Abstract
To describe the impact of delayed call time for chest pain in the salvage of ST-segment elevation myocardial infarction (STEMI) patients and its associated independent risk factors, and to identify risk factors associated with cumulative morbidity and mortality in STEMI patients at 4 years after percutaneous coronary intervention (PCI). Retrospective analysis of 398 patients diagnosed with STEMI and treated with emergency PCI within 24 hours of symptom onset in Fuyang People's Hospital from April 2018 to April 2021. The enrolled patients were divided into ≤60 minutes group (193 cases), and > 60 minutes group (205 cases), according to the delayed call time of patients with chest pain. Analysis of basic clinical data, rescue time, and major cardiovascular adverse events in the 2 groups. Multifactorial logistic regression analysis of independent correlates of delayed chest pain calls and Cox proportional risk regression modeling of risk factors for cumulative morbidity and mortality at 4 years after surgery. Compared to the delayed call time ≤ 60 minutes group, the > 60 minutes group had a higher proportion of females, a history of diabetes, rural remote areas, and farmer occupation (P < .05). Binary logistic regression analysis shows the history of diabetes and female as independent risk factors for delayed call time >60 minutes for chest pain. In the delayed call time ≤60 minutes group, the time from symptom onset-to-balloon (S0-to-B) and from symptom onset-to-first medical contact (SO-to-FMC) were smaller than in the delayed call time >60 minutes group (P < .05). The sum of postinfarction angina and major cardiovascular adverse events was lower in the group with delayed call time ≤60 minutes than in the group with delayed call time >60 minutes (P < .05). The Kaplan-Meier survival curve and the survival curve without the occurrence of major adverse cardiovascular events were statistically significant in both groups (P < .05). Multifactorial Cox regression analysis showed that delayed call time for chest pain >60 minutes, left main + 3 branch lesions, and cardiac function Killip ≥ III were all risk factors for cumulative morbidity and mortality at 4 years after PCI in patients with STEMI. Delayed call time for chest pain >60 minutes, left main + 3 branch lesions, and cardiac function Killip ≥ III are all risk factors for cumulative morbidity and mortality in STEMI patients at 4 years after PCI. Reducing the delayed call time for chest pain can improve the long-term prognosis of patients.
Keywords
Introduction
Acute ST-segment elevation myocardial infarction (STEMI) is characterized by acute onset and a high mortality rate. European studies have found in-hospital mortality in STEMI patients to be between 4% and 12%, with a 1-year mortality rate of approximately 10%.1,2 STEMI requires urgent target vessel revascularization, and percutaneous coronary intervention (PCI) within 120 minutes of first medical contact is the preferred revascularization, while fibrinolytic therapy may be an option for other patients. 3 In recent years, domestic and international studies have focused on symptom onset-to-first medical contact (SO-to-FMC), door-to-balloon (D-to-B), first medical contact-to-balloon (FMC-to-B), and symptom onset to balloon (SO-to-B), where onset refers to the time point of symptom onset that forces the patient to seek medical attention. 4 In early studies, particularly D-to-B time has been used as a key quality indicator and publicly reported performance indicator for hospital treatment of STEMI provision. 5 Early reduction in D-to-B time is associated with a significant reduction in mortality; however, D-to-B time accounts for only a small fraction of total ischemic time. 6 Delayed call time for chest pain refers to the time between the onset of discomfort such as chest pain and chest tightness and the time when the patient is compelled to seek medical attention and call the emergency system or prepare to go to the hospital, which is one of the main factors causing myocardial infarction and major adverse cardiovascular events (MACE). 7 The time until first medical contact is the sum of the delayed call time for chest pain and the SO-to-FMC time, making it particularly important that reducing the delayed call time for chest pain determines the salvation and prognosis of the patient's condition. Studies have shown significant benefits of reperfusion in the first 2 to 3 hours after symptom onset. 8
Therefore, clinical studies have been focusing on the timing of the components in the FMC-to-B to implement relief. However, there are few studies on the delayed call time for chest pain, which plays an important role in the evolution of STEMI as an unappreciated time for patients to be rescued. The median medical decision time (delayed call time for chest pain) for STEMI patients in a large study of 24 662 patients was 60 minutes. 7 Therefore, in this study, the delayed call time for chest pain was divided into 2 groups using 60 minutes as the threshold for analysis, aiming to investigate the risk factors affecting the delayed call time for chest pain and the risk factors for morbidity and mortality after PCI in STEMI patients and to provide some clinical guidance for the management of STEMI patients.
Materials and Methods
General Information
In this retrospective study, 398 patients who visited our hospital from April 2018 to April 2022 with a diagnosis of AMI and treated with emergency PCI were analyzed.
Inclusion Criteria
(1) The criteria for the diagnosis of STEMI are in accordance with the relevant criteria in the 2017 European Society of Cardiology (ESC) Guidelines on the management of ST-segment elevation myocardial infarction published by: ① The patient has typical STEMI chest pain lasting ≥ 30 minutes. ② ST-segment changes on ECG with ST-segment elevation in at least 2 adjacent leads ≥1 MV or presence of left bundle branch block with elevated troponin/creatine kinase isoenzyme. 9 (2) The enrolled patients were all first-time PCI patients.
Exclusion Criteria
Patients who had undergone remedial PCI with thrombolytic therapy in an outside hospital; patients who were first received by an outside hospital and transferred to our hospital for transport PCI; patients who were unable to cooperate with the investigation and could not provide accurate time of onset; incomplete clinical data; and those with other serious infectious diseases or malignant tumors in combination.
Standard of Practice
A total of 398 patients were admitted to the hospital: some were admitted with family or friends driving, some were admitted on their own by public transportation, and some were admitted by emergency call. All patients were admitted to the hospital on an emergency basis and underwent emergency coronary angiography and PCI via the radial or femoral artery after chewing a packet of heart attack medication (aspirin 300 mg, Ticagrelor 180 mg, and Rosuvastatin 20 mg).
Observation Indicators
The main rescue time points, including SO-to-FMC, D-to-B, FMC-to-B, and SO-to-B times. General data such as age, sex, time point of disease onset, place of residence, education level, occupation, hypertension, diabetes mellitus, hyperlipidemia, smoking, alcohol consumption, left ventricular ejection fraction, cardiac function classification, infarct site and number of coronary lesion branches were counted in both groups. Record the MACE of patients in the first year after discharge and the death of patients in each year. MACE includes cardiac death, target lesion revascularization (TLR), malignant arrhythmia, ischemic stroke, and postinfarction angina. TLR is defined as rheumatologic reconstruction after stent placement in or within a 5-mm boundary near the stent.
10
The day is divided into 2 periods: daytime from 6:00 to 18:00 and nighttime from 18:00 to 6:00.
7
In this article, the rural area refers to the geographical characteristics such as more than 50 km from the hospital, imperfect public facilities, and inconvenient transportation. the urban area has various facilities and is closer to the hospital, and the urban residents have better living conditions than the rural area. Cardiac function in patients with STEMI is graded using Killip grading according to hemodynamic severity as follows: Killip class I (no significant heart failure); Killip class II (mild heart failure with wet lung rales < 50% lung field); Killip class III (with acute pulmonary edema with wet lung rales > 50% lung); Killip class IV (manifestations of cardiogenic shock).
11
Normally distributed measures are expressed as (
Statistical Analysis
The enrolled patients were divided into ≤60 minutes group (193 cases), and > 60 minutes group (205 cases), according to the delayed call time of patients with chest pain. Analysis of basic clinical data, rescue time, and major cardiovascular adverse events in the 2 groups. Multifactorial logistic regression analysis of independent correlates of delayed chest pain calls, and Cox proportional risk regression modeling of risk factors for cumulative morbidity and mortality at 4 years after surgery.
Results
Comparison of General Information Between the 2 Groups of Patients
Compared to the delayed call time ≤60 minutes group, the >60 minutes group had a higher proportion of females, a history of diabetes, rural area of residence, and farmer occupation. The difference was statistically significant (P < .05); see Table 1 for details.
Comparison of General Information of Patients in the Group With Delayed Call Time of Chest Pain ≤ 60 minutes and the Group With > 60 minutes.

Comparison of General Information of Patients in the Group With Delayed Call Time of Chest Pain ≤ 60 minutes and the Group With > 60 minutes.

Comparison of the Rescue Time of Patients in the 2 Groups
S-to-B and SO-to-FMC rescue times were longer in the >60 minutes group compared to the delayed call time ≤60 minutes group. The difference was statistically significant (P < .05); see Table 2 for details.
Comparison of the Rescue Time of Patients with Delayed Call Time for Chest Pain ≤60 minutes and >60 minutes Groups.

Abbreviations: SO-to-FMC, symptom onset-to-first medical contact; D-to-B, door to balloon; FMC-to-B, first medical contact to balloon; SO-to-B, symptom onset to balloon.
Risk Factors Independently Associated With Delayed Call for Chest Pain in Both Groups
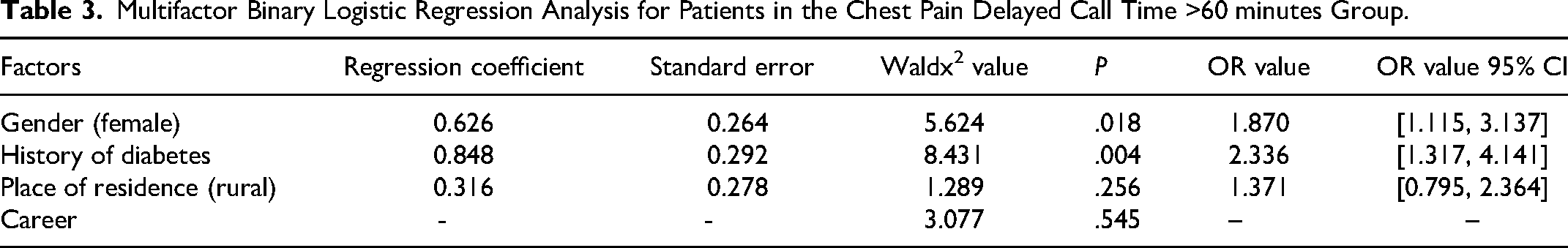
Females with and history of diabetes mellitus were independent risk factors for patients in the delayed call time for chest pain >60 minutes group; see Table 3 for details.
Multifactor Binary Logistic Regression Analysis for Patients in the Chest Pain Delayed Call Time >60 minutes Group.
Follow-Up of the 2 Groups
Patients in both groups were followed up for a cumulative period of 4 years after discharge from the hospital. The proportion of total postinfarction angina and MACE was greater in the >60 minutes group compared with the delayed call time for chest pain ≤60 minutes group. The difference was statistically significant (P < .05); see Table 4 for details.
Comparison of MACE Between Patients With Delayed Call Time for Chest Pain ≤60 minutes and >60 minutes Groups.

Abbreviations: MACE, major adverse cardiovascular events; TLR, target lesion revascularization.
Multifactorial Cox Regression Analysis of Risk Factors for Cumulative Morbidity and Mortality in AMI Patients at 4 Years After PCI
Delayed call time for chest pain > 60 minutes, left main + 3 branch lesions, and cardiac function ≥ grade III were all risk factors; see Table 5 for details.
Multifactor Cox Regression Model Analysis of Risk Factors for Cumulative Morbidity and Mortality in AMI Patients at 4 Years After PCI.

Note: Multifactor Cox regression model analysis included symptom onset-to-first medical contact, door to balloon, first medical contact to balloon, symptom onset to balloon, time, age, sex, disease onset time point, place of residence, education, occupation, hypertension, diabetes mellitus, hyperlipidemia, smoking, alcohol consumption, left ventricular ejection fraction, cardiac function class, infarct site, and number of coronary lesion branches.
See Figures 1 and 2 for details.

Kaplan-Meier survival curves for both groups (Log-rank P = .003).

Survival curve without major adverse cardiovascular events (MACE) occurrence in both groups (P = .013).
Predictive Model Construction for Chest Pain Delayed Call Time on MACE
The area under the ROC curve (AUC) = 0.59, 95% confidence interval (CI): 0.516 to 0.658, P = .02. See Figure 3 for details.

ROC curve of the degree of prediction of MACE by delayed call time for chest pain.
Discussion
The establishment and implementation of a national standardized “chest pain center” plays a crucial role in the successful treatment of acute myocardial infarction, and PCI is the first choice for reperfusion treatment of acute myocardial infarction, which is also the key to improving the survival rate and quality of life of patients with acute myocardial infarction. 12 As the component with the longest duration of ischemia, the prehospital delay from symptom onset to hospital admission is currently an important concern. 13 Total prehospital delay was defined as the time between the onset of myocardial infarction symptoms and arrival at the designated hospital emergency department, and the prehospital delay was further divided into “decision time” and “time from decision to hospital emergency.”9,14 The “decision time” is the time between the onset of the patient's symptoms and the decision to seek medical attention, the delayed call time for chest pain. The main reasons for delayed chest pain calls are that the patient believes the symptoms will go away, the symptoms are not severe enough, and that the patient believes the symptoms are caused by another disease. 15 Early studies overemphasized the D-to-B time period, but this period was only in-hospital treatment. STEMI patients often do not seek medical attention for about 1.5 to 2 hours after the onset of symptoms, and when patients with ischemic symptoms want medical attention, they are often sent to the hospital by a friend or family member and do not actively call 120 for ambulance assistance.9,14 Therefore, our study aims to identify the causes of delayed prehospital assistance and related measures to reduce the delayed assistance time.
In this study, analysis of the baseline data of both groups showed that females, history of diabetes, rural residence, and farmer's occupation were all factors influencing the delayed call of patients. Binary logistic regression analysis showed that women and their history of diabetes were independent influences on delayed calls in STEMI patients. In this study, through detailed questioning of patients’ basic conditions during hospitalization and retrospective analysis, the reasons affecting patients’ delayed call time for chest pain can be mainly summarized as follows: (1) Delayed call times are longer in women, more than twice as long as in men, possibly due to atypical symptoms and longer decision-making times. Atypical symptoms of myocardial infarction such as chest pain or nausea in the neck, throat, back, or shoulders are more than twice as common in women as in men. 16 In addition, the prevalence of fear that manifests in the face of physical discomfort among female patients motivates individuals to engage in defensive behaviors, including avoidance and is an important psychological factor associated with patient delay. 17 In a multivariate analysis it was noted that women had lower educational attainment than men and that this variable tended to be associated with longer prehospital delays in women, possibly due to women's lower socioeconomic status and lack of perception of the potential risk of acute coronary syndrome (ACS). 18 A large number of studies have shown significantly higher delayed call times in women with STEMI compared to men,7,19 consistent with our findings. (2) The type and severity of acute myocardial infarction symptoms depend on the activation of afferent neurons, which then transmit nerve impulses to the autonomic nervous system and induce symptoms. Patients with diabetes have a high prevalence of neuropathy and a high tolerance for chest pain disorders and do not present with typical symptoms (chest pain, sweating, and radiating chest pain) until the patient feels significantly uncomfortable and therefore does not seek medical help, thus leading to a prolonged delay in calling for chest pain. 20 Chowdhury et al 21 found that patients with acute myocardial infarction with atypical chest pain, diabetes mellitus, and prehospital delay were significantly associated. Another study in the Chinese acute myocardial infarction (CAMI) registry analysis found that patients with acute myocardial infarction combined with diabetes were less likely to experience persistent anterior chest pain, sweating, and fatigue than patients without diabetes, and patients in the diabetic group had a long time to visit the clinic compared to the non-diabetic group. 22 Sheifer et al 23 analyzed 102 399 patients with acute myocardial infarction and found that diabetes was an independent predictor of delayed treatment (OR: 1.11, 95% CI: 1.07-1.14). (3) Studies have shown that living in rural areas, difficulties in road transport (poor road conditions or high road traffic) and lack of accessibility are the reasons for long delays in prehospital treatment. 24 (4) Farmers have a relative shortage of education and lower socioeconomic status than workers, employees, retirees, and self-employed, while for patients with higher socioeconomic status earlier consultation findings reflect better medical information and greater health awareness. 25
In addition, the results of this study also concluded that delayed call time for chest pain >60 minutes, left main + 3 branch lesions, and cardiac function ≥ class III were all risk factors for cumulative morbidity and mortality in patients with AMI at 4 years after PCI. The analysis showed that the delayed call time of chest pain >60 minutes, left main + 3 branch lesions, and Killip class III regression coefficients of cardiac function were all greater than 1, with a relative risk of 4 or more, which had a greater impact on the risk of death. A Killip class IV regression coefficient of cardiac function greater than 2 and a relative risk of 19 or more have a greater impact on the risk of death and are more likely to affect the survival prognosis of patients. First, longer delays result in longer ischemic times, more myocardial injury, and adverse clinical outcomes, and reduce the effectiveness of reperfusion therapy, which is most beneficial for patients with the shortest delays. 26 Ayuna and Sultan 27 study shows higher mortality with longer delay regardless of age. Therefore, in addition to focusing on the timing of in-hospital treatment, the delayed call time for chest pain plays an important role in the rescue time and long-term prognosis of patients with acute myocardial infarction. The prolongation of the delayed call time for chest pain directly affects the actual myocardial ischemic time in each segment of SO-to-B. Therefore, the delayed call time for chest pain occupies a very important role in the whole rescue time for patients with acute myocardial infarction, and if patients and their families can effectively improve their awareness of myocardial infarction, a new level of rescue will be added for this disease. In addition, coronary angiography with STEMI showed that multivessel disease was associated with a poorer prognosis, including lower reperfusion success and higher risk of adverse cardiac events and death, compared with single coronary lesions. 28 Cardiogenic shock remains the leading cause of in-hospital death in patients with STEMI, and its causative mechanisms involve decreased coronary perfusion pressure and reduced ventricular pumping, resulting in reduced cardiac output or inadequate target organ perfusion, leading to multiple organ dysfunction syndrome (MODS) or systemic inflammatory reactive syndrome (SIRS). 29 Hou et al 30 found that cardiac function Killip class III-IV was associated with long-term survival in patients with STEMI, which is consistent with our study. Mizuguchi et al 31 found a strong correlation between cardiogenic shock and survival of STEMI patients after PCI. Therefore, medical personnel and grassroots workers should vigorously promote the early symptoms and risk factors of myocardial infarction, so that people can achieve early prevention, early detection, and early treatment and improve their quality of life. In addition, the delayed call time for chest pain in this study was bounded by 60 minutes, and the ROC curve was established to assess the occurrence of MACE, and its predictive degree AUC area was 0.59, which has some value.
In conclusion, this study retrospectively analyzed the data of 398 STEMI patients treated with PCI in Fuyang People's Hospital and evaluated the influencing factors affecting the delayed call time for chest pain and the prognosis of patients after PCI. The results of this study showed that a history of diabetes mellitus and female were independent risk factors for prolonged delayed call time for chest pain, and delayed call time for chest pain >60 minutes, left main + 3 branch lesions, and cardiac function ≥ class III were all risk factors for cumulative morbidity and mortality in STEMI patients at 4 years after PCI. These findings provide a reference for shortening the delayed call time of chest pain in STEMI patients, reducing the rescue time of STEMI patients, reducing the MACE and morbidity and mortality rate of patients, and improving the long-term prognosis of patients. Shortcomings of this study: The longest follow-up period of this study was 4 years, and further extension of the follow-up period is still needed; this study is a single-center study with a small sample size, which may affect the results and conclusions. No information is provided on other factors that may influence seeking medical care such as the presence of a caregiver, availability of transportation and/or communication methods to activate emergency medical response, etc.
Supplemental Material
sj-xlsx-1-cat-10.1177_10760296231186811 - Supplemental material for Prognosis Analysis of Delayed Call Time for Chest Pain in Patients With Acute ST-Segment Elevation Myocardial Infarction Undergoing Direct Percutaneous Coronary Intervention
Supplemental material, sj-xlsx-1-cat-10.1177_10760296231186811 for Prognosis Analysis of Delayed Call Time for Chest Pain in Patients With Acute ST-Segment Elevation Myocardial Infarction Undergoing Direct Percutaneous Coronary Intervention by Yangyang Yang, MM, Yuanzhuo Zhang, MM, and Lei Ren, MM in Clinical and Applied Thrombosis/Hemostasis
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Anhui Medical University Research Fund Project Grant, Scientific Research Program of Fuyang Science and Technology Bureau, Anhui Province (grant numbers 2022xkj226, FK202081001).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
