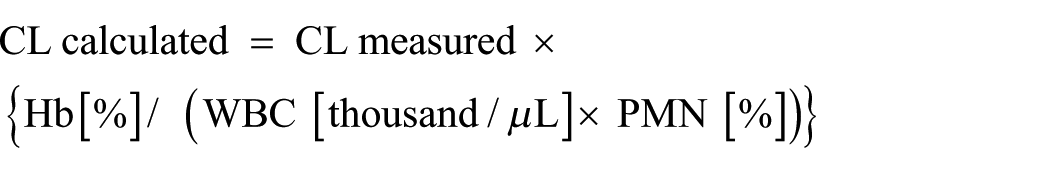Abstract
Lymphocytes Th17 and other types of immune system cells produce IL17. By induction of cytokines and chemokines, the IL17 cytokine is involved in mechanisms of allergic reaction with participation of neutrophil granulocytes. It affects activation, recruitment, and migration of neutrophils to the tissues, regulating inflammatory reaction intensity. Excited neutrophils secrete inter alia elastase and reactive oxygen species (ROS) – significant mediators of inflammation process responsible for tissues damage.
The aim of the study was to evaluate the concentrations of serum interleukin 17A, serum neutrophil elastase, and ROS production by neutrophils in patients with food allergy.
The study included 30 patients with food allergy diagnosed based on interview, clinical symptoms, positive SPT, placebo controlled double-blind oral provocation trial, and the presence of asIgE in blood serum against selected food allergens using fluoro-immuno-enzymatic method FEIA UNICap 100. The control group consisted of 10 healthy volunteers. The concentrations of IL17A were determined in all patients using ELISA method with eBioscience kits, and elastase using BenderMed Systems kits. Chemiluminescence of non-stimulated neutrophils was evaluated using luminol-dependent kinetic method for 40 min on Luminoskan (Labsystems luminometer).
The results of serum IL-17A concentrations and the values of chemiluminescence obtained by non-activated neutrophils, as well as elastase concentrations, were higher in patients with food allergic hypersensitivity compared to healthy volunteers.
This study demonstrates a significance of IL-17A and activated neutrophil granulocytes in the course of diseases with food allergic hypersensitivity.
Keywords
Introduction
A significant increase in the incidence of allergic reactions to food has been observed in recent years. This problem concerns not only children and youths, but also adults. Clinical symptoms observed after allergenic food consumption may be a result of various pathogenic immunological mechanisms and may concern different organs and systems. 1 The studies conducted so far on immunological system functioning in food allergy hypersensitivity patients were mainly related to an evaluation of adaptation response factors. Also, the elements of non-specific immunity system seem to be significant in that context, since it not only initiates but also affects and forms specific response.
An activity of IL-17A is strongly related to the cells of innate immune response. This cytokine is essential in the protection against numerous extracellular pathogens. IL-17A is able to induce an expression of numerous mediators of inflammatory reaction by its participation in proliferation, maturation, and chemotaxis of neutrophils, important elements of non-specific immune response. Pro-inflammatory properties of neutrophils depend on their ability of formation and release of numerous mediators of inflammation processes. 2 The process of enhanced cells activation may involve an excessive generation of reactive oxygen species (ROS), release of numerous proteases, like elastases, cathepsin G, proteinase 3, myeloperoxidase, and metalloproteinases. Neutrophils constitute the most important ROS source in peripheral blood. In case of insufficiently functioning tissue defense mechanisms, created or separated mediators may destructively affect the tissues and contribute to the occurrence of clinical signs of disease.3,4
The aim of the study was to evaluate the concentrations of serum interleukin 17A, serum neutrophil elastase, and ROS production by non-stimulated neutrophils. Additionally, the relationship between the concentration of serum IL-17A and metabolic activity of neutrophils was determined using a chemiluminescence test, and neutrophil elastase concentration in food allergic patients.
Materials and methods
The examined group consisted of 30 adult patients (18 women, 12 men; mean age, 41 ± 8.7 years), who were subject to a detailed diagnostics to exclude diseases other than allergic ones. Food allergy was diagnosed based on an interview, physical examination, and laboratory diagnostics, as well as placebo-controlled double-blind oral provocation trial. The patients suffered the following gastrointestinal tract disorders most often: bloating, abdominal pain, nausea, and diarrhea. The incidents of acute urticaria were demonstrated in all the patients during the interview. Patients with exacerbation of the symptoms associated to food allergy were qualified to the study. The reasons of disease symptoms in the examined group included peanuts, celery, apple, eggs, and fish. In eight of the examined patients, the allergy concerned more than one allergen. The patients with an elevated concentration of allergen-specific IgE (asIgE) – class ⩾2 (0.70 KU/I), were qualified to the examined group. The reference group consisted of 10 healthy volunteers (5 women, 5 men; mean age, 37 ± 6.3 years) with negative atopic interview, without symptoms of infection, and not taking any drugs.
Blood for examination was collected from the ulnar vein to the test tube with lithium heparin of a final concentration of 10 U/mL using a closed Vacutainer system, and on clot to test tube without anticoagulants. Basic morphological blood parameters were additionally determined in all patients. Analyses (asIgE) were performed using the fluoro-immuno-enzymatic method (FEIA) on UNICAP100 apparatus using the kits of Phadia company. The concentrations of asIgE antigens in class ⩾2 was accepted as a positive result. The concentration of serum interleukin IL-17A was determined by ELISA enzymatic method using the kit from the company eBioscience, characterized by a moderate minimum detectable dose (MDD) on a level of 0.5 pg/mL. The test was performed according to the manufacturer’s instructions. The readout and calculation of the concentrations was done using apparatus and software of Bio-Tek Instruments Inc., ELx800.
An evaluation of non-stimulated neutrophils tissue metabolism (BS) was conducted using chemiluminescence method (CL) enhanced with luminol (5-Amino-2,3-dihydro-1,4-phthalazinedione, Sigma) dissolved in 0.4% NaOH solution up to the concentration of 28 µmol/mL. Luminol is a compound which is subject to excitation in the process of oxidation, which enables considerable intensification of lightning effects. The examinations were performed using Luminoskan Ascent apparatus (Thermo Labsystems Helsinki, Finland). Analyses were performed using kinetic method for 40 min at a temperature of 37°C ± 1°C, measuring CL in 2 min intervals. The results were presented as the values of CL integration, i.e. the surface area under the emission curve in time function measured for 40 min, and they were provided in RLU (Relative Light Units). Each analyzed sample contained full blood, luminal, and was completed with PBS to the constant volume. The blood was added directly before the readout. The readouts were made 2 h from material collection at the latest. Each measurement was repeated three times, and mean value was calculated. Chemiluminescence values were corrected with the values of hemoglobin concentration and absolute neutrophils count, and expressed as RLU according to the following formula:
The obtained result (RLU) was related to 1000 cells, which allowed to eliminate an effect of differentiated number of neutrophil granulocytes in the sample, and thus higher optimization of obtained results. The concentration of elastases bond in a stable complex with proteinase inhibitor α1-IP (EL-α1-IP) was determined in blood serum using ELISA enzymatic method with an application of commercial kits (BenderMed Systems). The analyses were conducted according to the manufacturer’s instructions. Calibration curve and calculation of the concentrations were made using apparatus and software of Bio-Tek Instruments Inc., ELx800.
The following statistical methods were used in results elaboration: arithmetic mean estimations (x); estimations of standard deviation for the mean value (s). Analysis of examined features distribution was performed using the Shapiro–Wilk test. The Mann–Whitney U test was used for an analysis of significance of the differences between the groups which distribution differed significantly from the normal one (Shapiro–Wilk test, P <0.05), while Spearman’s correlation was applied to determine the correlations between the examined variables. Computer software Statistica v. 6.0 (StatSoft) was used for statistical data processing.
The study was conducted under an agreement of the University Bioethics Committee CM in Bydgoszcz UMK (agreement no. KB 683/2009).
Results
The results of the study evaluating the concentrations of IL-17A and elastase in blood serum and resting state of neutrophils activation based on ROS production is presented in Table 1 and in the Figures (together with significance levels). Correlations between examined parameters are presented in Table 2.
Concentrations of IL-17A and elastase in blood serum, and rest state of neutrophils activation based on ROS production.

Correlation between the examined parameters.

Analysis of the results obtained demonstrated significantly higher mean concentrations of serum IL-17A, and significantly higher mean values of chemiluminescence emitted by resting, non-stimulated peripheral blood neutrophils in the patients with food allergy hypersensitivity compared to the reference group. Also significantly higher mean values of elastase determined in the complex (EL-α1-IP) was noted in the group of the examined patients compared to healthy volunteers. The study demonstrated statistically significant positive Spearman’s correlation between the concentration of IL- 17 and chemiluminescence (CL-BS) in the examined patients. However, no correlation was found between the concentration of IL17A and serum elastase.
Discussion
Despite intensive research, the pathogenesis of food allergy is still not fully explained. Complex interactions between immune system cells constitute the background of allergic inflammation process. The possibility of neutrophils participation in reactions on food is increasingly often undertaken in the research. Interleukin 17A belongs to the family of cytokines IL-17. Family IL-17 includes interleukins of a similar structure, marked subsequently with alphabet letters from A to F. IL-17A is mainly related to the participation of neutrophils, and strongly pro-inflammatory cytokines of multidirectional mechanism of activity.2–4 It has a significant role in diseases of inflammatory, auto-immunological, and cancer backgrounds.5–7
Experimental research demonstrated that administration of IL-17A to animals resulted in an intensified local accumulation of neutrophils caused by chemotactic factors synthesized in parenchymal cells.4,8 It was confirmed that IL-17A affects the process of progenitor CD34+ cells maturation in bone marrow enhancing their differentiation towards neutrophil granulocytes by induction of synthesis of granulocyte colony-stimulating factors (G-CSF), and granulocyte-macrophage colony-stimulating factors (GM-CSF). It was also proved that this cytokine increases expression of genes encoding biologically active substances responsible for inflammatory reactions development and maintaining. IL-17A induces nuclear transcription factor (NF-ĸß) in fibroblasts, macrophages, and chondrocytes. The observations concerning the cells of small intestine and colon epithelium are interesting. It was demonstrated that IL-17A by activation of NF-ĸß may initiate inflammation process. Other mechanism confirming this cytokine participation in inflammation promotion should be related to its participation in the process of an induction of production of adhesion molecules ICAM and pro-inflammatory cytokines: CXCL8, CXCL1, CXCL2, and CXCL5. Mentioned molecules are mainly addressed towards neutrophils,9,10 although lymphocytes Th17, IL-17A may also be generated by activated CD8+ cells, lymphocytes T gamma delta, cells NK, NKT, and macrophages as well as neutrophils. Excitation of receptor for IL-17A – IL-17AR observed on leukocytes, fibroblasts, keratinocytes, endothelial cells, bronchial epithelial cells, kidney, and spleen results in the production of chemokines and pro-inflammatory cytokines, accumulation of neutrophils, their excitation, activation, and release of mediators, which leads to a development of certain diseases.2,9,11 There is some evidence that apart from an effect on recruitment of neutrophils and monocytes, IL-17A also contributes in some mechanisms underlying allergic reaction in respiratory tract.8,12,13
The contribution of IL-17A in allergic diseases – especially in asthma, allergic rhinitis (AR) and atopic dermatitis (AD) – has been confirmed in recent years.14–17 Pro-inflammatory properties of neutrophils are related to their ability of production and release of numerous significant mediators of inflammation processes, including ROS and some enzymes. It was demonstrated in in vitro experiments that human epithelial cells in the respiratory tract synthesize de novo when affected by IL-17A, and release IL-8 – an important neutrophilic chemoattractant – as well as IL-6, which is responsible for elastase release from neutrophils.9,18
This study conducted in patients with confirmed food allergy demonstrates a relationship between IL-17A, an enhanced neutrophils activation evaluated by the range of oxygen metabolism, and ability of elastase release. We demonstrated a significant increase in serum IL-17A concentrations (range, 0.5–2.7 pg/mL) in the patients during the period of clinical symptoms intensification compared to the healthy volunteers (range, 0.3–1.5 pg/mL) (Figure 1).

Concentration of IL-17A in serum of the study groups.
So far, only sparse experiments demonstrated the participation and relationship of IL-17 in development of bronchi hypersensitivity in mice depending on allergen administration and the stage of allergic reaction.15,19 An increase in de novo IL-17A synthesis in lungs and an increase in the number of BAL neutrophils were noted on mice asthma model after an inhaled allergen provocation trial. 20 The study in the groups of asthmatics demonstrated an increase in IL-17 concentrations in sputum, bronchoalveolar lavage fluid, and blood serum. Also, the correlation with the number of neutrophils and degree of disease severity was noted.21–23 Linden et al. also demonstrated in the examined asthmatics, that IL-17A and IL-17 F are responsible for an intensified accumulation of neutrophils, affect increased mucosa secretion and excessive activation of macrophages, and cause an increase in bronchi smooth muscles reactivity, pointing concurrently towards this cytokine significance, especially in moderately chronic and acute asthma. 24
In turn, the study conducted by Chen demonstrated that IL-17A, indirectly, by IL-6 release from respiratory epithelium, enhances mRNA expression for mucin in these cells. 25 Ramirez-Velazques et al. confirmed the role of neutrophils as an important source of interleukin IL-17 in asthma caused by allergy for allergens of mold spores and plant pollen. 26 The presence of IL-17A was analyzed in neutrophils with surface expression of molecule CD177+ in patients with mild, moderate, and severe asthma. An increased number of these cells was observed in patients with chronic moderate asthma, especially in these allergic to molds allergens. However, due to the low number of examined patients, it was not possible to determine more precise reaction between neutrophils CD177+IL17+ and asthma severity.
A previous study reported that IL-17A is one of the key mediators related to regulation of inflammation processes. 27 However, in the future, this cytokine may still be a goal of the strategy of various inflammatory diseases treatment.
High levels of IL-17 were detected in the patients with mono-sensitization to birch pollen, which is severe allergic rhinitis (AR), regardless of the allergen exposure, which was associated with inflammation process chronicity. 28 The study conducted on patients with AR also demonstrated a significant contribution of this interleukin and increased number of lymphocytes T producing IL-16 in nose mucous membrane. This study also attracted an attention to observed numerical disproportions between peripheral lymphocytes Th17 and Treg cells in these patients. 29
It was proved that lymphocytes T producing IL-17 are characterized by surface expression of molecule CD161. The study by Poggi et al. confirmed an increased number of lymphocytes T CD161 in peripheral blood of patients with AR. 30 It concerned lymphocytes T CD4+CD161+ and CD8+CD161+. 30 It was also demonstrated that an intensity of this molecule expression on the cells was strongly related to the severity of clinical disease symptoms.
Leonardi et al., in comparable groups of children with atopic dermatitis (AT) and healthy children, observed increased concentrations of IL-17 only in the blood serum of ill children. 31 Other observations also pointed a strict relationship between symptoms severity and interleukin concentration, which according to some researchers may be an important marker in an evaluation of AT severity degree.7,31,32 Most of the studies conducted so far on the role of IL-17A in allergic diseases were performed on animal models, therefore it is difficult to relate the conclusions obtained to humans.
Non-stimulated neutrophils circulating in peripheral blood are little active metabolically. Their excitation may result in an increased production of reactive oxygen species. This phenomenon is called “respiratory burst” and is related to light emission. The number of formed photons may be measured using a luminometer. Created oxygen species may affect nuclear transcription factors and stimulate synthesis of pro-inflammatory cytokines, cause inactivation of important proteinases inhibitors, and lead to an acceleration of proteolytic enzymes activity on tissues. 11
In the study conducted on patients with food allergy type hypersensitivity, we demonstrated statistically significantly higher values of spontaneous chemiluminescence generated by neutrophils (range, 0.40–4.01 RLU), compared to the values in the group of healthy volunteers (range, 0.12–0.55 RLU) (Figure 2). A positive, statistically significant Spearman’s correlation was demonstrated between the concentration of serum IL-17A, and chemiluminescence emitted by resting non-stimulated peripheral blood neutrophils (Table 2). Also, our previous research conducted on the selected group of patients with air-borne and food allergies confirmed an increased metabolic activity of neutrophils evaluated using a chemiluminescence method.33,34 Similarly, increased production of ROS, both by resting and stimulant-induced neutrophils, were observed in the studies conducted on a large group of children with well-documented food allergies. 35

Concentration of elastase bound with longlasting complex with proteinases inhibitor (EL-α1-IP) in the study groups.
It was demonstrated in animals that interleukin IL-17 affects not only the accumulation of neutrophils, but also their activation leading to an increased release of serine proteases, e.g. myeloperoxidase and elastase – an enzyme having high activity and broad spectrum of activity.8,36 The role of elastase is closely connected with the function of neutrophils. Its enzymatic activity allows the proper course of many physiological functions of granulocytes. It is involved in the process of degradation of the components of cell membranes and proteins, elastin, several types of collagen, fibronectin, laminin, proteoglycans, soluble plasma proteins, and transport proteins. Serum endogenous protein inhibitors, α1 protease inhibitor (α1-IP), α2-macroglobulin (α2-MG), and elafin, control and are responsible for extracellular elastase activity forming non-active complexes. Increased activity of neutrophils is associated with a release of increased amounts of elastase, which in the form of complex with α1-IP is transferred into the blood. The increase in the concentration of these complexes in blood serum or plasma is commonly regarded as an important exponent of neutrophil granulocytes stimulation in the focus of inflammation, and as a measure of an activity of ongoing inflammatory process. 37
We demonstrated an increase in the concentrations of elastase determined in the complex with inhibitor (EL-α1-IP) in the patients with food allergy (range, 52.30–980.70 ng/mL) compared to the control group (range, 43.82–201.30 ng/mL) (Figure 3). No positive Spearman’s correlation was noted between the concentrations of IL-17A and elastase. The participation of elastase evaluated in the complex with (EL-α1- IP) was pointed in the study on food hypersensitive patients, confirming thus its significance in inflammatory process caused by an allergy. 33
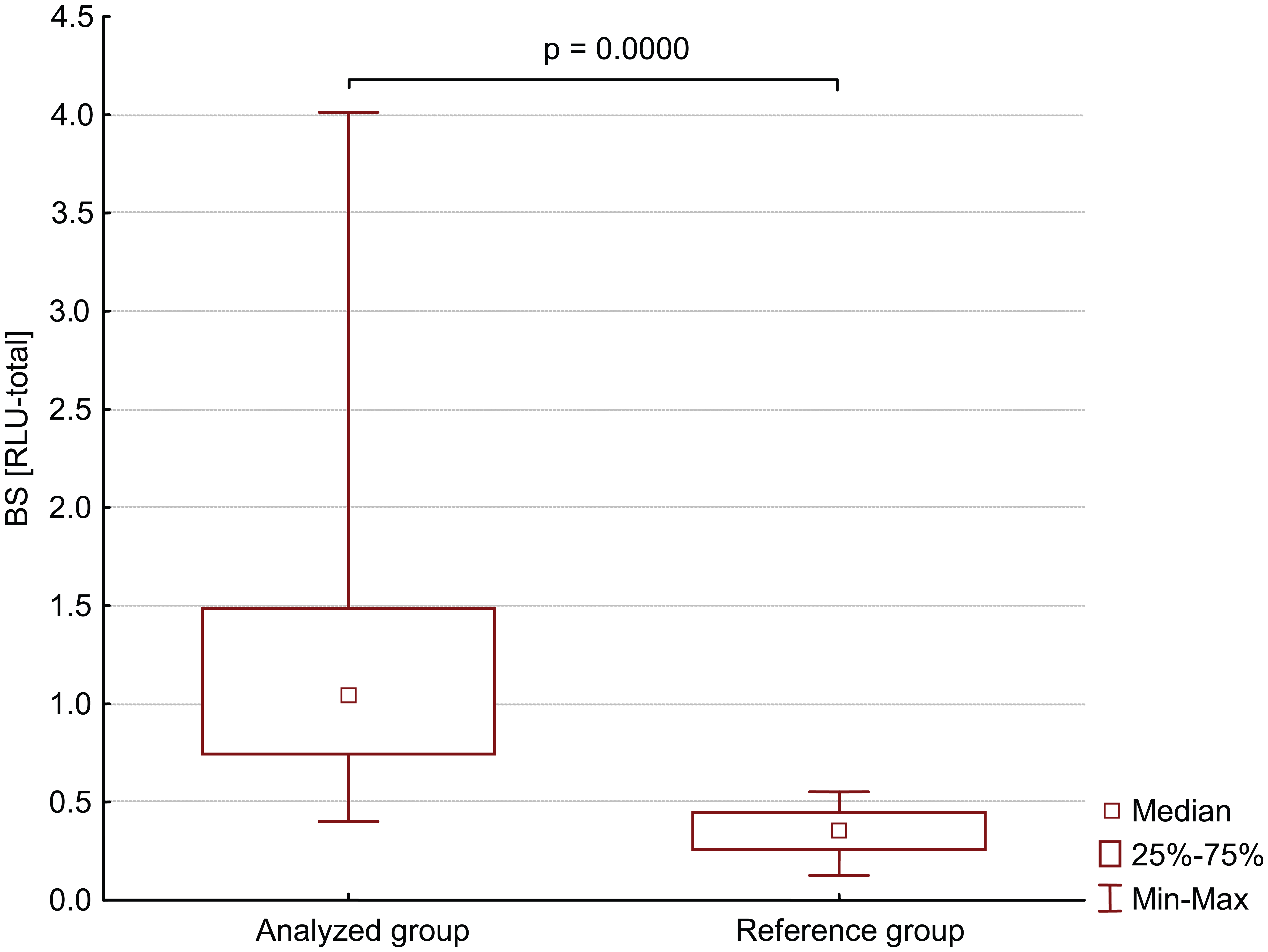
Non stimulated neutrophil chemiluminescence BS in study groups.
An increased neutrophil elastase activity in the plasma of patients with asthma, atopic dermatitis, and allergic rhinitis was indicated in previous studies, which demonstrated a significantly higher concentration of elastase in asthma patients, particularly during exacerbations, with a tendency to grow with the severity of the disease.38–41 Similarly, an increase in elastase concentrations was noted in NAL (nasal airway lavage) in the patients with allergic rhinitis. 42 Monteseirini et al. also demonstrated that allergen stimulation of neutrophils in asthmatics resulted in an increased elastase release. This effect was observed only when a specific reaction character characterized the reaction. 43 Although the current state of knowledge quite clearly explains the function of IL-17A as a protein responsible for the development and regulation of many inflammatory diseases, attention should be paid to the reports indicating the possibility of both pro- and anti-inflammatory effects of IL-17, depending on the environmental conditions. 44
The involvement of IL-17A in the course of atopic diseases already proven in many studies was also confirmed in the patients with allergic food hypersensitivity and with gastrointestinal and skin symptoms.33,34,36 We demonstrated that it is primarily associated with an increased activity of neutrophil granulocytes evaluated by the amount of oxygen metabolism, and to a lesser extent, an increase in serum elastase concentrations. The results presented in the study indirectly indicate the involvement of non-specific immune mechanisms, which, apart from the obvious specific reactions, are important in allergic reactions to foods. It cannot be excluded that IL-17 produced by Th17 and other cells may be a link between an activation of T-cell caused by allergens, and recruitment and activation of neutrophil granulocytes in allergic inflammation process in allergic reactions. The role of IL-17A in allergic diseases, i.e. especially in allergic food hypersensitivity, requires further research.
In summary, the present study adds important findings to the food allergy immunological mechanisms. The study revealed that patients with food allergies demonstrate a relationship between IL-17A, an enhanced neutrophils activation evaluated by the range of oxygen metabolism, and ability of elastase release.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.