Abstract
In this study, we validated a thromboelastography (TEG) method to evaluate the hemostatic effects of 3 peptides. The first peptide is an ideal amphipathic peptide composed of 22 leucine and lysine in a ratio of 2:1. At a very low concentration, the peptide had a procoagulant effect shown by decreases in reaction time (R) and coagulation time (K) but was impaired by a decrease in maximum amplitude (MA). At higher concentrations, the peptide had an anticoagulant effect. The α angle was minimally affected by the peptide. The second peptide is melittin derived from bee venom. Melittin showed procoagulant effects reflected by a decrease in clotting time but led to lower MA. The third peptide derived from fibrinogen γ chain promoted hemostasis only at an optimal concentration and became anticoagulant at a higher concentration. The hemostatic mechanisms of each peptide were discussed. Our study would facilitate further development of peptides for either hemorrhage control or thrombosis treatment.
Introduction
Hemorrhage is the leading cause of death on the battlefield and the second leading cause of death in civilian trauma.1,2 The latest statistics from the Iraq wars show that approximately 90% of combat deaths among potentially preventable casualties are contributable to uncontrolled hemorrhage, and a little more than half of those are caused by noncompressible (torso) hemorrhage. 3
We are interested in developing a material-based method for mitigating noncompressible hemorrhage sustained by frontline casualties on the battlefield. Specifically, considering the coagulation system consists of blood and blood vessels, it is desirable to develop a sprayable biomaterial that can promote blood coagulation and create a seal on damaged blood vessels of wounds that are not compressible. Previously, we have reported a number of in situ-forming hydrogels that may be injected/sprayed to fill any shapes of deep, cavity wounds, and to deliver and retain hemostatic agents at the bleeding sites. 4 Such hydrogels can be designed for topical applications to both external and internal bleeding tissues. To improve its effectiveness, we need to incorporate other components that can activate blood coagulation pathways. Although certain coagulation factors have been used to promote extrinsic and intrinsic blood coagulation, they are very large molecules and may lose their functions when incorporated into our hydrogel materials.
Peptides have broad biomedical applications ranging from therapeutic drugs to tissue engineering. 5 Compared to their counterpart proteins, peptides are stable and can be chemically synthesized to avoid biological contamination. The therapeutic use of peptides includes cancer and antibacterial treatment. 6 A number of peptide-based hemostatic vasoactive drugs are under development for treating hemorrhage.7,8 A self-assembling peptide has been reported to result in complete hemostasis immediately when applied in a solution directly to wounds in the brain, spinal cord, femoral artery, liver, or skin of hamsters. 9
In particular, we investigated 3 peptides. The first one is an “ideal amphipathic peptide (IAP),” a synthetic amphipathic peptide with an “ideal” helical structure composed of leucine and lysine in a ratio of 2:1. The second one is a natural peptide called “melittin.” It is a 26-amino acid peptide with the sequence NH2-GIGAVLKVLTTGLPALISWIKRKRQQ-CONH2 and is the main constituent of bee venom, comprising about 50% of its dry weight. 10 The amphipathic helical nature of the 2 peptides can be exploited by self-assembly to construct supramolecular architectures through a combination with synthetic polymers,11,12 leading to another mechanism for hemostatic effects. The third one is a “γ peptide,” derived from fibrinogen γ chain: a 19-amino acid peptide comprising the sequence TIGEGQQHHLGGAKQAGDV. Recently, the changes of fibrin formation and proteolysis induced by different segments of the peptide have been reported. 13 It is expected that our hydrogels and peptides can synergistically function well for hemorrhage control.
Although the promotion of blood coagulation is desirable for our applications, such as hemorrhage control in trauma and surgical injuries,14,15 it is noteworthy that anticoagulants are also needed for the treatment of certain cardiovascular diseases. 16 Therefore, it is desirable to develop both the peptide-based pro- and anticoagulants for different applications.
A number of in vitro tests have been reported for assessing hemocompatibility on biomaterials. However, these tests are mainly concerned with the effects of solid materials on different parts of the coagulation system, such as thrombus formation and platelet functions, and emphasized on material surface-blood interaction phenomena,17,18 but they are not suitable for testing biomaterials soluble in blood. It is also difficult to relate the findings from such tests to overall effects on whole blood, as actually occurs in clinical settings.
In contrast, thromboelastography (TEG) is a useful measure of global hemostasis, from the beginning of coagulation through clot formation to the ending with fibrinolysis (Figure 1).19–21 It provides the information about the hemostatic properties of tested materials through the measurement of the following parameters: reaction time ([R] time to first clot formation), which is related to plasma clotting factors and circulating inhibitory activity; coagulation time ([K] rate of clot strengthening), which is associated with the activity of the intrinsic clotting factors, fibrinogen and platelets; maximum amplitude ([MA] maximum strength of the clot), which is a direct function of the maximum dynamic properties of fibrin and platelet number and functions; and rate of clot polymerization; α angle, which is a main function of platelets, fibrinogen, and plasma components residing on the platelet surface. It may also identify the relative contributions of clotting factors, such as fibrinogen and platelets, to the overall coagulation process. 22
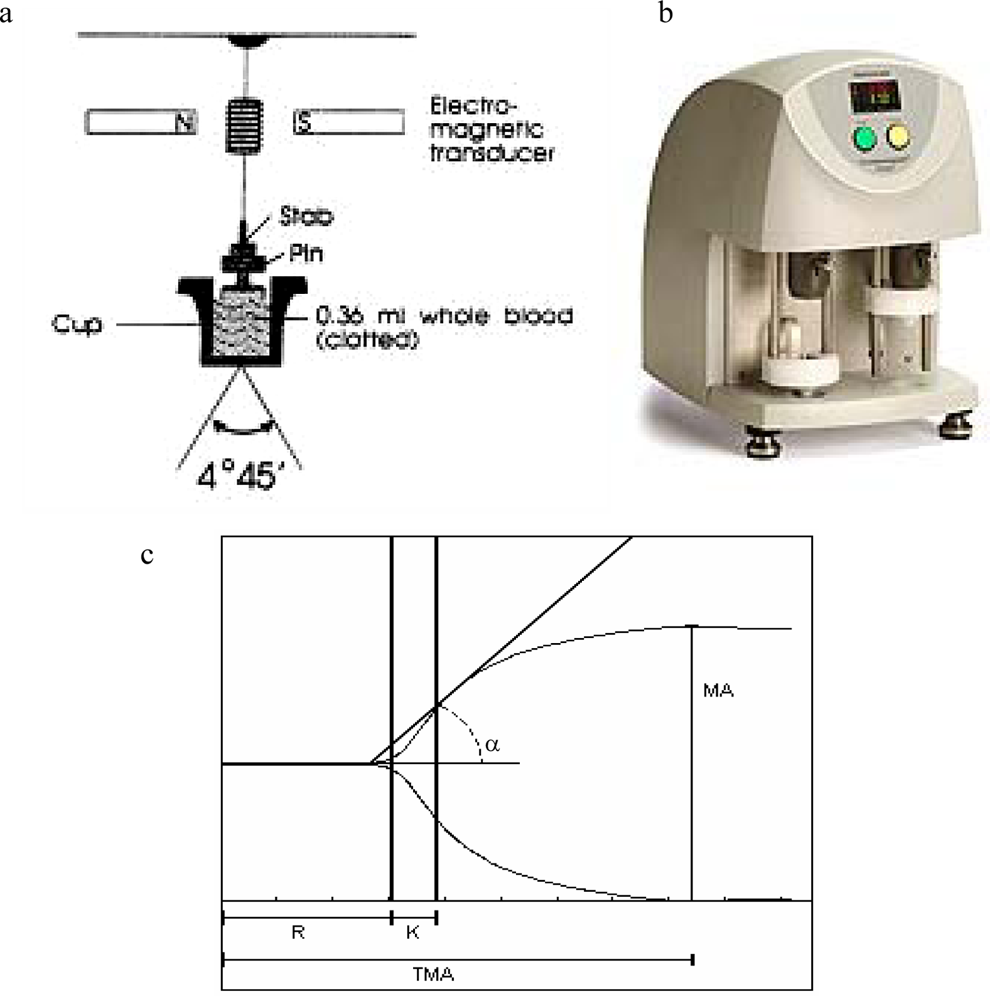
Schematic illustration of (A) TEG mechanisms, (B) the TEG machine, and (C) a representative TEG tracing showing the relationship between the qualitative tracing and the quantitative parameters. TEG indicates thromboelastography.
In this study, we successfully applied a TEG method to assess the effects of different blood-soluble hemostatic agents including our novel peptides on blood coagulation. This represents the first report on the application of TEG for the study of the effects of a series of hemostatic peptides on whole-blood coagulation. This study may lead to the development of new material-based methods for hemorrhage control.
Materials and Methods
Activated human coagulation factor VIIa in Tris buffer (1.45 mg/mL) was purchased from Enzyme Research Laboratories (South Bend, Indiana). Ideal amphipathic peptide with >90% purity was synthesized by the Alberta Peptide Institute (Edmonton, Alberta, Canada). Fibrinogen γ peptide comprising the sequence TIGEGQQHHLGGAKQAGDV was custom synthesized using a standard solid-phase method by Advanced Protein Technology Center at The Hospital for Sick Children (Toronto, Ontario, Canada). The peptide was cleaved with trifluoroacetic acid and confirmed by Matrix-assisted laser desorption/ionization mass spectrometry (MALDI MS) and purified by high-performance liquid chromatography ([HPLC] purity, >85%). Bovine albumin and melittin with >90% purity were purchased from Sigma-Aldrich (Mississauga, Ontario, Canada). Other chemicals were of American Chemical Society (ACS) grade and were used as received.
Thromboelastography
In our study, to evaluate the potential hemostatic peptides, human coagulation factor VIIa and bovine albumin were used as a positive and a negative control, respectively. Each solution of peptides and controls in a pH 7.4 Tris buffer was measured by TEG. Specifically, with the approval by the local research ethics committee and patient consent, blood samples were taken from healthy volunteers via venipuncture and collected into separate Vacutainers (Fisher Scientific, Nepean, Ontario, Canada) containing 0.109 mol/L sodium citrate solution (citrate:blood volume = 1:9) and gently inverted 3 times. The citrated whole blood was stored at room temperature for at least 30 minutes prior to TEG analysis, since it has been consistently documented that a sample stored for <30 minutes is not stable.23–25 Thromboelastographic measurements were carried out using a computerized TEG Hemostasis System 5000 (Haemoscope Corporation, Niles, Illinois). After the system had passed the electronics testing and quality control according to the manufacturer’s protocol, a peptide solution (20 μL) prepared at different concentrations in the Tris buffer was loaded into a TEG cup prewarmed to 37°C. An aliquot of 20 μL of 0.2 mol/L calcium chloride solution and 320 μL of blood were then added into the TEG cup. The measurement was started immediately after uniformly mixing the whole solution by pipetting in and out once. Thromboelastography was also conducted after mixing the pH buffer and 0.2 mol/L calcium chloride solution at 20 μL each with 320 μL citrated human blood, following the same procedure to take into account any hemodilution effects on blood coagulation. Analysis was run until all interested parameters (ie R, K, α, MA, and Time to MA [TMA]) were finalized. Thromboelastography study on melittin was also carried out using the same procedure on platelet-rich plasma (PRP) and platelet-poor plasma (PPP), which were obtained by centrifuging the citrated whole blood at 240 g and 2500 g for 10 minutes, respectively. 26
Hemolysis
Red blood cells (RBCs) were isolated by centrifuging the blood samples from healthy volunteers for 10 minutes at 6000 rpm and extracting the supernatant from each tube. The RBCs were washed 3 times with phosphate buffer saline (PBS), pH 7.4, and suspended in PBS (final 5% volume/volume [v/v]). A peptide solution was added to RBC suspension to yield a final volume of 120 μL (final RBC concentration, 2.5% v/v) and a peptide concentration of 30 µmol/L for IAP and 40 µmol/L for melittin. The mixture was incubated at 37°C for 1 hour and centrifuged for 5 minutes at 2500 rpm. The supernatant was extracted and diluted with PBS 10 times. Its absorbance was measured at 540 nm by UV-Visible spectrophotometer (Agilent Technologies Canada Inc, Mississauga, Ontario, Canada). For the positive control of 100% hemolysis, 1% v/v Triton X-100 was used to suspend the RBC. For negative control, RBC suspended in PBS was used. Both positive and negative controls had a final RBC concentration of 2.5% v/v. Percentage of hemolysis was calculated using the following equation: % hemolysis = [(A sample − Aneg)/(Apos −Aneg)] × 100%, where Asample, Aneg, and Apos are the absorbance of the sample, negative and positive controls, respectively.
Data Analysis
Data were presented as mean ± standard error of mean (SEM) and compared using a 2-tailed t test with 95% confidence to identify significantly different groups.
Results
Factor VIIa and Albumin
Figure 2A shows the TEG profiles as a function of factor VIIa concentration in the blood. It indicates a sharp decrease in R time by more than 70%, at concentrations from 0.032 to 0.32 μmol/L, followed by a gradual decrease of about 90% at 1.7 μmol/L. Thromboelastography α values displayed an even larger increase by more than 100%, but the increase reached a plateau between 0.32 and 1.7 μmol/L. There is a minimal but statistically significant increase by 10% in MA. The most significant changes are observed in α, followed by changes in R time, K time, and MA. The pattern of TEG changes suggests activations of coagulation factors and platelets. While factor VIIa showed a dose-dependent effect on blood coagulation, consistent with the in vitro effects as reported in the literature,22,27,28 albumin showed no appreciable changes in the TEG parameters from the blank (Figure 2B).
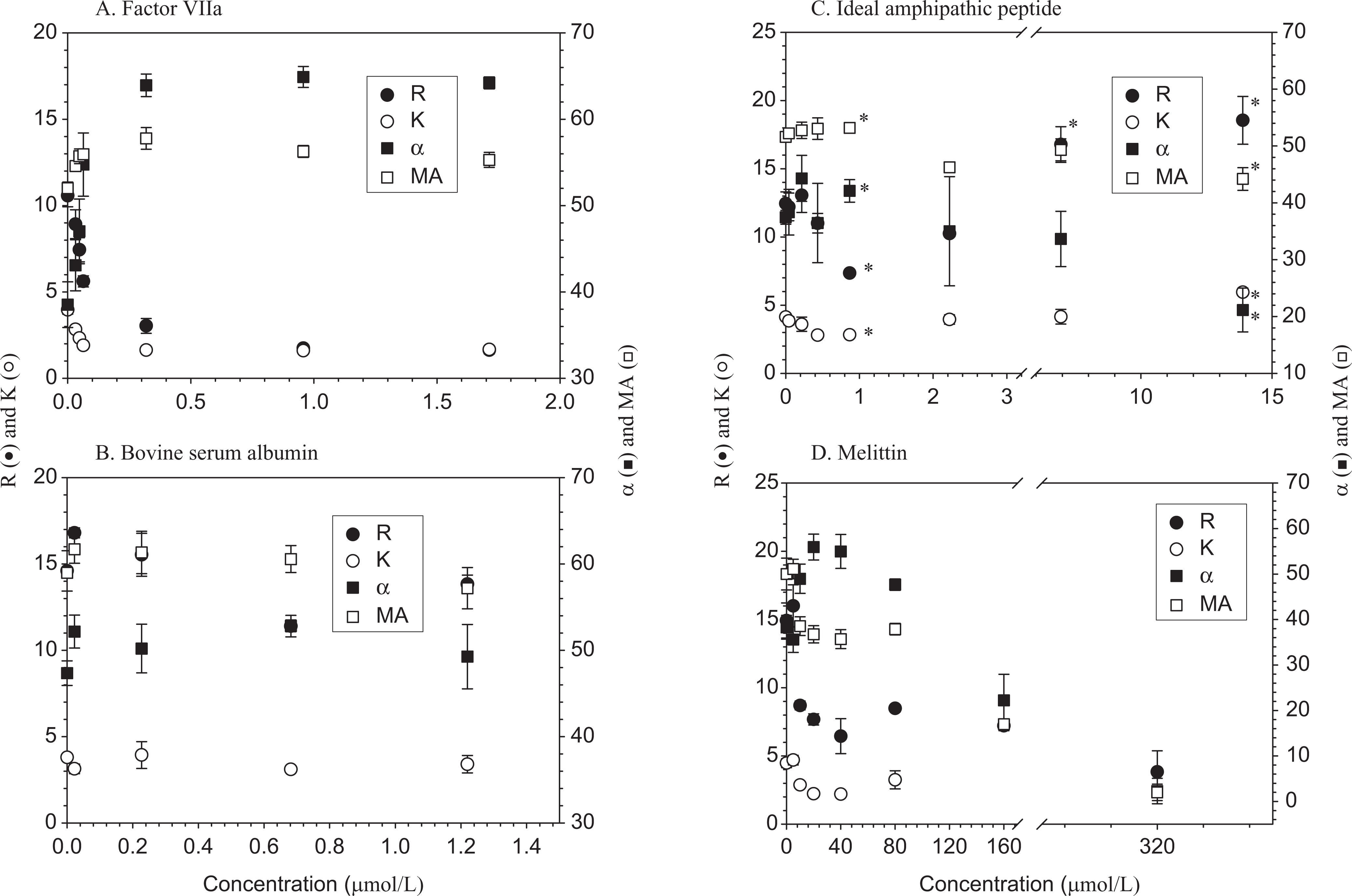
Dose-response curves of (A) human plasma-derived factor VIIa (molecular weight, 47 000); (B) bovine serum albumin (molecular weight, 66 000); (C) ideal amphipathic peptide (IAP); (D) melittin. Data are expressed as mean ± standard deviation ([SD]n = 4 except n = 3 for albumin). *Different from blank (P < .05).
Therefore, we have confirmed that our method was able to show hemostatic activities of factor VIIa in citrated whole blood with respect to the changes in TEG variables, in a clear dose-dependent manner. We then applied the established operating procedure to assess 3 different peptides.
Ideal Amphipathic Peptide
The effects of IAP supplementation on multiple thromboelastographic variables were examined as a function of its concentration, ranging from 0.038 to about 14 μmol/L. Figure 2C shows that the peptide generally slowed down clot formation in a prolonged R and K, and decreased MA, reflecting anticoagulation effects, except for a shorter R and K at a very low concentration below 1 μmol/L. The rate of clot formation, as measured by the α angle, was not significantly altered in the presence of the peptide (Figure 2C). The anticoagulant effects were increased with the peptide concentration.
Melittin
Our TEG results showed shortened R and K for the blood spiked with melittin solutions in a Tris buffer (pH 7.4) at final concentrations ranging from 5 to 320 μmol/L (Figure 2D). The procoagulant effects were also implied by an increase in α. On the other hand, melittin decreased MA. An increase in the peptide concentration increased its effects on blood coagulation as indicated by the 4 TEG parameters.
Table 1 summarizes that melittin caused 99.5% ± 1.4% hemoglobin release at the concentration of 40 μmol/L relative to Triton X-100. In contrast, IAP resulted in minimal hemolysis and instead prevented it. Figure 3 shows a fair correlation between the hemolysis and the initial coagulation time and maximum clot strength of whole blood mixed with melittin at different concentrations ranging from 5 to 40 μmol/L. Both R and MA values decrease with increasing hemolysis.
Hemolysis of IAP and Melittin on Red Blood Cells b
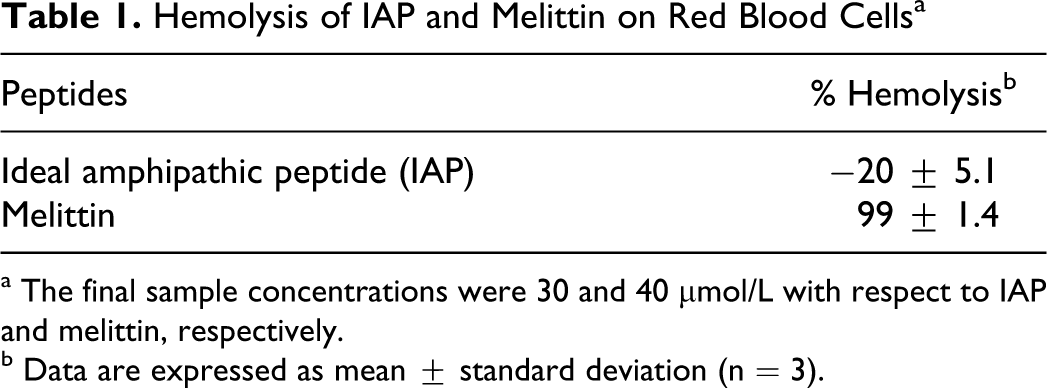

a The final sample concentrations were 30 and 40 μmol/L with respect to IAP and melittin, respectively.
b Data are expressed as mean ± standard deviation (n = 3).
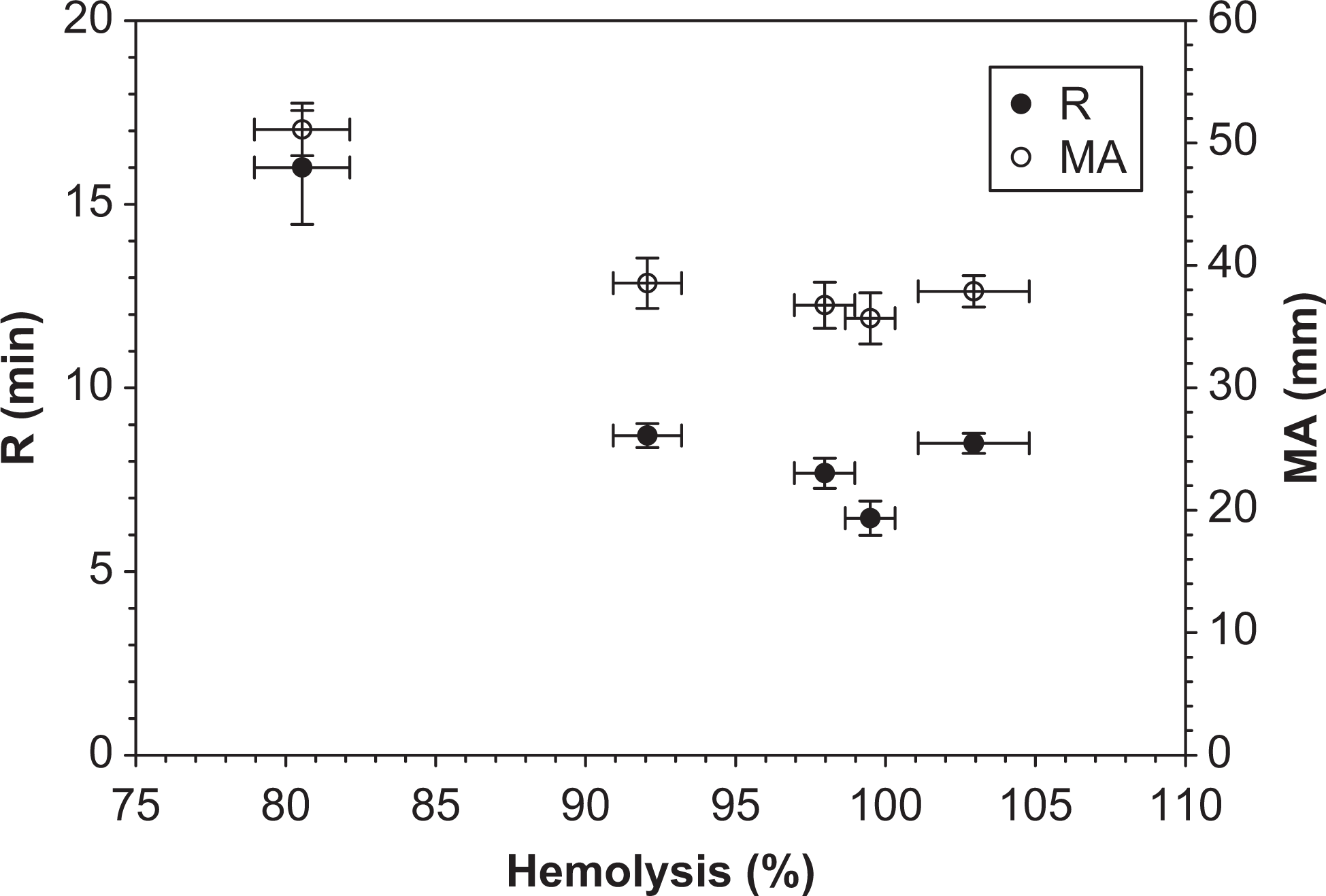
Correlation between hemolysis and blood coagulation. Data represent mean ± standard deviation (n = 3).
Figure 4 shows different effects of melittin on all main blood components (blood cells, platelet, and plasma proteins). Specifically, melittin significantly reduced R and MA (ie, the onset time of clot formation and maximum clot strength) of the whole blood, but exhibited no effects on PRP. Moreover, melittin caused an increase in R and no changes in MA of the PPP.
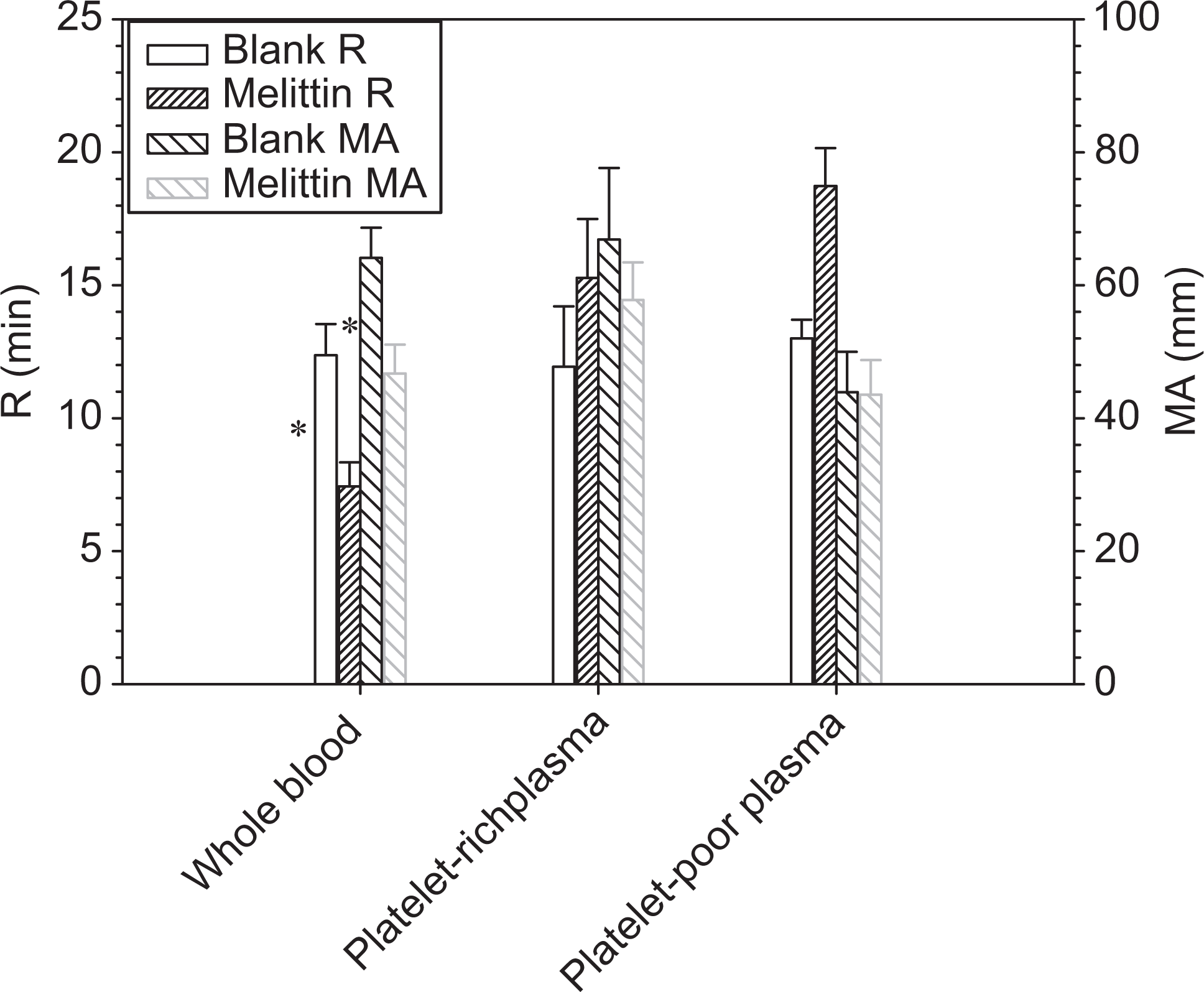
Effects of melittin on coagulation with different blood components. Data represent mean ± standard error of the mean ([SEM] n = 4). The final melittin concentration was 40 μM. *Difference from blank (P < .05).
Fibrinogen γ peptide
Figure 5 shows the concentration-dependent effects of a fibrinogen γ peptide on blood coagulation. An optimal concentration of 736 μmol/L was observed for most profound hemostatic effects as indicated by a 12% decrease in R, 13% decrease in K, and 27% increase in α. The 3% increase in MA is not significant. Below and above this concentration, there were no effects except anticoagulant effects at 2890 μmol/L as indicated by 23% increase in R and 27% decease in MA.
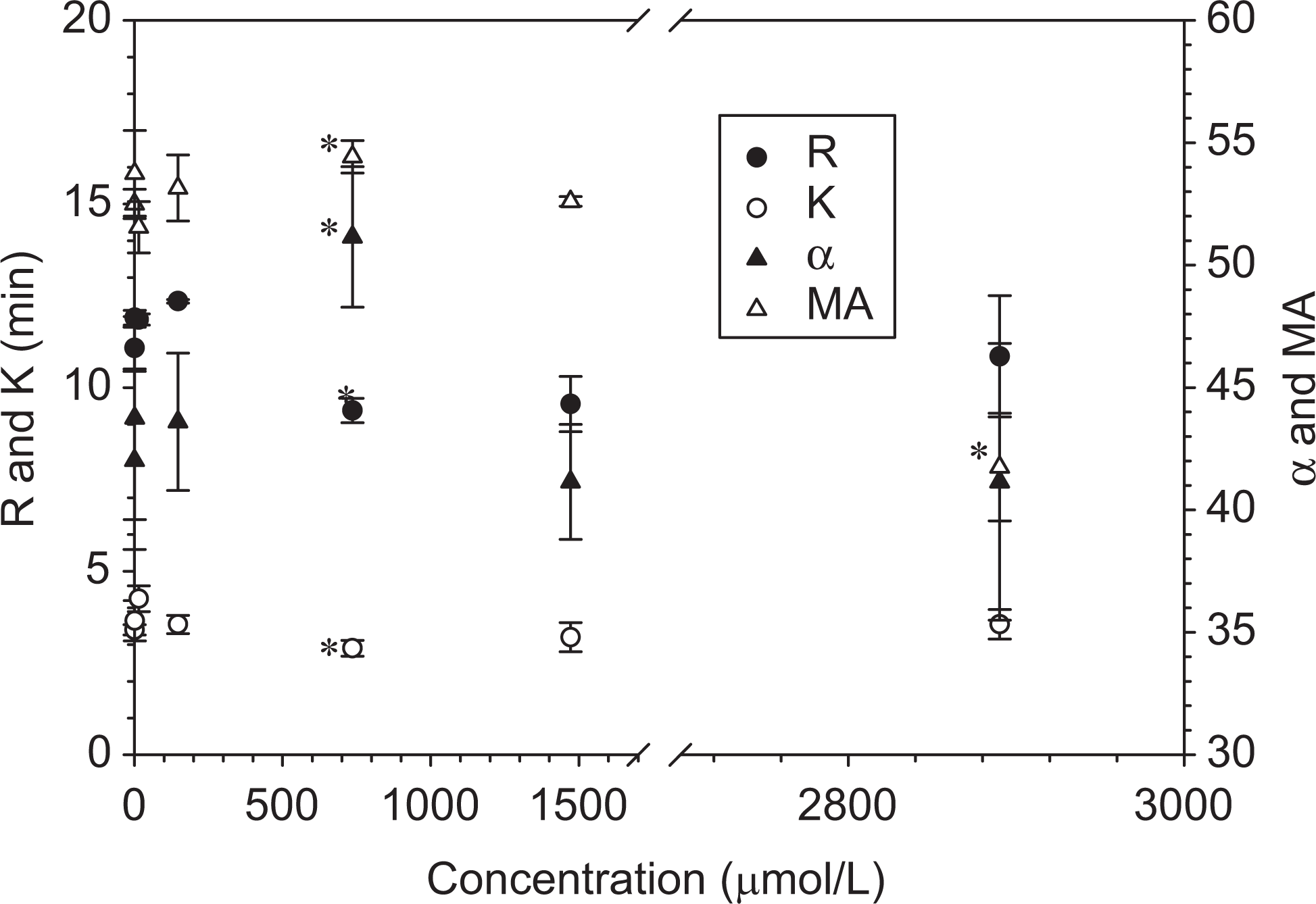
Dose-response curves of fibrinogen γ peptide. Data are expressed as mean ± standard deviation ([SD]n = 4). *Different from blank (P < .05).
Comparison of Factor VIIa and Peptide Effects
Figure 6 shows TEG profiles of the blood containing respective factor VIIa and peptides at their most hemostatic concentrations. Factor VIIa shows the highest procoagulant potency. The thromboelastographic value indicating clot initiation time (R) was decreased for all tested materials to different extents with the most reduction by factor VIIa, followed by melittin, IAP, and γ peptide. At the highest tested concentration of 1.7 μmol/L, factor VIIa decreased R, K, and TMA by 84%, 64%, and 40%, respectively. Factor VIIa and melittin resulted in a significant increase in α angle. However, melittin reduced the maximum clot strength, in contrast to the positive effects of factor VIIa. In general, IAP and γ peptide had a comparable effect on R, but half the effect as melittin and one third that of factor VIIa. The 2 peptides had no major effects on α-angle and IAP-reduced MA. All the peptides, except for γ peptide, significantly decreased TMA, while factor VIIa and melittin showed a significant effect in each of the measured TEG variables. As far as the concentration is concerned, the γ peptide needs the highest molar concentration among all tested agents to show appreciable hemostatic efficacy.
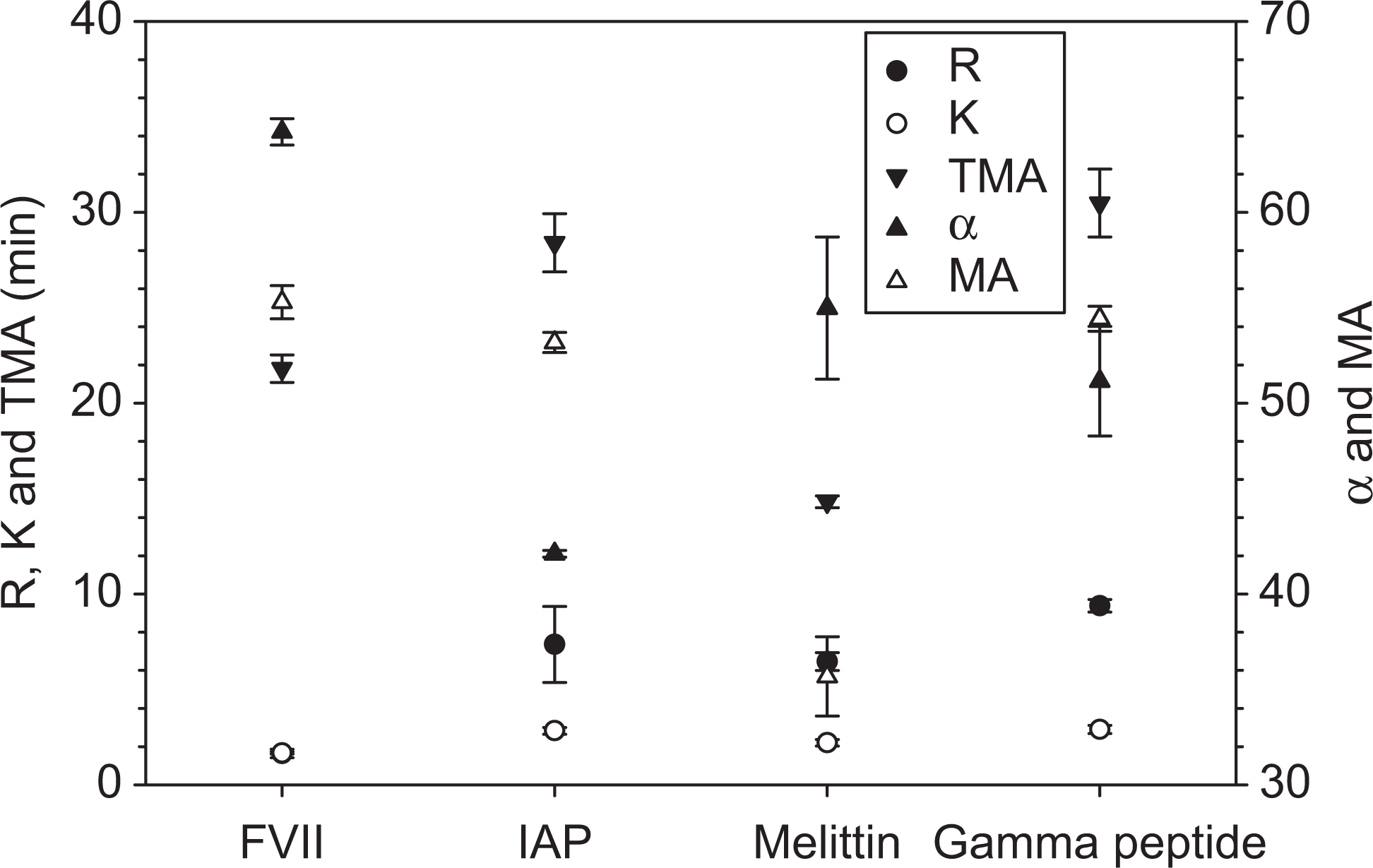
Comparison of IAP (0.87 μmol/L), melittin (40 μmol/L), and gamma peptide (735.7 μmol/L) with factor VII (1.71 μmol/L). Data are expressed as mean ± standard deviation ([SD] n = 4). IAP indicates ideal amphipathic peptide.
Discussion
Thromboelastography has found tremendous clinical applications for guiding the appropriate therapy to correct the defects in hemostasis. 29 However, its use for in vitro studies of hemostatic agents is limited to pharmacological agents 30 and coagulation factors.27,31 On the other hand, the TEG method has been used for evaluating the effects of resuscitation fluids and plasma substitutes, such as starch, dextran, on blood coagulation in vitro 32 and in vivo. 33
When a blood-soluble material (eg, a biopolymer) is tested, its hemostatic effects could be partially caused by the intrinsic viscosity of the material. 34 This can be verified by a TEG measurement of blood with the material in the absence of calcium. If there is no coagulation (ie, tracing of a straight line), the observed hemostatic effects, where calcium was added, could be attributed to the activation of coagulation by the added material, rather than by an increase in blood viscosity. In addition, hemodilution, when solutions are mixed with blood, should be taken into account by including appropriate controls. In our study, controls (eg, the Tris buffer) were included to exclude any effects other than those of the peptides. We further explored the TEG method for understanding the mechanism behind melittin-blood interactions using PRP and PPP.
The dose response of factor VIIa observed in our study is in accordance with that reported by Kawaguchi et al who studied the dose-dependent effects of activated recombinant factor VIIa in a concentration range from 0 to 45 mg/mL on R time and MA of citrated whole blood and showed a similar decrease in the former and increase in the latter. 27 Tomokiyo et al showed the in vitro hemostatic potency of human plasma-derived factor VIIa on TEG R + K time of coagulation factor VIII- or IX-inhibited whole blood, in a concentration range from 0.3 to 25 nmol/L (equivalent to 0.015-1.25 mg/mL). 35 They also confirmed its hemostatic effects at the concentration within this range on the TEG parameters in vivo using a monkey hemophilia B model.
All the results clearly highlight different concentration-dependent hemostatic properties of these peptides and may explain the underlying mechanisms, based on the association of TEG parameters with various blood components. The reduced R by the peptides implies interactions with coagulation factors. Specifically, the effect of IAP on blood coagulation seems to be most significant in clot formation. The pattern of TEG changes suggests that the activation of coagulation factors may be involved in the promotion of blood coagulation by the peptide. The peptide may accelerate the activation of coagulation factor X, which is responsible for the conversion of prothrombin to thrombin. 36 This is in accordance with the activation of factor Xa by other helical peptides in the reports37,38 that characterized the binding of factor Xa and factor IXa to the peptides. Modified TEG tests, using factor-deficient blood supplemented with the peptide, may further elucidate specific coagulation factors (eg, factor Xa) that could be activated by the peptide. On the other hand, the overall anticoagulant effects are in agreement with our study, showing that the peptide can act as an anticoagulant at concentrations above 1 μmol/L by competing for phospholipid-binding sites with blood coagulation factors. 39 The concentration-dependent dual activity has also been reported for detergent sclerosants that are procoagulants at low concentrations and anticoagulants at high concentrations. 40
Clot strength is the result of a modest contribution of fibrin and a significant contribution of platelets. The changes in MA by the peptides may be due to their effects on fibrin polymerization and platelet functions.
Although both are amphipathic, it appears that IAP and melittin may act differently in hemostasis. In contrast to IAP, melittin strikingly decreased MA, reflecting the profound impairment of platelet functions leading to a weaker clot (Figure 2D).
The good correlation between the hemolysis and the TEG values implies that melittin may act on blood coagulation through its hemolytic effects on cellular components of blood, particularly on erythrocytes and platelets. Specifically, the release of hemolysates and the platelet lysis were attributed to a shortened R and reduced MA in TEG measurements.41,42 Hemolysis has also been reported to enhance thrombin generation and result in a severe procoagulant state. 41 These are supported by our further TEG studies on PRP and PPP, which showed increased R and unchanged MA by melittin compared to the whole blood. Therefore, melittin appears to affect blood coagulation through hemolysis of erythrocytes and interactions with plasma proteins but not much with platelets. In addition, melittin caused very early fibrinolysis as compared to other hemostatic agents and control, which may be responsible for the diminished MA. Anticoagulant effects of melittin on whole blood have also been reported and ascribed to its inactivation of phospholipids. 43
The role of the γ peptide in blood coagulation is 2-fold 13 : on one hand, it accelerates blood coagulation by enhancing fibrin polymerization and reducing proteolysis; on the other hand, the sequence represented a binding motif of activated glycoprotein IIb/IIIa (αIIbβ3−) receptor on platelets that inhibits its interactions with fibrinogen, leading to anticoagulant effects. This explains the observed biphasic effects of the peptide on blood coagulation and is consistent with decreased R and MA by its analog of fibrinogen γ365-380 in TEG when added to a mixture of fibrinogen and thrombin. When attached to a polymer substrate, 44 the peptide is expected to promote platelet aggregation, leading to improved hemostatic ability as demonstrated by albumin particles carrying fibrinogen γ-chain sequence 400-411.
The peptides examined in this study are found to be effective, to various extent, in promoting the activation of clotting factors. However, the maximum enhancement is less than that of factor VIIa and occurs at an optimum concentration. The hemostatic activities of IAP and melittin may also be strongly linked to its helicity and amphipathic properties, 37 while that of the γ peptide depends on its sequences. It is noteworthy that IAP and γ peptide may reduce fibrinolysis of clot, which is desirable for hemorrhage control. 38
Of greater importance for this project is to incorporate the peptides into a biomatrix for optimal use for hemorrhage control. PEGylated γ peptide could form a gel in the presence of factor XIII and calcium ions with different network structure from that of fibrin clots. 45 The implication for hemorrhage control needs to be investigated. Preliminary results in animal bleeding models are promising for IAP incorporated into our in situ-forming hydrogels. 46
In summary, a number of hemostatic agents have been elucidated using a validated TEG. Methods that can be used to further modify and formulate the peptides for hemorrhage control were discussed.
Conclusions
Our TEG method confirmed the hemostatic effects of activated human coagulation factor VIIa, in consistent with the literature, thus validating the method for the evaluation of novel and potentially hemostatic peptides described in this study. All the peptides demonstrated concentration-dependent effects on blood coagulation but in different ways. The IAP primarily acts as an anticoagulant, although it appears to have some clot-promoting activities at low concentrations; and γ peptide influences fibrin polymerization and platelet fibrinogen interaction. Melittin affects both clotting time and strength due to its hemolytic activities. We believe that the TEG method is well suited for identifying peptides that may have the potential for further development as hemostatic products for hemorrhage control.
Footnotes
Acknowledgments
The authors thank Darik Gamble, Huang Huang, and Heather Wright for their excellent technical support and Defence Research and Development Canada for financial support.
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was financially supported by Defence Research and Development Canada.
