Abstract
Introduction
Treatment of neuropathic or neuralgic head and facial pain due to dental, traumatic or surgical nerve lesions or post-herpetic neuropathy is often challenging.
Cases
We are reporting on four patients with neuropathic pain syndromes successfully treated with a capsaicin 8% patch in the affected area of the head or face.
Discussion
Treatment with the capsaicin 8% patch seems to be effective and safe for application to the facial and head region. The capsaicin 8% patch might be an additional treatment option if first-line treatment with anticonvulsants or antidepressants was ineffective or limited by side effects.
Introduction
Neuropathic pain (NP) is defined as pain arising as a direct consequence of a lesion or disease affecting the somatosensory system either in the periphery or centrally (1). NP can be caused by a variety of diseases and conditions, such as diabetes mellitus, multiple sclerosis, stroke, radiculopathy, post-herpetic neuralgia, cranial neuralgia, human immunodeficiency virus (HIV)-associated neuropathy, nerve compression by tumors or damage resulting from trauma or surgical procedures (2,3). Epidemiologic data suggest that NP affects up to 8% of the general population in Europe (4,5). Despite the availability of several pharmacological treatment options, the management of NP remains challenging. The current pharmacologic therapies for the treatment of NP include anticonvulsants, antidepressants (e.g. tricyclic antidepressants), opioids, and topical agents like lidocaine. The use of systemic treatment options is often limited by poor tolerability and, in addition, the overall response is often unsatisfactory (6–8). These limitations have led to an interest in the use of non-systemic approaches to manage peripheral NP.
Recently a dermal application system containing 179 mg (8%) capsaicin (research code NGX-4010; Qutenza™) was approved for the treatment of peripheral NP (9). Capsaicin, the primary pungent ingredient in hot chili peppers, is a highly selective agonist for the transient receptor potential vanilloid 1 (TRPV1) receptor, which is a temperature- and ligand-gated, non-selective cation channel (10,11) and has been identified as a key receptor involved in the transmission and modulation of pain signals (11,12). Although capsaicin induces TRPV1-mediated initial hypersensitization, it is followed by defunctionalization or desensitization on continuous stimulation (13). Topical application of low-concentration capsaicin for the treatment of NP has already been used for decades. Studies have shown some evidence of pain relief, but the efficacy was rather moderate and compliance with this therapy has been poor because of the need for repetitive application every day and initial burning sensations (14,15).
In the clinical setting, a single 30- to 60-minute application of the high-concentration capsaicin patch has resulted in marked and prolonged analgesia in randomized, controlled clinical trials in patients with NP (including post-herpetic neuralgia, HIV-associated neuropathy, diabetic neuropathy and others causes of NP). Single and repeated applications of the capsaicin patch were shown to be safe and well tolerated (16–22). However, special warnings and precautions for use exist for the application of the capsaicin patch on the head or facial areas; a single patient suffering from trigeminal post-herpetic neuralgia was published (23). We report on four patients suffering from NP in the face and the head area refractory to previous standard therapy who were treated with the capsaicin 8% patch, which is not in accordance with the current Summary of Product Characteristics (SmPC) (9).
Treatment with the capsaicin patch
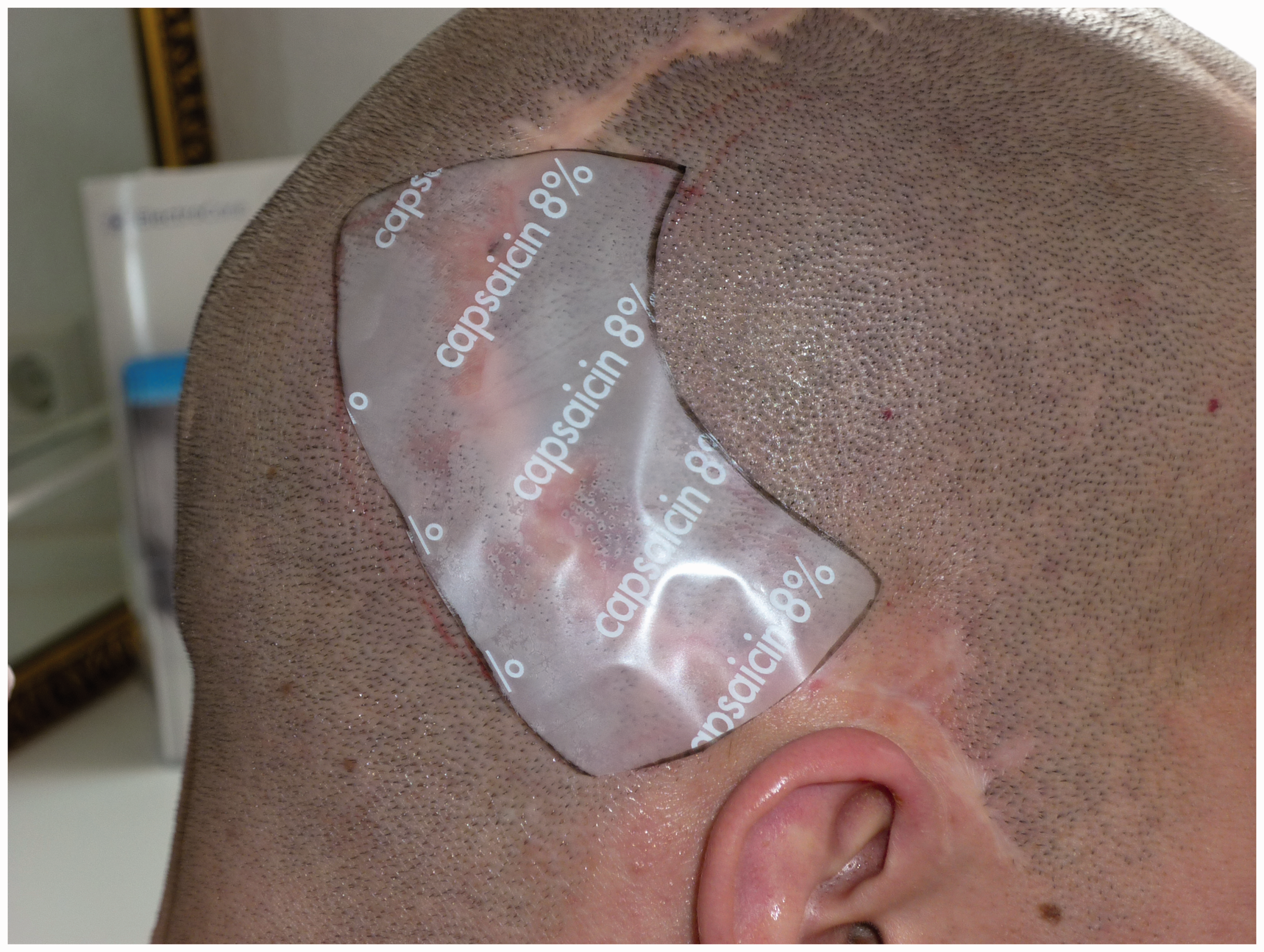
To prepare the application of high-concentration capsaicin, the area to be treated was identified in all patients using pinpricks and a brush and was marked on the patient’s skin. The markings were used to match the size of the capsaicin 8% patch to the treatment area. As recommended (9), the patient was pretreated with lidocaine cream 4% for 60 minutes before application of the capsaicin 8% patch. Following removal of the topical anesthetic, the capsaicin 8% patch was applied for 60 minutes and fixed with compress and plaster (Figures 1–4). After patch removal, the area was carefully cleaned with cleansing gel to remove any residual capsaicin.
Craniotomy scar in patient 2, distal part exhibiting neuropathic pain. Pretreatment with lidocaine cream 4% for 60 minutes in patient 2. Application of the capsaicin 8% patch in patient 2. Patch fixed with compress and plaster in patient 2 for 60 minutes.


Case reports
Patient 1
In 2007, a 51-year-old otherwise healthy man developed NP due to surgical injury of the great auricular nerve following removal of a benign tumor of the parotid gland. The pain was clearly described as NP with burning, pungent, and electric shock-like sensations. Pain was located in the skin of the scar area, parts of the ear, region dorsal of the ear and the cheek. In addition to spontaneous pain attacks, pain could be evoked by wind or light touch to the above-mentioned areas. An average pain intensity of 8 was estimated on a numeric rating scale (NRS; range 0–10).
Over a five-year period, the patient was treated with various drugs (e.g. pregabalin, gabapentin, carbamazepine, oxcarbazepine, amitriptyline, duloxetine and various opioids) in monotherapy or in combination. Twice he was hospitalized for multimodal pain therapy with a series of local anesthetic interventions and topical lidocaine application. None of these therapies resulted in sustained pain reduction or led to intolerable adverse effects. The distance from the patch to the eye was 3 cm, therefore no special protection of the eye was carried out when treatment with capsaicin was performed. Following treatment, the skin was reddened but no relevant pain amplification requiring analgesic therapy occurred during or after application and no further acute or long-term adverse effects were observed in this patient. The reduction of allodynia and the decrease of the permanent pain were evident within 12 hours after application of the capsaicin 8% patch from NRS 8 to NRS 2. The decrease of pain lasted eight to 12 weeks after application and the patient was re-treated four times with the same effect.
Patient 2
In 2005, a 21-year-old man suffered from right-sided intracerebral hemorrhage in the basal nuclei with additional subarachnoidal bleeding due to an intracerebral angioma. Decompressive ipsilateral craniotomy was required for treatment. Following the intracerebral hemorrhage, the patient suffered from left-sided spastic hemiparesis, symptomatic epilepsy, and permanent right-sided dull headache as well as a burning and pungent NP in the area of the parieto-temporal craniotomy scar. He rated mean pain intensity NRS 6; pain increased spontaneously or on touching to NRS 8. According to the International Classification of Headache Disorders, third edition beta (ICHD-3 beta), the underlying headache has to be classified as 5.6 Persistent headache attributed to craniotomy (24). However, the NP component resulted from the more superficial nerve injury due to the craniotomy and was not a headache. Various systemic treatments including anticonvulsants (carbamazepine, gabapentin, pregabalin, lamotrigine) and antidepressants (amitriptyline, doxepine, imipramine) and topical application of a lidocaine plaster did not result in significant relief of the NP. The patient was treated with high-dose pregabalin (900 mg/d) because of the seizures, which led to pronounced fatigue. The application of high-concentration capsaicin was undertaken as described (Figures 1–4). No additional analgesic therapy was needed during or after application and apart from transient reddening of the skin no further acute or long-term adverse effects were observed in this patient. There was a marked reduction in NP (allodynia and spontaneous and provoked pain attacks) in the area of the craniotomy scar. As expected, no relevant influence could be achieved on the permanent right-sided dull headache. The decreases of allodynia and pain attacks were sustained and no repetition of the treatment was needed over a follow-up period of eight month until now.
Patient 3
In 2009, a 75-year-old woman suffered from acute herpes zoster infection and developed a left-sided post-herpetic neuralgia in the first branch of trigeminal nerve with itching and electric shock-like pain. Pain attacks occurred spontaneously or by light touch on the forehead; pain intensity was rated NRS 8–10. The patient’s major complaint was the itching that triggered electric shock-like pain. According to the ICHD-3 beta the diagnosis has to be classified as 13.1.2.2 Post-herpetic trigeminal neuropathy (24). Treatment with amitriptyline was not effective; anticonvulsants (gabapentin and pregabalin) could reduce pain but led to intolerable adverse effects and the patient refused further systemic medication. The application of high-concentration capsaicin was carried out as described above. Because of the closeness to the left eye, we covered the eye with a compress and plaster before and during application of capsaicin. Apart from mild burning of the skin during and a few hours after treatment, needing no additional analgesic therapy, and temporarily reddened skin no further acute or long-term adverse effects were observed in this patient. In particular, no problems with or damage to the eye occurred. Pain decreased only slightly on the following day, but a marked reduction of the very disturbing itching sensations could be achieved that led to a reduction of the frequency of electric shock-like pain.
Patient 4
In 2007, a 51-year-old man suffered from dysesthesia and NP of the ipsilateral chin following left-sided extraction of a wisdom tooth complicated by local osteomyelitis of the mandible. He complained of continuous burning pain superimposed by electric shock-like pain triggered by speech and chewing. Clinical examination revealed allodynia in the distribution of the left-sided mental nerve. According to the ICHD-3 beta, the diagnosis has to be classified as 13.1.2.3 Painful post-traumatic trigeminal neuropathy (24). Treatment with carbamazepine resulted in only temporary pain reduction; treatment with amitriptyline as well with pregabalin had to be stopped because of side effects. Neither lamotrigine nor topical lidocaine resulted in significant pain relief. Following a topical treatment with the capsaicin 8% patch as described above, pain intensity was reduced more than 50% (Figures 5 and 6). No additional pharmacological therapy was needed. Treatment was repeated every three months with the same success for more than three years.
Area of continuous burning pain superimposed by electric shock-like pain triggered by speech and chewing. Area of allodynia in the distribution of the left-sided mental nerve revealed by clinical examination. Pretreatment with lidocaine cream 4% for 60 minutes in patient 4.

Discussion
We have reported here on four patients suffering from circumscribed, clearly NP on the head or the face caused by different mechanisms. Since these patients were shown to be refractory to recommended first- and second-line systemic or topical medication for the treatment of neuropathic pain (8) or suffered from intolerable adverse effects of systemic medication, treatment with capsaicin 8% was offered, not in accordance with SmPC. Although recent studies have shown that there is no need for pretreatment with topical anesthetics (25), all patients were pretreated with lidocaine cream 4% for 60 minutes before the capsaicin patch was applied as recommended previously (9). If the capsaicin 8% patch was to be applied close to mucous membranes, specifically close to the eye, special protection of these areas was carried out (covering the eye with compress and plaster before application). In patients 1 and 2, marked pain relief occurred rapidly after treatment with the capsaicin 8% patch, becoming evident within 24 hours post-application. The fast onset of analgesic effect in these patients was consistent with published data of capsaicin treatment of NP in areas excluding the head or the face (18,26). Patient 1 was re-treated four times at intervals from 12 to 16 weeks with consistent effect. Patient 2 showed sustained reduction of the NP after a single treatment and no repetition of capsaicin treatment was necessary. However, the long-lasting effect might also be attributed to the additional therapy with lamotrigine. Pain relief in patient 3 was only mild but a marked reduction of the itching sensations was achieved. Patient 4 showed sustained treatment response for more than three years with repetitive treatment. All reported patients showed transient, mild application-site erythema and burning pain during and a few hours after capsaicin application. However, none of them needed rescue medication and all patients completed the duration of patch application. No further adverse effects were reported and in particular no damage to eyes or mucous membranes occurred.
Although there are various recommended systemic treatments, NP is challenging to manage because patients are often refractory to – or unable to tolerate – recommended existing systemic treatments (6). The high-concentration capsaicin patch is a further treatment option for NP. However, special warnings and precautions for the use in the treatment of head or facial areas exist. Notably, in our view, the capsaicin patch is a treatment option not only for patients suffering from post-herpetic neuropathies. It can likewise be used in traumatic (or surgical) nerve lesions following craniotomy or tooth extraction (if the pain occurs extraorally). This is especially valuable since treatment of those pain syndromes is often difficult. Our case reports indicate that capsaicin patch treatment in these areas is effective, safe and well tolerated, and randomized, controlled trials on efficacy, safety and tolerability should be conducted.
Clinical implications
Treatment with the capsaicin 8% patch seems to be effective and safe for application to the facial and head region. The capsaicin 8% patch might be an additional treatment option for neuropathic facial and/or head pain if first-line treatment with anticonvulsants or antidepressants was ineffective or limited by side effects.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest
C.G. has received honoraria for participation in clinical trials, contribution to advisory boards or oral presentations from MSD, Bayer AG, Berlin Chemie AG, St Jude Medical, ATI, ElectroCore, Complen Health GmbH, Allergan, Boehringer Ingelheim, Astellas, and Hormosan. He has no ownership interest and does not own stocks in any pharmaceutical company.
S.R. has nothing to declare.
