Abstract
Background
In recent years, traditional Chinese medicine has shown advantages in treating ischemic cerebrovascular diseases, including multi-component, multi-target, and low toxicity effects.
Objectives
The aim of this study was to clarify the impact of ginkgo diterpene lactone meglumine injection (GDLMI) on promoting microvascular neovascularization and improving cerebral perfusion after cerebral infarction (CIF) in rats and to explore its underlying mechanisms in promoting angiogenesis.
Materials and Methods
Seventy-five rats were randomly rolled into Sham (sham surgery) group, Model (acute CIF model) group, low-dose (LD) (1 g/kg bw GDLMI) group, medium-dose (MD) (3 g/kg bw GDLMI) group, and high-dose (HD) (5 g/kg bw GDLMI) group. The neurological function of rats was evaluated using the Longa method. Micro-PET was performed to evaluate brain metabolism status at 7 days post-reperfusion. Serum expression levels (ELs) of interleukin (IL)-1β, IL-6, and tumor necrosis factor (TNF)-α were measured. Brain tissue samples were collected to assess cerebral infarct volume and to measure oxidative stress (OS) markers, including superoxide dismutase (SOD), catalase (CAT), and malondialdehyde (MDA). TdT-mediated dUTP nick end labeling (TUNEL) was performed to detect the apoptosis rate of cortical neurons. Western blotting was conducted to determine brain tissue’s ELs of vascular endothelial growth factor (VEGF), angiopoietins-1 (Ang-1), p-PI3K, and p-AKT proteins.
Results
Rats in Model group exhibited higher Longa scores and increased cerebral infarct volume, decreased brain 18F-FDG content, elevated serum ELs of IL-1β, IL-6, and TNF-α, reduced SOD and CAT activities, increased MDA content in brain tissue, elevated apoptosis rate of cortical neurons, and elevated protein ELs of VEGF and Ang-1 in brain tissue, accompanied by decreased ELs of p-PI3K and p-AKT proteins compared to the Sham group (p < 0.05). Rats in the LD, MD, and HD groups showed decreased Longa scores and cerebral infarct volume, increased brain 18F-FDG content, decreased ELs of IL-1β, IL-6, and TNF-α, increased SOD and CAT activities, decreased MDA content in brain tissue, decreased apoptosis rate of cortical neurons, and increased protein ELs of VEGF, Ang-1, p-PI3K, and p-AKT in brain tissue versus Model group (p < 0.05). The effects on all indicators in rats showed a dose-dependent trend.
Conclusion
GDLMI has a protective effect against acute CIF/reperfusion injury (RI), which may be attributed to its ability to suppress inflammation and OS damage by activating PI3K/AKT signaling.
Introduction
Ischemic cerebrovascular disease is characterized by a high incidence, disability, and mortality rate. Timely and effective restoration of blood flow in the ischemic area is the primary therapeutic principle for this disease (Gao et al., 2020). However, reperfusion of cerebral tissue in the ischemic area can lead to tissue damage and functional impairments to some extent, triggering cerebral ischemia (CI)/reperfusion injury (RI) (Han et al., 2015). The pathogenesis of CI/RI is highly complex and is believed to involve various factors such as inflammation, oxidative stress (OS) response, and endothelial cell damage (Yilmaz et al., 2023). Moreover, CI/RI constitutes a major pathological process in various ischemic cerebrovascular diseases, underscoring the importance of identifying effective treatment methods or measures.
In recent years, Traditional Chinese Medicine has shown advantages in treating ischemic cerebrovascular diseases, including multi-component, multi-target, and low toxicity effects. Moreover, Chinese herbal medicine with blood-activating and collateral-circulating effects may potentially induce endogenous angiogenic factor expression, thereby promoting endothelial cell proliferation and migration, accelerating post-ischemic angiogenesis, and effectively improving cerebral perfusion (Liu et al., 2022). Ginkgo biloba, belonging to the family Ginkgoaceae, contains active ingredients such as flavonoid glycosides, terpene lactones, and polyisoprenoids. Ginkgolides, important active components found in ginkgo leaves, exhibit various biological activities including neuroprotective and anti-aging effects (Zhao, Guo, et al., 2022; Zhao, Lu, et al., 2022; Zhao, Wang, et al., 2022). Additionally, ginkgolides can enhance blood circulation, dilate blood vessels, and improve local blood circulation (Gachowska et al., 2021). Ginkgo diterpene lactone meglumine injection (GDLMI), composed of ginkgolide A, ginkgolide B, and ginkgolide K, possesses blood-activating and collateral-circulating effects and is clinically used in the treatment of cerebral infarction (CIF). Chen et al. (2023) found that GDLMI treatment significantly improved anti-platelet function in patients with acute ischemic stroke, leading to favorable outcomes at day 90. Liu et al. (2019) prepared a hypoxia/reoxygenation SH-SY5Y cell model and found that GDLMI treatment inhibited cell apoptosis and increased mitochondrial membrane potential. These findings suggest that GDLMI has potential preventive and therapeutic effects on cerebrovascular diseases, although its specific mechanisms require further investigation.
Phosphoinositide 3-kinase (PI3K) is a critical cell signaling protein that possesses serine/threonine kinase and phosphatidylinositol kinase activities. The primary function of PI3K is to catalyze the phosphorylation of phosphatidylinositol diphosphate (PIP2) to generate phosphatidylinositol triphosphate (PIP3), thereby activating a cascade of protein kinases, including Akt, which initiates intracellular signaling pathways (Deng & Zhou, 2023). This signaling pathway plays a crucial regulatory role in various cellular processes, including survival, proliferation, metabolism, and motility. Numerous studies have established that the PI3K/Akt pathway is significantly involved in the pathogenesis of CIF, influencing the pathological process through modulation of inflammatory responses, OS, inhibition of apoptosis, and promotion of angiogenesis (Abe et al., 2010; Cui et al., 2024; Zhao et al., 2023). However, the potential of GDLMI to mediate the PI3K/AKT signaling pathway for therapeutic effects in CIF remains to be further investigated. To understand the protective effects of GDLMI on acute CI/RI, this study used a rat model of acute CI/RI and preliminarily explored the protective effects of GDLMI on CI-RI in animal models. The research aims to provide experimental evidence for the further promotion and application of GDLMI.
Materials and Methods
Experimental Animals
This experiment used 45 male Sprague–Dawley rats with a weight range of 250–300 g (Chengdu Dashuo Laboratory Animal Co. Ltd., China), kept in a specific pathogen-free barrier environment. Animals were housed on a 12-h light/dark cycle at 23 ± 1°C, with a humidity of 45–60%. They were provided with standard rodent chow and water ad libitum, fasting overnight before surgery but with unrestricted access to water.
Animal Model Construction and Grouping
Seventy-five rats were randomly and evenly assigned to five groups: Sham surgery group, Model group, low-dose (LD) group, medium-dose (MD) group, and high-dose (HD) group, using a random allocation method. The allocation sequence was generated by a computer-generated random number list to ensure an even distribution of rats across all groups.
Sham Group
The surgical procedure was the same as for the Model group but without middle cerebral artery occlusion (MCAO) treatment.
Model Group
Rats fasted for 12 h before MCAO surgery. They were anesthetized by intraperitoneal injection of 1% pentobarbital sodium (PS, Sigma–Aldrich, USA) at 30 mg/kg bw, then fixed on the operating table in a supine position. The surgical area on the neck was shaved and disinfected with iodine, and a midline incision was made. The right common carotid artery (CA), external CA, and internal CA were bluntly separated to expose the middle CA, which was then occluded using a nylon suture with a diameter of 0.24 mm and a length of 60 mm. Two hours after MCAO, the nylon suture was removed, followed by reperfusion for 24 h. The reperfusion duration was consistent across all groups.
LD Group
Rats received tail vein injections of 1 g/kg bw GDLMI (Jiangsu Kangyuan Pharmaceutical Co., Ltd., China) 2 days before MCAO and after reperfusion. The MCAO surgery procedure was the same as that for the model group.
MD Group
Rats received 3 g/kg bw GDLMI tail vein injections. The MCAO surgery procedure was the same as that for the model group.
HD Group
Rats received 5 g/kg bw GDLMI tail vein injections. The MCAO surgery procedure was the same as that for the model group.
After surgery, rats in all groups were transferred to a warm environment, individually housed, and closely monitored until they regained consciousness. An independent assessment team was established during the experiment. The members of this team were blinded to the group allocation and treatment protocols of the rats, ensuring unbiased evaluation and assessment of the outcomes across the different groups.
Neurological Function Score
According to the Longa scoring criteria (Gao et al., 2022), assessments were made at 1-, 3-, 5-, and 7-days post-reperfusion. A score of 0 indicated normal limb activity in rats without any symptoms of neurological deficits; 1 indicated flexion of the left forelimb without extension; 2 indicated spontaneous leaning to the left; 3 indicated unstable gait with the entire body leaning to the left; 4 indicated impaired consciousness or inability to walk voluntarily; 5 indicated the death of the rat. Rats with breathing difficulties, unstable vital signs, or intracranial hemorrhage at the time of euthanasia were excluded from the study.
Micro-PET Scanning Evaluation of Brain Metabolism
Seven days after reperfusion, rats were anesthetized by 30 mg/kg bw 1% PS. After anesthesia, rats were immobilized on the examination bed. First, a tail vein injection channel was established, and 0.5 mCi of 18F-FDG aqueous solution (Yantai Dongcheng Pharmaceutical Group Co., Ltd., China) was intravenously administered. One-hour post-injection, static Micro-PET (Shenzhen Zhanye Dahong Technology Co. Ltd., China) scanning was conducted for a duration of 10 min. Following scanning, data reconstruction was performed using ordered subset expectation maximization (OSEM) 3D methodology, and regions of interest (ROI) were delineated to evaluate the uptake of 18F-FDG in the target area. Radioactive substance uptake values (% ID/g) were calculated according to the equation.
2,3,5-Triphenyltetrazolium Chloride (TTC) Staining for Assessing CIF Volume
Seven days after reperfusion, rats were anesthetized by 30 mg/kg bw 1% PS. After anesthesia, rats were euthanized by decapitation, and brain tissues were collected. The olfactory bulbs, cerebellum, and brainstem were removed from the brain tissue, and the remaining tissues were frozen at −20°C for 10 min. Using a TTC staining kit (Shanghai LMAI Biotechnology Co., Ltd., China), coronal sections were prepared, and 2 mm-thick slices were made. The brain slices were incubated in 1% TTC staining solution at 37°C for 20 min, with flipping every 2−3 min. After normal tissues turned red and ischemic tissues turned white, the brain slices were transferred to 10% formaldehyde solution and fixed for 1 h. Images were captured, and the infarct area was detected employing Image-Pro Plus 5.0 to calculate the volume ratio of CIF.
Determination of Serum Inflammatory Cytokine Content
Seven days after reperfusion, blood samples were collected via the abdominal aorta and centrifuged at 3,000 rpm for 10 min to collect supernatant. Expression levels (ELs) of interleukin (IL)-1β, IL-6, and tumor necrosis factor (TNF)-α in serum were determined via enzyme-linked immunosorbent assay (ELISA) kit (Shanghai Beyotime Biotechnology Co. Ltd., China). After color development with the stop solution, the absorbance was measured at 450 nm employing a Varioskan LUX multifunctional microplate reader (Thermo Fisher Scientific, China). Standard curves were plotted based on standard samples, and sample concentrations were calculated accordingly.
Determination of Biochemical Indicators in Brain Tissue
Seven days after reperfusion, rats were anesthetized by 30 mg/kg bw 1% PS. After anesthesia, rats were euthanized by decapitation, and brain tissue was collected. The weight of the brain tissue was measured, and then the tissues were homogenized in 1% tissue homogenate prepared with precooled physiological saline. The homogenate was centrifuged at 3,000 rpm for 10 min to collect the supernatant. Activities of superoxide dismutase (SOD), catalase (CAT), and malondialdehyde (MDA) content in brain tissue were determined regarding instructions of the ELISA kit (Shanghai Beyotime Biotechnology Co., Ltd., China). After color development with the stop solution, absorbance was measured. Standard curves were plotted based on standard samples, and sample concentrations were calculated accordingly.
TdT-mediated dUTP Nick End Labeling (TUNEL) Assay for Apoptosis Detection of Cortical Neurons in the Brain
The cerebral cortex was separated from the brain tissue and fixed in a 10% formaldehyde solution, followed by preparation of paraffin sections. After deparaffinization and dehydration of the paraffin sections, tissues were immersed in 0.1% sodium citrate solution with 0.1% Triton X-100 for 20 min via TUNEL assay kit (Sigma–Aldrich, USA). After rinsing with phosphate-buffered saline, the tissues were incubated with TUNEL staining solution at 37°C for 1.5 h. Subsequently, the tissues were incubated with peroxidase at 37°C for 30 min. After rinsing, tissues were incubated with diaminobenzidine for 5 min for color development. Following counterstaining with hematoxylin, dehydration was performed, and the sections were mounted with neutral gum for observation under a CX43 microscope (Olympus, Japan). Cells stained brown or brownish were considered apoptotic. Five random fields were selected, and the number of apoptotic cells was counted.
Western Blotting
Radioimmunoprecipitation assay (RIPA) lysis buffer was added to the brain tissue to homogenize the sample, followed by total protein extraction from the tissue. The bicinchoninic acid assay kit determined protein concentration. Thirty micrograms of protein were loaded and separated by sodium dodecyl sulfate-polyacrylamide gel electrophoresis, then transferred to polyvinylidene fluoride membranes using a semi-dry transfer methodology. Membranes were blocked with 5% skim milk powder at 25°C for 1 h, then incubated overnight at 4°C with primary anti-bodies diluted at a ratio of 1:2,000, including vascular endothelial growth factor (VEGF), angiopoietins-1 (Ang-1), phosphatidylinositol 3-kinase (PI3K), p-PI3K, serine/threonine protein kinase B (Akt), p-Akt, and β-actin anti-bodies (Abcam, UK). After rinsing, membranes were incubated with secondary anti-bodies labeled with horseradish peroxidase diluted at a ratio of 1:5,000 (Abcam, UK) at 25°C for 1 h. Enhanced Chemiluminescence detection reagents were added, and images were captured using a BioDoc-It 220 Gel Imaging System (UVP, USA). The relative grayscale values of the target protein bands were analyzed using LABWORK with β-actin as a control.
Statistical Methods
All data were presented as mean ± standard deviation and were analyzed employing SPSS 19.0. For comparisons between two groups, normally distributed data were analyzed via t-test, while non-normally distributed data were analyzed via non-parametric tests. One-way analysis of variance (ANOVA) was employed for multiple-group comparison, and statistical significance was set at p < 0.05.
Results
Effect of GDLMI on Neurological Function in Rats with CIF/Reperfusion
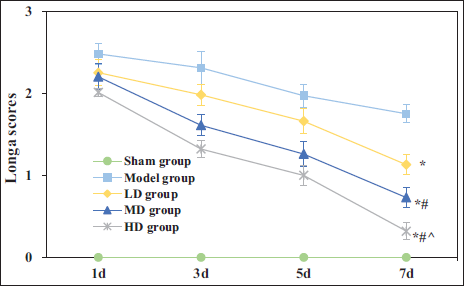
The results of Longa scoring for evaluating neurological function in each group of rats are depicted in Figure 1. No neurological deficits were observed in the Sham group. At 1 day after reperfusion, there existed negligible differences between the LD, MD, HD, and Model groups (p > 0.05). Nevertheless, from 3 to 7 days after reperfusion, the Longa scores in the LD, MD, and HD groups were markedly inferior to the Model group (p < 0.05). As the dose of GDLMI increased, the Longa scores in rats decreased, with notable differences observed (p < 0.05).
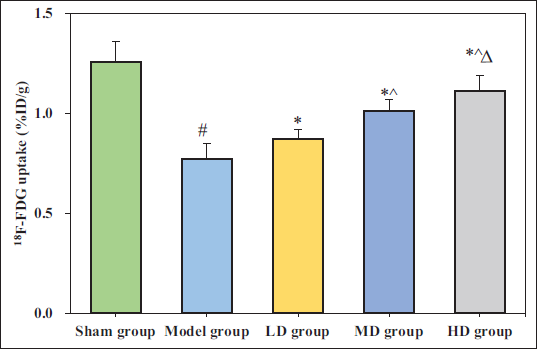
Effect of GDLMI on Brain Metabolism in Rats with CIF/Reperfusion
The results of the Micro-PET assessment of cerebral metabolism in each group of rats are presented in Figure 2. The content of 18F-FDG in brain tissues of the Model group was significantly decreased compared to the Sham group (mean difference = 0.490, 95% CI: 0.308–0.572, p < 0.05). 18F-FDG in brain tissues of LD group (mean difference = 0.400, 95% CI: 0.250–0.550), MD group (mean difference = 0.290, 95% CI: 0.140–0.440), and HD group (mean difference = 0.307, 95% CI: 0.133–0.447) were significantly increased compared to Model group (p < 0.05). As the dose of GDLMI increased, the content of 18F-FDG in rat brain tissues also increased, with considerable differences observed (p < 0.05).
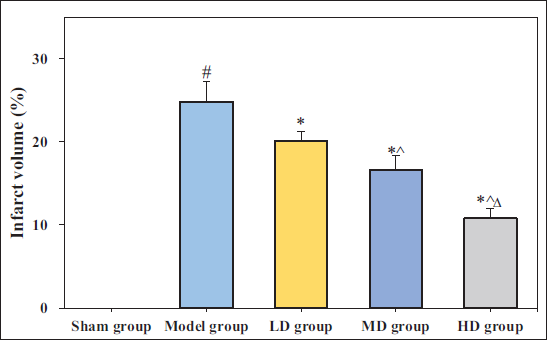
Influence of GDLMI on CIF Area in Rats with CIF/Reperfusion
The evaluation of cerebral infarct volume in each group of rats using TTC staining is presented in Figure 3. The cerebral infarct volume in Model group was greatly larger than the Sham group (mean difference = 24.70, 95% CI: 23.43–25.97, p < 0.05), and that in the LD group (mean difference = 4.80, 95% CI: 3.18–6.42), MD group (mean difference = 5.84, 95% CI: 4.42–6.54) and HD group (mean difference = 10.05, 95% CI: 8.51–12.07) were notably smaller than Model group (p < 0.05). As the dose of GDLMI increased, the cerebral infarct volume in rats decreased drastically (p < 0.05).
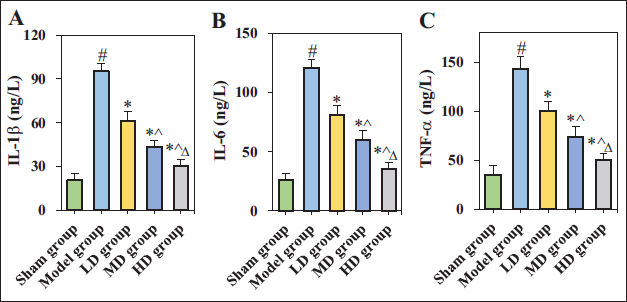
Effect of GDLMI on Inflammatory Response in Rats with CIF/Reperfusion
In Figure 4, IL-1β, IL-6, and TNF-α in the Model group were substantially increased compared to the Sham group (p < 0.05), and those in LD, MD, and HD groups were significantly decreased compared to the Model group (p < 0.05). As the dose of GDLMI increased, IL-1β, IL-6, and TNF-α in rats significantly decreased (p < 0.05).
Influence of GDLMI on OS Response in Rats with CIF/Reperfusion
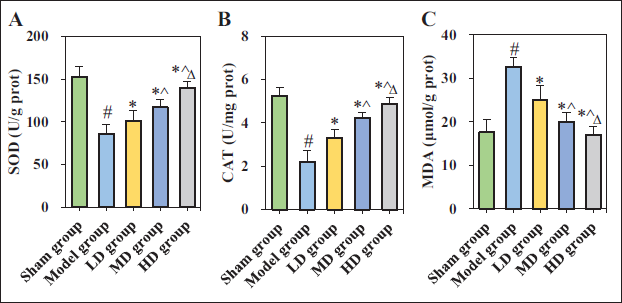
In Figure 5, SOD and CAT activities in the brain tissues of the Model group were significantly lower versus the Sham group, while the MDA content was significantly higher versus the Sham group (p < 0.05). Activities of SOD and CAT in the brain tissues of LD, MD, and HD groups were significantly increased compared to the Model group, while the MDA content was significantly decreased compared to the Model group (p < 0.05). As the dose of GDLMI increased, SOD and CAT activities in the brain tissues of rats increased, while the MDA content decreased, with marked differences observed (p < 0.05).
Effect of GDLMI on Apoptosis of Cortical Neurons in Rats with CIF/Reperfusion
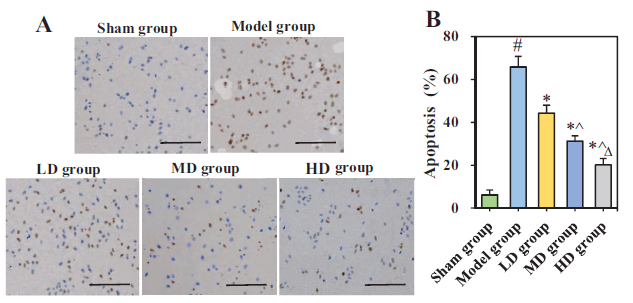
The results of the TUNEL assay for detecting neuronal apoptosis in the cerebral cortex of each group of rats are presented in Figure 6. The apoptotic rate of neurons of the Model group was notably higher versus the Sham group (mean difference = 59.70, 95% CI: 56.89–62.507, p < 0.05). The apoptotic rate of neurons in the cerebral cortex of the LD group (mean difference = 59.70, 95% CI: 56.89–62.507), MD group (mean difference = 34.90, 95% CI: 33.11–36.69), and HD group (mean difference = 45.90, 95% CI: 44.32–47.48) was significantly lower versus Model group (p < 0.05). As the dose of GDLMI increased, the apoptotic rate of neurons in the cerebral cortex of rats significantly decreased (p < 0.05).
Influence of GDLMI on the ELs of Brain Tissue-related Proteins in Rats with CIF/Reperfusion
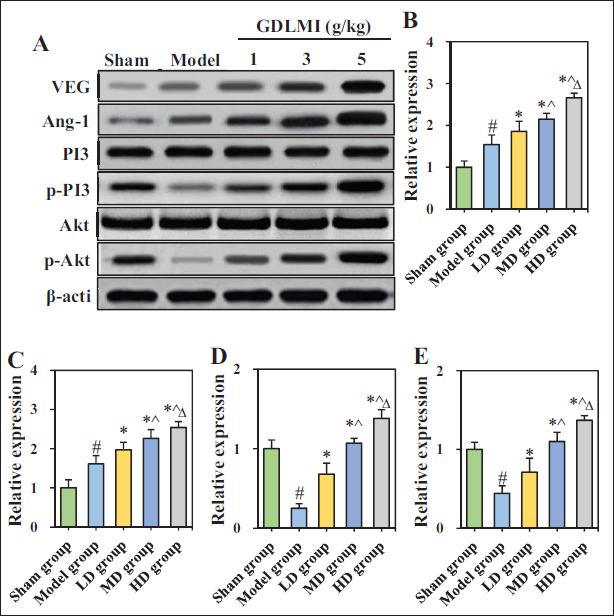
The results of protein ELs of VEGF, Ang-1, PI3K, and Akt in rat brain tissues are shown in Figure 7. The relative expression levels (RELs) of VEGF and Ang-1 proteins in the Model group were considerably superior to the Sham group, while the RELs of p-PI3K and p-AKT proteins were greatly inferior to the Sham group (p < 0.05). RELs of VEGF, Ang-1, p-PI3K, and p-AKT proteins in LD, MD, and HD groups were greatly higher versus the Model group (p < 0.05). As the dose of GDLMI increased, RELs of VEGF, Ang-1, p-PI3K, and p-AKT proteins in rat brain tissues also increased significantly (p < 0.05).
Discussion
When cerebral arteries are blocked without compensatory collateral circulation, corresponding ischemic pathophysiological reactions occur, releasing apoptotic and inflammatory factors, and leading to cellular damage (Sharma et al., 2018). With prolonged ischemia and hypoxia, oxygen free radicals and lipid peroxides accumulate within damaged brain cells, leading to microvascular necrosis, further breakdown of the blood–brain barrier (BBB), and progression of infarction (Copen et al., 2015). Studies noted that the active ingredients of G. biloba extract are primarily flavonoids and terpenoids, which have effects such as improving microcirculation, antioxidation, inhibiting platelet aggregation, and protecting vascular endothelium (Ballarin & Tymianski, 2018; Geng et al., 2017). GDLMI is suitable for the recovery period of phlegm and blood stasis obstruction in stroke patients, enhancing blood circulation and removing obstruction (Luo et al., 2017; Ma et al., 2014). However, more evidence is needed to confirm the protective mechanism of GDLMI against CI/RI.
The Longa scoring method is a widely used approach for assessing the degree of neurological deficits in animals (Li et al., 2023), particularly in rodents such as rats. A higher Longa score indicates a greater degree of neurological impairment. In this study, the Longa score in rats with CI was elevated, whereas treatment with different concentrations of GDLMI led to a reduction in these scores in a dose-dependent manner. These findings imply that GDLMI may alleviate the extent of neurological deficits in rats following CIF, potentially through mechanisms such as inhibiting inflammatory cytokine release and reducing inflammatory responses, thereby protecting neuronal cells from further damage. Clinical studies have also reported (Fan et al., 2020) that, following GDLMI treatment, levels of inflammatory cytokines (such as IL-17 and IL-28A), chemokines (such as CCL14), and coagulation factor III were reduced in patients with ischemic stroke.
Micro-PET is an advanced molecular imaging technique that allows for non-invasive, real-time detection of functional and metabolic changes in biological systems using radiolabeled deoxyglucose, such as 18F-FDG, as a tracer (Yu et al., 2019). In certain neurodegenerative diseases, such as Alzheimer’s disease, patients exhibit a characteristic reduction in 18F-FDG levels in regions such as the temporoparietal junction cortex, anterior cingulate gyrus, and posterior cingulate gyrus (Nam et al., 2023). The Micro-PET analysis revealed a significant decrease in 18F-FDG levels in the brain tissue of rats with CI. However, treatment with varying concentrations of GDLMI resulted in an increase in 18F-FDG levels in the brain tissue of these rats. This suggests that GDLMI may improve the metabolic state of the brain following CIF.
The pathogenesis of ischemic stroke is not fully elucidated, but increased inflammation and oxygen free radicals are potential mechanisms underlying CI/RI (Mahemuti et al., 2023). When ischemic stroke/reperfusion occurs, inflammatory signals are activated, leading to the release of proinflammatory cytokines (Franke et al., 2021). IL-1β, IL-6, and TNF-α levels increased in rats with CIF, and this can further amplify the cascade of inflammatory damage (Zhong et al., 2022). GDLMI is a traditional Chinese medicine composed of ginkgolides A, B, and K. Ginkgolides have been shown to inhibit cyclooxygenase activity, suppress the release of proinflammatory cytokines, and block inflammatory signaling pathways [such as nuclear factor kappa B (NF-κB) and mitogen-activated protein kinase (MAPK)], thereby exerting anti-inflammatory effects (Li et al., 2020). This study found that GDLMI can inhibit the release of proinflammatory cytokines IL-1β, IL-6, and TNF-α following CIF. Based on these findings, we speculate that GDLMI may mitigate the inflammatory response after CIF. This finding is consistent with the results of Bukke et al. (2024), which demonstrated that extracts from the stem bark of Gmelina arborea can inhibit the expression of TNF-α in rat brain tissue following CI/RI, thereby exerting anti-inflammatory effects (Bukke et al., 2024).
SOD, an important antioxidant enzyme, catalyzes the dismutation of superoxide radicals into oxygen and hydrogen peroxide, and its activity reflects the organism’s ability to scavenge oxygen-free radicals, serving as a key indicator of antioxidant system function (Kishimoto et al., 2019). CAT, another crucial enzyme in the biological antioxidant defense system, catalyzes the decomposition of hydrogen peroxide into water and oxygen, thereby helping to maintain the body’s antioxidant status and mitigating oxidative damage to tissues or cells. MDA, a product of lipid peroxidation, is one of the end products of lipid peroxidation, and elevated levels typically indicate the extent of oxidative damage to cellular membrane lipids (Vongsfak et al., 2021). The results indicate that GDLMI dose-dependently inhibits the activation of proinflammatory signaling pathways and exerts neuroprotective effects in acute CI/reperfusion animal models. This study also demonstrated that different doses of GDLMI increase the activity of SOD and CAT and decrease MDA ELs in the brain tissue of acute CI/RI animal models, with more pronounced changes observed with higher doses. This suggests that GDLMI dose-dependently reduces the OS EL in the brain tissue of acute CI/RI animal models. Under OS conditions, free radicals attack the polyunsaturated fatty acids in cell membranes, triggering lipid peroxidation and the production of byproducts such as MDA. These byproducts are highly reactive and can reduce the fluidity of mitochondrial membranes, increase membrane permeability, and ultimately lead to severe consequences such as apoptosis (Zhao et al., 2018). Ginkgolides possess strong antioxidant properties and are capable of scavenging free radicals and reducing OS-induced cellular damage (Li, Xia, et al., 2021). These effects are clearly seen in this study.
TUNEL is a widely used method for detecting apoptosis (Zhao et al., 2024). This study utilized TUNEL staining to analyze the cortical tissue of rats, revealing a significant increase in the number of positively stained cells in the cortical tissue of rats with CIF. However, following treatment with varying concentrations of GDLMI, the number of positively stained cells in the cortical tissue decreased accordingly. This suggests that GDLMI may inhibit neuronal apoptosis in the cerebral cortex of rats following CIF.
After CIF, various adhesion factors, cell molecules, and extracellular matrix are involved in the process of vascular neogenesis. VEGF and Ang-1 are important angiogenic factors that play distinct roles in angiogenesis, vascular stability, and disease progression. Among them, the VEGF is one of the primary regulators of angiogenesis, promoting endothelial cells’ proliferation, migration, and survival, thereby stimulating the formation of new blood vessels (Fei et al., 2021). Early studies demonstrated that intraventricular injection of exogenous VEGF 24 h after MCAO can promote vascular neogenesis and reduce cerebral infarct volume (Zacharek et al., 2010). Nevertheless, VEGF, also acting as a vascular permeability factor, promotes endothelial cell proliferation while concomitantly causing degradation of the vascular basement membrane, thereby increasing microvascular permeability and exacerbating cerebral edema (Chen et al., 2020). Ang-1, a member of the angiopoietin family, is not a mitogen and cannot directly induce endothelial cell proliferation in vitro, but it can stimulate sprouting of endothelial cells cultured in vitro (Zhao, Guo et al., 2022; Zhao, Lu, et al., 2022; Zhao, Wang, et al., 2022). Ang-1 enhances tight junctions between endothelial cells, reducing vascular permeability and maintaining the integrity of the BBB (Mi et al., 2021). Moreover, Ang-1 plays a promoting role in vascular generation and remodeling, and in synergy with VEGF, it can promote angiogenesis (Rufaihah et al., 2017). This study found that treatment with varying concentrations of GDLMI resulted in an increase in the RELs of VEGF and Ang-1 proteins in the brain tissue of rats with CIF. This suggests that GDLMI may promote angiogenesis in these rats by enhancing the translation of the angiogenic factors VEGF and Ang-1, which is significant for facilitating angiogenesis following CIF. Additionally, PI3K/Akt is a key molecule in the normal physiological activities of cells and can be used to regulate cell proliferation and growth (Ates et al., 2022). The research found that when the PI3K/Akt pathway is active, it effectively promotes the metastasis and invasive abilities of tumor cells, which is closely related to VEGF (Husain et al., 2022). The PI3K/Akt signaling is widely present in brain tissue, with Akt acting as a downstream signaling factor of PI3K, controlling processes such as protein synthesis, cell cycle, and vascular neogenesis (Samakova et al., 2019). The BBB is composed of vascular endothelial cells, their tight junctions, the basement membrane, and the end feet of astrocytes. Under normal physiological conditions, the BBB provides nutrients to brain tissue while preventing harmful substances from entering, ultimately maintaining the stability of central nervous system cells (Knox et al., 2022). Following CIF, various factors such as ischemia/hypoxia, inflammation, and OS can disrupt the structure of the BBB, leading to increased permeability. This allows harmful substances from plasma to infiltrate brain tissue, exacerbating edema and neuronal damage. The PI3K/Akt signaling pathway plays a crucial role in regulating BBB permeability (Gong et al., 2023). Research indicates that activation of the PI3K/Akt pathway can promote the proliferation and migration of BBB-related cells, thereby accelerating the repair process of the BBB and enhancing its integrity, which helps prevent harmful substances from entering the brain and protects the central nervous system from further injury (Peng et al., 2024; Zhou et al., 2024). Extensive research has confirmed that the PI3K/Akt pathway regulates the activation of inflammatory cells and the release of inflammatory factors, thereby alleviating the inflammatory response in brain tissue following CIF (Li, Xiang, et al., 2021; Zhou et al., 2024). Additionally, this pathway modulates antioxidant enzymes and enhances cellular antioxidant capacity, reducing OS damage in the brain after infarction. Moreover, it plays a critical role in angiogenesis by promoting the proliferation and migration of endothelial cells (Zhao, Guo et al., 2022; Zhao, Lu, et al., 2022; Zhao, Wang, et al., 2022). This study found that treatment with varying concentrations of GDLMI led to an increase in the phosphorylation levels of PI3K and Akt in the brain tissue of rats with CIF. This suggests that GDLMI may exert its effects by activating the PI3K/Akt signaling pathway, thereby inhibiting the progression of disease in rats following CIF. Furthermore, GDLMI may also improve the state of the BBB following CIF through the activation of the PI3K/Akt signaling pathway, thereby contributing to the protection of neural function after ischemia/reperfusion. Coupled with previous findings that GDLMI inhibits the synthesis of proinflammatory cytokines IL-1β, IL-6, and TNF-α, as well as increases the activities of antioxidant enzymes SOD and CAT while reducing MDA synthesis, these results collectively indicate that GDLMI activates the PI3K/Akt signaling pathway and exerts protective effects against CIF/RI by inhibiting inflammation and OS.
In this study, the TTC staining method was employed to observe differences in the infarct area of brain tissue in rats with CIF following treatment with varying concentrations of GDLMI (1, 3, and 5 g/kg bw). The results indicated that the infarct area in the 3 and 5 g/kg bw treatment groups was significantly smaller than that in the 1 g/kg bw group, with the 5 g/kg bw group showing a further reduction compared to the 3 g/kg bw group. This confirms that, as the concentration of GDLMI increases, its efficacy in reducing the infarct area in the brain tissue of rats with CIF also improves. Therefore, we propose that there exists a quantitative relationship between the dosage of GDLMI and its biological effects in inhibiting CIF.
This study indicated that GDLMI significantly improved neurological function, reduced infarct volume, enhanced brain metabolism, lowered levels of inflammatory cytokines and OS, and promoted the expression of angiogenesis-related proteins, particularly through the activation of the PI3K/Akt signaling pathway. These findings suggest that GDLMI exerts a protective effect against acute CIF/RI injury, providing potential mechanistic support for clinical treatment. However, this study has certain limitations, such as the lack of exploration into the specific mechanisms by which GDLMI affects the BBB in the CIF/reperfusion animal model. Future research should aim to design more detailed experimental protocols, including the use of Evans blue staining to assess the integrity of the BBB in these models, or isolating and culturing endothelial cells and astrocytes related to the BBB to observe changes in morphology, proliferation, migration, and membrane permeability.
Conclusion
GDLMI can improve neurological function in rats with CIF/reperfusion while also inhibiting inflammation and OS damage. Additionally, GDLMI can dose-dependently promote angiogenesis by activating the PI3K/AKT signaling pathway, further suppressing cortical neuronal apoptosis and facilitating the repair of the BBB structure following CI/RI. In conclusion, the findings of this study provide a foundation for the clinical application of GDLMI in the treatment of CIF.
Footnotes
Abbreviations
CIF: Cerebral infarction; ELISA: Enzyme-linked immunosorbent assay; GDLMI: Ginkgo diterpene lactone meglumine injection; HD: High dose; IL: Interleukin; LD: Low-dose; MCAO: Middle cerebral artery occlusion; MDA: Malondialdehyde; MD: Medium-dose; OS: Oxidative stress; ROI: Regions of interest; SOD: Superoxide dismutase; TNF: Tumor necrosis factor; TTC: 2,3,5-Triphenyltetrazolium chloride; TUNEL: TdT-mediated dUTP nick end labeling; VEGF: Vascular endothelial growth factor.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval and Informed Consent
The studies were approved by the ethics committee on the Care and Use of Laboratory Animals of The Affiliated Suzhou Hospital of Nanjing University Medical School.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was funded by Suzhou High-tech Zone “Science and education strong health” science and technology project (No. 2019Q005).
