Abstract
As the global population grows and access to remote environments expands, travel to high altitude destinations has become increasingly common, now attracting ∼100 million visitors annually. This trend coincides with a population that is increasingly medically complex, emphasizing the importance of understanding how preexisting medical conditions are influenced by ascent to high altitude. This narrative review summarizes the current evidence describing the physiologic and clinical implications of altitude exposure among individuals with chronic medical conditions. A comprehensive literature search was conducted across multiple databases and sources using inclusive keyword and phrase strategies related to high altitude and preexisting medical conditions. All relevant peer-reviewed studies, reviews, and consensus statements were reviewed to ensure a thorough synthesis of available data. The discussion is organized by body system, encompassing cardiovascular, pulmonary, neurologic, metabolic, hematologic, and other relevant conditions. Findings indicate that while many patients with stable, well-managed chronic illnesses can tolerate moderate or even high altitudes, those with advanced cardiopulmonary disease or cerebrovascular pathology face heightened risk and warrant individualized evaluation prior to ascent. This review provides practical, evidence-based guidance to clinicians, expedition planners, and emergency providers caring for high altitude travelers with preexisting conditions. Recommendations emphasize pretravel risk stratification, optimization of chronic disease control, and strategies to mitigate altitude-related complications, supporting safer and more informed participation in high altitude activities.
Keywords
Introduction
As the global population grows and infrastructure expands, access and visitation to wilderness environments continues to rise. This includes high altitude travel, which is growing in popularity, with now roughly 100 million visitors annually. Paired with a global population that is increasingly medically complex, understanding how preexisting medical conditions are impacted on ascent to high altitude is imperative. This narrative review synthesizes the current available evidence surrounding common medical conditions impacted by travel to high altitude and is organized by body system, addressing a range of pertinent diseases and underlying conditions. Furthermore, this review aims to equip clinicians, expedition providers, and rescuers with practical advice for those traveling to altitude with preexisting conditions.
General Approach to Patients Traveling to Altitude
Providers must understand the physiology of acclimatization to altitude, which will enable such providers to advise their patients about high altitude travel with preexisting conditions. Various physiologic changes occur in the body beginning minutes into and sometimes lasting weeks after high altitude exposure (Figure 1).
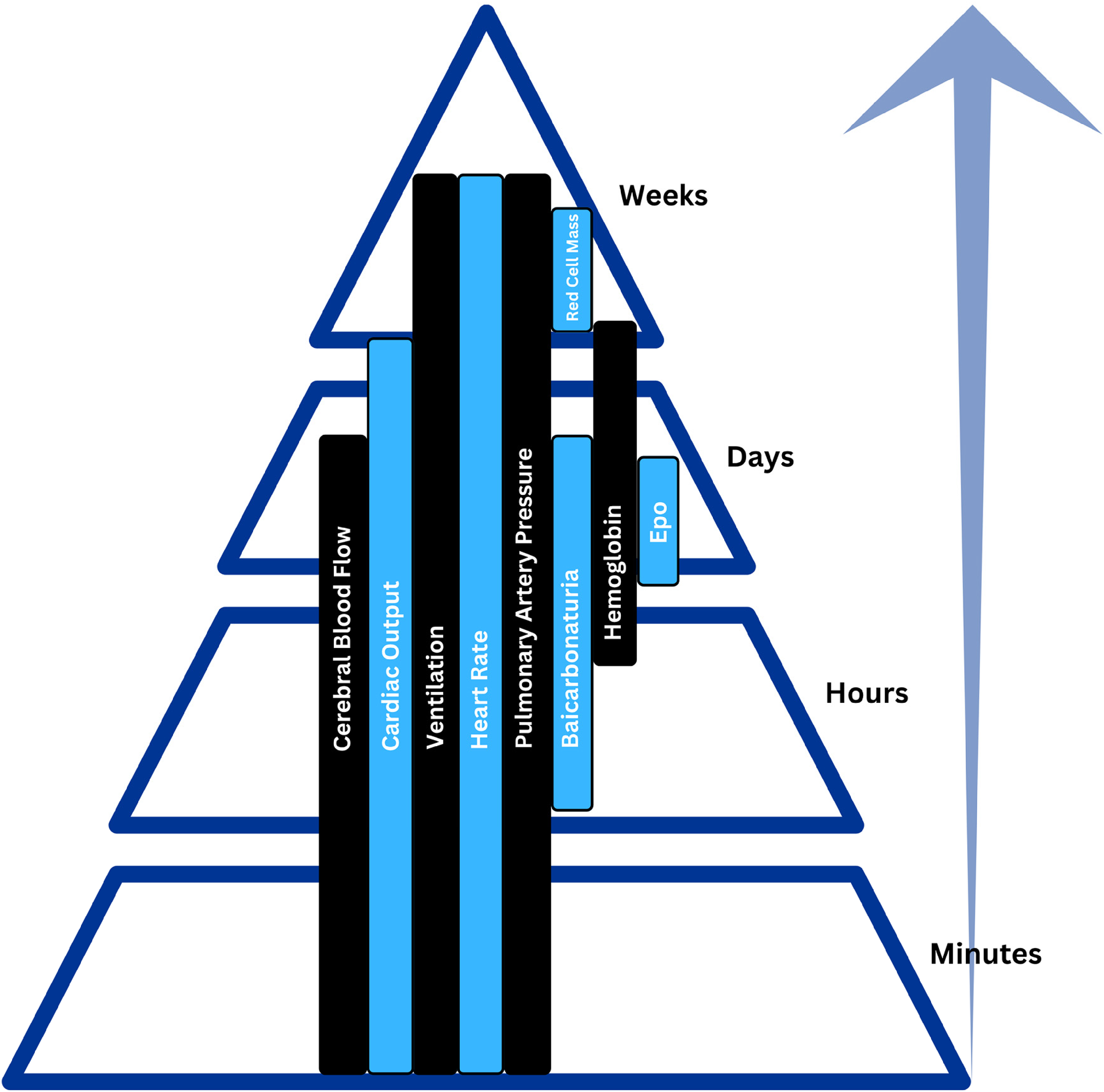
Physiologic changes occurring in the body that enable acclimatization begin minutes after exposure and sometimes last weeks after exposure to high altitude. Bars represent the peak physiologic effects. Modified from Luks and Hackett. 1
Rapid ascent incurs significant risk, particularly when flying directly to high altitude destinations. 2 Practitioners must be familiar with the planned terrain and acclimatization strategy and, in certain cases, must be ready to recommend a more conservative ascent profile tailored to the individual patient and associated preexisting medical conditions.
Clinicians will want to consider the following:
Is/are the patient's medical condition(s) stable before a planned trip to altitude? Might the condition predispose to altitude illness or be exacerbated by hypobaric hypoxia, the acclimatization process, or exercise or through the increase in ventilation (Table 1). If the answers to questions 1 and 2 are yes, what strategies will aid in ameliorating that impact and/or help mitigate risk of altitude illness?
General consideration when traveling to altitude with preexisting medical conditions.
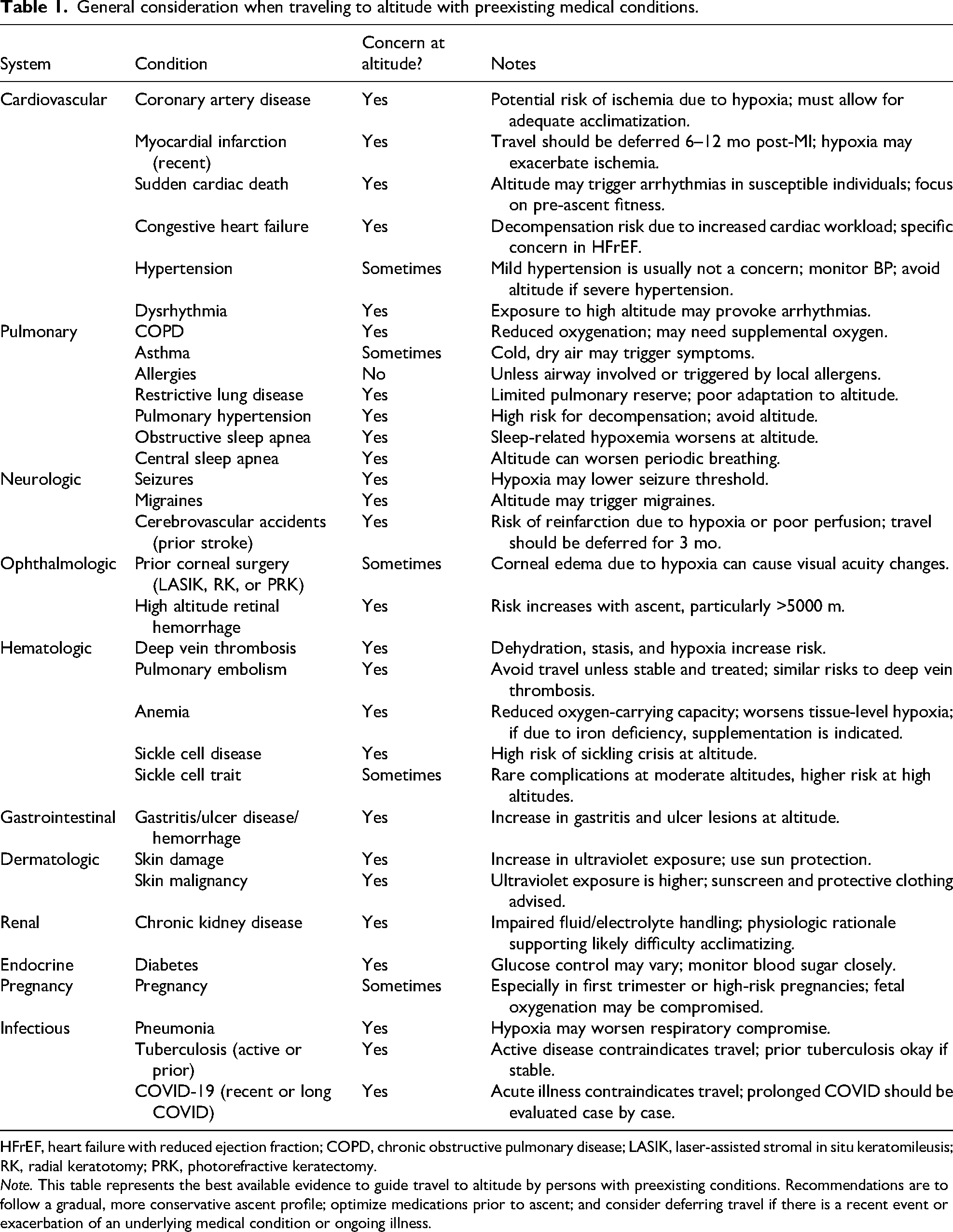
HFrEF, heart failure with reduced ejection fraction; COPD, chronic obstructive pulmonary disease; LASIK, laser-assisted stromal in situ keratomileusis; RK, radial keratotomy; PRK, photorefractive keratectomy.
Note. This table represents the best available evidence to guide travel to altitude by persons with preexisting conditions. Recommendations are to follow a gradual, more conservative ascent profile; optimize medications prior to ascent; and consider deferring travel if there is a recent event or exacerbation of an underlying medical condition or ongoing illness.
Clinicians advising their patients may find it beneficial to create a graph plotting sleeping altitude against days of ascent, which can be a valuable visual tool for identifying potential acclimatization challenges and risk of altitude illness. A detailed discussion of altitude illness is outside the scope of this article. Please refer to the “Wilderness Medical Society clinical practice guidelines for the prevention, diagnosis, and treatment of acute altitude illness: 2024 update.” 3
Additionally, recommending a preliminary exposure to moderate altitude—such as a visit to a local mountain/ski area—may provide a practical means of assessing an individual's tolerance to altitude prior to undertaking a more committing tour, trek, climb, or expedition.
Cardiovascular Disease
Cardiovascular disease (CVD) is increasingly common, with roughly 18 million affected individuals in the United States. 4 Ascent to high altitude (typically considered >2500 m) involves important considerations for those with CVD. Altitude-related hypobaric hypoxia induces chemoreceptor-mediated sympathoadrenal activity, triggering increases in heart rate, cardiac output, and myocardial oxygen demand paired with decreased overall maximal oxygen uptake.
Altitude travel can involve various additional stressors, including exposure to harsh environmental conditions with cold and thermal stress and possible dehydration (which may further drive sympathetic activation) as well as suboptimal dietary changes. 5 Thus, understanding how the high altitude environment impacts those with preexisting CVD, including coronary artery disease (CAD), prior myocardial infarction (MI), congestive heart failure, hypertension, and dysrhythmia, is important for clinicians providing guidance to and proper risk stratification for individuals planning high altitude travel. 4 This section examines the potential impact and considerations for high altitude travel in individuals with preexisting CVD.
Coronary Artery Disease
Given altitude-related physiologic changes, concern for both occult and manifest CAD warrant consideration. Altitude travel both lessens oxygen supply and increases myocardial oxygen demand. Hypoxia can cause paradoxical vasoconstriction in those with coronary atherosclerosis, 6 with the overall potential to worsen myocardial oxygen supply-demand mismatch and cause ischemia. Thus, at altitude, hypoxic stress and exercise have the potential to induce ischemia in individuals with CAD.
Although there is limited research or guidance on occult CAD at altitude, it is reasonable for individuals with good exercise tolerance (including absence of exercise-induced angina) to defer any pre-ascent screening. 7 Individuals with traditional risk factors for CAD and who do not perform exercise at low altitude should consider pre-ascent stress testing. Individuals with known CAD who are asymptomatic when exercising at sea level generally can tolerate moderate altitude exposure (up to 3000 m).
Allowing adequate time for acclimatization can potentially mitigate risk in those with CAD. Data suggest that in patients with CAD, acute ischemia may be provoked at modestly lower myocardial and systemic work rates, but this can be mitigated by allowing adequate time for acclimatization. 8 Levine et al found that the double-product (ie, peak systolic blood pressure × peak heart rate—used as a surrogate for myocardial oxygen requirement) necessary to cause 1 mm of ST depression on electrocardiogram (ECG) during exercise at 2500 m was 5% less when compared with sea level; however, this relationship disappeared after 5 d of acclimatization. 8 Additionally, in acclimatized individuals with CAD at 4200 m, exercise test echocardiography demonstrated no wall-motion abnormalities. 9 A 2021 scientific statement from the American Heart Association (AHA) recommended that individuals with known CAD should ensure adequate hydration, follow gradual and more conservative ascent profiles, and ensure CAD medication optimization prior to ascent. 4 Currently, there is no evidence to guide unstable disease, and thus, those with severe CAD, for example, unstable angina, should avoid travel to altitude. 10
Myocardial Infarction and Sudden Cardiac Death
Although limited data exist, outside of traditional risk factors including severe CAD, 8 altitude alone does not appear to be a risk factor for MI. 11 Given the described cardiovascular stressors imposed by the high altitude environment, physiologic rationale suggests that individuals with a recent MI should avoid altitude travel. A 2018 joint statement involving multiple cardiology and mountain medicine societies including the International Society of Mountain Medicine and the European Society of Cardiology (2018 European guidelines) recommended waiting 6 mo after an uncomplicated acute coronary syndrome revascularization and 6 to 12 mo after coronary stenting before travel to altitude. 12 Schmid et al in 2005 examined 22 patients during a rapid ascent to 3454 m 6 to 18 mo after either ST-segment elevation MI or non-ST-segment elevation MI (all patients had undergone either percutaneous angioplasty or coronary artery bypass). The authors reported no significant adverse events, including ECG abnormalities, ischemia, or arrhythmias, during exercise. 13
Sudden cardiac death (SCD) can be observed at high altitude, although direct linkage to altitude exposure or precise incidence is unclear. 14 Data demonstrate that roughly 50% of SCDs occur during the first day of high altitude exposure. 14 Additional risk factors include dehydration and caloric depletion as well as prior MI, CAD, hyperlipidemia, diabetes, and inexperience with exercise at altitude. 15 However, the most important risk factor remains strenuous physical activity on the first day of altitude exposure. For males older than 34 y, those with history of CAD and/or prior MI, and those unaccustomed to physical activity at altitude, sleeping at moderate altitude before exercising at altitude may reduce the risk of SCD. 16 Pre-ascent fitness preparation is associated with a significant decrease in the risk of SCD at high altitude. 15
Congestive Heart Failure
Many physiologic adaptations at high altitude are potentially harmful for individuals with heart failure, including increased sympathetic tone (with a resulting increased heart rate), increased systemic and pulmonary blood pressure, and potential volume dysregulation.17,18 Currently, there is no significant evidence surrounding heart failure with preserved ejection fraction and altitude exposure, 4 with investigation focusing primarily on heart failure with reduced ejection fraction. Despite the theoretical risks of altitude exposure, limited data fail to demonstrate significant adverse effects of altitude for patients with heart failure.19,20 For example, in 2015, Schmid et al examined individuals with ejection fractions of <40% with New York Heart Association (NYHA) functional class I and II heart failure with reduced ejection fraction with rapid ascent to 3454 m and demonstrated a decrease in exercise capacity of ∼7.4% per 1000 m of ascent, similar to the expected drop for healthy individuals, 21 with overall good tolerability. 20 Despite this, and perhaps relying largely on physiologic rationale, the 2018 European guidelines recommended that stable NHYA class I and II patients avoid heavy physical activity at altitude, stable NYHA class III patients should not exceed light activity, and NHYA class IV patients should avoid high altitude exposure. 12
Travel to altitude may have important pharmacologic implications for individuals with heart failure. Individuals with heart failure on diuretic medications should use caution when initiating acetazolamide for acute mountain sickness (AMS) prophylaxis or treatment given the risk of hypokalemia and over diuresis. 4 Use of nonselective ß-blockers such as carvedilol may lead to reduced hyperventilation at altitude, possibly limiting normal physiologic adaptations to the high altitude environment. 22 Although data are limited, given these considerations, individuals with heart failure should discuss therapeutic considerations with their provider managing their heart failure regimen prior to travel to altitude.
Hypertension
The data suggest that there are brief and significant increases in blood pressure at high altitudes; however, observed changes in blood pressure on ascent to altitude are mixed,23–25 including in individuals with a personal history of hypertension. 24 The changes in blood pressure during ascent to altitude do not appear to be generalized or associated with complications such as AMS or end-organ dysfunction. This includes conditions such as retinopathy, intracranial hemorrhage, and MI. Although blood pressure may spike temporarily, it does not correlate with serious adverse health outcomes when traveling at altitude.11,26 Despite these data, the AHA recommends ensuring adequate blood pressure control prior to ascent as well as considering augmented therapy for those with sustained blood pressure values of >180/110 mm Hg, particularly for persons with preexisting CVD. 4 The 2018 European guidelines recommended periodic checking of blood pressure during altitude travel for individuals with moderate to severe hypertension and avoiding high altitude exposure for individuals with uncontrolled or severe hypertension to prevent end-organ damage. 12
Dysrhythmia
Many of the normal physiologic adaptations induced by exposure to the hypobaric hypoxia at altitude may trigger an underlying cardiac dysrhythmia. One hypothesis is that the hypoxia-mediated sympathetic increases at altitude theoretically pose an increased risk of cardiac dysrhythmias, but data are limited. Previous literature suggested a lower risk of dysrhythmia at simulated high altitude in healthy individuals, 27 but a recent prospective cohort study on Mount Everest demonstrated a roughly 38% incidence of new dysrhythmias (including tachy- and bradydysrhythmias) in otherwise healthy climbers without a previous history of dysrhythmia. 28 Another study investigated the risk of dysrhythmia in individuals with a known history of dysrhythmia using ECG analysis and 14-h ambulatory ECG on exposure to altitudes of 4500 to 5056 m and found 1 isolated incidence of an asymptomatic congenital preexcitation syndrome (Wolf-Parkinson-White). 26 The scarcity of literature on this topic prohibits evidence-based recommendations or guidance on risk stratification. However, the AHA recommends caution for individuals traveling to altitude with uncontrolled dysrhythmias at sea level. In addition, the AHA recommends that individuals with a known dysrhythmia on warfarin should consult their physician to discuss alternative options because it is well known that diet, travel, and intercurrent illness all can impact international normalized ratios (INRs). Additionally, limited data suggest that high altitude may impact INR in stable warfarin dosing. 29
Pulmonary Disease
Chronic Obstructive Pulmonary Disease at Altitude
High altitude conditions can create significant challenges for individuals suffering from chronic obstructive pulmonary disease (COPD). Lower partial pressure of oxygen results from increases in elevation, causing a decline in arterial oxygen saturation in all individuals. Patients with COPD develop increased airway resistance and parenchymal loss of lung tissue, both of which contribute to compromised lung function and impaired capacity for gas exchange.30,31 Therefore, patients with COPD will experience greater hypoxemia and lower oxygen saturations than their healthy counterparts. This hypoxemia, both at rest and with exertion, significantly predisposes individuals to altitude illness. 32 Decreases in ambient barometric pressure at altitude and subsequent alveolar hypoxia may lead to worsening airflow obstruction and decreased FEV1, but this finding has not been consistently found across all studies.32–36 In addition to the primary mechanism of alveolar hypoxia, lower oxygen saturations can stimulate sympathetic tone and hypoxic pulmonary vasoconstriction, subsequently exacerbating pulmonary hypertension, a condition that is often present in more advanced stages of COPD.32,37 The risk of COPD-associated rupture of lung blebs does not appear to be increased at altitude. 32
Individuals with COPD must prepare and use altitude acclimatization strategies when traveling to high altitude locations. They also may require supplemental oxygen at lower elevations compared with individuals without COPD when traveling to altitude.32,38 Portable pulse oximeter monitors may guide the use of supplemental oxygen in these situations, and previously prescribed inhalers and steroids should be continued when traveling to altitude. Additionally, nifedipine therapy blunts the effects of hypoxic pulmonary vasoconstriction and should be considered. 32 Travel to moderate altitude appears safe in patients with COPD who avoid excessive exertion, although caution is recommended. Caution should be taken with patients traveling to very high altitudes (>3048 m) because data are lacking for this patient group above this elevation.
Asthma at Altitude
Despite the extensive variety of asthma triggers, high altitude travel is considered safe for individuals with asthma.38,39 High altitude therapy has been used as a treatment for asthma for years, and evidence shows beneficial effects of altitude on reduced asthma symptoms, improved pulmonary function, and reduced corticosteroid requirements. 39 Individuals with asthma have fewer medical exacerbations and an overall decreased mortality at altitude, an effect thought to be due to decreased allergens, lower levels of air pollen and pollution, decreased air viscosity and resulting improved flow, and increased ultraviolet light.39,40 Additionally, the incidence of AMS is not higher in individuals with asthma when compared with the general population, except for 1 study demonstrating a slight increase above 6400 m. 38
Asthma exacerbations are frequently triggered by certain environmental allergens, and early-onset disease is thought to be related to allergic inflammation. 41 Fortunately, the high altitude environment contains fewer allergens. Although certain allergens, such as pine tree pollen, are more common at altitude, others, such as dust mites, are less common.41,42
Individuals with asthma traveling to higher elevations should continue their usual medications and carry a rescue supply of bronchodilators and steroids. Remote areas may necessitate reserve quantities of medications. Individuals with asthma triggered by cold or dry air should be mindful that these environmental conditions exist in the high altitude environment and take steps to prevent symptom exacerbations (including keeping inhaled medications warm). Patients with known allergic triggers should carry antihistamines. 43 Acetazolamide appears to prevent AMS in patients with asthma as effectively as in healthy individuals.39,44
Restrictive Lung Disease at Altitude
Unlike obstructive lung diseases (ie, asthma and COPD), restrictive lung diseases affect the lung tissue's ability to expand fully during inhalation. Few data exist assessing the risk of altitude exposure in this broad category of illnesses, but 1 study demonstrated a significant decrease in arterial oxygenation with exercise at simulated moderate elevation (2438 m).32,45 Decreased ventilatory capacity may impact acclimatization, but no studies provide insight into which patients with restrictive lung disease are vulnerable to high altitude illness. 32 Those with restrictive lung disease may be susceptible to developing high altitude pulmonary edema (HAPE) because many of these patients develop pulmonary hypertension. 32
Extreme caution should be advised for any patient with restrictive lung disease considering travel to high altitude. If high altitude travel is unavoidable, supplemental oxygenation should be provided because it has been shown to reduce the exaggerated hypoxemia these patients may experience. 45 Prophylactic nifedipine (30 mg sustained release [SR] twice daily) or phosphodiesterase-5 (PDE-5) inhibitors (tadalafil 10 mg every 12 h or sildenafil 50 mg every 8 h) should be considered for HAPE prophylaxis.32,37
Pulmonary Hypertension at Altitude
Pulmonary hypertension is a relative contraindication to high altitude travel, but the data are scarce and ambiguous. A recent study of 27 patients with Class I/II pulmonary vascular disease (defined as pulmonary artery hypertension or distal chronic thromboembolic pulmonary hypertension) concluded that these patients, when traveling to 2500 m, tolerated the 30-h sojourn, but approximately half experienced severe nocturnal hypoxemia and about a third developed AMS. 46 If travel to high altitude is unavoidable, given the elevated risk of HAPE, these patients may benefit from calcium channel blockers or PDE-5 inhibitor, especially if they are not already taking a scheduled pulmonary vasodilator. 37 Low-flow oxygen, prophylactic nifedipine (30 mg SR twice daily), or PDE-5 inhibitors (tadalafil 10 mg every 12 h or sildenafil 50 mg every 8 h) should be strongly considered.32,37
Sleep Apnea
Obstructive Sleep Apnea at Altitude
Obstructive sleep apnea (OSA) is a sleep disorder characterized by repeated interruptions in breathing during sleep due to the relaxation of throat muscles, leading to temporary airway blockage, which can result in disrupted sleep and hypoxemia. OSA is highly prevalent in the adult population, and prevalence rises with advancing age. At moderate to high elevations, hypobaric hypoxia promotes periodic breathing and, when combined with OSA, causes compounded, intermittent, and sustained hypoxemia. 47 This hypoxemia may worsen the downstream effects of OSA, such as hypertension and increased risk of cardiovascular events. 47 Continuous positive airway pressure (CPAP) machines are the mainstay of OSA treatment, and although performance of these devices can be inconsistent at altitude, CPAP therapy (auto CPAP) is effective and recommended.48,49
Central Sleep Apnea at Altitude
Central sleep apnea (CSA), characterized by intermittent respiratory cessation or decreased ventilatory effort, can occur in otherwise healthy individuals at elevations >2000 m, with prevalence rising with increases in altitude. 50 CSA may be caused by certain health conditions, respiration-suppressing medications such as opioids, or prior stroke. 51 Similar to OSA, these apneic events lead to intermittent and prolonged periods of hypoxemia, particularly at altitude.50,51
Sleep-disordered breathing, resulting from OSA, CSA, or a combination of both, leads to increased hypoxemia and may increase the risk of developing altitude-related illness. Patients with OSA at low elevations experience a decrease in OSA severity but increased CSA events at altitude. 47 Patients who use CPAP should continue to do so while sleeping at altitude. 47 CPAP alone will not effectively mitigate CSA episodes, so combined treatment with acetazolamide and CPAP should be considered, because acetazolamide can decrease periodic breathing episodes.47,50 Additionally, supplemental oxygen may be considered in combination with CPAP in patients with known cardiopulmonary disease by preventing hypoxemia. 47 Mandibular advancement devices or acetazolamide monotherapy also may be effective when electric or battery power is not available.47,50
Neurologic Disease
Seizures
Cases of breakthrough seizures occurring at altitude in individuals with well-controlled seizures are rare, though reported. 52 Although both the association and mechanisms are unclear, sleep deprivation, hypoxic ventilatory response related hyperventilation, and hypoxia may be inciting factors. 53 Seizures have rarely been reported in cases of high altitude cerebral edema. 53 Individuals with known seizure disorders should ensure the their seizures are well controlled prior to ascent. Topiramate use when combined with acetazolamide may worsen metabolic acidosis and increase the risk of nephrolithiasis; thus, alternative medications (eg, dexamethasone) should be considered in these individuals for AMS chemoprophylaxis.54,55
Migraines
While headache is a common occurrence at altitude, exposure to altitude likely increases the risk of acute migraine. 56 AMS and high altitude headache share key features with migraine headache, including throbbing quality, aggravation with activity, and gastrointestinal distress.57,58 Proposed AMS and migraine pathophysiologies are also similar, including trigeminovascular activation, cerebral vasodilation, and increased cerebral blood flow, with meningeal inflammation.58,59 Thus, elucidating the difference between acute migraine and altitude illness can be challenging 60 and likely confounds the true risk of acute migraine at altitude. Patients with migraine should, in consultation with their physician, carry abortive medications when traveling to altitude.
Cerebrovascular Accident
Data surrounding individuals with a history of prior cerebrovascular accident traveling to altitude are limited to observational studies, case reports, and expert consensus statements. Cerebrovascular accidents have occurred at altitude, including in individuals without known significant risk factors. 61 Although some studies suggest that high altitude exposure may increase the risk of thromboembolic disease, 62 data are overall lacking and inconclusive.63,64 Despite this, the 2018 European guidelines recommended that individuals should avoid high altitude travel for 3 mo following a cerebrovascular accident or transient ischemic attack, and those at risk or with a history of either should never travel alone and follow a low-risk ascent profile. 12
Ophthalmologic Disease
Altitude and the Eye
At high altitudes, lack of humidity, increased ultraviolet radiation, cold temperatures, hypoxia, and reduced atmospheric pressure can lead to ocular complications for both healthy individuals and those with preexisting ocular disease.65,66 The cornea is avascular, absorbing oxygen directly from the atmosphere or via the aqueous humor, and thus may become hypoxic in these conditions, impairing its function. Additionally, individuals with a history of intraocular gas bubbles should avoid high altitudes because the decreasing atmospheric pressure can cause these bubbles to expand. Patients with previous eye surgeries or existing ocular conditions are advised to consult their ophthalmologist before traveling to high altitudes to assess any risks associated with their specific circumstances.65,66
Altitude Exposure After Corneal Surgeries
High altitude-related hypoxia can lead to corneal edema and thickening. Although this thickening usually does not affect vision in healthy eyes, it can be problematic for those who have undergone radial keratotomy (RK), laser-assisted stromal in situ keratomileusis (LASIK), or photorefractive keratectomy (PRK).67,68
In RK, incisions weaken corneal stability, and the edema from hypoxia can cause the cornea to flatten, resulting in increased far-sightedness and decreased visual acuity. 67 The extent of vision changes can vary based on the amount of residual myopia at sea level, making predictions difficult. Most changes typically resolve on return to normal altitudes, but patients with RK should consider bringing various levels of corrective lenses during their trip. A practical option could be wearing glasses under goggles and having multiple pairs of glasses available. Ideally, having prescription goggles with differing levels of correction would be beneficial in case of significant visual changes.
For patients having undergone LASIK or PRK, the impact of altitude on vision is generally less pronounced. Studies show mixed results, with some indicating no change in visual acuity and others showing minor blurring. A recent study of climbers with LASIK-treated eyes reported no significant visual changes, although they did report dry eye symptoms, a known complication of LASIK, which still can occur and may be worse at high altitudes.69,70 Consultation with an ophthalmologist is crucial for obtaining the right eyewear and understanding personal risk before traveling to high altitude.
High Altitude Retinal Hemorrhage
At high altitudes, increased retinal blood flow and subsequent dilation of retinal veins can lead to retinal hemorrhages, a phenomenon documented since the 1970s. The prevalence of these high altitude-associated retinal hemorrhages among climbers varies widely, with reported rates ranging from 0 to 79%, and increases with higher elevations.71–73 Most retinal hemorrhages do not affect vision unless they involve the macula. If no visual disturbances are present, patients with retinal hemorrhages can continue their ascent, but if vision changes are present, patients must descend immediately to seek further expert evaluation. 71 It is important to note that the presence of retinal hemorrhages is associated with altitude illness, but the relationship is unclear. 65 The occurrence of retinal hemorrhages should prompt healthcare providers to consider the potential development of other altitude-related complications. 65 Monitoring and addressing symptoms promptly can help ensure the safety and well-being of those at high altitudes. 73
Hematologic Disease
Deep Venous Thrombosis, Venous Thromboembolism, and Pulmonary Embolism
Exposure to high altitude conditions is associated with a substantially elevated risk of deep vein thrombosis (DVT) and venous thromboembolism (VTE)/pulmonary embolism (PE).74–76 This is likely multifactorial, and factors such as dehydration, reduced mobility, extended travel, and prolonged periods of hypoxia all likely contribute to the increased risk.76–80 In general, risk factors for DVT/VTE/PE are similar at any altitude and include immobilization or decreased mobility, surgery, trauma, cancer, inherited clotting disorders, pregnancy, hormone-replacement therapy, and oral contraceptive use. PE may result in symptoms of shortness of breath, hemoptysis, chest pain, elevated heart rate, and syncope or sudden death. Many of these symptoms, especially shortness of breath and elevated heart rate, are experienced by individuals with other altitude-related conditions, complicating the diagnosis of PE/VTE at altitude.
Preventive strategies for those at high risk for DVT/VTE/PE include maintaining adequate hydration, avoiding prolonged immobility, using compression stockings, and considering prophylactic antiplatelet or anticoagulation therapy. Individuals undergoing treatment for VTE/PE should reconsider high altitude travel.76–80
The treatment of DVT/VTE/PE consists of anticoagulation or, in severe cases, thrombolytic therapy. People taking warfarin should be counseled that high altitude, dehydration, illness, dietary changes, and other medication interactions can alter INR levels and lead to increased clotting or bleeding. 81 Direct oral anticoagulants (DOACs), according to the US Food and Drug Administration, are less affected by diet and are thought to have fewer drug-drug interactions. Patients on DOACs should maintain adequate hydration because dehydration can increase plasma concentrations of DOACs and may lead to bleeding. 82
Anemia
Anemia during altitude travel, regardless of the etiology, results in greater dyspnea and reduced exercise performance; with every 1% decrease in serum hematocrit, expected V(dot)O2 max decreases by 1% (and measured endurance by 2%).83–85 Iron supplementation may have a role in improving symptomatic anemia depending on its etiology. Additional caveats exist for sickle cell disease/trait, which will be discussed in subsequent sections.
Anemia at Altitude/Iron Supplementation
Iron supplementation may be beneficial in multiple types of anemia, such as blood loss, renal disease, heavy menstrual bleeding, inflammatory bowel disease, bariatric surgery, and some genetic disorders. 86 Additionally, individuals with nonanemic iron deficiency also may benefit from iron supplementation, which is recommended when ferritin levels fall below 50 micrograms·L–1. 87 Physician awareness of the underlying source and severity of anemia is critical and can help guide appropriate therapy to be initiated well in advance of travel. Supplementation may be provided prior to high altitude exposure via either oral or intravenous methods. If iron supplementation or transfusion is warranted, this can improve exercise tolerance and decrease the likelihood of altitude-related illness (such as AMS).86,88 Supplemental iron, particularly when provided by the oral route, may precipitate gastritis, a common high altitude condition. 89 Physicians should be mindful of the potential side effects of gastritis, upper gastrointestinal bleeding, constipation, and black stools, particularly when providing oral iron supplementation in the high altitude environment.
Sickle Cell Disease at Altitude
Hypoxia related to altitude significantly increases the risk of pain crises in sickle cell disease (SCD), because travel to even modestly hypoxic conditions can cause a pain crises.90,91 Hypoxemia promotes sickling through polymerization of hemoglobin S, creating long, insoluble chains of hemoglobin, and therefore, lower oxygen tension leads to more pain at altitude through more frequent red blood cell sickling. 92 Visitors with SCD to Colorado at moderate elevations >2000 m have a 20% likelihood of pain crisis, with the risk rising proportionally to further increases in altitude.91,93 Additionally, the cold and windy conditions at altitude further increase the risk of sickling. 94 Travelers with SCD exposed to short periods of hypoxia may develop symptoms (eg, aircraft pressurized to an altitude of 2500 m). 91
Consequently, individuals diagnosed with SCD should be advised against traveling to high altitudes. When exposed to temporary periods of hypoxia (ie, plane rides) or when altitude travel is unavoidable, supplemental oxygen should be provided. 92 Gradual conditioning and exercise may decrease the likelihood of pain crises developing with travel to altitude. 94 Additionally, clinicians should be mindful that these patients are functionally asplenic; therefore, appropriate vaccinations and precautions should be initiated prior to any travel. 92
Sickle Cell Trait at Altitude
Most individuals diagnosed with sickle cell trait (SCT) may travel safely to moderate altitudes. However, there are numerous case reports of observed splenic infarctions in this population. 95 Because SCT is common in several ethnicities, the possibility of splenic infarct may be present in certain individuals exposed to high altitude and presenting with left upper-quadrant pain without a known diagnosis of SCT. 92 Additionally, dehydration and strenuous physical activity may precipitate sickling in individuals with SCT.
Individuals with SCT may travel safely to moderate elevations, but increased caution and surveillance for symptoms of splenic infarct are warranted. Descent from moderate elevation should be recommended for any individual with SCT with left upper-quadrant pain if splenic infarct cannot be sufficiently excluded. 92 Patients with SCT also should be advised to be aware of muscle cramps and to stop their activities if symptoms develop. 92
Gastrointestinal Disease
Gastrointestinal Ulcer Disease/Hemorrhage
Gastrointestinal (GI) disturbances are common at high altitude and are often a part of the AMS syndrome. 96 Other GI diseases are reported on ascent to altitude, including peptic ulcer disease 97 and GI bleeding (with increased risk of GI bleeding with elevation gain). 98 A 2019 study conducted on 25 healthy mountaineers involved esophagogastroduodenoscopy pre-ascent and at altitude and found a significant increase in the frequency of endoscopic lesions and ulcer disease. 97 The relationship between altitude travel and GI pathology is unclear, although exposure to hypoxia may lead to increased stomach acid production and disrupt intestinal mucosal layers, immune function, and microbiota—all possibly compounded with physical exertion-related intestinal injury. 99 Although nonsteroidal anti-inflammatory drugs are implicated in GI hemorrhage, their use at altitude and its direct link to GI disturbance has not been well studied. 99 Additionally, the impact of acetazolamide use on the GI system at altitude is not well understood, although its side effects are known to include nausea, vomiting, and abdominal pain. 99 Individuals ascending to altitude with a known history of peptic ulcer disease or GI bleeding should be cautious using agents known to increase bleeding (eg, alcohol, anticoagulants, and nonsteroidal anti-inflammatory drugs).
Dermatologic Disease
Skin Damage and Malignancy
High altitude dermatologic pathophysiology is driven primarily by abiotic factors such as decreased humidity, increased ultraviolent radiation, and elevated wind speed. 100 These harsh environments predispose individuals to skin desiccation—leading to xerosis, which can manifest as flaking, scaling, and pruritus. While primarily more bothersome than hazardous, xerosis increases the susceptibility for skin infections and should be treated with lotions, moisturizers, or other emollients. 100 The far more insidious result of high altitude exposure stems from the oncologic properties of ultraviolet radiation. One study found that exposure to ultraviolet light increased by 11 to 19% per 1000 m of residential elevation gained. 101 In the acute phase, solar radiation causes sunburn, melanogenesis, and local immunosuppression. 101 Chronic exposure leads to photocarcinogenesis in sun-exposed areas such as the upper lip, limbs, shoulders, ears, and nose. 102 Nonmelanomatous skin cancer (ie, basal and squamous cell carcinomas) is positively correlated with cumulative ultraviolet radiation exposure, whereas melanoma is associated with adolescent skin exposure. 103 Preventative measures such as sunscreen and ultraviolet-blocking garments are paramount in high elevation environments. 104
Renal Disease
Chronic Kidney Disease and High Altitude Renal Syndrome
Currently, our understanding of the impact of high altitude on individuals with chronic kidney disease (CKD) is limited, 105 although data have suggested that prolonged altitude exposure may be associated with an increase in renal disease. 106 Prolonged exposure to high altitude can lead to polycythemia, hyperuricemia, and resulting systemic hypertension, which collectively are referred to as high altitude renal syndrome. 107
In CKD, limited evidence has demonstrated increased weight gain between dialysis sessions on ascent to altitude of 2000 m. 108 How CKD impacts risk of altitude illness is unknown. Expert opinion has postulated that the typical metabolic acidosis of CKD theoretically may serve to protect against AMS by increasing ventilation, 105 although no studies have formally investigated this relationship. However, given the significant prevalence of pulmonary hypertension in individuals with CKD, 109 those with CKD may be at increased risk of HAPE. 105 Dosing considerations for those with CKD are important. For acetazolamide, the current recommendation for individuals with glomerular filtration rates (GFRs) between 10 and 50 mL·min–1 include limiting dosing to every 12 h and avoiding use in individuals with a GFR of <10 mL·min–1. 105 For tadalafil, in individuals with a GFR of <30 mL·min–1, the recommendation involves decreasing tadalafil use for HAPE prophylaxis or treatment to no more than 5 mg once daily. For sildenafil, in individuals with a GFR of <30 mL·min–1, the recommendation is to decrease sildenafil use for HAPE prophylaxis or treatment to 25 mg 3 times a day. 105
Endocrine Disease
Diabetes at Altitude
Travel to high altitude in individuals with diabetes is common,110,111 and limited evidence suggests that diabetes is not a risk factor for the development of AMS. 112 Insulin regulation is poorly studied among individuals with diabetes at high altitudes, but the lability of blood glucose levels in these environments is well documented. 113 Previous studies have found that hemoglobin A1C increases for both diabetics (on insulin) and nondiabetics after high altitude expeditions, illustrating the negative impact of altitude on glycemic control. 110 When venturing to high altitudes, individuals with diabetes are often subjected to reduced food intake, increased aerobic/anaerobic exercise, loss of appetite, and increased caloric needs. 112 Some data indicate that factors such as increased catecholamines, cortisol, and sympathetic activity increase acute insulin needs at high altitudes. Due to the individualistic nature of glucose regulation, it is important for those who are insulin dependent to understand the factors impacting their personal glucose requirements before traveling to these areas. Individuals with diabetes also need to be cognizant of other risks, such as the overlapping symptomatology of diabetic ketoacidosis and AMS as well as temperature/oxygen-related effects on glucometers, glucose sensors, insulin pumps, and hypoglycemic medications when traveling to austere environments.112,114
Altitude-related hypoxia incurs presumed increased risk of poor wound healing in individuals with diabetes, and these individuals should check their extremities frequently for wound formation and ensure proper care for existing wounds. Individuals with diabetes and diabetic retinopathy who travel to high altitude do not increase their risk of high altitude retinal hemorrhage, although baseline diabetic retinopathy is currently thought to be a relative contraindication for high altitude travel. 115
Pregnancy
Pregnancy induces a number of physiologic changes at sea level, including increases in ventilation and tidal volume, oxygen consumption, cardiac output, and plasma volume expansion with decreases in blood pressure. 116 Retrospective data demonstrate that women who are pregnant have commonly traveled to high altitude. 117 Evidence suggests that high altitude residence attenuates observed cardiovascular changes in pregnancy, 118 although it results in an absolute increase in minute ventilation. 119 High altitude residence is associated with an increased incidence of lower birth weight as well as increased rates of gestational hypertension and preeclampsia.120,121 However, no significant data exist regarding physiologic changes and risk of altitude illness in women who are pregnant ascending rapidly to high altitude; thus, recommendations for altitude travel are largely based on expert opinion.116,122,123
Recommended contraindications for high altitude travel involve maternal heart or lung disease, chronic hypertension (or factors that increase the risk of preeclampsia), preeclampsia, placental function impairment, intrauterine growth restriction, and history of VTE, anemia, and smoking. 116 During the first trimester, individuals at higher risk of spontaneous abortion should avoid high altitude travel. 116 Additionally, individuals should confirm the intrauterine location of pregnancy to alleviate potential risks of traveling with an ectopic pregnancy. 116 For individuals in their second trimester, altitude travel should be avoided in those with increased risk of preeclampsia (including advanced maternal age, nulliparity, history of preeclampsia, family history of preeclampsia, multiple pregnancy, diabetes, hypertension, renal disease, autoimmune disease, antiphospholipid syndrome, and elevated body mass index). 116 Individuals who are pregnant and are considering chemoprophylaxis or therapeutics for altitude illness should be counseled that acetazolamide, dexamethasone, nifedipine, and salmeterol are classified as pregnancy Category C (animal studies have shown an adverse effect on the fetus but there have been no adequate and well-controlled studies in humans). In contrast, tadalafil and sildenafil are Category B (animal studies have demonstrated a fetal risk, but there are no well-controlled studies in humans or animals that have shown an adverse effect, but that effect was not confirmed in human studies). 124
Infectious Disease
Pulmonary infections can impair oxygenation at high altitude by altering pulmonary mechanics and disrupting gas exchange. This may predispose affected individuals to altitude-related illnesses. Additionally, the hypobaric hypoxic environment at altitude may weaken the immune system, potentially leading to clinical deterioration in individuals with pulmonary infections.
Pneumonia
Respiratory tract infections are a known risk factor for altitude-related illness, including HAPE. 125 The hypoxic environment associated with high altitude can impair immune system and respiratory function, leading to increased susceptibility to community acquired pneumonia, caused most frequently by Mycoplasma pneumoniae, Streptococcus pneumoniae, and Hemophilus influenzae. 126 Pulmonary infections may decrease alveolar ventilation and thus impact the partial pressure of oxygen, causing hypoxemia and increased morbidity when at altitude.127,128 Although limited datasets exist comparing outcomes of pneumonia treatment between low and high elevations, the mortality from pneumonia at altitude appears higher. 128
Treatment of community-acquired pneumonia is poorly studied, and no treatment guidelines for the high altitude setting exist. Any acute infectious lung process, especially one that results in hypoxemia, should be considered a contraindication for high altitude travel. Individuals with a history of tuberculosis should be screened for cavitary lung lesions or COPD because these illnesses increase the likelihood of altitude-related illness significantly. Oxygen supplementation and prophylactic acetazolamide may be considered for high altitude travel.
Tuberculosis
Although influenza and community-acquired pneumonia appear to increase mortality at high altitude, tuberculosis has a lower mortality 128 as well as decreased prevalence and likelihood of infection. 129 Nonetheless, tuberculosis infection carries a high likelihood of post-treatment sequelae, including cavitary lung lesions, emphysema, COPD, and pulmonary fibrosis,130,131 conditions that face increased risk of morbidity with high altitude exposure.
Severe Acute Respiratory Syndrome Coronavirus 2 Infection
Although individuals who have experienced severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection are at increased risk of cardiovascular and pulmonary sequelae, most recover with no persistent effects on gas exchange, respiratory mechanics, cardiovascular function, or exercise capacity. 132 A subset of these individuals will have persistent functional deficits and therefore are at increased risk when traveling at altitude.3,133 Nonsevere SARS-CoV-2 infection does not appear to increase the risk of AMS. 134 However, evaluation prior to high altitude travel should be considered for individuals whose symptoms persist for >2 wk following positive SARS-CoV-2 testing as well as for those who experienced severe SARS-CoV-2 illness. 133 These individuals should undergo pulse oximetry at rest and with activity, pulmonary function testing, plain chest radiography, electrocardiography, B-type natriuretic peptide determination, high-sensitivity troponin determination, and echocardiography.3,133 Abnormal results from these tests may necessitate modifying any high altitude travel plans.
Although high altitude pre-exposure may be potentially effective in reducing severity of SARS-CoV-2 infection in some patients, ongoing hypobaric hypoxia is likely associated with an elevated risk for patients with active SARS-CoV-2 infection. 135 Acute SARS-CoV-2 infection should be a contraindication to high altitude travel until symptoms resolve.
Conclusion
As travel to high altitudes continues to increase and our global population becomes more medically complex, understanding how preexisting conditions fare at high altitude is critical. While knowledge in this field is growing and experts have previously reviewed this general topic (notably Hackett and Luks in 2022), 1 data overall remain limited in certain areas. In this review, we’ve synthesized important literature while highlighting notable gaps—hopefully inspiring researchers to address these vital topics. Furthermore, this review is intended to equip providers with the necessary information to provide evidence-based guidance to patients planning high altitude travel, missions, and expeditions.
Footnotes
Author Contribution(s)
All contributed to the completion of the entire project.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
