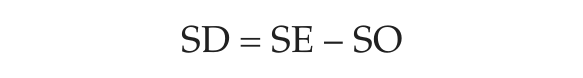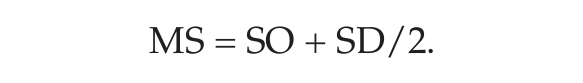Abstract
Sleep is systematically modulated by chronotype in day-workers. Therefore, investigations into how shift-work affects sleep, health, and cognition may provide more reliable insights if they consider individual circadian time (chronotype). The Munich ChronoType Questionnaire (MCTQ) is a useful tool for determining chronotype. It assesses chronotype based on sleep behavior, specifically on the local time of mid-sleep on free days corrected for sleep debt accumulated over the workweek (MSFsc). Because the original MCTQ addresses people working standard hours, we developed an extended version that accommodates shift-work (MCTQShift). We first present the validation of this new version with daily sleep logs (n = 52) and actimetry (n = 27). Next, we evaluated 371 MCTQShift entries of shift-workers (rotating through 8-h shifts starting at 0600 h, 1400 h, and 2200 h). Our results support experimental findings showing that sleep is difficult to initiate and to maintain under the constraints of shift-work. Sleep times are remarkably stable on free days (on average between midnight and 0900 h), so that chronotype of shift-workers can be assessed by means of MSF—similar to that of day-workers. Sleep times on free-days are, however, slightly influenced by the preceding shift (displacements <1 h), which are smallest after evening shifts. We therefore chose this shift-specific mid-sleep time (MSFE) to assess chronotype in shift-workers. The distribution of MSFE in our sample is identical to that of MSF in day-workers. We propose conversion algorithms for chronotyping shift-workers whose schedules do not include free days after evening shifts.
In individuals without socioeconomic obligations, the timing of sleep shows a characteristic relationship to the light-dark cycle (Roenneberg et al., 2007b). Around the equinoxes, for example, individuals fall asleep several hours after dusk and awake around dawn. Like most organisms, humans synchronize their internal, circadian clock to the 24-h rotation of the earth. In humans (like in other mammals), the pacemaker of the circadian system is located in the suprachiasmatic nuclei (SCN; Antle and Silver, 2005; Reppert and Weaver, 2002). Yet, individuals vary in how their circadian clock synchronizes to the light-dark cycle (phase of entrainment, Roenneberg et al., 2003a, 2010), with early chronotypes showing an advanced entrained phase compared with late chronotypes.
The Munich ChronoType Questionnaire (MCTQ; introduced by Roenneberg et al., 2003b; see http://www.theWeP.org) assesses chronotype based on sleep behavior. The MCTQ consists of simple questions about sleep timing (separately on work and free days), allowing the computation of its key parameters: mid-sleep (the midpoint between sleep onset and offset) and sleep duration (SD). To avoid contamination of social influences as much as possible, we assess chronotype based on mid-sleep on free days (MSF), excluding individuals who use alarm clocks or cannot wake up voluntarily (e.g., disturbed by children or pets). MSF shows high test-retest reliability (Kuehnle, 2006) and correlates strongly with sleep logs, wrist actimetry (Kantermann et al., 2007; Kuehnle, 2006), and physiological rhythms. Martin and Eastman (2002) found that mid-sleep on days free of social constraints accurately predicts dim-light melatonin onset (DLMO), even when the sleep schedules are irregular (see also Burgess and Eastman, 2005). A validation of the MCTQ-based MSFsc as a reliable marker of phase of entrainment with physiological measures is lacking but is currently in preparation.
In general, sleep timing and sleep duration are considered independent in humans (Roenneberg et al., 2005), yet sleep can differ considerably between workdays and free days (National Sleep Foundation, 2002; Groeger et al., 2004; Kronholm et al., 2006; Roenneberg et al., 2007a): the later mid-sleep on free days (MSF), the shorter workday sleep, and the longer sleep on free days (Roenneberg et al., 2007a). Sleep timing and duration are also chronotype-specific on workdays; the late third of the population falls asleep almost 2 h after the early third but sleeps only 30 min longer into the morning. Late types are therefore systematically sleep deprived during the workweek (Roenneberg et al., 2003b) and consequently “over”-sleep on free days, thereby delaying their mid-sleep time. To control for this sleep compensation, MSF is corrected for "oversleep" (MSFsc, see MCTQShift). MSFsc has a slightly skewed distribution with an overrepresentation of late types. MSFsc is a continuous variable (like MSF; Roenneberg, 2012) but can be grouped into distinct categories for practical reasons (e.g., early types: MSFsc ≤3:59; intermediate types: MSFsc = 4:00-4:59; late types: MSFsc ≥5:00; the exact limits depend on population).
Having so far accumulated entries by more than 150,000 people across the world, the MCTQ has been a useful tool in capturing human sleep-wake demographics and in monitoring chronotype across the life span as well as in different seasons and geographical locations (e.g., Kantermann et al., 2007; Roenneberg, 2012; Roenneberg et al., 2007b, 2003a). Yet, these findings are based on individuals who work “normal” hours. How chronotype and sleep-wake behavior interact with work times in shift-workers could so far not be reliably investigated with the standard version of the MCTQ since it does not accommodate answers for irregular work schedules.
To allow chronotyping in shift-workers, we developed a shift-work version of the Munich ChronoType Questionnaire (MCTQShift) that expands its questions for individuals working in (changing/rotating) shifts. First, we validated MCTQShift-assessed mid-sleep and sleep duration with daily sleep logs in a sample of 52 shift-workers as well as with actimetry-derived sleep and wake behavior in a subsample of 27 shift-workers (all participants worked in rotating schedules). Second, we explored MCTQShift-assessed mid-sleep and sleep duration in 371 shift-workers. Again, all participants were employed in rotating shift schedules comprising morning, evening, and night shifts (transition times: 0600 h, 1400 h, and 2200 h).
As a reliable phase marker for chronotype in shift-workers, MSF should remain as stable as possible across shifts, that is, with sleep times between 0030 h and 0845 h as described for day-workers (Roenneberg et al., 2007a). If MSF differed significantly between shifts, the least affected MSF would be the best choice, since this suggests that an individual can most likely sleep within his or her “circadian sleep window” and accumulates the least sleep deprivation during the preceding workdays. On the basis of this analysis, we propose a procedure to chronotype shift-workers.
To accommodate the complex nature of the data sets, we split the methods and results sections in two: first, we cover the validation of the MCTQShift parameters and then focus on the procedure to assess chronotype in shift-workers. The results of both parts are discussed in a common section.
The MCTQShift
The MCTQShift (see supplementary online material, Suppl. Fig. S1) applies the standard MCTQ items (workdays, labeled W, and free days, labeled F) separately to the morning (M), evening (E), and night (N) shift (in reference to sleep onset being either before a workday or a free day). As for the standard MCTQ, items guide the participant step-by-step through the process of going to bed to getting up (accompanied by images).
The following variables are assessed: bedtime (item 1/image 1); image 2 is merely a reminder of potential “in-bed” activities before preparing for sleep; time of preparing to fall asleep (item 2/image 3), sleep latency (item 3/image 4), time of awakening and whether this occurred with or without the use of an alarm clock (item 4/image 5), and time to get up (item 5/image 6). Also, participants indicate whether they cannot freely choose their sleep times on free days. Note that all abbreviations, descriptions, and calculations of the variables are given in the supplementary online material, which can thus be used as a glossary.
As in the standard MCTQ, this set of items allows the computation of sleep onset (SO = time of preparing to fall asleep + sleep latency) and sleep end (SE = time of awakening). SO and SE are the basis for calculating sleep duration (SD) and mid-sleep (MS):
These are separately computed for workdays and free days (SDW and SDF; MSW and MSF). While the standard MCTQ only differentiates workdays and free days for a standard workweek, the MCTQShift allows collection of information for sleep on different shifts (e.g., mid-sleep on workdays, MSWM/E/N for M: morning, E: evening, and N: night shift) and on their subsequent free days (MSFM/E/N). Analogously, SDW and SDF are calculated in a shift-specific way (SDFM/E/N). While ØSD represents the weighted average of sleep duration for work and free days over the course of a standard week, the weighting of ØSD in the MCTQShift is based on the respective shift schedule. Thus, an exact knowledge of work schedules for each shift-worker is crucial to evaluate this questionnaire (see supplementary online material, Evaluation of the MCTQShift).
The weekly average sleep duration (ØSD) is calculated by considering the number of respective workdays and free days: ØSD = (Nworkdays * SDW + Nfree-days * SDF)/7. In day-workers, chronotype is assessed using MSF (see above) corrected for “oversleep”(sc = sleep corrected): MSFsc = MSF – (SDF – ØSD)/2.
A procedure to assess chronotype by the MCTQShift is proposed in the second part of this article (see the section Assessing Chronotype With the MCTQShift).
The MCTQ allows for the assessment of numerous additional variables that are not part of this article. For an overview of these, see the supplementary online material of Roenneberg et al. (2012).
Validating the Key Parameters of the MCTQShift by Actimetry and Sleep Logs: Mid-Sleep and Sleep Duration
Before proposing a procedure to chronotype workers employed in rotational shift schedules, we validated the MCTQShift-derived variables mid-sleep and sleep duration in a subsample of shift-workers, by actimetry and sleep logs. Given that the MCTQShift is a one-time assessment of sleep-wake behavior, a validation with continuous (daily) assessment methods, such as sleep logs and actimetry, is necessary to evaluate the validity of the generalized answers reported in the questionnaire, a procedure that is standard for assessing this type of questionnaires (e.g. Monk et al., 2003).
Validation Methods
Participants
Fifty-two participants (26 males and 26 females; mean age = 32.5 years, range 21-50 years) from a manufacturing plant in Germany filled out the MCTQShift and kept daily sleep logs. Of these, 27 (16 women, 11 men; mean age = 30.98 years, range 21-50 years) also wore wrist actimeters. All participants worked in a weekly, forward-rotating 3-shift model (see Suppl. Fig. S2). We omitted the split weeks to compare similar lengths of workdays and free days in the sleep log and activity recordings from our analyses.
Participants were thoroughly briefed before the study and gave their informed consent (according to the Declaration of Helsinki, last updated in Seoul, 2009). The study was approved by the ethics committee of the Psychology Department at the Ludwig-Maximilian-University of Munich, Germany.
Instruments
Wrist actimetry and sleep logs
Both sleep logs and wrist actimeters were distributed at the workplace, after participants filled out the MCTQShift, in June 2008. Sleep logs assessed the following items (similar to MCTQ): time of preparing to fall asleep, minutes required to fall asleep (sleep latency), time of awakening, and use of alarm clocks, as well as whether the respective day at wake-up was a free day or a workday (morning, evening, or night shift). These variables were used to calculate the day-specific sleep onset (SO), sleep end (SE), mid-sleep (MS), and sleep duration (SD).
Sleep bouts were coded as work or free days, according to the relative impact of the work schedule: sleep before morning shifts is influenced by the upcoming shift, thereby coded as a workday (associated with the prior shift). The reverse is true for evening and night shifts: here, individuals cannot freely choose their sleep times after the respective shifts, so the last sleep bout after one of those was still coded as a workday sleep. Yet, sleep before evening and night shifts is hardly influenced by the subsequent schedule, so it is coded as free day sleep. Participants were asked to keep sleep logs on a daily basis, right after wake-up for the entire study period. For this study, we only considered main sleep episodes and not naps.
For an objective assessment of sleep-wake behavior, we recorded locomotor activity with a wrist-worn device (weight: 21 g, dimensions: 40 mm × 44 mm × 12 mm; Daqtometer, Daqtix GmbH, Oelzen, Germany). Participants wore the actimeters continuously over the 5-week study period. Activity was sampled every second and stored in 10-sec intervals, and the data were subsequently binned in 10-min intervals for data analyses. Day types (e.g., free day, workday, and shift-schedule) were categorized according to the sleep log information. In case participants took off the device, they were asked to enter time and date into a protocol; these times were later marked as missing data.
Data Processing
Sleep logs
For the computation of mid-sleep and sleep duration, we averaged across 4 workdays per shift, obtaining mean MSW and SDW for the morning shift (MSWM/SDWM), evening shift (MSWE/SDWE), and night shift (MSWN/SDWN) and for 2 free days after each shift (potential excess free days were not included in the shift-specific free-day analysis), resulting in MSF and SDF for the shift-specific free days (MSFM,E,N/SDFM,E,N).
Wrist actimetry
We used the daily actimetry profiles to compute sleep onsets, offsets, and durations. Although these variables are commonly part of the standard software packages provided by actimeter companies, the underlying algorithms are commonly not declared. We therefore developed a simple method for detecting sleep onsets and offsets (and thereby sleep duration). The 4-h sleep episode (stored in 10-min bins) used to describe the procedure of the method below is a purely fictional example.
In a first step, activity time series were first digitized according to a selectable threshold (generally 20% of the 24-h mean) yielding a time series of “1s” and “0s” (1 representing activities below threshold, i.e., sleep, and 0 representing activities above threshold, i.e., awake). Sleep onsets and offsets were initially defined by three 10-min bins of activity below or above threshold (bold in the example below). Since activity can occasionally rise above threshold even during sleep, the following binary series for the fictional 3-h sleep episode may look like this: 0000
To detect consolidated sleep episodes, we therefore applied—in a second step—a method that aims to distinguish between movement during sleep and actual sleep interruptions: the binary sleep episode identified in the first step was correlated with a series of binary masks containing an increasing number of 1s, starting at sleep onset, filling up the rest of the sleep episode with 0s:
1: 000011100000000000000000000 2: 000011110000000000000000000 3: 000011111000000000000000000 … 24: 000011111111111111111111111
The mask that gave the highest correlation was then defined as a continuous sleep episode. In the example given above, this was the case when all 24 bins were filled with “1” (r = 0.714; extending 1 sec beyond gave lower correlation coefficients). Based on these activity-derived sleep onsets and offsets, MSFM,E,N and MSWM,EN were calculated in analogy to the computations described above.
Data Analysis
MCTQShift-derived mid-sleep and sleep duration were correlated to those based on sleep logs and actimetry, separately for each of the shift-specific work and free days. We report Spearman’s correlation coefficients (rho, rS) for the correspondence between sleep logs, actimetry, and the MCTQShift. Since we had an a priori hypothesis that the MCTQShift produces a good representation of sleep-wake behavior, significance levels are reported for 1-tailed distributions.
Validation Results
MCTQShift-derived mid-sleep times highly correlate with those assessed by sleep logs and actimetry (Table 1). So does the comparison of sleep duration between MCTQShift results and those derived from sleep logs and actimetry on workdays. Notably, free-day sleep duration assessed by actimetry did not correlate with that obtained by the MCTQShift.
Correlations between mid-sleep and sleep duration assessed by MCTQShift and the assessed sleep logs and actimetry.
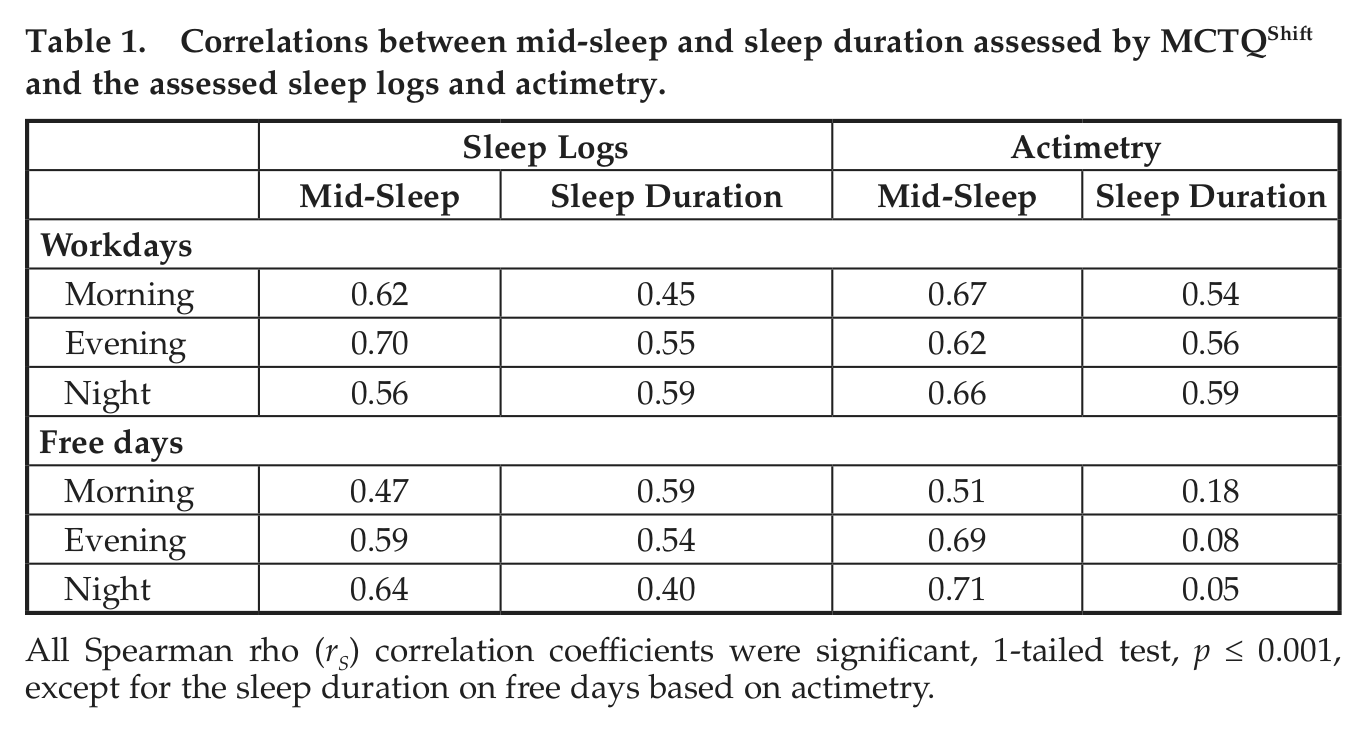
All Spearman rho (rS) correlation coefficients were significant, 1-tailed test, p ≤ 0.001, except for the sleep duration on free days based on actimetry.
Assessing Chronotype with the MCTQShift
Here, we report the descriptions of the main MCTQShift variables, collected in a sample of 371 shift-workers. Then, we propose a procedure for the assessment of chronotype in shift-workers, based on the results in the subsample of participants waking up on free days without alarm clocks.
Assessment Methods
Participants
The MCTQShift was filled out by 371 (111 women and 260 men; mean age 39.8 years; range 19-57 years) shift-workers from 4 manufacturing plants in Germany and Luxembourg, who worked in rotating, 3-shift schedules (transition times: 0600 h, 1400 h, and 2200 h). Of these, 55 rotated forward (M-E-N) in either a weekly (n = 32) or a 3-week (n = 23) rotation speed; 177 rotated backward (M-N-E) in either a weekly (n = 98) or a rapid (2-3 days) rotation (n = 79); 139 workers rotated forward in a weekly fashion, followed by 1 week of rapid backward rotations. Employees had their days off on different days of the week. Participants gave their informed consent according to the Declaration of Helsinki (last updated in Seoul, 2009). The ethics committee of the university approved the study.
Procedure
Between February 2006 and October 2008, participants filled out a paper version of the MCTQShift once, at the workplace or at home, including demographic information (e.g., age and gender) and information about their shift-work schedules (speed of rotation, e.g., fast: 2-3 days or slow: 5-7 days; direction of rotation: forward or backward; relative occurrence of work and free days).
Data Analyses
Based on the MCTQShift-assessed sleep onset (SO) and sleep end (SE), we computed mid-sleep (MS) and sleep duration (SD) for work and for free days on the respective shifts (see the section The MCTQShift). First, we explored how sleep timing (mid-sleep) and sleep duration are influenced by the different shift schedules by computing a mixed-design analyses of variance (MANOVA, controlled for differences in rotation speed and direction) for shift days and their respective free days. Due to missing data, sample sizes differed between variables (n = 289 up to 330 individuals); the sample sizes for each computation are reported within the tables.
Second, we investigated which shift affected sleep timing on free days least, but only in participants waking up voluntarily (e.g., without using an alarm clock; n = 178). As in day-workers, these individuals cannot be chronotyped. We compared this subgroup to the total population in terms of age and sex with a 1-way ANOVA as well as Pearson’s chi-square test.
If we assume no chronotype bias in individuals who do shift-work, their MSFsc times should show an identical distribution to that of day-workers (Z-test for independent samples). We have shown that chronotype systematically depends on longitude within a given time zone, being delayed by 4 min/longitude from east to west (Roenneberg et al., 2007b). To control for this geographical effect, we corrected chronotype of the workers in each study site to the average longitude of the population represented in the large MCTQ database (+9.18°) using the following equation:
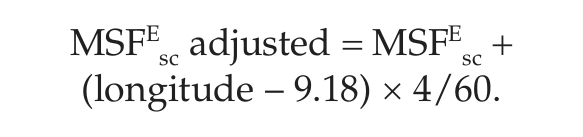
Unless reported otherwise, average values are given with their standard deviation.
Assessment Results
Descriptions: Mid-Sleep and Sleep Duration
Raw MCTQShift variables (time of preparing to fall asleep, sleep latency, time of awakening, and time to get up; see Suppl. Fig. S1) are shown in Table 2. To give an overview of the total population, we included all individuals in this table; we also included those who indicated to be woken up involuntarily (alarm clock or other disturbances). These were excluded from further analyses.
Parameters assessed by the MCTQShift.
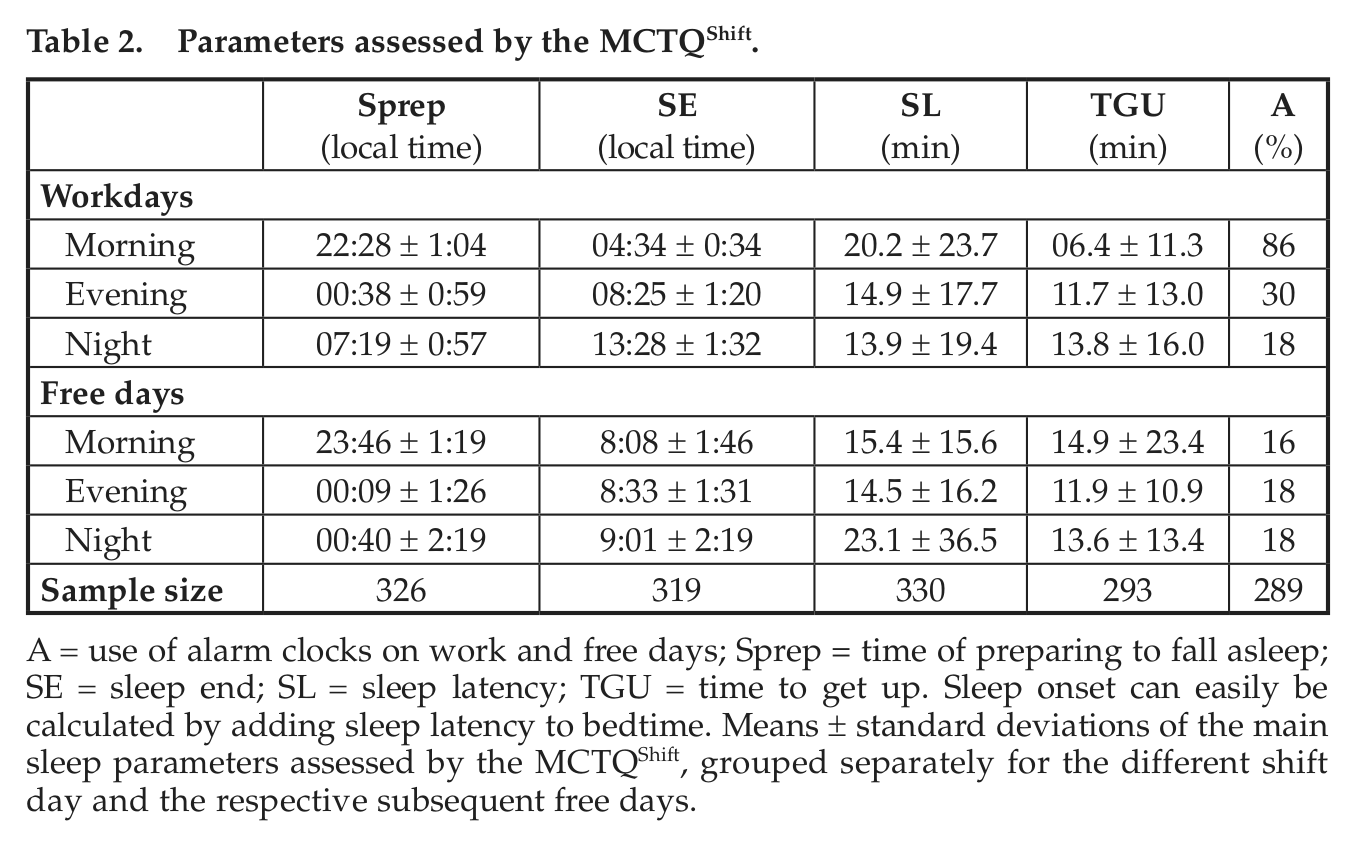
A = use of alarm clocks on work and free days; Sprep = time of preparing to fall asleep; SE = sleep end; SL = sleep latency; TGU = time to get up. Sleep onset can easily be calculated by adding sleep latency to bedtime. Means ± standard deviations of the main sleep parameters assessed by the MCTQShift, grouped separately for the different shift day and the respective subsequent free days.
To explore shift-workers’ timing and duration of sleep, we computed individual mid-sleep (MS) and sleep duration (SD), separately for work and free days, in each shift (see The MCTQShift section and Table 3). When controlled for the type of shift schedule (rotation speed and direction), the MANOVA showed that the 3 shifts differed significantly in MSW (F1.95, 642.46 = 7294.37, p ≤ 0.001), in MSF (F1.39, 463.67 = 29.91, p ≤ 0.001), and in SDW (F1.86, 607.97 = 118.59, p ≤ 0.001) but not in SDF (F1.78, 594.11 = 0.49, p = 0.59).
Key parameters of the MCTQShift: Mid-sleep and sleep duration.
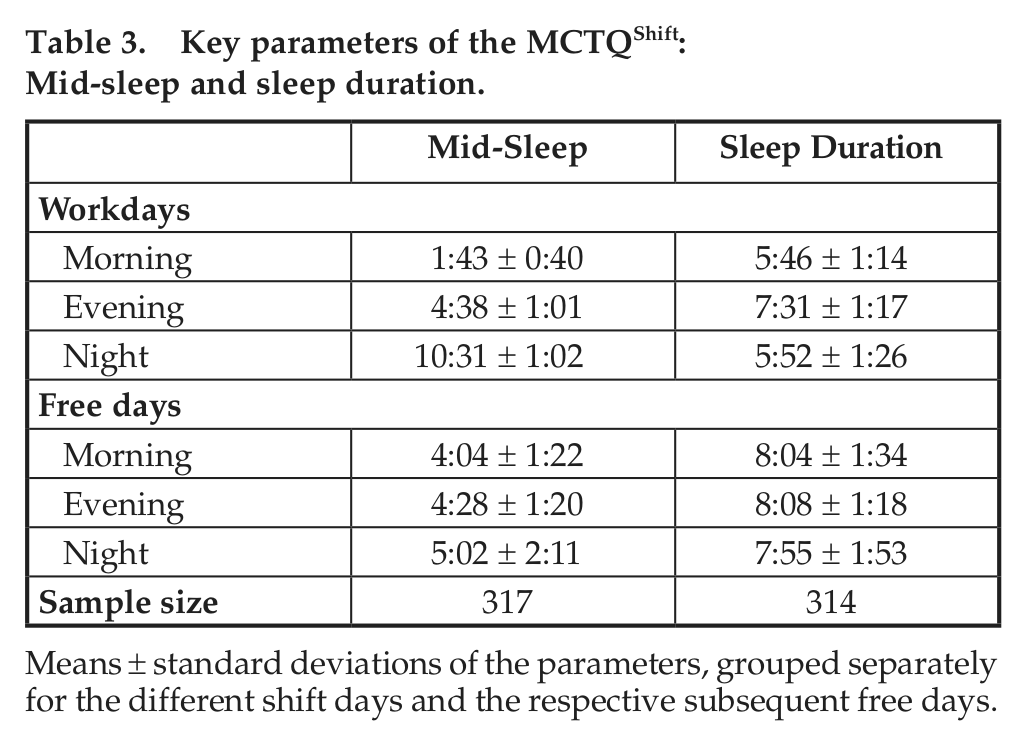
Means ± standard deviations of the parameters, grouped separately for the different shift days and the respective subsequent free days.
How to Assess Chronotype?
After we excluded workers who reported waking up involuntarily on free days following any shift, the sample consisted of 179 (63 women and 116 men; mean age 37.7 years; range 19-56 years). A 1-way ANOVA showed that the 2 samples (i.e., waking up with alarm on free days, n = 371, vs. no alarm on free days, n = 179) were significantly different in age (F1, 544 = 5.95, p ≤ 0.05) but not in sex (Pearson’s χ21, 550 = 1.54, p > 0.05). An effect size computation revealed that the factor “subgroup” only explains 0.1% (r = 0.01, effect size measure for 1-way ANOVAs) of the variance in the dependent variable age. Such an effect size is conventionally classified as a very small and therefore is negligible.
Although the sleep-corrected version of mid-sleep (MSFsc) is used for chronotyping, free-day sleep in real life includes “oversleep” (MSF). We therefore tested the shift-specific effects on MSF (the basis to calculate MSFsc) by a within-subject-design ANOVA. Preceding shifts had a small but significant effect on the respective MSF times (F1.42, 246.78 = 9.67, p ≤ 0.05, controlled for shift model, partial η2 = 0.05; Fig. 1).
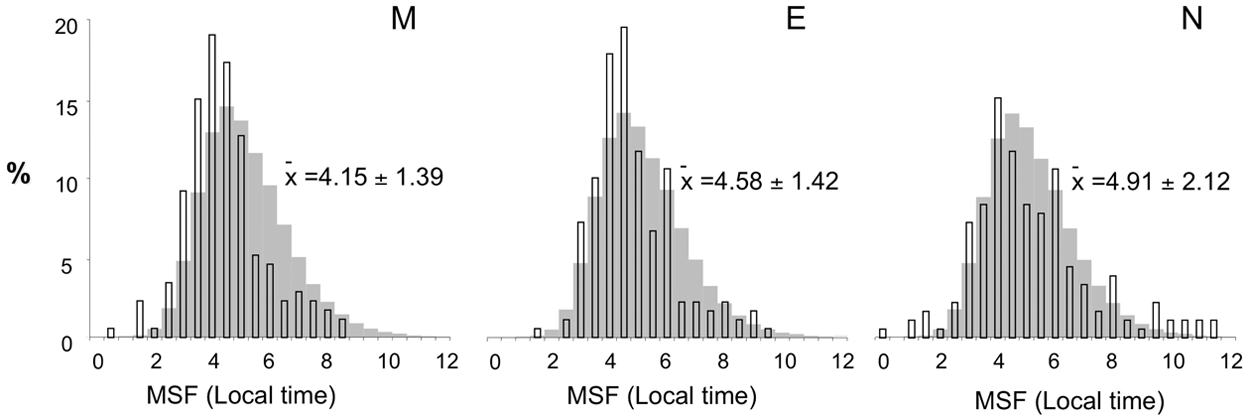
Distribution of mid-sleep on shift-specific free days. The graphs show the distribution of mid-sleep times on free days (MSF) after morning (M), evening (E), and night shifts (N) of 179 shift-workers (in half-hour bins with mean MSF ± standard deviation indicated to the right of each panel). The distribution of MSF in the non-shift-working German population is indicated in gray in each panel (sample size in the MCTQ database in 2010, N = 54.091; mean MSF: 4.86 ± 1.56)
MSW during and MSF after evening shifts (MSWE/MSFE) showed the best correlation both for rs (Spearman’s rho coefficient) and for slope (Fig. 2; we examined both to test for a 1:1 relationship). Since sleep during and after late shifts is least influenced by social constraints, this suggests that MSFE is the best candidate for chronotyping shift-workers.
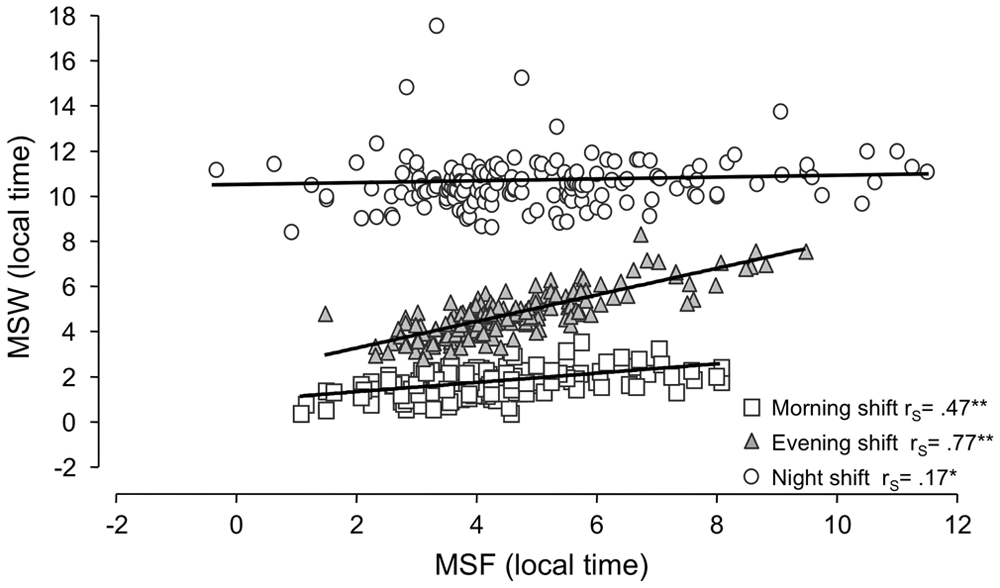
Mid-sleep on work and free days. The correlations between Mid-sleep on workdays (MSW) and on free days (MSF) depend on shift (morning shift: squares; slope = 0.21, rS = 0.47**; evening shift: triangles; slope = 0.59, rS = 0.77**; night shift: circles; slope = 0.07, rS = 0.17*; *p ≤ 0.05, **p ≤ 0.01). The reduced number of individuals (n = 169) is due to missing MSW values. The evening shift shows the greatest similarity between work and free days.
As is done for day-workers, MSF in shift-workers is corrected for sleep-debt (MSFMsc, MSFEsc, MSFNsc) using a weighted average based on the number of workdays and free days (see The MCTQShift; note that in shift-workers, we consider the free days following a specific shift).
We have shown that chronotype depends on longitude within a time zone (Roenneberg et al., 2007b), so that the chronotype measure, MSFEsc, of the shift-workers (working in different German locations) should be adjusted to the average longitude represented in the database of German day-workers for comparison between the two populations (see Assessment Methods). When we applied this adjustment, the 2 chronotype distributions were statistically not distinguishable (average MSFEsc of 4.49 ± 1.55, average MSFsc in the population of 4.45 ± 1.4, z177 = 0.35, p > 0.5). Figure 3 shows the correlation between the distribution bins of German chronotypes within the MCTQ database and that of the shift-worker sample.
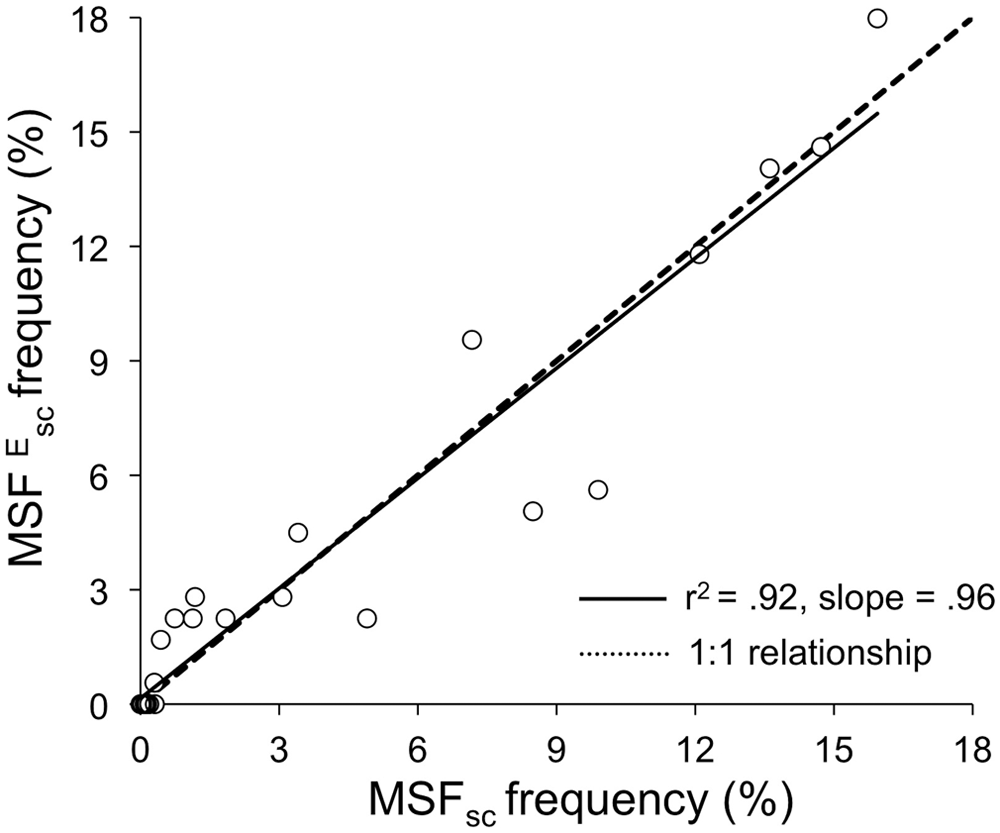
Comparing MSF of shift-workers with that of the general population. The MSFsc times of the German population in the MCTQ database (N = 51,803) and those after evening shifts (MSFEsc, adjusted to match Germany’s average longitude) of our shift-work population (N = 178, 1 missing participant due to lacking geographical information) were binned in half-hour steps, and the resulting bin frequencies were plotted against each other. The stippled line represents a 1:1 relationship. The black line corresponds to the regression fitted against the binned data (r2 = 0.93, slope = 0.73).
Chronotyping Shift-Workers Whose Schedules Do Not Include Free Days after Evening Shifts
Our analyses have shown that MSFEsc is the best candidate to chronotype shift-workers. However, not all rosters include evening shifts or free days after evening shifts (e.g., certain fast forward rotating shifts, or permanent morning and night shifts). In these cases, we propose to derive MSFEsc from its correlations with MSFMsc and MSFNsc (Fig. 4). Based on the shift-work population represented here, the calculation of MSFEsc based on morning shifts (MSFMsc) is more reliable than that based on night shifts (MSFNsc; showing higher interindividual differences).

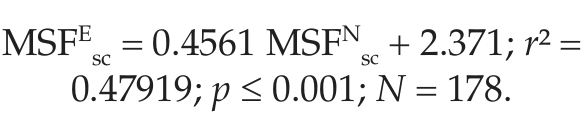
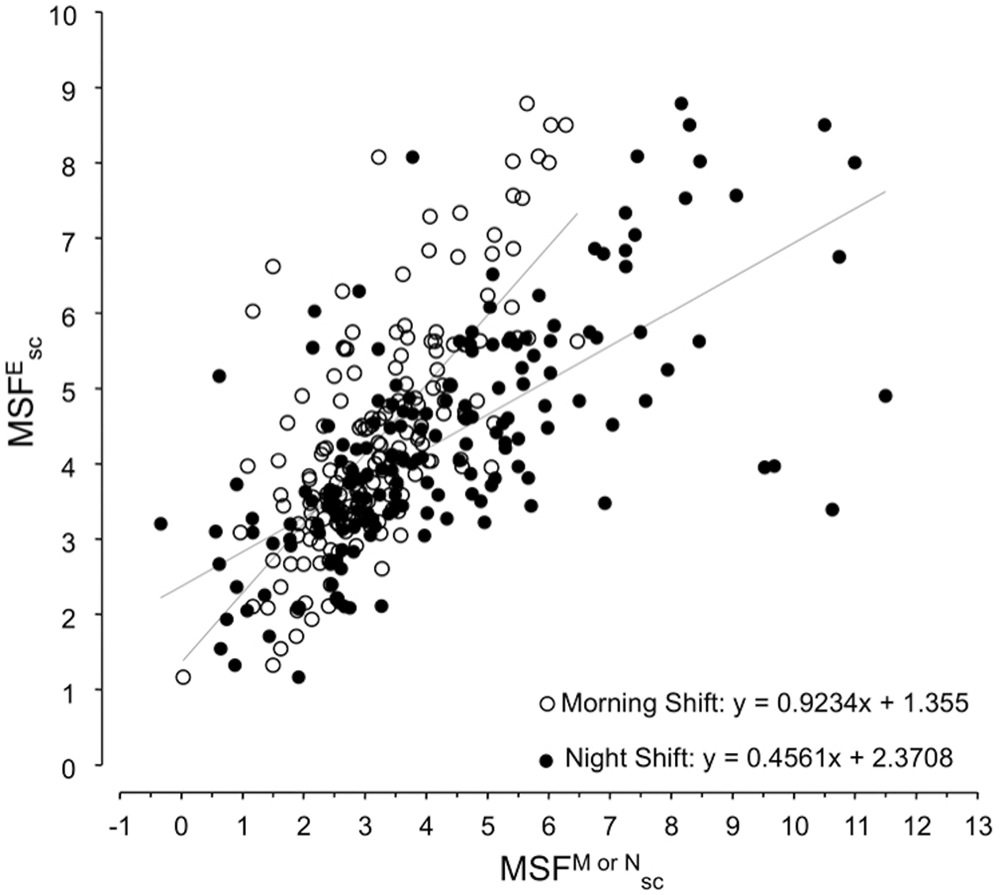
Mid-sleep corrections for shift-workers whose shift schedules do not include free days after evening shifts. The equations represent linear regressions of MSFEsc with MSFMsc (circles; N = 177; y = 0.9234x + 1.355) and MSFNsc (dots; N = 178; y = 0.4561x + 2.3708), respectively, and can be used to estimate MSFEsc values when the workers’ schedules do not include evening shifts.
Discussion
The validation results described in the first part of this article show that the MCTQShift adequately reflects sleep behavior in shift-workers when compared with daily sleep logs and actimetry. One exception is the comparison between sleep duration on free days assessed by the MCTQShift and sleep logs versus actimetry (Table 1). This may simply reflect the low number of shift-specific free days (on average 3). It is, however, remarkable how well mid-sleep times on free days (MSF) assessed by the MCTQShift correspond to those derived from both sleep logs and actimetry, supporting MSF as a reliable basis for chronotype. On their free days, shift-workers sleep on average between midnight and 0900 h, similar to day-workers—regardless of the preceding shift. The stability of MSF times also supports the view that the circadian clock of shift-workers does not readily adjust to rotating schedules (Eastman et al., 1995; Folkard, 2008).
When corrected for "oversleep" (and for longitude), the mid-sleep phase of shift-workers on free days following evening shifts (MSFEsc) is almost identical to that of day-workers. Given the cross-sectional nature of this study, further research is needed to elucidate the question of chronotype-specific bias to choose shift-work or—if possible—certain shift schedules. Yet, our results suggest that such a bias does not exist, possibly because current shift systems and socioeconomic pressures do not allow much choice. This also shows that shift-managers so far do not incorporate individual chronotype in their scheduling—a possibility that could in future drastically reduce an individual’s misalignment between biological and social time (social jetlag; Wittmann et al., 2006), thereby potentially also reducing the detrimental effects of shift-work on health (Roenneberg et al., 2012).
Although MSF remains remarkably stable (compared with MSW), small but significant shift-specific displacements do occur. It is likely that day-to-day circadian phase is affected by different light exposures on the respective shifts, resulting in slightly different sleep times. After all, sleep and its concurrent dark exposure are important components of the entrainment process under conditions that are dominated by self-exposure to light and darkness, as is the case in shift-workers. Studies have shown, for example, that the phase of dim-light melatonin onset can be shifted by scheduled bedtimes (Burgess and Eastman, 2004, 2006).
The large displacements in sleep timing during the respective shifts (MSW) are concurrent with differences in sleep duration, supporting previous reports of shorter sleep on night and morning shifts (Åkerstedt, 2003; Garde et al., 2009; Pilcher et al., 2000; Pires et al., 2009; Seo et al., 2000, Torsvall et al., 1989).
Our results suggest that a short version of the MCTQShift (containing only questions pertaining to evening-shifts) would be sufficient to assess chronotype in workers (provided that their schedules contain evening shifts and subsequent free days). For this assessment, it still is essential to gather information concerning all workdays and free days to correct for potential “oversleep” on free days (MSFEsc). We therefore suggest collecting information about all shifts—even when using a short, evening shift version of the MCTQShift—to allow comparisons between different schedules and their start times.
Given the benefits in time- and cost-efficiency inherent to questionnaires, the MCTQShift could be used as a proxy for classic markers of circadian phase, such as body temperature or dim-light melatonin onset (DLMO). These are generally measured in constant routine protocols, where subjects remain awake in bed for more than 24 h in a semirecumbent position in dim light and constant room temperature (for a comprehensive review, see Duffy and Dijk, 2002). Even when circadian markers are assessed at home (such as DLMO under dim light), they are costly and cumbersome for participants. Many studies use questionnaire-based assessments of circadian phase—most commonly the Morningness-Eveningness Questionnaire (MEQ; Horne and Østberg, 1976). Being primarily based on daily preferences, the MEQ assesses behavioral aspirations rather than actual behavior (Roenneberg, 2012; Roenneberg et al., 2007a; Zavada et al., 2005). More important, the original MEQ does not differentiate between work and free days. Note that DLMO shows a stronger correlation with MSF times than with the MEQ score (Martin and Eastman, 2002). Torsvall and Åkerstedt (1980) have proposed the Diurnal Scale for the assessment of morningness in shift-workers but have recently suggested that other measures of chronotype would be more adequate (Saksvik-Lehouillier et al., 2012).
Finally, we would like to emphasize that any comparison between different populations needs to be corrected for geographical location (e.g., longitude). Our previous work has shown that phase of entrainment, as assessed by the MCTQ, depends on longitude (Roenneberg et al., 2007b), so that geographical corrections would make analyses more reliable. Given that the circadian clock entrains to the specific light-dark cycle of a geographical location, any comparison across populations and locations should apply correction procedures for changes in photoperiod. Labels such as “early” or “late” are relative (see also Roenneberg, 2012), and categorizations of the continuous variable MSF cannot be simply transposed from one nation or continent to the other.
Limitations
The findings reported in the validation section are restricted to the specific shift schedules of our sample. Although the 3-shift system is very common, further validations of the MCTQShift extending to a wider range of schedules would provide more insights into chronotype-specific effects of shift-work and would add more power to epidemiological research on health and shift-work exposure. However, highly irregular shift schedules, as often encountered in hospitals, may be more prone to errors in assessing chronotype with the MCTQShift. Systematic analyses, supported by actimetry and sleep logs, would help to validate the MCTQShift under these conditions.
Historically, activity has been a good place to start for inferences on phase, but since humans in real life aren’t as reliable as model systems in the laboratory, any procedure proposed to assess circadian phase, such as MSFEsc, ultimately needs to be validated against physiological markers (e.g., cortisol and/or melatonin). Mid-sleep has already been shown to correlate well with the timing of melatonin (Martin and Eastman, 2002), we therefore expect MSFEsc to correlate well with physiological rhythms. Further validations of the relationship between behavioral rhythms of humans in any real life situation (including shift-work) and physiological phase markers will also be useful to identify the most useful questionnaire.
A further limitation relates to the fact that we cannot exclude mood or sleep disorders in our participants. Given time restriction within the plants that allowed us to carry out this research, we were unable to collect this information. Although the interactions and causes still need to be elucidated, a strong relationship between the circadian clock and mood and sleep disorders is beyond doubt. Yet, if many of our participating shift-workers were affected by one or more disorders, the validations for sleep duration and timing should have shown differences to those of the general population, which was not the case (note that mood disorders suggest a phase delay in such patients; e.g., Emens et al., 2009). Future studies examining the interactions between mood, shift-work, and sleep may provide further insights by including the MCTQShift.
In summary, the MCTQShift is a time-efficient and economical instrument for chronotyping shift-workers. Beyond chronotyping shift-workers, the detailed information collected by the MCTQShift can also be useful to assess even subtle effects on sleep timing and duration. Thus, the MCTQShift allows the investigation of the human phase of entrainment and sleep and their relationship to health, well-being, and metabolism in the context of work times.
Footnotes
Acknowledgements
This research was supported by the CLOCKWORK Kolleg (funded by the Gottlieb Daimler and the Karl Benz-Foundation) and by Siemens AG, Volkswagen AG, and ArcelorMittal SA. The authors thank the numerous people who assisted them in organizing and implementing the studies, in particular Wolfgang Kloke, Wolfgang Eichinger, Dr. Friederike Dunkel-Benz (Siemens AG), Dr. Angelika Guth (Volkswagen AG), and Dr. Marc Jacoby (ArcelorMittal SA). Above all, they thank the many workers who volunteered their participation in this study.
Conflict of Interest Statement
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.