Abstract
Background
Vitiligo is a skin condition characterized by depigmentation and has proven difficult to treat. Traditional Chinese Medicine (TCM) offers potential therapeutic alternatives. Compound Baqian Danshen Liniment (CBDL) is a multicomponent herbal formula used in TCM. This study aimed to investigate its mechanism of action in treating vitiligo using network pharmacology, molecular docking, and animal experiments.
Objectives
The purpose of this study was to explore the interactions between CBDL components and vitiligo-related biological pathways, confirm the binding of active compounds to key protein targets, assess the therapeutic efficacy of CBDL using an animal model, and measure serum levels of inflammatory and oxidative stress markers in treated mice.
Materials and Methods
Network pharmacology was utilized to explore the interactions between CBDL components and vitiligo-related biological pathways. Molecular docking was then employed to confirm the binding of active compounds to key protein targets. To assess the therapeutic efficacy of CBDL, animal experiments involving a vitiligo mouse model were conducted. Finally, enzyme-linked immunosorbent assay (ELISA) was performed to measure serum levels of inflammatory and oxidative stress markers in the treated mice.
Results
CBDL exerted therapeutic effects on vitiligo by modulating key pathways such as immune response regulation [tumor necrosis factor (TNF) and mitogen-activated protein kinase (MAPK) signaling], melanogenesis (tyrosinase activation), and oxidative stress [nuclear factor erythroid 2-related factor 2 (Nrf2) pathway], targeting specific proteins like tyrosinase to promote melanocyte activity and pigmentation. Molecular docking revealed that the active components of CBDL, particularly luteolin, showed strong binding affinity to the core targets, including tyrosinase. CBDL treatment significantly promoted melanocyte proliferation, and luteolin demonstrated potent tyrosinase activation. In animal models, vitiligo-affected skin showed substantial improvement, with white plaques receding and hair follicles regenerating. ELISA results indicated that CBDL reduced inflammatory cytokines [TNF-α and interleukin (IL)-6] and oxidative stress markers [acetylcholinesterase (AChE), malondialdehyde (MDA), and monoamine oxidase A (MAOA)] while enhancing tyrosinase levels in serum.
Conclusion
CBDL exerts therapeutic effects on vitiligo through multitarget interactions and promotes melanocyte activity, likely due to the activation of tyrosinase by its active compounds. These findings suggest that CBDL could be a promising alternative treatment for vitiligo, offering insights into the potential of TCM in managing this condition.
Keywords
Introduction
Vitiligo is a chronic disorder characterized by progressive loss of melanocytes, leading to depigmented patches on the skin. It affects 0.5%–2.0% of the global population, with incidence rates increasing due to societal stress and lifestyle factors (Akl et al., 2024). The condition is primarily driven by autoimmune mechanisms, particularly the interferon (IFN)-γ-mediated attack on melanocytes by CD8+T cells (Frisoli et al., 2020). Vitiligo not only alters physical appearance but also causes psychological distress, including anxiety and decreased quality of life (Bibeau et al., 2023). Western treatments, such as glucocorticoids and immunosuppressants, aim to reduce immune responses and inflammation. However, they often have side effects and high recurrence rates (Böhm et al., 2022). This highlights the need for alternative therapies with more sustainable benefits.
Traditional Chinese medicine (TCM) offers a holistic approach, viewing vitiligo as resulting from internal imbalances and external factors. TCM classifies the condition into stable and progressive stages, addressing qi, liver, and kidney function imbalances. Compound Baqia Danshen Liniment (CBDL), an herbal formulation used in TCM, targets vitiligo’s underlying syndromic patterns. Its ingredients, such as sarsaparilla and Salvia miltiorrhiza, aim to promote blood circulation, detoxify, and support melanocyte proliferation, offering potential advantages over Western treatments by minimizing side effects. To explore CBDL’s therapeutic mechanisms, we applied network pharmacology, integrating bioinformatics and systems biology to identify key protein targets and pathways. This approach, complemented by animal models, aims to bridge traditional and modern pharmacology, enhancing our understanding of CBDL as a potential treatment for vitiligo.
Materials and Methods
Network Pharmacology Analysis
Traditional Chinese Medicine Systems Pharmacology (TCMSP)-based Screening of CBDL Active Ingredients and Target Proteins
The primary components and their corresponding targets in CBDL were screened using the TCMSP platform (
Screening of Vitiligo Targets
Anti-vitiligo targets were identified by searching GeneCards (
Development of Active Ingredient-target Network
Active components and potential action targets were uploaded into Cytoscape 3.8.0 to create a network that illustrates the relationships between the active ingredients and their targets in the context of vitiligo treatment. The network was analyzed for connectivity using the CytoNCA function to identify the top 20 active components (Li, Liu, et al., 2023; Li, Miao, et al., 2023).
Construction of Protein–Protein Interaction (PPI) Networks
PPI networks were constructed using the STRING platform (
Gene Ontology (GO) and Kyoto Encyclopedia of Genes and Genomes (KEGG) Pathway Enrichment Analysis
GO and KEGG pathway enrichment analyses were conducted to uncover CBDL’s therapeutic mechanisms in vitiligo. The GO terms were analyzed for biological processes, molecular functions (MF), and cellular components (CC), focusing on terms with p values <0.05. KEGG analysis highlighted enriched pathways like melanogenesis, nuclear factor-kappa B (NF-κB) signaling, and oxidative phosphorylation, demonstrating CBDL’s multifaceted potential in vitiligo treatment.
Molecular Docking
Molecular docking studies were performed to investigate the binding interactions between CBDL’s active compounds and vitiligo-related protein targets. The active compound luteolin was prepared and docked against tyrosinase (TYR) and other relevant targets using AutoDock Vina. Key binding interactions were visualized using PyMOL. Luteolin showed strong binding affinity with TYR, suggesting its potential to enhance melanocyte activity.
Animal Model Validation
Extraction and Preparation of Medicinal Liquids
The herbal ingredients were weighed and extracted with aqueous ethanol. The extract was filtered, and the filtrates were concentrated. Tacrolimus was used as a positive control drug (Singh et al., 2021).
Animals and Reagents
Seventy male C57BL/6 mice (18–22 g) were acquired from the Animal Experiment Center at Xinjiang Medical University. The mice were housed under controlled conditions (temperature: 23°C ± 2°C, humidity: 45% ± 5%) (Niu & Aisa, 2017).
Establishment of Vitiligo Model Mice and Group Administration of Drugs
Vitiligo was induced in C57BL/6J mice by daily subcutaneous injections of 30% hydrogen peroxide for 7 days. Afterward, the mice were treated with CBDL or tacrolimus. Groups included normal controls, vitiligo model, CBDL low-, medium-, and high-dose groups, and positive control group (PG).
Naked Eye Observation of the Effect of CBDL on Vitiligo Mice
The therapeutic effects of CBDL were evaluated by visual grading of repigmentation and skin condition. The treatment was assessed based on the size and color of white spots, pigmentation, and skin changes over 14 days.
Effect of CBDL on Lesional Skin of Vitiligo Model Mice by Amino–Silver Staining
Skin sections were stained with ammonia silver to assess histopathological changes. Images were analyzed using CaseViewer 2.4 software, and three samples from each group were examined.
Effect of CBDL on the Expression of Tumor Necrosis Factor (TNF)-α, Interleukin (IL)-6, Acetylcholinesterase (AChE), TYR, Malondialdehyde (MDA), and Monoamine Oxidase A (MAOA) in Serum by Enzyme-linked Immunosorbent Assay (ELISA)
Blood samples were collected, and the supernatant was used for ELISA assays to measure TNF-α, IL-6, AChE, TYR, MDA, and MAOA expression levels. Standard curves were used for quantification.
Statistical Analysis
Data were analyzed using GraphPad Prism 8.3.0. A t-test was performed for each group, and statistical significance was established at p < 0.05.
Results
Network Pharmacological Results
Identification of Active Compounds and Associated Targets
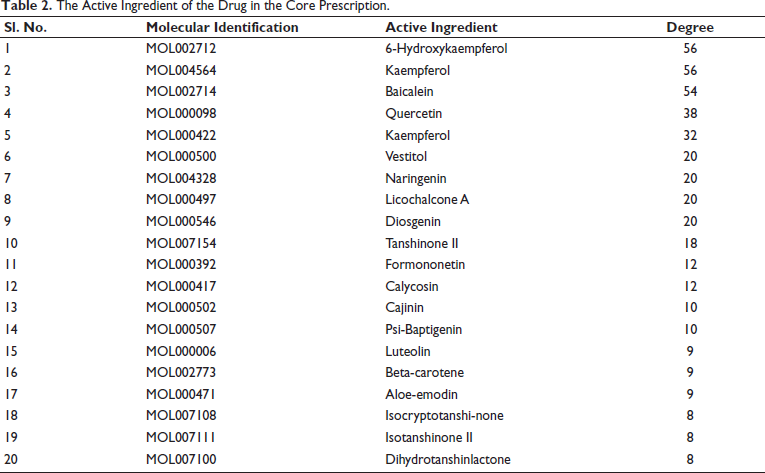
The chemical constituents of the mixed herbs were identified using the TCMSP database. After applying screening and deweighting criteria, 106 key components were selected for further analysis. Using Cytoscape 3.8.0, these components were ranked based on their degree values, and the top 20 active ingredients were identified. These active ingredients are summarized in Table 2. Additionally, relevant target proteins for the herbs were compiled, focusing on targets linked to the Chinese herbal medicines used in the compound prescription. These proteins were converted into gene names via the UniProt database, and duplicate targets were removed, resulting in a total of 352 unique targets (Figure 1).
A Research Model of the Efficacy of Compound Baqia Danshen Liniment (CBDL) in the Treatment of Vitiligo.
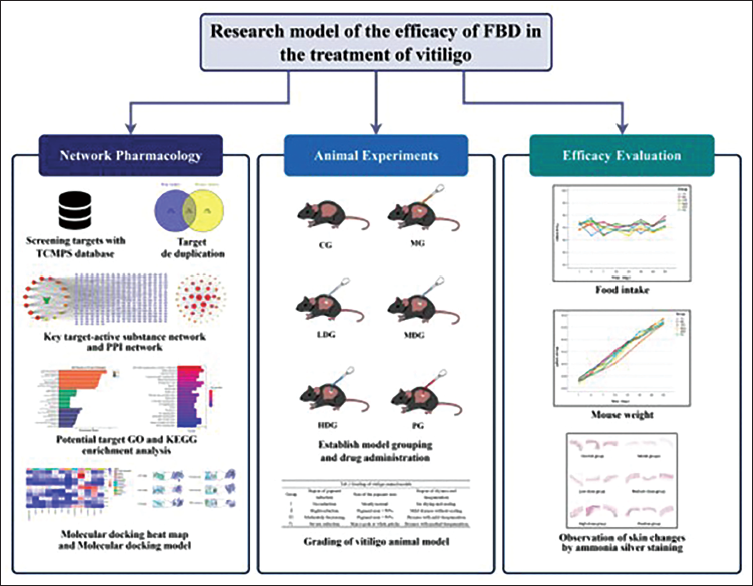
Screening and Confirmation of Vitiligo-related Genes
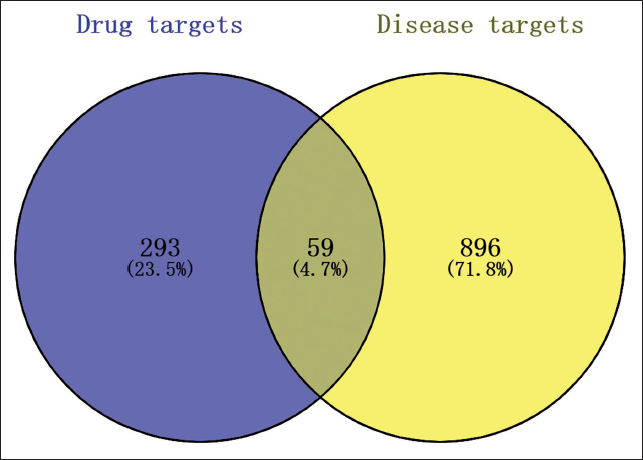
A total of 892 potential vitiligo-related targets were obtained from GeneCards, along with 95 targets from OMIM. By merging and refining these datasets, we identified 955 unique disease-predictive target genes. After intersecting these targets with the targets identified for the compound, 59 vitiligo-related targets were identified. This intersection is illustrated in Figure 2.
Venn Diagram of Main Active Ingredient Targets and Vitiligo in Drug Group.
Active Ingredient-target Network Construction
The active ingredient-target network for treating vitiligo using sarsaparilla S. miltiorrhiza extract was constructed based on 59 vitiligo-related targets and 106 active ingredients. This network comprised 162 nodes representing the active ingredients and their corresponding targets. Topological analysis was performed using CytoNCA within Cytoscape, revealing the top 20 components, as shown in Table 1. The network interactions were visually represented in Figure 3(A), with active compounds highlighted in red and yellow and targets indicated by purple rhombuses.
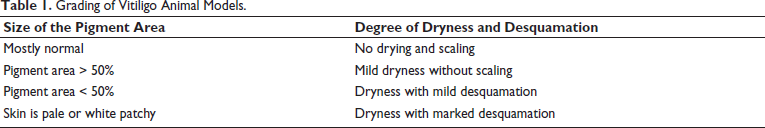
Grading of Vitiligo Animal Models.
The Active Ingredient of the Drug in the Core Prescription.
(A) Key Target-active Substance Network. The Red–Yellow Gradient Color Represents the Active Substance, and the Purple Color Represents the Target; (B) Protein–Protein Interaction Organize Network; (C) Core Targets and Topological Parameters in the Key Core Drug Group; and (D) Potential Target Gene Ontology (GO) and Kyoto Encyclopedia of Genes and Genomes (KEGG) Enrichment Analysis.
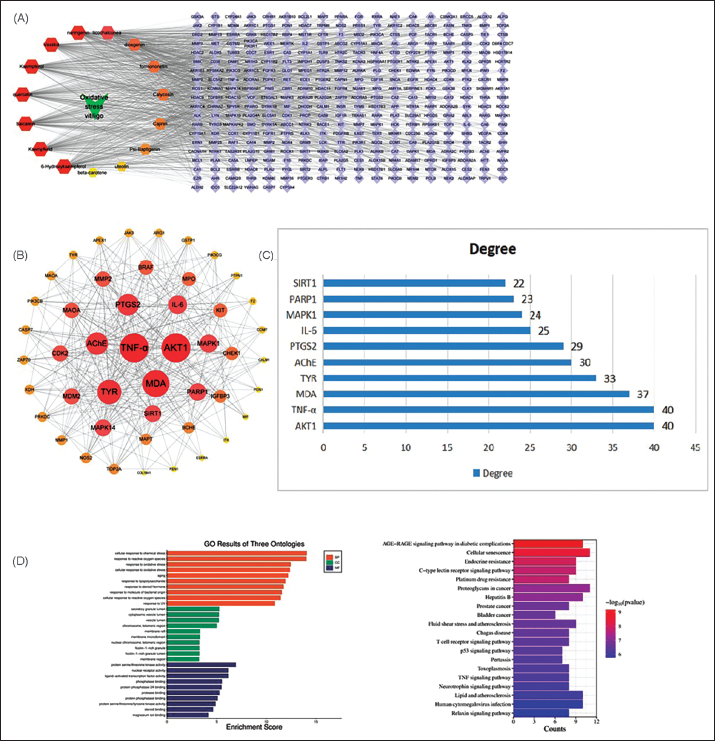
PPI Network
The PPI network for the identified targets was built using data from the STRING platform, resulting in a network of 59 protein nodes and 388 edges. This network was further analyzed using Cytoscape, and topological analysis revealed that 21 active components had significant centrality values (betweenness centrality, closeness centrality, degree, local average connectivity, and network centrality). These components are likely key active ingredients in the compound used to treat vitiligo. Further evaluation of these 21 genes led to identifying 10 core genes, including AKT1, ANF-α, MDA, TYR, AChE, PTGS2, IL6, MAPK1, PARP1, and STAT1. These 10 genes are believed to be crucial in the treatment of vitiligo with CBDL, as shown in Figure 3(B) and (C).
GO and KEGG Enrichment Analysis
The GO analysis for vitiligo treatment with CBDL revealed 3,100 biological process (BP) terms, primarily focusing on oxidative stress responses, reactive oxygen species (ROS) reactions, and cellular responses to chemical stressors. In terms of MF, 309 items were identified, including activities related to protein kinase activity, nuclear receptor functions, ligand-activated transcription factors, and magnesium ion interactions. A total of 166 CC terms were identified, with a focus on the outer membrane, cell sac lumen, chromosomes, and vesicular cytoplasm, as illustrated in Figure 3. Additionally, the KEGG pathway enrichment analysis revealed 157 signaling pathways involved in vitiligo treatment, with the advanced glycation end-products and receptor for advanced glycation end-products (AGE-RAGE) pathway, IL-17 signaling, TNF signaling, and Th-17 cell pathways being particularly relevant, as shown in Figure 3(D).
Molecular Docking
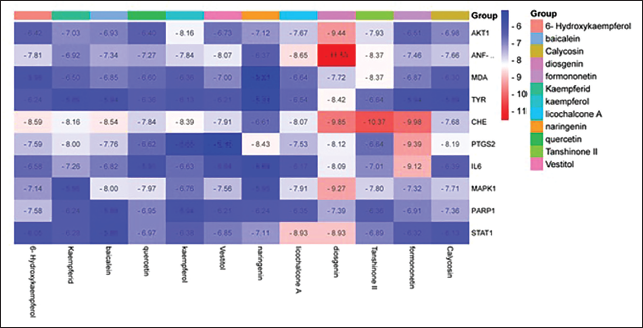
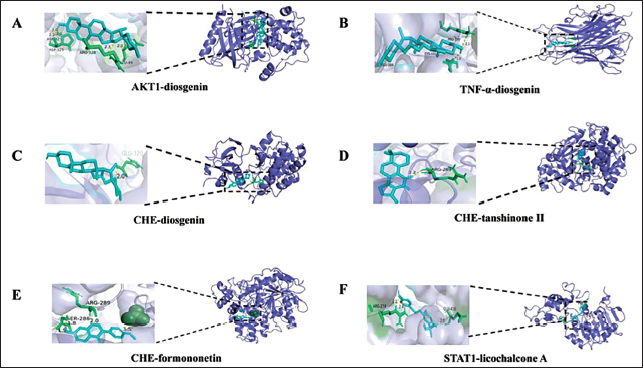
Molecular docking simulations were performed to assess the binding affinity between the core targets (AKT1, ANF-α, MDA, TYR, AChE, PTGS2, IL6, MAPK1, PARP1, and STAT1) and the active components of CBDL. After conducting a topological analysis and evaluating the top 20 KEGG pathways, TYR was identified as a crucial target for vitiligo treatment. The molecular docking results indicated that the binding energies between CBDL’s core components and the vitiligo-related targets were all negative, suggesting stable interactions between the compounds and their receptors. Visual representations of these stable complexes are shown in Figures 4 and 5.
Molecular Docking Heat Map.
Molecular Docking Model of Pharmacodynamic Component and Target.
Animal Experiment Results
Body Weight and Food Intake
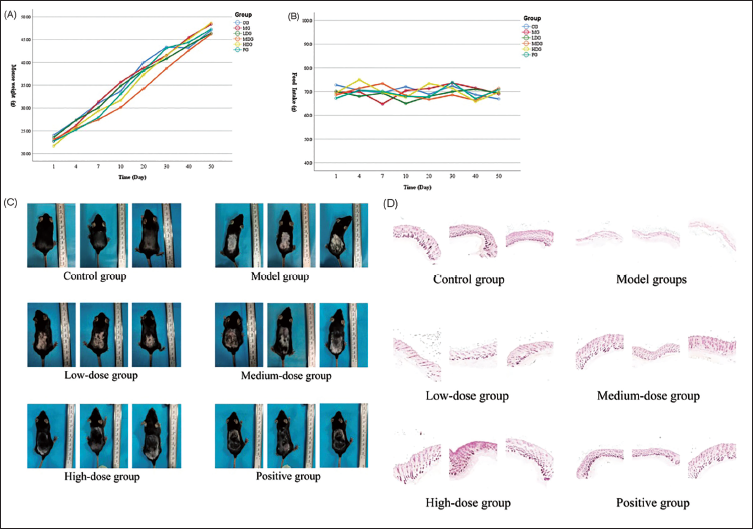
The mice’s body weights were monitored throughout the experiment, showing no significant differences in the initial weights among the six groups at week 0. However, starting from week 2, the body weights of the control group (CG) were slightly higher than those of the experimental groups (p < 0.05). After 4 weeks of treatment, 32 out of 60 mice exhibited higher average weights than the normal group, with no significant differences observed between the experimental groups, as depicted in Figure 6A. Food intake was also monitored, and there were no significant differences between the experimental and normal groups at weeks 2, 4, 6, and 8, as shown in Figure 6B. Overall, the experimental mice showed normal fluctuations in body weight and food consumption during the study period.
(A) Changes in Weight in Experimental Mice, (B) Changes in Food Intake in Experimental Mice, (C) Therapeutic Effect of Compound Baqia Danshen Liniment (CBDL) on Mice With Vitiligo, and (D) Ammonia Silver Staining Results.
Visual Assessment of CBDL’s Effect on Vitiligo Mice
To evaluate the therapeutic effect of CBDL on vitiligo, mice were modeled to develop vitiligo and then treated with low, medium, and high doses of CBDL, as well as tacrolimus (positive control). After 14 days of treatment, significant improvements were observed in the skin of the vitiligo model mice. The white patches on the back skin gradually decreased in size, and the changes in skin pigmentation were recorded. The extent of discoloration was graded (Table 3), and the results demonstrated a marked improvement in the affected areas as the dose of CBDL increased. The therapeutic effects were visually captured in photographs and are shown in Table 4 and Figure 6(C).
Grading Evaluation of Vitiligo Animal Modeling Performance Indicators.
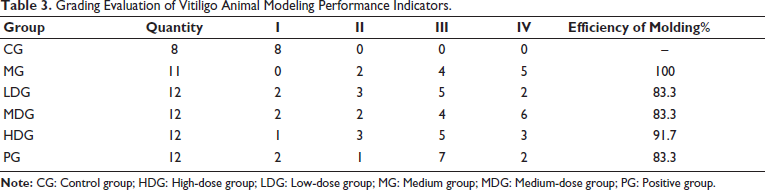
Grading Evaluation of Performance Indicators in the Treatment of Vitiligo Animals.
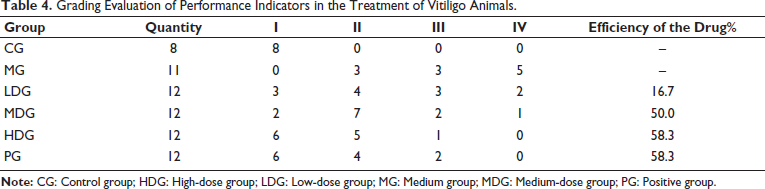
Ammonia Silver Staining Results
Silver staining was used to assess histological changes in the skin. In the normal group, the epidermis showed no hyperplasia, and the dermis contained abundant melanin granules. In contrast, the vitiligo model group exhibited a marked reduction in melanin granules and hyperplasia of the epidermis. In the CBDL-treated groups (low, medium, and high doses) and the PG, a significant increase in melanin granules and hair follicles was observed compared to the vitiligo model group, as illustrated in Figure 7.
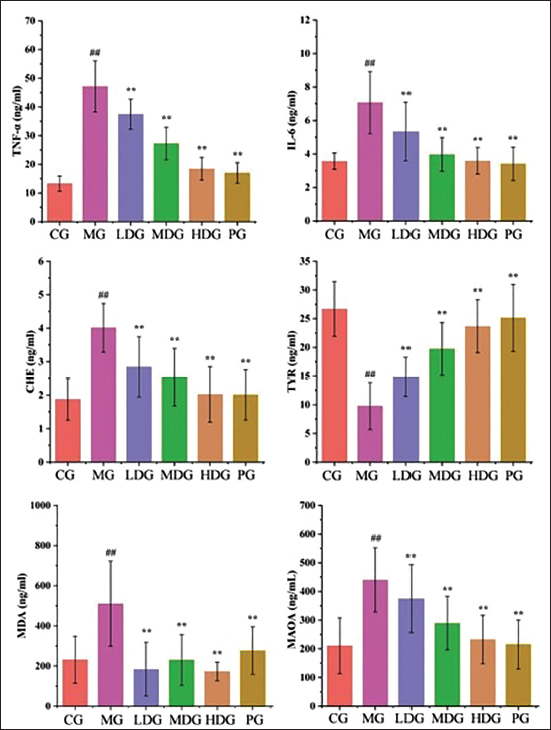
The Contents of Tumor Necrosis Factor (TNF)-α, Interleukin (IL)-6, Acetylcholinesterase (AChE), Tyrosinase (TYR), Malondialdehyde (MDA), and Monoamine Oxidase A (MAOA) in the Peripheral Blood of Mice Were Determined by Enzyme-linked Immunosorbent Assay (ELISA). Compared to the Normal Group, ##p < 0.01; Compared to the Model Group, **p < 0.01.
Melanocyte Proliferation and TYR Activation
Histological analysis was performed on skin biopsies from the treated mice to assess melanocyte proliferation. Ki-67 staining, a marker for cell proliferation, revealed an increase in proliferating melanocytes in the treated groups compared to the vitiligo model group. TYR activation, essential for melanogenesis, was evaluated by measuring serum TYR levels using an ELISA. Increased TYR activity in the CBDL-treated groups suggests enhanced melanin production. Moreover, quantitative reverse transcription polymerase chain reaction (qRT-PCR) analysis of TYR messenger ribonucleic acid (mRNA) expression confirmed that CBDL treatment upregulated TYR gene expression in skin tissue.
Effects on Inflammatory and Oxidative Stress Markers
Inflammatory markers TNF-α and IL-6 were assessed in the blood of the treated mice. Significant reductions in TNF-α and IL-6 levels were observed in the low-, medium-, and high-CBDL-dose groups compared to the vitiligo model group, indicating that CBDL alleviates inflammation. Additionally, AChE levels were significantly reduced, while TYR levels were elevated in the treated groups, especially with increasing doses of CBDL (p < 0.01). The levels of oxidative stress markers, including MDA and MAOA, were also significantly reduced in the CBDL-treated groups (p < 0.01). These results suggest that CBDL has a potent effect in reducing oxidative stress, which is crucial in the treatment of vitiligo. Notably, the vitiligo model group showed minimal self-repair capacity at the end of the treatment period (p > 0.05), highlighting the therapeutic potential of CBDL in vitiligo treatment.
Discussion
This study explores the therapeutic potential of CBDL in treating vitiligo, using network pharmacology, molecular docking, and animal experiments to identify its active components, molecular targets, and pharmacological mechanisms. Quercetin, kaempferol, and baicalein emerged as key bioactive compounds, acting on pathways such as TNF, mitogen-activated protein kinase (MAPK) signaling, and melanogenesis. Findings suggest that CBDL reduces inflammation, promotes melanogenesis, and alleviates oxidative stress. The integration of network pharmacology and in vivo experiments underscores CBDL’s multitarget approach, but further clinical validation is necessary to confirm its efficacy and safety.
Vitiligo is a complex depigmenting disorder with significant impacts on patients’ quality of life. Its pathogenesis involves multiple factors, including autoimmune responses, oxidative stress, and genetic predisposition. Current treatment options, like corticosteroids, phototherapy, and surgical interventions, have limited success and notable side effects, necessitating the exploration of safer and cost-effective alternatives. TCM offers promising approaches, with CBDL demonstrating therapeutic potential, though its mechanisms remain underexplored. This study utilized network pharmacology, supported by animal experiments, to elucidate CBDL’s pharmacological basis.
Network pharmacology identified 106 bioactive components in CBDL, targeting 59 proteins linked to vitiligo. Key targets include TNF-α, IL-6, TYR, and AChE, which are critical in regulating inflammatory responses, melanogenesis, and oxidative stress. TNF-α and IL-6 are central to the inflammatory cascade and contribute to melanocyte destruction in vitiligo. CBDL significantly reduced these inflammatory cytokines in animal models, mitigating inflammation and protecting melanocytes.
Oxidative stress is a pivotal factor in vitiligo pathogenesis, with increased ROS leading to melanocyte apoptosis. CBDL’s active compounds—quercetin, kaempferol, and baicalein—exhibited strong anti-oxidant properties, reducing ROS and markers like MDA while enhancing anti-oxidant enzyme activity. These effects help preserve melanocyte integrity, a critical factor for repigmentation.
Quercetin demonstrated remarkable protective effects by reducing melanocyte apoptosis, enhancing cell viability, and improving TYR activity. Kaempferol and baicalein further contributed to anti-oxidant defenses, reducing UV-induced oxidative damage and modulating inflammation. Collectively, these compounds target TYR, a key enzyme in melanin synthesis, promoting pigmentation and potentially reversing depigmentation.
Molecular docking results corroborated these findings, showing strong interactions between active compounds and key targets like TYR, TNF-α, and IL-6. These interactions suggest that CBDL enhances melanogenesis while simultaneously suppressing autoimmune responses. Pathway enrichment analysis revealed that AGE-RAGE signaling, MAPK signaling, and melanogenesis are critical pathways modulated by CBDL.
Animal experiments supported the network pharmacology results. CBDL-treated mice displayed increased TYR activity, improved melanin synthesis, and reduced epidermal hyperplasia. Oxidative stress markers, such as MDA, were significantly reduced, while anti-oxidant capacity was enhanced, demonstrating CBDL’s protective role against melanocyte damage. These outcomes highlight CBDL’s potential to address multiple aspects of vitiligo pathogenesis, aligning with its multitarget therapeutic approach.
The study also underscores CBDL’s potential advantages over existing treatments. Unlike corticosteroids or phototherapy, which often target isolated aspects of vitiligo, CBDL acts on multiple pathways, addressing both inflammatory and oxidative stress components. Its bioactive compounds provide a synergistic effect, enhancing therapeutic outcomes while minimizing side effects.
Despite its promising results, this study has limitations. First, network pharmacology predictions require further validation through clinical studies. Second, while animal experiments provide preliminary evidence of efficacy, human trials are essential to confirm safety and therapeutic benefits. Additionally, the complexity of CBDL’s multicomponent formulation poses challenges for standardization and quality control. Future research should optimize formulations, explore dose–response relationships, and validate findings in diverse patient populations.
In conclusion, CBDL demonstrates significant potential as a therapeutic agent for vitiligo. By targeting inflammation, oxidative stress, and melanogenesis, it offers a comprehensive approach rooted in TCM. The integration of network pharmacology and experimental validation highlights the importance of multitarget strategies in addressing complex disorders like vitiligo. Future clinical studies will be crucial in translating these findings into practical applications, paving the way for CBDL’s inclusion in modern therapeutic regimens.
Footnotes
Abbreviations
AChE: Acetylcholinesterase; AGE-RAGE: Advanced glycation end-products and receptor for advanced glycation end-products; CBDL: Compound Baqia Danshen liniment; CHE: Cholinesterase; COX-2: Cyclooxygenase-2; IL-6: Interleukin-6; MAOA: Monoamine oxidase A; MAPK: Mitogen-activated protein kinase; MDA: Malondialdehyde; Nrf2: Nuclear factor erythroid 2-related factor 2; PPI: Protein–protein interaction; ROS: Reactive oxygen species; TNF: Tumor necrosis factor; TYR: Tyrosinase.
Acknowledgments
None.
Author Contribution
Conceptualization, J.W., and J.L.; methodology, J.W.; software, K.A.; writing—original draft preparation, J.W.; writing—review and editing, W.S.; visualization, M.A.; supervision, M.A.; All authors have read and agreed to the published version of the manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval and Informed Consent
The animal study protocol was approved by the Experimental Animal Ethics Committee of Xinjiang Medical University (protocol code IACUC-JT-20230831-06).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by Major Science and Technology projects of Xinjiang Uygur Autonomous Region, grant number 2022A03005.
