Abstract
Background:
Appropriate lessons and formalized training concerning emergency medicine is becoming increasingly important in undergraduate medical education. There is an urgent need to evaluate undergraduate emergency medicine education of students enrolled on the 8-year Doctor of Medicine degree programs nationwide in China with the aim that the data extracted could ultimately be used to help develop a standardized emergency medicine curriculum in China.
Objectives:
The aim of the study is to accurately describe emergency medicine education of 8-year Doctor of Medicine program in China, including emergency medicine classes, clinical practice in emergency medicine department, and expectations toward emergency medicine education.
Methods:
An online questionnaire was distributed to all the medical students of 8-year Doctor of Medicine program who have attended emergency medicine education in 14 medical schools in China. Participation in the survey was voluntary and anonymized.
Results:
In total, 529 valid responses were collected. There was a clear difference between students with a career aspiration in emergency medicine and those without. Comparing to countries that have an established emergency medicine curriculum, shortage of classroom hours and clinical practice time is a major cause of unsatisfactory educational outcomes in China. A detailed uniform emergency medicine curriculum that outlines exact requirements for medical students is required as well.
Conclusion:
A consolidated syllabus and curriculum should be compiled by all the medical schools with the 8-year integrated Doctor of Medicine degree program in China. The specific diseases and skills that should be covered in emergency medical education remain up to debate.
Introduction
In China, the 8-year integrated Doctor of Medicine (MD) program admits candidates directly after finishing secondary education and awards the students with an MD degree upon completion. This time-honored model has existed over a century and is adopted by 14 medical schools in China. 1 Contrastingly, there are about 120 medical schools in the country who also admit students directly from high school, providing either a standard 5-year Bachelor of Medicine (MB) program or an integrated 7-year Master of Medicine (MMed) program. This suggests that students enrolled on the 8-year MD program may be part of a small elite of high achievers and possible future leaders in the medical field. Compared with the 8-year program, the 5- or 7-year program has less opportunities for scientific research, and usually adopts large-class lecture, but its clinical rotation time is longer.
Regardless of specialty choice, junior doctors are often responsible to assess new patients, recognize those who require urgent care, and initiate emergency management. Failure to learn procedural skills before residency training is likely to lead to individual incompetence and negative clinical outcomes. 2 Appropriate lessons and formalized training concerning emergency medicine (EM) is becoming increasingly important in undergraduate medical education. One of the Core Entrustable Professional Activities (EPA) identified by medical schools all over the United States is to recognize a patient requiring urgent care and initiate evaluation and management, stressing the importance of EM education. 3
Up to now, several countries have already come to a consensus of a national standardized EM curriculum.4,5 However, the implementation of these curricula is haphazard and varies among medical schools. 6 A national curriculum of EM education in medical schools with the 8-year MD degree program is still absent in China, both at preclinical and clinical clerkship level. Thus, there is an urgent need to evaluate undergraduate EM education in China, compare the current situation against countries with more established EM educational programs, and make recommendations to improve both the quality of EM education and the standards of tomorrow’s doctors. Accordingly, we conducted a questionnaire-based survey to assess the situation of undergraduate EM education of students enrolled on the 8-year MD degree programs nationwide with the aim that the data extracted could ultimately be used to help develop a standardized EM curriculum.
Methods
Questionnaire design
An online questionnaire was drafted and reviewed by our research group consisting of three medical students (representatives of the 8-year MD degree program: Dr. Zengzheng Ge/Shi Feng/Xiangning Liu) and five experienced doctors (experienced teachers specialized in teaching EM: Dr. Yi Li/Huadong Zhu/Jihai Liu/Di Shi/ Lina Zhao) from EM department of our hospital, until consensus regarding content and clarity was reached between the research group. We created this questionnaire by organizing school surveys, asking questions in class, and consulting literature, which was titled “A survey on the current state of emergency medicine education in medical students on the 8-year MD degree programs in China.” This survey was designed to assess three major domains: (1) the general schedule and implementation of EM classes of 8-year MD degree programs, (2) the current state of clinical practice in EM department at each respondent’s medical school, and (3) potential improvements toward a standardized curriculum. Each question had multiple-choice answers and/or an open-ended text option, some with non-mutually exclusive answers.
Patient and public involvement, data collection, and analysis
In May 2019, the final version was distributed through WeChat, the most popular message and social media software in China (akin to Facebook App in the United States), to all the medical schools providing the 8-year MD program. We send the link of the questionnaire to the teachers of the Academic Affairs Office of other universities with 8-year MD program through WeChat, then forward it to the students through WeChat, and click the link to participate in the questionnaire. After completing and submitting the questionnaire, WeChat ID and the answers to the questionnaire will be seen by researchers. But WeChat ID was de-identified by a medical student from a third party before analysis for participant privacy.
The questionnaire was only dispensed to 8-year MD program students who have already undertaken EM classes or attended clinical rotations in EM department, and it contained questions about whether the participants were 8-year MD program students. Participation in the survey was voluntary. Owing to the fact that teaching arrangements differ widely among schools, there was no restriction on the current year/grade of the student. All electronically completed questionnaires were collected and reviewed. For the convenience of comparison, students are asked to rank scores on a scale of 1 to 5 for questions (Q7/Q15/Q20/Q27) that measure the extent of understanding or achievements. A direction is given to the participants on what the 1 to 5 ranking represents in the questionnaire (Rank 1 indicates that you know/learn nothing or you did not hope to cultivate it; Rank 5 indicates that you are well informed or you experienced a fruitful learning about it or you hoped desperately to learn about it), so as to guarantee the validity of the grading. Thus, quantitative data were collected on learning objectives, study plans, clinical instructions, and local assessments/testing. As for open-ended questions, continuous variables are analyzed and displayed in Q4/Q8/Q16; high-frequency/representative responses will be selected and displayed in the article in Q9/Q29.
Results
General state of questionnaire collected
Overall, 571 students responded with the inclusion rate of 92.6%; 42 responses were excluded for various reasons (22 for incomplete responses, 18 for irrelevant answers in open-ended questions, and 2 for not answering as required). Among inclusions (Q2), 41 questionnaires are collected from Peking Union Medical College, 12 from Peking University Health Science Center, 4 from School of Medicine of Tsinghua University, 60 from Shanghai Medical College of Fudan University, 12 from Shanghai Jiao Tong University School of Medicine, 51 from School of Medicine of Zhejiang University, 64 from Tongji Medical College of Huazhong University of Science and Technology, 133 from Xiangya School of Medicine, 61 from Zhongshan School of Medicine of Sun Yat-sen University, 27 from West China School of Medicine of Sichuan University, 9 from Southern Medical University, 4 from Second Military Medical University, 26 from Third Medical University, and 25 from Fourth Military Medical University. The total number of medical students of the 8-year medical degree program varies among schools, ranging from 18 to 180 students (Q4).
Since medical students from Tsinghua University receive emergency medical training with those from Peking Union Medical College, the responses of two schools were analyzed and grouped as “Peking Union Medical College–Tsinghua University.”
Taking into account that military medical schools are distinctly different from other medical schools since they enroll only serving soldiers, we put Southern Medical University, Second Military Medical University, Third Medical University, and Fourth Military Medical University into a group called Military Medical Schools.
EM classes taught by the emergency department
The current schedule and implementation of EM classes (Q7–Q14 in the questionnaire) of 14 medical colleges are shown in Table 1.
The general situation of emergency medical classes.
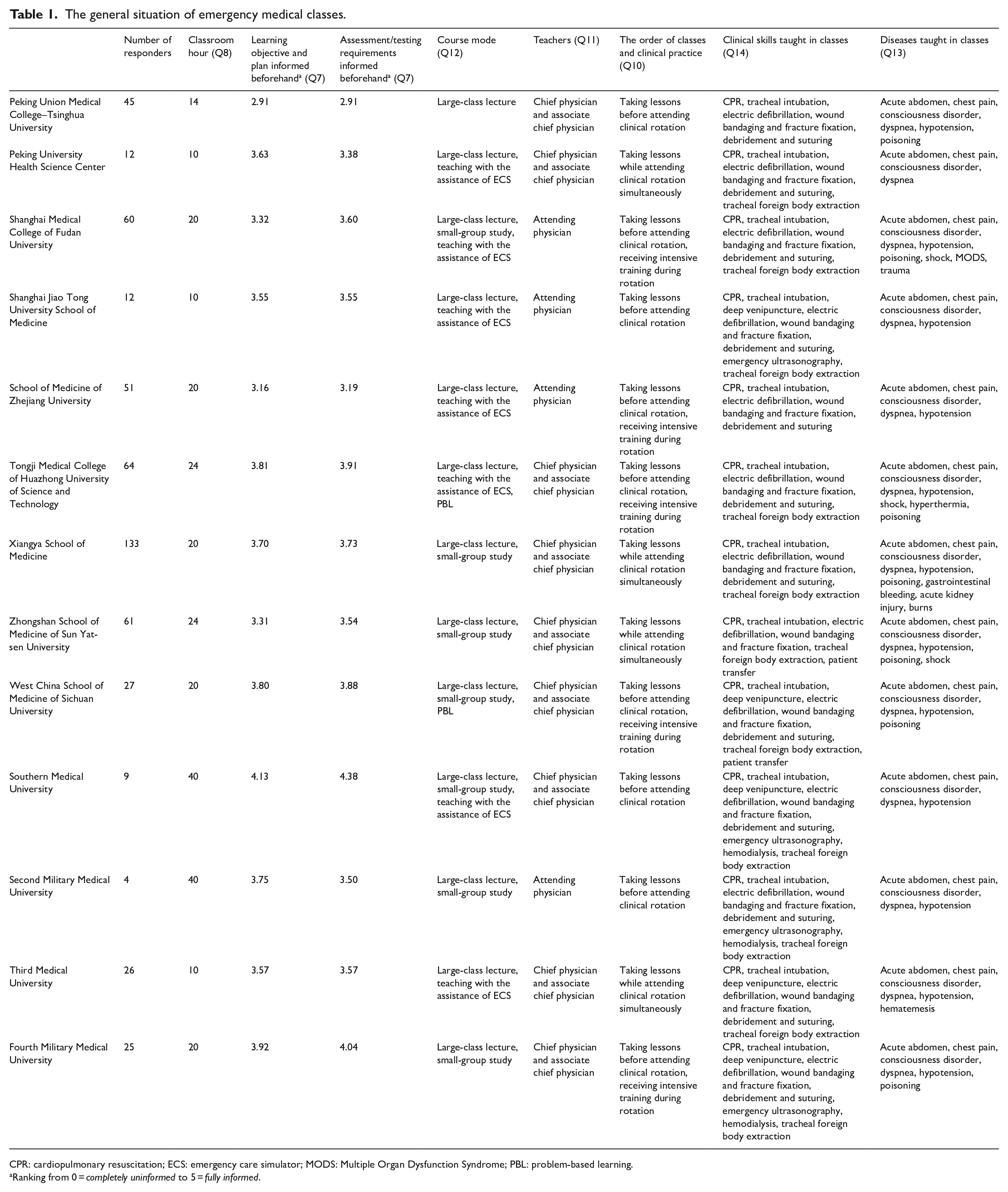
CPR: cardiopulmonary resuscitation; ECS: emergency care simulator; MODS: Multiple Organ Dysfunction Syndrome; PBL: problem-based learning.
Ranking from 0 = completely uninformed to 5 = fully informed.
The evaluation about whether students were well informed about the learning objectives, study plans, and assessment/testing requirements is displayed in Table 1. However, only Southern Medical University received over 4 marks in both questions. Peking Union Medical College–Tsinghua University comes in at the bottom, getting 2.91 marks in both questions.
The total number of classes within each EM teaching program ranged from 10 to 40. While Peking University Health Science Center and Shanghai Jiao Tong University School of Medicine scheduled only 10 classes, 40 emergency classes are taught in Southern Medical University and Second Military Medical University.
All medical schools provide large-class lecture, and some also offer small-group study or teaching with the assistance of emergency care simulator (ECS). West China School of Medicine of Sichuan University is the only one that delivers a problem-based learning course.
Chief physicians and associate chief physicians from the emergency department took charge of the classes in nine schools. In Shanghai Medical College of Fudan University, Shanghai Jiao Tong University School of Medicine, School of Medicine of Zhejiang University, and Second Military Medical University, the classes are taught by attending physicians.
Students from Shanghai Medical College of Fudan University, School of Medicine of Zhejiang University, Tongji Medical College of Huazhong University of Science and Technology, West China School of Medicine of Sichuan University, and Fourth Military Medical University take classroom lessons before attending clinical rotation and receive intensive training during the rotation. Other schools either ask students to take all classroom lessons before attending clinical rotation or let them take lessons during the rotation.
All schools cover tracheal intubation, electric defibrillation, wound bandaging, and fracture fixation in their classes. Other clinical skills, including debridement and suturing, venipuncture, emergency ultrasonography, hemodialysis, and tracheal foreign body extraction, are taught in some schools. As for the acute diseases commonly seen in the emergency department, acute abdomen, chest pain, consciousness disorder, and dyspnea are learnt in every medical school. All schools except Peking University Health Science Center have classes for hypotension. Poisoning, gastrointestinal bleeding, acute kidney injury, burns, Multiple Organ Dysfunction Syndrome (MODS), trauma, and safe patient transfer are taught in some schools as well. Apart from the classes given by the emergency department, students also learn related knowledge in clinical skill practice, basic life support, Advanced Cardiac Life Support (ACLS), internal medicine classes, surgical rotation, and basic sciences (Q9). Noticeably, the military medical schools prioritize the teaching of disaster medicine, which is not taught in other medical schools.
Clinical practice in the emergency department
In Table 2, we summarize the current state of clinical rotations in emergency departments from the questionnaires (Q15–Q22).
The current state of emergency medical clinical practice.
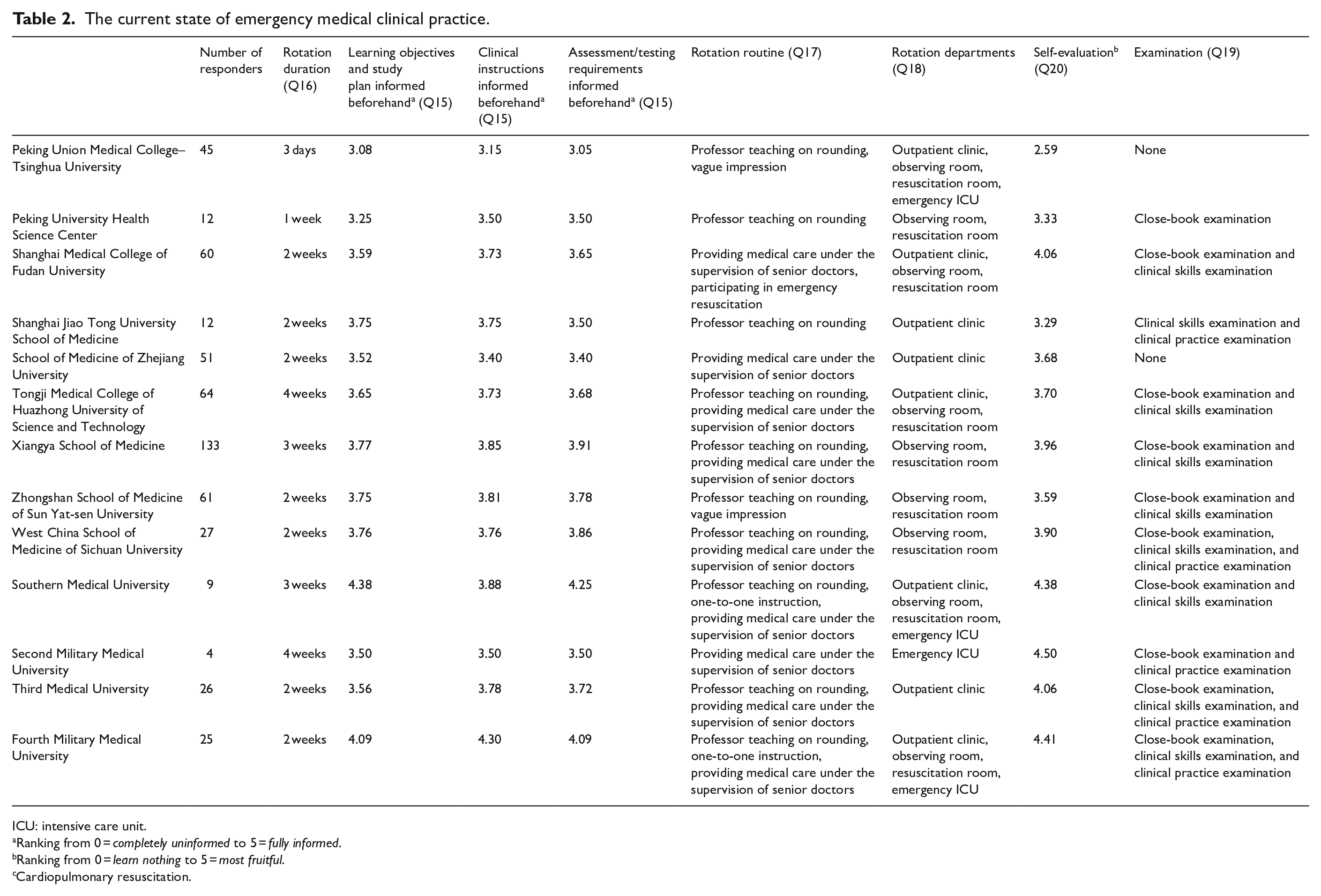
ICU: intensive care unit.
Ranking from 0 = completely uninformed to 5 = fully informed.
Ranking from 0 = learn nothing to 5 = most fruitful.
Cardiopulmonary resuscitation.
The rotation duration varies from 3 days to 4 weeks. Among the 13 schools, students from Peking Union Medical College–Tsinghua University have merely 3 days to attend clinical practice. Tongji Medical College of Huazhong University of Science and Technology and Second Military Medical University allow the students to spend 4 weeks in clinical practice. Therefore, Second Military Medical University takes the first place both in classroom hours and clinical practice period.
As for whether students were well informed about the learning objectives and study plan, clinical instructions, and assessment/testing requirement, we find that Fourth Military Medical University scores 4+ in all questions and Southern Medical University is one spot behind.
When it comes to the emergency departments students visit during rotation, students from Peking Union Medical College–Tsinghua University, Southern Medical University, and Fourth Military Medical University visited outpatient clinics, emergency observing units, resuscitation rooms, and emergency intensive care units (ICUs), arguably gaining a more comprehensive understanding of the emergency department.
The evaluation for students to rate for the learning efficacy of these diseases during rotation and to rate for learning efficacy of nine emergency clinical skills recognized as essential for medical students (Q20) is displayed in Supplementary Files 1 and 2. Peking University Health Science Center gets 22 points, the highest score in diseases studied in clinical practice. The first place of emergency skills falls to military medical schools with more than 36 points. The total score of Peking Union Medical College–Tsinghua University came last in both questions. The medical schools with the shortest EM rotation (i.e. 3 days) unsurprisingly yielded the poorest learning efficacy.
The average scores of self-evaluation about students’ learning were fruitful during their clinical rotation of four military medical schools, and Shanghai Medical College of Fudan University reaches over 4 points. The lowest score 2.59 shows up in Peking Union Medical College–Tsinghua University, which is in accordance with their shortest rotation period.
On one hand, those whose score is 3 or more in self-evaluation are asked to choose the capabilities they learn during rotation (Q21), shown in Table 3. More than half of students from 11 medical schools claim that they learn all capabilities listed in the choices. On the other hand, those whose score was 3 or less in self-evaluation were asked to pick out the limitations and deficiencies of their rotation (Q22), shown in Table 3. In the majority of medical schools, after the completion of classes and clinical rotations, students had to undertake a closed-book written examination and clinical skills examination to assess their competency.
The capabilities learnt during clinical rotation and limitations of rotation.
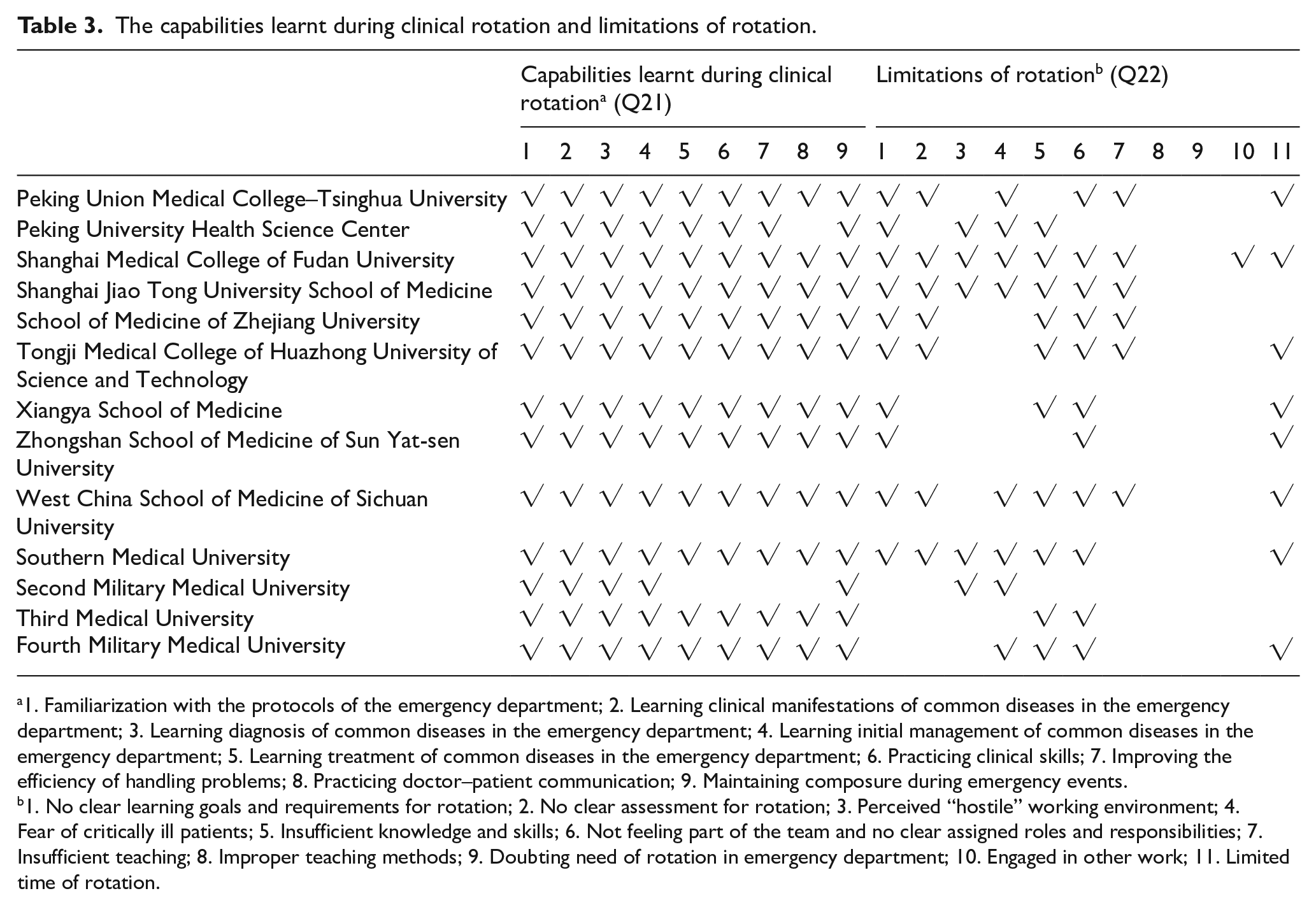

1. Familiarization with the protocols of the emergency department; 2. Learning clinical manifestations of common diseases in the emergency department; 3. Learning diagnosis of common diseases in the emergency department; 4. Learning initial management of common diseases in the emergency department; 5. Learning treatment of common diseases in the emergency department; 6. Practicing clinical skills; 7. Improving the efficiency of handling problems; 8. Practicing doctor–patient communication; 9. Maintaining composure during emergency events.
1. No clear learning goals and requirements for rotation; 2. No clear assessment for rotation; 3. Perceived “hostile” working environment; 4. Fear of critically ill patients; 5. Insufficient knowledge and skills; 6. Not feeling part of the team and no clear assigned roles and responsibilities; 7. Insufficient teaching; 8. Improper teaching methods; 9. Doubting need of rotation in emergency department; 10. Engaged in other work; 11. Limited time of rotation.
Student expectations and preferences
The suggestion for emergency medical education is collected, and the analyzed results are illustrated in Supplementary File 3.
Although all schools present students with large-class lecture, students seem to prefer small-group study instead (Q24). All students except those from Second Military Medical University and Third Medical University hope to take classroom lessons before attending clinical rotation and receive intensive training during the rotation. In this way, they can participate in medical care equipped with the basic knowledge and learn more in the intensive lessons. More than half of students from Shanghai Medical College of Fudan University, Southern Medical University, and Second Military Medical University intended to take classroom lessons and attend clinical rotation simultaneously, suggesting the importance of integrating theories with practice.
We listed six options and ask students to choose what they hope to do during clinical practice (Q26), shown in Supplementary File 4. Most students wished they could provide medical care under the supervision of senior doctors. They also appreciated one-to-one teaching and teaching on ward rounds.
When asked which areas of the EM department they want to visit during their clinical rotations (Q25), more than 95% of participants showed interest in all departments, namely, outpatient clinic, EM observation unit, resuscitation room, and emergency ICU department. High consistency of the answers indicates that medical students remain passionate in their learning of EM.
The importance of the learning capabilities students hope to cultivate during clinical practice is shown in Table 4. As for examination, students expected their assessments to comprise of clinical skills examinations and clinical practice examinations. Students from Southern Medical University, Zhongshan School of Medicine of Sun Yat-sen University, and Xiangya School of Medicine also expected closed-book written examinations.
Capabilities students hope to cultivate during rotation.
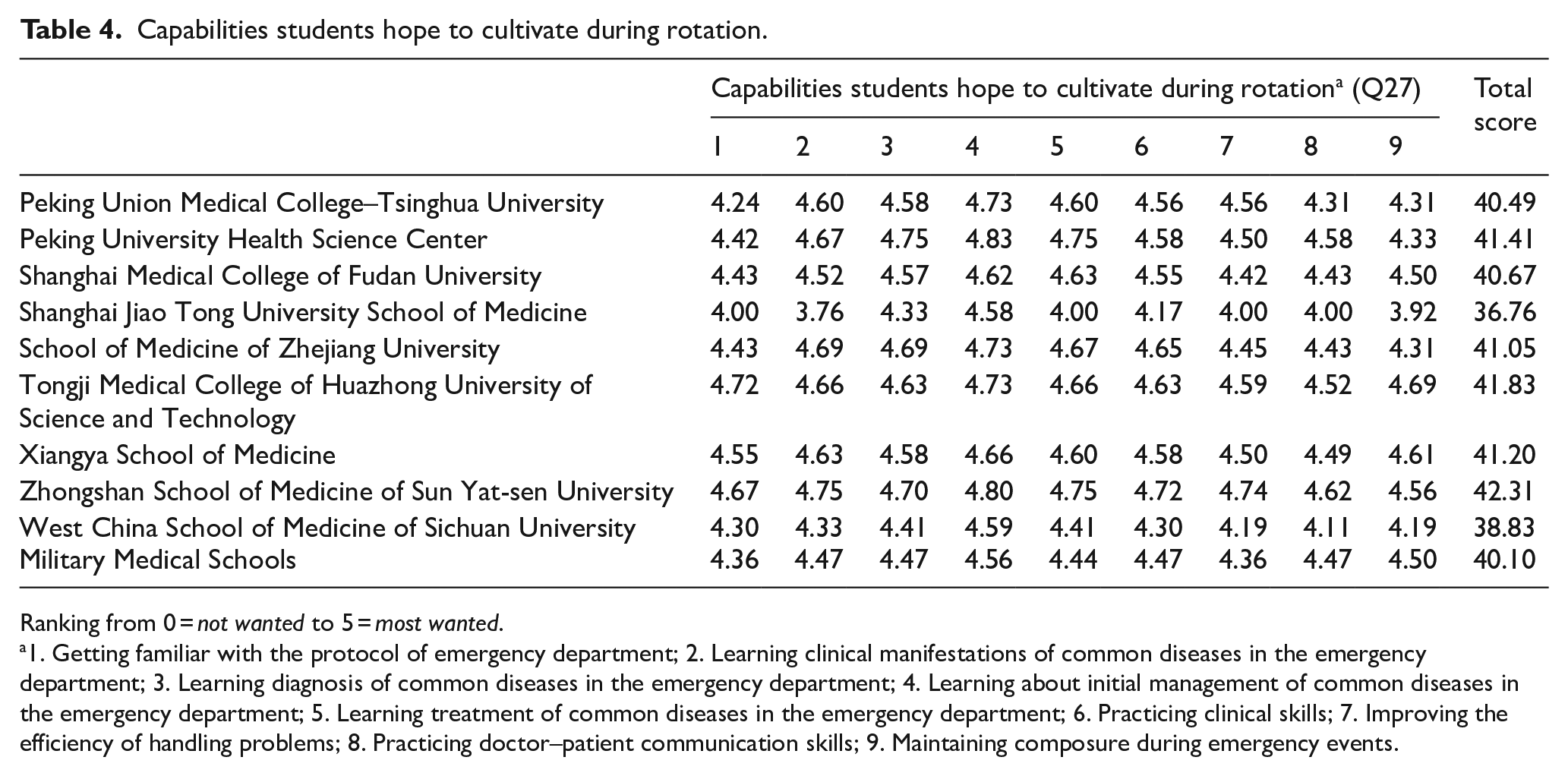
Ranking from 0 = not wanted to 5 = most wanted.
1. Getting familiar with the protocol of emergency department; 2. Learning clinical manifestations of common diseases in the emergency department; 3. Learning diagnosis of common diseases in the emergency department; 4. Learning about initial management of common diseases in the emergency department; 5. Learning treatment of common diseases in the emergency department; 6. Practicing clinical skills; 7. Improving the efficiency of handling problems; 8. Practicing doctor–patient communication skills; 9. Maintaining composure during emergency events.
At the end of the questionnaire where we left a free text section for additional comments, 12 students suggest increasing classes and the clinical rotation period. One student proposed that they should learn about the latest clinical guidelines in parallel with clinical cases.
There was a clear difference between students with a career aspiration in EM and those without
Medical students from the 8-year medical degree program are eligible to apply for training jobs in any department after graduation. Thus, nine students (Group A) with a career preference for EM were noticeably more motivated and interested in learning about EM during their rotation compared to the other 520 participants (Group B), shown in Supplementary File 5.
We investigated the academic performance of Group A. Five students claim their grade is between 1/10 and 1/3 in their class, three students rank between 1/3 and 2/3, while one student falls in the last 1/3. Although there was only a small number of students who had a career interest in EM, they were just as competitive as other students in terms of their grades.
Among these 9 students, 5 received additional emergency training apart from the obligatory classes, while there are only 83 students in Group B volunteered to undertake additional training.
Four students in Group A preferred to take classroom lessons and attend clinical rotation simultaneously, while three other students preferred taking lessons before attending clinical rotations and receiving intensive training during the rotation. In Group B, more than half of students preferred taking lessons before attending clinical rotation and receiving intensive training during rotations. The students in Group A turned out to be more cautious about taking on a more active clinical role and providing medical care in the emergency department. However, these same students preferred to take a closed-book written examination by the end of the rotation.
In comparison with Group B who had a score of 3.76, it is striking that Group A merely had an average score of 3.57 in self-evaluation of clinical rotation.
Discussion
Even though the 8-year MD degree program is a long-established model, it faces significant challenges today. There are significant changes taking place in the delivery of teaching in EM. Without a nationally recognized and uniform curriculum and standardized assessment, there is inevitable variation in both the standard of teaching and the standard of competence in tomorrow’s doctors.
Each clinical clerkship tailors their teaching methods according to their locally available resources and learning opportunities. Nevertheless, all schools had managed to cover the following topics: acute abdomen, chest pain, consciousness disorder, and dyspnea in classes, and tracheal intubation, electric defibrillation, wound bandaging, and fracture fixation in procedural skills practice. Among the 14 medical schools, military medical schools take the lead by elaborately scheduling clinical courses and practices. Another widely shared problem is insufficient classroom hours and clinical rotation duration (Figure 1), leading to inadequate exposure to the wide range of EM problems and diagnoses. National consensus on a uniform EM curriculum and standardized assessment could facilitate a more consistent learning experience for medical students in China. If we do not have standardized education, then the development of medicine may be slow. We suggest that discussions need to be held at a national level regarding the current problems in EM education and potential remedies.
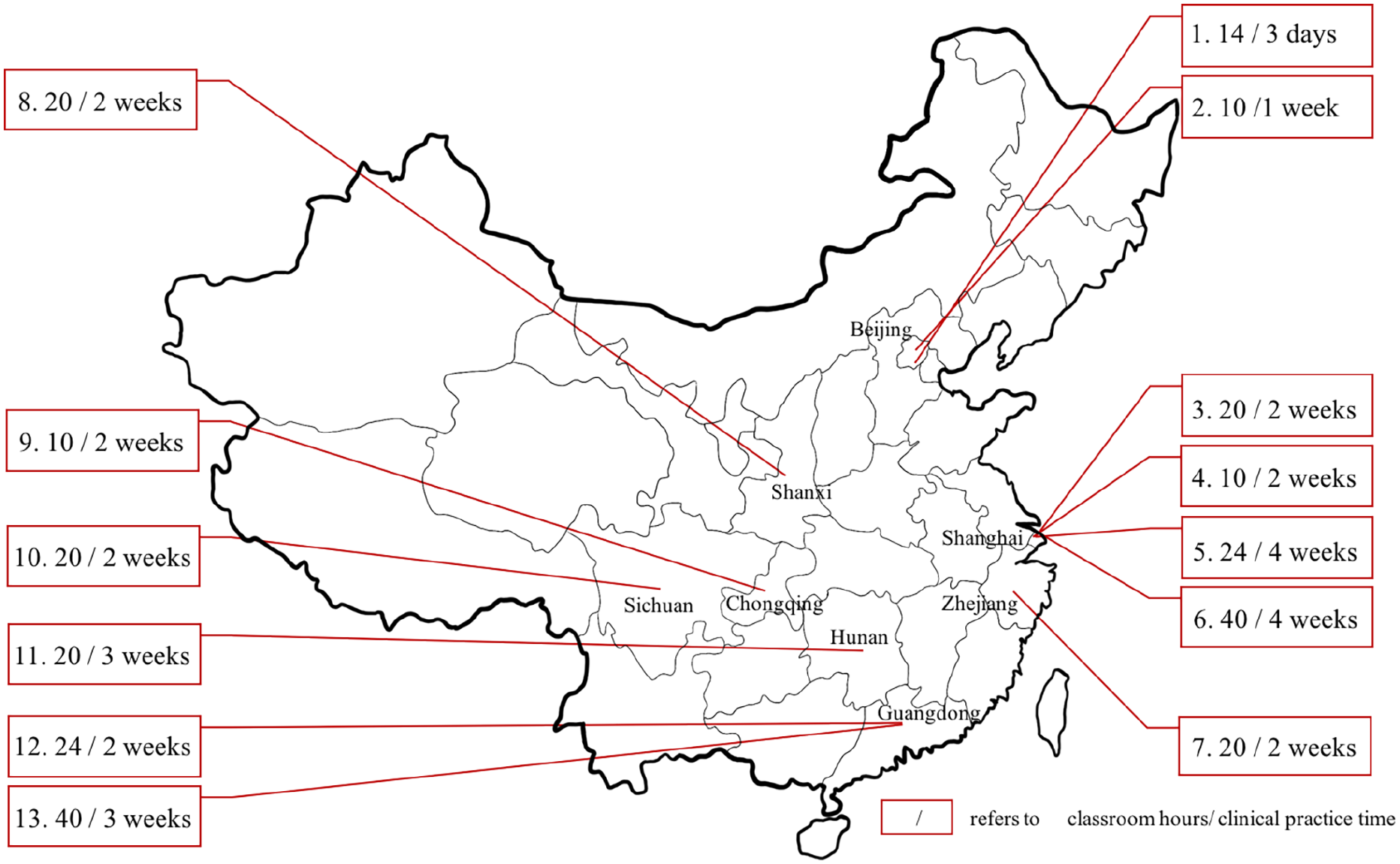
The geographic distribution of the medical schools and their time on emergency education.
These problems in EM undergraduate education are by no means unique to China, and many other countries are also facing similar issues and dilemmas.7–9 The lack of a uniform EM curriculum and standardized assessment among medical schools is also found in some European countries. In the United Kingdom, this lack of standardization has been blamed on the haphazard clinical competencies of medical students—a recent survey of 3732 medical students from 21 British universities revealed that only 9% of first-year students and 12% of fourth-year students were fully competent at basic life support. 8 Whereas in Germany, Beckers et al. found that in all of the 35 medical schools surveyed, the teaching of EM to medical students was not even supervised or delivered by the emergency department. 10 The Department of Anesthesiology was responsible for teaching EM to undergraduates in 32 of these medical schools, and in the remaining 3 faculties, the EM module was taught by the Department of Surgery or Department of Internal Medicine. The authors suggested that this less-than-ideal arrangement along with a lack of a standardized EM undergraduate curriculum lead to EM teaching being “very inconsistently structured” in Germany. 9 Even in countries with established EM curricula, the implementation and delivery of said curriculum can be haphazard, leading to senior medical students failing to achieve the required level of competency in EM. 6
However, when we compare countries that have an established EM curriculum such as of the United States 4 and Canada 5 to the current state of China, we find that the shortage of classroom hours and clinical practice time is a major cause of unsatisfactory educational outcomes. Medical students in the United States are required to be exposed to 10 courses and 34 specific diseases, and perform 24 procedural skills (including the indications, contraindications, and complications) competently during their 4-week rotation. As compared with the United States, obligatory courses that are not taught in all Chinese medical schools include cardiac arrest, gastrointestinal bleeding, headache, poisoning, shock, and trauma, while only three procedural skills are trained in China. This suggests that a detailed uniform EM curriculum that outlines exact requirements for medical students may be needed to improve educational attainment in China. For example, courses should be based on basic life support, advanced life support, common emergencies (chest pain, dizziness, abdominal pain, trauma, cardiac arrest, etc.), poisoning, emergency medication, and so on. At the same time, the emergency operation training for students should be standardized; teaching and assessment should be carried out in strict accordance with the guidelines. And we advocate that a consolidated textbook, syllabus, and curriculum should be compiled and agreed upon by all the medical schools with the 8-year integrated MD degree program.
In terms of the limitations of our survey, we acknowledge that although we contacted all 14 medical schools to distribute the survey, we receive few responses from certain medical schools, including School of Medicine of Tsinghua University and Second Military Medical University. Thus, the comprehensiveness and representative of our results are less than ideal. Besides, the accuracy of individual responses could not be fully validated. We tried to partially validate the individual questionnaire results, by comparing the responses of some compulsory questions which had a set answer, such as asking for the number of students in the respondents’ medical school. Responses whose answers differ from the majority of respondents were deemed to be invalid and not included in the data analysis.
Conclusion
Our observational survey suggests that EM curriculum varies widely in 8-year integrated MD program in China, and students have reported variable experiences. We found that though many medical students complained about deficient EM classes and inefficient clinical practice, they remained interested in attending further classes and training in EM department. The specific diseases and skills that should be covered in emergency medical education remain up to debate. It is overwhelmingly clear that there is an urgent need to create a uniform EM curriculum with clear learning objectives and standardized assessments to ensure the competency of tomorrow’s doctors, especially in resource-limited developing countries. 11
The questionnaire is translated into English and attached as Supplementary File 6.
Supplemental Material
sj-docx-1-hkj-10.1177_10249079211040971 – Supplemental material for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China
Supplemental material, sj-docx-1-hkj-10.1177_10249079211040971 for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China by Zengzheng Ge, Shi Feng, Xiangning Liu, Shigong Guo, Yanxia Gao, Xin Lu, Shiyuan Yu, Lina Zhao, Di Shi, Jihai Liu, Huadong Zhu and Yi Li in Hong Kong Journal of Emergency Medicine
Supplemental Material
sj-docx-2-hkj-10.1177_10249079211040971 – Supplemental material for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China
Supplemental material, sj-docx-2-hkj-10.1177_10249079211040971 for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China by Zengzheng Ge, Shi Feng, Xiangning Liu, Shigong Guo, Yanxia Gao, Xin Lu, Shiyuan Yu, Lina Zhao, Di Shi, Jihai Liu, Huadong Zhu and Yi Li in Hong Kong Journal of Emergency Medicine
Supplemental Material
sj-docx-3-hkj-10.1177_10249079211040971 – Supplemental material for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China
Supplemental material, sj-docx-3-hkj-10.1177_10249079211040971 for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China by Zengzheng Ge, Shi Feng, Xiangning Liu, Shigong Guo, Yanxia Gao, Xin Lu, Shiyuan Yu, Lina Zhao, Di Shi, Jihai Liu, Huadong Zhu and Yi Li in Hong Kong Journal of Emergency Medicine
Supplemental Material
sj-docx-4-hkj-10.1177_10249079211040971 – Supplemental material for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China
Supplemental material, sj-docx-4-hkj-10.1177_10249079211040971 for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China by Zengzheng Ge, Shi Feng, Xiangning Liu, Shigong Guo, Yanxia Gao, Xin Lu, Shiyuan Yu, Lina Zhao, Di Shi, Jihai Liu, Huadong Zhu and Yi Li in Hong Kong Journal of Emergency Medicine
Supplemental Material
sj-docx-5-hkj-10.1177_10249079211040971 – Supplemental material for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China
Supplemental material, sj-docx-5-hkj-10.1177_10249079211040971 for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China by Zengzheng Ge, Shi Feng, Xiangning Liu, Shigong Guo, Yanxia Gao, Xin Lu, Shiyuan Yu, Lina Zhao, Di Shi, Jihai Liu, Huadong Zhu and Yi Li in Hong Kong Journal of Emergency Medicine
Supplemental Material
sj-docx-6-hkj-10.1177_10249079211040971 – Supplemental material for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China
Supplemental material, sj-docx-6-hkj-10.1177_10249079211040971 for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China by Zengzheng Ge, Shi Feng, Xiangning Liu, Shigong Guo, Yanxia Gao, Xin Lu, Shiyuan Yu, Lina Zhao, Di Shi, Jihai Liu, Huadong Zhu and Yi Li in Hong Kong Journal of Emergency Medicine
Supplemental Material
sj-docx-7-hkj-10.1177_10249079211040971 – Supplemental material for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China
Supplemental material, sj-docx-7-hkj-10.1177_10249079211040971 for Current situation and expectation of emergency medicine education for 8-year Doctor of Medicine degree program in China by Zengzheng Ge, Shi Feng, Xiangning Liu, Shigong Guo, Yanxia Gao, Xin Lu, Shiyuan Yu, Lina Zhao, Di Shi, Jihai Liu, Huadong Zhu and Yi Li in Hong Kong Journal of Emergency Medicine
Footnotes
Acknowledgements
We are very grateful to Prof. Xiangyu Chen, Prof. Gang Zhao, Prof. Qilin Li, Prof. Yaxiong Zhou, Prof. Longyuan Jiang, Prof. Ruilan Wang, Prof. Jian Lu, Prof. Hongliang Zhang, Prof. Yuyan Ma, Prof. Zongru Li, Prof. Pengcheng Li, Prof. Meitang Wang, and Prof. Wenyuan Jia for their great help in issuing the questionnaires.
Author contributions
Dr. Zengzheng Ge and Dr. Shi Feng contributed equally to this study. All the authors participated in the conceptual design and development of the completed manuscript. Dr. Yi Li, Dr. Huadong Zhu, Dr. Jihai Liu, Dr. Di Shi, Dr. Yanxia Gao, Dr. Zengzheng Ge, Dr. Shi Feng, and Dr. Xiangning Liu set up the idea for writing the paper and wrote the draft of the questionnaire. Dr. Shigong Guo and Dr. Yanxia Gao revised the questionnaire. Dr. Xin Lu and Dr. Shiyuan Yu contact with medical schools and distribute the questionnaire. Dr. Lina Zhao, Dr. Zengzheng Ge, Dr. Di Shi, Dr. Jihai Liu, and Huadong Zhu collected and analyzed the data. Dr. Zengzheng Ge and Dr. Shi Feng wrote the first draft of the manuscript. Dr. Yi Li revised the paper and made the final version of the manuscript. All authors have reviewed and approved the manuscript for publication.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the CAMS Online Open Course Construction Fund (J2009022861), Chinese Academy of Medical Sciences (CAMS) Teaching Reform Research Fund (grant number 2018zlgc0101), and CAMS Innovation Fund for Medical Sciences (CIFMS), serial number 2020-I2M-C&T-B-014.
Ethical approval
Ethical approval was waived by Peking University Medical College Hospital (PUMCH) Ethics Committee because no information about patients or their families was involved. We researchers have no direct contact with participants, because this research survey deployed via an online survey platform called “Wenjuanxing” and the questionnaire was sent by WeChat.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
