Abstract
Background
A model for the testing of novel anti-migraine drugs should preferably use healthy volunteers for ease of recruiting. Isosorbide-5-mononitrate (5-ISMN) provokes headache in healthy volunteers with some migraine features such as pulsating pain quality and aggravation by physical activity. Therefore, this headache might respond to sumatriptan, a requirement for validation of any model. The hypothesis of the present study was that sumatriptan is effective in 5-ISMN-induced headache in healthy individuals.
Methods
In a double-blind, randomised, crossover design, 30 healthy volunteers of both sexes received 5-ISMN 60 mg on two separate days, each day followed by oral self-administered placebo or sumatriptan 50 mg. Headache response and accompanying symptoms were registered in a questionnaire by the participants themselves.
Results
5-ISMN induced a reproducible headache in all 30 participants. The headache had several migraine-like features in all participants and 20 individuals developed a migraine-like attack. Median peak headache score was 5 on both experimental days (p = 1.00). There was no reduction, but instead an increase in headache intensity 2 hours after sumatriptan (p = 0.003). Difference in area under the headache score curve (AUC) 0–4 hours between sumatriptan and placebo was not significant (p = 0.30).
Conclusion
5-ISMN is a very powerful inducer of migraine-like headache in healthy individuals but the headache does not respond to sumatriptan. The model is not useful for future drug testing.
Introduction
In previous human migraine models infusion of naturally occuring substances or their precursors were used and the headache was recorded together with a number of other biological variables (1–4). For a model to be useful in drug testing, it should preferably be effective in healthy volunteers who are easy to recruit and it should use tablet provocation. To be valid it must respond to triptans in a double-blind trial. Tablet formulation of the triptans is to be preferred, because companies primarily develop tablets, and because this allows outpatient administration. The present study is the second of a series aiming at developing and validating such a model. We have previously tested whether cilostazol-induced headache in healthy volunteers is a valid model, but the headache did not respond to sumatriptan and thus the cilostazol model did not fulfill our requirements.
Why a human migraine model
Experimental human models have several benefits compared to spontaneous migraine attacks. It is our experience that disability often prevents migraine patients from travelling to the hospital during an attack (5). That makes it difficult to study novel drug candidates. Experimental models allow the study of migraine and its treatment under conditions in which it is possible to register vital signs, take blood samples for pharmacokinetics and add imaging. Furthermore, a model makes it possible to test new drugs in a short period of time since participants do not need to await a spontaneous attack. Prophylactic drug trials in migraine require long-term toxicology information (three to five months) (6) while studying their effect on experimental attacks probably needs only two weeks of toxicology. Healthy volunteers are easy to recruit and therefore to be preferred.
Isosorbide-5-mononitrate (5-ISMN) is an organic nitrate which is metabolised to nitric oxide (NO) (7). NO induces migraine in migraine patients and headache in healthy individuals (8,9). The headache has similarities with migraine in most healthy volunteers (9,10). Thus, 5-ISMN seems to be a suitable provoking drug in healthy individuals. Our hypothesis was, therefore, that sumatriptan would have a significant effect against 5-ISMN-induced headache in a double-blind crossover experiment in healthy volunteers.
Material and methods
Design
This was a double-blind, randomised, balanced, placebo-controlled crossover study in which 5-ISMN 60 mg was given orally on two separate days five days or more apart, each day followed by oral self-administration of placebo or sumatriptan 50 mg.
The central pharmacy of the Capital Region of Copenhagen performed randomisation of the experimental drug in a balanced fashion. The randomisation code remained in the hospital during the study and was not available to the investigators. It remained unbroken until data management had been performed.
Participants
Thirty healthy volunteers (15 females/15 males) with no history of migraine were included. Inclusion criteria were: healthy individuals of both sexes aged 18–60 years and weighing 50–90 kg. Females were requested to use effective contraception.
Exclusion criteria were: any type of headache (except episodic tension-type headache <1 day per week), serious somatic or psychiatric disease, pregnancy, and intake of daily medication (except oral contraceptives). The participants were informed that 5-ISMN might induce headache or migraine in some individuals. One volunteer dropped out for personal reasons. She was replaced with a new participant.
Standard protocol approvals
All participants gave written, informed consent to participate in the study. The study was approved by the Ethics Committee of Copenhagen (H-6-2014-071), the Danish Data Protection Agency, and the Danish Medicines Agency and was conducted according to the Helsinki II declaration of 1964, as revised in 2008.
All participants were enrolled via the website: www.forsøgsperson.dk.
Study procedure
Full medical history, physical examination, electrocardiogram (ECG) and vital signs were collected on the day of recruitment. All participants had two study days at least five days apart. They arrived non-fasting at the clinic between 8:00 a.m. and 12:00 p.m. They had to be headache free 48 hours prior to the study and to not have taken any type of painkillers 12 hours before the study day. A pregnancy test was taken at the beginning of each study day on all female participants. All participants received 5-ISMN 60 mg orally on both study days and went home immediately after. When the participants reached headache intensity 3 on a 0–10 numerical rating scale (NRS) or six hours after 5-ISMN administration, placebo or sumatriptan was taken. In case of severe headache not responding to the experimental drug, the participants were offered rescue with paracetamol or nonsteroidal anti-inflammatory drugs (NSAIDs) but not before two hours after placebo or sumatriptan. During the study, an emergency phone was always open which patients could call if they experienced severe headaches or discomfort.
Headache parameters
Before starting the study, headache parameters and accompanying symptoms were recorded in the clinic. Afterwards, headache intensity was scored on a self-administered questionnaire every 30 minutes the first six hours after 5-ISMN and thereafter every hour until 12 hours after 5-ISMN. The intensity was scored on an NRS from 0 to 10, 1 representing a very mild headache (including feeling of pressing or pulsation), 5 a headache of medium severity and 10 the worst possible headache (11). Headache characteristics (unilateral/bilateral, quality and aggravation by physical activity) and accompanying symptoms (nausea/vomiting, phono- and photophobia) were also recorded in the questionnaire in order to compare with the International Classifications of Headache Disorders third edition beta (ICHD-3 beta) for migraine without aura (12). One participant went to sleep before 12 hours after 5-ISMN and missing data were filled in using last observation carried forward.
Statistical analysis
Headache intensity scores are presented as medians (range).
Calculation of sample size was based on the detection of a difference between two experimental days in changes of the head pain intensity (headache intensity before versus headache intensity after sumatriptan/placebo) at 5% significance with 90% power. We estimated that the effect on the placebo days was 20% and on the sumatriptan day 60%. Standard deviation was estimated based on previous data. The correlation within the two days was estimated conservatively at 0.5. We also assumed no carry-over effect. We estimated that at least 18 individuals should complete both experimental days. Due to uncertainty regarding these assumptions we decided to include 30 participants. The area under the curve (AUC) for headache score was used as a summary measure for analysing differences between the groups and was calculated according to the trapezium rule (13).
One primary end point was median headache score (regardless of type) at two hours after sumatriptan/placebo. We compared pre- and post-treatment headache scores within each day. Another primary end point was the difference in the area under the headache score curve (AUC) 0–4 hours after sumatriptan/placebo between the two experimental days. Secondary end points were nausea, photo- and photophobia, median peak headache score, median headache score four hours after sumatriptan/placebo and AUC for headache 0–2 hours after sumatriptan/placebo.
Headache intensity scores are presented as medians (range). Differences in AUC for headache intensity scores were tested using Wilcoxon signed rank test.
The incidence of headache and associated symptoms were analysed as binary categorical data with McNemar’s test. All analyses were performed with SPSS for Windows 11.5 (Chicago, IL, USA), or GraphPad Prism version 6.0. P < 0.05 was considered significant. Missing data were filled in using last observation carried forward. Age and weight are presented as means.
Results
Thirty healthy volunteers (15 females, 15 males), mean age 25 years (range 18–50 years) and mean weight 71 kg (range 55–85 kg) with no history of migraine completed both study days. 5-ISMN induced a reproducible headache (range 2–9 on NRS) in all participants.
5-ISMN-induced headache
Characteristics of the headache for each participant.

Characteristics: Location (+ = unilateral, − = bilateral)/quality (+ = throbbing, − = pressing)/aggravation.
Associated symptoms: nausea/photophobia/phonophobia.
Vomited.
Did not experience the symptoms at the same time.
Suma: sumatriptan; h: hours.
Clinical characteristics of headache and associated symptoms after 5-ISMN. There was no difference between the two treatment days. On both days 13 participants reported symptoms fulfilling criteria for a migraine-like attack.
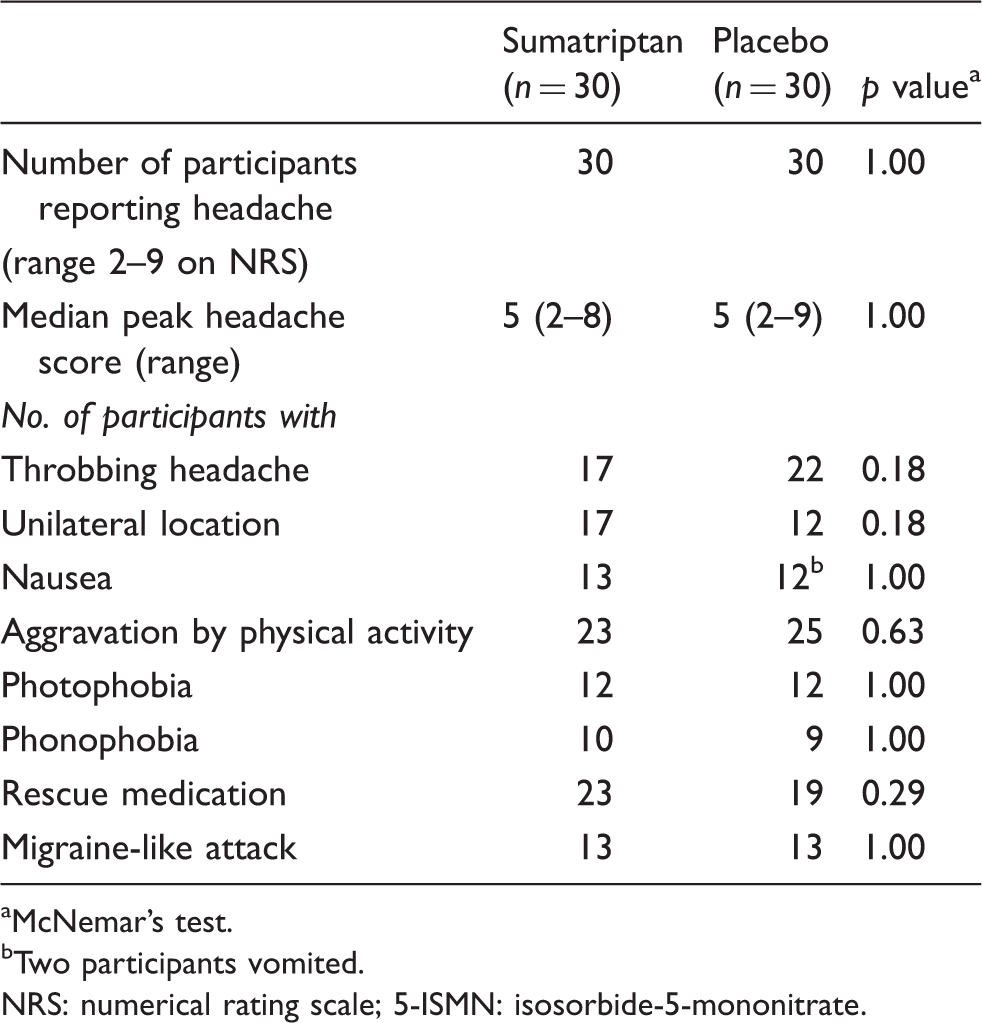
McNemar’s test.
Two participants vomited.
NRS: numerical rating scale; 5-ISMN: isosorbide-5-mononitrate.
Response to sumatriptan
The primary end point, median headache score two hours after treatment, is illustrated in Figure 1. There was no reduction in headache score. On the contrary, a significant increase in headache intensity was seen after both sumatriptan and placebo. Since there was an increase on both days, some of the increase must be due to the ongoing effect of 5-ISMN, but the more pronounced increase on the sumatriptan day can be a mechanism of sumatriptan. According to Burstein et al., sumatriptan can alter the physiological properties of meningeal nociceptors and cause a transient aggravation of the headache (14). Reduction in median headache score four hours after sumatriptan was not significantly different between sumatriptan and placebo (p = 0.615).
Box and whisker plot representing medians and quartiles of headache score 0 and 2 hours after treatment. (a) Sumatriptan day and (b) placebo day. There was no reduction, but instead an increase in headache intensity 2 hours after treatment (sumatriptan: p = 0.003, placebo: p = 0.018).
The other primary end point, difference in AUC 0–4 hours after treatment, was not statistically significant (p = 0.30). AUC 0–4 hours is illustrated in Figure 2. Our secondary end point, difference in AUC 0–2 hours after treatment, was not significant either (p = 0.13).
Box and whisker plot representing medians and quartiles of area under the headache score curve 0–4 hours after treatment. We found no difference between the two treatment groups (p = 0.30).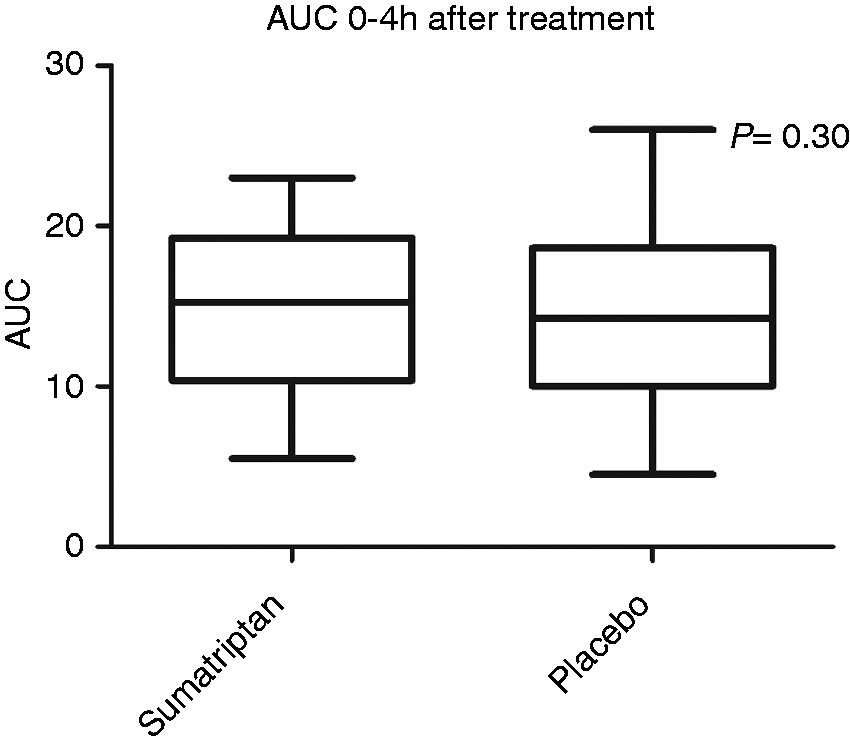
Median time for treatment was 3 hours (range 1–7 hours). Median headache score at treatment was 3 on both days. Median headache scores 0–12 hours after 5-ISMN for the two treatment groups are illustrated in Figure 3. There was no difference in treatment response on the two days (p = 0.62 for difference in AUC 0–8 hours after the two treatments).
Median headache score for the two treatment groups 0–12 hours after 5-ISMN intake. Median time for treatment was 3 hours (range 1–7 hours) illustrated with the thin dotted line. Median headache intensity at treatment was 3 on NRS on both days. There was no difference in treatment response between the two days (p = 0.62 for difference in AUC 0–8 hours after the two treatments). Note that the headache is reproducible on the two days. 5-ISMN: isosorbide-5-mononitrate; NRS: numerical rating scale; AUC: area under the curve.
Eight of the 30 participants had a first-degree relative with migraine (reported by the participants themselves). There were no differences in headache intensity or treatment response between disposed and non-disposed individuals. There were overall no differences in response between sexes either. One might think that the disposed individuals could represent a possible confounding factor in the study, but our other previous provocation study in healthy volunteers with cilostazol (15) showed no difference between disposed and non-disposed individuals.
In a secondary analysis, the 13 participants fulfilling criteria for migraine-like attacks on the sumatriptan day had a median headache score of 3 at the time of treatment. Two hours after sumatriptan the headache intensity had increased to 5 and thus the headache did not respond to sumatriptan in that subgroup either.
Discussion
Main findings
In line with previous studies (9,10), the present study found that 5-ISMN induces headache in healthy individuals. The most interesting finding is that the headache had several migraine-like features, and 20/30 participants fulfilled criteria for an experimentally induced migraine-like attack on one or both study days. This is the highest frequency of migraine-like attacks ever reported in healthy volunteers. Nevertheless, the headache did not respond to sumatriptan in a reasonably sized cohort. 5-ISMN-induced headache in healthy volunteers is a highly interesting model for the study of migraine mechanism but it is not a suitable model for the testing of new anti-migraine drugs.
Headache induced by 5-ISMN
5-ISMN induced a headache with one or more migraine-like features such as unilateral location, throbbing quality and aggravation by physical activity in all 30 participants. Thirteen of the 30 participants fulfilled criteria for an experimentally induced migraine-like attack on each study day and 20/30 fulfilled migraine criteria on at least one of the two experimental days. This demonstrates very clearly that continuously added NO is a very powerful migraine-inducing substance in healthy volunteers. For comparison cilostazol induced a migraine-like attack in 8 of 30 healthy volunteers (27%) in our previous study (15). It has been discussed whether healthy individuals can express a migraine attack given a sufficiently strong stimulus (16). The fact that 5-ISMN is able to induce migraine-like headache in 67% of healthy individuals supports the hypothesis that most people can reach the threshold and develop a migraine attack if exposed to a sufficiently strong stimulus.
An explanation for the absent response of sumatriptan might be that 5-ISMN works deeper than sumatriptan in the migraine cascade. If, for example sumatriptan works by inhibiting release of calcitonin gene-related peptide (CGRP), then it would have no effect on NO-induced increase of intracellular cyclic guanosine 3',5'-cyclic monophosphate (cGMP). We cannot rule out, however, that 5-ISMN-induced headache is different from a genuine migraine attack.
Pathophysiological implications
Previous studies have shown that neither zolmitriptan nor aspirin, nor olcegepant, have an effect on headache induced by long-lasting glyceryl trinitrate (GTN) infusion (17,18). The present results are in agreement as 5-ISMN releases NO continuously over many hours and we saw no effect of sumatriptan. Likewise our previous study with cilostazol in healthy volunteers (15), showed that sumatriptan was not effective when second messenger cyclic adenosine monophosphate (cAMP) was maintained at a high level. These studies indicate that migraine treatment, regardless of what kind, is not effective when second messenger levels are high.
On the other hand, pre-treatment with 6 mg subcutaneous sumatriptan reduced arterial dilatation and immediate GTN-induced headache (3,19). Thus, sumatriptan seems effective in immediate GTN-induced headache, possibly by vasoconstriction. Such effects are, however, not present with long-lasting increase of NO levels.
Implication for the mechanisms of action of sumatriptan
There are three favoured explanations for the mechanism of action of sumatriptan.
1: Cephalic vasoconstrictor, 2: Hyperpolarisation of sensory trigeminal nerve fibres, 3: Inhibition of impulse transduction across the first synapse in the trigeminal nucleus caudalis.
Regarding the first mechanism both cilostazol, as published previously, and 5-ISMN as used in the present study, are vasodilators. If that were the action of cilostazol and 5-ISMN induced headache in healthy volunteers, then it would be expected that sumatriptan which is a vasoconstrictor should be effective. It has previously proven unnecessary for effective migraine treatments to be vasoconstrictors, and now, it also seems that vasoconstriction is not of any major significance in cilostazol- and 5-ISMN-induced headache in healthy volunteers. Thus, vasoconstriction as a mechanism of action of sumatriptan is not supported by the present data. Regarding the second mechanism, all headaches are presumably generated by activation of peripheral trigeminal nerve fibres (and of the nerve fibres from the first three cervical segments). If the mechanism of action of sumatriptan were hyperpolarisation of trigeminal nerve fibres, then one would presume that sumatriptan should work also in experimental headaches such as induced by cilostazol and 5-ISMN. The fact that there was no effect in the present and our former study suggests that hyperpolarisation of sensory nerve fibres may not be a major mechanism of action of sumatriptan. The same could be said of the third mechanism. Inhibition of impulse transduction should be able to inhibit any kind of headache. The present study shows that this is not so and therefore our data do not support that inhibition of impulse transduction across the first synapse of the trigeminal nerve is a major mechanism of action of sumatriptan.
A last possibility, which in recent years has come slightly more in focus, is that sumatriptan may inhibit release of CGRP. It is presumed that this release is continuous to maintain the migraine attack. If the release is inhibited by sumatriptan, the migraine attack would resolve. Several animal studies have shown that triptans inhibit endogenous CGRP release (20–24). Whether sumatriptan in humans decreases plasma levels of CGRP is not unanimously accepted (25–28).
Future development
The present study is the second in a series aiming to develop and validate a pragmatic human model for the testing of novel migraine drugs. Since neither the previously tested cilostazol model (15) nor the present 5-ISMN model in healthy volunteers responded to sumatriptan, we next want to test a model in patients with migraine without aura. Another possibility is to use other migraine-provoking substances such as CGRP in healthy volunteers or migraine patients or to pre-treat with sumatriptan.
Clinical implications
Using a long-lasting nitro-preparation, 67% of healthy participants expressed a migraine-like attack. This suggests that most healthy individuals can express a migraine attack after a sufficiently strong stimulus. Unfortunately the induced migraine-like attack did not respond to sumatriptan. This and previous studies suggest that as long as NO is delivered to the body, triptans have no effect on the induced headache. The results also suggest that all three previously proposed mechanisms of action of sumatriptan may be of minor importance. New mechanisms such as inhibition of CGRP release should be studied.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: the European Union’s Seventh Framework program (2007–2013) under grant agreement no. 602633 (FP7-Euroheadpain).
