Abstract
Purpose
The International Classification of Headache Disorders (ICHD) is universally accepted and forms the basis of headache management and clinical, experimental and pharmacological headache research. The present review summarizes the history of the three different editions of the classification, concentrating on aspects of general interest that are still valid today.
Methods
The article is based on the memory of the chairperson of three editions of the International Classification and on his notes in the work copies and published scientific classification studies.
Results
Many of the crucial issues in headache classification are discussed in the review of the different editions. Some have been resolved and some remain unresolved. The 11th edition of the World Health Organization’s International Classification of Diseases (ICD) has been developed in close contact with the International Headache Society classification committee and is in fact an abbreviated version of ICHD-3. The principles of the ICHD have also been used by the International Association for Study of Pain in developing a pain classification now included in ICD-11. The many points of discussion of each of the three editions are still relevant for headache experts and all those who care for headache patients.
Conclusion
Headache classification is a living and developing discipline of research. Here, the gradual expansion and refinement of the classification through 3 different editions are discussed with a view to present day relevance.
Introduction
Today every headache scientist, every clinically working headache specialist and most general neurologists as well as the pharma industry accept and use the International Classification of Headache Disorders 3rd edition (ICHD-3) (1). The recent International Classification of Diseases 11th edition (ICD-11) (2) from the World Health Organization (WHO) has modelled its headache section after the ICHD-3. There are no competing classifications, and the ICHD-3 has been translated into more than 20 languages. Patients are now diagnosed in the same way throughout the world. Research results from one country are therefore valid in all other countries. Our migraine drugs have been developed in studies of patients diagnosed according to ICHD and therefore are valid throughout the world. The success of the headache classification has been considerable.
It is difficult to fully understand the classification and its explicit diagnostic criteria. Why not a simpler classification for clinical practice? Why distinguish between migraine with-and without aura? Why chronic migraine? Why not secondary migraine? Why persistent headache after causative events? etc. The questions are many, and they are perhaps best answered by an account of the history of our headache classification (3,4). The present author has had the privilege to chair the classification work during more than thirty years. His account in the following may therefore be of general interest. It will provide new insights into the classification and promote its correct use. Hopefully, reading about the many uncertainties will also stimulate increased classification research. The review finishes with some suggestions for the future.
Methods
The material used is the personal copies of all the published ICHD editions containing the chairperson's handwritten notes in addition to extensive postal mail and e-mails. Memories of discussions at important meetings have also been used as well as published classification studies. It also contains the author’s personal impressions and interpretations.
Headache classification and definition before ICHD-1
There are excellent published descriptions of migraine in the world literature dating all the way back to the 19th century, but also many different opinions and considerable variability from country to country and the nomenclature varied a lot between countries. Obviously, there was a need for international standardization. The first attempt at official classification (Figure 1) was made by an ad hoc committee of the US National Institutes of Health (NIH) published in 1962 (5).

The first official headache classification by an ad hoc committee of the US National Institutes of Health suffered from the use of many soft formulations here shown in red font (5).
The significance of this initiative was that it was authorized by a highly prestigious institution and not just the opinion of a single investigator or a group of investigators. On the other hand, it was a US institution and not an international institution. Furthermore, the classification was very limited in scope, and it was already disputed at the time of its publication. For example, cluster headache was grouped among vascular headaches of the migraine type. which already at the time was not generally accepted. The attempt at a “definition” of migraine was full of soft wording exemplified in Figure 1. Words like sometimes, often and usually meant that interpretation was totally up to each investigator and inter investigator reliability almost certainly must have been very low. In 1969 the World Federation of Neurology Research Group on Headache gave a definition (6). This time the classification was supported by an international body but unfortunately it suffered from the same limitations as discussed above. In practice the scientific literature has most often referred to the NIH publication.
When the present author started the Copenhagen Acute Headache Clinic in 1976, he saw hundreds of patients during an acute migraine attack. He noted a wide variation in symptomatology and problems in separating migraine from cluster headache and muscle contraction headache, as tension-type headache was then called. Existing criteria did not help deciding the diagnosis in the individual case. Based on an analysis of 750 acute headache cases with systematic and detailed recording of symptoms (7), he therefore developed his own more explicit diagnostic criteria for migraine without aura, then called common migraine: common migraine is a disorder characterized by recurrent attacks of headache of unknown etiology. The headaches must be associated with gastrointestinal dysfunction (nausea or vomiting) or with at least two of the following symptoms: unilateral pain location, pulsating quality of pain, sensory hyper irritation (photophobia or phonophobia) or other visual disturbances. A separate definition for migraine with aura then called classical migraine was also suggested. These relatively precise data-driven definitions of migraine were used in our studies of regional cerebral blood flow during migraine attack which showed major differences between the two types of migraine. But there was no hope of gaining international acceptance of these suggestions. It was obvious that an international association had to endorse a headache classification but there was no suitable organization.
The first International Headache Classification, later called International Classification of Headache Disorders 1st edition (ICHD-1)
In 1982 the International Headache Society (IHS) was formed and in subsequent years it obtained universal participation. IHS would be the right sponsor of a future headache classification. During the second IHS congress in Copenhagen 1985 the present author proposed an IHS classification committee. He was appointed chair of that committee with a free hand to choose committee members and define the methods of the work. Three challenges needed to be addressed: choice of work methods and scope; selection of membership; and finance.
The classification of the other neurological disorders was screened but nothing useful was found. The other neurological disorders were just as poorly defined as headache disorders. Among other somatic diseases rheumatological diseases had somewhat useful definitions but they depended heavily on biomarkers. Finally, the psychiatric classification diagnostic and statistical manual 3 (DSM-3) came to our attention (8). It did not use biomarkers but was exclusively based on patients' history. Furthermore, the psychiatrists had worked out a whole methodology of classification. We decided to use their methodology in a simplified version using only one axis.
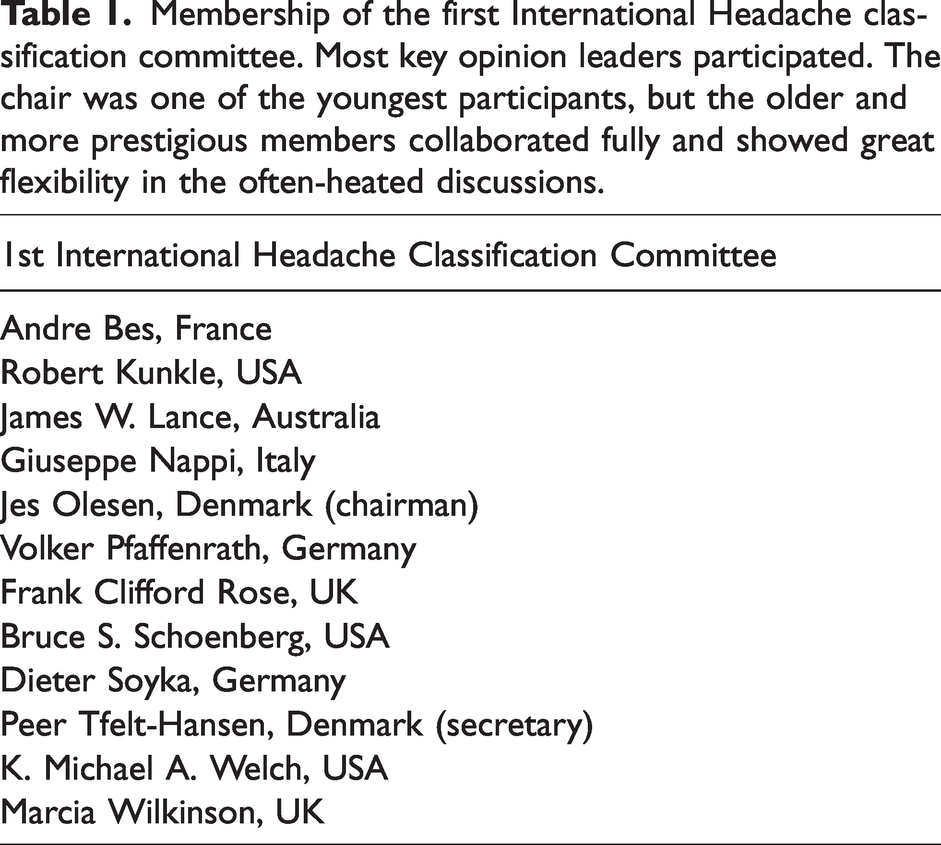
Regarding membership, several factors had to be considered. Most important was of course clinical and scientific expertise but also geographical spread and role as key opinion leader counted with a view to future acceptability of the classification. Everybody asked fulfilled these criteria and they all accepted (Table 1).
Membership of the first International Headache classification committee. Most key opinion leaders participated. The chair was one of the youngest participants, but the older and more prestigious members collaborated fully and showed great flexibility in the often-heated discussions.
Lastly the finances had to be found. The IHS had no money before the advent of triptans. The problem was managed with support from four major pharmaceutical companies: Janssen, Sandoz, ICI and Glaxo. They were contacted directly by the chair.
At the first meeting it was discussed whether there should be a simple classification for clinical practice and a more elaborate for research. External experts in disease classification Bruce S. Schoenberg and Harrison Graham Pope Jr. made it clear that there should be only one classification. Otherwise results from scientific studies could not be transferred to clinical practice. The solution would be a hierarchical classification where it was possible to diagnose at different levels of sophistication. General practice could diagnose at the one- or two-digit level and research also at digit 3,4 or 5. A proposed list of chapters of the classification was discussed and amended resulting in 13 groups (Table 2).
Major groups of headache agreed at the first meeting of the ICHD-1 committee.

It was decided that each group (chapter in the forthcoming publication) was to be chaired by a member of the committee. Each group chair should appoint members of a working party to prepare that chapter of the classification in a close dialogue with the main committee. To assure a certain homogeneity the chairman of the committee not only chaired migraine and tension-type headache groups but also became a member of all working groups. This meant that he received all minutes from the working parties and could comment. In deciding the diagnoses to be included in each chapter all available information should be used, such as positron emission tomography (PET) and other scanning results, advanced chemistry, genetics etc. They would not normally be available to the diagnosing physician but should be used in developing the hierarchy of diagnoses, the classification. But how many diagnoses should be included? This is most easily understood looking at headache attributed to infection. So-called splitters would include every single known infection that can cause headache while so-called lumpers would include only very major groups of infection. A compromise should be found taking into consideration how important the headache attributed to the particular infection is. Similar reasoning should be applied to all other secondary headaches.
Principles of operational diagnostic criteria (as they were called at the time, today explicit diagnostic criteria) were presented by the external experts in disease classification. Diagnostic criteria should only include clinical features and simple tests available to the diagnosing physician Everything should be explicit and unambiguous, and numbers should be given everywhere even in the absence of scientific support and just based on the opinion of experts. Once numbers are given they can easily be tested and amended in the future. This was successfully used in the development of the classification. The goal for a set of diagnostic criteria is to be both sensitive and specific. Highly sensitive criteria are very open. They require very little and therefore include all patients with a disorder, but also patients without it. Highly specific criteria are very strict. They require a lot and therefore include only the most typical cases but leave out many patients who actually have the disorder. The goal for diagnostic criteria is to have the right balance between sensitivity and specificity. Solid scientific data are necessary to get this completely right but they are often lacking, particularly when developing ICHD-1. In such a case the collective opinion of experts provides the best possible surrogate and it actually proved quite valid. Every word and every number were discussed and in this way the diagnostic criteria were fine tuned. Other requirements were that each different headache should fit one and only one set of diagnostic criteria. In other words, the diagnostic criteria must not overlap. Finally, the classification should be exhaustive meaning that there should be a diagnosis for every different headache that exists.
It was also decided how the text should be structured: Introductory text to the chapter, then for each disease: Previously used terms, Description (previously called definitions), Diagnostic criteria, Footnotes and Comment. At the end of the future document were References, Definition of terms and Index.
In the following section a few of the most controversial issues in ICHD-1 that are still valid today will be discussed. Should migraine with and without aura be distinguished? Many thought not but already the previous classifications had made this distinction. Now, studies of regional cerebral blood flow show marked changes in migraine with aura but no changes in migraine without aura (9,10). What about patients with both forms of migraine? The conclusion was to create separate diagnostic criteria and to give two diagnoses in those with both forms of migraine. This decision was in accordance with the principles of the WHO and has later been proven right by extensive imaging as well as genetic and other research.
Can migraine be secondary? There was no doubt that a headache phenotypically fulfilling the migraine criteria could arise in close temporal relation to a secondary cause, but it was decided that it was not migraine but a secondary headache of the migraine type. How similar are these migraine-like headaches to genuine migraine? They seem not to respond well to specific migraine medicine, but the issue is not yet fully clarified.
Muscle contraction headache had to be renamed as there was no evidence of muscle contraction as the cause of these common headaches. Tension headache used in the English-speaking countries had a psychiatric taste. We therefore chose Tension-type headache. It was hugely prevalent and ranged in severity from rare to daily and therefore might benefit from subdivision. Otherwise, it might be disregarded because of its extremely high prevalence and mild severity. In order to direct attention to the severe forms of tension-type headache it was decided to divide it into episodic and chronic tension-type headache, the latter requiring 15 days of headache or more per month. This limit was decided based on the opinion of experts, but it has later been substantiated and used also for chronic migraine and medication overuse headache. It has proven useful in those disorders, but chronic tension-type headache has not received much scientific interest or interest from the pharma industry. There are still no drugs registered for the treatment of chronic tension-type headache.
Regarding the secondary headaches, they were called: headache associated with the causative disorder because the causal relationship was felt to be uncertain in most cases. An important asset in ICHD-1 was a list of phenotypically different secondary headaches such as Migraine-like, Tension– type-like, local lesion-type etc. coded by a fourth digit. Chronic use of substances was recognized as a cause of headache but only after daily intake. However, the beginning was made for the recognition of medication overuse headache.
The International Classification of Headache Disorders 2nd edition (ICHD-2)
It was expected that a second edition should be published a few years after the first because we were not sure that the first was good enough. The receipt of ICHD-1 was, however, very positive. Approximately 100,000 copies were distributed by pharma companies and in addition it was translated into more than 20 languages. Furthermore, new data relevant to classification were very slow to come. For these reasons the work on ICHD-2 started only in the year 2000. It was a revision of the existing document and therefore expected to be fast, but it took three years, the same as for ICHD-1. The document was published in 2004 and it was double the size of ICHD-1 and extensively revised. Only the chair and two more members of ICHD-1 continued while the rest were new to classification and younger. Finance was now provided by the IHS keeping industry at arm’s length. As previously, all meetings were open to those interested and a couple of major public meetings were organized during the process. Only the most important changes can be mentioned in the following but there were changes on almost every page. The basic principles of ICHD-1 had stood the test in real life and virtually all of them were continued. Thus, it had been shown that the classification was exhaustive meaning that all headaches could be classified (11). It was valid because triptans given as injection relieved 80% of patients diagnosed with migraine according to ICHD-1 (12) and it had high reliability (13). It was also applicable in all medical settings (14) and, according to the results of triptan trials, it resulted in similar diagnoses across the world. Therefore, the new committee used the same general approach and it preserved many of the explicit diagnostic criteria with confidence, most notably the criteria for migraine without aura where only a minute change was made to criterion C4.
The ICHD-2 was now divided into three parts: 1. Primary Headaches, 2. Secondary Headaches and 3. Cranial Neuralgias, Central and Primary Facial Pain and Other Headaches (4). It was agreed to distinguish between non-pathological causative factors (trigger factors) that would still be compatible with a primary headache diagnosis and pathological factors such as disease, trauma or drugs. Therefore group 4 headaches were now primary without a doubt. The secondary headaches were now called ‘attributed to a disorder’, not ‘associated with a disorder’ as previously. We had become more confident of their causality.
In migraine a small addition was made that later in modified form proved to be very important and very beneficial: chronic migraine was included but as a complication to migraine and with very strict criteria requiring 15 days per month fulfilling the diagnostic criteria for migraine without aura and no medication overuse. This was too strict and softer criteria were published later in an article in Cephalalgia authorized by the whole committee (15). Migraine without aura criteria remained unchanged but there were small changes to migraine with aura. In ICHD-1 headaches not quite fulfilling the diagnostic criteria for any of the forms of migraine were called migrainous disorder. In ICHD-2 and ICHD-3 these headaches were called Probable migraine. This entity is necessary for the exhaustiveness of the classification but they can cause problems in epidemiological studies.
In tension-type headache the listing of most likely causative factor was dropped. Episodic tension-type headache was divided into infrequent (less than 1 day per month) and frequent (2–14 days per month). Further subdivision was made according to presence or absence of pericranial tenderness. Sadly, this has not been followed by relevant research. The term trigeminal autonomic cephalalgias was now used for chapter 3 and short-lasting, unilateral, neuralgiform headache attacks with conjunctival injection and tearing (SUNCT) was added. Paroxysmal hemicrania was divided into episodic and chronic. Chapter 4 now called ‘Other Primary Headaches’ was extensively revised and expanded. However, external compression headache and cold induced headache were moved to another chapter. Hypnic headache, thunderclap headache, hemicrania continua and new daily persistent headache were included for the first time. The explicit diagnostic criteria were all revised, expanded and made more operational.
ICHD-2 did not attempt to characterize the phenotype of secondary headaches except for a few specific causes of headache. In ICHD-1 there had been a list of the type of headache (migraine-like, tension-type-like etc.) but it was dropped in ICHD-2 (and ICHD-3). It should probably be reintroduced in forthcoming editions. In ICHD-1 the secondary headaches were generally quite superficially described. This was amended in ICHD-2 where the part on secondary headaches was much enlarged and the literature work behind the classification was much more thorough. It is beyond the scope of this article to give an account of all the many changes to each chapter, but a couple must be mentioned. Medication overuse headache had previously been called medication abuse headache, rebound headache, drug-induced headache and medication mis-use headache. It was the “psychiatrist of headache”, Fred Sheftell, untimely deceased, who promoted the balanced and acceptable term: medication overuse headache. The patients were not drug abusers, but mostly innocent over-users often encouraged by their doctors. The disorder was defined by strict numbers of days of intake decided as consensus among the experienced committee members in the complete absence of data. Remarkably these limits for intake have proved valid and no evidence has challenged them. The entity is probably the biggest iatrogenic problem of all and in the Global Burden of Disease (GBD) study it accounted for a lot of disability (16). In the most recent GBD study it is included in the burden of migraine and tension-type headache and adds considerably to their burden. For the ICHD it is, however, preferable to preserve medication overuse headache as a separate diagnosis as was also done in ICHD-3.
In ICHD-1 psychiatric disorders were thought in some cases to be causative for tension-type headache but to have no other relation to headache. The ICHD-2 committee believed that psychiatric disorders could sometimes cause headache. A parallel to somatic diseases. Therefore chapter 12 was devoted to headache attributed to psychiatric disorder. This was, however, not substantiated by data. For mostly historical reasons only two entities were therefore included: Headache attributed to somatization disorder and Headache attributed to psychotic disorder. The hope was that this small chapter would prompt psychiatrists to study headache in their patients.
The last major novel section in ICHD-2 was an appendix. The idea was to move diagnoses from the main body of the classification that remained unsupported by data to the appendix as a first step and to delete them in a subsequent edition if no scientific support had appeared. New diagnoses not yet sufficiently supported by data but to be considered for future editions were included. Finally, the appendix contained diagnostic criteria alternative to those in the main body of the classification in the hope that they be scientifically tested versus the main body criteria. A shortened pocket version and an official slide kit were produced and made freely available in order to spread the use of the classification as widely as possible.
During the development of ICHD-2 the committee kept in close contact with WHO, who were developing ICD-10. Professor Jean-Marc Orgogozo was an important liaison person at the WHO. It was possible to achieve major changes to ICD-10, thus making it more compatible with ICHD-2. After the publication of ICHD-2 Professor Hartmut Göbel and the present author published a go-between ICHD-2 and ICD-10 section on headache (17). This was meant to facilitate routine coding in the clinic where diagnosis would normally be made using ICHD-2 but ICD-10 code numbers were needed for reimbursement and other statistical purposes.
The International Classification of Headache Disorders 3rd edition (ICHD-3)
The course of developing ICHD-3 was somewhat different from the previous editions. Work started already in 2010 only six years after the publication of ICHD-2. The reason for this early start was partly that more evidence had been published, but more importantly there was a strong widespread desire to include chronic migraine in a better way. After 3.5 years of work, we decided to publish a beta version (18) for two reasons. Firstly, it would allow field testing of the document before it became final. Secondly, the development of ICHD-3 had been done in close collaboration with WHÒs work on ICD-11 and almost complete congruence and a separate headache chapter in ICD-11 had been secured. But from the almost final ICD-11 draft document until a lot of formal procedures had been finished would take a long time. Our hope was that after the test period of ICHD-3 beta final code numbers for ICD-11 would be available. Unfortunately, the ICD-11 was greatly delayed and in the end ICD-11 code numbers were not included in the final ICHD-3. Today the ICD-11 is a less detailed version of ICHD-3 without explicit diagnostic criteria. A crosswalk between the two classification code numbers would be useful, maybe as a pocket version.
In the following we skip ICHD-3 beta and discuss only the ICHD-3 proper published in January 2018 (1). It was financed by the IHS and it used the same basic construct as the previous editions. The committee membership was expanded to 18 of whom only four had previous experience. Only the chair had participated in both previous editions. The resulting document was more than 200 pages long and contained a lot of new scientific information. Only a few of the many changes can be mentioned here.
It is not always clear how the classification should be used and therefore all three editions have had a section with instructions for this. The ICHD-3 contains the largest and most elaborate version which should be read by all headache experts. Among the questions were: How detailed should one classify? What about headaches that have disappeared before the consultation? What if a patient has more than one type of headache? What about frequency and severity of the headache? Is a headache primary or secondary? Do less typical attacks also count? There are several additional answers to be answered in this section.
The subdivision of migraine was hotly debated before ICHD-2 and ICHD-3. Should we divide into menstrual and non-menstrual? Into sensitizers and non-sensitizers? Or into treatment refractory and not refractory? Several other proposals were presented. The problem is that every new way of subdividing has to be carried through the whole classification and will double its size and complexity. Therefore, all these possible subdivisions were refused. But subdivisions should be studied scientifically. Thus, it is desirable to study men vs women, sensitizers vs non-sensitizers, patients with prolonged aura vs normal auras etc., but that can be done perfectly well without making the classification more complicated.
Migraine without aura remained unchanged in ICHD-3 but field testing resulted in a major change in the criteria for migraine with aura (19). Three out of six characteristics now had to be fulfilled enabling a much better distinction between migraine with aura and transient ischemic attack.
Even more important was the inclusion of explicit diagnostic criteria for chronic migraine as a main sub form coded 1.3. Previously it was a complication to migraine. The inclusion presented a problem because it seemed to be a new subdivision into episodic and chronic migraine. Some felt that all the different kinds of migraine should then be subdivided, but this was avoided because chronic migraine includes both migraine with and without aura as well as tension-type headache. In this way we avoided that there should be an entity called episodic migraine. The fact that many authors have subsequently used this term is another matter which is up to each author to personally decide. Absence of medication overuse was no longer required for chronic migraine. Instead, patients should receive two diagnoses: chronic migraine and medication overuse headache.
No major changes were made in tension-type headache but in trigeminal autonomic cephalalgias short-lasting unilateral neuralgiform headache attacks with cranial autonomic symptoms (SUNA) was added. Hemicrania continua was moved to this chapter and divided into episodic and chronic. Following the decision that non-pathological causative factors were triggers and not causes of secondary headaches, cold stimulus and external pressure and traction headache were moved back to chapter 4 which generally benefitted from better published evidence.
A major improvement was made to the diagnostic criteria for secondary headaches. ICHD-1 and ICHD-2 required that headache should disappear or greatly improve after treatment or spontaneous recovery of the causative factor in order to make a definite diagnosis. Diagnoses must, however, often be made at the first patient encounter. The general diagnostic criteria for all secondary headaches in ICHD-3 made this possible. They were a template to be modified for each kind of secondary headache. These diagnostic criteria allowed immediate diagnosis because causality could be shown before the secondary cause improved (Table 3).
General diagnostic criteria for the secondary headaches in ICHD-3.

There are two reasons why the secondary headaches are important. Firstly, they direct doctors to the diagnosis of the causative disorder which is often serious and urgently in need of treatment. Headache is in fact the single most common neurological symptom leading to emergency visits. Secondly, some of the secondary headaches represent by themselves a therapeutic problem that must be addressed. Medication overuse headache and chronic post-traumatic headache are examples of this. ICHD-3 does not distinguish between these kinds of headache but headaches that persist after treatment or spontaneous remission of the causative disorder belong to this category and they received more attention. In ICHD-1 and 2 only persistent headache after trauma and after bacterial meningitis were recognized, but ICHD-3 included several such headaches for example headaches persisting after stroke, arterial dissection and reversible cerebral vasoconstrictor syndrome. But still most chapters included no persistent headaches because no data support was available. Persistent headaches probably occur after most of the secondary causes. They represent a very important field of research for the future.
The chapter on headache attributed to psychiatric disorder was not changed because it had not received any scientific study. In the hope of stimulating such research, explicit diagnostic criteria were presented for several psychiatric disorders in the appendix.
Considerable effort was spent on trigeminal neuralgia. The IHS working party collaborated with a group from the International Association for the Study of Pain. Later a group of independent researchers with an interest in trigeminal neuralgia published their own classification in Neurology (20). Their views were also taken into account and the end result published in ICHD-3 was a compromise.
The appendix was much enlarged compared to previous editions. It included explicit diagnostic criteria for vestibular migraine, a much-disputed entity previously very poorly defined. The appendix criteria were the result of collaboration between the working party on migraine classification and the Barany Society representing the expertise in vertigo. Unfortunately, no thorough field testing of the ICHD-3 criteria has been published during the five years following publication. Also, the rest of the extensive appendix has received little study.
Interestingly, the International Association for the Study of Pain (IASP) was inspired by the ICHD and received advice from Professors Stefan Evers and Arne May. In close contact with WHO the IASP committee headed by Professor Rolf-Detlef Treede developed a new pain classification that allowed inclusion of so-called primary chronic pain disorders in ICD-11. This was the first time that pain syndromes received their own section in WHO's disease classification. The collaboration also resulted in a classification of orofacial pain (21).
Future perspectives on headache classification
There were 16 years between ICHD-1 and ICHD-2. ICHD-3 followed 14 years after ICHD-2. If usual procedure is to be followed, work on the 4th edition of the ICHD will not start until approximately ten years after the publication of the ICHD-3. One might argue that the classification has been greatly improved over the three editions and therefore change should happen because of new scientific data and not because of personal views. This requires ample time for classification research to solve some of the outstanding issues. Fortunately, this type of research has increased considerably in recent years.
In 2014 right after publication of the ICHD-3 beta, the present author described many issues that remained unresolved (22). Some of them were later clarified and included in ICHD-3, but most remain unresolved to the present day. Other problems became apparent later.
It should be possible to diagnose migraine and tension-type headache unspecified i.e. at the first digit level. A solution has been suggested and amended and is ready for use (23). Tighter criteria for migraine with brain stem aura have been suggested based on extensive field testing (24) but it may still not provide sufficient distinction from vestibular migraine. The general rule is that appendix criteria can advance to the main body if supported by good studies, but they should be deleted if evidence is not published. Vestibular migraine is therefore a candidate for exclusion unless field testing results are soon published. The same can be said about the chapter on headache attributed to psychiatric disorder and the associated appendix criteria. Retinal migraine has long been a candidate to be moved to the appendix. There is still no good scientific support for its existence. It has proven useful that we singled out the severe end of the migraine specter as chronic migraine (CM). It directed interest towards the most affected patients and has promoted their treatment. However, its diagnostic criteria are bizarre including migraine without aura, migraine with aura and tension-type headache phenotypes. Evidence has been presented to simplify the criteria to just require 8 days with migraine per month (25,26). In the appendix of ICHD-3 criteria are given for CM with continuous pain and CM with pain free days. No formal testing of these criteria has been done but patients with continuous pain are known to be particularly difficult to treat. Tension-type headache is the most prevalent headache but lives a secret life. Scientifically it is where migraine was 50 years ago. However, as migraine mechanisms become known and a multitude of treatments become available, the search light will inevitably be directed towards tension-type headache. It remains a problem, therefore, that the separation between tension-type headache, cervicogenic headache and temporomandibular disorder is poor. A solution has been proposed but a decision of the new classification committee is necessary (22).
The word chronic is used with different meanings. In migraine and tension-type headache it means frequent, but in cluster headache it means without remissions. Cluster headache would be better defined as remitting and unremitting. Regarding chapter 4, the criteria have already been tested in Asians. They should be tested in Caucasians and Africans. The possibility of polythetic rather than the present monothetic criteria should be considered.
Novel general criteria for the secondary headaches have been suggested based on extensive study (26), but even these criteria do not always make causality certain. Chiari malformation remains, for example, an uncertain cause of headache but nevertheless many patients get operated on because of headache. Persistent headache secondary to another cause is missing in several chapters. Hopefully novel research will enable inclusion of more such headaches.
Headache attributed to insignificant head trauma such as banging the head on a door is common. It is similar to new daily persistent headache but has an (unlikely?) cause. It should be studied and included. Shorter titles or acronyms should be considered for post traumatic headaches. In fact, authorized acronyms should be developed for all headaches by the new committee. Criteria for headaches attributed to cerebrovascular disorders have been field tested (27,28) and the resulting changes should be considered for inclusion in ICHD-4.
Conclusion
Thirty years of extensive committee work on three editions of the International Classification of Headache Disorders has resulted in an excellent classification that probably is more advanced than the classification of most other neurological diseases. It has greatly promoted headache research, drug development and clinical practice. Nevertheless, a lot of possibilities for further research to improve the ICHD exist. Changes will be easy to implement because the explicit diagnostic criteria allow easy modification. Unfortunately, there is still a relative paucity of classification research.
Clinical implications
Everybody caring for headache patients should know the International Classification of Headache Disorders (ICHD). This historical account is an easy way to understand the principles behind ICHD. The article points to several important topics for future research.
Footnotes
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Jes Olesen was chairperson from 1985-2018.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
