Abstract
Cardiac sonographers are frequently exposed to ergonomic risks such as postural stress and high levels of physical exertion while performing scanning tasks, contributing to work-related pain, and discomfort among cardiac sonographers. Passive exoskeletons are a potential ergonomic intervention with the potential to mitigate some of the risks associated with scanning. This study examined the effectiveness of a passive upper body exoskeleton in reducing the levels of work-related pain, discomfort, and workload in cardiac sonographers while performing transthoracic echocardiograms (TTE). Twelve cardiac sonographers were asked to use the HAPO FRONT exoskeleton while performing TTEs during a full workday. Participants were asked to rate their body part discomfort and workload throughout the day, both with and without the exoskeleton. The exoskeleton did not significantly decrease discomfort or workload associated with performing TTEs, except for a slight reduction in the discomfort at the left hand/wrist. This result indicates that the HAPO FRONT was not effective or appropriate for use by cardiac sonographers. Future development and study of purpose-designed exoskeletons for healthcare applications may provide greater benefits to cardiac sonographers.
Keywords
Introduction
Work-related musculoskeletal disorders (WRMSDs) and discomfort are highly prevalent among cardiac sonographers. Previous studies have shown that as many as 91% of sonographers experience pain due to scanning (Russo et al., 2002). Cardiac sonographers often are exposed to postural stress and exertions from scanning patients. Cardiac scans such as transthoracic echocardiograms (TTEs) often require sonographers to abduct shoulder across patient while holding the transducer against the patient’s body to obtain quality images; which can elevate their risk of developing WRMSDs and work-related pain (Barros-Gomes et al., 2019; Russo et al., 2002; Tetteh et al., 2023). Additionally, scanning patients with higher body mass indexes often require additional effort from the sonographers to obtain quality pictures, further elevating their risk of developing musculoskeletal disorders in the upper extremities (Pallotta & Roberts, 2017).
Ergonomic interventions have been developed and trialed to mitigate the risks. One intervention that has been proposed is ambidextrous scanning (alternating between holding the transducer between the right and left hand for subsequent cases). This has been shown to significantly reduce the incidence of musculoskeletal disorders in sonographers, while maintaining image quality (Bastian et al., 2009; Seto & Biclar, 2008). However, this intervention is limited by the need for additional training for sonographers in ambidextrous scanning and the need to rearrange the workstation between cases, as the workstation layout differs between right- and left-handed scanning.
Recently, exoskeletons have been trialed in healthcare settings as a potential ergonomic intervention. Exoskeletons have been introduced and shown to be usable and acceptable in healthcare settings (Wang et al., 2021). Tetteh et al. (2023) tested two arm-support exoskeletons, the Levitate Airframe and the Levitate FLEX, in reducing muscle activity while performing TTEs. However, they found them to be of limited effectiveness in reducing muscle activation of the deltoid and upper trapezius muscles due to design limitations. Thus, with improved designs, exoskeletons remain a potential ergonomic intervention for cardiac sonographers.
The exoskeleton in this study (HAPO FRONT) has been shown to reduce muscle activation of the anterior deltoids and biceps and the perceived exertion during a simulated manual handling task (Le Tellier et al., 2021). The HAPO FRONT has shown to be effective in supporting the arms in laboratory studies. Thus, we hypothesized that the exoskeleton would potentially be an effective ergonomic intervention to reduce work-related pain, discomfort, and workload in sonographers, as sonography involves high levels of shoulder abductions and upper arm exertions (Barros-Gomes et al., 2019; Russo et al., 2002; Tetteh et al., 2023). The current study examined the effectiveness of the HAPO FRONT in reducing subjective work-related discomfort, fatigue, and workload in cardiac sonographers while performing TTEs over a full workday.
Methods
Participants
A total of twelve cardiac sonographers who regularly perform TTEs were recruited for this study from a quaternary care academic hospital in the midwestern United States.
Equipment
The HAPO FRONT (Ergosanté, Anduze, France) is a passive upper extremity exoskeleton that is designed to support the upper arms when the shoulder joints are abducted and/or flexed by offloading the weight of the upper arms to the upper back (Figure 1).
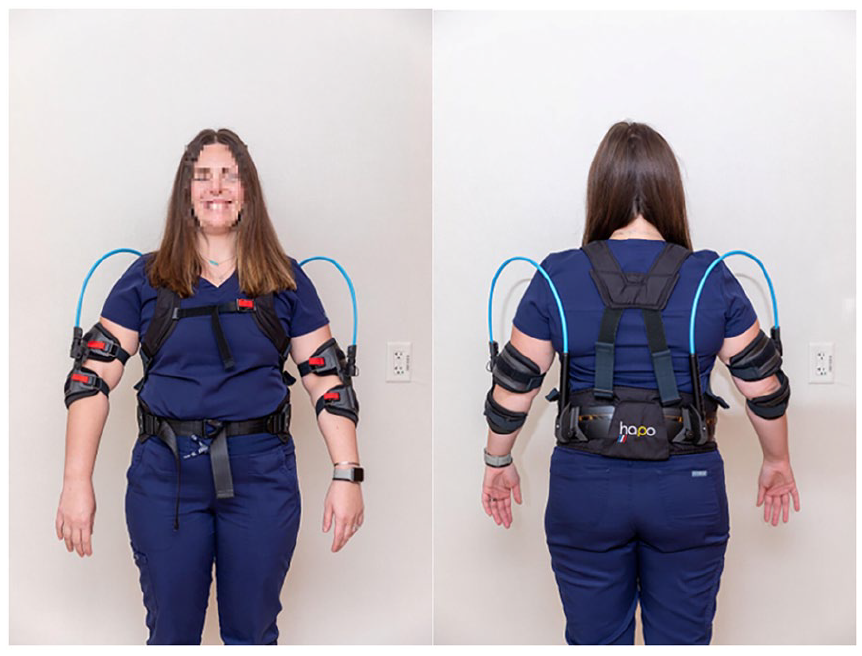
The front (left) and back (right) of a sonographer wearing the HAPO FRONT. Reproduced with permission of Mayo foundation for medical education and research. All rights reserved.
The HAPO FRONT supports the arms using two fiberglass composite elastic spring rods that attach onto a cuff at the elbow and the back. This provides support to the arms when the shoulders are abducted and/or flexed during a scanning task (Figures 2 and 3).
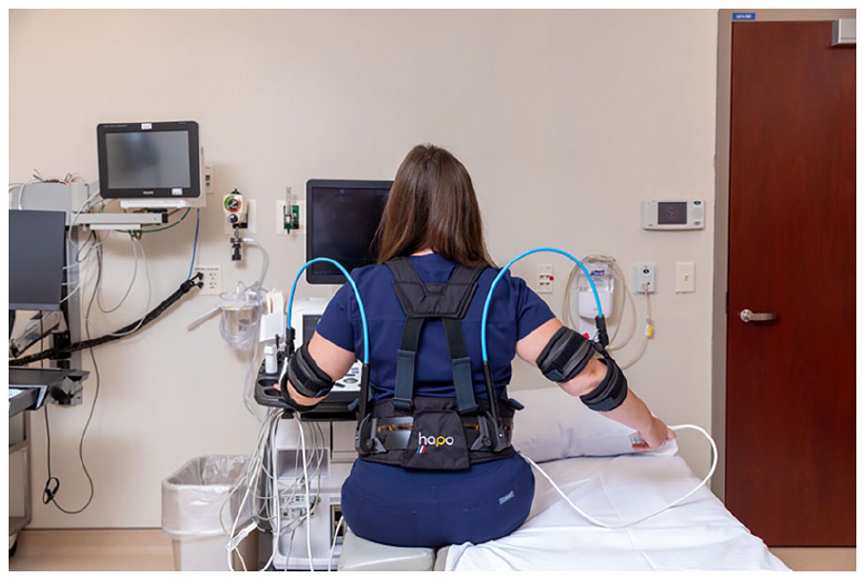
A typical right-handed scanning posture while wearing the HAPO FRONT. Reproduced with permission of Mayo foundation for medical education and research. All rights reserved.
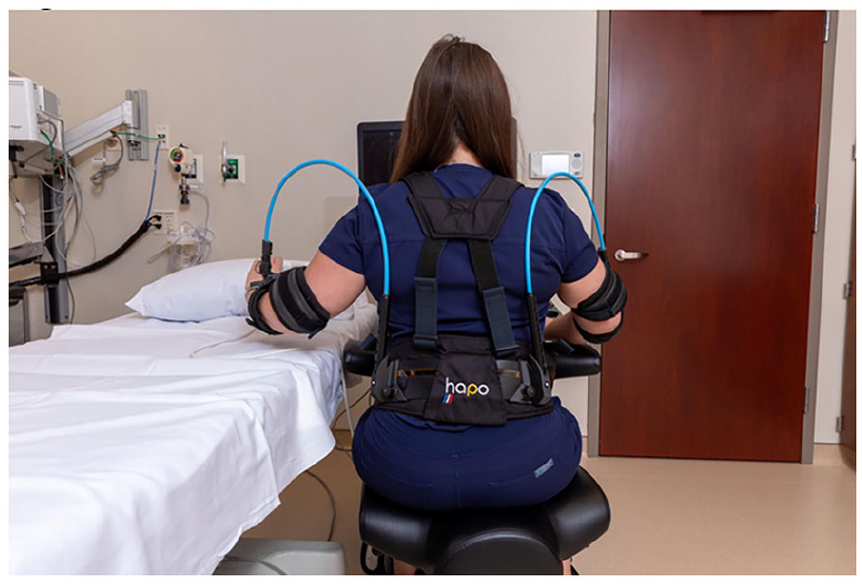
A typical left-handed scanning posture while wearing the HAPO FRONT. Reproduced with permission of Mayo foundation for medical education and research. All rights reserved.
The spring rods come in two strengths: a softer spring that can provide a support level of up to 4 kg and a stronger spring that can provide up to 6 kg. Users were allowed to select their preferred rod strength for the study.
Procedure
The feedback about the utility of the HAPO FRONT arm exoskeleton to mitigate the development of discomfort and workload throughout a scanning day while performing TTEs was accomplished by questionnaire.
For each trial participation day, each sonographer completed a questionnaire that asked them to rate the discomfort experienced in their shoulders, upper arms, wrist/hands, and their upper and lower back on a scale from 0 (none) to 10 (maximum) on a Borg CR-10 scale (Borg, 1982). Participants also noted if they used their right hand or left hand during the TTEs. This questionnaire was administered three times during the scanning workday: morning (before the first TTE), midday (at around noon or at the start of their lunch break), and at the end of the workday. During the midday and end of day, they also answered questions about their perceived workload utilizing the NASA Task Load Index (NASA-TLX) (Hart & Staveland, 1988). On the days that the participant wore the exoskeleton, a set of usability-related questions was administered at the end of the day. The usability questionnaire contained questions pertaining to any discomfort, interference, or other issues that they experienced while wearing the exoskeleton.
Each participant in the study performed TTEs both with and without the exoskeleton. Prior to the start of data collection for each participant, each sonographer was fitted with the HAPO FRONT with assistance from the study personnel trained to properly fit the exoskeleton. Each participant then performed a trial TTE with the exoskeleton where no data was collected for the sonographers to be familiarized with the exoskeleton to reduce learning effects. If needed, additional adjustments were made after the trial case.
Following the fitting and trial case with the exoskeleton, data was collected on each sonographer for an entire day. Each sonographer wore the exoskeleton for an entire shift, performing around 4 to 6 TTEs per day over an entire workweek (3–5 days). To obtain a baseline measurement for comparison, questionnaire responses were collected for an additional 1 to 2 scanning days without the exoskeleton following the completion of the exoskeleton trial period.
Experimental Design
Differences in discomfort scores were calculated for each body part between the HAPO FRONT and baseline conditions throughout the scanning day. The Mann-Whitney U test was used to compare the midday and end of day discomfort changes between the two conditions.
To determine if the use of the exoskeleton impacted subjective workload experienced by the sonographers, the NASA-TLX scores at midday and end of day were also compared between the HAPO FRONT and baseline conditions using the Mann-Whitney U test. Analyses were performed using SPSS (IBM Inc., Armonk, NY). A 5% level of significance was used.
Results
A total of 12 (2 male, 10 female) participants were recruited for this study. However, five participants did not wear the exoskeleton for the entire study period (e.g., the whole workweek). The reasons given for discontinuing use of the exoskeleton include increased fatigue/discomfort in the upper arms (4/5 participants) and range of motion (ROM) restrictions in the arm (1/5 participants). There were seven participants who wore the exoskeleton during the entire study period. The exoskeleton was worn for a total of 33 scanning days from the 12 participants. A total of 16 days of baseline data was collected from the 12 participants.
Body Part Discomfort
The results from the Mann-Whitney U test found that the left upper arm discomfort was significantly higher at midday in the exoskeleton condition with a mean increase of 0.48 points on a scale from 0 (none) to 10 (maximum) (M = 0.48, SD = 1.064), compared to the baseline condition (M = −0.08, SD = 0.289).
The left wrist/hand discomfort was significantly lower in the exoskeleton condition at the end of day (M = −0.03, SD = 0.984) when compared to the baseline (M = 0.50, SD = 0.905), indicating that the exoskeleton decreased the fatigue in the left wrist/hand throughout a scanning day; however, this alone is unlikely to justify use of the exoskeleton, as the exoskeleton was not designed to provide support to the wrist and hand. There were no other significant differences in the self-reported discomfort in any other body part.
Workload
The Mann-Whitney U test for differences in the workload between the two conditions measured midday and at the end of day on the NASA-TLX did not differ significantly between the exoskeleton and baseline conditions for the mental demand, physical demand, temporal demand, performance, effort, or frustration subscales. The use of the exoskeleton did not significantly affect the perceived workload during the TTEs for any of the subscales.
Usability
The usability data showed mixed results regarding the comfort and usability of the exoskeleton. Participants reported the most benefit from the exoskeleton when scanning patients with smaller body mass indexes, with 4 out of 12 participants describing a benefit and when scanning the apical window (3/12). The most common issues experienced with the exoskeleton included restriction of the range of motion (7/12), where some participants reported having to “fight” against the elastic springs in the exoskeleton while scanning the patients. Other issues include problems with clearance from the patient while scanning (4/12), and irritation and discomfort from the arm straps (2/12). When asked “Given the choice, would you want to use the exoskeleton in future TTE procedures?,” only 2/12 (17%) participants answered “yes,” with the remainder (10/12; 83%) answering “no.”
Discussion
In this study, we compared the subjective discomfort and workload of performing TTEs with and without the HAPO FRONT, a passive arm-support exoskeleton. While the use of the exoskeleton was associated with lower discomfort in the left wrist/hand, the degree of difference was not large enough to justify use of the exoskeleton. Additionally, the exoskeleton caused a significant degree of upper arm discomfort in some participants; this was consistent with the high attrition rate among the participants who mostly cited upper arm discomfort as their primary reason for discontinuing their trial of the exoskeleton. Additionally, the HAPO FRONT did not significantly change perceived workload on the NASA-TLX when compared to baseline at either midday or end of day for any of the subscales.
The lack of discomfort and workload reduction may have been due to the exoskeleton design, specifically the exoskeleton’s engagement angle, as the design of the HAPO FRONT may not have provided enough support to the arms when sonographers are holding a typical scanning posture. Tetteh et al. (2023) proposed that a shallow engagement angle of 25° to 35° is optimal for TTE scanning tasks.
In addition to the lack of discomfort and workload reduction, the exoskeleton was associated with significantly increased discomfort in the upper arms, leading to a high attrition rate in participation in this study. A systematic review by Kranenborg et al. (2023) found that discomfort was the most common side effect from exoskeleton use and identified improper exoskeleton fit and decreased range of motion as potential causes. Since the participants were fitted with the exoskeleton by study personnel who were trained on the proper fit of the exoskeleton, followed by a trial case prior to data collection, it is unlikely that the participants had significant issues in the fit of the exoskeleton. Consequently, the limitations of the range of motion (ROM) may have caused the discomfort. In our study, many participants reported that the exoskeleton restricted their ROM or made it more difficult to adopt certain postures while performing TTE. This is shown in the usability data where 7 of 12 participants experienced some ROM restriction during the trial. It is possible that the design of the HAPO FRONT did not provide the support that met the sonographers’ needs for the TTEs, resulting in the discomfort experienced as well as the lack of benefit from the exoskeleton.
The usability data and the information from those participants that stopped wearing the exoskeleton before the conclusion of the study show that the exoskeleton caused significant discomfort (in the form of upper arm soreness, skin irritation, and discomfort from the straps) to participants.
Additionally, as evidenced by the low rate of interest in using the exoskeleton in the future (2/12 participants) from the usability survey, and the high attrition rate in the study (5/12; 42%), this discomfort was significant enough to be a barrier to the use of the exoskeleton while performing TTEs.
Since this exoskeleton was not effective in reducing subjective work-related discomfort or workload associated with performing TTEs, and the increased upper arm discomfort caused by the exoskeleton, the HAPO FRONT could not be recommended for performing TTEs during cardiac sonography.
There are limitations that need to be considered when applying the results of this study. For example, the sample did not capture an equal number of male and female sonographers (10 out of 12 participants were female). However, this demographic distribution reflects the female dominance (74%) (Barros-Gomes et al., 2019) of the sonography profession.
Nevertheless, an increased sample size that includes more males would enable comprehensive analyses to explore gender differences in exoskeleton benefits as anthropometric or strength disparities may play a role in the effectiveness and comfort. Additionally, this study only examined subjective measures of discomfort and workload and did not examine variables such as postures or muscle activity. Thus, information on postural and muscle activity changes due to the exoskeleton cannot be extracted from this study.
Future studies should examine how to design exoskeletons to better fit the needs of sonographers to minimize the potential of any discomfort posed by the exoskeleton and to improve effectiveness in reducing work- related discomfort and workload associated with performing TTEs. Exoskeletons that are purpose-designed for healthcare use, particularly for sonography related tasks, may show better results in further testing.
Conclusion
This study examined the effectiveness of an arm support exoskeleton in reducing subjective discomfort and workload in cardiac sonographers while performing transthoracic echocardiograms. This study did not find evidence of a significant reduction in the discomfort or workload when compared to baseline metrics, and significantly increased arm discomfort. Further studies should examine other exoskeletons that may better meet the needs of sonographers or pursue other interventions.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
