Abstract
Doxorubicin is a broad-spectrum antibiotic and anticancer drug used to treat a variety of human malignancies like breast cancer and leukaemia. Unfortunately, a dose-dependent side effect of this drug is common, representing a major obstacle to its use despite its therapeutic efficacy. Photodynamic therapy is an emerging non-invasive potential adjuvant for conventional cancer treatment. In an attempt to circumvent the dose-limiting effect of doxorubicin, this study aimed to investigate cellular anticancer activity of doxorubicin and sulfonated zinc phthalocyanine–mediated photodynamic therapy on MCF-7 cells alone and in combination. Furthermore, we investigated the cell death pathway resulting from the combination treatment. MCF-7 cells were incubated with 0.5 µM concentration of doxorubicin for 20 h, afterwards, various concentrations of sulfonated zinc phthalocyanine were added and incubated for 4 h. Cells were irradiated using a 681.5 nm diode laser at 4.53 mW/cm2 for 18 min 24 s (5 J/cm2). Cell viability and proliferation were measured using trypan blue assay and homogeneous adenosine triphosphate quantitation assay, respectively, while qualitative changes in cellular morphology were observed under inverted light microscopy. Cellular DNA damage was assessed under fluorescent microscopy and Annexin V/propidium iodide stain was used to investigate the cell death pathway. Findings from this study shown that combined treatment with doxorubicin and photodynamic therapy was more effective in inhibiting the proliferation and growth of MCF-7 cells. Overall, the results indicate that combination of smaller dose of doxorubicin with photodynamic therapy is a promising combined treatment strategy for breast carcinoma. However, this combination warrants further investigation.
Introduction
Cancer is a genetic disease characterized by abnormal cell growth, proliferation, and metastasis that leads to high mortality.1,2 Over the past 50 years, breast cancer has continued to dominate among women in all areas of life with global estimate of one in every nine women developing the disease during their lifetime. 3 This global trend of breast cancer among women is attributed to rapid societ al, economic, and lifestyle changes leading to a steady rise in incidence (25%) and mortality (15%) rate, respectively. 4
Doxorubicin (DOX) is a DNA intercalating agent used to treat a variety of neo-plastic diseases and cancers, such as leukaemia, breast cancer, and cervical cancer. It is isolated from a mutant strain of Streptomyces peucetius and belongs to anthracycline family of antibiotics with structural similarities to daunorubicin, epirubicin, and idarubicin.5,6 Its molecular mechanism of action includes intercalating with DNA and disruption of topoisomerase II enzyme, thus halting biological process of DNA replication and ultimately leading to cell death. 7 Another recognized antineoplastic mechanism of DOX is linked to its ability to induce oxidative stress through production of reactive oxygen species where intracellular oxidoreductase reacts with DOX metabolites to produce semiquinone radical and reactive oxygen species. 8 Although DOX is effective in the treatment of breast cancer, its use is limited by cardiotoxicity, nephrotoxicity, alopecia, and hematopoietic suppression. 6 Hence, DOX alone is not preferable and an alternative intervention to supplement its activity with less toxic effects is needed. Therefore, combining DOX at low dose with alternative therapies like photodynamic therapy (PDT) might be promising.
PDT is a photochemical process of inducing localized tissue damage through administration of a photosensitizer followed by light irradiation that initiates tumour damage. 9 This treatment modality combines the interaction between an excited photosensitizer and molecular oxygen to cause injury and death of targeted cells.10,11 Sulfonated zinc phthalocyanine (ZnPcS) is one of the photosensitizers that has been used to understand the effect of PDT.12–14 ZnPcS-PDT has shown its efficacy as a potential novel therapeutic approach for in vitro breast cancer cell line. 10 Although PDT can be used to cure early tumours, it cannot achieve cure for advanced metastatic cancers due to its localized effect. Hence, PDT in combination with chemotherapy is among many strategies which have been proposed to potentiate the therapeutic outcome of low-dose chemotherapy and thus minimize side effects and acquisition of drug resistance.15,16 Thus herein, we examined the antitumour cellular responses of DOX treatment alone and in combination with ZnPcS-PDT on MCF-7 breast cancer cells and to further explore the possible cell death pathway induced by the combination therapy.
Materials and methods
Cell culture
Commercially purchased MCF-7 breast cancer cell line (ATCC HTB-22) was used and ethical approval was obtained for this study. Cells were cultured in Dulbecco’s Modified Eagle’s Medium (Sigma Aldrich: D5796) supplemented with 10% foetal bovine serum (FBS; Gibco), 1% penicillin/streptomycin (Sigma Aldrich; P4333) and 1% Amphotericin B (Sigma Aldrich, A2942) in an 85% humidified atmosphere at 37°C and 5% CO2. Cells were grown in T175 culture flask and subcultured twice a week when confluent. Experimental cells were seeded in 35 mm culture dishes at a concentration of 5 × 105 cells/3 mL of culture media and incubated for 4 h to allow the cells to attach and homeostatic recovery, prior to performing each experiment.
Treatments and laser irradiation
Experiments were performed with cells between passages 11 and 30. For dose–response studies, cells were treated with an increasing concentrations of DOX (0.3, 0.6, 0.9, 1.2 and 1.5 µM) and ZnPcS (0.125, 0.25, 0.5, 1 and 2 µM) for PDT treatments. Cellular responses were analysed after 24 h of treatment to determine optimal inhibitory concentrations. To perform combination therapy, cells were incubated with 0.5 µM concentration of DOX for 20 h. Afterwards, concentrations of ZnPcS were added and incubated for 4 h. Monolayers of MCF-7 cells in phosphate-buffered saline (PBS) (Sigma Aldrich; P5493) were irradiated from above with the lid off in the dark at room temperature with 681.5 nm diode laser at 4.53 mW/cm2 for 18 min 24 s (5 J/cm2). Time of exposure was calculated using the following equation: irradiance (J/cm2) = time (s) × [power (W)/surface (cm2)]. After irradiation, cells were rinsed three times with Hanks’ Balanced Salt Solution (HBSS) (Sigma Aldrich; H9394) and further re-incubated for 24 h before treatment, and cellular response assays were carried out and further re-incubated for 24 h before cellular response assays were carried out.
DOX and photosensitizer
DOX hydrochloride was purchased from Sigma Aldrich (D1515), dissolved in 0.5% dimethyl sulfoxide (DMSO), and stored as 0.0172 M stock solution. As a photosensitizer, a mixed isomer of ZnPcS with fuming sulphuric acid (30% SO3) synthesized at Rhodes University in South Africa 17 and dissolved in PBS was used in this study.
Morphological assessment
Morphological changes were assessed 24 h after treatment using inverted light microscope (Wirsam, Olympus CKX41) and pictures were taken using SC30 Olympus camera.
Trypan blue assay
Trypan blue assay (Sigma-Aldrich T8154) was used to determine the percentage viability of treated MCF-7 cells. Briefly, the cells were mixed with equal volume (10 µL) of trypan blue stain and loaded into plastic, disposable Countess® Cell Counting Chamber Slides. Cell count was performed with Invitrogen Countess II flan automated bench top cell counter. Viable cells with intact membrane will not take up the stain, while non-viable cells with damaged membrane will stain blue.
Adenosine triphosphate assay
Adenosine triphosphate (ATP) assay was used to evaluate mitochondrial activity of the cells. This assay homogenously measure and quantify the number of ATP produced by metabolically active cells. It involves the addition of equal volume (50 µL) of cell Titer-Glo® luminescent cell viability reconstituted reagent (Promega; G7570) directly to cells in culture medium, which results in the production of a luminescent signal that corresponds to the amount of ATP present. The mixture was allowed to stabilize at room temperature for 10 min before measuring the luminescence using the Perkin-Elmer, VICTOR3™Multilabel Counter (Model 1420) in relative light units.
Cytotoxicity assay
Cell membrane integrity was assessed by measuring the amount of lactate dehydrogenase (LDH) released into the culture medium. LDH is a cytosolic enzyme released due to membrane damage. The CytoTox 96® Non-Radioactive Cytotoxicity Assay (Promega; G1780) was used to measure the LDH by incubating equal volume (50 µL) of reconstituted reagent with the culture medium at room temperature for 30 min before measuring the absorbance at 490 nm using Perkin-Elmer, VICTOR3™Multilabel Counter (Model 1420).
Flow cytometry
Fluorescein isothiocyanate (FITC) Annexin V/propidium iodide (PI) Apoptosis detection kits (BD Pharmingen™; 556570) were used according to the manufacturer’s instruction to determine the percentage of cells undergoing apoptosis. Briefly, harvested cells were washed twice with cold PBS in a 5-mL culture tube and cells were suspended in binding buffer solution. Thereafter, 5 µL of FITC Annexin V and 5 µL of PI were added to the mixture. The tube with the mixture was incubated at room temperature in dark for 15 min and analysed using BD Acurri flow cytometry.
Nuclear assessment using Hoechst stain
MCF-7 cells were seeded at a concentration of 1 × 105 cells in a culture dish and treated with optimal inhibitory concentrations (IC50) of DOX (0.9 µM), ZnPcS-PDT (1.1 µM) and in combination (0.5 µM DOX, 0.4 µM ZnPcS-PDT). After 24-h incubation, cells were stained with 1 µg/mL Hoechst stain at room temperature for 15 min. Thereafter, the cells were rinsed with PBS buffer and were examined using Carl Zeiss Axio Z1 Observer.
Statistics
Results were represented as mean ± standard error. Replicate independent experiments were performed four times (n = 4) with assays run in duplicate. One-way analysis of variance (ANOVA) (Dunnett test) was performed to compare experimental control and treated cells. Statistical significance defined as p value less than 0.05 (*), 0.01 (**) and 0.001 (***) was evaluated using Sigma Plot version 13.0.
Results
Cellular morphology microscopy
After culture, cells were treated individually with DOX, ZnPcS-PDT and a combination of DOX and ZnPcS-PDT. The untreated control cells shows normal epithelia-like structure of MCF-7 cells with no morphological changes and present high level of cellular proliferation and viability. However, in cells that were treated with DOX, ZnPcS-PDT or combination of both, we observed morphological changes like rounding up and floating of cells in the culture medium which is an indication of dying cells (Figure 1). In addition, there was a considerable decrease in cellular number within the treated groups. These cellular changes appear to be in a dose-dependent manner with the highest decrease observed in combination group (0.5 µM DOX and 1 µM ZnPcS-PDT).

Morphological changes observed using inverted light microscopy. (a) Experimental control and (b) dark toxicity of zinc phthalocyanine showed normal epithelial morphology of MCF-7 cells. Cells treated with (c) DOX (0.5 µM) alone showed slight morphological changes compared to control. (d–f) Zinc phthalocyanine (0.25, 0.5 and 1 µM)-mediated photodynamic therapy, respectively, treated alone and (g–i) in combination with DOX (0.5 µM) showed visible changes in cell morphology whereby cells rounded-up, detached and floated in culture dish thus indicating cell death. Magnification 200× and scale bar: 100 µM.
Effects of DOX and ZnPcS-PDT on MCF-7 cell viability and proliferation
In this study, we aimed to investigate the effects of DOX and ZnPcS-PDT, alone and in combination on breast cancer cells. First, after a dose–response study with DOX and ZnPcS-PDT, it was observed that both treatments inhibit the viability of MCF-7 cells in a dose-dependent manner with an optimal inhibitory concentration (IC50) of 0.9 and 1.1 µM, respectively (Figure 2). The suboptimal concentration (IC30) of DOX was observed to be 0.5 µM and was subsequently used in further combination experiments. To evaluate the effect of a low dose DOX in combination with ZnPcS-PDT, cells were co-treated with a constant (IC30) dose of DOX and increasing concentration of ZnPcS-PDT (0.25, 0.5 and 1 µM). Results of this combination showed a significant reduction in the cell viability with highest inhibition seen when 0.5 µM DOX and 1 µM ZnPcS-PDT were used (Table 1).

Trypan blue cellular viability assay. Response of MCF-7 cell treatment with different concentrations of doxorubicin (DOX) and zinc phthalocyanine–mediated photodynamic therapy (ZnPcS-PDT) after 24 h. Cellular viability decreased in a dose-dependent manner in both cells treated with DOX and ZnPcS-PDT. Data are presented as the mean ± SE from four independent duplicate experiments.
Trypan blue viability and lactose dehydrogenase (LDH) membrane integrity cytotoxicity assay (A490 nm).

DMSO: dimethyl sulfoxide; ZnPcS-PDT: sulfonated zinc phthalocyanine–mediated photodynamic therapy; DOX: doxorubicin.
The cellular viability showed a significant decrease within the combined treated groups and increased dose of ZnPcS-PDT (0.5, 1 µM) when compared to experimental control. There was a dose-dependent increase in cytotoxicity when compared to experimental control cells. Values are mean ± SE of four independent assays performed in duplicates.
Significant differences between experimental controls and treated cells are shown as *p < 0.05, **p < 0.01 and ***p < 0.001.
Likewise, cellular proliferation was measured using ATP assay and significant decrease in cell proliferation was noticed (Figure 3). There was a significant reduction in the proliferation of MCF-7 cells when DOX and ZnPcS-PDT were used either alone or in combination compared to experimental control cells. There was no significant difference when each treatment was used alone at 0.5 µM concentration. However, when both treatments were combined together at lower doses of 0.5 µM DOX and 0.25 µM ZnPcS-PDT and above, a significant decrease in cell proliferation was observed (Figure 3).

Cell proliferation measured by adenosine triphosphate (ATP) luminescent assay. Doxorubicin (DOX) at 0.5 µM and zinc phthalocyanine–mediated photodynamic therapy (ZnPcS-PDT) at 0.25, 0.5 and 1 µM were not significant when compared to experimental control. But combination of both treatments results in significant decrease in cellular proliferation compared to experimental control. Results represent the mean ± SE of four independent duplicate experiments.
Cytotoxic effect of DOX and ZnPcS-PDT in MCF-7 cells
Cytotoxicity was analysed by measuring the amount of LDH released into the culture media subsequent to MCF-7 cell treatment with DOX and ZnPcS-PDT alone and in combination. After treatment, the amount of LDH released was measured in cells treated with DOX and ZnPcS-PDT alone and in combination. There was an increased amount of LDH release, which corresponds to increased cytotoxicity within the combined treated groups as compared with individual treatments (Table 1). It was also noted that the highest LDH release was observed with 0.5 µM DOX and 1 µM ZnPcS-PDT. This result supports trypan blue viability and ATP proliferation assays, which suggested a decreased viability and biological activity of MCF-7 cells treated with both DOX and ZnPcS-PDT.
Furthermore, we studied the combination treatment effect from the trypan blue viability results to assess the type of interaction that exists between the two anticancer agents. To this effect, viability assay results of the combination treatment were analysed using the combination index (CI). Sequentially, combination of 0.5 µM DOX with 0.4 and 1.1 µM ZnPcS-PDT inhibits 50% and 70% of MCF-7 cell viability in a synergistic manner (Table 2).
Combination index (CI) analysis.

DOX: doxorubicin; ZnPcS-PDT: sulfonated zinc phthalocyanine–mediated photodynamic therapy.
Suboptimal inhibitory concentration (IC30) of DOX (0.5 µM) was kept constant in combination studies. Combination of 0.5 µM DOX with 0.4 and 1.1 µM ZnPcS-PDT results in IC50 and IC70, respectively. The combination index was <1, which indicates a synergistic interaction.
Cell death analysis
We further investigated the mode of cell death of each individual treatment and their combination. To this effect, cells were stained after treatment with Annexin V-FITC/PI for 15 min and analysed using flow cytometry to determine the population of cells undergoing apoptosis. We observed that the majority of cells in the control group were negative to both Annexin V-FITC and PI stain, which suggests viable non-apoptotic cells, whereas the cells treated with DOX and ZnPcS-PDT or their combination showed significant changes. The result showed that greater percentage of cells in the combination group were undergoing early or late apoptotic cell death (Supplementary Material). Changes in necrotic cell populations (positive for PI) were not observed in any of the treated groups (Table 3).
Flow cytometric assessment of cell death pathway.

LL: live cells; LR: early apoptotic cells; UR: late apoptotic cells; UL: non-apoptotic cells; DOX: doxorubicin; ZnPcS-PDT: sulfonated zinc phthalocyanine–mediated photodynamic therapy; FITC: fluorescein isothiocyanate; PI: propidium iodide.
Annexin V-FITC/PI staining used to investigate apoptosis within the various treated groups. There was a slight number of cells undergoing apoptosis in DOX treated group whereas a significant number of cells were in both early and late apoptotic stages in the combined treated group (DOX + ZnPcS-PDT). Results represent the mean ± SE of three independent duplicate experiment.
Significant differences between treated and control are shown as ***p < 0.001 and **p < 0.01.
Nuclear assessment for DNA damage
The blue Hoechst nuclear stain was used to assess the level of DNA damage in each treatment groups and was compared to the untreated control cells. Results showed a perfectly dense spherical nucleus without any damage in the control cells, while the cells treated with DOX and ZnPcS-PDT alone and in combination showed irregular nuclear shrinkage with nucleus gradually becoming smaller, which suggests nuclear condensation and DNA damage.
Discussion
DOX remains subject of intense study after its introduction 40 years ago which reflects its importance as an anticancer agent. Conversely, its use has been limited despite its active effect against proliferating cancer cells due to the risk of cardiac damage and acquisition of resistance associated with it.18–22 PDT is an emerging treatment modality whose mode of action does not usually cause the emergence of resistance and can be used as a potential adjuvant for conventional cancer treatment.23–26 Some recent studies have focused on potentiating the advantage of single therapy by combining it with other treatment modalities to obtain a better response. Among these strategic treatment is the combination of chemotherapy and novel PDT.11,27 Lanks et al. 28 studied DOX photosensitizing potential on murine L929 cancer cells and the result showed an additional phototoxicity with an absorption maximum of 579 nm. They also observed an increased cytotoxic mechanism of DOX, which is dependent on increased production of oxygen radicals. 28 Moreover, unique 1O2-dependent cytotoxic effects of PDT have provided a rationale for its combination with DOX to enhance their antitumour effect without overlapping toxicity. 29
Hence, in this study, we investigated the effects of DOX and ZnPcS-PDT and examined whether the combination of low dose concentration of DOX and ZnPcS-PDT on MCF-7 cells could serve as a novel treatment for human breast cancer. Morphological assessment of the cells after treatment showed cellular changes like disruption of cell membrane and rounding up of cells indicating cell death. This is in line with the reports of Tynga et al. 10 and El-Hussein et al., 1 which showed an irregular disruption of MCF-7 cell membrane after PDT treatment using a metallophthalocyanine photosensitizer. DOX and ZnPcS-PDT treatment alone was found to inhibit the cell viability and proliferation of MCF-7 cancer cells in a dose-dependent manner. Regarding ZnPcS-PDT, current findings are in agreement with previous studies which demonstrates that increasing dose of phthalocyanine photosensitizer and laser irradiation adversely reduces the proliferation and viability of MCF-7 cancer cells.10,30 Similarly, increased dosage of DOX adversely decreases the breast cancer cell survival.31,32 ZnPcS-PDT also displays therapeutic efficacy in a similar manner within other cancer cell lines like human lungs (A549) and colon cancer cell (DLD-1).33,34 The combination of DOX and ZnPcS-PDT was found to significantly decrease the viability and increase the cytotoxicity of cancer cells compared to the ZnPcS-PDT and DOX alone. CI analysis used to quantitatively evaluate the interactive effects of DOX and ZnPcS-PDT and combination showed a CI <1. These according to Chou 35 and Tallarida 36 indicate that the effect of the combination is greater than the individual effect of the treatment regime. Thus, DOX and ZnPcS-PDT combination used in this study exerts a synergistic effect. Indeed, recent in vitro experiments reported better efficacy of about 25% cell survival of HeLa cells when combined chemotherapeutic treatment of DOX and pheophorbide a (PhA)-mediated photodynamic treatments is used unlike individual treatments. 37 Here, we also show that lower concentration of DOX with higher concentration of ZnPcS-PDT results in increased antitumour effect. Similar observations were made by Diez et al. 38 when leukemic murine cells were treated with a combination of DOX and aminolevulinic acid (ALA)-PDT. They reported a significant decrease in viability of leukemic murine cells in comparison with control cells and each treatment alone. Our findings were further confirmed by the results of flow cytometry investigation for cell death and DNA damage analysis using Hoechst nuclear stain. The results indicate that combination of DOX and ZnPcS-PDT triggers apoptosis and leads to increased yield of apoptotic MCF-7 cells. A similar study by de Freitas et al. 39 on cervical cancer cells noted an increased rate of apoptosis and percentage of dead cells with combined treatment of cisplatin and photogem-mediated PDT. Our results suggest that PDT can potentially serve as an adjuvant therapy for DOX. Likewise, it has been reported that DOX and aluminum disulfonated phthalocyanine–induced PDT significantly showed an additive antitumour effect on mice bearing L1210 leukaemia and P388 lymphoma. 40 In vitro and in vivo interactive combination studies of DOX and PDT mediated by meta-tetra (3-hydroxyphenyl)-chlorin (mTHPC) on murine hepatoma (MH-22A) cells have demonstrated that DOX potentiates the therapeutic efficacy of mTHPC-mediated PDT in both in vitro and in vivo conditions. 41 Elsewhere, adriamycin has been shown to enhance the antitumour effects of hematoporphyrin derivative–mediated phototherapy on murine tumour model through the production of toxic oxygen radicals. 42
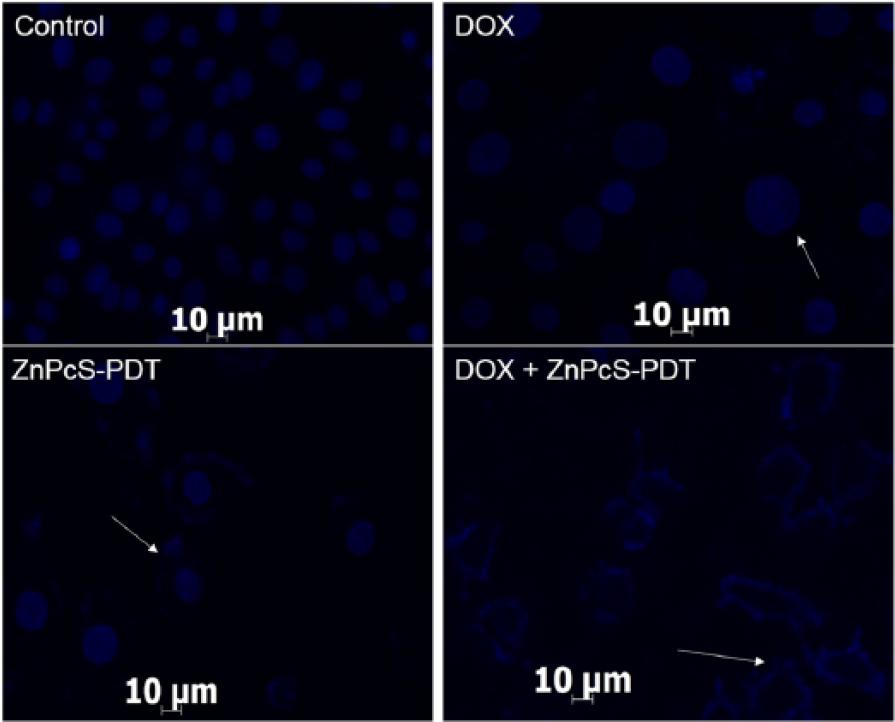
Investigation of nuclear DNA damage using Hoechst stain. Control cells showed a perfectly dense spherical nucleus without any damage. Cells treated with doxorubicin (DOX) showed cellular swelling and cells treated with zinc phthalocyanine–mediated photodynamic therapy (ZnPcS-PDT) showed chromatin granules shrinkage with smaller nucleus. Cells treated with combined therapy (DOX + ZnPcS-PDT) showed scattered nuclear granules, with irregular shape, indicative of nuclear fragmentation damage. Images were obtained using Carl Zeiss Axio Z1 Observer. Magnification 400× oil immersion and scale bar: 10 µm.
Programmed cell death otherwise called apoptosis is a vital process that maintains homeostasis within the cell. Its induction in cells is essential for cancer cure since defects in the regulation of apoptosis leads to cancer. 43 Apoptotic cell death pathway was observed in this study, which was more evidenced when both treatment modalities were used together. Various reports suggested that DOX activity is dependent on concentration and time of exposure thus triggering apoptotic induction of cell death.44,45 Within the mitochondria, DOX metabolism can disrupt respiration and lead to the release of cytochrome C, which initiates apoptosis. A significant apoptotic cells were observed when MCF-7 breast cancer cells were incubated with 10 µM DOX for 72 h when compared with 12-h incubation at same concentration. 32 Previous reports from our laboratory have showed that PDT induces apoptotic cell death.1,9 Moreover, Wu et al. 46 report a significant cleavage of PARP (poly (ADP-ribose) polymerase) and activation of caspase-7 when MCF-7 cells were treated with combined DOX (10 µM) and dihydroartemisinin (20 µM) for 24 h. Diez et al. 38 reported the morphological changes supporting the apoptotic cell death in murine leukemic cell line when combined therapies were used. They evaluated the exposure of phosphatidylserine on the plasma membrane of the cell and observed an increased apoptotic cell fraction when murine leukemic cells were treated with combination therapies of DOX and ALA-PDT. Although there were necrotic features observed but it was low when compared to the apoptotic features, thus suggesting that apoptosis is the major death pathway involved in the combination treatment of DOX and ALA-PDT on murine leukemic cells. Similarly, ZnPcS-PDT has also shown to trigger cell death through apoptotic mechanism in both enzyme-linked immunosorbent assay (ELISA)-based DNA fragmentation and flow cytometric assay. 47 After PDT and staining of cells with Annexin V/FITC, increased yield of apoptotic cells was observed. Mitochondria are one of the primary targets of PDT-mediated cellular damage. Thus, damage to mitochondria could lead to the release of cytochrome C and apoptotic inducing factors (AIF) which initiates apoptotic cascade and ultimately cell death. 48 A combination therapy is one of the leading forefronts of research towards cancer malignancies which have shown a more favourable outcome. This necessitates the development of different anticancer components that exert damage by different modes of action. However, the lack of understanding about the intersection of critical signalling pathways remains a major barrier. Our study has shown how important anticancer agent like DOX can be ultimately utilized in a more effective approach. Likewise, the selective effects of PDT on malignant cells enable its combination with other treatment modalities to enhance its therapeutic efficacy. In conclusion, this study suggests that lower dose of DOX when combined with PDT has significant synergistic effect on MCF-7 cancer cells and increases the yield of apoptotic cells. Thus, this approach may serve as a promising strategy for breast cancer treatment in future. We recommend further investigation of this combination to delineate its potential to reverse multidrug resistance cancer treatment in in vivo studies.
Footnotes
Acknowledgements
The authors sincerely thank the University of Johannesburg and the National Laser Centre, as well as the African Laser Centre (ALC) for postgraduate student monetary support.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work is based on the research supported by the South African Research Chairs Initiative of the Department of Science and Technology and National Research Foundation of South Africa (Grant No 98337).
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
