Abstract
Introduction
Cervical cancer is largely preventable through regular screening, yet uptake in the UK remains below national targets, particularly among harder-to-reach groups. Despite national efforts, barriers such as fear, embarrassment, and low health literacy continue to hinder participation. This retrospective study evaluates the impact of delivering information and education regarding cervical screening (CS) to hard-to-reach populations, with the aim of increasing CS uptake in line with the national target of 80% coverage.
Methods
Using a multidisciplinary team approach, women who had previously missed screenings were identified through electronic records. Remote interventions, including educational videos delivered via email and SMS, and an online booking system, were implemented to provide accessible information and flexible appointment options. These interventions aimed to address common barriers and encourage informed participation.
Results
Over 3 months, screening rates increased significantly. Uptake among women aged 25-49 rose from 77% to 80.5%, while rates among women aged 50-64 improved from 81% to 97%.
Conclusion
This study highlights the potential effectiveness of remote communication tools in increasing cervical screening participation, particularly among populations historically less likely to engage. Integrating digital resources into routine practice also has the potential to reduce administrative burdens, improve patient education, and make screening more accessible. By addressing key barriers and providing flexible booking options, primary care clinics can enhance screening uptake, supporting earlier cervical cancer detection and ultimately improving patient outcomes.
Plain Language Summary
What was the aim of this study?
Cervical cancer screening can save lives, but many women, especially in rural and deprived areas, do not attend their appointments. This study explored whether using remote digital tools, such as educational videos and online booking systems, could help increase participation in cervical screening within a primary care setting.
How was the study conducted?
This study reviewed electronic patient records from a rural primary care practice to identify women who had missed their cervical screening appointments. The practice then used digital communication methods, including:
- Short educational videos presented by a nurse to explain the screening process.
- Informational leaflets reinforcing key messages.
- A new online booking system to make scheduling easier.
Screening rates before and after these interventions were compared over three months to assess whether participation increased.
What were the key findings?
Overall cervical screening uptake improved, reaching the national target of 80%.
The greatest improvement was in older women (50-64 years), suggesting digital tools were particularly effective in this group.
Despite concerns that rural location and deprivation might reduce engagement, these factors did not appear to impact success.
Why is this important?
This study shows that simple, cost-effective digital interventions can help increase cervical screening participation. These findings support the wider use of remote communication strategies in primary care to improve cancer prevention efforts.
Who might be interested in this research?
- Healthcare professionals in primary care and public health.
- Policymakers working on cancer prevention and digital health.
- Researchers studying health inequalities and screening uptake.
Keywords
Introduction
Whilst the elimination of cervical cancer is within reach, 1 850 lives are claimed every year within the UK, with cervical cancer the 14th most common cause of female cancer death, accounting for 1% of all cancer deaths in females in the UK. 2 A primary reason for the development of cervical cancer is longstanding infection with types of human papillomavirus (HPV), which, since its discovery in the 1990s, can be screened for routinely, allowing for earlier detection and prevention strategies. 3 An estimated 4500 lives each year are saved through routine cervical screening (CS); however, uptake within the UK is at an all-time low and continues to decline year on year. 4
Established in 1988, the NHS Cervical Screening Programme (NHSCSP) invites women aged 25 and over for systematic, quality-assured screening whereby cells obtained from the cervix are examined using a liquid-based cytology method to reduce cervical cancer incidence and mortality. 5 The coverage of CS is defined as the percentage of eligible females screened within the appropriate timeframe, that being every 3.5 years for women ages 25-49 and every 5.5 years for women aged 50-64. 6 Coverage fell in the UK from 75% in 2010/2011 to 72% in 2018/2019, with no area in the UK achieving the national target of 80% coverage. 7 Whilst the COVID-19 pandemic has undoubtedly contributed to the steady decline in figures 8 there are several factors which have been attributed to having a negative impact CS uptake, such as sexuality, age, and socioeconomic status. CS uptake has been seen to be significantly lower in areas of higher deprivation with larger ethnic minority groups and potentially poor health literacy in those areas, meaning people may be less able to access, understand and use information and services to make informed decisions about their health. 9 The authoring practice is located in a rural area with high levels of deprivation, which is recognised as one of the most deprived regions in the country according to the Indices of Deprivation 2019. The area ranks among the 30 most deprived local authority regions in England, with a significant proportion of the population living in the 50% most deprived areas nationally.
Regarding age, CS uptake is documented to be lowest amongst 20-29-year-olds and those over 50, with studies reporting that women over 45 are more likely to decide to stop attending routine screening as they potentially associate ageing with diminished cervical cancer risk, 10 with a quarter of women aged 50-64 years opting not to participate in the UK. 11 Other potential causes for low uptake may be past painful or traumatic experiences, which the ageing process may exacerbate; a survey by Jos Cervical Cancer Trust found that nearly 30% of women over 50 found their CS more painful with age. 9 These barriers may contribute to the death of at least two women every day from cervical cancer. Identifying and addressing potential barriers is critical to improving the uptake of this vital and lifesaving screening effort and achieving the World Health Organisation’s (WHO) target of eradicating cervical cancer. 12
Regarding cancer care in England, the NHS long-term plan published its strategy to improve outcomes for cancer, with one of its ambitious goals being to increase early cancer diagnosis at stages 1 or 2 from 50% to 75%. 13 To implement this, the NHS plan is to utilise collaborative working across health and care at all levels to deliver better pathways and public health promotion of screening programmes. Primary care is contractually required to deliver cancer services through assessing and monitoring patients, screening and diagnosis and providing support services. By achieving an earlier diagnosis, patients have more treatment options, an increased survival rate, reduced inequalities, and a better quality of life.
Objectives
As a rural primary care practice in an English county with higher-than-average deprivation indices, this intervention aimed to demonstrate how a multidisciplinary team (MDT) approach (Figure 1) could effectively utilise remote communication resources to improve cervical screening uptake. Summary of enhanced process.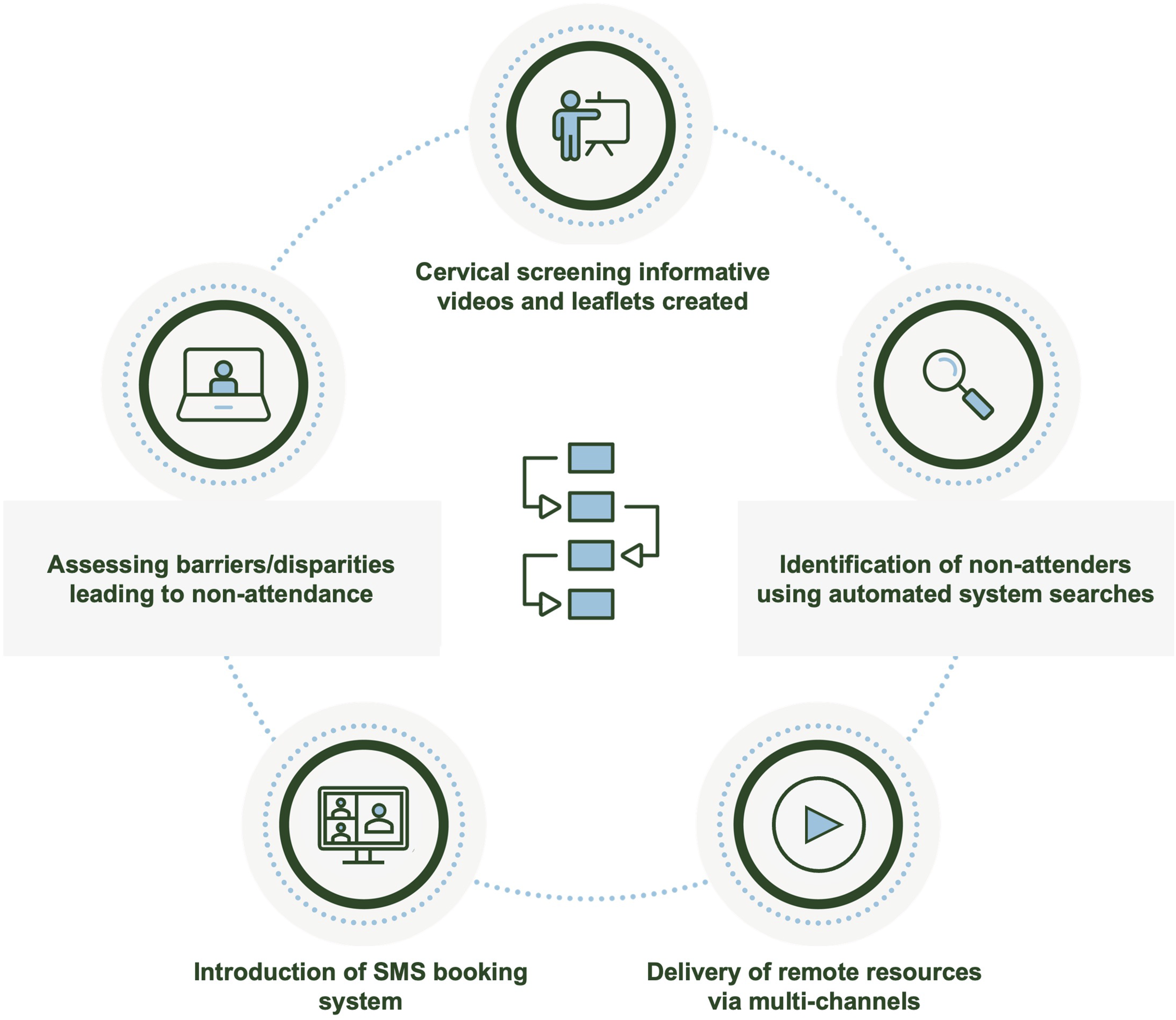
The process was developed based on the hypothesis that remote communication tools - providing accessible health information and education—would enhance screening participation, particularly among harder-to-reach and more vulnerable groups. This supports the NHS Cervical Screening Programme’s (NHSCSP) target of achieving 80% coverage among eligible women annually and aligns with the NHS Long Term Plan’s commitment to improving quality of life, enhancing patient experience, reducing variation, and addressing health inequalities.
Given that previous research has largely focused on SMS reminders and invitation-based strategies, with less emphasis on integrating digital educational resources to support informed participation, this paper aims to contribute to the ongoing discussion on digital patient engagement. By outlining how tailored, practice-led educational interventions can influence screening uptake, we provide a scalable model for enhancing patient awareness, reducing barriers, and improving access to preventive healthcare.
Methodology
This retrospective, observational study employed a structured, multidisciplinary approach to identify and engage patients who had not attended a cervical screening appointment for an extended period.
The Process
1. Patients were identified through targeted electronic patient record (EPR) searches using the following criteria: a. Women eligible for screening and aged 25-49 years who had not had a cervical screening test performed in the previous 3 years b. Women eligible for screening and aged 50-64 years who had not had a cervical screening test performed in the previous 5 years
The EPR was used because of its centralised and standardised data structure that ensures accuracy, consistency, and completeness in patient information. 2. Potential barriers and disparities contributing to non-attendance were evaluated to develop a patient-centred content strategy that would effectively engage and resonate with the target audience 3. Targeted cervical screening resources, including videos and leaflets, were developed with content tailored to the practice and local population. 4. Resources were selectively delivered to the identified groups through multiple channels, including email and SMS platforms like AccuRx 5. A new online appointment booking service was implemented to eliminate barriers associated with in-person or phone bookings. 6. Outstanding patients were actively followed up to reinforce key messages and further improve uptake.
This process was designed to utilise existing resources. The identification of eligible patients was conducted through the EPR using clinical decision support and population health management tools that were already licensed and routinely used by the practice. All communication materials were created in-practice using staff expertise, ensuring relevance to the local patient population. Distribution of the resources was carried out via pre-existing digital communication platforms, such as AccuRx, which were already embedded within the practice’s workflow. By leveraging these established systems and tools, the intervention was implemented efficiently without requiring additional training or financial and technological investment.
The process is easily replicable in other primary care settings, provided similar digital tools and patient outreach strategies are available. Researchers seeking to reproduce this study should ensure access to electronic patient records, automated communication platforms, and multidisciplinary collaboration to optimise patient engagement.
Patient-Centred Content
The communication resources developed for this initiative aimed to provide clear, accessible, and locally relevant information to encourage cervical screening participation. The video, presented by an Advanced Nurse Practitioner from the practice, was designed to create a personalised and familiar connection, helping to build trust and reduce anxiety associated with cervical screening.
The video was under two minutes in length, ensuring that it was concise and easy to engage with. It covered key topics, including why cervical screening is important, what the test involves, and how to book an appointment. The leaflet reinforced the same information, emphasising that cervical screening helps prevent cancer by detecting abnormal cells early. It reassured patients that the procedure is quick, typically taking less than 5 min, and that regular screening significantly reduces the risk of cervical cancer-related deaths. Additionally, the leaflet provided guidance for trans men and non-binary individuals with a cervix, acknowledging the importance of inclusivity in healthcare communications.
Data Analysis
The reporting of this study conforms to STROBE guidelines 14 with the results presented derived from a retrospective analysis of secondary data extracted from the electronic patient record (EPR) system of a single primary care practice. Screening participation rates were compared before and 3 months after the implementation of the intervention to evaluate changes in attendance during this period. Descriptive statistics were used to quantify uptake improvements, with subgroup analyses conducted to identify variations in response between age groups (25-49 and 50-64 years). Given the study’s retrospective, practice-based design, no inferential statistical tests were applied, and the results were interpreted in the context of real-world implementation rather than formal hypothesis testing. Additionally, qualitative insights were drawn from patient follow-up interactions to explore potential reasons for continued non-attendance.
Bias was minimised by using standardised, retrospective data extraction of all eligible non-attenders from the electronic patient record (EPR) system, ensuring systematic patient identification.
All patient data were de-identified prior to analysis to ensure confidentiality and compliance with data protection regulations. The intervention remained unchanged throughout the study period, ensuring that the findings accurately reflect real-world outcomes based on the structured methodology described.
Results
At the time of reporting, the authoring practice had 1441 registered patients aged between 25 and 64 eligible for CS (
Following the provision of remote communication resources, CS uptake increased across both target age groups, with 46% ( Summary of results over 3 months of process enhancement.
Despite the successful screening of over 80% of eligible patients across both age groups, there were still 156 patients who had not attended a screening appointment within the recommended timeframe at the end of 3 months [19% ( Summary of themes arising from qualitative analysis for reasons for non-attendance (
Discussion
This paper emphasises that the national target of 80% coverage of CS in eligible patients in England is realistic and achievable. Working as an MDT using pre-existing automated systems and searches may help reduce administrative and clinical burdens in identifying patients who previously have not responded to screening invitations. This group benefited from a more targeted approach to encourage uptake.
Engaging with non-participants via remote multi-channel methods enables more effective and understandable communication tailored to individuals with potentially poor health literacy. This may encourage them to make more informed decisions about cancer screening services.
Our population appeared to have no limitations regarding using remote technology tools. The most significant improvement in screening uptake was in the older patient group (50-64 years.), suggesting that IT solutions are well-received in this group. Despite concerns that rurality and deprivation could negatively impact uptake, the findings of this study suggest these factors do not appear to impact the success of remote communication methods - it potentially highlights that remote resources improve health literacy, understanding of health information, and screening uptake.
Time invested in considering patient experience may help improve future services and uptake. Our qualitative analysis suggests that a compassionate, patient-centred approach is recommended when exploring why some women are reluctant to undergo screening. Adopting a nonjudgmental understanding strategy ensures patients feel comfortable explaining their reasons for declining screening. This holistic approach allows for further therapeutic relationships between healthcare professionals (HCP) and the patient to be developed.
Policy Implications
This study supports the wider adoption of remote resources to improve cervical screening uptake, aligning with the NHS Long Term Plan and its focus on digital transformation and early cancer detection. Integrating digital education tools into Quality and Outcomes Framework (QoF) indicators and Enhanced Access Services could encourage standardised, proactive patient engagement. Embedding remote strategies within the Investment and Impact Fund (IIF) could further incentivise Primary Care Networks (PCNs) to use digital communication and clinical decision support tools for targeted outreach. Policymakers should consider incorporating practice-led digital education initiatives into national screening guidance to help achieve the 80% screening uptake target, improving early detection and reducing cervical cancer mortality.
Other Relevant Evidence
The findings of this study align with existing research demonstrating the effectiveness of educational interventions in promoting cervical cancer screening. A systematic review highlighted that health education programs significantly increase cervical cancer knowledge and screening behaviours among women, particularly when utilising community-based approaches. 15
Similarly, a quasi-experimental study employing the PEN-3 model found that tailored educational interventions led to a significant rise in participation rates for cervical cancer screening. 16
Furthermore, a systematic review focusing on rural populations identified that theory-driven, community-involved, and healthcare professional-led educational interventions effectively increased both knowledge and uptake of cervical cancer screening. 17
These studies underscore the importance of targeted educational strategies in enhancing screening participation, supporting the approach utilised in our practice.
Study Limitations
While this study provides valuable insights into the role of remote communication strategies in improving cervical screening uptake, its limitations should also be acknowledged.
The sample size was limited to a single primary care practice, meaning the findings reflect practice-specific outcomes rather than broader, generalisable national trends. As a process evaluation, the focus was on the approach and implementation, rather than conducting sensitivity analyses, generating statistical inferences, or assessing cervical screening efficacy at scale. Further research, including focus groups and interviews to obtain qualitative data at a population level is needed to examine specific barriers influenced by socio-economic status, ethnicity, cultural factors, and digital literacy, which could inform more tailored approaches across diverse communities.
As a single-arm study without a control group, potential confounding factors—such as natural variations in screening uptake, external public health campaigns, or other unmeasured influences—could not be fully adjusted for. Future studies could include multiple primary care practices to assess generalisability across different populations and settings.
Additionally, the data presents a short-term snapshot rather than long-term trends in screening behaviour. A follow-up study, once the initiative has been in place for a longer period, could assess sustained engagement, re-screening rates, and potential diminishing effects over time, leading to the modelling of health economic benefits.
Further investigation exploring patient experience and their potential lack of engagement in CS may also be warranted. This could consider the effects of menopause, mobility, psychological issues, trauma, social factors, and chronic/acute illness.
Conclusion
In the authoring practice, the use of remote communication tools raised awareness in the community about the importance of CS and increased uptake. The outcomes of this study suggest that a compassionate, patient-centred approach may enhance the therapeutic relationship between HCPs and patients, potentially enhancing health outcomes.
Unlike large-scale national campaigns, a personalised, practice-level approach, where familiar healthcare professionals deliver educational content, may foster trust and engagement within the local patient population.
By leveraging existing resources, this study presents a scalable, cost-neutral model that can be readily implemented across other primary care settings and Primary Care Networks (PCNs), enhancing cervical screening uptake without imposing significant financial or administrative burdens.
Footnotes
Acknowledgements
The Authors would like to thank the practice staff at Marsh Medical Practice for their ongoing contribution to the provision of care for its patients.
Statements and Declarations
Consent to Participate
Due to the nature of this case series and the absence of any patient-identifiable information, formal patient consent was not required. All data presented in this article were anonymised and obtained from medical records and healthcare professionals involved in the patients' care. No personal or identifying details of the patients are included in this report. The cases described herein are based solely on clinical information relayed by the treating physicians and other healthcare team members, ensuring patient confidentiality while maintaining the integrity of the medical observations and outcomes reported.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that support the findings of this study are derived from clinical case notes and healthcare professional observations. Due to the nature of this research, supporting data is not available.
