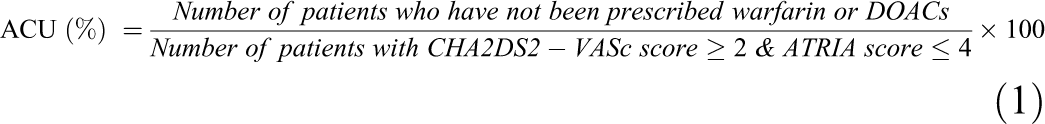Abstract
Background:
Patients with atrial fibrillation not being adequately treated with oral anticoagulant (OAC) therapy, with therapy underutilization or premature termination, have been commonly reported. However, studies on the utilization pattern of OAC therapy for patients with atrial flutter (AFL) are few. The aim of this study was to investigate the utilization of OAC therapy, and its influencing factors for patients with AFL in South Korea, as well as the types and percentages of anticoagulants used.
Methods:
We analyzed Aged Population Sample data compiled by the Health Insurance Review & Assessment Service from 2011 to 2015. We identified patients with AFL having the KCD-6 code I48.1. Patients at high risk of stroke with a congestive heart failure, hypertension, age ≥75 years, diabetes mellitus, stroke (or transient ischemic attack), vascular disease, sex score of ≥2 and at low risk of bleeding with an anticoagulation and risk factors in atrial fibrillation score of ≤4 were included in the study. Oral anticoagulant therapy underutilization was estimated in these patients using anticoagulant underutilization (ACU) scales. Demographic and clinical factors associated with OAC therapy underutilization were investigated using a logistic regression model.
Results:
The mean ACU value was calculated as 67.4% between 2011 and 2015. Positive risk factors for ACU were identified as follows: female sex, aspirin utilization, and limited anticoagulant options. Negative risk factors included comorbidities, such as congestive heart failure and valvular heart disease, and a history of stroke or transient ischemic attack.
Conclusions:
Our study demonstrates that two-third of patients with AFL in South Korea failed to obtain adequate stroke prevention treatment, even in the era of direct OAC availability. This tendency was more profound in women or those on aspirin therapy.
Atrial flutter (AFL) is a type of supraventricular tachycardia that shares some clinical features with atrial fibrillation (AF). Some distinctions exist between AF and AFL in terms of prevalence, underlying electrophysiologic mechanism, and rhythm control strategy. As AFL is far less common than AF, 1 it has been combined with AF in many epidemiological studies and drug-related trials. 2 –6
Although AF is caused by electrical spikes occurring at ectopic sites within the atrium, typical AFL is the consequence of a reentrant circuit around the tricuspid annulus, which shows “saw-tooth” features in 12-lead electrocardiography. 7
The same medications used for rate control in patients with AF are also used in patients with AFL. 8 Regarding rhythm control, antiarrhythmic drug therapy is usually attempted. However, catheter ablation therapy plays a crucial role in patients with AFL. 8 Cavotricuspid isthmus (CTI) ablation restores sinus rhythm with a high success rate (>90%) and prevents AF recurrence, which often emerges as a complication in patients with AFL. Thus, CTI ablation is recommended for patients in whom cardioversion failed with antiarrhythmic agents or for those who prefer it as the first-line treatment. 8
Similar to patients with AF, patients with AFL also have an increased risk of thromboembolism. 9 Morbidity and mortality among patients with AFL do not significantly differ from those observed in patients with AF. 10,11 The chronic utilization of antithromboticagents is therefore essential to prevent strokes in patients with AFL. Currently, no separate guidelines for the management of patients with AFL exist, but the 2014 AHA/ACC/HRS guidelines 12 and 2016 European guidelines for AFL 8 recommend antithrombotic therapy according to the same risk profile used for patients with AF. The congestive heart failure [CHF], hypertension, age ≥75 years, diabetes mellitus, stroke [or transient ischemic attack [TIA]], vascular disease, sex (CHA2DS2-VASc) score is used to determine the risk of stroke, whereas the risk of hemorrhage can be assessed based on criteria such as hepatic or renal disease, ethanol abuse, malignancy, old age, reduced platelet count or function, rebleeding, hypertension, anemia, genetic factors, excessive fall risk, and stroke (HEMORR2HAGES), hypertension, abnormal renal/liver function, stroke, bleeding history or predisposition, labile INR, elderly, and drugs/alcohol (HAS-BLED), or anticoagulation and risk factors in atrial fibrillation (ATRIA) scores. Chronic oral anticoagulant (OAC) therapy is recommended in high-risk patients (usually patients with CHA2DS2-VASc of ≥2) for stroke prevention. 9,13 –15
Oral anticoagulant therapy has been proven to be superior to placebo or aspirin in reducing the risk of stroke and mortality. 16 –19 Despite this evidence, many studies have reported that patients with AF have not been adequately treated with OAC therapy, and its underutilization or premature termination is common. 17,20 –23 A previous study reported that more than half of patients with AF failed to obtain satisfactory stroke prophylaxis in South Korea, even in an era when direct OAC (DOACs)were available. 23 However, studies regarding the utilization pattern of OAC therapy for patients with AFL are scarce globally as well as locally.
The aim of this study was to investigate the utilization of OAC therapy, and its influencing factors, in patients with AFL in South Korea as well as the types and percentage of anticoagulants used.
Methods
Study Data
This was a cross-sectional study. We analyzed Aged Population Sample data compiled by the Health Insurance Review & Assessment Service (HIRA-APS), which holds all medical records covering 20% of elderly patients in Korea aged ≥65 years.
The Korean Classification of Diseases-6 code (KCD-6 code, Korean version of the International Classification of Diseases, Tenth Revision code) was used to extract data. Data sets held by HIRA include prescription records and medical practices in the Korean National Health Insurance (NHI) Service. Types of health insurance in Korea include NHI, Medical Aid (MedAid), and Patriots and Veterans Insurance (PVI) plan. Approximately, 97% of the total population of South Korea is NHI covered, and approximately 3% are covered by the MedAid plan, a form of medical insurance that provides affordable medical care to low-income families; 0.5% of the population benefits from the PVI plan.
Study Participants
We identified patients with AFL having a KCD-6 code of I48.1. Patients at high risk of stroke were first identified using the CHA2DS2-VASc score, and those at high risk of bleeding were excluded based on the ATRIA score. Subsequently, only patients with a CHA2DS2-VASc score of ≥2 and an ATRIA score of ≤4 were included in the study. To calculate the CHA2DS2-VASc and ATRIA scores, we checked the patient’s diagnosis code (see Appendix A). Patriots & Veterans Insurance plan participants were excluded (n = 14), as their prescriptions were often filled in an inpatient pharmacy in South Korea, unlike the other plans. Moreover, we excluded those patients with AFL who had AF as a comorbidity.
Anticoagulant Underutilization
First, oral anticoagulants (eg, warfarin, dabigatran, rivaroxaban, and apixaban) used in the study participants were identified and counted in the outpatient prescription records each year from 2011 to 2015. We operationally defined ACU as the percentage of patients with AFL (CHA2DS2-VASc score of ≥2 and an ATRIA score of ≤4) medicated with oral anticoagurants in a given year (Equation 1). 23
Patterns of Oral Anticoagulant Utilization
Anticoagulant utilization was estimated and expressed as a percentage in all patients who were prescribed a minimum of 1 anticoagulant at least once. We also examined aspirin utilization in addition to oral anticoagulants.
Statistical Analysis
Baseline characteristics of patients and medical institutions are presented using univariate statistics. Data are presented as mean and standard deviation (SD) for continuous variables and as percentage for categorical variables. P value was determined using independent sample t tests for continuous variables and χ2 tests for categorical variables.
We performed multiple logistic regression analysis of ACU data and individual, social, and health factors to determine their significance. Explanatory variables included age and sex as individual factors; insurance coverage and duration as social factors; and ablation, CHF, hypertension, diabetes, stroke, vascular disease, anemia, renal disease, and hemorrhage as health factors. We grouped the study participants by age: 65 to 69, 70 to 74, 75 to 79, 80 to 84, and ≥85 years.
The Hosmer-Lemeshow test was used to ensure accuracy of the goodness of fit for the model. Data analysis was performed using SPSS version 23 (IBM Corporation, New York) with a statistical significance set at a P level of <.05.
Results
Characteristics of Study Participants
The prevalence of AFL was approximately 1% each year. A total of 2315 patients with CHA2DS2-VASc scores of ≥2 and ATRIA scores of ≤4 were selected as study participants (Figure 1). The mean age of the study participants was 73.37 (6.53) (SD). There were more male than female patients (57.8% vs 42.2%; Table 1). The mean CHA2DS2-VASc and ATRIA scores were 3.81 (1.22) and 1.84 (1.03), respectively.

Case extraction diagram.
Demographic Characteristics and Anticoagulant Therapy Underutilization.

Abbreviations: AC, anticoagulant (eg, warfarin, apixaban, dabigatran, ribaroxaban) users; ACU, anticoagulant underutilization rate; AFL, atrial flutter; ATRIA, anticoagulation and risk factors in atrial fibrillation; CHA2DS2-VASc, congestive heart failure, hypertension, age ≥75 years, diabetes mellitus, stroke (or transient ischemic attack, vascular disease, sex.
Anticoagulant Underutilization
Among the 2315 patients, 32.6% (n = 754) used at least 1 anticoagulant. The mean ACU value between 2011 and 2015 was estimated to be 67.4%, which showed improvement over that time period (P = 0.022). We did not observe any difference in ACU value in relation to age groups (P = 0.941). Female patients had a tendency to underutilize OACs, although this was not statistically significant (P = 0.127). Anticoagulant underutilization value was almost halved in patients with concomitant valvular disease (P < 0.001) but unaffected by ablation therapy. Of note, patients who had used aspirin had significantly higher ACU value (P < 0.001; Table 1).
Predictors of High Anticoagulant Underutilization
Table 2 shows results from the logistic regression analysis. In 2012 to 2015, the degree of undertreatment was smaller than that in 2011, but it did not decrease linearly over time. Anticoagulant utilization in women was observed to be relatively lower than that in men (odds ratio [OR] = 1.353; P = .002). Oral anticoagulant therapy was more prevalent in patients with CHF as a coexistent disease or those who had experienced stroke or TIA; (OR = 0.687 and 0.460, respectively; P < .001 for both). However, if patients had experienced bleeding (OR = 1.683; P = .060) or were taking aspirin (OR = 2.026; P < .001), they were often less likely to receive appropriate treatment than those who did not. The most significant difference in ACU was seen with respect to valvular heart disease and its presence or absence. The value of the odds of underutilization was very low at 0.195 (P < .001) when valvular heart disease was coexistent.
Adjusted Odds Ratios and 95% Confidence Intervals From Multiple Logistic Regression Analysis of Anticoagulant Underutilization.

Abbreviations: (R), reference; adjusted OR, adjusted odds ratio; CI, confidence interval.
Patterns of OAC Utilization
The most utilized OAC therapy to prevent stroke in patients with AFL was warfarin from 2011 to 2015. In 2013, dabigatran was used as the first DOAC but not to a great extent. In 2015, 3 DOACs (dabigatran, rivaroxaban, and apixaban) were used in small quantities, but not edoxaban, which was unavailable in South Korea until 2016 (Figure 2).

Distribution of anticoagulant therapies among patients with AFL who utilized OAC therapy from 2011 to 2015. AFL indicates atrial flutter; OAC, oral anticoagulant.
Discussion
Patients with AFL have been included as a subgroup of patients with AF in most clinical studies regarding the OAC use and have received relatively less attention than patients with AF. We previously investigated the utilization of OAC therapy in patients with AF for stroke prevention including the time period when DOACs were available in South Korea. In the current study, we concentrated on AFL-only patients by excluding patients with AFL who had the diagnosis code of AF at the same time or later. We found that a large population of patients with AF failed to obtain adequate stroke prophylaxis in South Korea (ACU of 68.0%-62.5% from 2011 to 2014), and this had not improved as much as expected even when DOACs are readily available. Risk factors for OAC therapy underutilization were identified as being a woman, being of advanced age, or being at a greater social disadvantage. 23
The mean age of patients with AFL (73.37 [6.53]) in the study here was a little lower than that of patients with AF from the previous report. 23 This tendency is also seen in other studies comparing patients with AF and AFL. 10,24 The annual prevalence of AF had been increasing in the previous study, whereas the prevalence of AFL did not increase or decrease. 20,24 From these observations, we can hypothesize that AFL may be less affected by aging compared to AF.
In addition, unlike our previous study, 23 men were more than women in the current study (57.8% vs 42.2%). Other AF investigations have also shown more men than women in their studies. 10,24
The results of our study indicate that more than two-thirds of patients with AFL requiring OAC therapy did not receive adequate OAC therapy (overall ACU = 67.4%). Of note, ACU in patients with AFL was slightly higher than that in patients with AF over the time period covered (72.9% vs 68% in 2011, 68.8% vs 66.7% in 2012, 63.0% vs 66.1% in 2013, and 66.1% vs 62.5% in 2014). 23
Throughout this period of assessment, the most utilized OAC therapy had been warfarin, which was prescribed to >95% of patients every year with the exception of 2015. Direct oral anticoagulant utilization increased to 7.6% for dabigatran and rivaroxaban in 2015 (Figure 2). Although apixaban utilization is still relatively low, the verification of its cost-effectiveness in a previous study suggests this will increase. 25 In addition, edoxaban has been included in the Korean NHI system since February 2016, and its utilization is expected to increase in the future.
Thus far, the risk of stroke in patients with AF and the need for OAC utilization have been extensively studied. 19,20,23,26,27 In the case of AFL, however, there has been insufficient research. Although the risk of stroke associated with AFL is not higher than that associated with AF, studies have shown that high rates of conversion from AFL to AF and the risk of developing stroke itself are not negligible. 9,10,28
According to the logistic regression analysis, risk factors for ACU were being a woman, aspirin utilization, and limited anticoagulant options. Conversely, OAC therapy was better in patients with previous stroke experience, concurrent valvular heart disease, or CHF. In particular, the OR for ACU in the group taking aspirin was doubled. In most Asian countries, including South Korea, many clinicians are concerned about the risk of unintentional bleeding when treating patients having AF or AFL with anticoagulants. 29 According to previous studies, the risk of stroke was significantly lower in warfarin patients than in aspirin patients over the entire CHA2DS2-VASc score range. 17 –19 However, there was no significant difference in the risk of intracranial bleeding (hemorrhagic stroke + traumatic intracranial bleeding) between the 2 groups. 18,19,30 Therefore, aspirin utilization as an alternative to OAC therapy should be discouraged. Some patients with AF/AFL may need combination therapy with OACs and antiplatelet agents. Both sets of guidelines (AHA and European) recommend continued OAC therapy and addition of an antiplatelet agent (aspirin or clopidogrel) or both agents if patients with AF/AFL require antiplatelet therapy due to acute coronary syndrome or when undergoing percutaneous coronary intervention. 8,12
The underutilization of DOACs is thought to be partly due to the restrictions of previous benefit guide for using them in South Korea. An eligible patient had to present a documentation proving he or she had tried warfarin first, resulting in proven contraindication, sensitivity, or treatment failure in association with it.
There are some limitations to our study. First, the initial purpose of the data set we used was not for research but for handling insurance benefits. Second, in the ACU measurement, we did not know the patient’s exact clinical laboratory data, contraindications, and allergies to anticoagulants (warfarin or DOACs). Finally, in reference to the previous study, participants with intermittent AFL may not have been categorized and included within this study, as it is difficult to diagnose. Furthermore, it is difficult to say whether patients with intermittent AF had been excluded from the entire cohort of participants because of challenges relating to diagnosis. 31
This was the first large population cohort study to examine the lack of OAC therapy in patients with AFL and to investigate the type and frequency of anticoagulants used in South Korea. Overall, there is still ACU in patients with AFL in South Korea, and the DOAC utilization is still insignificant considering their cost-effectiveness. Direct oral anticoagulants have been available for utilization as first-line agents in South Korea since July 2015, and high-risk patients can now be insured without restrictions. 23 Therefore, we expect that OAC therapy utilization will significantly improve in the near future.
Conclusions
Our study demonstrates that a large population of patients with AFL failed to obtain adequate stroke prevention treatment in South Korea, even in an era when DOACs were available. This tendency was more profound in women or those on aspirin therapy.
Footnotes
Appendix A
Authors’ Note
Sanghun Lee contributed to design, analysis, and interpretation; drafted the manuscript; crtically revised the manuscript; and gave final approval. Nam Kyung Je contributed to conception and design, acquisition, and interpretation; drafted the manuscript; critically revised the manuscript; and gave final approval. Both authors agree to be accountable for all aspects of work ensuring integrity and accuracy.
Acknowledgments
The authors used the Health Insurance Review & Assessment Service (HIRA) Aged Population Sample from 2011 to 2015 (HIRA-APS-2011-0060, HIRA-APS-2012-0055, HIRA-APS-2013-0054, HIRA-APS-2014-0055, and HIRA-APS-2015-0052) for this study, but the results have no concern with the Ministry of Health and Welfare or HIRA.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by a 2-Year Research Grant of Pusan National University.