Abstract
Introduction
Basic life support (BLS) is an emergency skill that includes performing appropriate cardiopulmonary resuscitation (CPR). Out-of-hospital cardiac arrest (OHCA) is a leading cause of mortality worldwide and is rising in Nepal. After an OHCA event, a bystander starting CPR quickly has been shown to increase the survival rate. While the Nepali police are generally the first responders to emergencies in rural parts, they are not trained in BLS. This program assesses a pilot training of hands-only CPR and choking first aid to the Nepal Police and Nepal Army participants in rural Nepal.
Methods
A community-based nonprofit organization, HAPSA-Nepal, coordinated with local government to pilot this program. The program included pre- and post-tests, lectures, videos, and small group hands-on exercises; facilitators included faculty emergency physicians, residents, and medical officers. Structured pre- andp post-test questionnaires, confidence surveys, and skills checklists were conducted. Descriptive analysis examined the respondent's characteristics, and paired t-test was used to compare pretest and post-test scores.
Results
A total of 126 participants received the training in this pilot phase. Prior to this training, 98.4% of the participants had not received any CPR training, and 100% of the participants had not received training on first aid for choking. The average pretest score was 4.4 with 95% CI ± 1.75, and the average post-test score was 8.06 with 95% CI ± 1.73 (out of a total of 11). All participants passed the skills assessment.
Conclusions
Locally adapted BLS training programs that included hands-only CPR and choking first aid showed a significant knowledge gain and skills competence among the frontline participants.
Introduction
Basic life support (BLS) is a life-saving skill provided by first responders that includes recognizing and performing appropriate cardiopulmonary resuscitation (CPR) and relieving obstructed airway in cases of choking. 1 According to the American Heart Association (AHA), CPR is “an emergency procedure that combines chest compressions often with artificial ventilation in an effort to manually preserve intact brain function until further measures are taken to restore spontaneous blood circulation and breathing in a person who is in cardiac arrest.” 2 Out-of-hospital cardiac arrest (OHCA), most commonly caused by cardiovascular diseases, is a leading cause of mortality worldwide.3,4 Though there is limited data availability on OHCA in Nepal, cardiovascular diseases have been on the rise, accounting for almost 27% of total deaths. 5 Additionally, the prevalence of predisposing risk factors for major cardiac events, such as diabetes and hypertension, has also been rising.6,7 Due to these factors, OHCA poses a significant burden on health care in Nepal, and this is estimated to rise as the population ages. 5
If performed within the first few minutes, CPR can increase the chance of survival for an OHCA victim by nearly 2- to 3-fold. 8 A bystander starting CPR quickly has also been shown to increase the survival rate after an OHCA event. 9 Hands-only CPR has been shown to be as effective in the first few minutes as conventional CPR and has been shown to improve the chain of survival after a cardiac arrest, with some studies showing an increased willingness of bystanders to respond after a cardiac arrest. 10
In Nepal, Emergency Medical Services (EMS) is in its infant stages, and the health system suffers from a significant shortage of health service providers. Estimates show that there are only 8.67 medical providers per 10,000 residents, which is much below the WHO-defined essential level.11,12 Furthermore, no formal community-based prehospital BLS training program exists, and statistics on OHCA are lacking. 13
The first response after a medical emergency is generally provided by the police or other community laypersons, especially in rural Nepal. 14 Nepali police are highly trusted and integrated within the Nepali community, and as such, they are well-positioned to provide lifesaving BLS in cases of cardiac arrest or choking events. 15 However, the Nepali police are not trained in and do not actively participate in, BLS. This pilot program focused on training key frontline responders, the Nepali police and the Army, on a BLS program that included hands-on CPR and choking first aid for an obstructed airway. The process of implementing this training program and preliminary results are presented in this paper.
Methods
Design and Setting
A community-based organization called Health Advancement Programs to Serve All (HAPSA-Nepal) partnered with local municipal leadership to plan a training program for local police and army officers. HAPSA-Nepal has a decade-long history of working with community-level responders, including community health workers, female community health volunteers, and local leaders, and focuses on disaster response and health knowledge advancement. 16 The local government chose the participants and organized the local logistics for the training program. Figure 1 shows the map distribution of the areas where police and army-based BLS training has been conducted by the facilitators and authors of this paper. The training performed in Doti, Nepal, is the primary focus of this program, and the results presented here are from that location.
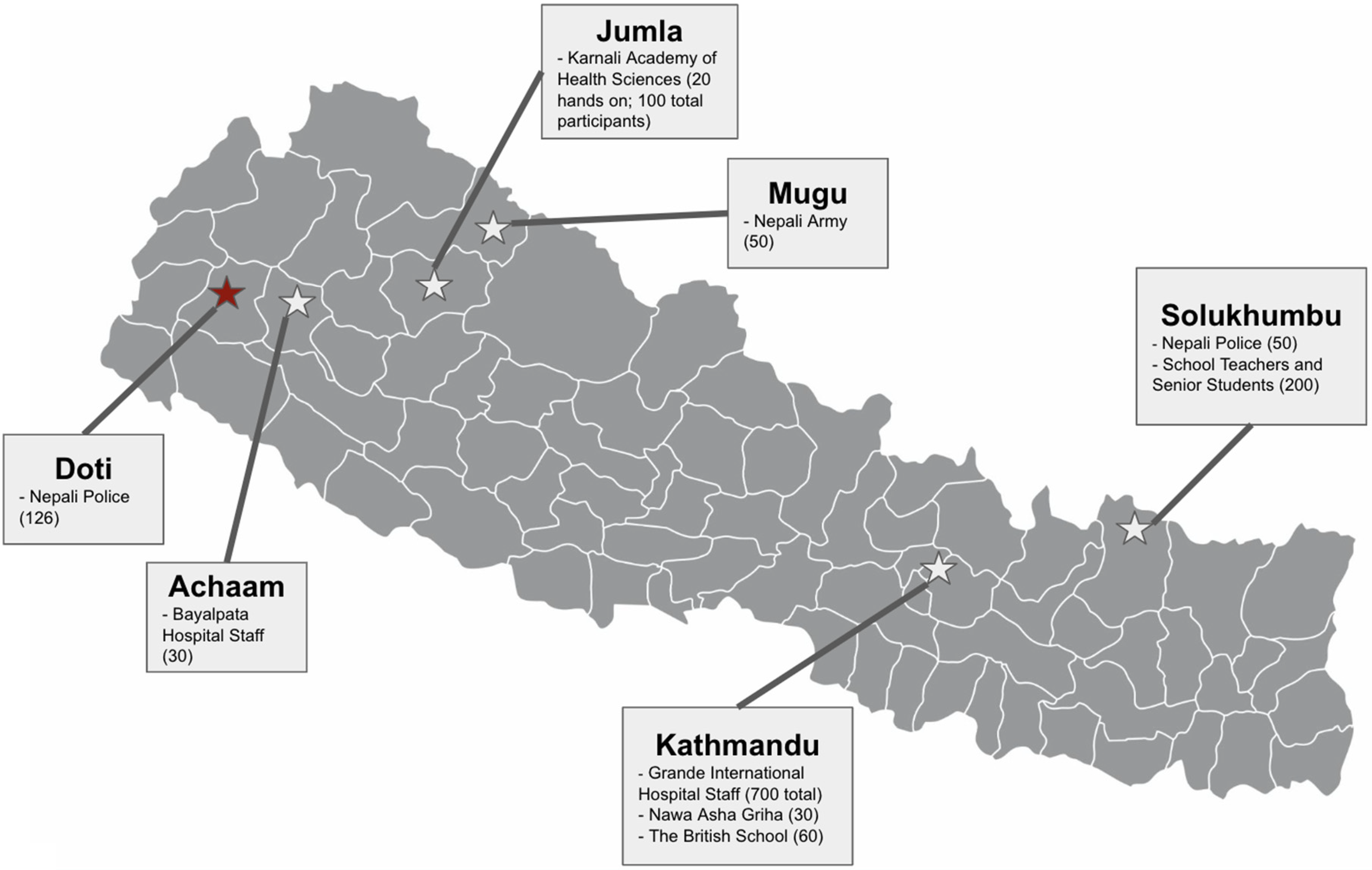
Areas of CPR program for police and army conducted by the primary facilitators. Red indicates the area where pilot data was collected.
Course Design and Implementation
The training program was designed by a US ABEM board-certified emergency medicine physician and a Nepali emergency medicine specialist. Two adult manikins were procured by the nonprofit organization, and partnerships were made by the NGO with the local municipality where the training was conducted. A team of experts traveled to the training site with manikins and printed training/assessment materials. The local logistics of participant recruitment, training venue, audio-visual, and participant snacks were supported by the municipality office. Experts conducting the training held active BLS and Advanced Cardiac Life Support (ACLS) training from the American Heart Association (AHA). The training program included pre-and postassessments, a didactic lecture, video supplements, and individual hands-on exercises. Training included local cultural references and was entirely taught in the local language by the course designers and assistants. The lecture portion was designed to be intermixed with discussion among participants where questions, comments, and/or concerns could be addressed by the lecturer. The total length of the lecture was approximately 1 hour. The lecture was followed by live demonstrations of hands-only CPR and choking first aid by the master trainers and individual hands-on sessions for each participant, facilitated by assistant trainers. Assistant trainers were also BLS and ACLS certified by the AHA and included emergency physicians, residents, and medical officers. The total training and assessment duration was nearly four hours.
Assessment
Immediately following the hands-on practice in small groups, a skill assessment was conducted using a standard skills checklist adapted from the Pakistan Life Saver's Program. 17 The facilitator provided case scenarios and asked individual participants to respond accordingly. The CPR performance checklist included participants’ ability to ensure scene safety, call for help, initiate CPR, perform high-quality CPR, and discontinue CPR when needed. Pre- and postknowledge assessments included 11 multiple-choice questions testing various topics pertaining to hands-only CPR and choking first aid. At the end of the training program, anonymous feedback was also conducted using a Likert scale questionnaire of 10 item statements, ranging from “Strongly disagree” to “Strongly agree.”
Data Collection and Analysis
All data was collected on paper forms. The forms were only accessible to the core training team. Results were input into a password-protected computer on Excel sheets, excluding identifier data. Each response was recorded with a unique serial number to match the pre- and post-test response. All the analyses were performed using Statistical Package for the Social Sciences (SPSS), version 26. Descriptive statistics such as frequency, percentages, mean, and standard deviations were used to analyze respondent's characteristics, pretest scores, and post-test scores. A paired t-test was used to compare pretest and post-test scores.
Results
Sociodemographic Characteristics
A total of 126 participants received training in the pilot phase of this program. The majority of the participants were male (n = 92, 73%). Prior to this BLS training program, 98.4% of the participants had not received any CPR training, and 100% of the participants had not received training on choking first aid; 65% of the participants were in the police force (Nepal police or Allied Police Force), 16.7% were from the Nepali Army, 15.6% were other health professionals, and 2.2% were other layperson participants.
Knowledge Results
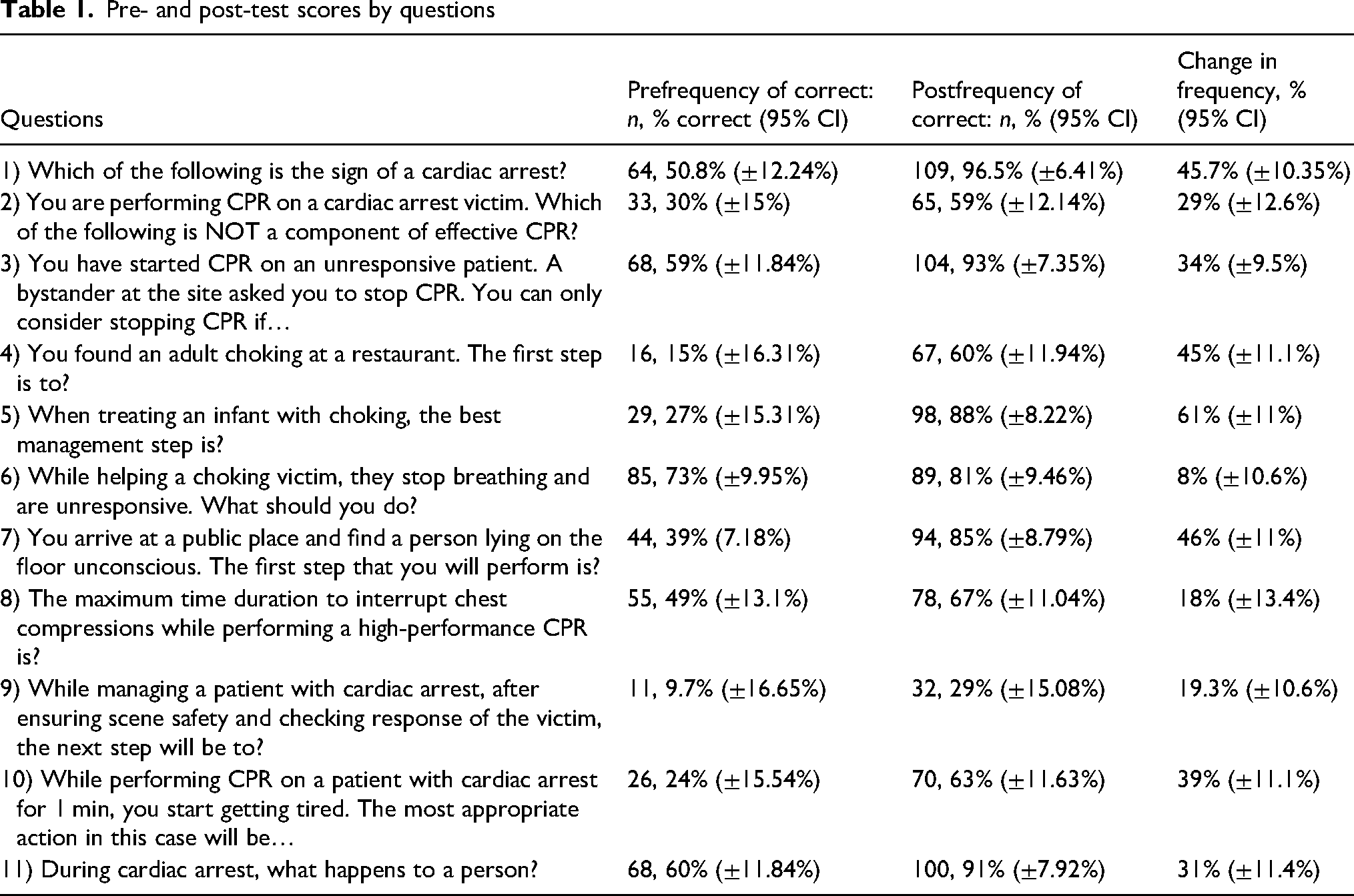
The mean pretest score was 4.4 (out of a maximum of 11) [95% CI ± 1.75], and the average post-test score was 8.06 [95% CI ± 1.73], showing a statistically significant difference in the mean pretest and post-test scores. Table 1 shows the pre- and post-test score with change in frequency, with 95% confidence interval for all items tested. All tested topics had statistically significant gain in knowledge except for 1 item. The item related to the next best step after a choking victim becomes unresponsive (#6 in Table 1) did show an increase in post-test score but was not statistically significant. Most substantial gains in knowledge were seen in items that tested the management of choking infants, rescue management of choking in adults, and the first step in the management of an unconscious person.
Pre- and post-test scores by questions
Skills Assessment
Skills assessment was a checklist conducted by the facilitator for each participant, ensuring the participant's ability to act safely, perform high-quality CPR, understand when to stop CPR, and identify and respond to choking incidents. All participants (100%) passed the skills assessment. The skills checklist is available in the Supplemental Material.
Feedback
Figure 2 shows results from the feedback survey, of which 89.68% of the participants completed. A majority of respondents agreed or strongly agreed that the course learning objectives were clear (99.1%). Similarly, opinions regarding the appropriateness of the course's overall difficulty showed 99.1% of participants agreeing or strongly agreeing. Majority of the respondents agreed or strongly agreed on training sessions with clear presentation(100%), 96.5% on good quality video being used, 100% on professional instructors, 100% on helpful trainers for completion of objectives, 100% on effective assistance, and 100% on confidence of skills. While 87.5% of participants agreed or strongly agreed that they would be able to respond if they came across someone who was in cardiac arrest or choking, 3 participants either disagreed or were neutral.
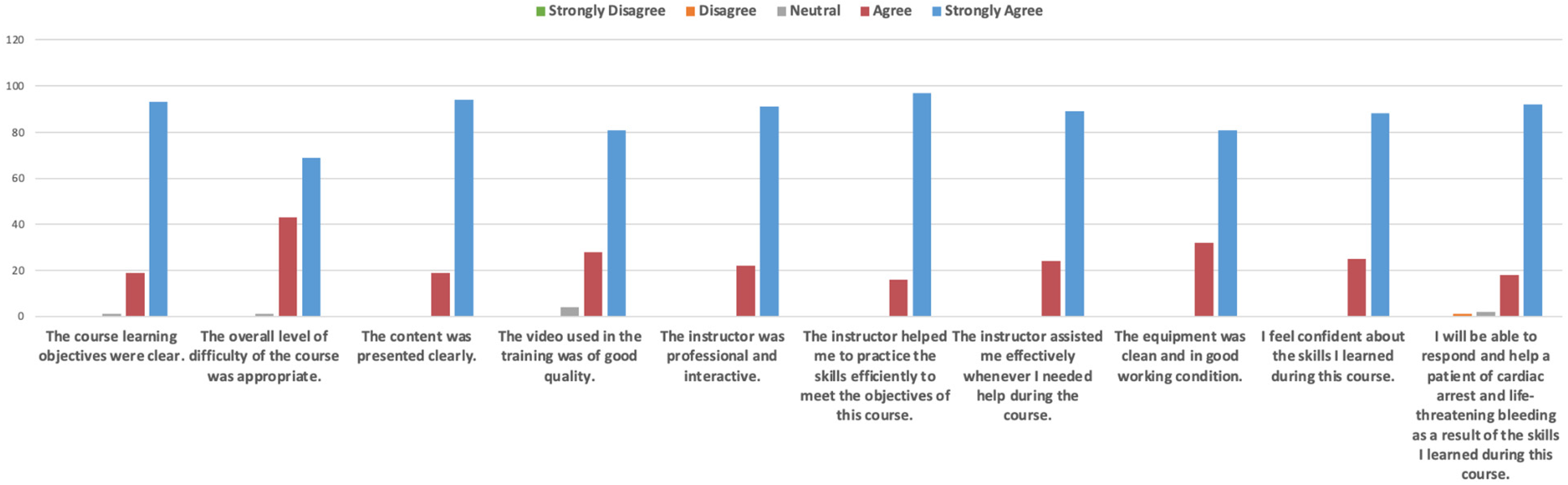
Confidence and feedback survey.
Discussion
This paper presents a pilot assessment of a hands-only CPR and choking first aid program for the Nepali police, who are the most common first responders in their communities. The results demonstrated the feasibility of conducting such a program in Nepal's setting and showed that the proposed program increases the knowledge and skills of participants. At the end of the program, all participants demonstrated adequate skills in hands-only CPR and choking first aid to relieve airway obstructions, and nearly 97% of participants felt comfortable caring for cardiac arrest or a choking victim. This training in Nepal was adapted from a similar program being conducted in Pakistan—the Pakistan Life Saver's Program (PLSP). The PLSP conducts hands-only training for layperson participants with a goal to train nearly 10 million laypersons across the country. This program in Nepal was established in close coordination with colleagues from the PLSP program, and this pilot training program shows that a similar program can be feasible in Nepal's setting as well.
In low- and middle-income countries (LMICs), there is a dearth of literature on OHCA, but poor outcomes are widely reported.18,19 In Nepal, where the health care system is fragile, and the emergency response system is in its infant stage, it is important to equip first responders with basic life-saving skills. As they are typically the first to respond to rural emergencies, police officers’ knowledge of CPR can be beneficial to those in rural settings where, otherwise, no other health care help is available promptly. Having a skilled first responder present can be especially impactful in situations that don’t necessarily require a health system, such as a choking victim. With Nepal's newly minted federal system, the municipal governments have adequate autonomy to improve health service delivery specific to their local challenges, and HAPSA-Nepal's program equips local governments through this partnership. The quantitative and qualitative results of this pilot work can be used to expand such programs across Nepal's rural municipalities. Future iteration of this work is underway, which will expand the scope of the BLS training program to include training for the use of automatic external defibrillators.
The limitations of this pilot program should be considered when interpreting the results. Firstly, the training was conducted among police personnel in a specific district of Nepal, which may limit the generalizability of the findings to other contexts or populations. Nepal is diverse in ethnicity, language, literacy rate, and socioeconomic status, and these findings cannot be generalized to the entire country. Future research should include a more diverse sample that encompasses different regions, occupations, levels of training, and demographics to ensure the broader applicability of the results. Furthermore, this program assessed the knowledge and skill level of participants immediately following the training program. Long-term retention of skill, confidence, and knowledge must be studied in the future. Furthermore, no current mechanism exists to ensure the participants get recertification at appropriate intervals. Local municipal coordination and buy-in is important to allow for appropriate interval recertification. Future iterations of this work could consider designing a training-of-trainers (TOT) course and empowering local participants. Other research could include comparison of findings of similar programs in other regions of the world and study of patient outcomes as an impact of training.
Conclusions
This pilot program providing BLS training program, which included hands-only CPR and choking first-aid for police first responders in rural Nepal, found significant knowledge gain, skills competency, and confidence. These results support the value of incorporating BLS training into the professional development of police personnel as a means to enhance their preparedness and effectiveness in emergency situations requiring CPR intervention.
Supplemental Material
sj-docx-1-wem-10.1177_10806032241226691 - Supplemental material for Pilot Training Program on Hands-Only CPR and Choking First Aid for Frontline Police Responders in Rural Nepal
Supplemental material, sj-docx-1-wem-10.1177_10806032241226691 for Pilot Training Program on Hands-Only CPR and Choking First Aid for Frontline Police Responders in Rural Nepal by Ghan B. Thapa, MD, Roshan Sapkota, BS, Anjana Thapa, BPH, Rajesh Sharma, MBBS, Derek Lubetkin, MD, Camille Lubetkin, MPH, Samuel Nesemann, MD, and Ramu Kharel, MD, MPH in Wilderness & Environmental Medicine
Footnotes
Acknowledgments
The authors would like to acknowledge Mr Ethan Register and Ms Hailey Tomasekh for their contribution to the graphic and figures. Authors acknowledge Mr Pankaj Bhattarai of HAPSA-Nepal and Mr Keshav Balayar of Doti in coordinating the training program logistics.
Author Contribution(s)
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: American Nepalese Medical Foundation (ANMF – https://www.anmf.org/) provided funding to HAPSA Nepal (www.hapsaglobe.org) to support logistical cost for this training program. The Doti local municipality provided local logistical support in the program.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
