Abstract
In the Taihang Mountain areas, known as the “esophageal cancer zone” in China, the incidence of esophageal cancer (ESCA) ranks the first in the country and shows a familial and regional clustering trend. Taihang Mountain areas are located in a mountainous area, with inconvenient transportation, limited living conditions, unbalanced diet, and poor nutrition. Ninety percent of the pathological types of ESCA in Taihang Mountain areas are squamous cell carcinoma, among which the risk factors have not been well understood. These areas are usually remote villages and mountains with low population mobility, large family members, similar environmental factors, and a clear and stable genetic background. Therefore, according to the current situation, second-generation sequencing and multigroup analysis technology are used to analyze the familial ESCA patients; disease-related genetic variation are located; and then disease-related susceptibility genes associated with ESCA are screened and analyzed. Health education, tobacco control, endoscopic screening, and other health management projects for suspected and high-risk patients in areas with a high incidence of ESCA can be carried out for screening and early diagnosis, and the incidence of ESCA in Taihang Mountain areas can be reduced. A comprehensive continuous care pattern based on traditional medical nursing to track, monitor, evaluate, and intervene with patients diagnosed with ESCA to facilitate them with medications guidance, dietary guidance, and timely health problem-solving is established. Furthermore, statistical analysis of epidemiology, gene sequencing, and family genetics information can be performed on patients with ESCA in the Taihang Mountains areas to clarify the relationship between genetic phenotype and genotype during the occurrence of ESCA.
Keywords
Introduction
Geographic differences in the incidence of esophageal cancer (ESCA) are apparent, with different histological characteristics including esophageal squamous cell carcinoma (ESCC) and esophageal adenocarcinoma (EADC) having diverse pathogenic factors and etiology in different regions. Familial aggregation is a prominent epidemiological feature in the high incidence of ESCA in China, manifested as multiple cases of ESCA in the same family. In past studies, the high-incidence pedigree was often used to indicate the familial high-detection phenomenon of ESCA, which generally refers to at least two patients with ESCA in three consecutive generations.
Previous epidemiological studies have suggested that ESCA cases tend to cluster in families. Chinese scholars have long noticed this familial high-detected phenomenon of ESCA. Li Pingjuan et al. conducted an epidemiological survey on the areas with a high incidence of ESCA. They found that 47% of the families with three generations of direct family members had more than three people suffering from ESCA. In a family of 23 people in three generations, there were as many as 16 patients with ESCA, and the prevalence rate is as high as 70% 1 . In addition to similar genetic basis, similar living environment and lifestyle are also the cause of familial clusters distribution in the high-incidence areas of ESCA, which indicates that the occurrence of ESCA may be the result of the interaction between genetic factors, environment, and lifestyle.
Despite rapid advances in medical care, the incidence of ESCC in developing countries and EADC in developed countries is still increasing. This increase is worrying, which is a public health problem facing many countries and even the world. Therefore, the clinical and pathological characteristics of patients with a high incidence of ESCA are clarified. The clinical evaluation and early prevention of patients with a high incidence of ESCA and prognosis provide a scientific basis. Due to some uncertain causes, it is difficult for non-Chinese scientists and scholars to research specific ESCA that contains familial and genetic factors and is geographically concentrated. This review aims to reveal the environmental, ethological, and biological risk factors by comparing them with those described in other communities in China and other parts of the world, to give a comprehensive view of the epidemiology of familial ESCA of Taihang Mountain areas in China.
Descriptive Epidemiology of ESCA in the World and China
The geographic variation in ESCA incidence is noticeable, and the exact cause is unclear. It is widely acknowledged as the result of comprehensive factors including diet and lifestyle, environmental, demographic, and genetic factors 2 . According to global cancer statistics, ESCA is higher in East Asia and South Africa, while the incidence is lower in Western and Central Africa and Central America, with a difference of nearly 12 times in incidence (Fig. 1). The area stretching from Northern Iran through the central Asian republics to North-Central China is referred to as the “esophageal cancer belt” because of the significantly higher incidence. Especially, Eastern Asia has the highest incidence rate of ESCA, in which the rate in China is in the top 5 worldwide 3 . The incidence of EADC has remarkably risen during the last decades, and it was about three times higher in males than in females, while the 5-year overall survival rate for all types of ESCA was only 18%. Meanwhile, EADC has become the predominant type of ESCA in Northern America and Northern Europe, accounting for nearly 60%, while ESCC accounts for about 34% 4 . The high incidence of ESCA is concentrated in China and Mongolia in East Asia, Iran in Central Asia, East Africa, South Africa, and other developing countries. The most common histological subtype is ESCC, accounting for more than 90%, significantly different from Western countries 5 . Among them, China is a particularly high-risk area where ESCA cases accounted for more than half of the world 6 . In China, the incidence is concentrated in rural areas and more common in males. Areas with a high incidence of ESCA are generally located in poor areas with a lack of water, barren land, low production, and lack of nutrition in the diet. Several high-incidence areas of ESCA in China are mainly concentrated in the vicinity of the Taihang Mountains at the junction of Henan Province, Shexian, Cixan of Hebei Province, and Changzhi, Yangcheng of Shanxi Province, forming a unique geographical distribution pattern of concentric circles (Fig. 2) 7 . Statistics showed that in these areas with a high incidence of ESCA, the middle esophagus had the highest incidence, followed by the lower esophagus, and the upper esophagus was the lowest 8 .
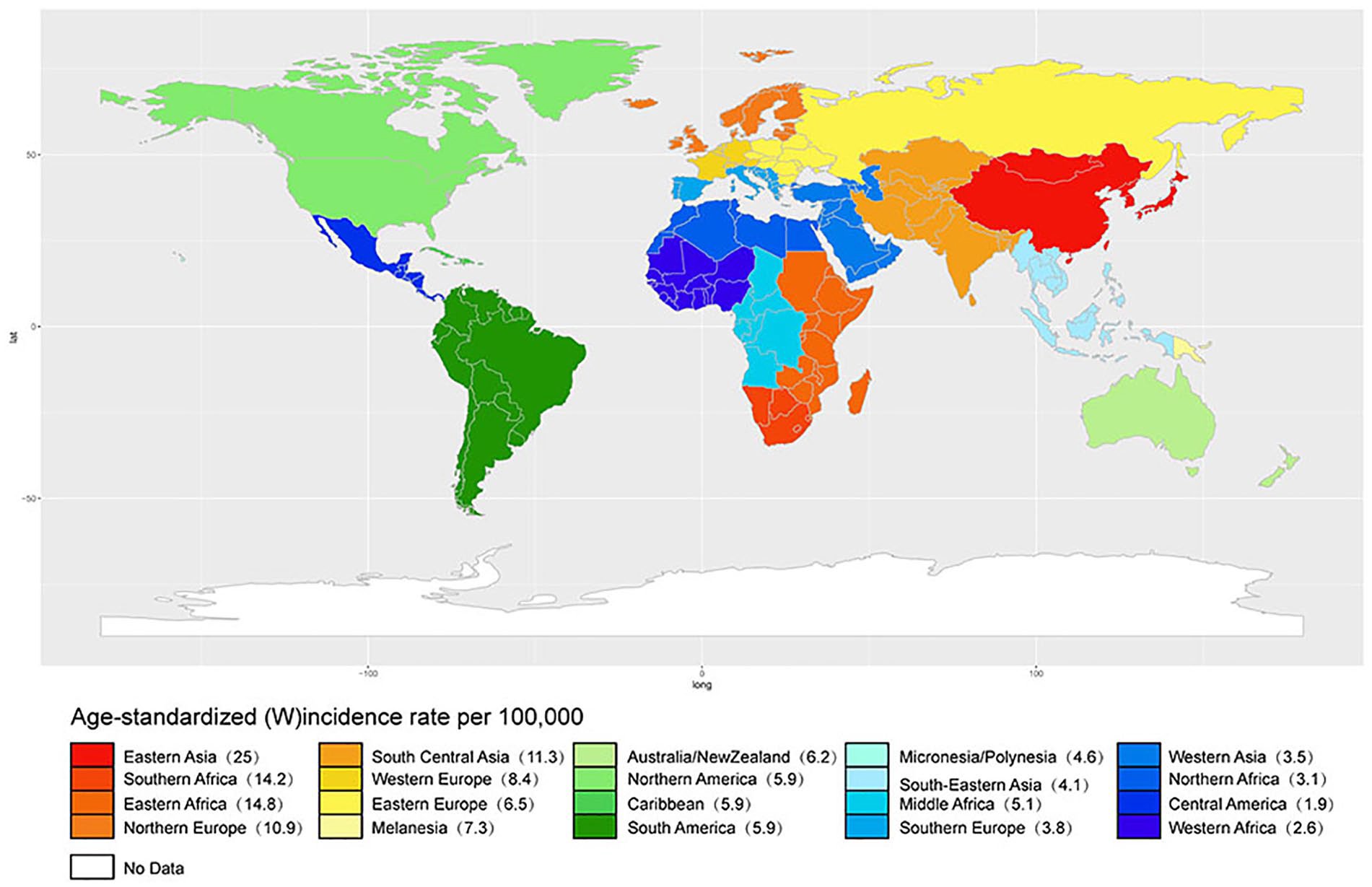
Region-specific incidence rates of esophageal cancer in 2010 are shown around the world. The sizes of the populations with esophageal cancer in each region are included in the legend. Source: United Nations Procurement Division/United Nations Development Program.

The geographic location of high-risk areas of esophageal cancer in the China. The high incidence of esophageal cancer in China is concentrated in the vicinity of the Taihang Mountain areas.
Westerners are susceptible to ESCA, including obesity, smoking, drinking, and gastroesophageal reflux gastritis 9 . In addition to obesity, male sex, Barrett’s esophagus, gastroesophageal reflux disease, decreased acidity, and reduced secretion of gastric juice are also risk factors that cause an increase in the incidence of ESCA 10 . In comparison, Eastern people’s risk factors include adverse lifestyle, environmental factors, susceptibility genes, vitamin deficiency, especially riboflavin, and nitrosamine exposure2,11. In a prospective study of 29,584 adults in Linxian County, China, subjects were followed up for 15 years regarding demographic characteristics, personal and family history, and lifestyle factors (including birth year). To evaluate the risk factors of ESCA using the Cox proportional hazard model: including being born in Linxian, height, smoking, and increasing number of pipes; factors to prevent ESCA including formal education, tap water, meat, eggs, and fresh fruits increased consumption and increased body mass index 12 .
Description of ESCA in Taihang Mountain Areas
According to data from the National Cancer Registry and the Center for Disease Control and Prevention of the Ministry of Health, ESCA was among the top five causes of death from malignant tumors from 1973 to 2005, with the death rate increasing in every age group 13 . The latest annual tumor registry report shows that the incidence and mortality of esophageal cancer are 477.9/100,000 and 375.0/100,000, respectively. Among them, the incidence of esophageal cancer in rural areas (364.1/100,000) accounted for 76.18% of the total incidence, and the mortality rate (285.9/100,000) accounted for 76.24% of the total mortality 14 .
Data show that from 1998 to 2002, the incidence of esophageal cancer in Taihang Mountains was 105.4/100,000 men and 75.8/100,000 women. According to the research results of Zhang Nan et al., the total incidence of upper gastrointestinal tumors in Linzhou and Shexian with less mountainous areas near the Taihang Mountains is lower than that in Yangcheng and Cixian with more mountainous areas, and the incidence is higher—mainly men. However, in Ci County, which has the fewest mountainous areas, the total incidence of esophageal cancer is higher than other counties and cities, regardless of gender (Table 1) 15 . Analysis of esophageal cancer cases in Linzhou City, Taihang Mountains, found that from 1988 to 2010, there were 14,159 esophageal cancer deaths in Linzhou City, and the esophageal cancer mortality rate showed a downward trend from 1988 to 1990 and 2001 to 2005 16 . Analysis of ESCA morbidity and mortality in each age group found that the morbidity and mortality of ESCA were at a low level below the age of 35, rose rapidly above the age of 60, and reached a peak at the age of 84 17 . Overall, the morbidity and mortality rates of ESCA in Taihang Mountains were higher in males than in females, and higher in rural areas than in urban areas. Although there are some differences between urban and rural areas, the overall distribution is similar.
World ASRs of Esophageal Cancer Incidence in Taihang Mountain Areas, 1998–2002 (1/100,000).

Source: Zhang et al. 15
In Shexian County, the data are for 2000 to 2002.
Risk Factors for ESCA
Environmental Factors Causing High Incidence of ESCA in the Taihang Mountain Areas
ESCA in Taihang Mountain areas with significant morbidity and mortality of geographical differences was analyzed. The morbidity and mortality rate gradually decreased by taking these counties around Taihang Mountain as the center and expanding to the periphery. This decline was negatively correlated with nitrosamine exposure, indicating that nitrates and amides in the environment may cause ESCA11,18. Nitrate and nitrite are the ubiquitous contaminants present in the environment, which can function as precursors for the formation of carcinogenic N-nitrosamines when biogenic amines (mainly obtained from farm fertilizers) are present19,20. Nitrate, nitrite, amines, and amides enter shallow wells, ponds, rivers, and other water systems with surface runoff and soil penetration and can enter the human body to synthesize nitrosamines under certain conditions leading to the occurrence of ESCA 21 . In addition, due to the long-time limited safety water supply system of Taihang Mountain, people have to rely on unsanitary surface water, which is considered another vital source of nitrosamine exposure 22 . At the same time, since 1970, ESCA has been found in chickens, sheep, and cattle in Taihang Mountain areas. Chinese scholars have proved the evidence of ESCA in chickens and mice caused by water pollution from farm fertilizers, suggesting that human ESCA and animal ESCA seem to have the same environmental risk factor 23 .
The natural nitrogen cycle, farmhouse fertilizers (human excreta), and moldy food all include microorganisms’ activities, which are closely related to meteorological factors such as temperature and humidity. Kusheng Wu et al. used a geographic information system (GIS) to collect climate variables such as annual average precipitation and evaporation in the past 30 years in China. They drew digital distribution maps to compare with the distribution of ESCA. The results showed that the drought index was positively correlated with ESCA mortality, and the environmental factors in the occurrence and development of ESCA cannot be underestimated24,25. Taihang Mountain areas are located in north latitude 35°12′~36°55′ to east longitude 112°~114°40′. Shexian has an average elevation of 1,000 m. More than half of the areas in Linzhou and Yangcheng are mountains with an altitude of more than 600 m, while the mountains, hills, and plains of Cixian each account for one-third of the areas 26 . The climate type of Taihang Mountain areas is a temperate monsoon climate with annual precipitation of about 700 mm, and annual precipitation/annual evaporation greater than 1, which is a mid-latitude semi-arid climate zone 24 . These climates are characterized by distinct dry and rainy seasons throughout the year, conforming to a semi-arid and semi-humid climate. After nitrate is formed, it penetrates the soil with water in an arid environment and then migrates with groundwater in a humid climate.
Excessively high nitrate content in the earth and the formation of amides in human and animal excrement after alkylation, and the formation of nitrosamines and nitrosyl under certain conditions, are the inducement for the high incidence of esophageal cancer. The semi-arid and semi-humid climate in the Taihang Mountains areas has expanded the impact of these substances on people, thereby increasing the incidence of esophageal cancer. Compared with other high-incidence areas of esophageal cancer in the world, such as Kenya in Africa and Iran in Asia, neither meets the above conditions simultaneously27,28. It is speculated that there may be other environmental factors affecting the high incidence of esophageal cancer in these areas.
Dietary Factors With High Incidence of ESCA in the Taihang Mountain Areas
Some evidence showed that ESCA risk is significantly different between urban and rural areas and is related to economic status, suggesting that risk factors related to lifestyle and environmental factors have different effects on ESCA (Table 2). Taihang Mountain areas have an average elevation of 1,200 m, with many mountains, extremely inconvenient transportation, low rainfall, and dry climate, so material resources are scarce. The people’s living conditions are difficult, which formed the traditional diet that people eat roughage most often but lack fresh vegetables and fruits 40 . Vegetables and fruits are rich in dietary fiber and a variety of micronutrients that offer health benefits. It is not only a sign of a well-balanced diet but also negatively correlated with many diseases. A study has shown that lower consumption of fresh vegetables and fruits is a risk factor for ESCA, while modifying the nutritional model can effectively reduce the prevalence of ESCA 41 . Scientists from the National Cancer Institute and the Cancer Institute of the Chinese Academy of Medical Sciences jointly launched a nutritional intervention experiment in the Taihang Mountain areas to reduce the incidence and mortality of ESCA. In 6 years, 29,584 adults have been supplemented with 26 vitamins and minerals. The results show that supplementation of vitamins, β-carotene, selenium, and other substances in people below 55 years of age can reduce ESCA mortality by 17% [hazard ratio (HR) = 0.83, 95% confidence interval (CI) = 0.71–0.98; P = 0.025]. Beneficial effects can still be observed 10 years after stopping the supplement 42 . The above illustrated the importance of vitamin supplementation for the occurrence and development of ESCA and provided ideas for the prevention and treatment of ESCA.
Environmental, Nutritional, and Behavioral Factors in Esophageal Cancer in the World.

ESCA: esophageal cancer.
Due to the severe water shortage, the residents near the Taihang Mountain areas mainly feed on dry field crops and fewer fresh vegetables, so pickles that are easy to preserve have become a traditional eating habit. A large amount of salt is always added in the processing of making pickles, and impurities in salt will readily produce a lot of harmful substances such as nitrosamines during the production and storage process. Meanwhile, high-salt food will destroy the natural barrier of the digestive tract, accelerate the absorption of nitrosamines, and increase the susceptibility of humans to carcinogens 43 . In addition, by analyzing the extracts of common pickled vegetables in the Taihang Mountain areas, it was found that long-term feeding of pickled vegetables in rats can lead to hyperkeratosis and dysplasia of esophageal epithelial cells. The findings support the presence of mutagenic and potentially carcinogenic substances in pickled vegetables 44 . Twofold increased risk of ESCA associated with the intake of pickled vegetables and the concentration of nitroso in pickles are higher than the samples from low-incidence areas according to the meta-analysis from Islami et al. 39 In addition, a cohort study from the Netherlands showed that consumption of processed meat increases the risk of ESCA in men 45 . In addition, nitrous acid substances can synthesize N-nitroso compounds and polycyclic hydrocarbons with secondary amines in meat, which can lead to the occurrence of digestive tract tumors 46 . The Working Group of the International Agency for Research on Cancer (IARC) has classified the edible processed meats as carcinogenic to humans (Group 1), which is based on the past results of some scientific literature and epidemiology data 47 .
Furthermore, a worldwide meta-analysis of data suggests that both tea and coffee are risk factors for ESCA 33 . Local eating habits (such as drinking scalding tea, boiled water and soup, and fast feeding speed) cause the high incidence of ESCA that is not to be ignored 38 . Data from Taiwan indicate that drinking drinks that are too hot increases the risk of ESCA 34 . A case-control study of ESCA in Taihang Mountain areas showed that bad eating habits such as eating overnight food, eating too fast, and eating hot food were all risk factors of ESCA in the Taihang Mountain areas 48 . The Chinese have a tradition of drinking tea. Active ingredients of green tea include tea polyphenols, most of which are flavonoids, which account for about 30% to 40% of the extractable solids of dry green tea, and have been proven to be the prevention factor for cancer 36 . However, some prospective studies have proved that the bad habit of drinking high-temperature tea in the Taihang Mountain areas is regarded as a defined factor that increases the risk of ESCA. In addition, drinking high-temperature tea has a synergistic effect with smoking and excessive drinking consumption in increasing the risk of ESCA 37 .
Poor Oral Health in ESCA
Poor oral health, including tooth loss, dental fluorosis, low tooth brushing frequency, and poor periodontal health, is a potential risk factor for ESCA (Table 2). However, few conclusions have been seen from epidemiological studies investigating a possible link between global oral health and ESCA. In addition, like other cavity organs of the digestive system, the esophagus provides a potential environment for microbial colonization, but little is known about the exact significance and nature of the bacterial microbial population present in the esophagus. In recent years, the Human Microbiome Project and the development of high-throughput sequencing of the human microbiome have provided direct evidence for the relationship between the microbiome and human health. Some studies have shown that the abundance of microorganisms in different organs may be related to the occurrence and development of ESCA 2 . Data from both case-control studies and cohort studies show a significant association between oral problems and ESCA in developing countries, including China, India, Iran, and Kenya. People who lose teeth have an approximately 1.5-fold increased risk of developing ESCA49–51. Results of a prospective 5.25-year study in Linxian County showed a significant association between tooth loss and ESCA risk (95% confidence interval, 1.1–1.6). Researchers speculate that this may be related to secondary metabolites such as acetaldehyde, active nitrate, and nitrite produced by the oral microflora 49 . Another study compared the pseudomonas gingiva and normal esophageal tissue conditions in ESCA patients and found that the pseudomonas gingiva infections were positively correlated with the disease stage, degree of differentiation, distant metastasis, and total survival rate of patients with ESCA 52 . In addition, data from the Taihang Mountain areas showed that porphyromonas gingivalis infection was associated with lymph node metastasis, tumor stage, chemotherapy resistance, and a lower 5-year survival rate in patients with ESCA 53 .
Factors With Tobacco, Alcohol, and the Sex in ESCA
In Western countries, most ESCA cases are observed in male and are strongly associated with tobacco use and high-degree spirits consumption (Table 2) 31 . In the world, the incidence of esophageal cancer is very high among men, and the difference in morbidity and mortality between men and women is 2 to 3 times 30 . In East Asia, most of the ESCA cases with risk factors for drinking and smoking are men, which could explain the gender difference in ESCA incidence 29 . In a case-control study based on the population of Taihang Mountain areas, information about dietary factors, alcohol consumption, and smoking was collected using an effective food frequency questionnaire. The results showed that the combination of smoking and drinking increased the risk of ESCA 54 . Interaction analysis showed that tobacco smoke has a toxic effect on the esophageal epithelium and is significantly related to the DNA damage of the patient’s esophageal epithelium (P < 0.01). Smoking not only plays a role in inducing DNA damage to the esophageal mucosa but also causes relaxation of the lower esophageal sphincter and increases the risk of gastroesophageal reflux, which can also cause damage to the esophageal mucosa55,56. A case-control study found evidence of an association between frequent smoking and increased Barrett’s esophagus risk. Accumulation of exposure to cigarette smoke can increase the risk of esophageal adenocarcinoma. At the same time, their results showed that smoking might be strongly associated with Barrett’s esophagus in men, which indicates that smoking has gender differences in the pathogenesis of ESCA 35 . A 15-year prospective study of the general population in Lin County found that cigarette smoking and pipe smoking are risk factors for upper gastrointestinal tumors, including esophageal cancer 12 . Smoking has become a consensus in recent years that a large number of carcinogens in tobacco smoke, such as polyaromatic hydrocarbons and nitrosamines, can promote the formation of tumors in various organs.
In parallel, drinking has various effects on ESCC, mainly reflected in the degree and dose of drinking. Slight alcohol consumption increases the risk of ESCC meanwhile rapidly growing risk associated with dose 57 . Acetaldehyde, a major metabolite of ethanol and one of the components of cigarette smoke, is believed to have a carcinogenic effect, mainly controlled by the ALDH2-encoding enzyme. It has been reported in several kinds of literature that polymorphisms of ALDH2 and ADH1B alleles play a vital role in the pathogenesis of ESCA 58 . A cohort study based on Chinese alcohol consumption and ESCA showed that low activity of ALDH2 was associated with an increased risk of esophageal cancer in male heavy alcohol consumers (30 g/d) 59 . In the meta-analysis by Bagnardi et al. 57 , alcohol consumption was positively dose-response with esophageal squamous cell carcinoma [light drinking RR 1.26 (1.06–1.50), moderate drinking RR 2.23 (1.87–2.65), and heavy drinking RR 4.95 (3.86–6.34)]. However, there is no direct evidence to show that alcohol consumption is a high-risk factor for ESCA in Taihang Mountain areas 32 . We can further explore the weight of alcohol consumption in the occurrence of ESCA in Taihang Mountain areas under the influence of various factors.
Family Genetic Susceptibility of ESCA
Although the high incidence of familial esophageal cancer cannot be ruled out due to the patients’ relatives’ everyday exposure to specific environmental factors or similar dietary habits, it has to be suspect that these patients and their families share a common genetic background. The people of the Taihang Mountain area migrated to the Chaoshan area of Guangdong due to historical factors. Y chromosome polymorphism analysis and mtDNA haplogroups analysis confirm that the populations of the two places have a common genetic background 60 . But the incidence of ESCA is still very high for people who migrate from high-incidence areas to low-incidence areas, such as the descendants of Henan and Shanxi immigrants on Nan’ao Island in Guangdong Province. It also cannot explain the migration of people living in low-incidence areas such as Shangqiu, Henan. People in areas with relatively high incidence rates, such as Dongxihu District of Wuhan City, still have low incidence rates 61 . Therefore, there are endless disputes about the reasons for ESCA, the influence of environmental and genetic factors. Through familial correlation analysis of Chaoshan and Taihang populations using the FPMM program of S.A.G.E., we found that in some large families, the best models of genetic susceptibility to esophageal cancer were autosomal dominant patterns and dominant or recessive significant genes with polygenic inheritance 62 . All evidence accumulated to date strongly suggests the role of genetic predisposition in ESCA development in Taihang Mountain areas. Collectively, this suggested that genetic predisposition plays an essential role in the development of ESCA.
Genome-wide association (GWAS) mainly uses single-nucleotide polymorphism (SNP) in the genome as molecular genetic markers to conduct genome-wide control analysis or correlation analysis. The development of GWAS has deepened our understanding of tumorigenic genes in recent years. A GWAS analysis of 10,158 patients and 21,062 controls in European people indicated that polymorphisms near TBX5 and GDF7 are related to the increased risk of Barrett’s esophagus, which is a significant risk factor for EADC 63 . Another GWAS analysis of EADC cases in Western Europe, Australia, and North America over the past 30 years showed the polymorphism of 19p13 in CRTC1, 9q22 in BARX1, and 3p14 in FOXP1 was significantly related to the incidence of EADC. Activating of the CRTC1 signaling pathway promotes the cancer cell migration and invasion and is associated with tumor metastasis; BARX1 participates in the differentiation of the esophagus and trachea and is associated with the downregulation of Wnt pathway activity; FOXP1 is overexpressed in esophageal cancer 64 .
The results of a case-control study showed that compared with the control group, people with a family history of ESCA had a higher risk of ESCA, and the prevalence has increased by 60% to 80% 32 . Li-Dong Wang et al. compared more than 5,000 cases of ESCA in the Chinese population through GWAS. They found new susceptible gene loci of ALDH2 and ADH1B, particularly in the high-risk ESCA population in Taihang Mountain areas 65 . Another study showed that patients with a family history of ESCA had a significantly earlier age of onset than patients with sporadic ESCA and had worse survival rates and prognosis and more significant differences in disease stages (the difference was statistically significant, P < 0.05) 66 . A genomic DNA analysis of peripheral blood from 117 ESCA patients showed that MSH2 c.2063 G allele and WRN c.4330 C allele are the risk factors of ESCA compared with healthy individuals who had been screened and had no history of cancer 67 . Moreover, aldehyde dehydrogenase 2 (ALDH2) and alcohol dehydrogenase (ADH) encode enzymes that can eliminate acetaldehyde, which is related to the progression of ESCA, and its metabolites were considered as carcinogens of ESCA 68 . From this point of view, carcinogenic environmental factors and genetic factors do not conflict, and up to now, all evidence points to the influence of high genetic susceptibility in high-risk areas like Taihang Mountain areas. The long-term effects of environmental factors will be transformed into the cancer risk of the population through a variety of genetic factors (such as methylation, and accumulation, and inheritance).
Associated Infection of ESCA
Helicobacter pylori
Studies have shown that the colonization of Helicobacter pylori in the stomach is a proposed protective factor for EADC, mostly seen in the infection of CagA-positive strain. The mechanism is that the infection reduces gastric acid secretion, leading to gastric atrophy and thereby reducing the risk of gastroesophageal reflux 69 . Helicobacter pylori infection has been shown to be an important factor in distal gastric cancer, but has not been found with the ESCC correlation in multiple studies69,70. A meta-analysis based on the association between H pylori infection and CagA-positive H pylori strains was not significantly associated with ESCA; even a negative correlation was found between CagA-positive H pylori strains and ESCA in Asian populations 71 . However, based on the study of Taiwan, China, the positive correlation of H pylori is shown to induce the rupture of the DNA chain of NE3 cells (esophageal epithelial cells), which can affect the increased instability of the genome and improve the risk of esophageal epithelial cell cancer72,73. In a study on ESCC and H pylori, it was found that the infection rate of H pylori in the ESCC tissues was significantly higher than that in the adjacent tissues (62.5% vs 26.7%) in the high-incidence areas of ESCA in northern China 72 . Another prospective study found that multiple seropositivity for H pylori was associated with an increased risk of gastric non-cardia cancer (GNCA). The relationship between H pylori infection and ESCA seems to be controversial, so large-scale prospective studies are needed in the future to clarify the role of H pylori and the mechanism of ESCA.
Epstein-Barr Virus
The association between Epstein-Barr virus (EBV) and ESCA is ambiguous. Existing studies have provided diametrically opposed results for the two associations, which different EBV detection methods may cause. Using the real-time quantitative polymerase chain reaction (RT-PCR) method to detect EBV, the presence of EBV lymphocytes in the human body will increase the false-positive rate of the results 74 . While the immunohistochemical method for EBV positive detection is specific, the disadvantage is that the low viral load sensitivity is low. The results often show no correlation between the two75,76. Whether EBV infection can be used as clinical immunotherapy or adjuvant cytotoxic therapy is still controversial. At present, there is no reliable evidence to prove that EBV infection is related to the ESCA incidence in Taihang Mountain areas. A study found that 51 cases of ESCA tissues in the high-risk areas were tested and found that all cases were negative for EBV in situ hybridization and PCR 77 .
Human Papillomavirus
Compared with EBV, human papillomavirus (HPV) research is multidirectional. Studies have shown a strong association between the occurrence of EADC and HPV-BD (Barrett’s esophagus dysplasia)-EADC sequence, and increased transcriptionally active HPV load is related to the severity of BD and EADC 78 . Exon sequencing analysis of HPV-positive/negative ESCA patients found that HPV-positive and HPV-negative patients had significant differences in the genome, suggesting that the biological mechanisms of esophageal cancer formation are different. HPV may induce the inactivation of the TP53 gene through E6 structure, loss of regulation of the cell cycle, and promote tumor formation 79 . A paper mentioned that the overall detection rate of HPV infection was 30.9%, after summarizing the worldwide 203 studies on the relationship between HPV and esophageal cancer published from 1982 to 2017. The high incidence of ESCA was associated with a high HPV infection rate, and most of them were HPV16 and 18 subtypes 80 . A retrospective analysis study around the Taihang Mountain areas found that high-risk HPV accounted for more than 90% of HPV-positive lesions in esophageal and cervical tissue. High-risk HPV infection increases the prevalence of ESCA fourfold 81 . However, the results of another cross-sectional study of ESCA and HPV infection in high-risk areas showed that high-risk HPV infection was not detected in patients with ESCA, while high-risk HPV infection was detected in both normal individuals and individuals with precancerous lesions. Infect 82 . HPV infection is common in ESCA independent of region and ethnic group of origin. Therefore, further studies are warranted to determine whether high-risk HPV infection plays a key role in the etiology of high-risk areas of ESCA.
Medical Research Based on Internet Medical Treatment Will Be a New Trend in the Field of ESCA Prevention and Treatment
Early Screening, Diagnosis, and Treatment of ESCA
At present, there is no unified early screening model and early diagnosis and treatment standard for ESCA in the world. A perfect screening mechanism and accurate screening methods guarantee early detection and early diagnosis and are also effective measures to improve the prognosis of ESCA. After fully understanding the causes of the high familial incidence of ESCA in the Taihang Mountain areas of China, it will help to carry out prospective studies on the high incidence of familial cancer and help promote the implementation of relevant measures to reduce the incidence and mortality of ESCA.
Because of the current status of ESCA in China, the best screening plan is to directly carry out endoscopy with iodine staining and indicative biopsy pathological screening of the target population. This method is currently the most applicable and effective method for completing screening and diagnosis at one time, with high sensitivity and accuracy, which can transform ESCA from late treatment to early prevention and treatment. Deciduous cytology screening and liquid biopsy techniques have been used for many years in areas with a high incidence of ESCA and can detect multiple esophageal precancerous lesions. The fact that the survival rate of patients in high-incidence areas was significantly lower than that of patients in low-incidence areas reminds the government needs to strengthen effective tumor prevention and treatment for residents in high-incidence areas, improve the quality of drinking water and diet, and perform esophageal endoscopy on people with family history as soon as possible to reduce morbidity and mortality of ESCA effectively 83 . Yang et al. developed a model that can identify people at high risk for ESCA. This model in screening allows 16.6% of the sample to avoid endoscopy without missing precancerous lesions 84 . Another prospective study on the Chinese population showed that people over 50 need to be screened for inner diameter in high-risk areas. The re-examination time for moderate dysplasia (MD) and mild dysplasia under endoscopy is different for 3 and 5 years 85 . In the future, we can expand the number and scope of samples and develop ESCA screening models that can be applied nationwide.
Furthermore, the occurrence of ESCA usually undergoes a process from gene mutation to cell mutation and then to tissue mutation. For example, ERCC2 and ERCC4 gene mutations can be used as predictors of TNM staging of ESCA and further survival predictors of ESCA 86 . As a precancer warning, genetic variation is the best preventive intervention period. Applying molecular biology technology to screen for genomic mutations related to esophageal cancer can improve the accuracy and specificity of early diagnosis. Therefore, future prospective studies can be conducted on familial susceptibility genes to determine whether they can be used as diagnostic markers for familial ESCA to achieve early cancer screening.
Possible Methods to Improve the Diagnosis and Prognosis of Familial ESCA
Due to the long interval between ESCA onset in different generations of patients, it is difficult to obtain clinical data, pathological information, and treatment information. Therefore, ESCA’s relevant research progress in the Taihang Mountain areas is slow for a long time in the past. At present, scholars in Taihang Mountain areas have established a clinical case information database and sample database for familial ESCA and actively developed a new Internet medical model, enabling doctors to conduct remote diagnosis and treatment, remote consultation, and remote follow-up for patients. Meanwhile, Internet medicine can establish the mechanism of the “environment-diet-heredity-environment” of ESCA by using existing data, obtain the change of critical factors through multigroup studies, and carry out association analysis with clinical data 87 . Using this biological calculation model to screen out the molecular model of the high-risk population of ESCA will provide early screening criteria for the high-risk population, which can effectively prevent and control the occurrence of ESCA. At present, the development of the Internet in China has entered the era of product interconnection. Mobile apps are closely integrated with the medical, appearing producing “handheld hospital,” smart diagnostic guides, and other software to help patients registered in advance, pay medical expenses on mobile phones, and check the results of laboratory tests 88 .
In addition, the current wearable device can continuously monitor patients’ vital signs and was used for patients to complete self-collection of information at home and upload it to the network to realize information sharing with the health care sector, which is crucial for digital health. The mobile Internet development is paving the way for revolutionizing modern disease diagnosis and patient treatment monitoring. The popularization of wearable devices and telemedicine can identify specific disease patterns, better understand the disease, and monitor patients’ health status 89 . The information on high-risk groups should be collected, and those with changes in dietary habits, body weight, and vital signs should be screened through big data analysis to timely remind them to conduct digestive endoscopy examinations.
Conclusion
There are significant differences in epidemic characteristics, histological types, and risk factors of esophageal cancer between Chinese and Western populations. Squamous cell carcinoma is the primary tissue type of esophageal carcinoma in China, and the main risk factors are nitrosamine exposure, vitamin deficiency, and dietary habits. Esophageal adenocarcinoma is predominant in the Western population, and the main risk factors are obesity and reflux esophagitis. The epidemiological characteristics of esophageal cancer in China have noticeable regional distribution differences and apparent familial aggregation phenomenon. These results suggest that environmental and genetic factors play an essential role in the incidence of esophageal cancer in China. Accurately identifying high-risk patients based on epidemiological survey results in high-risk areas and implementing a census plan that meets cost-benefit evaluation is an effective guarantee for reducing ESCA incidence. Therefore, based on the epidemiological characteristics and actual cancer control situation in the Taihang Mountain area, it is recommended that local residents start endoscopic screening at the age of 50, improve their eating habits and diet structure, and the government improve the quality of drinking water, which can achieve better tumor prevention effect. Epidemiological studies on Taihang Mountain areas of ESCA can not only directly solve the main problems of tumor prevention and treatment in areas with increased incidence of ESCA in China, but also provide ideas for screening and early diagnosis in other areas with a high incidence of ESCA in the world.
Footnotes
Acknowledgements
The authors would like to acknowledge the contributions of specific colleagues, institutions, or agencies that aided the efforts of the authors.
Author Contributions
All authors contributed to the writing and editing of the manuscript and approved the final draft of the manuscript.
Ethical Approval
This study was approved by our institutional review board.
Statement of Human and Animal Rights
This article does not contain any studies with human or animal subjects.
Statement of Informed Consent
There are no human subjects in this article and informed consent is not applicable.
Data Availability Statement
All datasets generated for this study are included in the manuscript/supplementary files.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Collaborative Innovation Major Project of Zhengzhou (Grant No. 20XTZX08017), the National Natural Science Foundation of China (Grant No. 82002433), and Science and Technology Project of Henan Provincial Department of Education (Grant No. 18A320044, 21A320036), Young and Middle-aged Health Science and Technology Innovation Talents in 2020 (Grant No. YXKC2020049), Henan Province Medical Science and Technology Research Project Joint Construction Project (Grant No. LHGJ20190003, LHGJ20190055).
