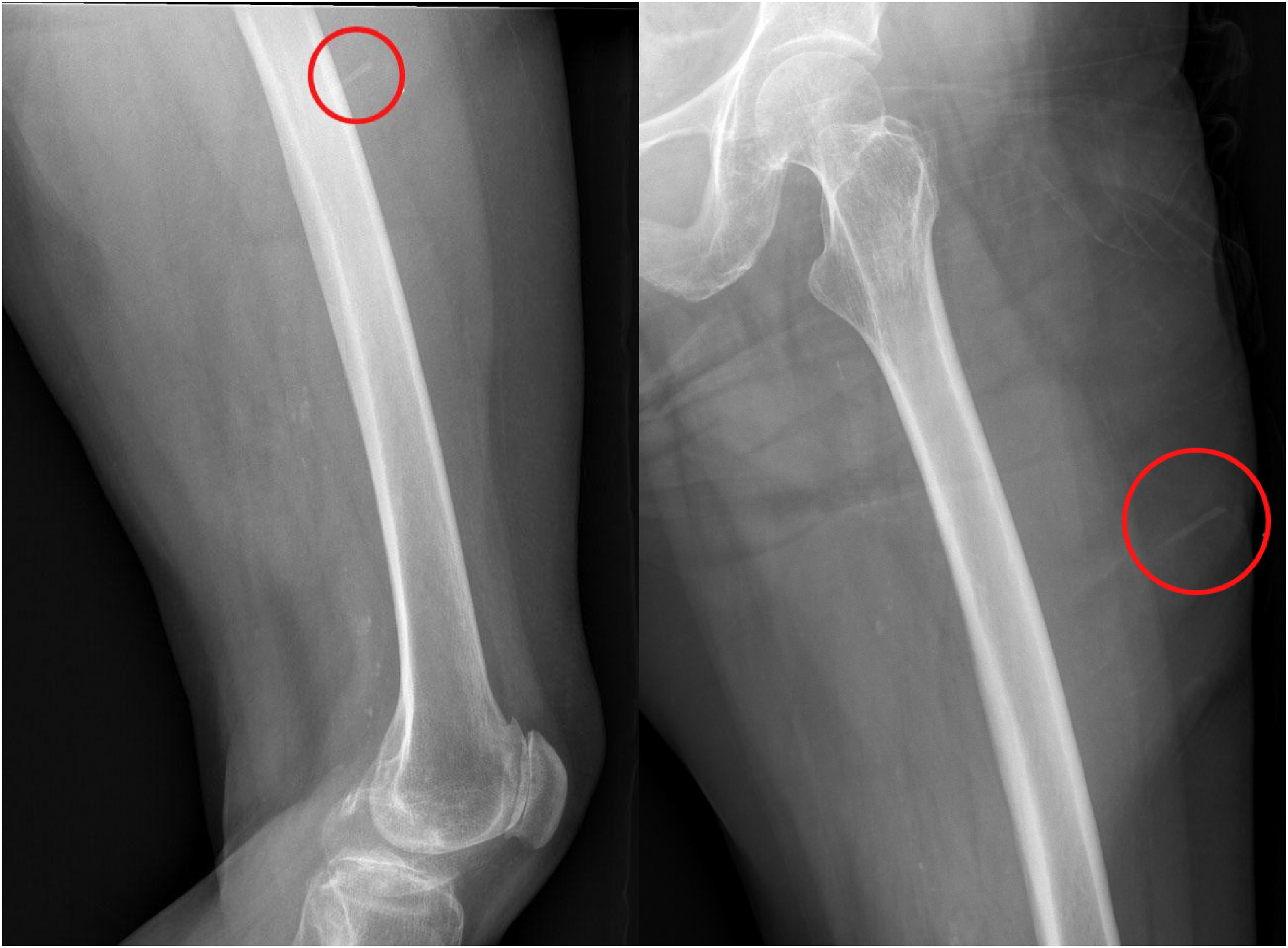
Postero-anterior and lateral X-rays of the left thigh. PA and lateral X-rays prior to catfish spine removal. Catfish spine is circled.
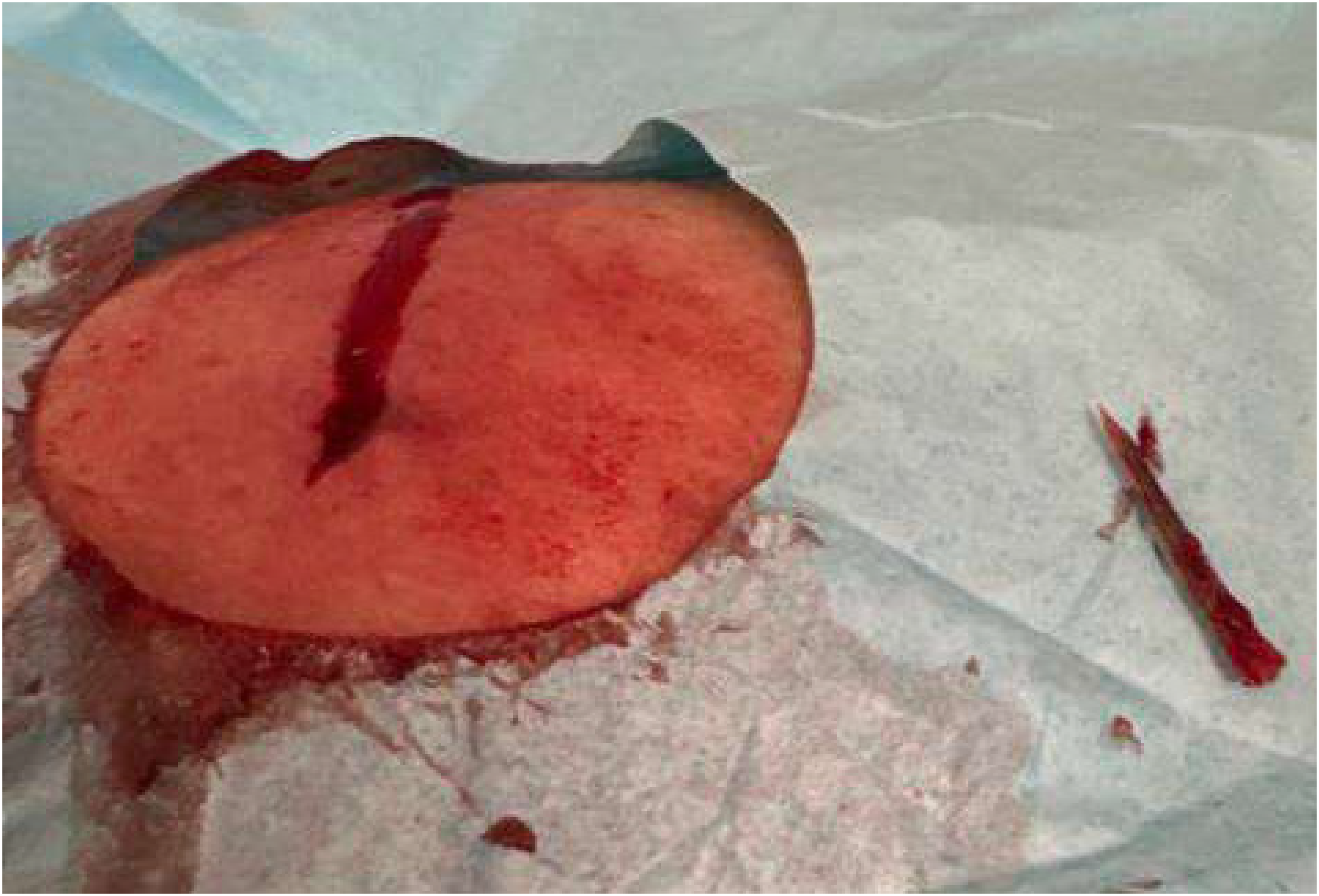
Post-excision specimen and left lateral thigh wound site. Image of the wound and catfish spine after removal.
Postprocedure care included updating her tetanus vaccine. The patient was prescribed levofloxacin 500 mg orally once daily for 10 days, and the wound was dressed with mupirocin ointment, sterile gauze, and paper tape. The patient was discharged in stable condition and instructed to follow up with her primary care provider and use acetaminophen and diphenhydramine for symptom control. Standard return precautions were discussed with the patient. She was contacted by the ED 11 days after discharge and reported feeling well, without any pain at the injury site.
Discussion of Implications for Clinical Practice
Catfish-related injuries are infrequent presentations in the ED. No consensus guidelines exist on the management of acute catfish injuries. Treatment is derived from case reports and expert opinion. Diagnosis of the extent of the injury is aided by a comprehensive history, physical exam, and X-ray imaging. Management should include spine removal, analgesia, and appropriate antibiotic coverage.
One modality of damage is direct trauma from the penetrating injury. Knowledge of the spine structure is essential to aid in the extraction of the foreign body and minimize tissue trauma. The spine, which has serrated and barbed edges, contributed to multiple prior attempts at removal in the patient described in this case report. 9 A good guideline for fishermen is not to forcibly remove the spine, as removal is greatly simplified by enlarging the entrance wound. However, this may not be possible in many cases, especially with larger fish or if the wound is unable to be safely enlarged on the scene. The anatomic location of the injury may determine whether to involve specialty physicians. Penetrating injuries to the face, hands, or feet may require surgical removal by a plastic surgeon. Most wounds can be left open to heal by secondary intention. Severe injuries may occur, with one case describing a penetrating injury to the myocardium of a fisherman resulting in death from myocardial rupture. 6 Patients may require inpatient admission for surgical drainage of a fluid collection, foreign body removal, or intravenous (IV) antibiotics. Consider a period of observation and IV antibiotics for those with injuries to high-risk locations or who are immunocompromised. One case report describes a patient with delayed presentation after spine penetration into his hand, resulting in multiple operations to clean out the wound site. 10 Damage from the initial injury may range from minor to severe but can be worsened by toxin-mediated effects.
Catfish venom is a second mechanism of tissue injury. The venom results in local tissue destruction by producing significant edema and pain secondary to its proteolytic and hemolytic effects. Typically, in the first few hours, the venom causes local pallor and may progress to cyanosis, but it is more commonly followed by local erythema and swelling. 10 The pain typically subsides 30 to 60 min after injection but can last upwards of 48 h. 4 Occasionally, local necrosis can be present. 11 Clinical presentation includes swelling of the involved extremity, a watery discharge from the puncture site, delay in wound healing, and local adenopathy, which have all been noted for weeks or even months in some cases. 11 There is no specific inpatient treatment other than supportive therapy. 6 Prior literature has advocated for therapeutic heat as this may inactivate heat-labile components of the venom and perhaps help to reverse local toxin-induced vasospasm. 4 One recommendation is to immerse the affected body part in non-scalding hot water between 45 and 50 °C (113 °F) for 30–90 min or apply warm compresses as the heat inactivates the toxin. 12 Additionally, injection of buffered lidocaine at the wound site may offer a reduction in pain and local tissue trauma compared to unbuffered lidocaine as the pH is raised to near-physiologic. The rise in pH is thought to neutralize the venom. 4 One percent lidocaine without epinephrine, buffered 10:1 with 8.4% sodium bicarbonate, was chosen for the patient described in this case report. Lidocaine without epinephrine was used, as the epinephrine may impede blood flow and, therefore, reduce toxin clearance.
Superimposed infection is the third mechanism of tissue damage. Antibiotic prophylaxis should be considered if the wound is of high infection risk, including deep wounds or those of the hands or feet. 4 The prophylactic antibiotic regimen should cover skin organisms, Staphylococcus and Streptococcus, and freshwater organisms, Aeromonas spp., Pseudomonas, and Vibrio. Empiric therapy against gram-negative rods is suggested, with ciprofloxacin being the single most popular and effective agent against freshwater and saltwater bacterial isolates. 9 For patients requiring initial inpatient therapy or having failed outpatient therapy, dual antibiotics are required. The recommendations are: (1) a tetracycline and a broad-spectrum beta-lactamase-stable beta-lactam antibiotic or (2) a tetracycline, beta-lactamase-stable penicillin and an aminoglycoside. 11 Delayed presentations can lead to chronic infection requiring long-term antibiotics, surgery, and chronic pain. 10 Additional risks from delayed presentation include sepsis or even death.6,10,13 For the patient described in this case report, levofloxacin was chosen for its broad-spectrum coverage and oral route of administration. Levofloxacin was chosen over ciprofloxacin for its 10 times higher tissue penetration and once-daily dosing. 8
There are several distinct points in the management of catfish spine injuries. Damage primarily occurs from 3 different mechanisms: direct trauma, toxin-mediated effects, and bacterial inoculation. Each of these mechanisms need to be addressed during the patient's visit. It is important for healthcare providers to understand the need for spine removal and potential damage to surrounding neurovascular structures, as specialists may need to be involved. Unique pain-control modalities are needed to mitigate the toxin's effects. This requires local infiltration with buffered lidocaine without epinephrine and hot water soaks to optimize toxin inactivation. Lastly, these injuries require copious irrigation and antibiotics to prevent long-term sequelae of infection. Clinicians should be aware that the level of evidence is expert opinions and case reports.
Footnotes
Author Contribution(s)
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
