Abstract
Background
Lumbar canal stenosis (LCS) is a degenerative spinal condition causing narrowing of the spinal canal, leading to nerve compression. Symptoms include pain, stiffness, tingling, numbness, and difficulty walking, which worsen with standing and improvement with sitting. Conventional treatments offer symptomatic relief, while surgery carries risks and a high recurrence rate. Ayurveda provides a holistic, non-surgical approach through Shodhana (purification) and Shamana Chikitsa (palliative care).
Objectives
This study evaluates the effectiveness of Ayurvedic therapies, including Panchakarma and oral medications, in managing lumbar canal stenosis.
Methodology
A 68-year-old male presented with lower back pain radiating to both legs, tingling, numbness, and difficulty walking for nine months following a road traffic accident. He underwent an 8-day Panchakarma therapy, including Sarvanga Snehana and Swedana, Kati Basti, and Yoga Basti, which included Matra Basti and Niruha Basti along with oral medications.
Results
After 8 days treatment, the patient experienced significant symptom relief, improved mobility, and enhanced ability to perform daily activities independently.
Conclusion
This case highlights the effectiveness of Ayurvedic therapies in managing LCS, suggesting Panchakarma and oral medications as a viable non-surgical alternative. Further research on larger populations is needed to validate these findings.
Keywords
Introduction
Due to the changing nature of work and lifestyles, low back pain is a prevalent condition in the modern world. Most people suffer from lower back discomfort that radiates to the foot and restricts their spine’s motion. When the spinal canal narrows and compresses the nerves and blood vessels at the level of the lumbar region vertebrae, a medical condition known as lumbar canal stenosis results. 1 Lumbar spinal stenosis symptoms include low back or buttock pain, numbness in the legs, thighs, feet, or buttocks, as well as loss of control over one’s bladder and bowels. 2 Possible causes of the disease include aging, trauma, spinal arthritis, spondylolisthesis, local tumors, and in rare instances, the disease’s congenital origin. 3 Common signs of the condition include pain, compressive sensations, and difficulty walking. It is determined by the patient’s medical history, physical examination, and imaging tests. In the conventional medical system, it is treated with physiotherapy, non-steroidal anti-inflammatory drugs (NSAIDs), and surgical laminectomy. 4 According to reports, there are five incidents of lumbar canal stenosis per 100,000 individuals yearly, four times more than the cases of cervical canal stenosis. 5 According to a community-based cross-sectional survey conducted in Wardha, the majority (82%) of brick-making employees reported having musculoskeletal complaints at some point in the previous year in their shoulders, followed by their lower backs (71%). 6 Research studies show that 10–30% of patients experience recurrent symptoms after surgical treatment for lumbar canal stenosis, highlighting the need for effective non-surgical alternatives like Ayurvedic therapies. 7 While conventional pharmacological treatments can manage pain and inflammation, they often result in side effects such as gastrointestinal issues and dependency. Ayurvedic treatments focus on restoring balance and enhancing overall wellness, employing techniques like Panchakarma to detoxify the body and potentially offer more sustainable outcomes. Integrating Ayurvedic methods with conventional treatments could provide a comprehensive strategy for managing lumbar canal stenosis, improving patient quality of life while reducing recurrence rates.
The classics do not describe Katigraha as a separate entity. Charaka Samhita mentions it as one of the Vatavyadhi. Eighty Nanatmaja Vatavyadhi has been stated in Charaka Samhita. 8 It comes from two terms, Kati and Graha. The disease causes pain and stiffness as the vitiated Vata becomes localized in the Kati Pradesh. 9 Since the lumbar spine is one of the primary seats of the Vata Dosha, it becomes vitiated in its seat, including the Sphik (buttock), Kati (waist), Uru (thigh), Janu (knee), Jangha (calf), and Pada (foot). 10 The cardinal symptoms of the disease are Ruk (pain), Toda (pins and needles), Stambha (stiffness), and Muhuspandana (twitching and cramping). 11 Snehana (oleation therapy), Swedana (sudation therapy), and Vatahara Shamana Yogas (palliative care) are among the Ayurvedic treatments. 12 The major treatment for the vitiated Vata is the Basti procedure (medicated retention enema). Acharya Charaka indicated that “Kshir Basti” and “Sneha Basti” were in charge of managing “Asthi Prodoshaj Vyadhi.” 13 Hence, this case study describes how the Vatavyadhi principle has been applied to treat lumbar canal stenosis effectively.
Case Report
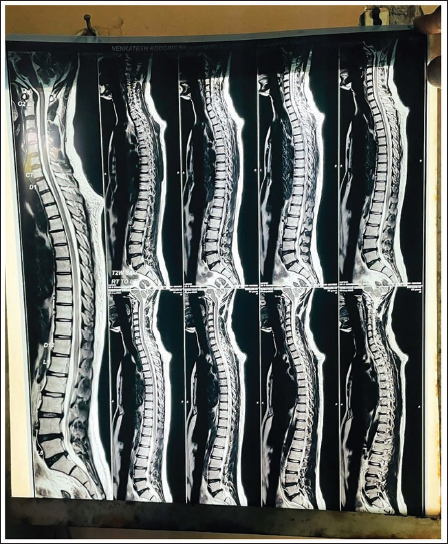
A male patient of 68 years visited the outpatient department of MGACH & RC with chief complaints of pain and stiffness in the lower back, radiating to both legs, associated with a tingling sensation, numbness, and difficulty in walking for the past 9 months. He had a history of a road traffic accident and developed these symptoms as a result. The patient was diagnosed with lumbar canal stenosis at MGIMS, Sevagram, Wardha, and was treated with Cap Pregaba 75 1 BD for 8 weeks, Tab Flexon MR 1 BD, and Tab Pantop 40 1 OD for 10 days, but did not get total relief. He experienced partial relief from the prescribed medication but had concerns about side effects and was dissatisfied with the overall effectiveness. Motivated by the desire for a more holistic and effective treatment, he decided to pursue Ayurvedic therapy, hoping to alleviate his symptoms and improve his quality of life. So, he approached our institution for further management. His magnetic resonance imaging (MRI) LS Spine reports suggested lumbar stenosis at L3-L4 and L5-S1 due to a diffuse disc bulge with a posterior-central annular tear, as shown by the MRI (Figures 1 and 2). All vital signs were normal (Table 1).
Magnetic Resonance Imaging (MRI) Report.

Magnetic Resonance Imaging (MRI) LS Spine.
Ashtavidha and Dashavidha Parishka.
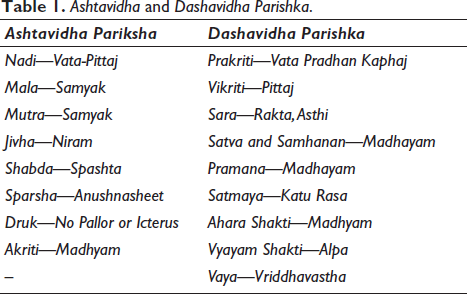
Specific Examination
The central nervous system, respiratory system, and cardiovascular system examinations were all normal. Upon inspection, no swelling, scar, or deformity was observed on the bilateral examination of the sacroiliac joint. However, palpation revealed mild tenderness of grade 2. The compression test was positive, and the range of motion (ROM) was restricted and painful. On inspecting and palpating the lumbar spine, specifically the L3-L5 region, no deformity, scar, or swelling was observed, though mild tenderness of grade 2 was present. The straight leg raising test (SLRT) yielded a negative result, indicating no significant nerve tension. In terms of the nervous system, the motor system of the right lower limb showed reduced muscle tone, which is classified as hypotonic. Muscle bulk in both lower limbs was symmetrical and equal. However, coordination was impaired, as the individual could not perform tandem walking (heel-to-toe walking). The examination of the spine’s ROM revealed a forward flexion of 10° and an extension of 0°. Lateral flexion was limited to 5° on both the right and left sides. Additionally, the visual analog scale (VAS) score for pain was recorded at 9, indicating a high level of pain and discomfort.
Investigations
(03/08/2023) MRI LS spine suggested lumbar stenosis at L3-L4 and L5-S1 due to diffuse disc bulge with postero-central annular tear. All routine hematological tests were within normal ranges.
Diagnosis
From the above symptoms and findings of investigations, the patient was diagnosed as having lumbar canal stenosis (Katigraha). 13
Treatment Objective
The treatment objective is to eliminate aggravated body humors and reduce the symptoms of lumbar canal stenosis (Katigraha). Treatment given is Shodhana and Shamana Chikitsa mentioned in Tables 2–4.
Shodhana Chikitsa (Purificatory Treatment).
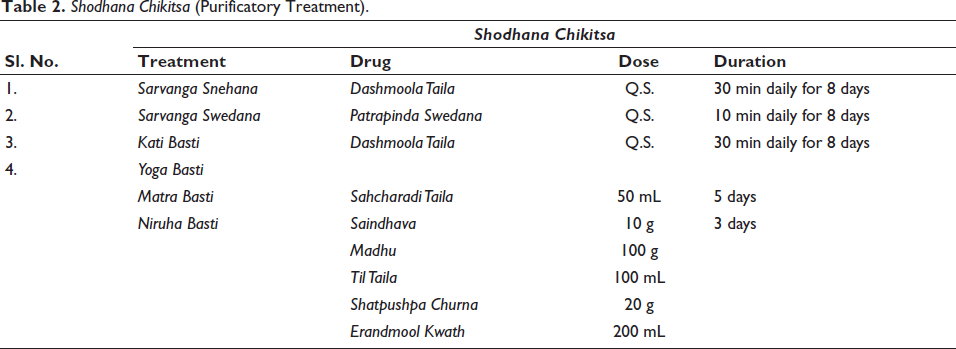
The Yoga Basti schedule consists of eight number of Basti. The first Basti was Matra Basti (oil enema) followed by alternate administration of three Anuvasan Basti and three Niruha Basti (decoction enema), and lastly, one Matra Basti as shown in Table 3. The Basti Pratyagamana Kala for Niruha Basti was 15–20 min.
Showing Basti Chart.

Showing Shamana Chikitsa.
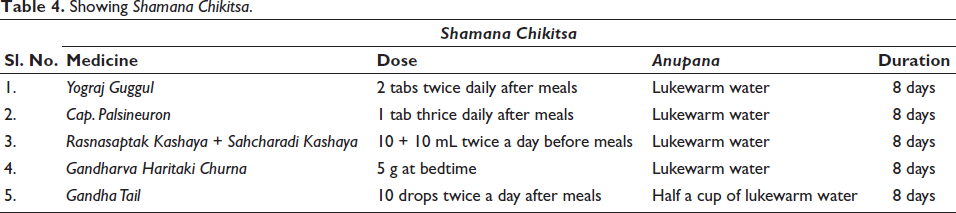

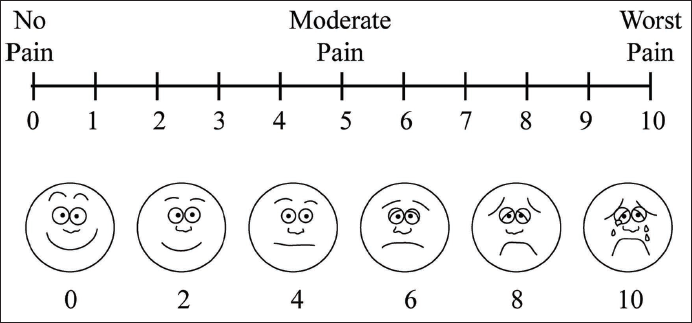
The assessment was done on the following parameters. The pain (VAS) scale 14 which is shown in Figure 3.
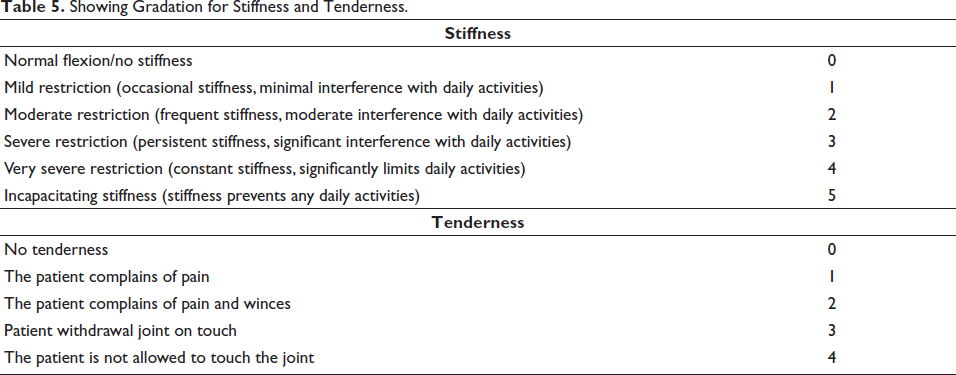
Showing Pain Scale. Stiffness and Tenderness Scale Grading is shown in Table 5.
Showing Gradation for Stiffness and Tenderness.
Results
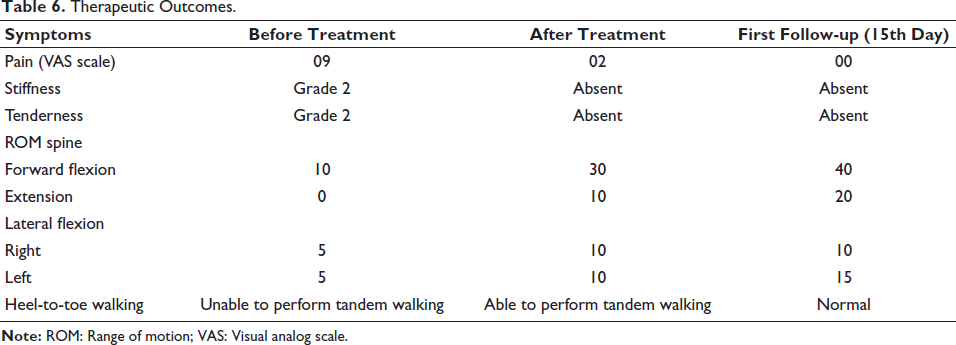
The therapeutic outcome and improvement in the patient’s symptoms before and after treatment are mentioned in Table 6.
Therapeutic Outcomes.
Discussion
Lumbar canal stenosis is where the spinal canal narrows, compressing nerve roots and causing pain, numbness, or weakness in the lower back and legs. 15 Degenerative changes like disc herniation or arthritis often cause it. This constriction can lead to compression of spinal nerves, resulting in symptoms like pain, numbness, and weakness in the lower extremities. It typically affects people over 50 and results in severe pathological alterations to the locomotor system. It is due to genetic variables in younger individuals. 16
Management of lumbar canal stenosis typically involves non-surgical treatments such as physical therapy, medications (like steroidal anti-inflammatory drugs (SAIDs)), and lifestyle modifications. If these measures fail, surgical options like laminotomy or discectomy are considered. 17
Surgical treatments for lumbar stenosis may provide immediate relief, but they carry risks of complications and recurrence rates between 10% and 30%. Despite their effectiveness, the invasive nature raises concerns about recovery time and potential adverse effects. 18 Similarly, pharmacological options like NSAIDs can manage symptoms but often come with side effects, including gastrointestinal issues, dependency, and long-term tolerance. 19 This highlights the need for non-invasive alternatives that address underlying issues without these drawbacks. Ayurvedic approaches, particularly Panchakarma, emphasize detoxification and systemic balance, offering sustainable health benefits without the risks associated with surgery or medication. Combining these Ayurvedic methods with conventional treatments could improve efficacy and patient satisfaction while minimizing recurrence rates.
When vitiated Vata Dosha settles in the Kati Pradesh, it causes “Katigraha,” which results in “Stambha” (stiffness) and Shoola (pain). 20 According to Acharya Sushruta, Shoola cannot develop if Vata is not vitiated. Furthermore, Gada Nigraha makes it very clear that Shoola’s results from Stambha were caused by the migration of Sama and Nirama Vayu into Kati Pradesh (the lumbar region). 21 In this case, trauma and Jara (aging) are the causes of Dhatukshaya. Another pathognomonic component is Atichinta (stress) at the first stages of the illness. The Vata Dosha was vitiated by all the factors and resulted in Kshaya Janya (degenerative) and Sankocha (compression) related symptoms. 22 Untreated lumbar stenosis can result in morbid ailments, incontinence, and paralysis. Vata Vyadhi is treated in Ayurveda via Shodhana (Snehana, Swedana, and Vasti), Shamana (drugs having Madhura-Amla-Lavan-Snigdha qualities), and Nidana Parivarjana (noting etiological factors). 23
Mode of Action of Shodhana Chikitsa
Abhyanga, categorized under external (Snehana) oleation therapy, affects muscles and enhances their strength. The root of Mamsavaha Srotas is Snayu (ligaments), Tvacha (skin), and Raktavahini (blood vessels). Abhyanga is performed on the skin and tendons, and it involves the blood vessels.23, 24 The direct benefit is attained in Mamsavaha Srotas. Abhyanga also softens and relaxes the muscles and tissues, reducing stiffness, alleviating pain, and nourishing the deeper Dhatus. Abhyanga strengthens the muscles, hence stabilizing the joints. 25
The properties of Dashmool Taila (oil) used for Abhyanga are Snigdha (unctuous), Guru (heavy), and Mridu (soft), which are opposite to the qualities of Vata. Abhyanga alleviates the aggravated Vata, which is responsible for the deterioration of Dhatus and the manifestation of symptoms such as pain and stiffness. 26 Dashamoola Tail can slow the onset of degenerative processes, and analgesic and anti-inflammatory properties mitigate inflammation and nerve compression, promoting improved blood circulation. 27 This enhanced circulation helps remove metabolic wastes and nourish spinal tissues. These properties help reduce the clinical symptoms of lumbar stenosis.
Swedana is Sandhichestakar (improvises joint movements), Agni Deepaka, Kapha Vata Nirodhan (the opposite of Kapha), and Sroto Shuddhikar (clears out the microchannels). 28 It lessens stiffness or Stambha. Patra Pinda Swedana is an unmatched remedy for painful illnesses mostly brought on by Vata Dosha, particularly in the case of degenerative disorders. Patra Pinda Swedana is mostly done to relieve pain, inflammation, edema, and rigidity related to bone, joint, or skeletal discomfort. 29
Kati Basti (oil pooling therapy) involves pooling warm Dashmool oil on the lower back to treat lumbar stenosis. The warmth of the oil promotes vasodilation, enhancing blood circulation and nutrient delivery to the affected area. 30 The Dashmool oil, known for its anti-inflammatory and analgesic properties, penetrates deeply into the tissues, reducing inflammation and pain. 31 This therapy helps in softening and relaxing the surrounding muscles and tissues, alleviating nerve compression.
Basti is thought to be the most effective remedy for managing Vata. It is Vata Shamaka, which strengthens tissues, revitalizes the body, and prevents recurrence. The vitiation of Vata is eliminated with the help of Matra Basti. 32 According to Ayurveda, the Virya of the Basti’s ingredients is absorbed, travels to the affected site via circulation, and cures the condition. Sahacharadi Tail is indicated for the treatment of Vata disorders. The constituents of this oil are Sahachara, Devdaru, Nagara, and Til Tail. All drugs possess high potency and serve as pacifiers for Kapha and Vata Doshas. Sahachara, Nagara, and Devdaru possess Vedanasthapak (analgesic) and Shothara (anti-inflammatory) qualities that alleviate pain and inflammation. Matra Basti with this oil alleviates discomfort, stiffness, and pricking sensation, and improves lumbar mobility. 33
Erandmooadi Niruha Basti, an Ayurvedic enema therapy, utilizes a decoction comprising Saindhava (rock salt), Madhu (honey), Til Taila (sesame oil), Shatpushpa Churna (dill seed powder), and Erandmool Kwath (castor root decoction) to treat lumbar stenosis. This combination helps balance Vata Dosha, which lumbar stenosis aggravates. Saindhava and Madhu aid in the elimination of toxins and improve the absorption of medicinal compounds. Til Taila lubricates and nourishes tissues, reducing dryness and stiffness. Shatpushpa Churna provides anti-inflammatory and analgesic effects; when combined with Erandmooladi Basti, it aids in promoting the smooth flow of Vata and helps in reducing nerve-related pain and stiffness, complementing the other components of the Basti, like Eranda, which has strong Vatahara (Vata-alleviating) effects and enhances bowel movement, aiding in detoxification. 34 Erandmuladi Niruha Basti is Deepana (appetizer) and Lekhana (scraping), which helps to calm Kapha and lessen symptoms like stiffness and heaviness. 35 The primary component of Erandmuladi Niruha Basti, Eranda (Ricinus communis Linn.), has anti-inflammatory, antioxidant, analgesic, and bone-regeneration qualities. 36
These ingredients reduce inflammation, alleviate nerve compression, and enhance circulation, thereby mitigating pain and improving mobility in lumbar stenosis patients.
Mode of Action of Shamana Chikitsa
Yograj Guggul helps reduce inflammation and pain in the lower back, improves joint mobility, and supports the detoxification process by aiding in the removal of metabolic wastes. Its regular use can alleviate stiffness and enhance overall spinal health. 37 Cap. Palsineuron is composed of Mahavata Vidhwansak Rasa, which enhances the central nervous system and PNS metabolic functions. It makes neuromuscular communication active. 38 Sameerpannaga Rasa controls blood flow and enhances tissue oxidation in afflicted areas. 39 Ekangveera Rasa aids in the repair of damaged blood vessels and nerves. 40 Sootshekhara Rasa helps injured organelles recover more quickly by providing nutritional support. Lajjalu heals neuro-lesions. Ajamoda is Nidrakaraka, Vatahara, and Shoolahara.
Rasnasaptak Kwatha has a great Vata Shamaka property. In addition to Aampachana, Rasna, Gokshura, and Eranda are all recognized for their analgesic, anti-inflammatory, and anti-arthritic properties. Some of them, such as Guduchi and Aragvadha, are even well-known for their immunomodulatory abilities. 41 Sahcharadi Kashaya is Vatakaphahara, Vedanashamaka, Avaranahara, and acts on Adhakaya. It also supports musculoskeletal health and improves circulation. 42 Together, they work synergistically to alleviate symptoms of lumbar stenosis by reducing inflammation, enhancing mobility, and relieving pain. Gandharva Haritaki Churna helps pacify Vata Dosha and has Vrishya, Agnideepana, Anulomana, and Snigdha Virechaka properties. 43 It also regulates bowel movements, which can reduce the pressure on the lower back. This, in turn, can alleviate discomfort and support spinal health.
Gandha Taila, a formulation referenced by Acharya Sushruta and Vagbhatta, is used primarily to enhance bone strength (Asthidhatu). 44 It possesses properties such as Vatahara, Brahamana, and Asthidhatu Vardhaka, making it effective in treating conditions like osteopenia, osteoporosis, and osteonecrosis. Key ingredients include Sesamum indicum, cow milk, Madhuka, and several herbs and minerals. This formulation acts on Asthidhatu, the bone tissue, and helps counteract Vata Dosha imbalances, which can lead to bone degradation and associated pain. 45 Regular intake of Gandha Taila can strengthen bones and alleviate symptoms related to bone deficiencies.
Conclusion
In Katigaraha’s patient, there was a marked reduction of symptoms like pain and stiffness in the lower back, radiating to both legs and associated with a tingling sensation, numbness, and difficulty walking. No unwanted effect of therapy was observed during the treatment and follow-up period. So, it can be concluded that these herbal medicines and Panchakarma procedures are very effective in the management of Katigaraha, but to establish this effect, further study of longer duration and larger sample is required.
Limitations and Recommendations
A limitation of this case study is its small sample size, which limits the generalizability of the results. Furthermore, the absence of a control group prevents the evaluation of placebo effects. A longer follow-up period would provide important information regarding the long-term efficacy of the Ayurvedic treatments and any possible recurrence of symptoms. It may be beneficial to propose further studies, such as randomized controlled trials (RCTs) involving a larger sample size to validate findings.
Footnotes
Abbreviations
Bd: Bis in Die (twice a day); Cap: Capsule; MRI: Magnetic resonance imaging; OD: Once a day; OPD: Outpatient department; ROM: Range of motion; SLRT: Straight leg raise test; Tab: Tablet; VAS: Visual analog scale.
Acknowledgments
The authors would like to express their heartfelt gratitude to all those who contributed to the contribution of this study. Special thanks to the PG-STAR Team at the Central Council for Research in Ayurvedic Sciences (CCRAS) for their invaluable support, funding, and guidance throughout this study. The authors acknowledge their dedication to promoting evidence-based practices and fostering innovation within the field of Ayurveda. This study would not have been possible without their encouragement and collaboration.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
This case study was conducted on a single patient and hence, ethical committee approval was not done.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research is funded under the project “Scheme for Training in Ayurveda Research for Post Graduate Scholars” (PG-STAR), Central Council for Research in Ayurveda Sciences (CCRAS), Ministry of AYUSH, Government of India under grant number STAR/283/7.
Informed Consent
A written informed consent form was obtained from the patient before starting treatment and for publication in an esteemed journal. The patient was fully informed about the study’s objectives, procedures, potential risks, and benefits. Confidentiality was assured, and participation was voluntary. The patient agreed and signed the consent form, with a copy provided for their records.
