Abstract
Cutaneous and rhinofacial infections by Pythium insidiosum have previously been reported in sheep in Brazil. In the current study, a new form of pythiosis involving the alimentary tract of 2 nursing lambs from 2 different farms in the semiarid region of Brazil is described. The first lamb showed food regurgitation, lethargy, and anorexia, and died 5 days after the presentation of clinical signs. The second lamb had no history of gastrointestinal disease before death. Necropsy findings were similar in both lambs. The mucosa of the esophagus, reticulum, rumen, omasum, and abomasum showed ulcerated areas covered by yellowish caseous granular exudate. The lesions were transmural and extended to the serosal surfaces, and adhesions were observed between the serosa of the forestomachs and abomasum to the liver and diaphragm. Histologic lesions consisted of pyogranulomatous necrotizing transmural esophagitis, rumenitis, reticulitis, omasitis, and abomasitis with vascular thrombosis and intralesional hyphae. Pythium insidiosum was confirmed as the etiology by immunohistochemistry and culture. The presence of sheep in the vicinity of water ponds during the hot, dry season when forage is not available in the pastures seems to be the main predisposing factor for the occurrence of pythiosis in sheep in the Brazilian semiarid region.
Pythium spp. are oomycetes (fungus-like microorganisms) that are primarily plant pathogens. Pythium insidiosum has been identified as an important animal pathogen in mammals 5 and birds. 8 In sheep, 2 forms of infection by P. insidiosum have been reported: a rhinofacial form, with severe granulomatous necrotizing lesions of the mucocutaneous junction of the nose, nasal vestibule, superior lip, and hard palate,9,11,12 and a cutaneous form, with severe ulcerative lesions of the skin of the legs. 13 Gastrointestinal infection by P. insidiosum has been reported in cats, 10 dogs,2,4,14 and horses 7 but not in ruminants. The current study describes infection of the digestive tract by P. insidiosum in lambs in the Brazilian semiarid region.
Case 1 was a 21-day-old nursing Santa Inês crossbred hair sheep admitted to the Veterinary Hospital of the Federal University of Campina Grande (VH-FUCG; Patos, Paraíba, Brazil) during the dry season of July 2001, with a history of food regurgitation, lethargy, and anorexia. The animal died 5 days after onset of clinical signs. The flock remained grazing for extended periods in the water at the edge of a pond where green grass was available. Another lamb from the same herd had also died after showing similar clinical signs, but diagnostic work-up was not performed. At necropsy, an approximately 3 cm in diameter, focal brownish transmural necrotizing lesion surrounded by a red halo was observed on the serosal surface of the reticulum and a similarly sized and shaped, yellowish, raised, moderate hemorrhagic area was present on the ruminal serosal surface adjacent to the spleen (Fig. 1A). In the distal portion of the esophagus, the mucosa showed an ulcerated area protruding into the esophageal lumen that was covered by yellowish exudate, which extended to the cardia and reticulum. Moderate esophageal dilatation was observed cranial to the lesion. The lesions in the prestomachs extended from the mucosa to the serosa and, on cut surface, the lesions showed a yellowish granular appearance interspersed with dark reddish areas. There were adhesions between the serosal surfaces of the rumen and spleen.
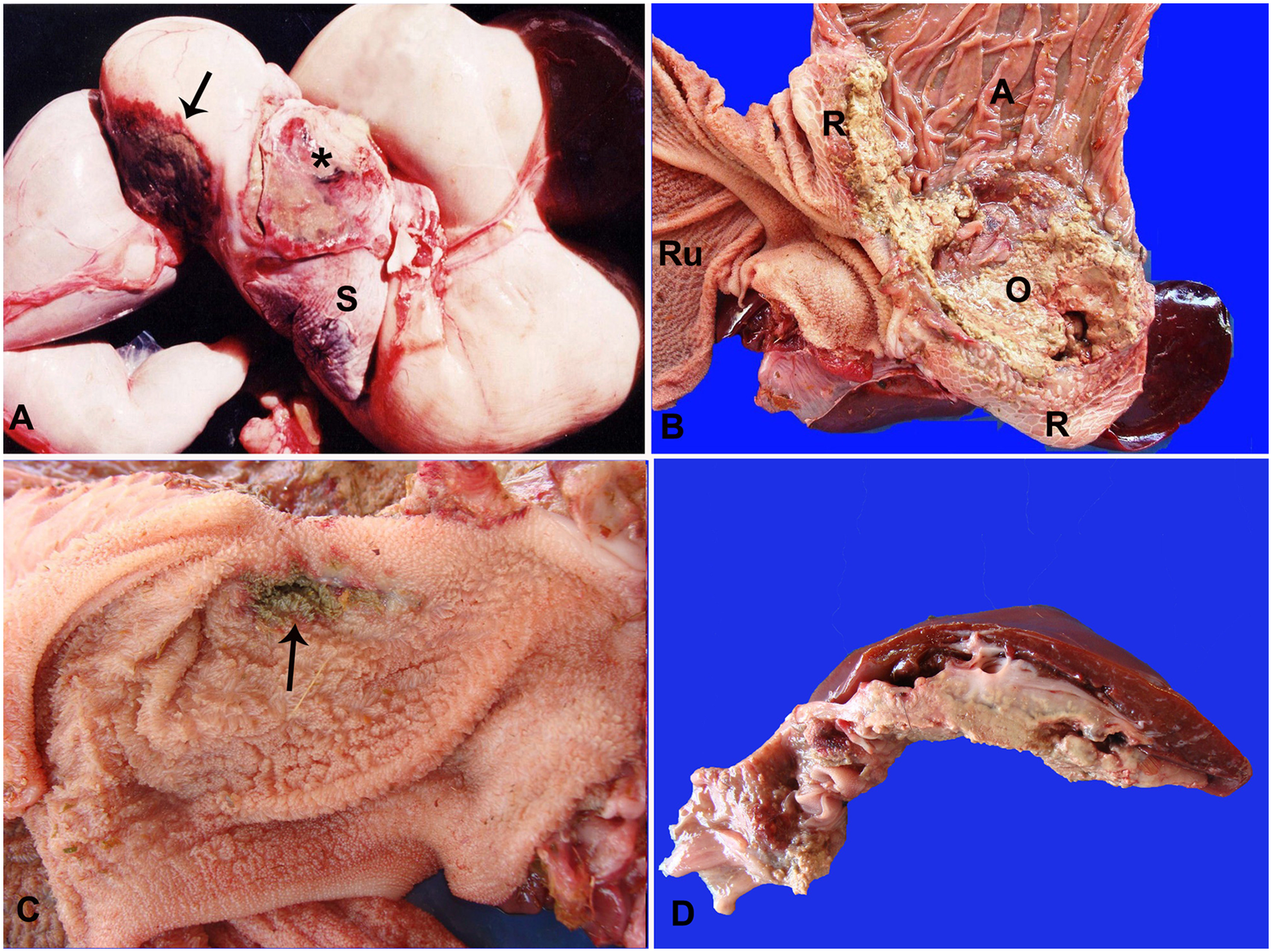
Case 2 was a 30-day-old crossbred hairless lamb admitted to the VH-FUCG with complete fracture of the tibia, also during the dry season, on September 2011. The fracture was reduced, but the animal showed hyporexia and was found dead 3 days after hospitalization. At necropsy, adhesions were observed between the serosa of the omasum and abomasum to the liver, but the liver parenchyma was not affected. Multiple serosal nodules measuring approximately 0.1 cm in diameter were observed in the omasum and abomasum. Focally extensive areas covered by a yellowish caseous granular exudate were observed in the mucosa of the reticulum, omasum, and abomasum. The omasum was most severely affected, with destruction of a few omasal folds (Fig. 1B). An ulcerated dark brown area measuring 2 cm in diameter and surrounded by a red halo was observed in the mucosa of the rumen (Fig. 1C).
Samples of lesions from both lambs affected by digestive pythiosis, and tissue samples from liver, spleen, kidney, adrenal, lymph nodes, lung, heart, skeletal muscles, thyroid, esophagus, forestomachs, abomasum, large and small intestine, tongue, skin, brain, and spinal cord, were collected and fixed in 10% buffered formalin, embedded in paraffin, cut into 5-µm sections, and stained with hematoxylin and eosin. Sections of the esophagus, reticulum, and omasum were also stained with Grocott methenamine silver (GMS) and periodic acid–Schiff (PAS) for fungi. Sections were submitted for immunohistochemistry to identify P. insidiosum using an anti–P. insidiosum polyclonal antibody produced in rabbits followed by streptavidin–alkaline phosphatase using a commercial system, a as described previously. 6 Known negative and positive controls were included with all samples. Fresh tissues from case 2 were cultured on potato–dextrose–agar (PDA) and incubated at 25°C.
Histologic lesions were similar in both cases. The animals had severe necrotizing pyogranulomatous transmural esophagitis, reticulitis, rumenitis, omasitis, and abomasitis, with thrombosis and intralesional hyphae. The lesions were characterized by locally extensive areas of necrosis and hemorrhage infiltrated by degenerate and viable neutrophils and granulomatous inflammation, often characterized by a central core of caseous necrosis surrounded by macrophages, epithelioid macrophages, Langhans-type multinucleate giant cells, eosinophils, lymphocytes, and plasma cells (Fig. 2A). Occasionally, blood vessels had fibrinoid necrosis with fibrin thrombi occluding their lumen. Fibroplasia and neovascularization were also observed in the lesions. Longitudinal and cross sections of negatively stained hyphae surrounded by Splendore–Hoeppli material were randomly observed within multiple areas of necrosis. The hyphae stained poorly with PAS, but stained black or dark brown with GMS (Fig. 2B). Hyphae were observed in necrotic areas and within giant cells, thrombi, and vessel walls. These hyphae were 3–7 µm wide and 10–30 µm long, rarely septate, sometimes branched at right angles, and had almost parallel walls. Globose mild or moderate dilations were also observed. In both cases, intralesional hyphae were positive for P. insidiosum by immunohistochemistry (Fig. 2C).
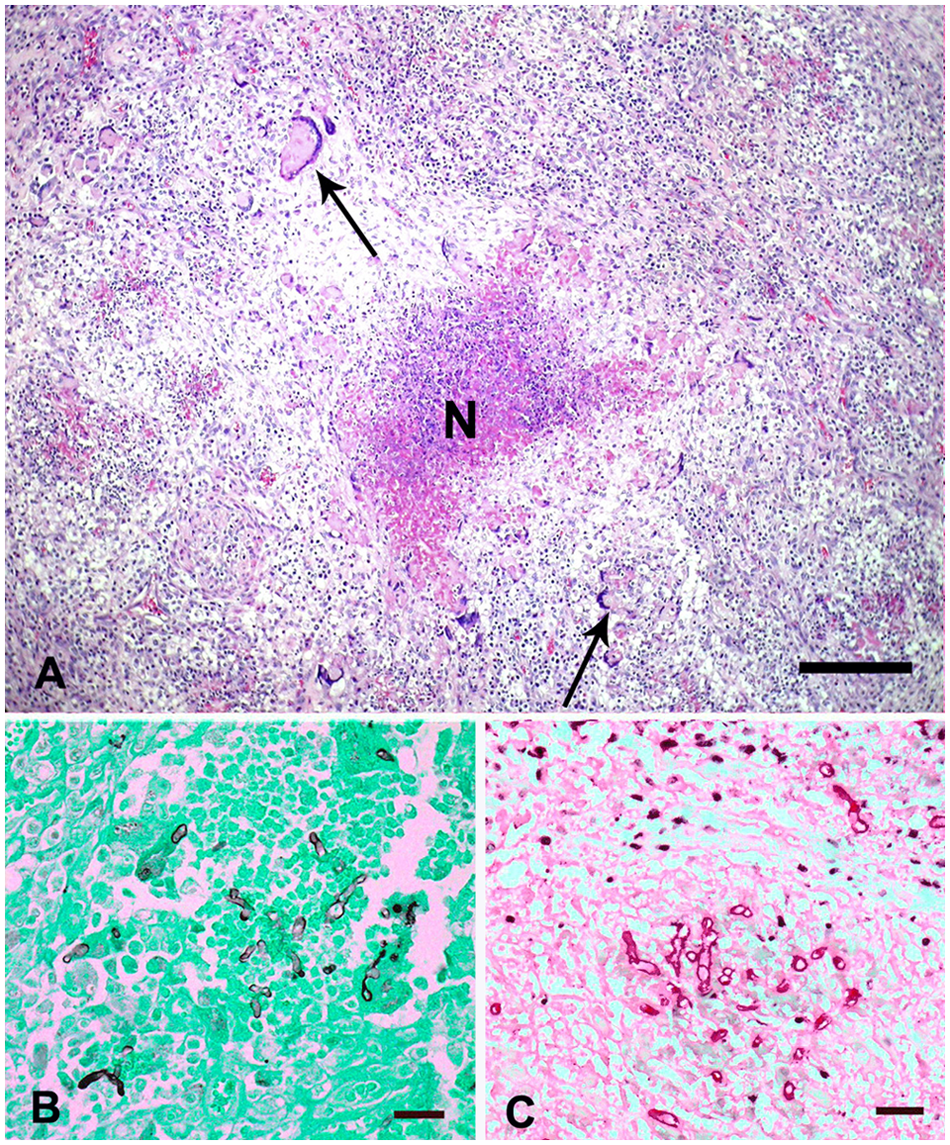
Digestive pythiosis; omasum; sheep.
After a 48-hour incubation on PDA, cotton-like mycelial growth was observed. Microscopically, after clarification with 10% potassium hydroxide, hyphae were branched at right angles and rarely septate. Although zoosporogenesis was not performed, the organisms were morphologically similar to Pythium sp.
The clinical signs observed in one of the sheep were similar in some aspects to gastrointestinal pythiosis in cats and dogs, which includes weight loss and vomiting.1,2,4,10,14 The food regurgitation observed in case 1 is most likely a consequence of the esophageal lesions observed in this lamb. Intestinal lesions that are sometimes associated with diarrhea, as observed in some dogs,6,14 were not present in the sheep in the present study. In dogs, horses, and cats, the lesions in gastrointestinal pythiosis are pyogranulomatous2,4,6,14 or eosinophilic.7,10 The histological lesions in the 2 lambs described herein were mainly pyogranulomatous, necrotizing, and with only a few eosinophils, similar to the lesions reported in rhinofacial9,11,12 and cutaneous 13 pythiosis in sheep. During a visit to the farm of case 2, 1 adult female sheep was diagnosed with rhinofacial pythiosis by histology of a facial biopsy and culture of Pythium sp. from the lesion site, suggesting that more than 1 form of the disease can occur simultaneously in the same flock.
It is most likely that the digestive tract infection by P. insidiosum in the 2 lambs occurred through the consumption of water or plants with the infective zoospores. Contaminated water consumption is suggested as the manner of infection for gastrointestinal pythiosis in dogs. 2 The Brazilian semiarid region is characterized by high temperatures and a long dry period from May–June to January–February. Under these meteorological conditions, there is a considerable shortage of forage, and sheep flocks look for wetter areas around water ponds where grasses and plants are available. The high water temperature and the presence of vegetation in the water provide a suitable environment for the multiplication of P. insidiosum.2,4 Such epidemiologic conditions are also observed in cutaneous pythiosis in sheep. 13 In domestic animals, mycotic diseases in the gastrointestinal tract have been associated with low host resistance and primary local lesions. 3 The occurrence of the disease only in nursing lambs suggests that insufficient or no colostrum intake with failure of passive immunity transfer may be an important predisposing factor for the occurrence of gastrointestinal pythiosis in lambs; however, information about colostrum intake in the 2 animals included in the current study was unavailable. Young age, drought conditions, and the breed of sheep could be other possible predisposing factors for the occurrence of the disease. In conclusion, the rhinofacial, cutaneous, and digestive forms (as described herein) of pythiosis in sheep in the Brazilian semiarid region are usually associated with high temperatures, low availability of forage during the dry season, and the presence of stagnant water, which create a favorable environment for the multiplication of and infection by P. insidiosum.
Footnotes
a.
LSAB+ System-AP, Dako North America Inc., Carpinteria, CA.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Glaucia D. Kommers has a fellowship from CNPq (National Council of Scientific and Technological Development, Brazil; PQ-2 no. 305337/2010-6).
