Abstract
Introduction
As cancer care increasingly shifts to outpatient settings, patients with incurable cancer and their caregivers face growing challenges in addressing supportive oncology needs across five domains: informational, physical, emotional, social, and spiritual. Integration of supportive care in routine oncology practice—or primary palliative care—remains limited. Oncology encounters prioritize clinical agendas, leaving little time for supportive care and setting the stage for adverse outcomes. This study pilot tested a primary palliative care communication intervention, PRECURSOR (NCT05995860), using a nonrandomized (10 usual care control, 10 intervention) approach in a gynecology oncology clinic.
Methods
PRECURSOR combines a brief Freelisting activity—used to elicit communication intentions about supportive oncology needs among patients, caregivers, and providers—with an educational handout on the five domains of supportive oncology needs. Primary outcomes were feasibility (≥25% enrollment rate; ≥4 enrollments/month) and acceptability (overall and by component). Exploratory outcomes were communication behaviors (qualitatively coded from audio-recorded encounters) and post-encounter outcomes (via surveys).
Results
Of 1356 screened, 78 were eligible, and 20 enrolled (26%) in 38 weeks (2 enrollments/month). Most (70-78%) patients, caregivers, and providers rated PRECURSOR as acceptable overall. Patients and caregivers found both components acceptable, but providers favored the educational handout. Among exploratory outcomes, a greater proportion of the supportive oncology needs discussed during encounters were initiated by patients in the intervention group (46%), compared to control (37%). Average distress and anxiety scores were lower in the intervention group. No other patterns were observed among the exploratory outcomes. Qualitative findings indicated PRECURSOR was valuable, but refinements were suggested to increase impact.
Conclusions
PRECURSOR was a feasible and acceptable primary palliative care communication intervention in the outpatient oncology setting. PRECURSOR holds potential to foster more patient-centered communication about supportive oncology needs and improve the psychological well-being of patients and caregivers facing incurable cancer, though refinements are needed.
Introduction
Advances in treatment have made it possible for patients with incurable cancer to live long periods of time before their illness enters the terminal phase.1,2 Among the six most common cancers alone (bladder, breast, colorectal, lung, melanoma, prostate), it is estimated that nearly 700 000 people are living with incurable cancer as a chronic condition in the United States, and these numbers are expected to increase. 3 This growing cohort of cancer survivors and their caregivers experience needs that extend beyond the routine clinical aspects of care to include complex supportive oncology needs, yet research efforts to address these needs in this population are limited.3-7
Supportive oncology needs fall into five domains: informational, physical, emotional, social, and spiritual.4,8 The prevalence of these needs is high among patients with incurable cancer and their caregivers, where informational (eg, treatment risk/benefit) and physical (eg, fatigue, pain) needs approach 100%, emotional (eg, anxiety) needs approach 75%, and social (eg, social support) and spiritual (eg, spiritual pain) needs approach 50%.9,10 As cancer care increasingly shifts to the outpatient setting,11,12 patients with incurable cancer and their caregivers are experiencing greater demands navigating these supportive oncology needs. Consequently, comprehensively addressing supportive oncology needs is of critical importance to delivering high-quality cancer care when patients and caregivers interact with providers in the outpatient setting.
Unfortunately, supportive care is not routinely integrated into outpatient oncology care.4,13-16 Nearly all patients with incurable cancer and their caregivers report unaddressed supportive oncology needs due to inadequate communication during outpatient oncology encounters.5,13,17-22 Supportive care delivered by oncology providers alongside routine oncology care (ie, hereafter, primary palliative care [PPC] 23 ) requires expert communication to address supportive oncology needs. However, oncology providers disproportionately focus communication during outpatient encounters on clinical agendas (routinized assessment, test results review) and tend to dominate the conversational space (53-70% of spoken content is provider-driven).21,24-30 As a result, patients and caregivers have few opportunities to fully communicate their supportive oncology needs.21,29 Even when these needs are discussed, the conversation is typically limited to needs under the physical domain. 5 Furthermore, caregivers are frequently overlooked during these encounters, despite their central roles in supporting patients and having their own supportive oncology needs.17,26-28,31 Poor outcomes ensue from this inadequate communication, including negative patient and caregiver perceptions of the quality of care and communication received as well as increased distress, anxiety, and depression.17,32-35 When accumulated across the incurable illness trajectory, unaddressed needs also result in poor outcomes downstream, including missed opportunities for supportive care referrals and increased healthcare utilization (eg, hospitalization) that may be unwanted or burdensome.14,36,37
The impact of PPC communication interventions to address these pitfalls among the oncology population has been limited or mixed to date.38-42 Provider-directed interventions dominate, where only 18% of interventions have patient- and caregiver-directed components.36,43 This ignores the often triadic (patient-caregiver-provider) nature of encounters and generates approaches that are not patient- and caregiver-centered. Moreover, PPC interventions remain infrequent in the outpatient setting and are less likely to involve patients with incurable cancer and their caregivers, despite their elevated supportive oncology needs and growing representation within the cancer survivor population.44,45 Thus, there is an urgent need for PPC communication interventions that expand the focus of outpatient oncology encounters to address a broader set of patient- and caregiver-centered supportive oncology needs in the context of incurable illness. 14
The purpose of this study was to pilot test a theory-informed intervention called PRECursOr (
Methods
Design
This was a nonrandomized pilot study with the usual care control group (
Participants
Setting
This pilot study took place at Indiana University Melvin and Bren Simon Comprehensive Cancer Center, and Indiana University Health Joe and Shelly Schwarz Cancer Center, a satellite cancer center that is a part of Indiana University Health healthcare system.
Sample and Eligibility Criteria
Recruitment
All participants provided informed consent prior to study enrollment. Clinic appointment schedules of consented providers were screened for eligible patients. Eligible patients were identified and recruited first, followed by their primary caregivers. Eligible patients were sent a study packet (ie, standardized informational letter, copies of the patient and caregiver informed consent forms) approximately three weeks in advance of their appointment. A follow-up recruitment call was made using a standardized script within one week of the date the study packet was mailed. If interested and eligibility confirmed, verbal consent was obtained by phone and documented in the secure Research Electronic Data Capture (REDCap) study database. Caregivers were recruited either during the patient call (if cohabiting) or via a separate phone call (if living separately), with verbal consent obtained accordingly. All participants were informed of their rights and the voluntary nature of the study. Additionally, if potentially eligible patients and their caregivers were identified in real time during the clinic day, in person written informed consent was conducted on-site. Following the non-randomized approach, participants were sequentially enrolled in the study were assigned to the control group first until the control group recruitment goal was reached, followed by assignment to the intervention group until the intervention group recruitment goal was reached.
Study Conditions
PRECURSOR Intervention
PRECURSOR is a PPC communication intervention delivered immediately prior to the outpatient oncology encounter. PRECURSOR is rooted in an adapted version of the Integrative Model of Behavior Prediction and Behavior Change Theories,
49
which posits that the performance of a behavior, such as communication, is the direct result of one’s intentions to perform it (Figure 1). PRECURSOR is also informed by the Basic Science of Communication Conceptual Framework,
36
which links communication behaviors (ie, verbal and non-verbal) to immediate (ie, how communication was perceived), proximal (ie, how communication was experienced, markers of effective information exchange), and distal (ie, long-term impacts on healthcare utilization) communication outcomes. Theoretical Underpinnings of PRECURSOR
PRECURSOR integrates Freelisting to elicit communication intentions about supportive oncology needs among the patient-caregiver-provider triad. This involves participants Educational Handout for PRECURSOR
Control Group
Participants in the control group received usual care.
Data Collection
The principal investigator or a trained research assistant collected data in a private clinic room. All study data were securely stored and captured in the REDCap study database. Data collection included: pre-encounter: collecting Freelists from the patient, caregiver, and provider independently using an electronic tablet (intervention arm only); during encounter: audio-recording the encounter; post-encounter: administering survey-based outcome measures and conducting an audio-recorded qualitative interview with patients and caregivers; and post-study: conducting a qualitative interview with providers. Participants each received a $50 gift card.
Outcome Measures
Primary Outcomes
Feasibility
This was determined through overall accrual (at least 25% of those eligible will enroll 52 ), accrual rate (4 enrollments/month), and encounter duration.
Acceptability
Perceived benefits of the intervention overall were measured using an adapted version of an 11-item, 5-point Likert scale measure.
53
The
Exploratory Outcomes
Communication Intentions Before Encounters
Communication intentions about supportive oncology needs were measured via the Freelisting responses generated by patients, caregivers, and providers in the intervention arm.
Communication Behaviors During Encounters
Communication behaviors were measured by qualitatively coding the transcribed encounter recordings for conversation content consistent with the five domains (informational, physical, emotional, social, and spiritual) of supportive oncology needs.
Communication Outcomes Following Encounters
Immediate
The
Proximal
Some proximal outcomes focused on the individual level. The
Other proximal communication outcomes were relational in nature. The
Qualitative Interview
A post-encounter qualitative interview was conducted with patients and caregivers to add explanatory insights into the feasibility and acceptability of PRECURSOR as well as opportunities for intervention refinement. The interview guide contained open-ended questions with probes to encourage in-depth responses (eg,
Analysis
Primary Outcomes
Descriptive statistics (eg, frequency counts to tabulate proportions/averages) were used to assess the feasibility and acceptability benchmarks, except for average encounter duration, where a t-test (
Exploratory Outcomes
Communication Intentions Before Encounters
Freelisting responses were standardized by the principal investigator (KL) by grouping similar responses (eg, fatigue and tiredness; “Will chemo work?” and treatment response) and morphological derivatives (eg, anxious and anxiety). Descriptive statistics were used to assess the average length (ie, number of support oncology needs in each Freelists at the participant-level). Freelisting responses were synthesized at the domain level (proportion of patient, caregiver, and provider Freelisting responses matching to the five domains of supportive oncology needs). Individual Freelisting responses were examined for triadic concordance (proportion of encounters where patients, caregivers, and providers had at least one supportive oncology need they intended to discuss in common).
Communication Behaviors During Encounters
Communication behaviors were identified by qualitatively coding the transcriptions of the audio-recorded encounters for conversation content that was consistent with the five domains of supportive oncology needs. To do so, directed content analysis
65
was utilized, which involves a structured approach to qualitative coding wherein
Communication Outcomes Following Encounters
Given the pilot nature of this study, group differences in the average scores on the immediate and proximal outcome measures were explored descriptively only.
Immediate
For the
Proximal
For the
Results
Participant Flow
Of 1356 screened, 78 were eligible (6% eligibility), 62 approached, and 20 enrolled (Figure 3). Control group participants were recruited between June and November 2023 and intervention participants between May and November 2024. The lag between control and intervention recruitment was planned Recruitment Diagram
Sample Characteristics
Sample Characteristics

*missingness.
Outcomes
Primary Outcomes
Feasibility
Among those approached, 32% enrolled (26% of those who were eligible). There were no withdrawals. This indicates PRECUSOR was feasible based on the
Acceptability
With respect to the overall acceptability of PRECURSOR (intervention group only), 70% of patients and 78% of caregivers responded “agree” or “completely agree” to at least 80% of the overall acceptability items. With respect to the Freelisting component, 70% of patients and 89% of caregivers responded “agree” or “completely agree” to at least 80% of the
Exploratory Outcomes
Communication Intentions Before Encounters
Among participants in the intervention group, patients ( Communication Intentions Before Encounters and Communication Behaviors During Encounters. 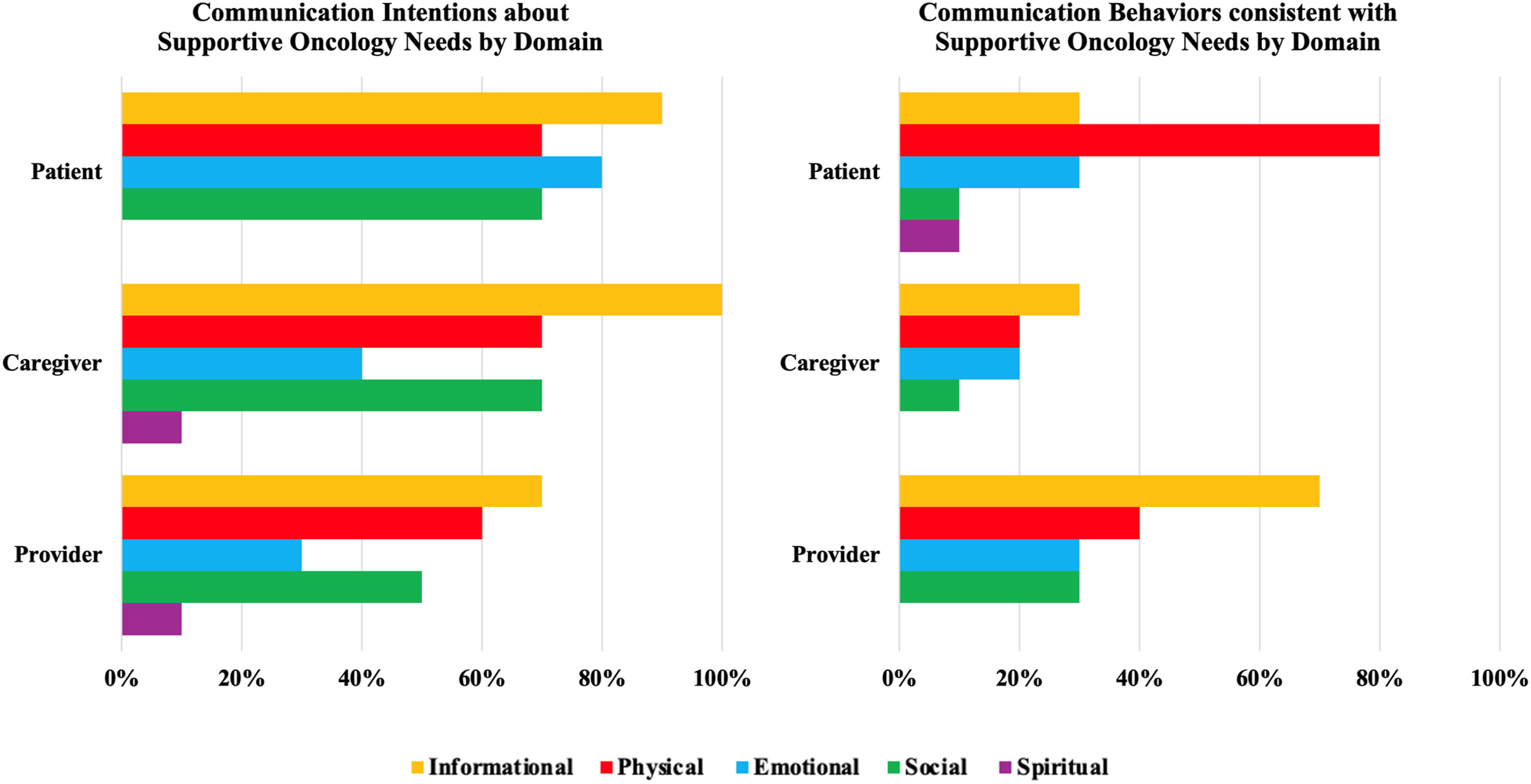
At the level of the individual Freelisting responses, patients, caregivers, and providers entered encounters with intentions to communicate about diverse and differing supportive oncology needs (Supplemental Table A). Supportive oncology needs were highly individualized, where only two (20%) of the intervention encounters demonstrated concordance among the patient-caregiver-provider triad on any one intention to discuss a supportive oncology need (eg, treatment side effects, pain control).
Communication Behaviors During Encounters
Participants in the control group initiated discussion about a greater number of supportive oncology needs (110 total, patient = 41, caregiver = 24, provider = 45) than participants in the intervention group (69 total, patient = 32, caregiver = 11, provider = 26) (Figure 5). This suggests that PRECURSOR may have led to more targeted communication during outpatient oncology encounters, making more efficient use of the conversational space. A greater proportion of the individual supportive oncology needs discussed during encounters were initiated by patients in the intervention group (46%), compared to the control (37%). This also suggests that PRECURSOR holds potential to make communication about supportive oncology needs more patient-centered during encounters. However, this pattern did not hold for caregivers, where 16% of the supportive oncology needs that surfaced during conversations were initiated by caregivers in the intervention group, compared to 22% in the control. The distribution of these discussed supportive oncology needs across the supportive care domains did not vary greatly between the intervention and control groups (Figure 5). For example, 69% of the supportive oncology needs discussed by patients in the intervention group, and 68% in the control group, fell under the informational and physical domains (Figure 5). Similar, patterns were true for caregivers and providers, indicating that when communication about supportive oncology needs occurred it typically was limited to the informational and physical domains, regardless of study condition. Supportive Oncology Need Communication Behaviors During Encounters by Domain
Freelisting responses (ie, communication intentions) were compared to the communication behaviors during encounters (Figure 4). While the providers’ communication behaviors during encounters largely mirrored their communication intentions before encounters, patients’ and caregivers’ intentions did not consistently surface during encounters. For example, 90% of patients and 100% of caregivers Freelisted intentions to communicate about supportive oncology needs under the informational domain, but only 30% of both patients’ and caregivers’ communication behaviors reflected this domain. This pattern may reflect a reluctance by patients and caregivers to bring up these supportive oncology needs or that the provider may have addressed those needs first, negating the need to bring them up.
Communication Outcomes Following Encounters
Immediate
Communication Outcomes Following Encounters

Proximal
Patients’ and caregivers’ average distress ratings approached or slightly exceeded clinically significant levels in both study conditions, but were lower in the intervention group, compared to the control (Table 2). While average anxiety scores were not clinically significant, they were lower in the intervention group, compared to the control. Patients’ and caregivers’ average ratings of their self-efficacy to communicate with providers and activation in care approached maximum ratings, regardless of study condition. Both patients and caregivers indicated high levels of therapeutic alliance with their providers, regardless of condition. Triadic concordance on the goals of treatment was infrequent—only present following 20% of the intervention encounters and 40% of control encounters. Finally, there were slightly more supportive care referrals following encounters in the intervention group (
Qualitative Interviews
Patients’ and caregivers’ qualitative interview responses largely reflected enthusiasm for PRECURSOR. One patient stated,
Providers had similar observations as patients and caregivers, valuing PRECURSOR’s impact on the range of topics they planned to discuss with patients and caregivers,
Discussion
The primary outcome data collectively demonstrate the acceptability and mixed feasibility of implementing a PPC communication intervention, PRECURSOR, prior to outpatient oncology encounters for patients and caregivers facing incurable gynecologic cancer.
Primary Outcomes
Acceptability was high, with 70% or more of patients and caregivers indicating that PRECURSOR and its components were acceptable. This mirrors the high acceptability documented in other communication-based interventions in the oncology population.68-70 Caregivers rated the Freelisting component particularly favorably with qualitative data suggesting that this stemmed from the validation caregivers felt in being asked about their supportive oncology needs. Providers favored the educational handout component of, where qualitative evidence indicated that providers felt the educational handout reminded them to think beyond their clinical agendas to consider what supportive oncology needs patients and caregivers may need to discuss.
Most feasibility benchmarks were met, including overall accrual being attained, a lack of withdrawals, and the limited impact of PRECURSOR on encounter duration. However, recruitment was slow and likely stemmed from a lower than anticipated number of eligible patients at the study sites—only 6% of those screened were eligible. While PRECURSOR was received well by patients with incurable gynecologic cancer and their caregivers, this suggest the need to test PRECURSOR where it has potential to make a larger impact—among outpatient oncology clinics who are seeing larger numbers of cancer survivors living with incurable cancer, such as breast, colorectal, lung, and prostate cancers. Among the eligible participants, refusals were partially due to a lack of interest in the present study, which may have stemmed from participants’ already strong relationships with their providers and high perception of their communication, as indicated by the high therapeutic alliance and quality of communication scores prior to intervention roll-out (ie, in the control arm). PRECURSOR did not significantly impact encounter duration, thus aligning with evidence that effective communication interventions do not necessarily add significantly more time to clinical encounters.71,72
Exploratory Outcomes
Patterns in the exploratory outcomes point to preliminary evidence of the positive impact of PRECURSOR on patients with incurable cancer and their caregivers. With respect to communication behaviors during encounters, a greater proportion of the supportive oncology needs that were discussed during the encounters were initiated by patients in the intervention group compared to the control—suggesting PRECURSOR holds the potential to drive more patient-centered communication about supportive oncology needs in the outpatient setting, facilitating efforts to move away from solely provider-driven communication agendas. This finding holds significance given calls in the field to design palliative care interventions that are responsive to the individualized needs and experiences of patients with cancer and caregivers. 73 Activating patients and their caregivers in this way has been suggested as an underutilized means of improving patients’ communication with their providers. 74 Individualized patient-facing materials (ie, not structured or standardized materials) that allow time for self-reflection as a means for structuring the conversational space have been advocated in the literature, and the Freelisting component of PRECURSOR is emblematic of these recommendations.16,75
With respect to communication outcomes following encounters, patterns suggest PRECURSOR holds the potential to enhance the psychological well-being of patients and caregivers through more targeted communication about supportive oncology needs, given the lower distress and anxiety scores in the intervention group. Even though the scores were lower, it should be noted that the distress ratings were of borderline clinical significance and the anxiety scores were non-clinically significant across groups. No other discernable patterns were noted among these outcomes, particularly the more immediate communication-centric outcomes. This sample of participants reported high quality communication and feeling completely heard and understood regardless of study condition, which may be because of the patients well-established relationships with their providers. Collectively, these findings may indicate a need to identify patients and caregivers with worse quality of communication ratings or higher distress or anxiety in future studies to demonstrate greater impact.
Among participants in the intervention group, patients’ and caregivers’ communication behaviors during encounters did not always reflect their communication intentions (ie, Freelisting responses) prior to encounters, while providers’ communication behaviors were more consistent with their communication intentions prior to encounters. While Freelisting helped individuals to identify potential supportive oncology needs to discuss during the encounter, this finding suggests that more focused efforts to prioritize and negotiate discussion about these supportive oncology needs among the patient-caregiver-provider triad are necessary to structure the conversational space during outpatient oncology encounters. 76 Thus, teaching skills like agenda setting in PRECURSOR may lead to more patient- and caregiver-centered discussions in future iterations of this PPC communication intervention. Such efforts may make the best use of the limited time during outpatient oncology encounters, and prior research documents the desire for this type of visit efficiency. 77 Alternatively, it may indicate that there is not enough time to meet all supportive oncology needs during outpatient oncology encounters, suggesting an alternate solution to follow-up on these needs is warranted in future research.
Opportunities for Intervention Refinement
PRECURSOR was initially designed with scalability in mind, intending to test whether a low-touch solution (ie, triadic Freelisting about supportive oncology needs with an educational handout) was enough to create reshape PPC communication behaviors during outpatient oncology encounters and communication outcomes following encounters. The qualitative findings suggest that while PRECURSOR was acceptable and potentially beneficial, it could be improved with several refinements in future studies to augment its impact: (1) enhancing the educational handout with expanded examples of supportive oncology needs, (2) visualizing the triadic Freelisting responses, and (3) leveraging agenda setting prior to the outpatient encounter. Patients, caregivers, and providers all expressed the desire to visualize the Freelisting responses. Providers noted that knowing this information would be critical in understanding the patient’s and caregiver’s readiness to discuss difficult topics such as prognosis. Formal feedback channels after assessments of need have been endorsed as critical step toward aligning individualized priorities and enhancing communication in the oncology setting.75,77,78 Thus, refining the intervention to include the visualization of the Freelists offers a structured formal feedback mechanism for agenda setting that enables the triad to identify shared and divergent communication priorities, thereby fostering a more democratized approach toward addressing supportive oncology needs. 76
Limitations
Eligibility criteria required patients to have incurable gynecologic cancer, which could mean that patients were actively receiving treatment for their incurable disease or were on surveillance alone. This criterion along with the non-randomized approach could indicate that groups were unbalanced with respect to patients’ treatment context. If so, this may have had an underlying influence on the patterns observed among the exploratory outcomes. Given the pilot nature of this study and its small sample size, it was not statistically powered, so patterns described among the exploratory outcomes are not meant to suggest efficacy, nor generalizability. The demographic homogeneity of the sample indicates the need for more intentional recruitment strategies in future studies. Additionally, the study was limited to patients with incurable gynecologic cancer who had established relationships with their oncology providers, highlighting the importance of testing PRECURSOR among more heterogenous samples of patients with incurable cancer—including those earlier in the illness trajectory and with less established provider relationships—to better assess its generalizability in future studies.
Conclusions
PRECURSOR was a largely feasible and acceptable PPC communication intervention when delivered in the outpatient oncology setting. Exploratory outcomes underscored that PRECURSOR may have fostered a shift away from the providers agenda to more patient-centered communication about supportive oncology needs during outpatient encounters. Exploratory outcomes also suggest PRECURSOR holds potential to improve the psychological well-being of patients and caregivers when facing incurable cancer through enhanced PPC communication about supportive oncology needs. However, findings suggest that refinements to PRECURSOR’s components that augment their agenda setting potential may enhance PRECURSOR’s impact in enhancing PPC communication and outcomes in future studies. Such efforts will help actualize triadic communication intentions about supportive oncology needs during outpatient encounters, serving to address existing gaps in PPC for patients with incurable cancer and their caregivers.
Supplemental Material
Supplemental Material - A Pilot Study of a Primary Palliative Care Communication Intervention (PRECURSOR) to Address Supportive Oncology Needs for Patients With Incurable Cancer and Their Caregivers in the Outpatient Oncology Setting
Supplemental Material for A Pilot Study of a Primary Palliative Care Communication Intervention (PRECURSOR) to Address Supportive Oncology Needs for Patients With Incurable Cancer and Their Caregivers in the Outpatient Oncology Setting by Kristin Levoy, Alexia M. Torke, Krista Longtin, Marianne S. Matthias and Susan Hickman in Cancer Control
Footnotes
Acknowledgements
With deep gratitude to the patients, caregivers, and providers who participated in this research. With great appreciation to Ashley Sheets, Cheri West, and Lynne McCranor for their steadfast commitment to participant recruitment and data collection throughout the conduct of this trial. With great appreciation to Lizzie Mauro for her diligent efforts serving as a dual coder for the directed content analysis of the transcribed encounter recordings.
Ethical Considerations
This study was approved by the Indiana University Institutional Review Board (Approval Date: 04/26/2023; IRB#18860) as well as the Indiana University Melvin and Bren Simon Comprehensive Cancer Center’s Scientific Review Committee (Approval Date: 03/10/2023; Protocol# CTO-IUSCCC-0827). All participants provided informed consent prior to study enrollment. If phone-based recruitment occurred, then verbal informed consent was obtained. If in-person recruitment occurred, then written informed consent was obtained.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by an American Cancer Society Institutional Research Grant from Indiana University Melvin and Bren Simon Comprehensive Cancer Center [grant number 19-144-37] as well as Richard and Kaye Woltman Endowed Graduate Fellowship in Health Communication.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request with appropriate approval. Access to the data may be subject to restriction due to privacy, ethical, or legal considerations.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
