Abstract
Ergonomic microbreaks such as the OR-Stretch can address work-related musculoskeletal pain among surgeons and potentially alleviate burnout and early retirement. Fifteen surgeons at a single institution completed two operative cases using the OR-Stretch, once using the Scheduled (every 45 min) timing strategy and once using the Self-Determined (between 30 and 60 min based on surgeon preference) strategy. Eight surgeons preferred the Scheduled timing strategy, and seven preferred Self-Determined (p = .80). The stretch was skipped 16% of the time using the Scheduled strategy and 6% with the Self-Determined strategy (p = .18). Personal interest, improved mental focus, and ease of remembering were cited as the most influential factors for continued usage, while the most influential factor for not continuing was forgetting to use it. Self-determined intervals for intraoperative microbreaks represent a valid and potentially preferable implementation approach. Efforts to promote long-term adoption of microbreaks should focus on reminding surgeons to use them during operations.
Introduction
Surgery is a capital-intensive service requiring significant physical and human capital resources. Surgeons represent the primary human capital input, and, like tools and technology, they are susceptible to physical depreciation over time. Due to the nature of their work, surgeons’ health can be impacted by work-related pain and musculoskeletal disorders (Epstein et al., 2018; A. Park et al., 2010). A meta-analysis by Epstein et al. (2018) estimated a 35% to 60% prevalence of work-related musculoskeletal pain among surgeons and interventionalists. Among surgeons who regularly perform laparoscopic surgery, A. Park et al. (2010) discovered that 87% report associated physical symptoms or discomfort. This results in a substantial “disability burden,” and as Epstein et al. (2018) report, 12% of surgeons and interventionalists who had work-related musculoskeletal disorders required restrictions or modifications in their practice, a leave of absence, or early retirement.
The consequence of premature retirement is significant in the context of an ongoing physician shortage. By 2034, the Association of American Medical Colleges forecasts a supply deficit of 15,800 to 30,200 surgical specialists (AAMC, 2021). Early retirement due to occupational pain and discomfort contributes to further constriction of our nation’s surgical workforce relative to patient demand. In addition to an individual well-being perspective, addressing the ergonomics of surgery is of value to the national workforce and patient population.
Intraoperative breaks, which may be called “micropauses” or “microbreaks,” have been proposed as effective, evidence-backed solutions to improve surgeons’ pain, fatigue, accuracy, and stress during an operation (Dorion & Darveau, 2013; Engelman et al., 2011; Hallbeck et al., 2017; A. E. Park et al., 2017). In a 2010 randomized trial with seven surgeons over 51 laparoscopic operations, Engelman et al. (2011) reported that 5 min breaks every 25 min were associated with improvements in fatigue and stress. Dorion and Darveau (2013), in a crossover experiment of 10 surgeons and six surgery residents each over two cases, demonstrated that 20 s “micropauses” every 20 min during an operation improved discomfort and muscular fatigue. Hallbeck et al. (2017) performed a multicenter study of 56 surgeons over two operative days each, in which the first was a control day and the second involved guided stretching microbreaks of 1.5 to 2 min every 20 or 40 min throughout the operation. This intervention resulted in a significant reduction in shoulder pain compared to operating without the microbreaks, with 57% of surgeons reporting improved physical performance when using the stretch (Hallbeck et al., 2017).
As the evidence base builds for stretching microbreaks as an effective ergonomic intervention for surgeons, a couple of key questions remain unanswered. First, the aforementioned studies were designed to introduce stretching microbreaks at predetermined intervals throughout the operation. However, surgery is a high-pressure environment where disruptions to the workflow can have significant consequences for the patient and operative team. It is therefore important to balance the implementation of microbreaks with the continuity of the operation. Rather than rely on a timer to determine when to stretch, surgeons could decide on their own when to take a break. The former strategy (Scheduled) gives them less to think about during the operation but may conflict with critical moments in the operation, leading to skipping the stretch to avoid compromising the operative outcome. The latter strategy (Self-Determined) may fit better within the natural flow of the operation but does require more thought for the surgeons and may be distracting. To our knowledge, these distinct strategies for microbreak implementation have yet to be compared, which is the primary objective of this project.
Second, for long-term efficacy, microbreaks need to be performed consistently over time. Hallbeck et al. (2017) report that 87% of the surgeons involved in their multicenter study said they would like to routinely incorporate stretching microbreaks into their practice. They did not report follow-up data, however, that examined whether this interest led to adoption. It is the second objective of this study to examine the degree to which surgeons continue to employ microbreaks after they have been introduced, as well as which factors are influential in helping or hindering continued use. This question of permanence or adoption has workforce-level implications. As described by Leggott et al. (2016), there is often a gap between the discovery of an effective innovation and its widespread implementation across a system. To help address the labor implications of early retirement secondary to work-related musculoskeletal disorders, ergonomic interventions such as microbreaks must be adopted over long periods of time and diffused widely among the workforce. Accordingly, in addition to their efficacy and efficiency, an essential question for microbreaks is how they can be more easily adopted into routine practice. This is the second objective of this project.
The specific microbreak intervention that we examine in this study is the “OR-Stretch” a 70 s stretching routine that surgeons can perform during an operation while maintaining the sterile field (Mayo Clinic, 2024a). The OR-Stretch was developed by Dr. Susan Hallbeck and colleagues at the Human Factors Engineering Lab at Mayo Clinic in Rochester, Minnesota (Mayo Clinic, 2024b). Our objective is to investigate how to make the OR-Stretch more efficient to implement and easier to permanently adopt for surgeons who wish to incorporate it into their practice. First, we will investigate whether participating surgeons prefer the Scheduled or Self-Determined timing strategy. Second, we will explore factors influencing continued OR-Stretch adoption.
Methods
Surgeons from various specialties at Mayo Clinic in Florida were recruited by email invitation to participate in this IRB-approved study (IRB #: 23-006415). Among those willing to join, participants were selected based on the inclusion criteria of expected case lengths of 2 to 6 hr during which the participating surgeon performed at least 50% of the procedure. Sixteen surgeons were selected to perform two cases using the OR-Stretch from July 24 to August 25, 2023. Cases for each surgeon were selected to optimize the similarity of the two procedures given the project’s scheduling constraints including personnel availability and overlapping operations between participants. Surgeons were randomized to either the Scheduled (every 45 min) or Self-Determined (between 30 and 60 min based on surgeon preference) timing strategy for their first case and completed their second case using the other timing strategy. Randomization was performed using block randomization with a block size of 4.
During each case, the publicly available OR-Stretch Web App (Mayo Clinic, 2024a) was used to provide both a timer and video demonstration for the stretch, which, when feasible, was broadcast to one or more television screens in the operating room. The timer was started following the operative “time-out.” For Scheduled cases, a 45 min timer (the default interval for the OR-Stretch app) marked when to stretch. At each alarm, the surgeon could decide to stretch, “snooze” the stretch for up to 10 min, or skip the stretch. The timer was reset to 45 min after each stretch or skip. For Self-Determined cases, the timer was set to 30 min. At the alarm, the timer was reset for 30 min, and the surgeon was instructed that their 30 min stretching window had begun. During the window, they could decide at any point to stretch. This window encouraged a stretching interval of 30 to 60 min, selected to approximate the 45 min interval from the Scheduled strategy for reasonable comparison. If they had not yet performed the stretch at the end of the window, their options were to stretch, snooze for up to 10 min, or skip. At the end of each stretch or skip, the timer was reset for 30 min. All 30 cases were personally overseen by the primary author.
Postoperative surveys were administered following each case to collect case-specific data and feedback on the usability of the OR-Stretch and to assess the surgeon’s preference between the two break-timing strategies. The intraoperative impact of the OR-Stretch on four variables was assessed: mental focus, physical performance, body pain/discomfort, and level of fatigue.
A 2 month follow-up survey and optional interview were conducted to evaluate continued usage and discuss strategies to promote adoption. Preference for timing strategy was analyzed using the z-test for proportions; the difference in the number of skips under each timing strategy was assessed with Chi-square analysis.
Results
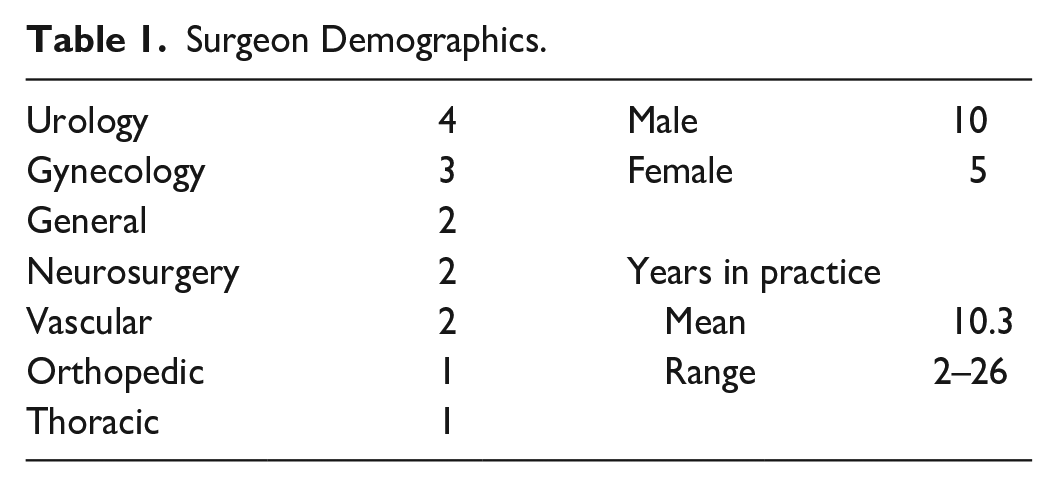
Fifteen surgeons from seven specialties completed two surgical cases according to the study protocol (Table 1). Thirty-three percent of participants were female. Mean years in practice was 10.3 with a range of 2 to 26 years.
Surgeon Demographics.

Cases included open, robotic, and laparoscopic surgical approaches (Table 2). The platform was identical across the Scheduled and Self-Determined cases for all but one surgeon.
Case Statistics.
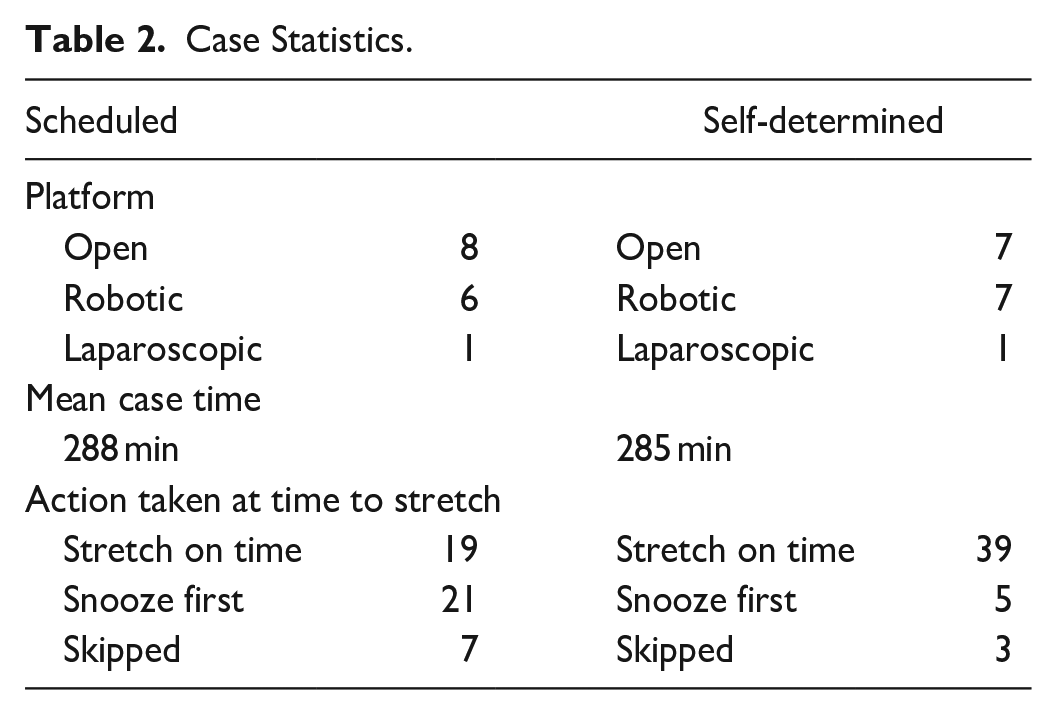
After completing one case with either strategy, eight surgeons preferred the Scheduled timing strategy, and seven preferred the Self-Determined strategy, resulting in an insignificant difference in preference (p = .80). At the alarm, the stretch was skipped 16% (7/47) of the time under the Scheduled strategy and only 6% (3/47) of times with the Self-Determined strategy; however, the difference was not significant (p = 0.18) (Table 2).
For all participants, using the OR-Stretch either improved or did not impact mental focus, physical performance, body pain/discomfort, or fatigue. No participant reported that the OR-Stretch worsened any of these four outcome measures during the 30 cases studied. The impact on each outcome was comparable between timing strategies without significant differences (Figure 1).
Of the 14 surgeons who completed the 2 month follow-up survey, six (43%) had used the OR-Stretch at least once on their own following its introduction during the two study cases. Of these, five utilized the Self-Determined timing strategy, and one used both strategies. Among those who continued to use the OR-Stretch, the most influential factors for continued usage as measured by influence (scale: 0–3; 3 = highest influence) were improved mental focus (2.0), personal interest (2.0), and ease of remembering (2.0). Other supporting factors included improvements in body pain/discomfort (1.8) and fatigue (1.7), support from the operative team (1.7), and desire for physical longevity (1.7). Among the others, the most influential factor for not continuing to employ the OR-Stretch was forgetting to use it (2.4), followed by distraction from the operation (1.5) and inefficiency (1.4) (Table 3).
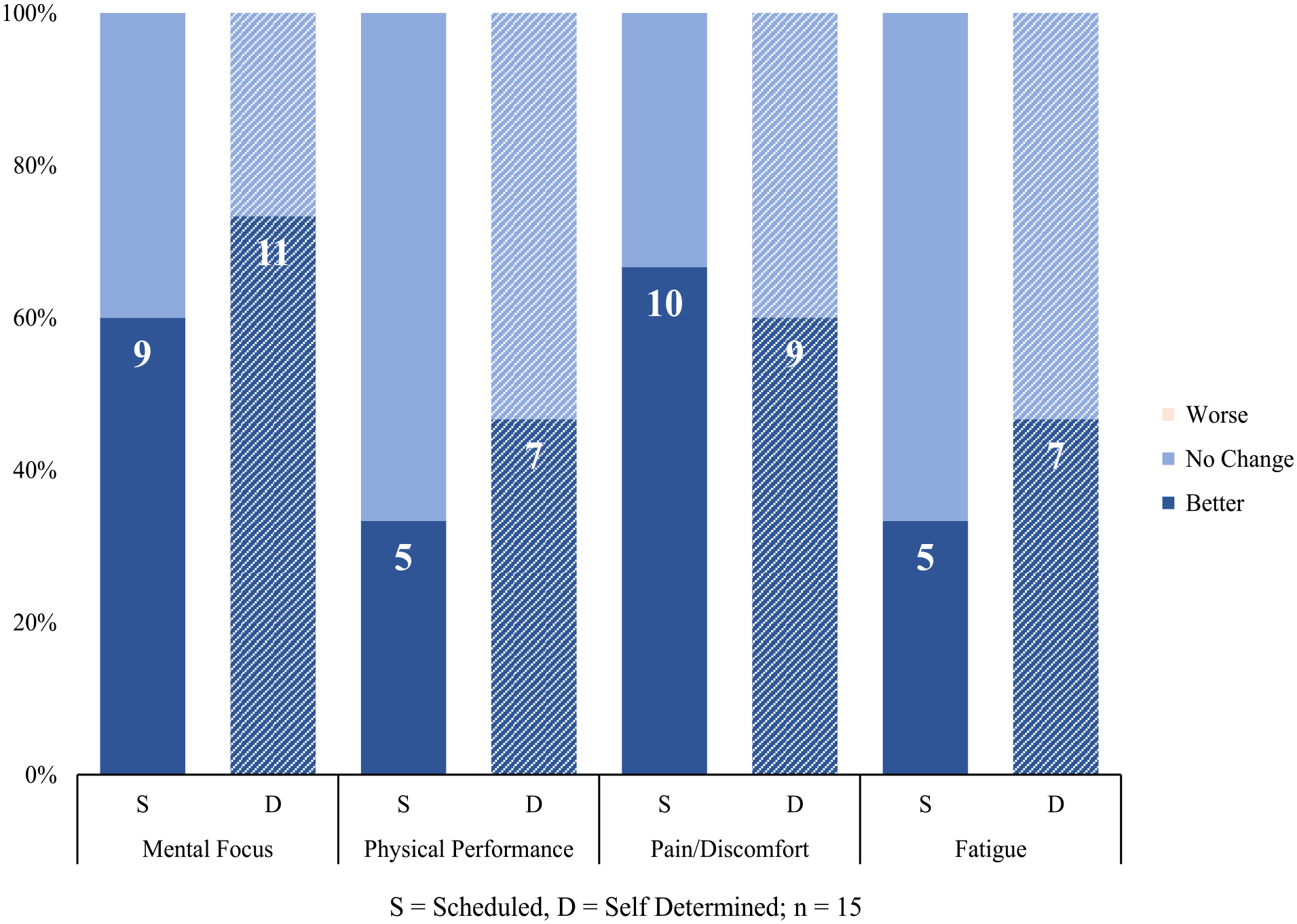
Intraoperative impact of the OR-stretch.
Factors Impacting Decision to Continue Using the OR-Stretch.
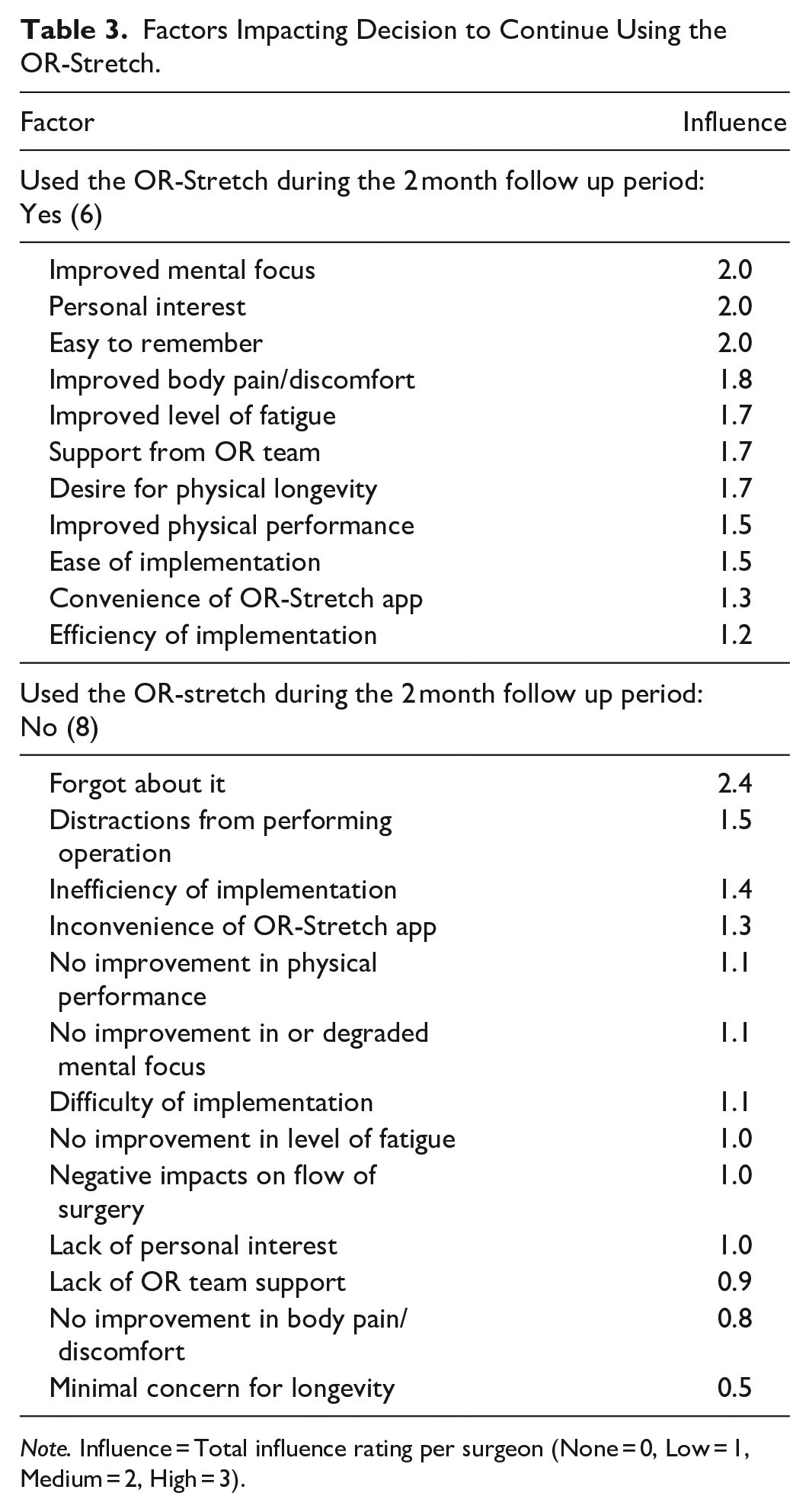
Note. Influence = Total influence rating per surgeon (None = 0, Low = 1, Medium = 2, High = 3).
Discussion
This small-scale crossover study of 15 surgeons and 30 operative cases sheds light on two key questions facing the proposed solution of intraoperative microbreaks to the widespread problem of work-related musculoskeletal pain and injury among surgeons. First, our survey results are equivocal for a preference for either strategy but suggest that Self-Determined timing is a valid approach for microbreak implementation. There were fewer (statistically nonsignificant) skipped stretching opportunities under the Self-Determined approach (3/47; 6%) compared to the Scheduled approach (7/47; 16%). This indicates the benefit of flexibility offered by a Self-Determined strategy, as surgeons are able to incorporate breaks into the flow of the operation at natural transition points or moments of low intensity and thereby avoid skipping the stretch. Furthermore, all six of the surgeons who employed the OR-Stretch on their own after the two introductory cases used the Self-Determined strategy, whereas the Scheduled strategy was employed by only one surgeon (who employed each on at least one occasion). This contrast in strategy selection occurred when surgeons were no longer supervised and assisted by study personnel, with the freedom to use the OR-Stretch according to their preference, suggesting that the Self-Determined timing may be more favorable for long-term individual use.
Second, the follow-up data adds to prior studies by assessing post-introduction adoption of intraoperative microbreaks. Only 6 of 14 surgeons used the stretch on their own at any point in the 2 months after their second introductory case. Whether surgeons found it easy to remember or whether they forgot about the OR-Stretch was a primary reason for determining their continued use. Therefore, for surgeons or departments who want to implement the OR-Stretch or similar interventions individually or at scale, identifying methods to help the surgeon and his or her team remember the stretch at the time of operation should be a primary focus. The development and assessment of reminder strategies, which could include placing posters on the operating room wall, involving the surgical team in the microbreak process, or incorporating microbreaks into the surgical time-out (Papadakis et al., 2019) are avenues for future investigation.
This study includes major limitations, principally its small sample size. With 15 participants over 30 total cases, it falls short of being able to provide statistical significance for its findings. While the two cases were randomized to which timing strategy a surgeon employed first, differences in the operations performed even if they were on the same platform and differences in patient-specific operative findings even if the two procedures were similar prevented an adequately controlled environment for a direct comparison of superiority between the Scheduled and Determined strategies. Furthermore, this project was confined to a single institution.
Despite these recognized limitations, the study offers to the existing literature an initial investigation of diverse timing strategies for intraoperative microbreaks, proposing Self-Determined timing (selected within in interval of 30–60 min, in this study) as a legitimate and potentially preferable approach for implementation. Though not a controlled trial, internal validity was promoted by all cases being overseen by the first author.
As a small, single-center study, this project may serve as a “three-quarter turn” of the Plan-Do-Study-Act cycle for future projects focused on the introduction and adoption of the OR-Stretch or similar ergonomic interventions. Based on our study design (Plan), execution and data collection (Do), and analysis (Study), other researchers may use this study as a basis for developing larger-scale projects focused on similar questions (Act) in efforts to address the day-to-day physical demands borne by our nation’s surgeons.
Conclusion
Self-determined intervals for intraoperative stretching microbreaks are not evidently superior to predetermined intervals but represent a valid and potentially preferable implementation approach. Strategies to promote surgeons’ continued adoption of the OR-Stretch or similar resources for maximal ergonomic benefit should focus on reminding surgeons to use them during operations.
Footnotes
Acknowledgements
We thank David Sklar, MD for his guidance throughout this project.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
