Abstract
Peripheral gangrene is rare in children. Protein C, protein S, and antithrombin deficiency, positivity for anticardiolipin antibodies or lupus anticoagulant and factor V Leiden mutation are important causes of thrombosis in the venous system. There is paucity of literature on the contribution of these factors in children with peripheral gangrene. We evaluated the role of aforementioned factors in children with peripheral gangrene. Protein S deficiency was seen in one case and another was transiently positive for lupus anticoagulant. None of the 11 age- and sex-matched normal controls had protein C, protein S, or antithrombin deficiency. Our results indicate that deficiency of protein C, protein S, and antithrombin, and positivity for anticardiolipin antibodies, lupus anticoagulant, and factor V Leiden are uncommon causes of peripheral gangrene in children in north-western India. Fibrinolytic and antiplatelet parameters were not tested. Testing for these may yield further clues to the etiology of this condition.
Introduction
Under physiological circumstances, both the coagulation system and the fibrinolytic system remain constantly active to maintain an intact and patent vascular tree. Peripheral gangrene results from vascular occlusion, which in turn could be secondary to hypercoagulability. The hypercoagulable state may be due to inherited deficiency of natural inhibitors of coagulation protein C (PC), protein S (PS), antithrombin (AT), or due to acquired causes especially, infections and trauma. Septicemia secondary to pneumococcal, staphylococcal, and streptococcal infections, measles and chickenpox have also been associated with limb gangrene. 1 Malignancies, therapy with drugs like bleomycin, 2 and cocaine abuse 3 have also been reported to cause peripheral gangrene.
There are limited studies on peripheral gangrene in children as peripheral gangrene is an uncommon clinical event; when it occurs, it is usually associated with serious illnesses. There is an increased interest in the role of natural inhibitors of coagulation in the thrombotic disorders and few studies have addressed the role of fibrinolysis in children with gangrene. 4 Deficiency of PC, PS, and AT have been reported in association with gangrene. To the best of our knowledge, there has been no study on these patients from the Indian subcontinent. We report the results of the prothrombotic profile of 11 children with peripheral gangrene along with their clinical course.
Materials and Methods
This study was carried out of in the department of Hematology, on patients referred from the Advanced Pediatrics Centre of the Postgraduate Institute of Medical Education and Research, Chandigarh, India, over a period of 4.5 years (January 2004 to June 2008). Our institute serves as a tertiary-level referral center for north-west India. The clinical and coagulation profiles of 11 children with peripheral gangrene were analyzed. Children aged less than 18 years, with gangrene of the distal extremities and with well-defined lines of demarcation were included in the study. The case histories of patients were reviewed from the patient record files. Presence of arthralgia or arthritis, history suggestive of Raynaud’s phenomenon and cold intolerance, was looked for; treatment for recent infections and history of drug intake was recorded. The results of laboratory tests for workup for autoimmune disorders and supportive tissue histology (where done) were noted.
Blood was collected by sterile venepuncture and plasma was aliquoted for PC, PS, AT estimation, and lupus anticoagulant (LA) testing, after screening the prothrombin time (PT), activated partial thromboplastin time (APTT), and fibrinogen levels. Plasma samples for estimation of PC, PS, and AT were delivered in 1 mL aliquots into plastic tubes and frozen at −20°C to be tested in batches. The clotting and chromogenic assays were performed on the STA-Compact coagulation analyzer (Diagnostica Stago, France). Functional activity of PC and PS were assessed using STA-clot protein C and S kits on clot-based assays, and antithrombin levels were estimated by the chromogenic-based STA-chrom antithrombin assay kit. The values were matched to published data on mean values of same age. 5,6 Testing for LA was by the kaolin clotting time and diluted Russell viper venom time (Screen and Confirm kits, Dade Behring). All patients were tested for the above factors after at least 6 weeks of the acute event or after 4 weeks of cessation of oral anticoagulant therapy.
Anticardiolipin antibodies (ACA) were tested with a commercial enzyme-linked immunosorbent assay (ELISA) kit (Orgentec GmBh). Serum samples were stored till testing. Anticardiolipin antibodies immunoglobulin G (IgG) values >10 GPLU(IgG phospholipid unit)/mL and ACA IgM values >7 MPLU(IgM phospholipid unit)/mL were taken as positive. Patients testing positive for LA or ACA were tested again after 12 weeks to confirm the antiphospholipid syndrome. DNA analysis of factor V Leiden (FVL) mutation was done by method described by Bertina et al. 7
Results
In this period, 267 pediatric patients were referred for workup for prothrombotic states. This constituted 28.6% of all cases referred to the laboratory for similar problems. Of these, 13 (4.9%) patients had peripheral gangrene. Two patients were excluded due to incomplete workup. The median age of the 11 patients available for analysis was 5 years (range 1 month-17 years), with a male: female ratio of 1.2:1.
One patient gave history of cold intolerance and one had arthritis. The latter had tubercle bacilli in the sputum and bilateral apical opacities in lung on chest X-ray. Another patient had previous history of tuberculosis for which he was on antitubercular drug therapy for 6 months. None of the patients had history of drug intake or smoking. Five children presented in the acute phase (within ≤4 weeks of onset of symptoms) with characteristic black, necrotic patches of variable size on the extremities at presentation. In 3 cases the symptoms had been present for 1 to 6 months (subacute), shrivelling of the digits was seen. In the remaining 3 cases, digital autoamputation had already occurred by the time the patient presented at our center. Seven patients had unilateral involvement of the limbs, whereas in 4 patients, there was simultaneous involvement of both limbs at presentation. Cold agglutinins and parvovirus serology was positive in 1 patient each. There was no hemoglobinuria. History of recurrent episodes of digital gangrene was present in 1 case. Blood cultures were sterile and complete blood count and erythrocyte sedimentation rate (ESR) were normal in all patients. Though PC and AT levels were within normal limits in all patients, PS was deficient in 1 patient. One patient showed transient positivity for LA but did not test positive on repeat testing. Table 1 summarizes the clinical data and laboratory prothrombotic profile of the patients with peripheral gangrene. Protein C, PS and AT in 11 age-matched controls tested in the same time period were within normal limits.
Clinical and Laboratory Findings of Children With Peripheral Gangrene
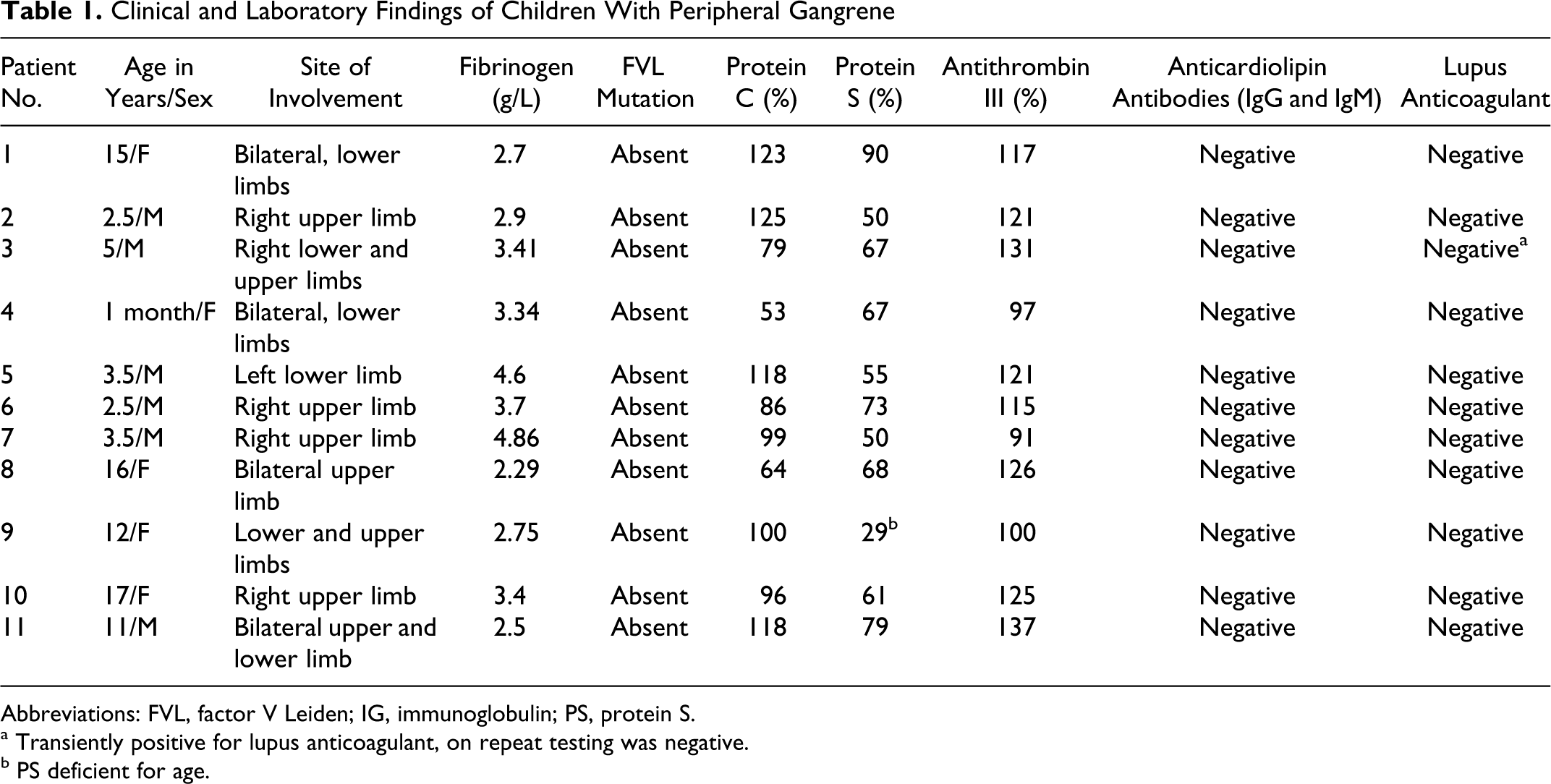
Abbreviations: FVL, factor V Leiden; IG, immunoglobulin; PS, protein S.
a Transiently positive for lupus anticoagulant, on repeat testing was negative.
b PS deficient for age.
Follow-up information over 1 to 9 years after the diagnosis was made was available in 6 patients and none showed any episode of recurrence.
Children seen in the acute phase were treated with heparin and started on oral anticoagulants (warfarin). Heparin was discontinued within 5 days. Warfarin dosage was titrated against the international normalized ratio (INR), which was maintained between 2 and 3. One patient underwent surgical amputation. Patients seen in the subacute or chronic phase were started on low-dose aspirin, while tests for autoimmune disorders were completed.
Discussion
Peripheral limb gangrene is an extremely uncommon condition in children. It is a complication of ischemia characterized by decay of tissue of distal part of extremity, which becomes black and malodorous. It usually occurs following trauma, surgery, infections, and a variety of other causes. Though reported in very sick children; peripheral gangrene occurring in an apparently normal child is extremely uncommon. We report here 11 children with peripheral gangrene, with results of testing for thrombophilia. To the best of our knowledge, such cases have not been reported from this part of the subcontinent.
There are few reports of patients presenting with peripheral gangrene with no identifiable cause from other parts of the world. Bass et al 8 reviewed 36 children with peripheral gangrene and found that in 11% (4 cases) of their patients no apparent cause of gangrene was obvious. Tropical idiopathic lower limb gangrene reported from Africa is a condition of unknown etiology with bilateral simultaneous gangrene of the lower limbs. The type B variant of this condition has been described in neonates and children less than 1 year of age. Children with this variant have blistering lesions on the extremities. These patients often need below-knee amputations. Presently, there is no definite diagnostic test available and the diagnosis rests largely on clinical features. 9 Blisters were seen on the foot of a neonate in the present study, who had developed bilateral gangrene. However, this child does not meet the clinical criteria of tropical idiopathic gangrene.
Platelets and the fibrinolytic system have an important role to play in arterial thrombosis. Platelet function evaluation studies were considered but deferred as many patients were either on aspirin or steroids, which would have affected the assessment. The role of fibrinolytic factors was examined by Turpie et al 4 in 3 cases of idiopathic peripheral gangrene in African children. This study reported a reduction in the plasma fibrinolytic activity, contributed partly by an increase in fibrinolytic inhibitors. Barr et al 10 described 2 cases of idiopathic peripheral gangrene in adults in whom no primary etiological factors were identified. In both their patients, impaired fibrinolysis as a result of diminished levels of plasma activator and increased levels of inhibitor were noted. In addition to raised levels of plasma fibrinogen, factor V, and factor VIII, consequent shortening of the kaolin-cephalin clotting time and thrombin time was present in both their patients. They postulated abnormalities in the blood coagulation and fibrinolytic enzyme systems as a possible explanation for the clinical manifestations of the peripheral gangrene in these patients without any obvious cause. Though one of the above studies addressed the issue of gangrene in children, it did not examine the role of the natural inhibitors of coagulation. The fibrinolytic system was not evaluated in our patients. Our patients did not show any abnormalities in fibrinogen levels, other than borderline elevation in 2 cases, possibly because they were tested in the quiescent phase of the disease.
Deficiencies, inherited or acquired, of natural anticoagulants PC, PS, and AT are well documented in literature to be associated with skin necrosis and peripheral gangrene. Functional PC deficiency was suggested as a contributory factor for thrombosis, resulting in skin necrosis and digital gangrene in 25 patients with renal failure and calciphylaxis. 11 The importance of searching for PS deficiency was stressed in a report wherein a 42-year-old female had progressive painful discoloration of the digits of the right foot. She was found to have PS deficiency and progressed to develop peripheral gangrene. 12
Antiphospholipid syndrome can also result in digital gangrene. Muwakkit et al 13 reported transient antiphospholipid syndrome as a cause for severe digital gangrene in a child who presented post hepatitis A infection. The patient had normal coagulation study results (PC, PS, AT, and activated protein C resistance) except for ACA, which were positive on initial presentation but resolved later. A single case in our study was transiently positive for LA. Similar to the case reported in above study; repeat testing in our case for LA was negative. With the current criteria, both cases would not qualify for antiphospholipid antibody syndrome.
Investigation in 5 pediatric patients by Levin et al, 14 with idiopathic purpura fulminans, of which 1 had peripheral gangrene, revealed virtually undetectable PS levels. The authors attributed autoimmune PS deficiency for thromboembolic manifestations and gangrene in their patients. A similar mechanism is believed to operate in patients with varicella infection who developed thrombosis. Chuansmurit et al 15 studied 60 pediatric patients with thromboembolic complications, of which 12% had peripheral gangrene. Though overall 42% of cases were found to have low levels of either PC or PS, this study included patients with thrombosis at other sites and in the venous system as well. This is in contrast with our study wherein we had a single patient who had PS deficiency and no history of previous thrombosis at any other site. It would be worthwhile highlighting the importance of testing the patients when the gangrene has settled, because in the acute phase there is a possibility of falsely low values, due to consumption of the inhibitors of coagulation at the sites of thrombosis.
Borman et al 16 reported a case of gangrene of the hand in a patient following extravasation of antibiotics and hereditary resistance to activated protein C. Factor V gene analysis showed that the patient was heterozygous for the common FVL mutation. Serious bacterial infections and septicemia have been associated with a reduction in the inhibitors. Though by itself, FVL may not be a strong risk factor, it has a contributory role when associated with other prothrombotic states. None of our cases had the FVL mutation.
Meningococcemia is an important cause for gangrene. Powars et al 17 reported 113 patients with Neisseria meningitides infection, of which 10 had peripheral gangrene. Not only was a deficiency of PC documented, an adverse impact of declining levels of PC on the severity of the illness was also demonstrated. This study advocated that therapy directed at replacement of the naturally occurring anticoagulants, such as PC, may ultimately improve the prognosis for individuals. Infectious trigger could not be identified with any certainty in our cases because of sterile cultures, even prior to administration of antibiotic therapy, though 1 patient had tuberculosis at the time of diagnosis.
The above studies indicate decrease in natural anticoagulants in cases of peripheral gangrene, with and without a predisposing secondary cause. The infective causes of peripheral gangrene are one-time events, with a low risk of recurrence. The association of other thrombophilic states raises concerns about recurrence of an ischemic event in other predisposing situations, such as immobilization, pregnancy, and trauma in later life.
In the current study, patients reporting with an acute presentation received heparin for 5 days, with overlap of warfarin from the third day. They were maintained on warfarin for 6 months, with dosage adjustment to maintain the INR of 2 to 3. Four weeks after cessation of oral anticoagulant therapy, the patients were sampled for assessment of PC, PS, AT, LA, ACA, and FVL. There are multiple challenges with oral anticoagulant therapy in children, especially related to compliance, dietary inferences, and need for close monitoring. This therapy would be warranted in the presence of PC, PS, AT deficiencies, FVL mutation, and in the antiphospholipid antibody syndromes. Steroids as such may not have a definite role in the medical management of gangrene in children. In this study, patients with clinical features suggestive of immune etiology received glucocorticoids till investigations excluded autoimmune disorders. Patients who presented after the acute phase was over, or after autoamputation had occurred, were maintained on low-dose aspirin. In digital gangrene, autoamputation is the usual outcome. 18 In the current study, 3 patients had autoamputation of digits. In patients where the gangrene has extended higher than the digits, embolectomy (though available as a treatment option) is usually never successful alone. Partial amputation of the limb, after well-formed lines of demarcation at distal limits, has been successful in children with peripheral gangrene when it has extended beyond the digits. This wait is often worthwhile as the line of demarcation often appears more distal than expected, thereby preserving more limb length than is initially expected. Surgical amputation was resorted to in 1 case in this study. No recurrences of gangrene or other thromboembolic events were seen in the cases where follow-up was available.
Conclusion
Our study has shown that deficiency of PC, PS, and AT and positivity for ACA, LA, and FVL mutation are uncommon causes of peripheral gangrene in children in north-western India. Our results need to be corroborated with large prospective studies from other centers. In addition, workup for fibrinolytic parameters and platelet activation may yield further clues to the causation of this life-threatening and enigmatic condition.
Footnotes
The author(s) declared no conflicts of interest with respect to the authorship and/or publication of this article.
The author(s) received no financial support for the research and/or authorship of this article.
