Abstract
Five 1-month-old kid goats from a local herd in Kozani (northwest Greece) developed neurological disorders characterized by decreased appetite, ataxia, and head pressing. The animals received a 3-day course of treatment with intramuscular administration of enrofloxacin and ketoprofen. However, no significant clinical improvement was achieved, and 2 kids died. The remaining 3 animals were euthanized, and a necropsy was performed within 1 hr. Macroscopic lesions were confined to the central nervous system, with congestion and petechiae in the meninges. Microscopic lesions in all 3 animals revealed multifocal acute meningoencephalitis characterized by infiltrations composed of mononuclear inflammatory cells, lesser numbers of lymphocytes, and occasionally neutrophils and eosinophils. Additionally, in the kidney, there was multifocal expansion of the glomerular tufts by eosinophilic amorphous material, multifocal interstitial hemorrhages, and multifocal glomerular hypercellularity. The above noted lesions are consisted with an acute ongoing nephropathy indicative of a septicemic–toxemic procedure at its primary stages. Small, gray bacterial colonies, 3–4 mm in diameter, were obtained in pure culture from the brain of all 3 necropsied animals and were confirmed as Escherichia coli O157:H7 by use of phenotypic and genotypic methods. The isolates were sensitive to cefuroxime, ceftazidime, and gentamicin. In contrast, resistance to enrofloxacin, trimethoprim–sulfamethoxazole, and tetracycline was displayed. Additionally the bacterial isolates were found to carry a plasmid that harbored qnrS, sulII, and tetB genes that contribute to high-level resistance to fluoroquinolones, co-trimoxazole, and tetracycline, respectively.
Escherichia coli O157:H7 is the most frequently isolated form of Shiga toxigenic E. coli (STEC) from human illnesses. During the past decade, E. coli O157:H7 has been recovered from many human clinical specimens, including urine of patients with hemolytic uremic syndrome, bloody stools of patients with hemorrhagic colitis, and blood of bacteremic patients. 11 It is also well documented that several mechanisms involving plasmids contribute to an increased resistance of this Gram-negative pathogen to different antibacterial compounds. 4
Meningoencephalitis is an inflammation of meninges and the brain. In young kid goats, this central nervous system (CNS) disease is most commonly recognized as a manifestation of septicemia. 14 An outbreak of meningoencephalitis in 1-month-old goats due to an E. coli O157:H7 strain that carried plasmid-mediated resistance to enrofloxacin, tetracycline, and trimethoprim–sulfamethoxazole (co-trimoxazole) is reported in the current study.
Five 1-month-old kid goats out of a total of 57 kids within a flock located in Kozani (northwest Greece) developed neurological disorders characterized by decreased appetite, ataxia, and head pressing. Serological tests for Caprine arthritis encephalitis virus (CAEV) were performed using a commercially available enzyme-linked immunosorbent assay. a The animals were treated intramuscularly with 10 mg/kg of enrofloxacin b (one-time administration) and 0.5 mg/kg of ketoprofen c twice a day. However, there was no clinical improvement, and 2 of the affected kids died between 2 and 3 days after the onset of symptoms. The remaining 3 diseased animals were euthanized, and a necropsy was performed within the hour. Specimens of the brain and kidneys from each kid goat were fixed in 10% neutral buffered formalin, embedded in paraffin wax, and cut in 5-μm-thick sections for subsequent hematoxylin and eosin staining. In parallel, blood samples and specimens of the brain and kidneys from each kid goat were cultured on Columbia agar plus 5% sheep blood plates that were incubated aerobically, in an atmosphere that contained 5% CO2, and anaerobically at 37°C. Three bacterial colonies, 1 per animal, from the aerobically cultured brain samples were randomly selected for the following analysis: species identification with polymerase chain reaction (PCR), 1 serotyping with a slide agglutination latex test kit, d toxin gene presence by multiplex PCR, 15 and antimicrobial susceptibility testing via a disk diffusion method (http://www.eucast.org/clinical_breakpoints/).Furthermore, plasmids were extracted from the 3 bacterial colonies using a commercial extraction kit. e The extracted plasmids were electrotransformed into E. coli competent cells, and transformants were selected on lysogeny broth agar plates containing enrofloxacin (2 μg/ml), tetracycline (10 μg/ml), and sulfamethoxazole (4 μg/ml). The total DNA of 3 randomly selected transformants, one from each of the original isolates, was analyzed by PCR for the presence of qnrA-B and -S, 8 sulI-II and -III, 13 and tetA-B and -C resistance genes. 10 The resultant PCR amplicons were sequenced on a genetic analyzer f by using dRhodamine-labeled terminators.
Serological tests for CAEV proved negative. The 3 necropsied animals shared the same macroscopic lesions and histological findings. Gross lesions were confined to the CNS, with congestion and petechiae in the meninges and, to the kidneys, with multifocal petechiae and diffuse mild congestion. Microscopic examination of brain sections revealed multifocal acute meningoencephalitis characterized by infiltrations composed of mononuclear inflammatory cells (gliosis), lesser numbers of lymphocytes, and occasionally neutrophils and eosinophils. Additionally, there were multifocal perivascular mononuclear infiltrates (cuffing) composed of lymphocytes and macrophages, and multifocal to coalescing hemorrhage, vascular wall hypertrophy, neovascularization, and perivascular edema (Fig. 1). Furthermore, microscopic examination of the histologic section of the kidneys revealed mild to moderate, multifocal expansion of the glomerular tufts by eosinophilic amorphous material, multifocal presence of granular and hyaline casts within moderately dilated tubules, multifocal to coalescing interstitial hemorrhages, and multifocal mild glomerular hypercellularity presumably due to the mesenchymal proliferation and the increased number of intracapillary leukocytes (Fig. 2).
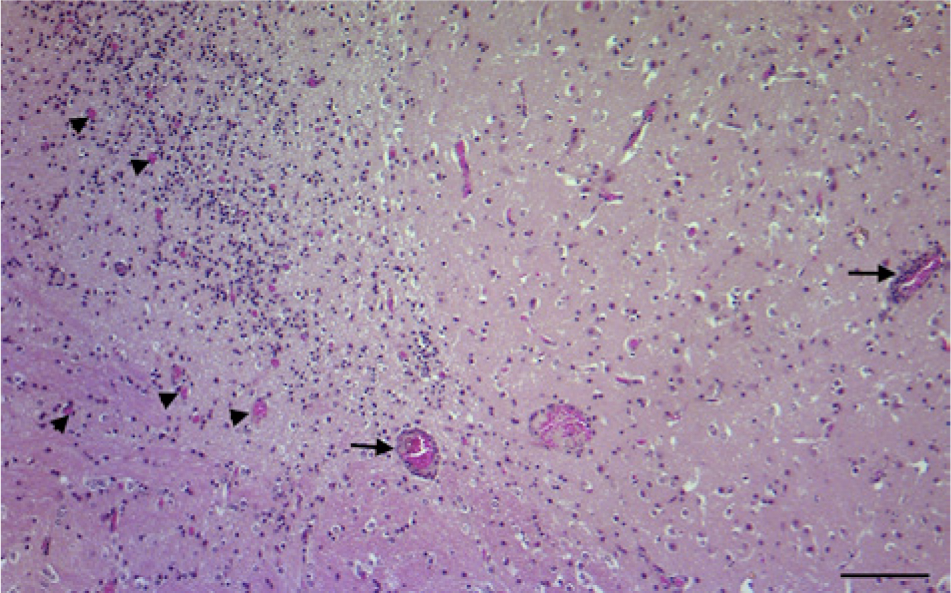
Brainstem; goat. Extensive mononuclear infiltration within gray matter, adjacent to underlying white matter, which disrupts the normal architecture. Note the neovascularization indicative of the restoration process (arrowheads), and the perivascular cuffs (arrows), indicative of the hematogenous origin of the pathogenic agent. Hematoxylin and eosin. Bar = 100 μm.
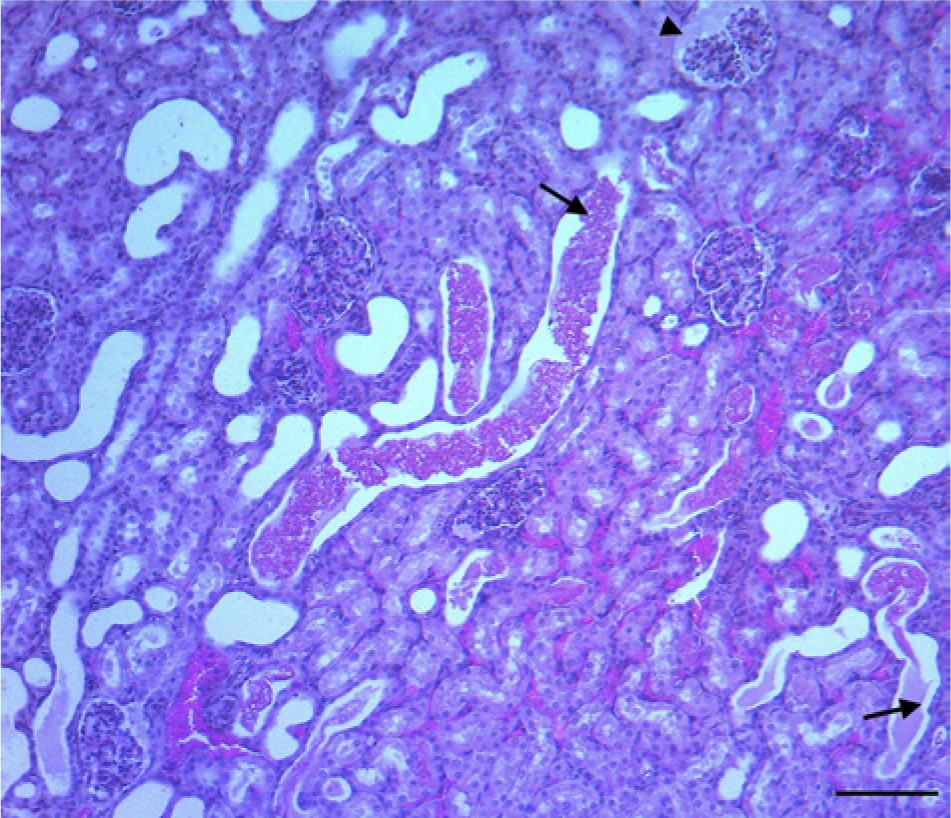
Kidney; goat. Acute ongoing nephropathy characterized by multifocal interstitial hemorrhage, granular and hyaline casts within tubules (arrows), and amorphous eosinophilic material, which expands the tufts of the hypercellular glomeruli (arrowhead). Hematoxylin and eosin. Bar = 100 μm.
After 48 hr of incubation, all blood and kidney cultures showed no growth. In contrast, gray colonies with a diameter of 3–4 mm were obtained in pure culture from all the cultured brain specimens. Three bacterial isolates (1 per animal), randomly selected from the aerobically incubated plates were identified as E. coli, agglutinated with the O157 antiserum, and carried both the VT1 and VT2 genes. Additionally, the isolates showed resistance to enrofloxacin, trimethoprim–sulfamethoxazole, and tetracycline while they were found sensitive to cefuroxime, ceftazidime, and gentamicin. Finally, all transformants obtained from the original E. coli isolates were found to carry qnrS, sulII, andtetB genes, which encode resistance to fluoroquinolones, co-trimoxazole, and tetracycline, respectively.
A previous study in Greece reported that adult goats could be subclinical carriers and execrators of STEC serovars at levels detectable only by sensitive selective enrichment culture procedures. 2 In addition, enteric infections of newborn and young goats associated with E. coli O157:H7 as a result of fecal–oral contamination have been extensively reported. 9 Although colonization and persistence of STEC in the alimentary tract of young ruminants usually results in a hemorrhagic diarrhea that can be fatal, it is well documented that systemic infections due to the penetration of the gut epithelium also occur. 7 This known potential for systemic infection matches the results of the histologic findings and bacteriology culture results for the 3 diseased animals examined in the current study. Overall, the results of the study indicate that meningoencephalitis seen in these kids was a consequence of septicemia–toxemia associated with E. coli O157:H7 in pure culture. Additionally, septicemia–toxemia was indicated by the renal lesions consisted with an acute ongoing nephropathy. The isolates were found to carry both VT1 and VT2 virulence genes. Further studies, including examination of other virulence factors, are required to elucidate the association of E. coli O157:H7 with CNS disease in goats.
The global emergence of multiple antibiotic-resistant isolates of E. coli has been previously reported. 5 In the current study, the E. coli O157:H7 isolates showed resistance to enrofloxacin, trimethoprim–sulfamethoxazole, and tetracycline attributed to the presence of qnrS, sulII, and tetB genes, respectively. Because fluoroquinolones, co-trimoxazole, and tetracycline are recommended for the treatment of bacterial meningoencephalitis, 12 resistance patterns of the type found in the current study are significant in terms of therapy. Enterobacteria that harbor antibiotic resistance elements have been reported among food animals.3,6,13 In the current study, the association of qnrS, sulII, and tetB genes with a plasmid was confirmed by PCR using DNA of transformants obtained from all of the original E. coli isolates. The full sequence of this plasmid remains to be investigated.
In spite of being reported as a causative agent of CNS infections in human beings, 16 E. coli O157:H7 does not appear to have been reported as a causative agent of meningoencephalitis in animals. Based on the evidence that the isolates in the present study showed the same antibiotic resistance profile, it appears that these clinical cases were the consequence of the introduction into the herd of one highly resistant bacterial clone. Systemic infection with STEC-associated serovars is possibly underdiagnosed in the routine veterinary diagnostic laboratory because selective media for those serovars are not routinely used. The current case report indicates that E. coli O157:H7 should be included in the list of possible etiological agents of CNS infections in goats. In addition, antibiotic susceptibility testing of this bacterium may be of clinical importance and should be considered.
Footnotes
a.
Checkit MVV/CAE, IDEXX Laboratories Inc., Westbrook, ME.
b.
Baytril 100, Bayer HealthCare LLC, Shawnee Mission, KS.
c.
Anafen, Merial Canada Inc., Baie-d’Urfé, Quebec, Canada.
d.
DR0620, Oxoid Ltd., Cambridge, UK.
e.
NucleoBond PC100 kit, Macherey-Nagel GmbH & Co KG, Düren, Germany.
f.
ABI PRISMH 3100, Applied Biosystems, Foster City, CA.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The research committee of the Aristotle University of Thessaloniki funded the publication of the present study.
