Abstract
Background
The relationship between insomnia and depression is complex and two-way. Long-term insomnia may cause, maintain, and aggravate depression, and with the development of the disease, depression patients will also experience insomnia symptoms. Oral medication is currently the main treatment for insomnia with depression (ID). Drugs such as Estazolam have good anti-anxiety and insomnia effects, high safety, and relatively small side effects. They are widely used in the treatment of ID in clinics, but some patients still have adverse reactions or low efficacy when taking Estazolam and other drugs. In recent years, Chinese herbal medicine and TCM prescriptions for the treatment of mental illness have been more and more accepted and studied by international scholars. The efficacy of Wendan Decoction (WDD) has been tested by ancient China for nearly 1,400 years, and with the development of modern pharmacological research, it is widely used in the treatment of insomnia and depression.
Objectives
Therefore, based on the understanding of ID in TCM, this article discusses the pharmacodynamic effect of WDD, and based on existing clinical and experimental studies, comprehensively analyzes the clinical observation, mechanism of action, and pharmacological effect of WDD in the treatment of ID, to provide more clinical experience and experimental theoretical support for WDD in the treatment of ID.
Methodology
Retrieve Chinese and English literature on the treatment of ID with WDD from databases such as Web of Science, etc.
Conclusion
WDD has good therapeutic effects on ID.
Keywords
Introduction
Depression is an affective disorder characterized by long-term low mood (Rhead, 2018). The main clinical manifestations are low mood, insomnia, listlessness, loss of interest and pleasure, decreased libido, altered appetite, decreased attention, decreased self-evaluation, cognitive dysfunction, self-harm suicidal tendencies, etc. Depression has the characteristics of high prevalence, disability rate, and suicide rate (Anthes, 2014). Its existence will lead to the decrease of life span, quality of life, and work efficiency of patients, bring serious social burden, and often accompany other diseases, such as diabetes mellitus with depression, coronary heart disease with depression, functional dyspepsia with depression, etc. Insomnia is a common complication of early and middle depression. The relationship between them is complex and two-way. Long-term insomnia may cause, maintain, and aggravate depression, while patients with depression will also have insomnia symptoms such as early awakening, decreased sleep quality, shortened total sleep duration, easy waking up during sleep, and difficulty falling asleep (Gebara et al., 2018). Studies have shown that about 90% of people with depression have insomnia symptoms (Li, Wu, et al., 2016). Insomnia with depression (ID) patients have both insomnia and depressive symptoms. With the accelerated pace of life and life, work pressure increases, ID incidence in recent years continued to rise, so the prevention and treatment of ID more attention by the community and the medical community, and with the development of pharmacology of TCM, TCM prescription multi-target, multi-effect, low toxicity and side effects of the characteristics of the increasingly apparent, is widely used in clinical treatment of diseases, including ID treatment.
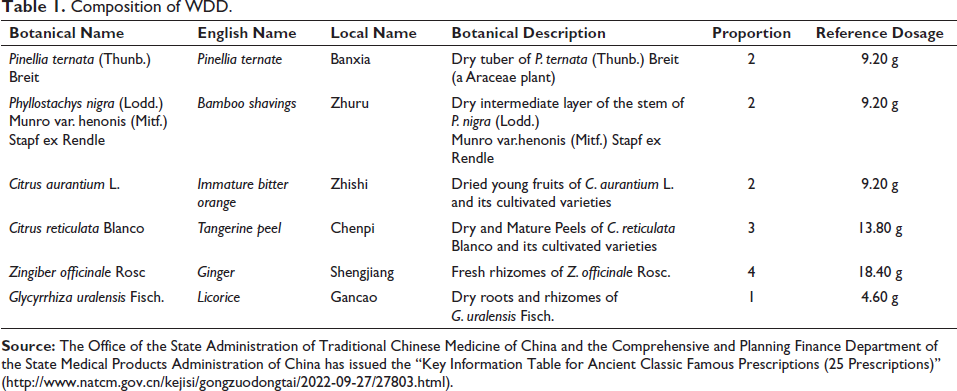
The theory of TCM originated in China and has a history of more than 2,000 years (Chi et al., 2019). Many modern diseases can find corresponding names and treatments of TCM. There is no disease name of “insomnia with depression” in TCM, but it can correspond to ancient diseases such as “zangzao,” “lily disease,” “beidie,” and “insomnia.” There are more and more researcher on the treatment of depression with TCM prescriptions (Lv et al., 2022). In the middle of the 7th century, Sun Simiao of the Tang Dynasty put forward the concept of “gallbladder-deficiency-cold,” and thought that the patients’ depression and easy to be frightened were caused by the deficiency of gallbladder-qi-deficiency and cold, which further led to the uneasiness of mind. He put forward the prescription Wendan Decoction (WDD) for treating this kind of disease in Beiji Qianjin Yaofang, which is composed of Pinellia ternata, Bamboo shavings, Immature bitter orange, Tangerine peel, Ginger and Licorice. Each medicine has its own effect. The combination of the medicines has a therapeutic effect on ID. It is mainly used for timidity and easy to panic, insomnia due to deficiency and restlessness, palpitation and dreaminess; or vomiting, hiccups, bitter mouth, dizziness, and other symptoms. In addition, the State Administration of TCM of China has included WDD in the Catalogue of Ancient Classic Prescriptions (Table 1). Therefore, this article reviews the classic prescription WDD for ID research status, to explore the role of TCM WDD understanding, WDD clinical research, and mechanism of action, for clinical treatment of ID to provide a new TCM treatment prescription.
Composition of WDD.
Methodology
We used a combination of specific keywords in databases such as Web of Science, Science Direct, PubMed, Elsevier, Wiley Online Library, and China National Knowledge Infrastructure, for example, “Wendan Decoction,” “Insomnia with depression,” “Clinical reports,” “Case studies,” “Pharmacology,” “Toxicology,” “Clinical observation,” “Mechanism of action,” etc., as well as the permutations of these words, the search period was set from January 1, 2007, to December 30, 2023, and a total of 230 valid documents were obtained, and 124 publications were obtained from the final screening. The criteria for inclusion in the literature are as follows: (a) Case reports on the treatment of ID using WDD and improved formulas, which have shown significant therapeutic effects; (b) investigating clinical trials or animal studies involving the use of WDD, improved formulas, or combination with Western medicine for the treatment of ID; (c) study the use of WDD, whether improving traditional Chinese medicine formulas or combining with Western medicine, to observe its effects on animals with insomnia and depression, analyze experimental data, and describe potential mechanisms of action; (d) research on the bioactive components of Chinese herbal medicine in traditional Chinese medicine formulas; (e) research on Chinese and English. Exclusion criteria: (a) Repetitive literature; (b) conference papers and other forms of literature.
Understanding of WDD in Treating ID in TCM
Understanding of ID in TCM
In TCM, the onset of human disease is affected by pathological factors from the external environment or the internal body, which affects the material basis such as qi, blood, essence, and body fluid of the human body, so that each Zang-fu organ is affected and cannot perform the original physiological function, which finally leads to the imbalance of the relationship between yin qi and yang qi of the whole person and various symptoms.
The records of insomnia and depression in TCM, such as “sadness” and “melancholy,” can be traced back to the Yellow Emperor’s Internal Classic of TCM, which was written from the Spring and Autumn Period and the Warring States Period to the Han Dynasty, In the Yellow Emperor’s Internal Classic, “It makes you want to lie down, but you can’t sleep” and “Sad emotions come from inside the human body” can be regarded as the understanding of insomnia and depression in TCM (Sun et al., 2021; Ye & Dong, 2017).
TCM believes that the world is composed of qi. There are two types of qi, one is yang qi and the other is yin qi. Yang qi rises upward and yin qi settles downward, forming a circular circulation movement to achieve balance. The same is true of the human body (Hao, 2000). Li Dongyuan, a physician of the Jin and Yuan Dynasties, put forward the theory of “the rising of gallbladder qi like spring” (Wei, 2016), believing that gallbladder qi is the source of yang qi, rising upwards, having the functions of warming, encouraging and encouraging, and is closely related to the mind that dominates the mental activities of the human body. Once the rising of gallbladder qi is abnormal, the functions of rising movement and encouragement will be weakened, and the mind cannot accept the encouragement and encouragement of yang qi. At the same time, yang qi cannot restrict yin qi, and yin qi will not decline normally. Too much yin qi affects the mind. There will be “sadness,” “depression,” “fear” and other negative emotions, and the mind night vacillation will lead to insomnia.
The onset of ID involves many viscera of TCM, which have certain pathological changes. Liver depression and qi stagnation, liver-blood deficiency, spleen deficiency and phlegm excess, kidney-qi deficiency, stomach-qi inversion, etc. will affect the normal movement and function of gallbladder qi, and then affect the mind, leading to insomnia and depression symptoms (Huang & Zhang, 2023; Liu & Teng, 2022; Wang et al., 2021). Therefore, there are many TCM syndrome types of ID in the clinic.
Understanding of the Effect of WDD in TCM
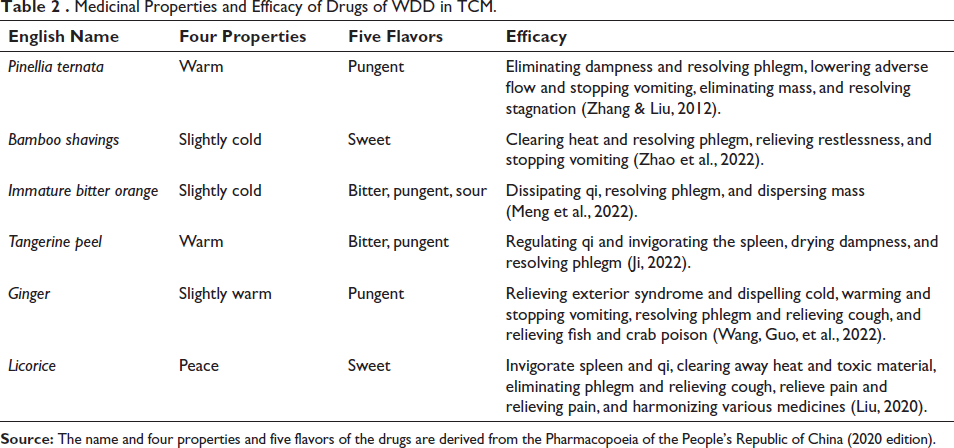
According to Shen Nong’s Herbal Classic and other herbal classics, China ancestors also tried to use drugs such as P. ternata, B. shavings, Immature bitter orange, Tangerine peel, Ginger, and Licorice to treat insomnia and depression (Table 2).
Medicinal Properties and Efficacy of Drugs of WDD in TCM.
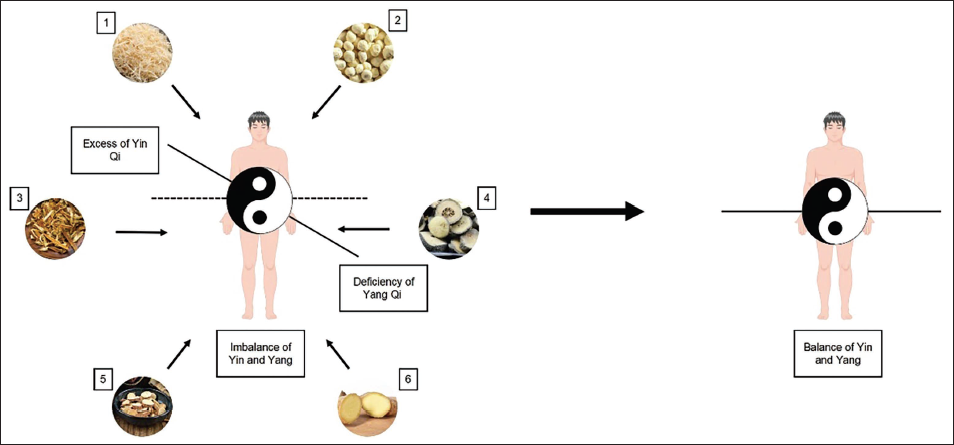
The main pathogenesis of ID treated by WDD is “disharmony between gallbladder and stomach, gallbladder depression and phlegm disturbance” (Zheng et al., 2019), that is, abnormal gastric physiological function, unable to metabolize water normally, water stops gathering into pathological phlegm, blocking gallbladder qi, making gallbladder qi unable to rise normally, gallbladder qi unable to rise and restrict stomach qi, then stomach qi hyperactivity rises. The disharmony between the gallbladder and the stomach itself will cause vomiting and other symptoms, while the stagnation of gallbladder qi affects the mind and leads to insomnia and depression. The main function of WDD is “regulating qi and resolving phlegm, harmonizing stomach and benefiting gallbladder,” that is, dissolving blocked phlegm, restoring the normal rise of gallbladder qi, lowering stomach qi and restoring the normal physiological function of the stomach. The six drugs in WDD have an expectorant effect. Immature bitter orange and Tangerine peel can comb qi and restore the rising of gallbladder qi. P. ternata, B. shavings, and Ginger have an antiemetic effect. P. ternata can lower adverse stomach qi, B. shavings can remove dysphoria and other negative emotions. Each drug is mild in nature and gentle in compatibility, and finally restores the balance of yin and yang of the human body (Figure 1). Therefore, this prescription has been widely used in the treatment of emotional disorders since its birth and has had a good effect on ID.
Clinical Application of WDD in the Treatment of ID
Clinical Case Research of WDD for ID
TCM pays attention to syndrome differentiation and treatment, which is based on the symptom group composed of multiple symptoms of patients, and treats multiple symptoms at the same time. Other viscera or pathological products affect the mind by affecting the gallbladder, which leads to the ID of different TCM syndrome types. Therefore, in clinical treatment (Qiu & Gao, 2021), the type and dosage of drugs in the prescription are often adjusted according to different syndrome types, resulting in many kinds of WDD, such as Huanglian WDD and Chaigui WDD.
Based on the basic pathogenesis of ID (Zhang et al., 2022), Professor Jin said that patients with this disease have pathological changes of viscera, resulting in pathological products such as phlegm and blood stasis, which block the rise of gallbladder qi and disturb the mind. Therefore, the treatment advocated for relieving depression and benefiting the gallbladder, clearing away heart fire and resolving phlegm, promoting blood circulation, and removing blood stasis. One patient suffered from insomnia for more than one year and was depressed due to work pressure. Two months ago, the insomnia was further aggravated due to family conflict. During the day, the patient had a head blindfolded, brain ringing, decreased memory, depressed mood, reddish tongue, thin yellow greasy fur, and wiry and slippery pulse. Hamilton Anxiety Scale (HAMA) and Hamilton Depression Scale (HAMD) evaluation showed: There may be anxiety, or mild depression, choose Huanglian WDD combined with Jieyu Pill for 38 days, sleep at night is normal, mood is stable.
According to Liu et al. (2020), the onset of ID is related to the liver, gallbladder, spleen, and kidney, and ID is divided into four syndrome types: liver depression and spleen deficiency, liver depression and kidney deficiency, liver depression and qi stagnation and liver depression and phlegm-heat. One patient had a sleep disorder for more than three years, accompanied by dysphoria, fear, depression, red tongue, yellow greasy fur, wiry and slippery pulse. He was diagnosed with gallbladder depression and phlegm-heat syndrome. The treatment was to soothe the liver and regulate qi, dissipate phlegm promote gallbladder, clear heat and calm the nerves. After taking Huanglian WDD for 28 days, the sleep state was improved, and other symptoms were relieved to varying degrees.
Professor Ma believes that (Kang et al., 2018), emotional abnormalities, overwork, and improper diet may become the etiology of ID, resulting in phlegm-heat disturbing the heart, causing an imbalance of yin and yang of the human body, so the method of “clearing heat, resolving phlegm and benefiting gallbladder” is adopted for treatment. Take one patient as an example, the patient had difficulty falling asleep three months ago, and the sleep time was less than 3 hours, accompanied by vexation, irritability, fat tongue, yellow greasy fur, wiry and slippery pulse, which was diagnosed as phlegm-heat disturbing spirit syndrome. After 60 days of treatment with WDD, the sleep was improved, and the symptoms such as fatigue were improved.
Clinical Observation of WDD in Treating ID
Clinical studies have confirmed that WDD alone, WDD plus or minus, or WDD combined with other drugs and treatments can effectively treat ID, and the effect is better than that of Estazolam and other drugs (Table 3).
Clinical Applications of WDD in the Treatment of ID.
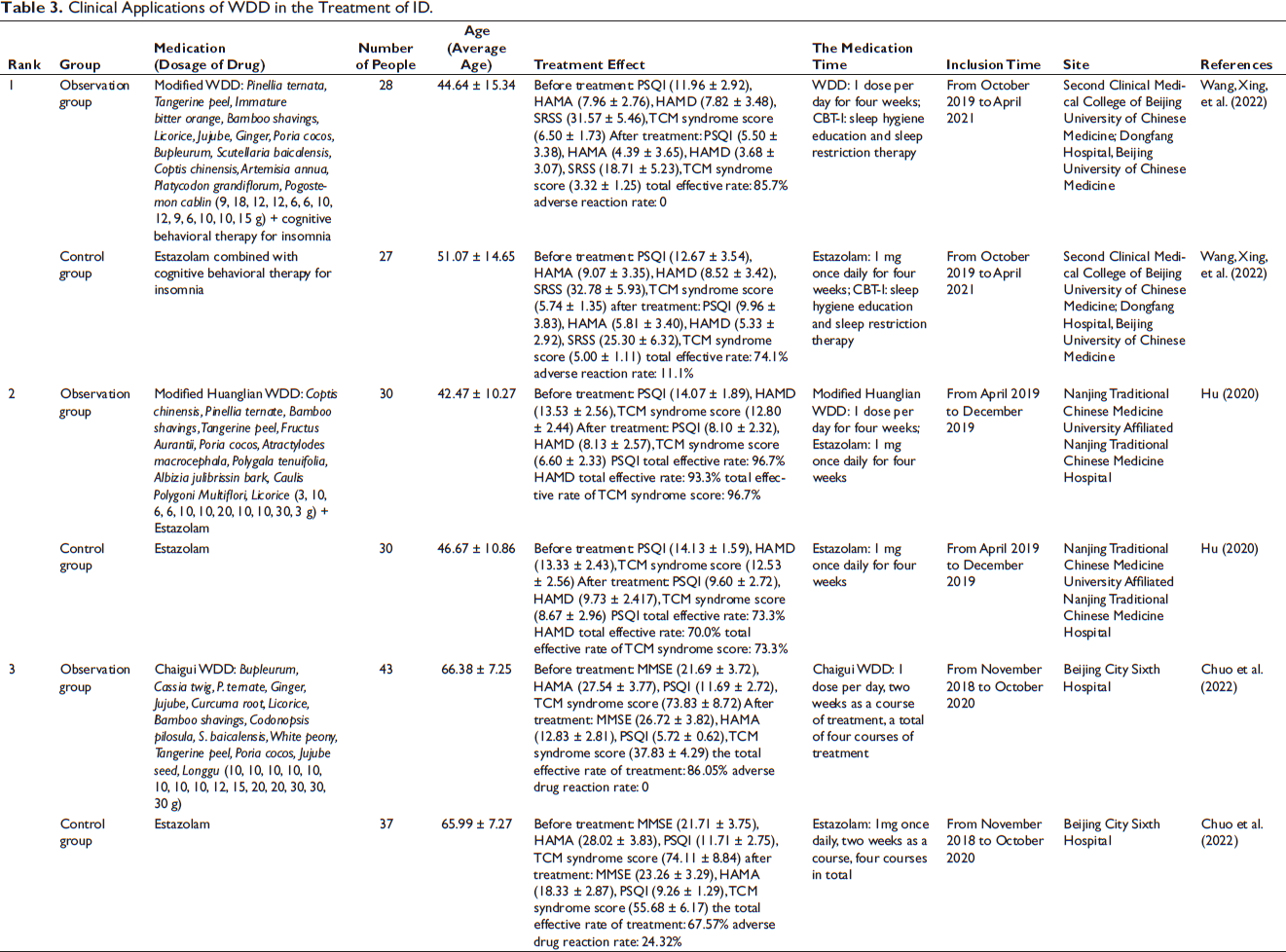
One study shoed that WDD plus or minus formula can be applied to ID patients with phlegm-heat syndrome (Wang et al., 2022). After taking WDD plus and minus formula combined with cognitive behavioral therapy (CBT-I) for four weeks, the scores of HAMA, HAMD, Pittsburgh Sleep Quality Index (PSQI), sleep status self-rating scale (SRSS) and TCM syndrome score were significantly reduced, and the symptoms such as insomnia and depression were significantly improved. The observation group was superior to the control group of Estazolam combined with CBT-I in reducing PSQI, SRSS, and TCM syndrome scores. The researchers also found that the two groups of patients can improve the peripheral serum 5-hydroxytryptamine (5-HT), glutamic acid (Glu), gamma-aminobutyric acid (GABA), melatonin (MT) concentrations were increased, and the observation group 5-HT, GABA, MT increased levels higher than the control group, suggesting that WDD can improve sleep by increasing the level of peripheral neurotransmitters. In another report, 60 patients with ID of phlegm-heat syndrome were equally divided into an observation group and a treatment group, and the course of treatment was four weeks (Hu, 2020). The results showed that, compared with the use of Estazolam alone, the combination of modified Coptis chinensis WDD and Estazolam had a more significant effect on the reduction of PSQI, HAMD, and TCM syndrome scale in ID patients with phlegm-heat syndrome. Another study randomly divided the ID patients with stagnation of liver qi and phlegm syndrome into the observation group (n = 43) and control group (n = 37). The observation group was treated with Chaigui WDD, and the control group was treated with Estazolam (Chuo et al., 2022). After eight weeks of treatment, the scores of PSQI, HAMA, and TCM syndrome in the two groups were significantly lower than those before treatment, and the scores of PSQI, HAMA, and TCM syndrome in the observation group were significantly lower than those in the control group. Minimum Mental State Examination scores were increased, and the observation group score was significantly higher than that of the control group, suggesting that Chaigui WDD addition and subtraction in anti-depression, insomnia can also better improve the cognitive function of patients, compared with the control group 24.32% of the adverse reaction rate, the observation group patients in the whole process of treatment without adverse reactions.
Mechanism of WDD in the Treatment of ID
WDD Can Regulate Neurotransmitters in ID
Neurotransmitters can participate in brain emotion, consciousness, thinking, and other activities, and the synergy and antagonism between neurotransmitters maintain the normal physiological function of the central nervous system (Masi et al., 2010). The abnormality of neurotransmitter levels is the cause of various mental diseases, and it is also the classical theory about the onset of depression (Obata, 2013; Petroff, 2022). 5-HT, Glu, GABA, norepinephrine (NE), and dopamine (DA) are important neurotransmitters that regulate sleep, and the disorder of their levels is also the cause of depression. 5-HT can promote the production of a pleasant mood, increase the effective amount of sleep, and improve the sleep structure. The decrease of 5-HT content will lead to depression, anxiety, and other symptoms, and will lead to insomnia symptoms. Glu is an excitatory amino acid transmitter, which plays an excitatory role in the activity of neurons. The excitotoxicity caused by the increase of its content will lead to depressive behavior and insomnia, while the inhibitory amino acid neurotransmitter GABA can block the excitotoxicity of Glu, to play an anti-insomnia and anti-anxiety role. The increase of Glu content and the decrease of GABA content led to the increase of the Glu/GABA ratio, which will inhibit GABA-related signals, cause neurotoxicity, and cause or aggravate depression and insomnia. NE is also an important neurotransmitter that regulates sleep and mental mood, and its level imbalance can also lead to insomnia and depression. Li, Wang, et al. (2021) prepared the rat model of ID by using chronic unpredictable mild stress combined with an improved multi-platform water environment sleep deprivation method. The results showed that the content of Glu in the hypothalamus increased, the content of GABA decreased (p < 0.01), the ratio of Glu/GABA increased, and the contents of NE, 5-HT, and DA in the hypothalamus decreased (p < 0.05).
Cai et al. (2021) divided 60 patients with phlegm-heat internal disturbance type insomnia into the Estazolam control group and the Huanglian WDD group for four weeks. At the same time, the total sleep time, REM sleep time, sleep latency, awake time, sleep efficiency, and the levels of 5-HT, NE, and GABA were observed. The results showed that Huanglian WDD could improve the total sleep time, sleep latency, awake time, and sleep efficiency of sleep EEG, and increase the levels of 5-HT, NE, and GABA. Zhou et al. (2008) divided rats into a normal group, model group, Chaiyu WDD group, and maprotiline group, and established a rat depression model by solitary feeding plus chronic mild unpredictable stress. The results showed that Chaiyu WDD could improve the behavioral changes of model rats, increase NE and 5-HT in the amygdala (p < 0.05) and increase 5-HT content in the striatum. Chen et al.’s (2010) study also showed that Chaigui Dingzhi WDD could effectively improve the expression of 5-HT and GABA in the hippocampus of chronic stress depression model rats and reduce the expression of Glu.
WDD Has an Anti-oxidative Stress Effect on ID
Oxidative stress can lead to oxidative damage of protein and DNA (Che et al., 2015), cause nerve tissue damage, mitochondrial dysfunction, inflammatory infiltration, etc., reduce the content of some neurotransmitters such as 5-HT, and then cause depression. Modern studies have also confirmed that the occurrence of oxidative stress also increases the possibility of insomnia (Gulec et al., 2012). Malondialdehyde (MDA) is an important product of membrane lipid peroxide, and its increase is related to the pathogenesis of depression and insomnia. Superoxide dismutase (SOD) and glutathione peroxidase (GSH-PX) can scavenge free radicals, have antioxidant capacity, and can reduce oxidative response, depression, and insomnia occurred when its content decreased significantly. Lin et al. (2021) established an insomnia mouse model by injecting p-chlorophenylalanine. The results showed that the SOD level in the brain tissue of the model group was lower than that of the normal group (p < 0.05), and the MDA content was higher (p < 0.05). Ren et al. (2022) established a chronic sleep disturbance model mouse with depression-like behavior by using a roller-type sleep disturbance instrument and found that the SOD level in the hippocampus of the model group mouse decreased by 12.6% compared with the blank group.
Li et al. (2023) divided 30 mice into a control group, model group, and low-concentration group of WDD (containing crude drug 0.5 g/mL), WDD high-concentration group (containing crude drug 2 g/mL), and Estazolam tablet group, the insomnia mouse model was established by improved horizontal rotary table sleep deprivation method, and the serum and brain tissue was taken for determination after continuous gastric administration of the drug for seven days. The results showed that compared with the blank group, the mental state and hair of the mice in the model group were poor, the food intake was reduced, the body weight was significantly reduced, the MDA concentration in the serum and brain tissue was increased, and the GSH-PX and SOD levels were significantly reduced, indicating that the oxidative stress of the mice was serious. The results showed that WDD could improve the symptoms of insomnia in mice, and its mechanism was related to the reduction of oxidative stress. Ni et al. (2023) divided 90 patients with depression after coronary artery bypass grafting into a control group and an observation group to observe the effect of WDD on oxidative stress and sleep of patients with depression after coronary artery bypass grafting. The control group was given oral sertraline hydrochloride tablets, and the observation group was given WDD on this basis the results showed that the scores of HAMD, PSQI, and Self-rating Depression Scale in the observation group were significantly lower than those before treatment (p < 0.05), the level of MDA was decreased (p < 0.05), and the level of SOD was increased (p <0.05).
WDD Can Regulate Neural Plasticity in ID
The change of neural plasticity is currently considered one of the pathogens of depression and sleep disorders (Duman & Monteggia, 2006). The dysfunction of neural plasticity can lead to the continuous decrease of the expression and signal transduction of brain-derived neurotrophic factor (BDNF), which further leads to the atrophy and prominent loss of neurons in the hippocampus and other regions, and finally affects the adaptability of the body to the environment. BDNF is produced by astrocytes and neurons, with the highest content in the cerebral cortex and hippocampus. BDNF itself can provide nutritional support, repair damaged neurons, increase synaptic plasticity, and promote neurogenesis. Its synthesis is controlled by the NE system and plays a key role in the pathophysiology of stress-related emotional disorders. Studies have confirmed that the interaction between stress and sleep can affect BDNF levels (Tian et al., 2020), and the decrease in BDNF levels can also cause sleep disorders and depression. TrkB is a high-affinity receptor of BDNF, and most of the functions of BDNF in neuronal growth and differentiation come from TrkB transmission. Li et al. (2023) established insomnia in rats with anxiety-like behavior by intraperitoneal injection of PCPA suspension. The results showed that the prefrontal cortex of model group rats was damaged and the expression of BDNF decreased compared with blank group rats (p < 0.01). Li, Zheng, et al. (2021) established the insomnia rat model by fasting every other day, intragastric administration of rhubarb decoction, and intraperitoneal injection of PCPA. It was found that the expression levels of BDNF and TrkB protein in the brains of insomnia rats were significantly decreased (p < 0.01).
The study of Ni et al. (2023) confirmed that WDD can significantly improve the depressive symptoms and sleep status of patients with depression after coronary artery bypass grafting, and can significantly increase the BDNF level of patients (p < 0.05), and the effect is better than that of the control group (p < 0.05). In Chen et al.’s (2010) study, the number of BDNF and TrkB immunoreactive neurons in long-term mild unpredictable stress plus solitary depression model rats was significantly reduced, while high and medium dose groups of Chaigui Dingzhi WDD could increase the expression of BDNF and TrkB in the hippocampus of rats to varying degrees. Wang (2019) evaluated the antidepressant effect of Shenhu WDD by establishing a chronic unpredictable mild stress model. The results showed that compared with the model group, the protein expression of BDNF in the intervention group of Shenhu WDD was significantly increased (p < 0.01), and the expression of BDNF mRNA and TrkB mRNA was significantly increased (p < 0.01), suggesting that Shenhu WDD could play an antidepressant role by regulating neurotrophic factor BDNF and its receptor TrkB.
WDD Can Slow Down the Inflammatory Reaction in ID
Inflammatory cytokines are immunoreactive factors secreted by immune cells. Some inflammatory factors can affect neurotransmitter metabolism, neural plasticity, neuroendocrine function, etc. while participating in immune response, and the increase of their content can lead to depression and sleep disorder (Beurel et al., 2020; Du et al., 2017). Proinflammatory cytokines such as interleukin-1 (IL-1), interleukin-6 (IL-6), tumor necrosis factor-alpha (TNF-α), and anti-inflammatory cytokines such as interleukin-4 (IL-4), interleukin-10 (IL-10) have been proved to play an important role in nervous, immune and endocrine systems. In Zhang’s (2021) study, the levels of pro-inflammatory factors such as TNF-α, IL-6, and IL-8 in depression patients with insomnia disorder were significantly higher than those in the normal group. Shen et al. (2018) established the insomnia mouse model by 72 hours multi-platform water environment method, and evaluated the anxiety-like behavior and depression-like behavior of mice by open-field test, tail suspension test, and forced swimming test, respectively. The results showed that compared with the normal group, the contents of IL-1β, IL-6, and TNF-α in the hippocampus of mice in the model group were significantly increased (p < 0.01), IL-4 content decreased significantly (p < 0.01), central exploration time in open field shortened significantly (p < 0.05), immobility time in tail suspension and forced swimming prolonged significantly (p < 0.05).
In Wang’s (2019) study, Shenhu WDD can up-regulate the levels of anti-inflammatory factors such as IL-4 and IL-10, and reduce the levels of inflammatory factors such as IL-1β, IL-6, and TNF-α. Xu et al. (2021) divided 40 mice into a blank group, model group, modified WDD group, and fluoxetine group. The rat model was established by solitary feeding and chronic unpredictable stress. After 28 days of intragastric administration of WDD, compared with the model group, the injury of glial cells in rats in the modified WDD group was significantly reduced, and the levels of IL-1β, IL-6, and TNF-α in serum were significantly reduced (p < 0.01). Li, Liu, et al.’s (2022) study also confirmed that the high and medium dose groups of WDD could significantly reduce the concentration of IL-1β, IL-6, and TNF-α in serum and brain tissue of sleep-deprivation mice (p < 0.05), suggesting that the anti-insomnia effect of WDD may be related to the reduction of inflammation level.
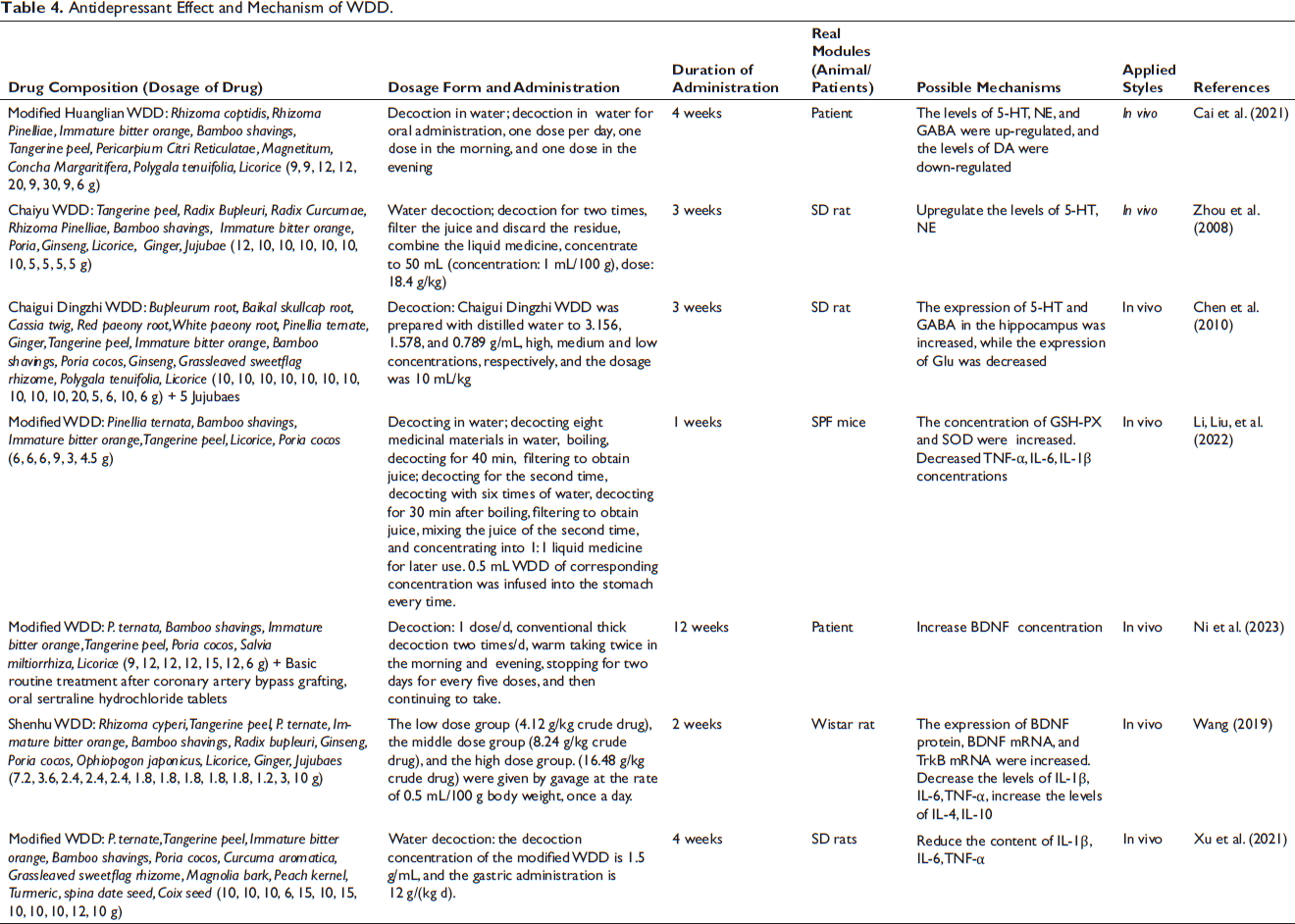
To sum up, WDD plays an anti-insomnia and anti-depression role mainly by regulating the levels of neurotransmitters such as 5-HT, anti-oxidative stress, improving the level of BDNF, improving neural plasticity and reducing the level of inflammation Table 4), but the specific mechanism of its treatment of ID needs to be further explored.
Antidepressant Effect and Mechanism of WDD.
Pharmacological Studies of Component Drugs in WDD
Pinellia ternata
P. ternata is one of the main components of WDD, which has the pharmacological effects of relieving cough and eliminating phlegm, stopping vomiting, anti-tumor, anti-oxidation, reducing blood lipid, etc. The main chemical components include alkaloids, organic acids, volatile oils, amino acids, proteins, sterols, flavonoids, etc. (Li, Xuan, et al., 2021; Zuo et al., 2019). The researchers extracted the alkaloid components in P. ternata in different ways and found that the alkaloid components in P. ternata include
Studies have confirmed (Zhao et al., 2011) that the water extract of P. ternata itself has no direct hypnotic effect, but its water extract can effectively prolong the sleep rate of animals with a subthreshold dose of pentobarbital sodium, and its alcohol extract can significantly prolong the sleep time of pentobarbital sleeping mice. Zhou et al. (2013) applied P. ternata extract to lipopolysaccharide-stimulated mouse aortic endothelial cells, and the results showed that P. ternata extract could reduce TNF-α and IL-6 levels. Feng’s research confirmed (Feng et al., 2021) that P. ternata total alkaloids can significantly reduce serum MDA levels and increase SOD and GSH-PX levels. Liu et al.’s (2004) research shows that β-sitosterol has a strong inhibitory effect on oxygen free radicals.
Bamboo Shavings
Bamboo shavings is famous for its effects of clearing heat and resolving phlegm, relieving restlessness and stopping vomiting, and has the effects of lowering blood lipid and antioxidation. It mainly contains chemical components such as polysaccharides, triterpenoids, flavonoids, sterols, organic acids, and amino acids (Yang et al., 2021; Yao, 2004; Zhang et al., 2011). The main triterpenoids in Bamboo shavings are friedelin, friedelin, lupeenone, lupeenol, and amyrin. The main sterols in Bamboo shavings include stigmasterol, campesterol, taraxasterol, β-sitosterol, etc. (Lou, 2005). At present, there are few studies on Bamboo shavings, mainly focusing on the pharmacological effects of Bamboo shavings polysaccharides.
Studies have confirmed (Yang et al., 2019) that Bamboo shavings extract can regulate hippocampus and microglia through HO-1 and Nrf-2 mediated pathways, and play a neuroprotective and anti-neuroinflammatory role. The study by Jin (2017) showed that Bamboo shavings polysaccharide could significantly reduce the mRNA expression of TNF-α, IL-1β, and IL-6 in adipose tissue of mice fed with a high-fat diet.
Immature Bitter Orange
The main effects of Immature bitter orange are to break qi and eliminate stagnation, dissipate phlegm, and dissipate mass and have the effects of anti-oxidation, exciting smooth muscle, increasing blood pressure, lowering blood sugar, anti-tumor and lowering blood sugar (Chen et al., 2022; Li et al., 2011; Zhang et al., 2009). Its main pharmacological components mainly include hesperidin, naringin, hesperetin, naringenin, neohesperidin, narirutin, isosakuranetin 7-O-β-
Studies have confirmed (Liu et al., 2017; Zhang & Huang, 2014) that eriodictyol, naringenin, hesperetin, luteolin, apigenin, aurantioxanthin, iso-cerasin, phloretin, diosgenin, etc. produced by the metabolism of water extract of Immature bitter orange in vivo can reduce TNF-α level. Kim et al.’s (2012) study also confirmed that the total flavonoid extract of Immature bitter orange can inhibit the expression of TNF-α, IL-6, etc., and play an anti-inflammatory role. In Wang’s (2012) study, synephrine extracted from Immature bitter orange can exert an antidepressant effect by increasing NE and 5-HT levels in the cerebral cortex of rats with chronic stress depression model superimposed on solitary depression.
Tangerine Peel
Tangerine peel itself has the effects of regulating qi and invigorating the spleen, eliminating dampness resolving phlegm, etc. Modern pharmacology has proved that it has antibacterial, anti-inflammatory, anti-oxidation, resolving phlegm, promotes digestion, softens blood vessels, anti-tumor, reduces lipid, reduces blood pressure, antiviral, improves glucose metabolism, anti-allergy, and other effects (Wang, 2020; Xu et al., 2022). The main components include hesperidin, neohesperidin, dihydronobiletin, nordihydronobiletin and other flavonoids, limonene, γ-terpinene, beta-myrcene and other volatile oil components, and synephrine and other alkaloids.
Zhang’s (2021) study showed that hesperidin, the main extract of Tangerine peel, can inhibit NF-κB, IL-1β, IL-6, TNF-α, and other pro-inflammatory factors and play an anti-inflammatory role. Meanwhile, hesperidin has also been proven to have good effects on regulating neural plasticity, BDNF levels, and antioxidant capacity. Studies have shown (Yu et al., 2022) that flavonoids in Tangerine peel have good antioxidant activity and high scavenging capacity for 2,2-diphenyl-1-picrylhydrazyl (DPPH), ABTS free radicals, and hydroxyl free radicals. The research results of Li et al. (2014) showed that nobiletin in Tangerine peel could up-regulate BDNF levels in hippocampus of mice with chronic mild unpredictable stress depression model, so as to protect nerves and significantly improve behavioral indicators of mice.
Ginger
Ginger is the component with the highest content in the original prescription of WDD, which has the effects of relieving exterior syndrome and dispelling cold, warming and stopping vomiting, resolving phlegm and relieving cough, relieving fish and crab poison, etc. Modern pharmacological studies have found that Ginger has effects of anti-inflammatory and analgesic, anti-tumor, anti-oxidation, anti-coagulation, regulating glucose metabolism, regulating lipid metabolism, etc. (Wu et al., 2019; Zhang et al., 2020). In addition to cellulose, starch, fat, protein, and other nutritional components, Ginger has diphenyl heptanes, polysaccharides, gingerol, volatile oil, glycoprotein, and other components. Gingerols, including shogaol, gingerol, and gingerone, are important active components in Ginger.
Li, Zhang, et al. (2016) study showed that Ginger alcohol extract could effectively improve the activities of SOD, GSH-PX, and catalase in liver tissue of rats with hepatic ischemia-reperfusion, and improve the level of total antioxidant capacity. The possible mechanism of gingerol in improving symptoms of depression and insomnia is to reduce inflammatory levels and resist oxidative stress. Studies have found that 6-shogaol and 8-gingerol have strong anti-inflammatory activity, while 6-shogaol has a strong scavenging capacity on DPPH free radicals (Ezzat et al., 2018; Sun, 2018).
Licorice
Licorice has the effects of invigorating the spleen and qi, clearing away heat and toxic materials, eliminating phlegm and relieving cough, relieving pain and relieving pain, and harmonizing various drugs. It has the pharmacological effects of anti-inflammation, anti-tumor, anti-virus, nerve protection, antibacterial, anti-fibrosis, protection of the cardiovascular and cerebrovascular system, anti-diabetes, liver protection, immune regulation, anti-osteoporosis, etc. The main chemical components include triterpenoids, flavonoids, polysaccharides, volatile oils, amino acids, etc. (Deng et al., 2021; Li & Li, 2019). Among them, triterpenoids represented by glycyrrhizic acid and glycyrrhetinic acid, and flavonoids represented by isoliquiritin, liquiritigenin, and licochalcone are the main active components of Licorice extract (Li, Hao, et al., 2022).
Studies have shown that glycyrrhetinic acid, isoliquiritin, licochalcone A, licochalcone B, and licochalcone E all have neuroprotective effects (Bak et al., 2016; Cao et al., 2020; Mirza et al., 2014; Seon et al., 2012; Wang et al., 2008). Total flavonoids of Glycyrrhiza can exert an antidepressant effect by enhancing central 5-HT function and inhibiting neuronal apoptosis, among which liquiritin and isoliquiritin can enhance 5-HT activity and promote NE release, while liquiritigenin can down-regulate the expression of phosphorylated NF-kB inhibitory protein and NF-kB/p-p65 and increase the levels of TrkB and BDNF, while isoliquiritigenin can also protect nerves and reduce nerve tissue injury (Su et al., 2016; Tao et al., 2016; Wang et al., 2008).
Toxicological Studies
No toxicological studies have been reported on the treatment of ID by WDD, and relevant studies have been conducted mainly on the medications that make up WDD, especially P. ternata, and Ginger. P. ternata has certain toxicity, with mucosal toxicity, liver and kidney toxicity, and pregnancy toxicity being its main toxic effects (Bai et al., 2022). Its widely recognized main toxic component is sharp raphides, composed of calcium oxalate and more than 100 proteins. Calcium oxalate has the effect of inducing inflammation, while the aphides can cause rabbit conjunctival oedema and foot metatarsus swelling of rats the main protein PTL in raphides had the obvious effect of pro-inflammation, and the toxic mechanism of P. ternata was PTL-induced inflammation only when the raphides pierce into the organization (Bai et al., 2022; Zhu et al., 2012). By using different auxiliary materials such as Alum, Lime, Ginger or Licorice, as well as soaking or boiling, and other different processes for processing, the toxicity of P. ternata can be effectively reduced, the structure of calcium oxalate crystals, and PTL can be destroyed, and the content of toxic substances such as radish glucoside can be reduced (Li, Cui, et al., 2021). By using different auxiliary materials such as alum, lime, Ginger, or Licorice, as well as soaking or boiling, and other different processes for processing, it can play a role in destroying the structure of calcium oxalate crystals and PTL, and reduce toxicity (Wang et al., 2019). Ginger is often considered a safe and effective traditional Chinese medicine, but there are reports showing that in utero exposure to Ginger tea can lead to an increase in early embryo loss and that Ginger taken orally can cause adverse reactions such as mild diarrhea in some healthy individuals (Ali et al., 2008). Apart from that, there are no relevant toxicological studies on Immature bitter oranges; Licorice is considered to be a commonly used antidote to toxins (Li et al., 2019); studies related to Tangerine peel and Bamboo shavings have also shown that both have a higher safety profile (Chien et al., 2018; Zhang et al., 2004).
Conclusion
In this study, based on literature research, we found that WDD has good therapeutic effects on ID. This provides a reference for the clinical treatment of ID with prescriptions such as WDD.
Summary
Depression, as a common mental disease, often accompanied by insomnia, seriously reduces the quality of life of patients, and clinically available drugs with low side effects are limited. Therefore, traditional Chinese medicine prescriptions with excellent curative effects, small side effects, and low cost have gradually become one of the choices for the treatment of ID.
The WDD has a history of about 1,400 years, and the original prescription consists of P. ternata, Bamboo shavings, Immature bitter orange, Tangerine peel, Ginger, and Licorice, and the main active ingredients in various medicines, such as Pinellia alkaloid, beta-sitosterol, Bamboo shavings polysaccharide, Immature bitter orange total flavonoids, synephrine, dried orange peel total flavonoids, gingerol, Licorice total flavonoids, and the like, play the role of resisting depression and insomnia by regulating neurotransmitters, resisting oxidative stress, protecting nerves, slowing down inflammation level and the like. Clinically, the composition of prescriptions is often flexibly adjusted according to the different symptoms of patients, and many kinds of prescriptions are derived from this, and the therapeutic effect is quite good.
However, there is still a lack of research on the treatment of ID with WDD, which includes the following issues: (a) the lack of the phytochemistry part for each plant—key phytochemicals components and their effects in mechanisms, including network pharmacology research and experimental verification. More research is needed to determine the key pharmacological active ingredients and their interactions; (b) lack of toxicological research and safety evaluation on the treatment of ID with WDD; (c) there have been no reports on the application of nanotechnology in the preparation of WDD; (d) there are issues with the lack of control and small sample size in related research, which alone cannot provide clear evidence; (e) it is unclear whether the mechanisms and pathways proposed based on in vitro and animal research can be transformed into humans. In response to the above issues, this review provides the following opinions: (a) Recognizing the necessity of human research, more rigorous clinical trials such as multicenter, prospective, randomized, double-blind controlled trials are used to verify the efficacy of WDD in treating patients with insomnia and depression; (b) conduct toxicological experiments on the treatment of ID with WDD to evaluate its safety; (c) attempt to apply nanotechnology to the preparation of WDD reagents, to promote the better clinical efficacy of WDD; (d) using various modern technologies such as genomics, transcriptomics, proteomics, metabolomics, network pharmacology, HPLC, etc., this study explores the mechanism and pathway of WDD in treating patients with ID, revealing its key pharmacological components and drug interactions.
Therefore, this article reviews the treatment mechanism, clinical cases, mechanism of action, and pharmacological effects of WDD, to provide a reference for clinical treatment of ID.
Abbreviations
5-HT: 5-Hydroxytryptamine; BDNF: Brain-derived neurotrophic factor; CBT-I: Cognitive behavioral therapy for insomnia; DA: Dopamine; DPPH: 2,2-diphenyl-1-picrylhydrazyl; GABA: Gamma-aminobutyric acid; Glu: Glutamic acid; GSH-PX: Glutathione peroxidase; HAMA: Hamilton Anxiety Scale; HAMD: Hamilton Depression Scale; ID: Insomnia with depression; IL-1: Interleukin-1; IL-10: Interleukin-10; IL-4: Interleukin-4; IL-6: Interleukin-6; MDA: Malondialdehyde; MMSE: Minimum Mental State Examination; MT: Melatonin; NE: Norepinephrine; PSQI: Pittsburgh Sleep Quality Index; SOD: Superoxide dismutase; SRSS: Sleep status self-rating scale; TNF-α: Tumor necrosis factor-alpha; WDD: Wendan Decoction.
Footnotes
Acknowledgments
Thank you to my girlfriend X. H. This review article is our first collaboration. Thank you to my enlightenment teacher T. T. for your support and encouragement.
Author Contributions
All authors contributed significantly to the present research and reviewed the entire manuscript.
L. K., X. H.: Writing—original draft preparation.
L. K, X. L: Writing—review and editing.
All authors have read and agreed to the published version of the manuscript.
Data Availability Statement
The data are available upon request from the author.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval and Statement of Informed Consent
Not applicable.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work is financially supported by the Natural Science Foundation of Shandong Province, China (No. ZR2020MH346; No. ZR2021MH003) and the National Natural Science Foundation of China (No. 81273667).
