Abstract
When the brain is exposed to large circulating levels of Clostridium perfringens type D epsilon toxin (EXT), microvascular damage with resulting severe, generalized, vasogenic edema seems to be principally responsible for the ensuing acute, and frequently fatal, neurologic disorder. However, although the blood–retinal barrier resembles in many respects the blood–brain barrier, retinal changes in livestock with acute epsilon intoxication have not, to the authors’ knowledge, been previously reported. In rats given an acute dose of ETX, retinal microvascular endothelial injury led to widespread vasogenic edema as assessed immunohistochemically by marked plasma albumin extravasation. As laboratory rodents are a good model of the domestic livestock disease produced by ETX, it is probable that the latter sustain some visual deficit when exposed to large doses of this potent neurotoxin.
Clostridium perfringens type D epsilon toxin (ETX) produces an acute or peracute neurologic disorder in lambs, goats, and, less commonly, calves, when high circulating toxin doses follow absorption of excessive quantities from the small intestine. Epsilon toxin then causes cerebral microvascular endothelial damage; severe, diffuse vasogenic edema; a marked increase in intracranial pressure; convulsions; and, often, death.1,3
Epsilon toxin accumulates preferentially in the brain and kidneys, but also in other tissues, including the eye. 9 However, ocular changes attendant on ETX exposure have not, to the authors’ knowledge, been previously reported.
Because the blood–brain barrier (BBB) is a prime target for ETX-induced disruption1,3 and the blood–retinal barrier (BRB) resembles the BBB in many important respects, 6 it seemed likely that this toxin might also injure the BRB. The BRB plays an important role in the homeostatic regulation of the retinal microenvironment and is comprised of inner and outer compartments. 6 The inner BRB is formed by interendothelial tight junctions in capillaries and the outer by tight junctions between retinal pigment epithelial cells. Disruption of the BRB produces increased vascular permeability and vasogenic edema, which impairs vision, 6 in a manner similar to the neurological disturbance caused by BBB breakdown in the brain. The rat is a good experimental model in which to study ETX-induced brain injury 4 and, accordingly, this species was used to examine ocular changes produced by ETX.
Studies were conducted in four 6-week-old, Sprague–Dawley rats weighing 160–180 g. The epsilon toxin a used was produced by growth of a highly toxigenic C. perfringens type D vaccine strain. Culture supernatant containing inactive prototoxin was activated at pH 7.5 by trypsin (0.08% weight/volume) for 30–45 min at 37°C to form the active epsilon toxin, which was then sterile filtered. Assay by a commercial facility a showed that the batch of toxin used in the present study contained 386 L+/ml (where 1 L+ = the amount of toxin neutralized by 1 International Unit of antitoxin) and 69,000 mouse minimum lethal doses (MLD)/ml. The toxin was then frozen at −60°C, at which temperature it is very stable (CSL, a personal communication, 2012). The trypsin-activated toxin was injected intraperitoneally at a dose rate of 1 ml per rat, after a 1:300 dilution of toxin as an acute dose, which causes death 4–6 hr after administration. 2 By contrast, a 1:3,000 dilution produced a sublethal, more prolonged clinical course with multifocal necrotic brain lesions,2,4 resembling those found in sheep after a more protracted intoxication with lower toxin doses (or in partially immune animals), termed focal symmetrical encephalomalacia.1,3 At 3-hr postinjection of toxin, rats were euthanized by perfusion-fixation of the brain with 4% paraformaldehyde via a needle inserted into the beating left ventricle; the right auricle was incised to permit escape of the perfusate. The eyes and optic nerves were then collected and immersed in Davidson fixative; 1 eye was also fixed in Karnovsky paraformaldehyde–glutaraldehyde fixative for electron microscopic examination. Brains were also collected and immersion-fixed in 10% buffered formalin for light microscopy. In immunohistochemical studies, endogenous albumin was used as a surrogate marker for visualizing the extravasation and spread of retinal vasogenic edema. Moreover, as a positive control to ensure that this dose of ETX produced BBB damage and resultant cerebral edema, brains were also examined immunohistochemically for extravasation of endogenous albumin. A goat anti-rat albumin b was used at a dilution of 1:20,000. No antigen retrieval was required for the albumin antibody. This was followed by a biotinylated anti-goat immunoglobulin secondary c at a 1:250 dilution for 30 min, then washing in phosphate buffered saline (PBS). Slides were then incubated with a streptavidin conjugated peroxidase tertiary d for 1 hr at a dilution of 1:1,000, washed in PBS, and visualized with 3,3′-diaminobenzidine tetrahydrochloride. Sections were counterstained with hematoxylin, dehydrated, cleared, and mounted. Positive and negative controls were included in these protocols.
For ultrastructural examination, small blocks of glutaraldehyde-fixed retina were postfixed in 2% osmium tetroxide buffered in 0.1 M cacodylate (pH 7.3) for 1 hr. The tissue pieces were then dehydrated in increasing concentrations of ethanol, cleared in propylene oxide, and embedded in Epon. e This protocol was approved by the Animal Ethics Committee of SA Pathology, Adelaide, South Australia.
In non–ETX-treated, perfusion-fixed control eyes, all retinal layers were compact, there was no albumin extravasation, and vessels were inconspicuous (Fig. 1A). However, in ETX-treated rats, there was diffuse albumin immunopositivity in all retinal layers, which was particularly prominent surrounding blood vessels, and within the endothelial wall (Fig. 1B, 1C). There were also a few pyknotic nuclei in the inner nuclear layer (Fig. 1B), with cells being separated by intercellular edema fluid. Injury to other retinal layers was limited to hydropic change in a few cells, which were surrounded by an increased, mildly edematous, interstitial space. As an internal positive control, the brains of ETX-treated rats showed multifocal to coalescing areas of albumin extravasation, albumin immunoreactivity being strongest around damaged, leaking blood vessels, and within the walls of these injured vessels (Fig. 1D). Albumin leakage in control brains was confined to non-BBB areas such as leptomeninges and circumventricular organs (data not shown). Ultrastructural examination of the retina revealed severe endothelial damage characterized by marked attenuation and increased electron density of endothelial cells, with frequent blebbing of the luminal surface and occasional platelet adhesion (Fig. 2).
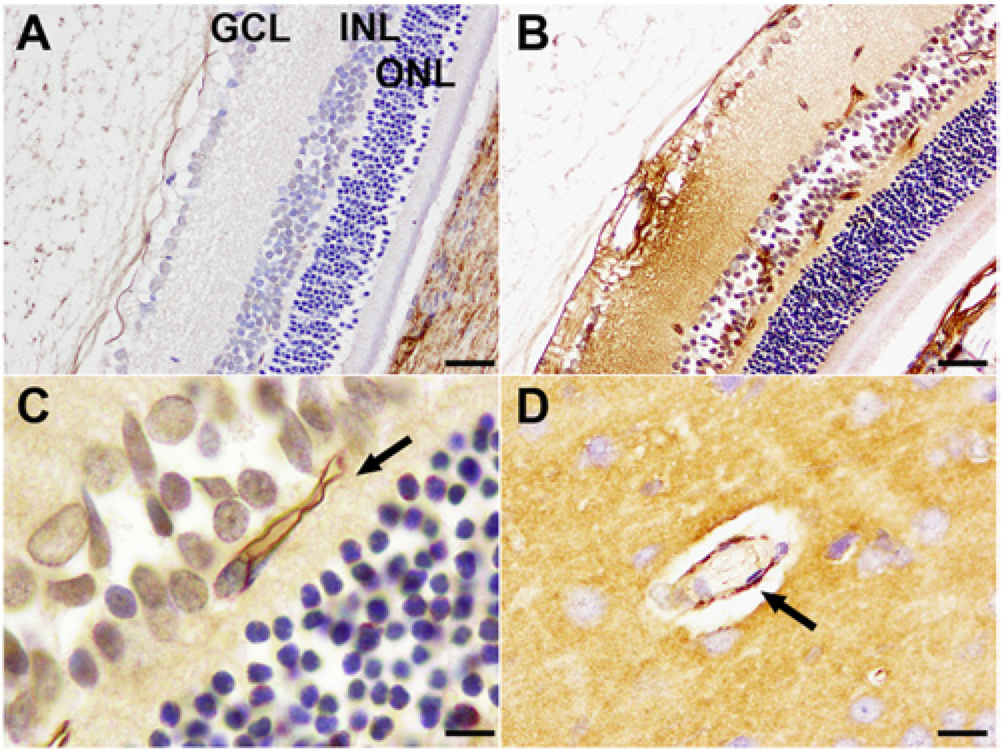
Light micrographs of albumin immunoreactivity in control and Clostridium perfringens type D epsilon toxin (ETX)-treated rats.
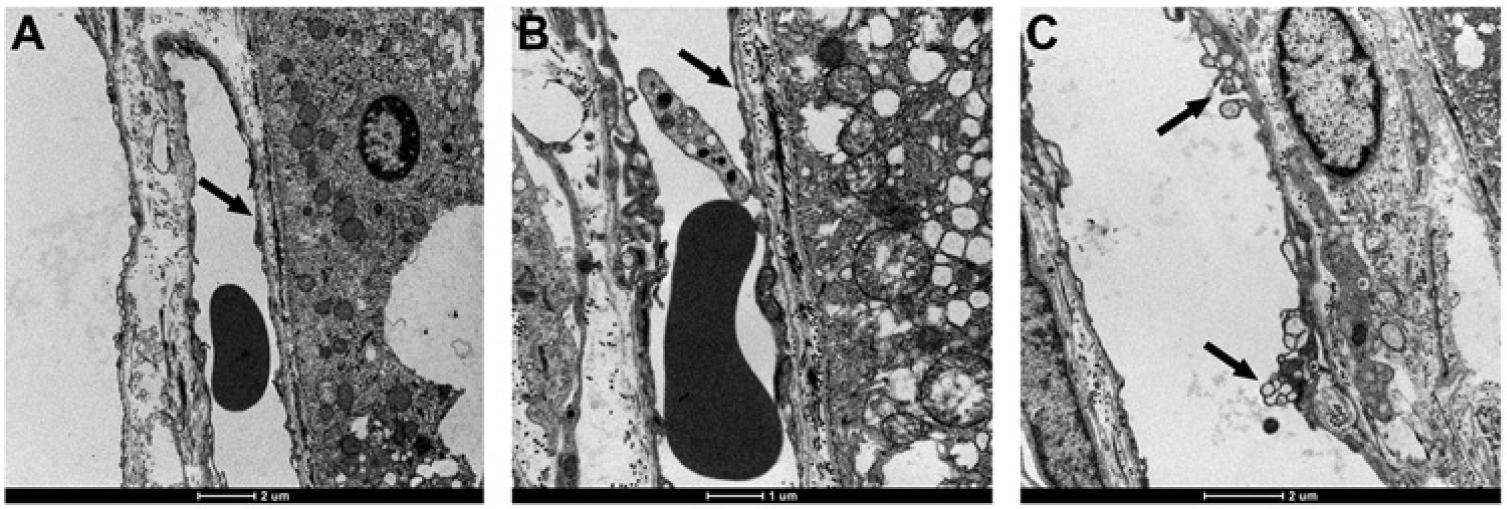
Electron micrographs of Clostridium perfringens type D epsilon toxin (ETX)-treated rat retina.
The current study has shown that ETX causes the fine structural retinal microvascular endothelial damage also found in brain microvessels after exposure to ETX preparations used in the present 2 and other studies (Gould DM: 1972, The development of the early brain lesions induced by the toxin of Clostridium perfringens type D in mice and lambs. PhD thesis. University of California, Davis, CA)5,7 resulting in widespread retinal vasogenic edema; these changes are likely to result in visual deficits in sheep and other domestic species susceptible to ETX damage. Moreover, this similarity in vascular injury in cerebral and retinal microvessels suggests that comparable mechanisms of ETX-induced damage are operative in both tissues.
The microscopic diagnosis of acute epsilon toxin-induced cerebral damage in domestic livestock can often be problematic as vasogenic edema is frequently difficult to detect, particularly in routinely stained, immersion-fixed brains and when the postmortem interval is prolonged. 8 However, perivascular deposition of a protein-rich fluid can be diagnostically useful. 10 In view of the difficulty with the neurohistological diagnosis of acute epsilon toxicity, examination of the eyes for retinal edema, with attendant damage to the inner nuclear layer, could be a useful adjunct in determining this etiology.
Blindness is one of the clinical signs observed in sheep after epsilon toxin exposure, 1 but the contribution of retinal damage to this visual impairment has not previously been appreciated. Furthermore, the results of the present study suggest that treatment with nonsteroidal anti-inflammatory drugs, corticosteroids, and intravitreal antivascular endothelial growth factor could be a beneficial therapeutic intervention after loss of retinal transparency due to edema has been detected opthalmoscopically.
Footnotes
Acknowledgements
The authors thank Mark Daymon, South Australian Institute of Ophthalmology, Ms. Ruth Williams, Adelaide Microscopy, for expert technical assistance, and Dr. Anthony Cameron, Zoetis Australia, for toxin information.
a.
Commonwealth Serum Laboratories (CSL), Melbourne, Victoria, Australia.
b.
Catalog no. 0113-0341, Cappel Labs, West Chester, PA.
c.
Catalog no. BA-9500, Vector Laboratories Inc., Burlingame, CA.
d.
Catalog no. 21127, Thermo Fisher Scientific, Waltham, MA.
e.
Catalog no. T001, TAAB Laboratories, Aldermaston Berks, United Kingdom.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
