Abstract
Aim
This study aimed to assess the impact of online health information and AI-based tools on treatment decisions, trust, and care-seeking behaviors among migraine patients in Arab speaking countries from MENA region.
Methods
A multinational, cross-sectional online survey was conducted among 4276 adults with migraine across 13 MENA countries. Data collected included sociodemographic characteristics, migraine history, digital health literacy (eHEALS), AI tool usage, and trust in health information sources.
Results
The mean eHealth literacy score was 29.9 ± 6.2. Overall, 75.6% demonstrated adequate digital health literacy. Neurologists and physicians were the most trusted sources, whereas social media influencers were the least trusted. Approximately one-third of participants reported modifying migraine treatment or delaying medical consultation based on online information. In multivariable analyses, higher trust in online information was strongly associated with delayed medical consultation (aOR 6.48, 95% CI 5.53–7.58, p < 0.001). In contrast, use of AI tools was associated with lower odds of reporting treatment modification based on online advice (aOR 0.29, 95% CI 0.17–0.49, p < 0.001). Higher trust in online information was consistently associated with both delayed care and treatment changes. Younger age, male sex, and active online information-seeking independently predicted AI use.
Conclusion
Digital health engagement, including trust in online sources and AI tool use, was significantly associated with migraine-related decision behaviors in this multinational MENA cohort. While AI use was linked to more cautious treatment behaviors, higher trust in online information was associated with delayed medical consultation and treatment modification. These findings highlight the importance of strengthening digital health literacy and promoting reliable online resources.
This is a visual representation of the abstract.
Introduction
Background
The rapid expansion of the internet and the accelerated integration of artificial intelligence (AI) into healthcare have fundamentally reshaped how patients’ access, interpret, and act upon medical information. 1 With more than 4.1 billion individuals worldwide having access to the internet, online health information has become an increasingly influential component of patient decision-making. 2 This shift was further amplified during the COVID-19 pandemic, when reliance on telehealth and AI-enabled tools intensified across populations and health systems. 3 Within this evolving landscape, patients with chronic neurological disorders—particularly migraine—have emerged as some of the most frequent users of digital health resources. Migraine is a highly prevalent and disabling disorder, and the episodic, unpredictable nature of attacks often prompts patients to seek immediate advice, symptom explanations, or treatment options online. As a result, digital health behaviors are becoming intertwined with real-world migraine self-management and decision-making. 4
In the Middle East and North Africa (MENA) region, the uptake of digital health resources mirrors global trends. Internet penetration has risen substantially, with countries such as Kuwait reaching usage rates approaching 90% of the population. 3 This widespread connectivity has facilitated a growing reliance on online health information. In Saudi Arabia, 90.9% of individuals report that Internet— or social media—based health information enhances their general health awareness, 5 and in the United Arab Emirates (UAE), online sources surpassed physicians as the most common initial reference for health information during the pandemic, with 67% of the public consulting the Internet first. 6 For patients with migraine who frequently navigate recurrent symptoms, medication options, and lifestyle triggers—such patterns suggest that digital platforms may play a substantial role in shaping illness perceptions, treatment choices, and health-seeking behaviors. MENA countries are also taking active steps toward integrating AI into healthcare. National strategies in the UAE and Saudi Arabia have established dedicated governmental bodies to facilitate AI innovation and apply intelligent systems across medical services.7–9 Early data indicates generally positive attitudes toward AI among both the public and healthcare professionals in the region. 10 Yet despite this optimism, practical integration remains limited. Challenges related to data quality, insufficient region-specific datasets, constrained infrastructure, and limited AI training for the healthcare workforce continue to impede meaningful adoption. Moreover, concerns persist regarding the potential for AI to widen health disparities if access is uneven or algorithms are not appropriately validated within local populations. 1
Given the high burden of migraine, its chronic and often self-managed nature, and the widespread regional use of digital health tools, there is a compelling need to understand how patients with migraine in MENA engage with online health information and AI-based resources. Existing studies in Arab countries have largely been single-nation or population-specific, leaving important gaps in regional understanding. 11 This multinational cross-sectional survey aims to address these gaps by examining how migraine patients across the MENA region seek health information online and how aware they are of, and how they utilize AI-enabled tools such as symptom checkers, chatbots, and digital decision-support applications. The objectives of this study are to assess the prevalence, patterns, and perceived trustworthiness of online health information sources among migraine patients; evaluate familiarity with, and use of, AI-driven health applications; and explore demographic and regional factors influencing these behaviors.
Understanding these patterns is essential for both clinicians and policymakers. When migraine patients rely on internet search engines or AI chatbots to guide treatment choices, this can influence medication adherence, trigger management, emergency department utilization, and expectations during clinical encounters. Insights from this work can support efforts to improve digital health literacy, guide clinicians in counseling patients who self-diagnose or self-treat using online tools and inform national strategies for the safe integration of AI in neurology. Additionally, the findings highlight opportunities to strengthen Arabic-language digital health platforms and enhance AI readiness across the region. Ultimately, a clearer understanding of how migraine patients use digital and AI resources can help optimize patient care, reduce misinformation-related risks, and support the development of equitable, patient-centered digital health ecosystems in the MENA region.
Methods
Study design
The current study is a cross-sectional, multinational investigation conducted among adults with a neurologist-confirmed diagnosis of migraine using a descriptive correlational methodology. The study adheres to the Checklist for Reporting Results of Internet E-Surveys (CHERRIES) and utilizes the STROBE reporting guidelines to ensure precision and accuracy in reporting.12,13
Study population
From April 2025 to September 2025, a cohort of 4276 individuals was recruited via an online survey from 13 Arabic-speaking countries within the MENA region, with the distribution of participating countries detailed in Table 1. Participants were recruited through different online recruitment channels (e.g., social media, migraine support groups, neurology clinics, Microsoft Teams groups, announcements in different groups on social media, and flyers posted in common areas as clubs). To ensure relevance and representativeness, inclusion criteria required participants to be an adult (18+) with a self-reported confirmed diagnosis of migraine by a certified neurologist, in accordance with the International Classification of Headache Disorders, 3rd edition (ICHD-3). 14 Also, participants were required to be residents of an Arabic-speaking MENA country and able to consent and complete an online or face-to-face questionnaire. Individuals with no formal diagnosis of migraine, non-internet users and those who live outside Arab countries were excluded from the study. To prevent duplicate participation or non-eligible participation, the questionnaire settings were configured to allow only one response per individual and to exclude non-eligible individuals automatically. All survey items were mandatory, resulting in complete datasets with no missing responses among submitted questionnaires.
Sociodemographic data of study participants (N = 4276).

Assessment
A self-administered questionnaire in Arabic and English was developed by the authors based on previous validated surveys5,6 and refined to include AI-specific items (For the full study questionnaire, refer to Online Supplementary File 1). The study questionnaire included five sections:
- Section 1: Consent and exclusion questions. - Section 2: Sociodemographic characteristics including age, sex, country of residence, educational level and occupation. - Section 3: Migraine profile and related online/AI health information behavior; includes data regarding migraine occurrence, frequency and medications use. This section also included items assessing the use of online/AI health information in migraine, and their impact on individuals’ behavior regarding their migraine. - Section 4: Digital health literacy assessing Online health-seeking behaviors using an adapted form of the eHEALS scale. The eHEALS is an 8-item scale that tends to measure perceived skills at finding, evaluating, and applying electronic health information to health problems.
15
The instrument proved to be a reliable and easy-to-use self-report tool and has been used in many studies with good reliability and reproducibility.16,17 The scale is based on a model that distinguishes between six types of literacy skills: traditional literacy, health literacy, information literacy, scientific literacy, computer literacy, and media literacy.
18
It contains eight items, measured with a 5-point Likert scale with response options ranging from “strongly disagree” to “strongly agree.” Total scores of the eHEALS are summed to range from 8 to 40, with higher scores representing higher self-perceived eHealth literacy. As no universally accepted cutoff exists to distinguish adequate from limited eHealth literacy, a score of 26 was used as the threshold in this study. Participants with eHEALS scores > 26 were classified as having adequate eHealth literacy, whereas those with scores ≤ 26 were considered to have limited literacy, in accordance with prior regional studies.19–21 This cutoff has been commonly applied in digital health research within similar populations - Section 5: Trust in different health information sources.5,6 Trust in health information sources was assessed using a 5-point Likert scale, where 1 indicated “No trust” and 5 indicated “Complete trust.” Participants rated their level of trust for each listed source. For each source, mean trust scores and standard deviations (SD) were calculated by summing individual ratings and dividing by the number of respondents. To facilitate interpretation, mean trust scores were categorized a priori into three levels based on commonly accepted Likert-scale conventions
7
: scores <3.0 were considered low trust, scores from 3.0 to <4.0 were considered intermediate (neutral) trust, and scores ≥4.0 were considered high trust. Sources were ranked according to their mean trust scores. In addition, an overall trust score was calculated by aggregating the mean scores across all sources.
The accuracy and face validity of the survey were evaluated by four experts from various fields, including general neurology, headache specialist, digital health, and statistics. Necessary modifications were made based on their feedback. The reliability of the survey was tested on 250 individuals who were excluded from the main study using appropriate statistical tests. The reliability test confirmed the efficacy of the tools. The Cronbach's Alpha for digital literacy, measured using the eHEALS scale, was 0.92, demonstrating excellent reliability. In contrast, trust ratings yielded a Cronbach's Alpha of 0.80, which also indicates a good level of reliability. A pilot study was also conducted on another 150 individuals to evaluate the applicability, clarity, and feasibility of the study's instruments, leading to further refinement. After completion of the validation and the pilot study, the questionnaire was modified with built-in eligibility filters using branching logic to exclude non-eligible participants at the start of the survey. As a result, no participants were excluded after survey completion.
Ethical approval
Ethical approval was granted by the Research Ethics Committee at the Faculty of Medicine, Alexandria University, Alexandria, Egypt, obtained in April 2025 under number 0307430. Each participant received a digital written explanation of the study's purpose and provided digital informed consent before data collection. The study emphasized anonymity, voluntary participation, and the right to withdraw at any time. Confidentiality was maintained, and responses were anonymous, with no identifying data collected. The study adhered to the ethical principles outlined in the latest version of the Declaration of Helsinki (2013).
Statistical analysis
Data were analyzed using IBM SPSS Statistics version 26.0 (IBM Corp., Armonk, NY, USA). Categorical variables were summarized as frequencies and percentages, while continuous variables were presented as means and SD. Statistical significance was set at a two-sided p value less than or equal 0.05.
Internal consistency of multi-item scales was assessed using Cronbach's alpha. Associations between categorical variables were examined using the chi-square test. Comparisons of normally distributed continuous variables between two groups were performed using Student's t-test, while one-way analysis of variance (ANOVA) was used for comparisons across more than two groups. Correlations between ordinal or non-normally distributed variables were assessed using Spearman's rank correlation coefficient, interpreted using conventional thresholds (weak <0.30, moderate 0.30–0.49, strong ≥0.50). Linear regression analyses were conducted for continuous outcomes, including digital health literacy (eHEALS score) and trust scores. Independent variables entered into these models included age, sex, educational level, occupation status, migraine duration, headache frequency, current migraine treatment use, frequency of online health information searching, and trust in online health information.
Binary logistic regression analyses were used for dichotomous outcomes, including AI tool use (Yes/No), treatment modification based on online information (Yes/No), and delayed medical consultation (Yes/No). Variables were initially screened using univariate analyses, and those showing significant associations or clinical relevance were entered into multivariable logistic regression models. Covariates included age, sex, education, occupation, migraine duration, attack frequency, current treatment use, online information-seeking behavior, and trust in online health information. Multicollinearity was assessed using variance inflation factors, and model fit was evaluated using the Hosmer–Lemeshow goodness-of-fit test. Results are presented as odds ratios (ORs) with 95% confidence intervals (CIs). Given the exploratory nature of the analyses, Bonferroni correction was considered; however, results are interpreted cautiously with emphasis on effect direction and consistency rather than isolated p-values.
Results
Demographics of study participants
A total of 4276 adults with a confirmed diagnosis of migraine from 13 MENA-region countries completed the survey. The mean age was 32.3 ± 18.2 years (range 18–62 years). Females represented 60.8% of participants. Table 1 summarizes sociodemographic data of study participants.
Migraine profile and online/AI health information use
Table 2 summarizes the migraine characteristics of the study population. Most participants (59%) reported a migraine duration exceeding one year, with attacks occurring at least once per month in the majority of cases (59.5%). Approximately half of the participants reported using acute and/or preventive migraine medications, reflecting a broad spectrum of disease activity and treatment engagement. Use of digital resources was pervasive; almost all participants reported using the internet or AI tools for health information, and the majority searched specifically for migraine-related information (81.3%). Around three-quarters had used at least one AI tool (e.g., ChatGPT) for migraine information. Participants most frequently used Google, AI tools, YouTube and social media platforms, and searched for causes, medications, side effects, home remedies, and others’ experiences, Table 2.
Migraine profile and online/AI health information use in study participants (N = 4276).

AI, Artificial Intelligence; WHO, World Health Organization.
Although some participants indicated that they did not search the internet for information about migraine (18.7%), questions related to treatment modification were presented to all participants to capture both direct and indirect exposure to online health information, including passive encounters through social media, shared content, or prior information-seeking experiences. Online information had a clear impact on behaviors. About one-third reported changing migraine treatment based on online advice without consulting a physician, and a similar proportion delayed or avoided visiting a doctor. In multivariable analysis (See Table 7 later), delayed or avoided doctor visits showed a strong independent association with online information exposure (OR 6.48, 95% CI 5.53–7.58, p < 0.001), while AI tool use was independently associated with lower odds of treatment modification based on online advice (aOR 0.29, 95% CI 0.17–0.49, p < 0.001). At the same time, most participants (77.6%) reported that online information helped them understand their migraine better and encouraged them to seek medical care earlier, Table 2.
Digital health literacy and trust in information sources
The mean eHealth literacy (eHEALS) total score was 29.9 ± 6.2, with a median of 31 (IQR: 27–31). Using the cut-off of 26, 75.6% of participants had adequate eHealth literacy (>26), while 24.4% had limited literacy (≤ 26). Item level scores are demonstrated in Table 3.
eHEALS scores among study participants (N = 4276).

Trust was highest for neurologists and general physicians, intermediate “neutral” for digital sources (Google results, patient forums, AI tools, YouTube), and lowest for social media influencers. Trust scores are clustered around the neutral range for most digital sources (23.7 ± 4.8), Figure 1.

Trust in health information sources.
Factors associated with eHealth literacy, AI use and trust
Higher eHealth literacy was associated with younger age, female sex, higher education, and being a student or employed (all p < 0.001). Country-of-residence differences were also significant, with generally higher eHEALS means in participants residing in Libya, Saudi Arabia, Palestine, and Syria compared to some other countries (p < 0.001), Table 4.
Relation between demographic characteristics with eHEALS and trust ratings among study participants (N = 4276).

F; F for ANOVA test, t; Student t-test, *; Statistically significant at p ≤ 0.05.
Trust scores also varied significantly according to age, education, nationality, country of residence, and occupation (all p < 0.001), but not by sex. Older age groups tended to have slightly lower trust scores, and modest differences were observed across education and occupational categories, Table 4.
Correlation analysis
The correlation patterns shown in Figure 2 revealed several weak associations relevant to digital health behavior among people with migraine. The strongest associations were observed between education and eHealth literacy (r = 0.29), trust scores and treatment modification (r = 0.25), and eHealth literacy and improved understanding of migraine (r = 0.21). Younger age and higher educational attainment were associated with higher digital health literacy (eHEALS), consistent with expected demographic gradients in digital competence. In contrast, older age showed a weak association with higher trust in online information despite lower literacy, highlighting a potential divergence between trust and objective digital skills. Engagement with online health information was consistently associated with higher literacy and trust. Participants who actively searched for migraine-related information, used the internet frequently for health purposes, or reported improved understanding and earlier medical consultation after accessing online information demonstrated modest positive correlations with both eHEALS and trust. In contrast, behaviorally impactful actions such as treatment modification or delayed medical visits were weakly associated with higher trust but not with literacy, suggesting that trust—rather than digital health literacy—may be more closely linked to potentially unsafe decision-making. Associations with AI tool use were generally weak, though trends indicated greater uptake among more digitally active individuals. Overall, these findings suggest a dual pattern whereby digital health literacy is primarily related to demographic and educational factors, while trust and its behavioral consequences are more closely tied to patterns of online engagement and perceived usefulness of digital information.
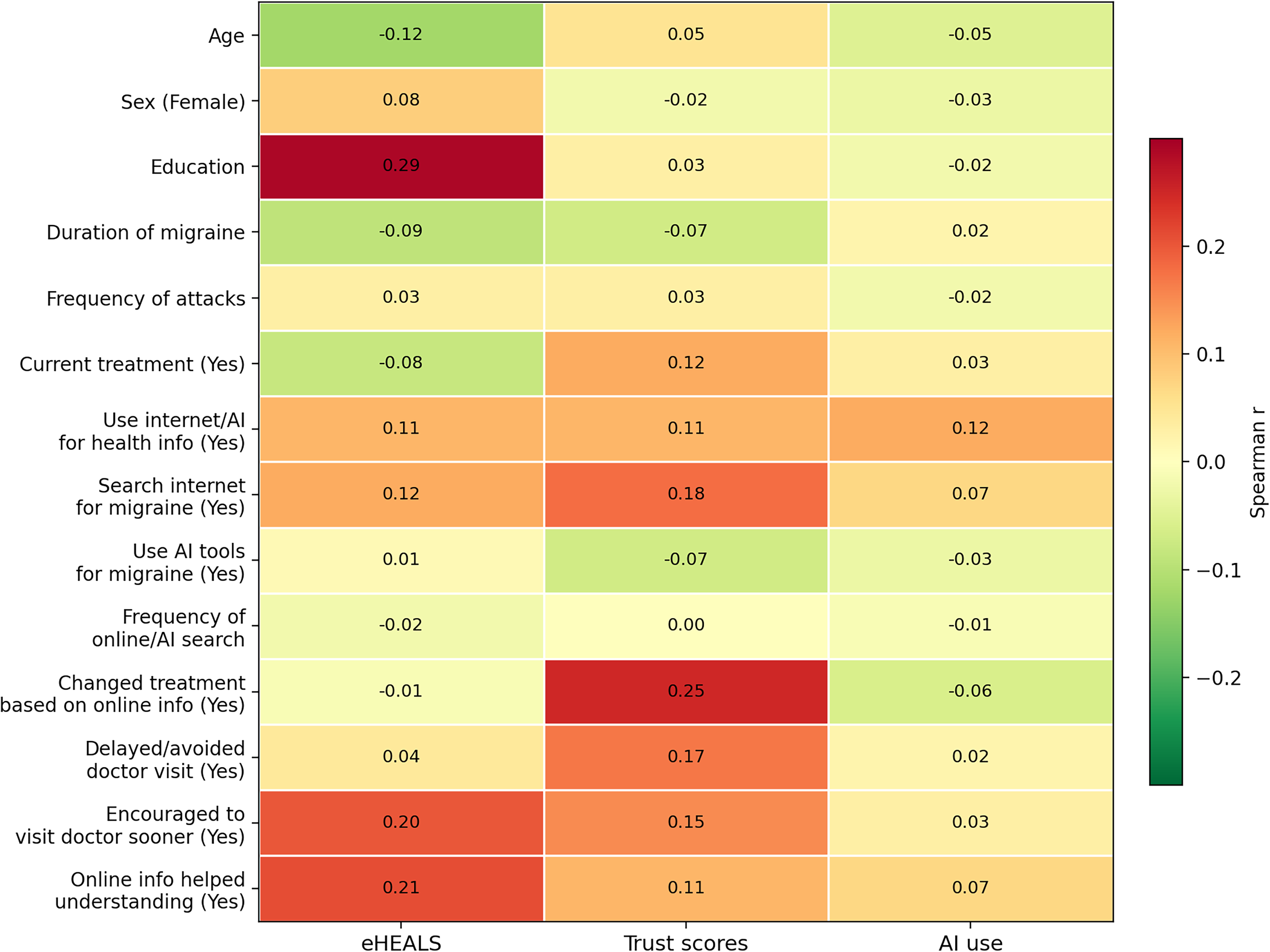
Heatmap illustrating Spearman correlation coefficients between participant characteristics, digital health behaviors, trust scores, and AI tool use. Negative correlations are shown in green and positive correlations in red, with color intensity reflecting correlation strength. Numeric values are displayed within cells to facilitate precise interpretation.
Predictors of AI use
In the multivariate logistic regression analysis presented in Table 5, the following variables were included in the model: age (years), gender, education, occupation, duration of migraine (years), frequency of migraine attacks (per month/week), current treatment use, internet search behavior for information about migraine, use of AI tools for information about migraine, changes in treatment based on online information, delayed or avoided doctor visits due to online advice, encouragement to visit a doctor sooner from online information, online health information understanding, eHEALS, and trust ratings. It showed that younger age and male sex were significant independent predictors of AI use for health information. Behavioral engagement was particularly influential; participants who actively searched the internet for migraine information had markedly higher odds of using AI tools, and those who felt that online information improved their understanding of migraine were also more likely to use AI. In contrast, participants who changed their migraine treatment based on online advice without consulting a physician were significantly less likely to use AI. Notably, eHealth literacy and trust scores were not significant predictors in the final model.
Predictors of AI use.

OR: Odds Ratio, CI: Confidence Interval, LL: Lower Limit, UL: Upper Limit. Asterisk (*) indicates statistical significance at p ≤ 0.05. Reference categories for all binary and categorical variables are specified as shown.
A multivariable logistic regression model was utilized, as shown in Table 6. This model adjusted for potential confounding variables to isolate the effects of key predictors on trust in online health sources. The covariates included age, education level, occupation, treatment usage, and trust ratings. Higher eHealth literacy was the strongest positive predictor of trust in online health sources. Trust was also higher among participants with greater educational attainment and those who used AI tools for migraine information. Conversely, older age, not working, and current use of migraine treatment were associated with lower trust. Behavioral responses to digital health information—such as delaying medical visits, changing treatment based on online advice, and feeling encouraged to consult a doctor sooner—were all independently associated with higher trust in online sources.
Predictors of trust in online health sources.

B; Unstandardized Coefficients, Beta; Standardized Coefficients, t; t-test of significance, CI; Confidence interval, LL; Lower limit, UL; Upper Limit, *; Statistically significant at p ≤ 0.05.
Demographic, behavioral, and treatment factors influencing online information of migraine management
Both univariate and multivariate analyses were performed to explore the behavioral outcomes among study participants. The univariate analysis assessed each variable's direct effect on the outcome, such as the likelihood of changing treatment based on online information or delaying a doctor's visit due to online advice. The multivariate analysis adjusted for other variables, providing a clearer picture of how each factor interacted when multiple predictors were considered simultaneously. Specific covariates in these models included demographic variables (age and gender), health behavior variables (treatment usage, internet searching habits), and trust ratings related to online information. The results of these analyses, including odds ratios with 95% confidence intervals, elucidated how demographic factors, trust, and usage behaviors influenced health decisions.
Changing migraine treatment based on online information (without medical consultation) was strongly associated with delaying/avoiding doctor visits and with higher trust in online sources, even after adjustment for sociodemographic and clinical variables. AI use showed a mixed pattern; overall AI users were more digitally engaged, but in adjusted models, AI use was associated with a lower likelihood of unsafe treatment change in some analyses while higher digital engagement (searching, trusting) increased the odds of change, Table 7.
Analysis of factors and behavioral outcomes influencing online migraine management among study participants: univariate and multivariate perspectives.
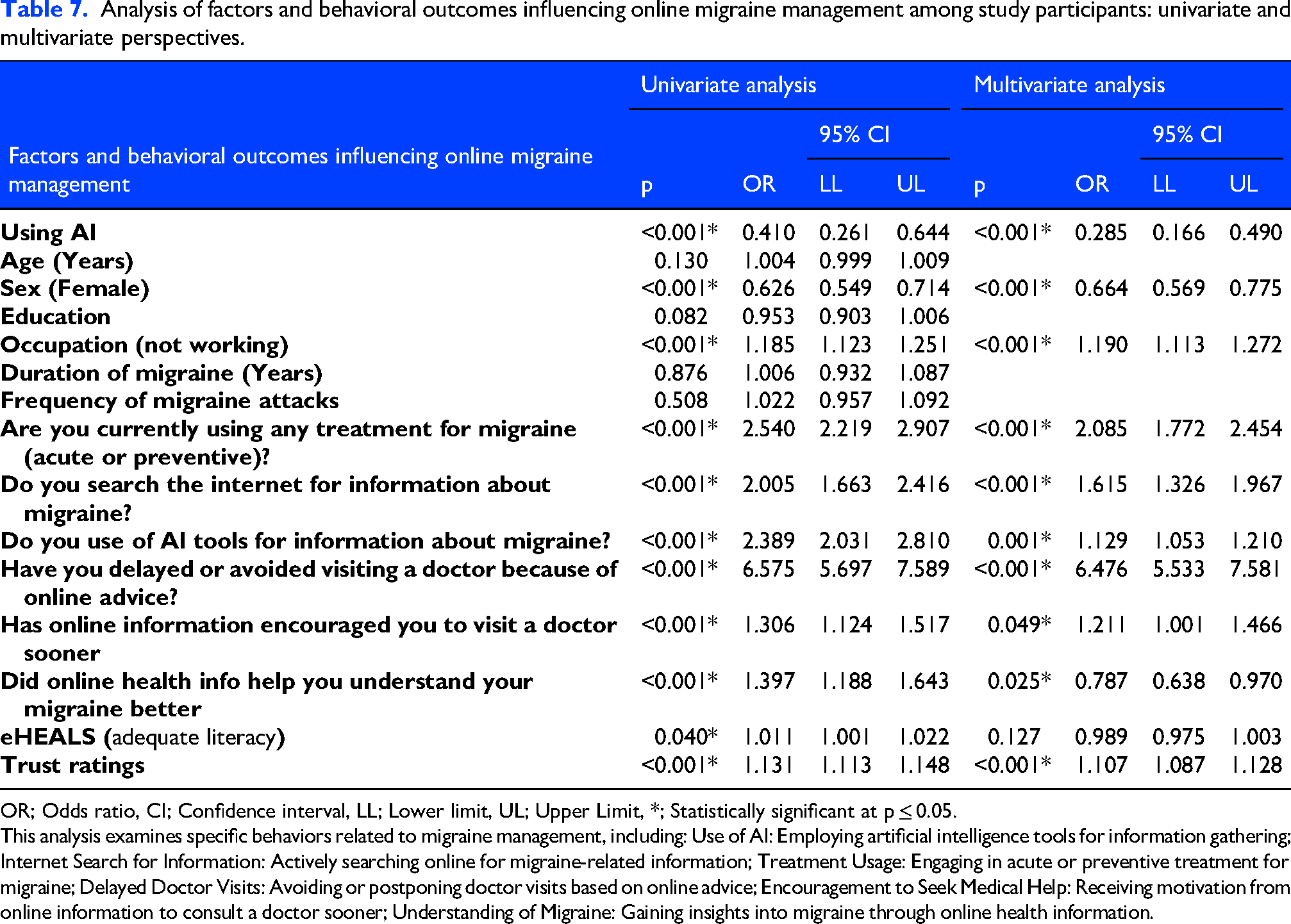
OR; Odds ratio, CI; Confidence interval, LL; Lower limit, UL; Upper Limit, *; Statistically significant at p ≤ 0.05.
This analysis examines specific behaviors related to migraine management, including: Use of AI: Employing artificial intelligence tools for information gathering; Internet Search for Information: Actively searching online for migraine-related information; Treatment Usage: Engaging in acute or preventive treatment for migraine; Delayed Doctor Visits: Avoiding or postponing doctor visits based on online advice; Encouragement to Seek Medical Help: Receiving motivation from online information to consult a doctor sooner; Understanding of Migraine: Gaining insights into migraine through online health information.
Discussion
The present findings underscore a pervasive reliance on digital sources for health information among migraine sufferers in the MENA region. Virtually all participants reported using the internet for health-related information, and approximately three-quarters had utilized at least one AI-based tool (e.g., ChatGPT) specifically for migraine information. This level of engagement aligns with global trends, as nearly 80% of internet users worldwide now seek health information online.22,23 However, the proportion of our cohort using AI chatbots is remarkably high. By comparison, only about 10% of Australian adults reported using ChatGPT for health queries in a 2024 national survey. 24 The notably higher uptake in our MENA sample may reflect the region's youthful, tech-savvy demographics and the need to fill gaps in healthcare access. Many MENA countries face limitations in healthcare infrastructure and specialist availability, which likely drives patients to supplement formal care with online resources.1,23 In addition, this difference may be partly explained by temporal factors, as AI-based health tools have received rapidly increasing public attention, improved usability, and wider dissemination in recent years between 2024 and 2026. Compared with studies conducted in 2024, AI platforms are now more accessible and routinely integrated into everyday information-seeking behavior, which may contribute to the higher prevalence of AI use observed in the present study. 21 Unfortunately, migraine care in the Middle East is often underdiagnosed and undertreated, with delayed referrals and restricted access to newer therapies being common. 25 In such a context, patients appear to have self-empowered through digital health avenues to understand and manage their condition in ways not fully addressed by traditional healthcare systems. Notably, healthcare providers remained the primary source of health advice in this study, reflecting a balance between traditional and online information channels. This aligns with global observations that the public still prefers and trusts physicians as their main health information source, regardless of digital literacy levels. 26 However, younger and more educated individuals tend to more readily supplement doctor's advice with online content.
A notable proportion of participants reported low headache frequency, with approximately 40% experiencing headaches less than once per month, and nearly half reporting no use of acute migraine medication. While this may initially appear inconsistent with migraine diagnosis, it reflects the well-recognized heterogeneity and fluctuating course of migraine. Individuals with a confirmed migraine diagnosis may experience prolonged interictal periods, remission phases, or low-frequency episodic attacks, particularly outside periods of heightened physiological or psychosocial stress. Moreover, underutilization of acute migraine treatment has been consistently reported in population-based studies, especially in regions where access to specialist care, medication availability, or health literacy may be limited. 11 In this context, digital health information–seeking may be particularly salient for individuals with infrequent attacks who are not engaged in regular pharmacological management but seek guidance during sporadic or unexpected episodes. Accordingly, the present findings should be interpreted as reflecting digital health behaviors primarily among individuals with lower-frequency or episodic migraine rather than high-burden or chronic migraine populations.
Our results highlight the double-edged nature of online health information on patient behavior. On one hand, a substantial subset of participants (roughly one-third) acknowledged changing or stopping their migraine medications based on online advice without consulting their physician, and a similar proportion reported delaying or avoiding a doctor's visit due to information obtained online. These findings echo growing concerns about misinformation and self-medication in the digital age. The ease of access to unverified advice can lead patients to make questionable decisions, a phenomenon sometimes referred to as the “Dr Google” effect. Prior studies have shown that information obtained from the internet can significantly influence patients’ treatment decisions and health behaviors, sometimes inappropriately.4,27 For example, exposure to unreliable or anecdotal claims may prompt patients to demand unnecessary interventions or forego established therapies. 27 In our study, this risk is particularly noteworthy given that participants reported comparatively low levels of trust in traditionally less reliable sources, such as social media influencers, while still demonstrating substantial behavioral impacts of online information use, including treatment modification and delayed care. This suggests that potentially unsafe behaviors may occur even in the absence of high explicit trust, likely reflecting repeated exposure, perceived convenience, or partial credibility attributed to digital content. Our observations of treatment changes and care delays are manifestations of this risk and underscore the importance of improving both the quality of online health content and patients’ ability to critically appraise information. Encouragingly, emerging research on AI-based health chatbots suggests that while these tools can deliver personalized and relevant information, they remain prone to inconsistencies and factual errors, reinforcing the need for robust digital health literacy among users. 1 In other words, patients must be equipped with the skills to distinguish credible guidance from misinformation when navigating online resources.
On the other hand, our findings also demonstrate clear benefits associated with online health engagement. The majority of participants felt that internet and AI resources helped them better understand their migraine and even prompted some to seek medical attention sooner. Such positive impacts illustrate the empowering potential of e-health for chronic disease management. By accessing educational materials and others’ experiences, patients may gain a greater sense of control and preparedness in dealing with their migraine. This is consistent with the concept of the “e-patient” — individuals who actively research their health conditions and arrive at consultations more informed and ready to discuss options. 28 Literature suggests that when used prudently, online information can improve patient–physician communication and engagement in care (for example, patients bringing well-formulated questions to their appointments).1,27,28 Possible explanation is that current AI chatbots often provide standardized, guideline-adherent advice with safety disclaimers. In fact, a 2023 evaluation of ChatGPT's medical responses found its information quality comparable to typical health websites (albeit still imperfect). 29 In our study, the fact that most respondents reported improved understanding and earlier help-seeking indicates that digital resources can complement professional care rather than only compete with it. Access to reputable online resources can empower patients by improving their understanding of the disease and its therapies, thereby reinforcing the importance of sticking to prescribed treatment plans. In the context of migraine, online communities and educational websites may help patients appreciate their treatment's mechanism and benefit, which in turn fosters compliance. A qualitative study from the UK found that migraine sufferers actively use social media to better understand their condition and treatment options, gaining peer support and validation in the process. 30 This suggests properly designed digital interventions might enhance patients’ knowledge and confidence in managing migraine. The challenge, therefore, is maximizing these empowering aspects while mitigating the hazards of incorrect self-management.
It is important to emphasize that trust itself is not negative – rather, the object of that trust (reliable versus unreliable sources) determines the outcome. Our regression analysis indicated that trust was higher among those with greater digital health literacy and education, which is encouraging since these individuals may be better at identifying reputable websites. In contrast, older age was associated with lower trust in online information (likely due to unfamiliarity or skepticism), and indeed prior studies confirm that older adults have more negative attitudes towards internet health content and prefer traditional sources. 31 We also found that current use of prescription migraine treatment was linked to lower trust in online info – perhaps reflecting that those actively managed by physicians rely more on their doctor's guidance. Overall, our findings underscore that trust is a critical mediator; when patients trust high-quality digital health information, it can reinforce positive health behaviors, but indiscriminate trust in the vast sea of online content can be hazardous. Taken together, the observed correlation patterns also suggest a dual pathway in digital health behavior among migraine patients. Digital health literacy appears to be shaped primarily by demographic and educational factors, whereas trust in online health information—and the behaviors it influences—seems more strongly linked to patterns of online engagement and perceived usefulness of digital information.
Balancing the pros and cons of ubiquitous online health information will require concerted effort. One immediate implication of our study is that healthcare providers in the MENA region should be cognizant of their patients’ online information-seeking and its influence. Clinicians should proactively initiate conversations about what patients have read online, to correct any misconceptions and guide patients to reputable, evidence-based sources. This supportive approach is crucial given that our data show patients are already heavily using – and sometimes acting on – digital content. If physicians dismiss or ignore this reality, there is a risk of eroding trust or missing an opportunity to steer patients toward safer choices. Conversely, embracing the role of a guide in the digital health landscape can strengthen the therapeutic alliance. For instance, providing patients with recommended websites or AI tools that are known to give reliable migraine information could harness the benefits of online engagement while reducing exposure to dubious advice. In Australia, where ChatGPT use for health is growing, general practitioners have noted the importance of offering patients vetted resources and discussing any online information they have encountered, to preempt misinformation-related harms. 32 A similar ethos should be adopted in the MENA context.
There are several limitations to our study. First, its cross-sectional design precludes any conclusions about causality. We identified associations between digital information usage and outcomes, but we cannot be certain of the direction of effect. For example, it is unclear whether using AI tools actively caused patients to avoid changing treatments, or if inherently more cautious patients tended to use AI tools. Longitudinal studies would be valuable to see if introducing a digital intervention changes patient behavior over time. Second, our data relied on self-reported behaviors and perceptions (e.g., treatment compliance, trust levels), which may be subject to reporting bias or inaccuracies in recall. Participants might have under- or over-stated their trust in online information or their tendency to change treatment, perhaps due to social desirability or recall error. Although all submitted questionnaires were complete, a conventional response rate could not be calculated because the survey was disseminated through open online channels without a predefined denominator. This limits the ability to assess non-response bias, a common challenge in large-scale web-based surveys. Third, there may be selection bias in our survey sample. Since the questionnaire was administered online, it inherently attracted respondents who are internet users and likely more eHealth-literate. This means our findings might not generalize to migraine patients who lack internet access or are not comfortable with digital tools (a group that still exists, especially among older or lower socio-economic demographics in the MENA region). The sample was also skewed by the characteristics of those who chose to participate; for instance, if more engaged or health-conscious patients responded, the dataset may overrepresent people inclined to be proactive about health information. Also, migraine diagnosis was self-reported, although participation was restricted to individuals who reported a prior diagnosis made by a neurologist. Nevertheless, the absence of independent diagnostic verification represents a limitation, particularly in light of the high proportion of participants reporting low headache frequency and should be considered when interpreting the overall disease burden in the study population. Consequently, the results should be interpreted with the understanding that the study population predominantly represents individuals with low-frequency or episodic migraine, and the generalizability of these findings to patients with high-frequency or chronic migraine may be limited. Future studies could further strengthen diagnostic reliability by incorporating independent diagnostic confirmation or validated screening instruments, such as the ID-Migraine questionnaire, particularly in large-scale or digitally administered surveys. Fourth, the present analysis did not differentiate between episodic and chronic migraine. The study was intentionally designed to focus on digital health information–seeking behaviors rather than detailed migraine phenotyping, and participants were not asked to self-classify migraine subtype. In large, self-administered surveys, self-reported differentiation between episodic and chronic migraine may be unreliable and could introduce misclassification bias. As most participants reported low monthly headache frequency, the findings likely reflect behaviors predominantly among individuals with episodic or lower-frequency migraine. Future studies specifically designed to capture migraine characteristics using validated instruments may explore subtype-specific differences. Fifth, while we focused on migraine patients in multiple MENA countries, there may be heterogeneity between countries that we did not fully explore. Cultural, economic, and healthcare system differences across the region could moderate how online information is used – but our analysis treated the MENA cohort mostly as a whole. This could mask important nuances (for example, trust in online health advice might be higher in countries with limited healthcare access, as people have fewer alternatives). Additionally, our measures of “using AI tools” or “internet search frequency” were fairly broad; we did not distinguish which websites or AI platforms were used. The quality and type of sources (e.g., consulting a certified health portal vs. random social media posts) were not tracked, yet these likely have a major impact on outcomes. Our measure of trust in online information was similarly general and not source specific. Also, the rapidly evolving integration of artificial intelligence into commonly used platforms introduces potential misclassification bias. Modern search engines increasingly embed AI-generated responses at the top of search results, and AI systems may draw on heterogeneous information sources, including social media platforms. Consequently, some participants may have reported using “Google” or social media without recognizing the presence of AI-generated content, or may have perceived these resources as distinct when, in practice, they overlap. This convergence of digital information sources may have blurred categorical distinctions between search engines, AI tools, and social media in participant reporting. Finally, there could be confounding factors we did not account for. Although we adjusted for several demographics and clinical factors in multivariable models, unmeasured variables (such as general health anxiety, personality traits, or access to healthcare) might influence both one's propensity to use online information and their health behaviors. These limitations suggest caution in interpreting the results and a need for further research to corroborate our findings.
As digital health tools grow in prominence, several areas warrant further exploration. In the MENA region, more research is needed to understand eHealth literacy across diverse populations, particularly older adults, rural communities, and those with limited education. Although participants were recruited from multiple MENA countries, we did not conduct sub-regional analyses, as the study was designed to provide a region-wide overview; future studies specifically powered for sub-regional or country-level comparisons are warranted. Such studies can guide targeted interventions like community workshops or clinical programs to build critical appraisal skills and combat misinformation. Intervention studies should test models like “online information prescriptions,” where clinicians recommend vetted digital resources or AI apps for migraine education. Collaborating with local health authorities to develop culturally relevant Arabic content and chatbots could improve access to trustworthy information.
Future work should also evaluate the behavioral impact of AI tools like ChatGPT through longitudinal designs, measuring whether access improves decision-making or reduces unnecessary care delays. As these tools become mainstream, monitoring not only their accuracy but also their influence on trust and compliance will be key. The rise of cyberchondria and mistrust in physicians underscores the need for psychological support and behaviorally informed interventions—especially for those prone to anxiety-driven internet use. Finally, comparative global studies would clarify whether observed patterns are universal or culturally specific. As digital-native generations age, integrating technology into care safely and equitably remains a critical challenge.
Conclusion
This study provides one of the first large-scale assessments of digital health engagement and its association with migraine-related decision behaviors in Arabic-speaking countries of the MENA region. While healthcare professionals remained the most trusted information sources, online health information and AI tools were widely used and were significantly associated with treatment modification and care-seeking behaviors. AI tool use was independently associated with younger age, male sex, and active online information-seeking, reflecting a distinct demographic profile of users. In multivariable analyses, higher trust in online information was associated with delayed medical consultation and treatment changes, whereas AI use was associated with more cautious treatment-related behaviors.
These findings should be interpreted in light of the cross-sectional and exploratory nature of the study, which precludes causal inference. Nonetheless, the results highlight the importance of strengthening digital health literacy and guiding patients toward reliable, evidence-based online resources to support safe and informed migraine self-management.
Article highlights
Digital information use is widespread among migraine patients in the MENA region, with over 80% searching online and 72% using AI tools. Digital health literacy was generally high and associated with younger age and higher education. Online information influences care-seeking behavior, sometimes leading to treatment modification or delayed consultation. Guidance toward reliable digital and AI resources is essential to ensure safe migraine self-management.
Supplemental Material
sj-docx-1-cep-10.1177_03331024261435594 - Supplemental material for Influence of online health information and artificial intelligence on decision-making among migraine patients: A multinational cross-sectional study from the MENA region
Supplemental material, sj-docx-1-cep-10.1177_03331024261435594 for Influence of online health information and artificial intelligence on decision-making among migraine patients: A multinational cross-sectional study from the MENA region by Ahmed Dahshan, Marwa Ibrahim Mahfouz Khalil, Dalia Abdelfatah, Moath Abu Ejheisheh, Mohammed Salfeeq H. Alshammari, Ahmed Khalaf Mekdad, Ali Malik Tiryag, Ghada Mohamed Attia Sherif, Fatima Hallaj, Asmaa Hammooz, Merghani A. Hussain Abdallah, Samia Ibrahim Mabrouk Baraka, Nagwa Ibrahim Mabrouk Baraka, Ahmed Nouralhadi Ali Ibrahim, Ali Mohammed Noor, Adam Mahmoud Salameh Khraisat, Ahmed Awad Osman Mohammed, Lina Ahmed Elmobarak Eltayeb, Majdi Alhadidi, Nada Ab. Hweissa, Hassan Abdullah Ahmed Al Buraiki, Olaa Abdalslam Ibraheem, Basma Salameh, Samaa Ahmad Akram Al Tabbah, Nabih Mohammad Lawand, Khulud Ahmad Rezq, Nadia Mohamed Ibrahim Wahba, Karrar Najah Abd Al Jaleel, Nawal Ali Albagoush, Wael Alwahchi, Khulud Mohammad Hashem Mansor, Ahmad Bahjat Ahmad Al-Rawashdeh, Taliaa Mohsen Al-Yafeai, Haia Mahdi Hindi Albalawi, Alaeldeen Hakim Mohamed Hakim, Enas Fouad Sayed Mousa, Hosny Maher Sultan Sultan, Nawara Khirallah Abd El Fatah and Mohammad A. Farrag in Cephalalgia
Footnotes
Acknowledgements (Use of AI):
The authors acknowledge the use of artificial intelligence (AI) tools specifically Qwen 2.5 max and chat GPT plus solely for drafting assistance and language corrections. These tools were utilized to enhance clarity, grammar, and overall readability of the manuscript while ensuring that all scientific content, data interpretation, and intellectual contributions remain the original work of the authors. The integrity and authenticity of the research are fully maintained.
ORCID iDs
Ethical considerations
Ethical approval was granted by the Research Ethics Committee at the Faculty of medicine, Alexandria University, Alexandria, Egypt, obtained in April 2025 under number 0307430. The study emphasized anonymity, voluntary participation, and the right to withdraw at any time. Confidentiality was maintained, and responses were anonymous, with no identifying data collected. The study adhered to the ethical principles outlined in the latest version of the Declaration of Helsinki (2013).
Consent to participate
Digital written informed consent was obtained from the study participants for publication of this manuscript and any accompanying images.
Author contributions
A.D., M.A.F., M.I.M.K., and D.A. contributed to the conceptualization and design of the study. Methodology was developed by A.D., D.A., M.A.F., A.K.M., and E.F.S.M. Questionnaire development and validation were performed by A.D., M.I.M.K., D.A., M.A.H.A., and K.A.R. Data collection and coordination were undertaken by M.A.E., M.S.H.A., A.K.M., A.M.T., G.M.A.S., F.H., A.H., M.A.H., S.I.M.B., N.I.M.B., A.N.A.I., A.M.N., A.M.S.K., A.A.O.M., L.A.E.E., M.A., N.A.H., H.A.A.B., O.A.I., B.S., S.A.A.T., N.M.L., N.M.I.W., K.N.A.J., N.A.A., W.A., K.M.H.M., A.B.A.A., T.M.A., H.M.H.A., A.H.M.H., H.M.S.S., and N.K.A.F. Statistical analysis was performed by D.A., M.A.F., D.A., and A.D., while data interpretation was carried out by A.D., M.A.F., D.A., M.I.M.K., and N.M.I.W. The manuscript was drafted by A.D., M.I.M.K., D.A., and M.A.F., and all authors contributed to critical revision of the manuscript. Supervision was provided by A.D., M.A.F., and M.I.M.K., and project administration was managed by A.D. and M.A.E. All authors approved the final manuscript and agreed to be accountable for all aspects of the work.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Open practices
Pre-print server
Supplemental material
Supplemental material for this article is available online.
