Abstract
Background:
This novel case report describes the problems of prescribing a prosthetic socket in a left transfemoral amputee secondary to chronic patellofemoral instability compounded by complex regional pain syndrome.
Case Description and Methods:
Following the amputation, complex regional pain syndrome symptoms recurred in the residual limb, presenting mainly with oedema. Due to extreme daily volume fluctuations of the residual limb, a conventional, laminated thermoplastic socket fitting was not feasible.
Findings and Outcomes:
An adjustable, modular socket design was trialled. The residual limb volume fluctuations were accommodated within the socket. Amputee rehabilitation could be continued, and the rehabilitation goals were achieved. The patient was able to wear the prosthesis for 8 h daily and to walk unaided indoors and outdoors.
Conclusion:
An adjustable, modular socket design accommodated the daily residual limb volume fluctuations and provided a successful outcome in this case. It demonstrates the complexities of socket fitting and design with volume fluctuations.
Clinical relevance
Ongoing complex regional pain syndrome symptoms within the residual limb can lead to fitting difficulties in a conventional, laminated thermoplastic socket due to volume fluctuations. An adjustable, modular socket design can accommodate this and provide a successful outcome.
Keywords
Background
This case report describes the challenges of amputee rehabilitation following a left transfemoral amputation due to chronic patellofemoral instability compounded by complex regional pain syndrome (CRPS). Following the amputation, CRPS symptoms recurred in the residual limb, presenting mainly with oedema. This caused extreme daily residual limb volume fluctuations that could occur within hours leading to severe socket fit problems. A conventional, laminated thermoplastic socket could not accommodate these daily changes. The aim of this case report was to describe the alternative socket design and the outcome. No previous case reports detailing this management approach were found by the authors.
CRPS is a clinical presentation of pain, autonomic dysfunction, functional impairment and trophic changes. 1 It is characterised by a continuous regional pain that does not follow a nerve territory or dermatome. The pain is disproportionate to the inciting injury. 1 CRPS is categorised into two main subtypes. CRPS type 1 is the most common and it is without a peripheral nerve injury involvement and CRPS type 2 is with a peripheral nerve injury. 2 The aetiology is unknown, but multifactorial in origin including both psychological and biological. 3 It is thought to be caused by a peripheral or central nervous system mechanism. 4
CRPS is estimated to have an incidence rate of 26.2 per 100,000 person-years. 5 It shows a female predominance. 5 The most common inciting injuries include fractures, crush injuries, sprains and surgery. 5 The diagnosis is made based on the clinical features and physical examination. The abnormal sensory, motor, sudomotor, vasomotor and trophic changes show a distal predominance. Signs include hyperaesthesia, allodynia, reduced range of movement, muscle weakness, dystonia, oedema, sweating changes, temperature and skin colour changes and trophic changes in the hair, skin and nails. 1 Long-standing CRPS can lead to the development of a severely dysfunctional limb, rarely an amputation can be considered as a treatment options when all others have failed. 6
Case description and methods
This case report describes the medical history of a 38-year-old woman who had suffered from a chronic left patellofemoral instability compounded by CRPS type 2 for over 24 years. The patient sought out a medical practitioner who would consider the treatment option of an amputation due to severity of the functional impairments experienced by the dysfunctional limb. She was referred for an outpatient assessment and was reviewed by a rehabilitation physician, plastic surgeon and counsellor.
At the age of 14, she was diagnosed with left patellofemoral instability. Over the next decade, she had up to 30 procedural and operative interventions to correct or improve the instability. Unfortunately, this was with limited success, and the patient started to develop symptoms consistent with CRPS. At the age of 24, she had a severely dysfunctional left leg with chronic CRPS changes. She requested the referral following exhausting all treatment options for both patellofemoral instability and CRPS. The last option offered was knee arthrodesis. At 1.88 m tall, it was deemed unsuitable, as the extended leg length would likely impose greater dysfunction on her day-to-day life.
On examination, she was found to have a profound weakness and wasting of the left leg, though hip muscle power was preserved. Throughout all her movements, the left knee remained in an extended position. A sensory deficit was present from the foot up to the level of the knee. She wore a modular knee ankle foot orthosis. She had walked with crutches for over 20 years and used a wheelchair for all outdoor activities. Walking was becoming increasingly difficult, and the left leg caused major limitations in her to day-to-day life. She lived in a ground floor adapted flat with wheelchair access.
She had suffered recurrent episodes of cellulitis and had required antibiotics multiple times a year for over 10 years. She had extensively researched the option of an amputation and felt that this would free her from a chronically infected non-functional limb, which she described as having to simply drag around.
Following extensive consultation with the multidisciplinary team (MDT) and a 6-month period of pre-amputation rehabilitation, she was both psychologically and physically prepared for the procedure. She had an uncomplicated elective left transfemoral amputation with a myoplasty closure. This was performed by the plastic surgeon with extensive experience in performing complicated amputations.
Post-operatively, the patient made a quick recovery and was discharged home within 3 days. The residual limb healed well, with optimal length to allow for competent clearance. There was return of oedema within the residual limb, as the post-operative swelling subsided. She had been made aware of the possibility of CRPS returning but continued to benefit from the freedom that the amputation had given her. She commenced an outpatient rehabilitation programme to evaluate the prosthetic walking possibilities.
Findings and outcomes
She made excellent progress within post-amputation rehabilitation, with a positive and motivated approach. Within a 6-week period, she had progressed to mobilising with a Femurett early walking aid with a stick. She then began her primary prosthetic rehabilitation. At week 9, she moved onto a conventional, laminated thermoplastic socket that fitted well with a seal in liner suspension, ischial weight bearing and a free knee mechanism. At 14 weeks post-operatively, the oedema started to cause significant residual limb volume fluctuations. The residual limb circumference (measured at 15 cm from the distal end of the residual limb) varied by 6 cm (between 38 and 44 cm) – this could occur within hours. This caused significant disruption to rehabilitation. During physiotherapy sessions, the residual limb volume at its smallest would piston within the socket and at its largest the circumference would be too large to allow her to donn the socket. The socket would often have to be removed throughout the session due to stump end strangulation.
Numerous strategies were used to allow for the residual limb volume fluctuations within the conventional socket. Over 10 weeks, multiple adjustments to the sockets were fabricated, layering and removing cotton socks, extra gel liners and multiple silicone socks were tried. All these strategies helped her to alter the circumference of her residual limb and to maintain continuous wear for only up to an hour. At the extremes of volume change, the socket could not be worn. At week 23, the MDT established that rehabilitation within a conventional socket was no longer feasible, as the static and finite structure could not accommodate for the changing residual limb size. An alternative socket design was required. At 35 weeks, an adjustable, modular socket design was custom made by LIM Innovations and trialled. Figure 1 compares the new and old socket design.

Photographic comparison of the old and new socket design. Left: conventional, laminated thermoplastic socket; right: adjustable, modular socket design.
The new adjustable, modular socket design was attached to her original knee, foot and ankle. The new socket was fabricated from residual limb measurements and a traditional plaster of Paris impression. The modular socket design can be deconstructed into the following components: heat mouldable textile brim, four carbon struts, flexible plastic inner cup, lanyard suspension unit and the anodised alignment base plate. The heat mouldable textile brim consists of overlapping medial and lateral panels that can tighten and loosen with dynamic volume fluctuations. She can adjust this tension using the adjustable ratchet mechanism (Figure 2). The brim was heated and contoured to her proximal thigh.

Photograph of the new adjustable, modular socket design with a close up of the adjustable ratchet tensioner.
The four carbon fibre struts (Figure 2) are mounted to the base plate in a manner that allows for radial slide and angular pivot adjustments of each individual strut. The sliding adjustments further accommodated her volume changes, while the pivoting adjustment redistributed localised pressures.
The flexible plastic inner cup contained and encapsulated the soft tissue, with flexibility, rather than within a rigid and static conventional socket (Figure 1). As the volume of the residual limb fluctuated, the flexible inner cup accommodated for the volume change through the modular frame design. The cup was heated to contract or expand with changing volume fluctuation.
The mechanism of suspension that can be implemented includes seal in suction, lanyard or pin lock. She utilised the lanyard suspension combined with a plastic inner cup for tissue containment (Figure 3).
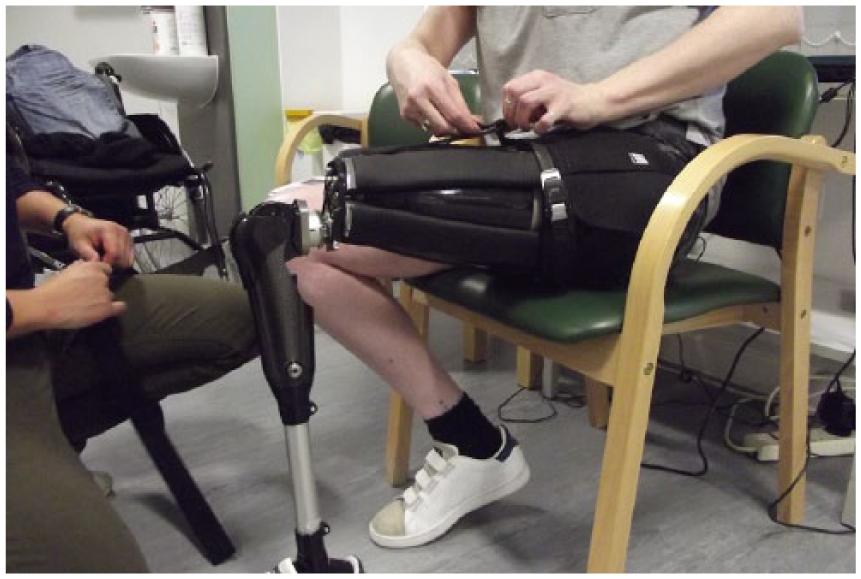
Photograph of application of the lanyard suspension combined with a plastic inner cup.
Day 1 after fit and adjustments to the socket, she was able to wear it for 6 h continuously. The socket could be worn for a 60-min physiotherapy session without any problems of fit, distal end strangulation or skin irritation. She restarted an intensive rehabilitation programme focusing on gait re-education, hip and trunk muscle strengthening. Her Special Interest Group in Amputee Medicine (SIGAM) mobility score 7 had risen from grade C to E with the new dynamic socket fit. The socket comfort score (SCS) 8 had risen from 4 to 8. She has been able to surpass many of her rehabilitation goals. She is able to drive her adapted car with the prosthesis on, attend medical appointments without a wheelchair and complete a food shop walking, without using a wheelchair. The patient is able to wear the prosthesis for 8 h daily and to walk unaided indoors and outdoors. The new socket design allowed her to complete a lifelong dream of riding a racing bike in a velodrome.
Discussion
The normal fitting process after a transfemoral amputation was unsuccessful in this case due to severe residual limb volume fluctuations. This was caused by the CRPS symptom of oedema returning. The first socket design was a conventional, laminated thermoplastic socket that could not accommodate for these daily changes. The adjustable, modular socket design had multiple inbuilt strategies that allowed the residual limb to shrink and grow within the socket while being worn. There is a paucity of literature on the outcomes of prosthetic rehabilitation following an amputation for CRPS. The authors could not find any information of prosthetic fitting outcomes or designs for a residual limb with volume fluctuations with symptoms of CRPS.
CRPS is to be managed with an integrated MDT approach and a focus to reduce pain, preserve or restore function, enable self-management and improve quality of life. 9 The evidence supporting surgical management including amputation is limited. 9 Amputation for long-standing treatment-resistant CRPS is controversial, and due to limited research, it is not possible to make an evidence-based decision. 6 It is mainly considered in the cases of chronic infection. 9 The primary reasons cited for an amputation in CRPS are pain (80%) and a dysfunctional limb (72%). 6 It is known that an amputation may worsen the CRPS, with it recurring in the residual limb. 10 CRPS type 1 recurred in around 48% of amputees. 6 As in this case, it is strongly recommended that when an amputation is to be performed, it is by a surgeon experienced in such cases and an anaesthetist who is also a pain specialist. 9 Looking into the functional outcomes, 38% of amputees will have a prosthesis fitted and only 15% will use the prosthesis to mobilise. 6 The reasons for such low use are unclear. However, amputees report improvements to quality of life. 6 The quality of life appears to increase after amputation, whether the prosthesis is worn or not. 11 The recurrence of CRPS in the residual limb has been identified as a factor that can limit prosthetic use, but most patients seem to be satisfied with the result of the amputation. 11
In this case report, an amputation for chronic patellofemoral instability with an ankylosed knee and CRPS type 2 was a successful treatment option. The overall general health of our patient improved with no further episodes of cellulitis and the malaise associated. The patient describes that her overall quality of life has improved significantly post-amputation.
Conclusion
The authors describe the first case report of a successful outcome of a transfemoral amputation with return of CRPS symptoms of oedema and daily residual limb volume fluctuation with the use of an adjustable, modular socket design. It is known that prosthetic use is limited post-amputation due to recurrence of CRPS. When oedema is present in a residual limb, an alternative socket design should be considered that can accommodate for the volume fluctuation. An adjustable, modular socket design may be able to increase the time the prosthesis can be worn in amputees with CRPS symptoms in the residual limb.
Footnotes
Acknowledgements
The authors thank the patient for her kind permission to use her material. The patient provided written consent for the imagery and information to be used. The authors thank the LIM Innovations company for their advice on the technical descriptions of the socket designs and imagery.
Author contribution
All authors contributed equally in the preparation of this manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
