Abstract
Neutrophils and lymphocytes (N/L) ratio and carotid intima–media thickness (C-IMT) value have been studied as new predictors of cardiovascular risk. We aimed to investigate N/L ratio and C-IMT value in patients with cardiac syndrome X (CSX) and compare patients with coronary artery disease (CAD) and normal participants. A total of 288 participants were enrolled in the study. The N/L ratio and C-IMT value were compared among the 3 groups. There were no statistically significant differences in N/L levels between CSX and CAD groups. The N/L ratio was found significantly increased in patients with CSX and CAD, compared to the control group. Patients with CAD and CSX had significantly higher C-IMT value compared to control participants. Significant positive correlation was found between C-IMT value and plasma level of N/L ratio. The relationship among CSX and higher N/L ratio level and C-IMT suggests that endothelial dysfunction may contribute to the etiopathogenesis of the CSX.
Introduction
Cardiac syndrome X (CSX) is a clinical entity that should be separated from typical obstructive coronary heart disease. The 3 characteristic features of CSX are angina or angina-like chest pain with exertion, ST-segment depression on treadmill exercise testing or pathological thallium scan and normal coronary arteriography, and no spontaneous or inducible epicardial coronary artery spasm on ergonovine or acetylcholine provocation. 1 Several studies have demonstrated that alterations of coronary microcirculation may induce myocardial ischemia. 2 Hence the term syndrome X, first introduced by Kemp et al in 1973 to define this clinical entity. 3 Although the exact mechanisms leading to CSX are not clear up to now, silent atherosclerosis and endothelial vasomotor dysfunction have been suggested as possible responsible factors.
The total white blood cell count (WBC) and its subtypes, neutrophil to lymphocyte (N/L) ratio, can be used as an indicator of systemic inflammation. 4 The N/L ratio has been demonstrated to have the greatest predictive power of death, myocardial infarction, and high risk for coronary artery disease (CAD). 5 In patients submitted for angioplasty, the N/L ratio is an independent predictor of long-term mortality. 6 Carotid intima–media thickness (C-IMT) is a marker of systemic inflammation, and it is widely used as a prominent marker for cardiovascular diseases. 7 To the best of our knowledge, there is no study regarding the assessment of N/L ratio and C-IMT in patients with CSX in the literature. From that point of view, we aimed to evaluate the levels of N/L ratio in patients with CSX and compare patients with CAD and normal control participants. We also investigated the relationship between C-IMT and N/L ratio based on inflammatory activity.
Methods
Patient Selection
A total of 1725 patients undergoing diagnostic coronary angiography, between August 2011 and July 2012, in a tertiary referral center were examined prospectively. Of all, 288 patients were enrolled into the current study, and they were divided into 3 groups. The CSX group consisted of 92 participants (47 men and 45 women, mean age = 48.4 ± 9.5 years). The diagnosis of CSX was based on the presence of a typical exercise-induced angina pectoris associated with either transient ischemic ST segment depression (≥1 mm) during the treadmill exercise test (54 patients) or reversible perfusion defect on myocardial perfusion scintigraphy (38 patients) with angiographically normal coronary arteries in the absence of coronary artery spasm (determined by hyperventilation maneuver). The CAD group consisted of 97 participants (51 men and 46 women, mean age = 51.3 ± 8.9 years) with newly diagnosed CAD defined as ≥50% stenosis in at least 1 epicardial coronary artery. The control group consisted of 99 age- and sex-matched individuals (49 men and 50 women, mean age = 47.2 ± 9.0 years) with anginal chest pain but a normal coronary angiography, without any sign of inducible ischemia on myocardial perfusion scintigraphy or treadmill exercise test. The institutional ethics committee approved the study protocol, and the study was conducted in accordance with the Declaration of Helsinki. All the participants were evaluated by detailed medical, physical examination, and biochemical analysis. Special emphasis was put on cardiovascular risk factors and diseases. All participants were questioned for any cardiovascular drug use, smoking habit and alcohol consumption, and underwent transthoracic echocardiography for analysis of structural heart disease. Image acquisition was performed in the left lateral decubitus position using a Philips IE 33 6.0 equipped with a 2.5-MHz transducer.
Exclusion criteria were defined as refusal to participate in the study, hypertension, presence of anemia, diabetes mellitus, left ventricular dysfunction (left ventricular ejection fraction <50%) or hypertrophy, acute coronary syndromes, valvular heart disease, congenital heart disease, any abnormality in thyroid function tests, renal or hepatic dysfunction (creatinine >1.5 mg/dL, aspartate aminotransferase, and alanine transaminase more than twice the upper limit of normal, respectively), inflammatory diseases, and any medication that can potentially interfere with the measurement of N/L ratio.
Cardiac Catheterization
Coronary angiograms were performed with a femoral approach using the Judkins technique without the use of nitroglycerin, adenosine, or a calcium channel blocker. All patients in the study population underwent elective coronary artery angiography using Siemens Axiom Artis DFC (Siemens Medical Solutions, Erlangen, Germany) following appropriate patient preparation. Coronary angiograms were judged with regard to smooth appearance, luminal wall irregularities, epicardial local or diffuse caliber reduction, and stenosis. Coronary arteries were classified as normal on the basis of visual assessment of the absence of any luminal irregularities. To exclude the possibility of coronary artery vasospasm, during coronary arteriography, the patients with normal coronary artery underwent a hyperventilation test that was performed by asking the patients to breathe quickly and deeply for 5 minutes.
Biochemical Measurements
Blood samples were withdrawn without stasis, in the morning of the day before coronary angiography and following a fasting period of 12 hours. Glucose, creatinine, and lipid profile were determined by standard methods. In all groups, we measured N/L ratio after the venipuncture of blood samples collected in tripotassium EDTA (7.2 mg) tubes at the same time. These blood samples were analyzed in 2 hours after vein puncture using an automatic blood counter (Sysmex SE 9500, Roche). Hematological parameters, including hemoglobin (Hb), WBC count, and platelet count, were also analyzed by standard methods.
Carotid Ultrasonography
All patients were evaluated by high-resolution ultrasound using the Philips IE 33 6.0 equipped with a L 11-3 broadband linear array transducer. The transducer was manipulated so that the near and far walls of the common carotid artery (CCA) were parallel to the transducer footprint, and the lumen diameter was maximized in the longitudinal plane. A region 1 cm proximal to the carotid bifurcation was identified, and the IMT of the far wall was evaluated as the distance between the lumen–intima interface and the media–adventitia interface. The IMT measurement was obtained from 4 contiguous sites at 1-mm intervals, and the average of the 4 measurements was used for analyses. After the measurements were taken from both right and left CCAs, the average of both values was calculated. All measurements were made manually on still images obtained during the sonographic scanning. The carotid plaques were excluded while measuring IMT.
Statistical Analysis
Statistical Package for the Social Sciences statistical software package version 15 for Windows (Statistical Package for the Social Sciences, Chicago, Illinois) was used for statistical analyses. Continuous variables were given as mean ± standard deviation, and categorical variables were defined as percentage. Data were tested for normal distribution using the Kolmogorov-Smirnov test. To compare continuous variable, 1-way analysis of variance test or Kruskal-Wallis test was used as appropriate. When a significant difference was observed between 3 groups, post hoc (Tukey test or Mann-Whitney U test) test was used for the determination of difference between couples. Pearson correlation test was used to evaluate the degree of association between the examined variables. To compare the categorical variables, chi-square test was used. Statistical significance was defined as P < .05.
Results
The main characteristics of the study population are given in Table 1. Age, sex, smoking, and alcohol consumption were not different between the 3 groups. Body mass index, lipid profiles, and fasting glucose levels were not different between the 3 groups (Table 1). There were no statistically significant differences in N/L ratio between CSX group and CAD group (P = .13; Figure 1). The N/L ratio was found to be significantly higher in both CSX and CAD groups compared to that of control group (P < .05; Figure 1). In the patients groups, patients with CAD and CSX had significantly higher C-IMT compared to control participants (P < .05; Figure 2 and Table 2). There were no statistically significant differences in C-IMT between CSX group and CAD group (P = .10; Figure 2). According to the correlation analysis, there were significantly positive correlations between C-IMT and plasma level of N/L ratio (P < .01 and r = .87; Figure 3). Hematological parameters, including Hb, WBC, and platelet count, were not statistically significantly different in among the 3 groups (Table 2).
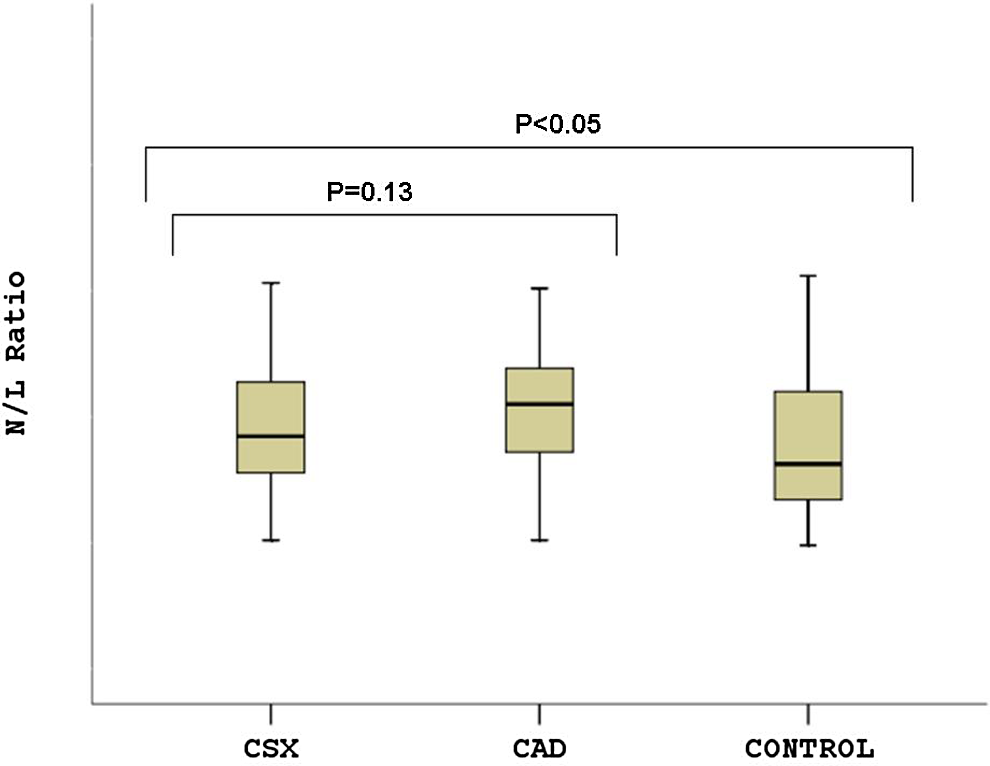
Neutrophils and lymphocytes ratio was significantly higher in both cardiac syndrome X and coronary artery disease groups compared to that of control group.
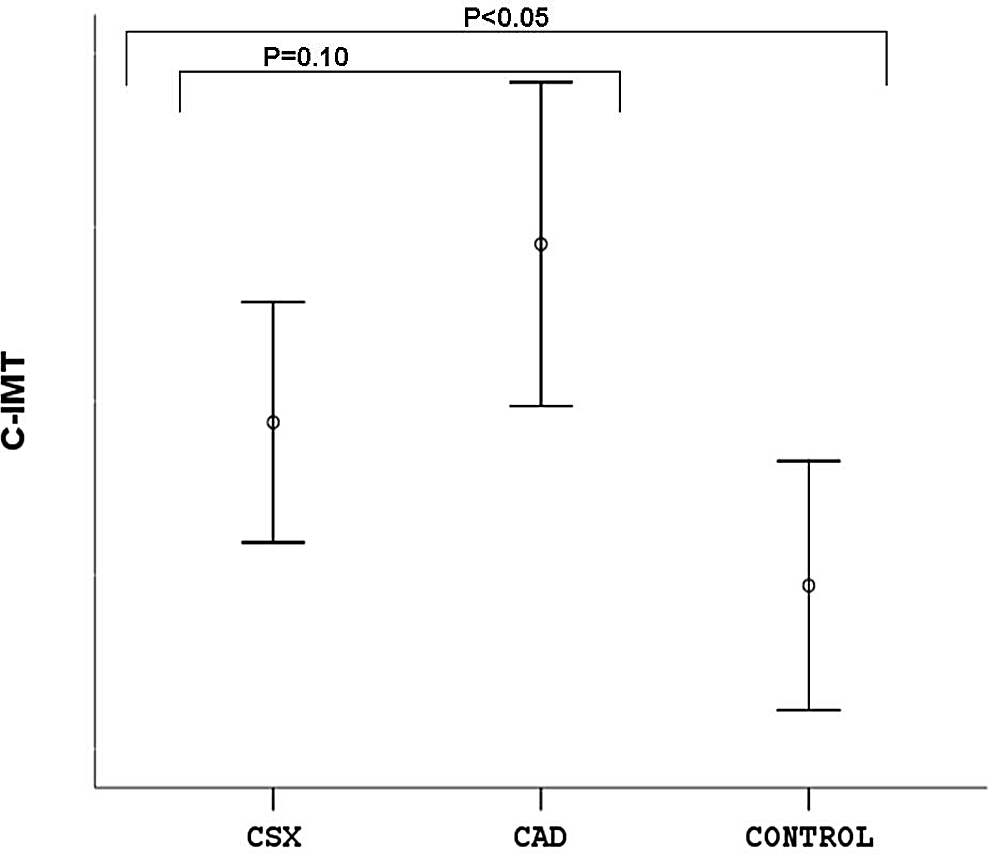
Coronary artery disease and cardiac syndrome X groups had significantly higher carotid intima–media thickness compared to that of control group.
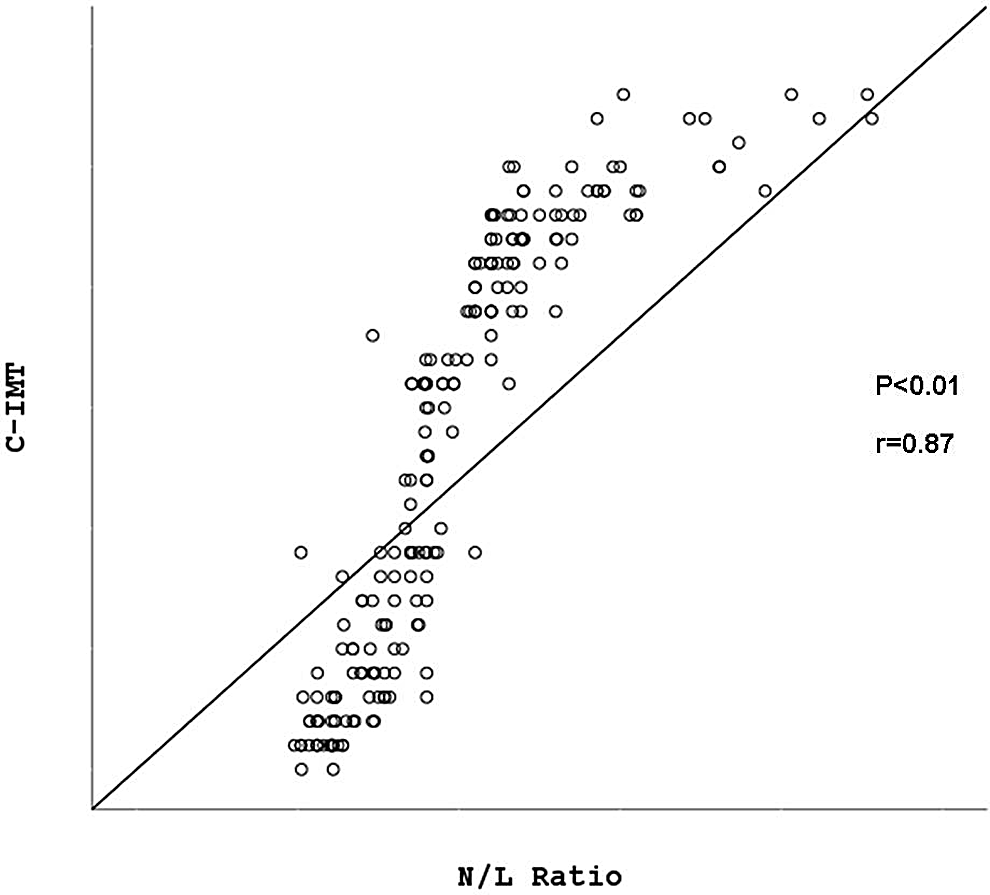
Correlations between carotid intima–media thickness and plasma level of neutrophils and lymphocytes ratio.
Baseline Clinical and Biochemical Characteristics of the Study Groups.a
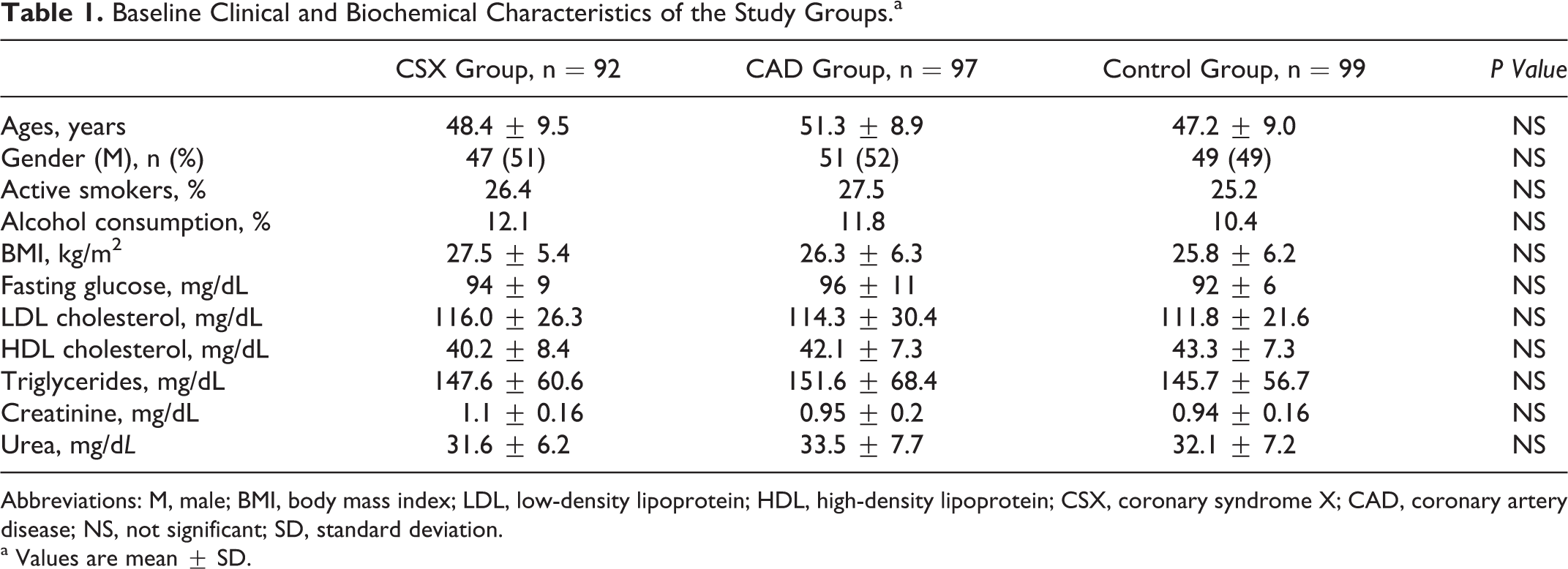
Abbreviations: M, male; BMI, body mass index; LDL, low-density lipoprotein; HDL, high-density lipoprotein; CSX, coronary syndrome X; CAD, coronary artery disease; NS, not significant; SD, standard deviation.
a Values are mean ± SD.
Comparison of the Neutrophils and Lymphocytes Ratio, Carotid Intima–Media Thickness, and Other Parameters Among the Study Groups.a
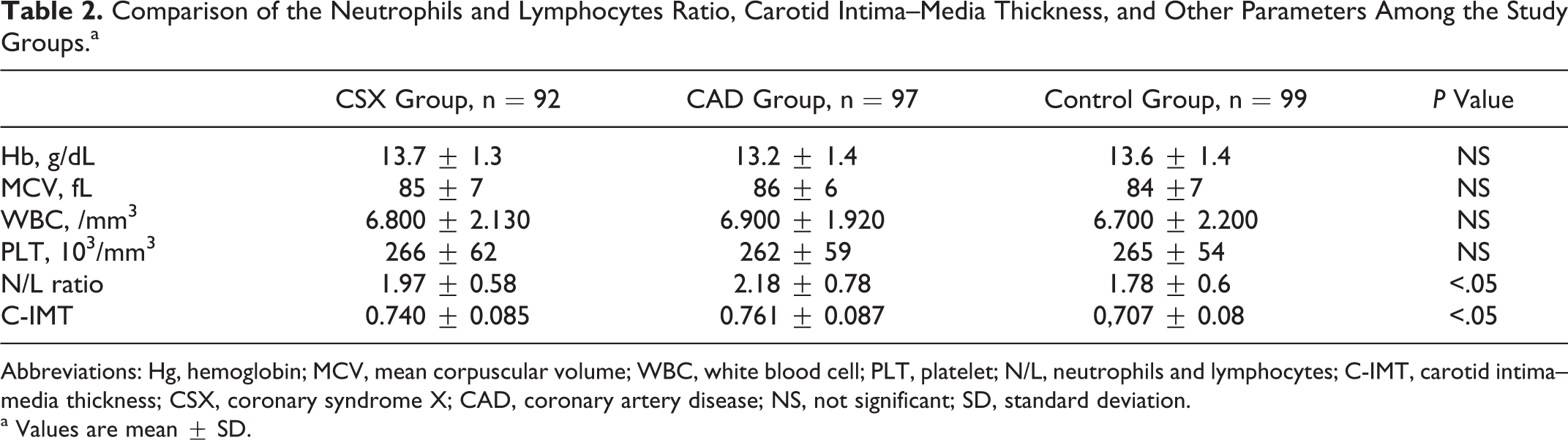
Abbreviations: Hg, hemoglobin; MCV, mean corpuscular volume; WBC, white blood cell; PLT, platelet; N/L, neutrophils and lymphocytes; C-IMT, carotid intima–media thickness; CSX, coronary syndrome X; CAD, coronary artery disease; NS, not significant; SD, standard deviation.
a Values are mean ± SD.
Discussion
In the present study, we have found that N/L ratio and C-IMT levels are significantly higher in both CSX and CAD groups compared to those of control participants. Besides, there were positive correlations between C-IMT and plasma level of N/L ratio. These results may indicate that elevated serum N/L ratio may be associated with the ongoing inflammation and silent atherosclerosis in the pathophysiology of CSX.
The pathophysiology of CSX has not been clearly identified yet, although multiple abnormalities including abnormal coronary flow reserve, insulin resistance, abnormal autonomic control, enhanced sodium hydrogen exchange activity, abnormal cardiac sensitivity, microvascular spasm, endothelial dysfunction, oxidative stress, and silent atherosclerosis have been reported. 8 Previous studies have demonstrated that elevated levels of inflammatory molecules are markers of atherosclerotic disease activity and also indicate an increased risk of the progression of atherosclerosis. 9 Inflammation has been shown to be associated with endothelial dysfunction and silent atherosclerosis in patients with CSX. Increased concentrations of circulating C-reactive protein (CRP) correlate with vascular abnormalities in patients with CSX. 10,11 Atmaca et al 12 showed that high-sensitivity (hs)-CRP and WBC count were higher in patients with CSX than in control participants. The increased levels of hs-CRP and WBC count may suggest that these markers may be used in clinical practice for the assessment of the inflammatory status of CSX.
Leukocyte subtype and N/L ratio are also the indicators of systemic inflammation. 13 –15 These markers have prognostic importance in cardiovascular disease. The relation between atherosclerosis progression and leukocyte subtype was evaluated in previous study. Progression rate was significantly high in patients with high N/L ratio, and N/L ratio was a predictor of progression of atherosclerosis. 16 More recently, N/L ratio has been proposed as a useful biomarker to predict cardiovascular risk. 17,18 Zazula et al investigated the relation between N/L ratio and the patient with suspicion of acute coronary syndrome. The N/L ratio was found to be significantly higher in patients with unstable angina, ST-segment elevation myocardial infarction (STEMI), and non-STEMI groups than in the patients diagnosed with noncardiac chest pain. 19 The N/L ratio has been associated with poor outcomes in patients who underwent coronary angiography. The maximum value of N/L ratio is a useful marker to predict subsequent mortality in patients admitted for STEMI. 20 The N/L ratio was a strong independent predictor of long-term mortality after ST elevation myocardial infarction treated with early revascularization. 21 In-hospital major adverse cardiac events were significantly higher in patients with no reflow, and there was a significant and positive correlation between hs-CRP and N/L ratio. 22 Gibson et al 23 investigated the leukocyte subtypes such as the N/L ratio in patient undergoing coronary artery bypass graft (CABG). An elevated N/L ratio is associated with a poor survival after CABG. 3 Because of all these interactions, etiology of the relationships between N/L ratio and CSX may be inflammation and oxidative stress. Therefore, we aimed to investigate N/L ratio in patients with CSX compared to patients with CAD and normal participants.
With the growing understanding of the role of inflammation in the pathogenesis of CSX, researchers have focused on C-IMT and other inflammatory markers for the evaluation of this disease. 24 Both C-IMT and other inflammatory markers are higher in the CSX compared to those of control participants. 25 Measurements of C-IMT using ultrasound assess the extent and the severity of systemic atherosclerosis. It has been shown that there is a direct relationship between C-IMT and clinical cardiovascular disease. 26 Due to these data, C-IMT assessment that is a strong inflammatory marker can be used to document regression or progression of atherosclerosis, and it can be used to correlate with the other newly inflammatory markers such as N/L ratio. 7 In our study, C-IMT was significantly increased in patients with CSX. There were significantly positive correlations between C-IMT and plasma level of N/L ratio in our study. It suggests that endothelial dysfunction may modulate the effect of CSX risk factors and promote endothelial dysfunction and intima–media thickening.
Conclusion
We have shown for the first time that patients with CSX and CAD have higher N/L ratio compared to control participants. We also found significantly positive correlations between C-IMT and plasma level of N/L ratio. The relation between CSX and higher N/L ratio suggest that, besides endothelial dysfunction, silent atherosclerosis may also contribute to the etiopathogenesis of the CSX phenomenon similar to CAD. However, large-scale prospective clinical studies are needed to prove that hypothesis.
Study Limitations
The major limitation of our study was the comparatively small size of the study population. Another limitation was the possibility of any underlying coronary artery spasm in patients with CSX, which was ruled out by a hyperventilation test despite the superiority of the ergonovine test. On the other hand, we did not analyze markers of inflammation such as CRP in the current study although the role of inflammation was previously reported in those patients. We did not have the opportunity to perform intravascular ultrasound (IVUS) in spite of the fact that IVUS provides more precise values about the presence and distribution of atherosclerosis in vessel lumen and throughout the wall. Finally, there are a lot of different pathophysiologic mechanisms involved in endothelial dysfunction (ED), preventing us from examining CSX and ED appropriately. Therefore, we have to exclude a number of patients and make a very homogenous group.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
