Abstract
Keywords
Implications for Knowledge Translation
The study will:
Assist in narrowing the gap between theory and practice in nursing education through improving communication skills among students and health-care providers. Contribute to enhancing a more dynamic, effective, and safe learning environment to meet the demands of students and future health-care professionals by increasing their satisfaction and self-confidence. Promote educators and students to design and create various scenarios that mimic real-life situations.
Background
Due to the challenges of working in complex health-care environments as well as deficiencies in clinical skills among undergraduate nursing students (Black, 2022; Ko & Choi, 2020), nursing educators seek to transform nursing education through the integration of theoretical knowledge in clinical practice and the use of innovative strategies appropriate for the rapidly evolving digital age, to prepare competent nursing students and produce qualified and professional nurses (Khraim et al., 2015; Mohamed & Fashafsheh, 2019; Shin et al., 2015).
Current Knowledge
Simulation-based education is a safe and active didactic strategy in nursing education that allows learners to practice skills without harm, mimics the reality of a clinical environment, and evaluates clinical skills at different levels of nursing (Edward & Chukwuka, 2020; Smith et al., 2024) by utilizing task trainers, high-fidelity simulators, scenarios and case studies, and standardized patients (Delisle & Hannenberg, 2020). There are three main components of the simulation model to plan and implement the simulation experience and achieve desired outcomes: (a) simulation design that creates a trusting environment and shared responsibility between facilitator and learner, (b) educational practices that include experiential, interactive, and collaborative learning, and (c) learners’ outcomes that focus on behavior (how learning transfers to the clinical environment), learning (changes in knowledge, performance skills, and attitudes), and reactions (satisfaction and self-confidence) (Aebersold, 2018; Jeffries et al., 2015).
Student satisfaction and self-confidence are the most crucial outcomes that simulation-based learning aims to accomplish throughout training (Santos et al., 2021). Satisfaction is a feeling of acceptance that which originates from the outcome of an event and from the individual's prior expectations of themselves (Oliver, 2014). Nurse student satisfaction is associated with greater involvement and motivation in the teaching and learning process, as motivated students learn more and better, focus more on patient-centered care, and demonstrate effective teamwork in health-care settings (Baptista et al., 2014; Omer, 2016). On the other hand, self-confidence is the ability to believe in one's powers, skills, and success in a given situation (McGee, 2020). Thus, self-confidence is demonstrated among nursing students who do not have doubts that are dangerous for understanding the patient care process and making decisions (Swift et al., 2022). Building self-confidence among students occurs through performance achievement (learning through personal experience), indirect experience (learning through observation), verbal urgency (persuading people that their tasks were finished successfully), and emotional arousal (influencing people's perception) (Ariffin et al., 2022; Khalaila, 2015).
Communication is considered the core of nursing. Communication skills in nursing education are critical skills that improve students’ performance and efficacy and allow them to communicate with people from different cultures and backgrounds, leading to the development of self-confidence (MacLean et al., 2017; Mikkonen et al., 2016; Sibiya, 2018). Large numbers of nursing students and a lack of clinical training sites cause a lack of opportunities for practicing individual communication with patients and with other health-care providers, which is evident in patient hand-offs between nurses and physicians (Ali, 2018; Müller et al., 2018; Quail et al., 2016), leading nurse educators to seek alternative teaching strategies alongside traditional ways and integrate them into nursing curricula.
Simulation-based education enables students to enhance psychomotor and cognitive skills and encourages critical thinking, problem-solving, and decision-making (Foronda et al., 2018; Martins, 2017). Standardized patients as an alternative to clinical placement provide exercises to improve students’ communication skills and increase their satisfaction and self-confidence (Cant & Cooper, 2017; Johnson et al., 2020). The situation-background-assessment-recommendation (SBAR) format, an important interpersonal communication strategy in simulations, allows nursing students to play different roles within a team, enhancing critical thinking, problem-solving, and taking effective clinical judgment toward the different scenarios they face (Cuchna et al., 2021; Lee & Doran, 2017).
Purpose
The purpose of this study was to examine the effectiveness of simulation-based education on the educational practices of communication skills, satisfaction, and self-confidence among undergraduate nursing students in their first year.
Methods
Study Design
The study used an uncontrolled before-and-after design. Some studies of simulation-based learning have used this type of design, usually involving an initial observation of the phenomenon of interest performed in a simulated environment, then introducing an intervention (training, new equipment, new procedures, etc.) and repeating the measurements. Additionally, it was adopted to demonstrate an association between the intervention and its outcome (Lamé & Dixon-Woods, 2020).
Setting
This study was conducted in the Nursing Department at Al-Quds University in Jerusalem, Palestine.
Participants
The total population comprised 220 students in the first year of the nursing program who were enrolled in a prerequisite Fundamental Nursing course, in the spring semester of the 2022–2023 academic year. The sample size was calculated via G*power 3.1 by considering alpha = 0.05, a medium effect size, and a margin of error of 10% with a 95% confidence interval (Faul et al., 2009). This provided a sample size of 68 undergraduate nurse students. In this study, a sample of 112 participants, which was greater than the required sample size, was chosen using a digital randomization tool.
Inclusion Criteria
All first-year nursing students who were enrolled in the Fundamental Nursing course (Theory and Lab) for the first time in the spring semester of the 2022–2023 academic year, who attended the simulation nursing lab.
Data Collection Instruments
Sociodemographic Data
This tool, designed by the researcher, gathered descriptive sociodemographic characteristics of participants such as gender, age, academic grade average, place of residence, previous work as a nursing assistant or nursing aid, information technology skill level at enrollment, digital tool used during course work, and satisfaction with simulation-based learning experience.
Educational Practices Questionnaire (EPQ)
This instrument, used with permission, was developed by the National League for Nursing (NLN) (2006), derived from the work of Chickering and Gamson (2006). It is frequently used to measure whether best practices are being used in the simulation. It includes four sections: 16 items (10 items measured active learning, and two were designed to examine collaboration, diverse ways of learning, and high expectations) are present in the instructor-developed simulation, and the importance of each practice to the learner is expressed in the form of a 5-point Likert scale ranging from 1 = strongly disagree to 5 = strongly agree. The Cronbach's alpha value of the scale was 0.91. (Chickering & Gamson, 2006; Hallmark et al., 2014). In this study, this instrument was used by the researcher to examine the effect of simulation-based education on undergraduate nursing students’ communication skills, which are an essential educational practice at clinical sites. Cronbach's alpha was 0.93 (see Table 1).
Reliability of Educational Practice Questionnaire (EPQ) and Student Satisfaction and Self-Confidence in Learning (SSSCL).

Student Satisfaction and Self-Confidence in Learning (SSSCL)
This instrument, used with permission, was developed by NLN-SSSCL (Kardong-Edgren et al., 2010; NLN, 2006) to measure students’ satisfaction and self-confidence during simulation-based education. It consists of two sections: satisfaction with current learning, which consists of five statements, and self-confidence in learning, which consists of eight statements in the form of a five-point Likert scale ranging from 1 = strongly disagree to 5 = strongly agree. Cronbach's alpha values were satisfaction = .94 and self-confidence = .87. (Jeffries, 2022; Kardong-Edgren et al., 2010). Notwithstanding the reliable application of these scales in previous literature, we recognize a potential for cultural desirability bias. So, the reliability of the EPQ and SSSCL instruments was also analyzed using the Statistical Packages for the Social Sciences (SPSS) to obtain Cronbach's alpha values, which were .93, .84, and .85, respectively (Cortina, 1993). See Table 1.
Simulation Type
In this study, standard patient simulation was used to enhance students’ collaboration and awareness in educational practice simulation (Dalwood et al., 2020). Based on the participants’ level, scenarios were designed and prepared in the simulation experience. Then, they were distributed in different roles based on a scenario using the SBAR technique, through a role-play (primary nurse, secondary nurse, physician, member of the health-care team, and member of the family).
Study Procedure
After the researcher discussed the aim of the study and obtained informed consent from all participants, they were divided into 20 groups of 5–6 participants each in the simulation laboratory. Then, different clinical scenarios related to the fundamental nursing course for each group were distributed, and the simulation roles were also included among them (primary nurse, secondary nurse, physician, patient, and family member). Next, a simulation strategy was conducted using the SBAR technique, which took between 10 and 15 min for each group, depending on the scenario context. After completing the procedure, filling out the questionnaire was required from each participant and took approximately 5–10 min. The data weres collected from March 1 to April 30, 2023.
Ethical Considerations
Approval for the study was obtained from the al-Quds University Institutional Review Board (IRB) (Ref. No.: RESC/2023-39). After explaining the study's aim, written consent was obtained from participants at the beginning of the study, by recording their contact information (phone number, address). The students were assured that their answers would be kept confidential and would not affect or interfere with their evaluation. The students were informed that their involvement in this research was voluntary, that anonymity was respected, and that no penalty would arise from nonparticipation or withdrawal. Then, the study data were collected.
Data Analysis
Data were analyzed using the Statistical Package for Social Science (SPSS) software version 25. The researchers used descriptive statistics such as means, standard deviations, frequencies, and percentages to describe the data. Pearson's Chi-square test was conducted to observe and quantify an association between different variables of the study, and a dependent sample t-test was used to determine the relationship between the study variables and pre–posttest scores. p < .05 was considered suggestive.
Results
Demographic Characteristics
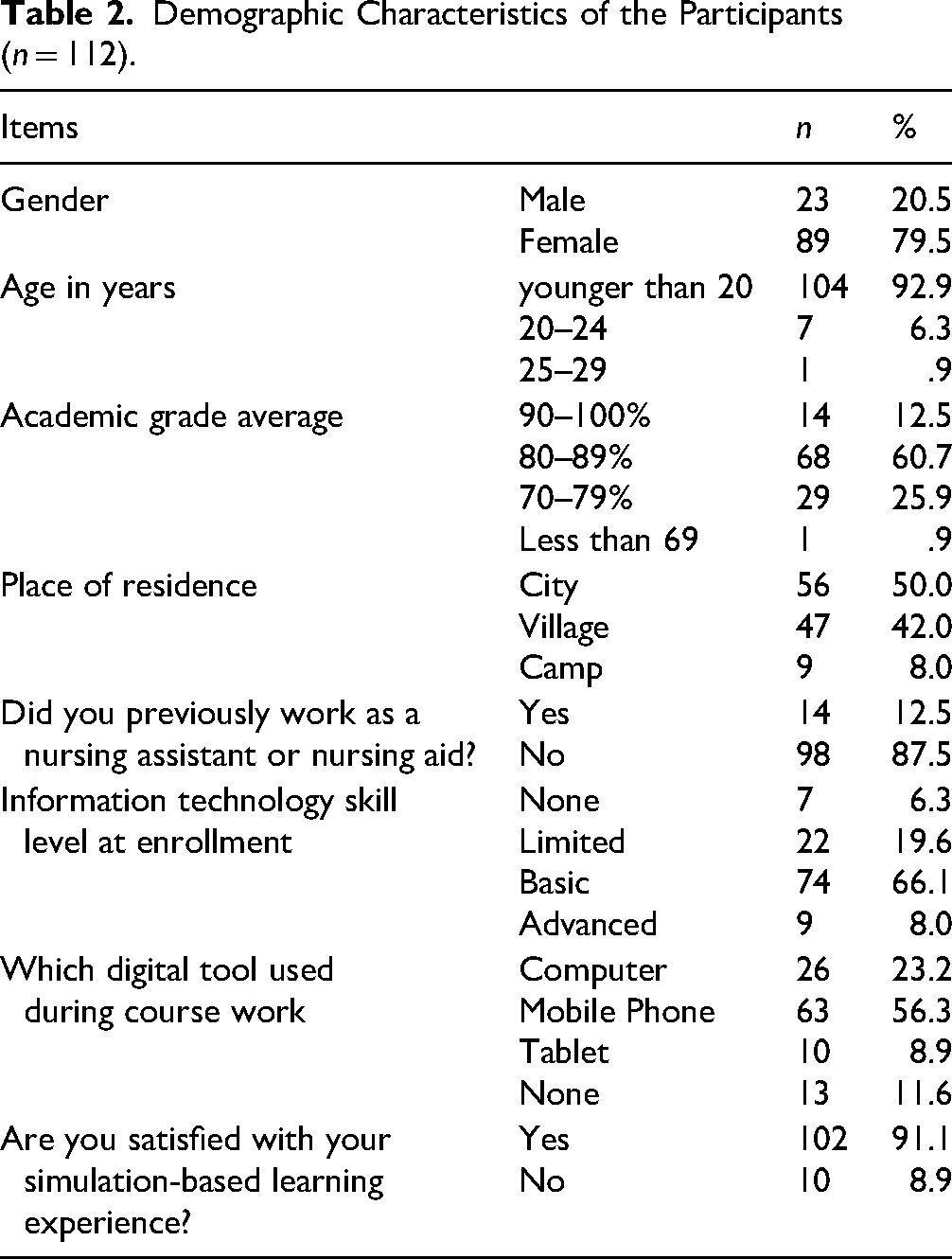
Out of the 112 participants in the study, 91% were satisfied with using simulation-based education; 92.9% were under the age of 20, 79.5% were female, and half were residents of cities. Only 12.5% had held a position as a nursing assistant and 60.7% had a grade average of 80–89%. More than half of them utilized their mobile phones as digital tools for their schoolwork and possessed rudimentary IT skills (Table 2).
Demographic Characteristics of the Participants (n = 112).
Educational Practices and Learning Scales
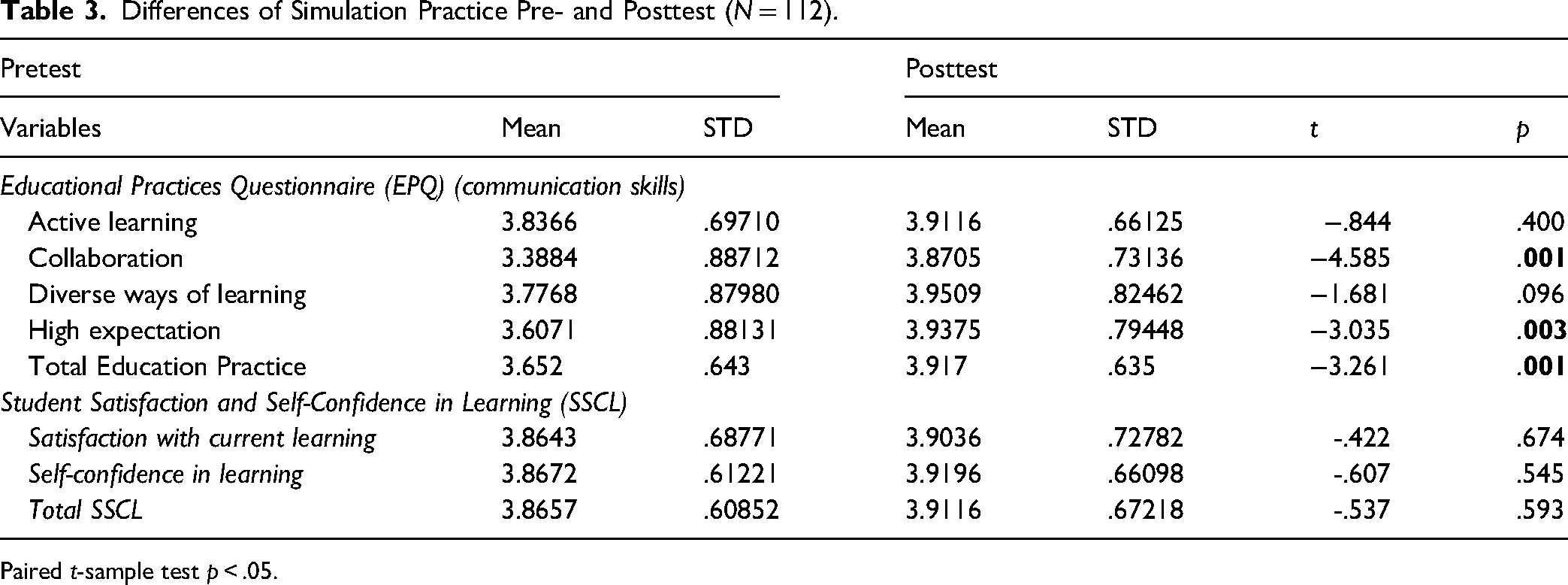
The statistical processes utilized to analyze the pretest and posttest mean scores and standard deviations for the EPQ and the SSSCL scales are shown in Table 3. The differences between the mean scores before and after the simulation sessions were compared using paired t-tests. The findings show that following the simulation session, students’ communication skills, as assessed by the educational practice questionnaire, improved. The posttest showed a higher education practice of communication skills than the pretest (M = 3.91). Additionally, there were statistically significant differences in communication skills (p = .001). Additionally, the results demonstrate that there were statistically significant differences in collaboration and high expectations (p < .01, p = .003, respectively) between the two tests. The posttest mean score for all subscales of the education practice questionnaire for communication skills was higher than the pretest mean score (M = 3.95, M = 3.93, and M = 3.91, respectively).
Differences of Simulation Practice Pre- and Posttest (N = 112).
Paired t-sample test p < .05.
The results also demonstrated students’ satisfaction and self-confidence with simulation-based education. The posttest had a higher mean score for student satisfaction and self-confidence than the pretest (M = 3.90 and 3.91, respectively), and the posttest's total mean score for SSSCL was higher (M = 3.91) (see Table 3).
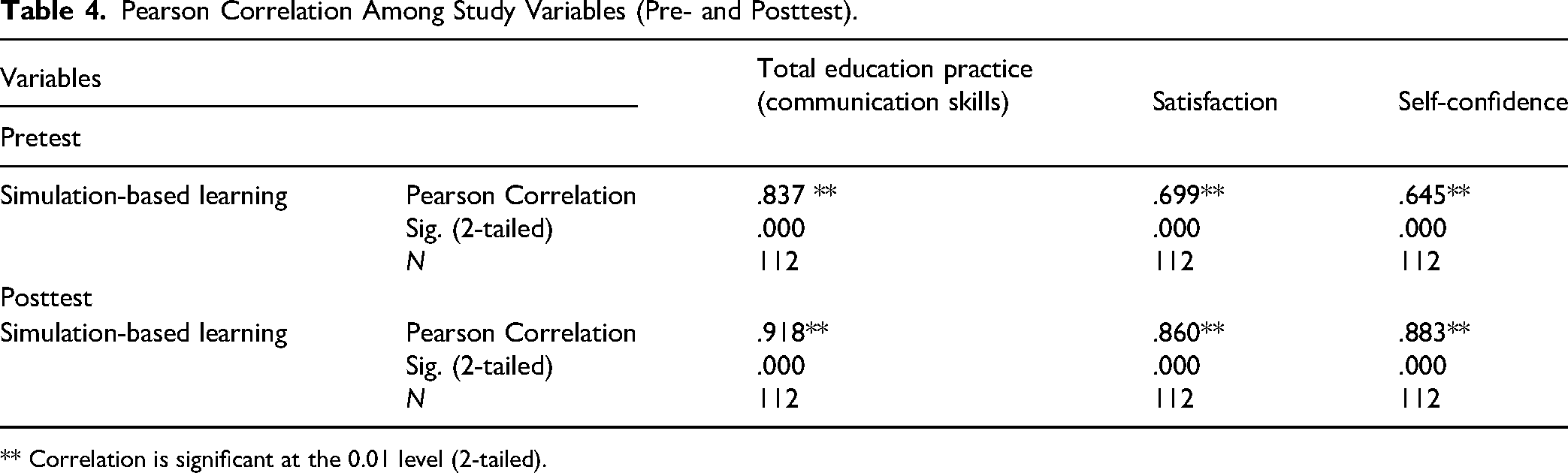
Table 4 shows the Pearson correlations of the study variables that measure simulation-based education and are correlated with communication skills, student satisfaction, and self-confidence in the pre–posttest. There is a statistically significant positive correlation between simulation-based education and the practice of communication skills, student satisfaction, and self-confidence (p < .05, r = .918; .860; .883, respectively).
Pearson Correlation Among Study Variables (Pre- and Posttest).
** Correlation is significant at the 0.01 level (2-tailed).
Discussion
This study implemented communication skills among nursing students during the fundamental nursing course by using a simulation strategy and SBAR technique, to examine the effect of simulation-based education on educational practices in communication skills, satisfaction with current learning, and self-confidence in learning, following Jeffries's Nursing Education Simulation Model (Jeffries, 2020, 2022).
The results indicate that the essential features of educational practice after simulation sessions for communication skills were arranged as follows: firstly, diverse ways of learning; then, high expectations and active learning; and finally, collaboration. There was a significant difference between collaboration and high expectations. These results may be attributable to dynamics and complexity in a clinical environment, in which communication and efficient teamwork among health-care professionals are important to meet the needs of patients and collaboration takes place in all stages of the nursing process to achieve desired outcomes (Granheim et al., 2018). Also, simulation is considered an effective approach to improving collaborative skills for nursing students to meet learning objectives (Foster et al., 2019). In this study to enhance students’ collaboration and awareness in educational practice simulation, the different roles and scenarios were designed and prepared in the simulation on standard patients, which takes place through distributed role-play among students; students were told that teamwork is common in clinical practice and that team support and collaboration can affect efficiency, cooperation, communication, and leadership, which agrees with the findings of Grover et al. (2017) and Mohamed and Mohamed (2020).
Although this study showed there are no significant differences between active learning and communication skills, active learning showed the highest mean score, which demonstrated that active learning is an intrinsic structure, a systematic and comprehensive feature of simulation educational practice that gives students an optimal chance to be engaged actively by using their psychomotor, cognitive, and affective skills that increase students’ satisfaction and self-confidence, which agrees with the findings of (Olaussen et al., 2020; Tosterud, 2015). In addition, active learning plays a vital role in interactive learning environments, allowing a learner-centered process (Allen & Armstrong, 2013; Jeffries, 2005), through structured learning experiences with several scenarios and debriefing criteria to enhance clinical judgment and performance in simulation (Chmil et al., 2015). Consequently, it allows students an opportunity to explain the concepts and ideas learned during the simulation with instructors and peers. Also, they could reflect deeply on their preexisting opinions during the debriefing, which is one of the key building blocks of simulation-based training that enables students feedback to observe the natural consequences of their mistakes and learn from it. Similarly, these findings were consistent with the study of Ali and Musallam (2018), Cho and Kim (2023), Mohamed and Mohamed (2020), and Saravana-Bawan et al. (2019).
On the Student Satisfaction and Self-Confidence in Learning tools in the current study, 91.1% of participants conveyed high satisfaction with using simulation-based education in communication skills toward effective, motivated, and helpful teaching methods and materials, instructors’ enjoyment teaching the simulation course, and satisfaction with their instructor's teaching style, which agrees with the quasi-experimental pre–posttest simulation study by Liaw et al. (2014) among nursing students at Singapore University. In a study by Zapko et al. (2018), satisfied students experienced different realities in a safe and controlled environment; felt meaning in their experience; reflected on contexts, scenarios, practices, and attitudes; minimized gaps in theoretical and clinical perceptions; and were more motivated to learn.
In this study, students agreed that their self-confidence increased after simulation training, which is consistent with studies by Omer (2016) and Larue et al. (2015) that concluded simulation enhances self-confidence and facilitates learning, which allows students to utilize their skills in a clinical setting. Hence, the simulation experience in this study reinforced students’ satisfaction and self-confidence, which may assist them in recognizing errors, participating as effective team members, performing an effective intervention, and improving their critical thinking. This concurs with several studies conducted to examine the same note (Costa et al., 2020; Foronda & Bauman, 2014; Mohamed & Mohamed, 2020; Nascimento Reis et al., 2020; Souza et al., 2020).
The current study found a significant positive relationship between simulation-based education and educational practice in terms of communication skills, satisfaction, and self-confidence after simulation training (p < .05). The satisfaction and self-confidence scores increased among students after learning the content and performing the simulation scenarios through role play, which agrees with the study by Saied (2017), which showed high student satisfaction and self-confidence after a simulated pediatric scenario experience, as well as similar studies (Al Khasawneh et al., 2021; Karataş & Tüzer, 2020; Saied, 2017; Zulkosky, 2012) that revealed student satisfaction increased as self-confidence increased.
The findings of this study also showed there are significant differences between high expectations and educational practice simulation of communication skills among students, which leads to evaluation of the ease and clarity of objectives and outcomes of simulation and the instructors’ achievement, allowing students to access desired expectations during performing scenarios in simulation training and increase their satisfaction and self-confidence, which agrees with a study by Cabrera-Mino et al. (2019).
So, this study showed that simulation is a learning modality emphasizing the importance of collaboration, teamwork, and effective communication among team members through shared activities and understanding that improves their satisfaction and self-confidence (Bland & Tobbell, 2016; Zajac et al., 2020). Implementing diverse learning styles in nursing simulations such as role-playing and small group practices can lead to high student satisfaction and confidence (Coleman, 2022; Zapko et al., 2018).
Limitations
In this study, the EPQ and the SSSCL instruments were used, relying on self-report for improvements in knowledge or performance, which is subject to bias and affects generalizability. So, further studies must enhance the survey instruments that are utilized to evaluate simulation-based education on students’ communication, satisfaction, self-confidence, and other aspects of nursing education even after their validity and reliability have been established. In addition, future research should include in-depth qualitative interviews with nursing students, integrating simulation-based education in several nursing courses, and developing practical skills.
Implications for Nursing Education
The study will contribute to developing nursing education by promoting constructive teaching strategies such as simulation and strengthening a more dynamic and efficient progressive learning environment to meet the demands of students and future health-care professionals. It is also expected to encourage nursing students’ learning skills and abilities. This study may direct experimental studies exploring whether simulation-based education improves students’ cognitive, psychomotor, and affective skills that depend on student-centered learning. Additionally, this study promotes more qualitative and quantitative research on student engagement and simulation experiences, helping to bridge the knowledge gap between nursing theory and practice regarding nursing students’ perceptions of simulation experiences in nursing education and their level of satisfaction, knowledge, and performance. Additionally, clients should be closely involved in the design and create scenarios that mimic real-life situations.
Conclusion and Recommendations
Simulation-based education is an essential strategy in preparing students for a successful transition to clinical practice; it contributes to improved communication skills, satisfaction, confidence, competence, and critical thinking. So, simulated experiences are an option to supplement the traditional nursing education approach. This study demonstrates that the simulation-based education experience that is accessible in the nursing skills laboratory is sufficient and suitable for the students to learn several skills in various nursing programs, such as fundamentals of nursing, medical/surgical nursing, critical care nursing, neonatal and pediatric nursing, and obstetrics and gynecology nursing. Teaching with simulated conditions leads to a focus on experiences in the teaching-learning process through the use of various simulation scenarios, and is integrated into the core nursing curriculum by involving suggestions for care improvements in the practice.
Consequently, this study recommended educational institutions be encouraged to enhance improvements in the laboratory infrastructure and in the faculty's capacity to work with the simulation strategy, and these teaching strategies emerged in nursing curricula. Furthermore, it encourages clinical instructors and nurse educators to create various real-life scenarios from these experiences by supporting training and clinical courses in several simulation sites. In addition, carrying out research is needed to explain the potential of simulation in different contexts and settings in nursing education.
Footnotes
Acknowledgments
The author is thankful to the simulation nursing lab administration in the nursing department of the Faculty of Health Professions at Al-Quds University for providing us with the opportunity to conduct this study and for all the resources and support they provided. Also, grateful to all the students who helped us collect data and to all the associated personnel in any reference who contributed to this research.
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
