Abstract
Aim:
Finger and partial finger amputations are commonly due to traumatic injuries; digit loss may also be attributed to congenital malformations and disease. Finger prostheses are difficult to fabricate as they demand both aesthetic and function. When dealing with these types of prostheses, the only method of gaining successful retention is to sleeve the remnant stump with thin silicone.
Case description and methods:
A 28-year-old man reported with a chief complaint of unaesthetic look due to amputated ring finger of left hand. In this case, the remnant stump was missing, the adjacent ring finger was splinted and an adhesive retained prosthesis instead of ring retained or glove-on prosthesis was planned. The retention was achieved by extending the prosthesis to palmar crease.
Findings and outcome:
This article describes the rehabilitation of a finger with prosthesis, which is simple to construct, aesthetic, retentive and easy to maintain. The prosthesis thus fabricated merged with the adjacent tissues providing desired aesthetics and psychological boost to the patient.
Conclusion:
Final prosthesis was found with adequate retention. The patient was satisfied with the aesthetic of the prosthesis.
Clinical relevance
Because of the missing residual stump, functional limitations were also there. This clinical report describes a technological process of designing and manufacturing a silicone rubber prosthesis for a patient who has a finger loss caused due to trauma.
Background
A finger is a type of digit, an organ of manipulation and sensation found in the hands of humans and other primates. Normally, humans have five digits, termed phalanges, on each hand. They enable us to interact with our environment and help in many day-to-day functions. It has been stated that the thumb is the most important digit from a functional standpoint. 1
‘Amputation’, derived from the Latin word ‘amput-are’ (to excise, to cut out), has been defined as the ‘removal of part or all of a body part enclosed by skin’ (Online Medical Dictionary). Until the 18th century, with the exception of Pare, few physicians gave thought to the condition of the amputation stump for prosthetic appliance during the period from 1846 to 1847. The introduction of antiseptics by Lister allowed surgeons to take more time to produce viable amputation stump capable of supporting prosthetics. 2
Finger and partial finger amputations are some of the most frequently encountered forms of partial hand losses resulting in significant functional deficiencies, in addition to immediate loss of grasp, strength and security. 3 The most suitable approach depends on the amount of tissue involved, the involvement of bone (distal phalanx), the angles and levels of amputation and the involvement of other fingers. Various methods such as titanium implants, osseointegration abutment and silicone elastomers are in use for replacing missing finger. Passing through various materials, the acceptance rate has been much higher when an individually sculpted custom restoration using silicone elastomer. 4
The success of the prosthesis depends on the precision in meticulous planning and designing of prosthesis, technique and materials used. 5 Hence, accurate impression technique, carving of wax patterns that would provide desired aesthetics, retention and stability, is of paramount importance. Most of the conventional custom finger prosthesis made up of autopolymerizing resin or polyvinyl chloride have not been able to provide the desired results due to poor aesthetics, lack of flexibility and the tendency to stain. The prosthetic rehabilitation should be as barely discernible as possible with an attempt to create the prosthesis life-like and natural. Fabrication of such prostheses with realistic skin surface and seamless visual integration with surrounding tissues requires high degree of clinical skill and laboratory expertise.
This case report describes the rehabilitation of a man whose ring finger was amputated following a road traffic accident (RTA). Although he was a candidate for autologous implant, he declined this option for various reasons.
Case description and methods
A 28-year-old man reported with a chief complaint of unaesthetic look due to amputated ring finger of left hand. History revealed that the reason for loss was traumatic accident 1 year back. A complete hand examination was carried out that revealed lost ring finger of the left hand without any residual stump. The area around the missing finger was found to be clear of any signs of inflammation and infection.
The case was discussed and a method to replace the finger was formulated. The treatment plan was then discussed with the patient. As a part of protocol, and to ensure the patient’s willingness and co-operation, an informed consent was signed before beginning the treatment. Ethical approval was not obtained as it was not required by our institution. Since the patient’s ring finger was splinted and there was no residual stump, an adhesive retained prosthesis instead of ring retained or glove-on prosthesis was planned.
Fabrication methods
The fabrication of the prosthesis consists of the impression making, the wax pattern, followed by laboratory procedures to fabricate it into silicone rubber prosthesis.
Impression making
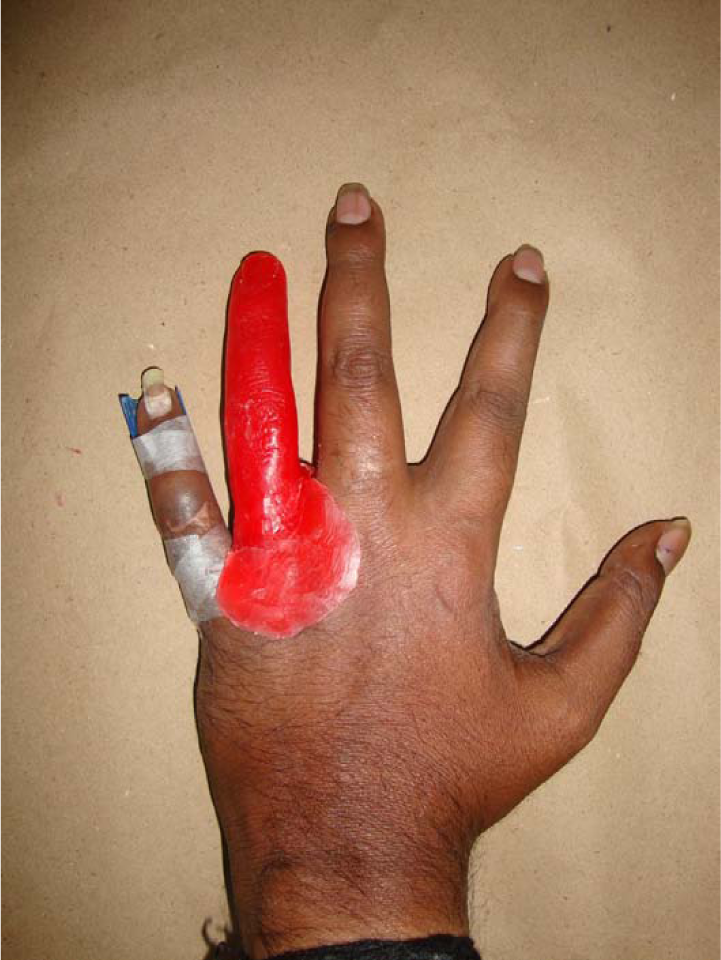
To maintain a natural appearance, it was decided to record the impression and fabricate the prosthesis with each joint slightly flexed when the patient was in a relaxed position (Figure 1).
The patient’s left hand was lubricated with a thin layer of petrolatum jelly to prevent the hydrocolloid impression material from adhering to the skin and hair of surgical site and the tissue surface. Irreversible hydrocolloid (Tropicalgin; Zhermack, Inc., CA, USA) was placed over the palmar side first and then the dorsal side. This two-part mould prevents the impression from tearing when the hand is removed after the material sets. A layer of gauge was placed on setting alginate and the impression is reinforced with fast setting plaster that is around 0.25 in thickness to provide adequate support to alginate impression and to avoid tearing and distortion on removal. The patient was instructed to keep the hand in resting position and not to stretch.
After the material set, the patient was asked to carry out light movement and remove the palm from the impression.

Impression.
Preparation of the model
The impression was poured with the dental stone (Kalstone; Kalabhai Pvt. Ltd, Mumbai, India) using vibrator to avoid voids, and a positive replica of hand was retrieved.
Fabrication of wax pattern
For wax pattern fabrication, impression of another person’s finger resembling to patient’s lost finger’s dimensions and contours closely was made to reduce time required for sculpting. A putty impression was made. Wax (Dental Product India, Mumbai, India) was then poured into the putty index and retrieved. The wax pattern was then adapted on the cast, and modifications in sculpting were carried out to resemble the digits of the contralateral hand accurately. The margins of finger prosthesis were thinned in order for the silicone to blend with natural tissues (Figure 2).

Wax pattern.
Trial of wax pattern on patient’s hand
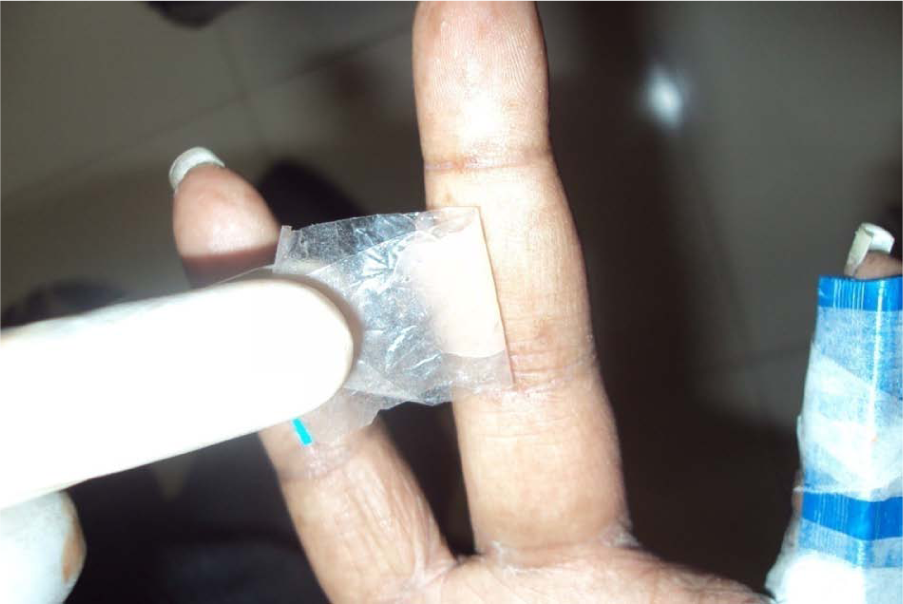
Proper fit of wax pattern was checked on both dorsal and palmar sides, and aesthetics, retention and stability were evaluated. Necessary modifications were carried out. Following successful try-in, nail bed was reduced to allow for acrylic nail (Figure 3).
Wax pattern trial.
Investment technique
Wax pattern was then invested in a custom-made box. The first pour was done until the junction of dorsal and ventral surface. Separating medium was then applied and a second pour was done to cover the entire wax pattern. Dewaxing was carried out in the conventional manner and the flask was allowed to cool. 6 A three-piece mould was thus obtained. The advantage of this technique is that it eliminates the unsightly voids in the prosthesis commonly seen while using silicone, as it is more viscous and does not flow easily into inaccessible areas. The prosthesis was packed with heat vulcanizing (high-temperature vulcanization (HTV)) silicone (Cosmosil M 511 series material) and coloured using intrinsic stains selected according to patient’s skin colour (Figures 4 and 5). Separate matching of shade was done for nail. Shade matching should be performed at the time of packing to ensure optimal aesthetics. The dorsal and palmar aspects were mixed and packed separately and characterization was incorporated (Figures 6 and 7). The patient’s presence was critical to gain his or her approval. The silicone was heated for 2 h at 90°C in air circulating oven (Oaao Rock health care), to reduce the curing time. After final curing, it was deflasked, trimmed and cleaned (Figure 8). Excessive polishing should be avoided to ensure matt finish, which is more natural and life-like.

Silicone material.
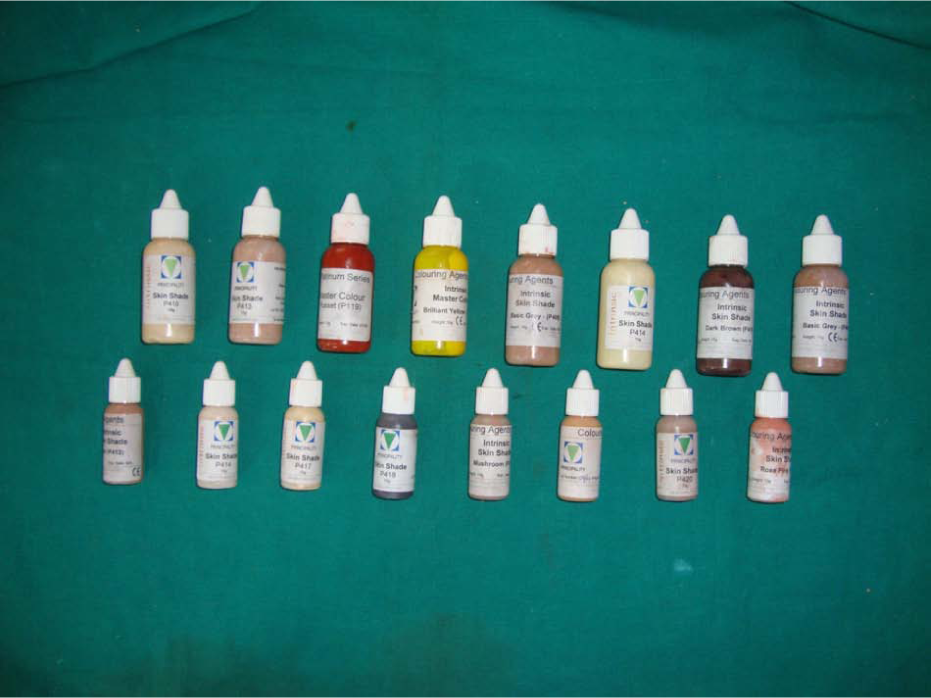
Intrinsic stains.
Shade matching.

Packing of silicone in the mould.
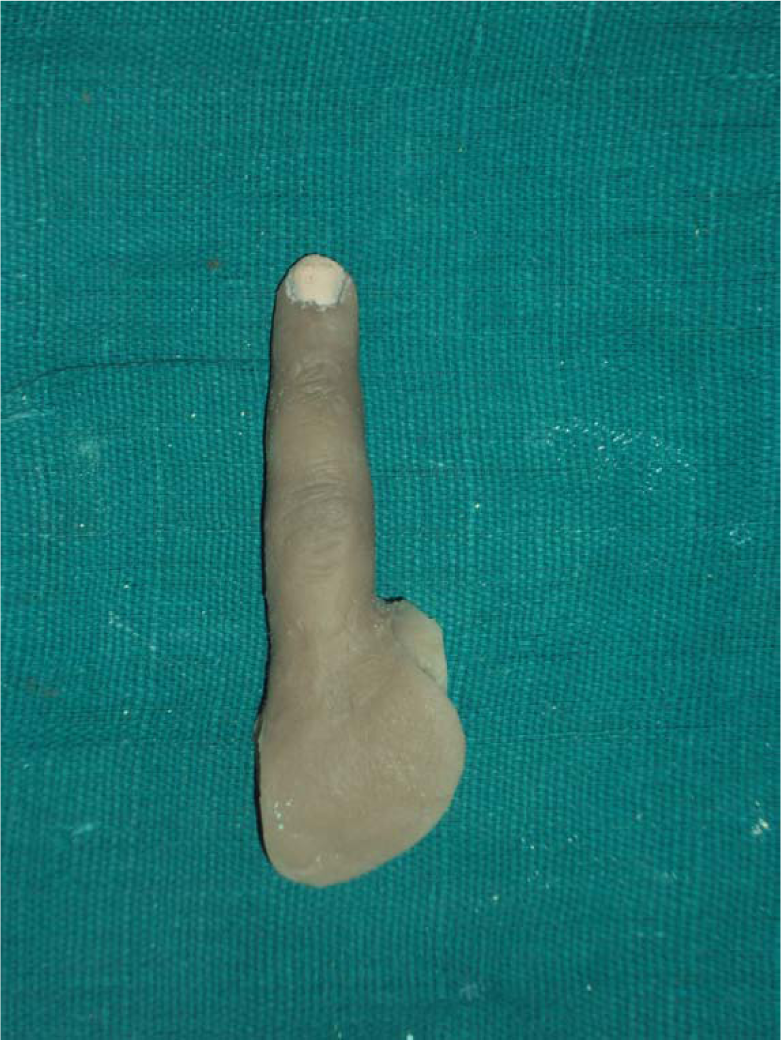
Prosthesis after deflasking and cleaning.
Final colour matching was done with extrinsic pigmentation (KT-699, Silicone Coloring Kit; Factor II, Lakeside, AZ, USA) in the presence of the patient. Colouring was done while the patient was wearing the prosthesis, under a variety of light sources.
Finally, an acrylic nail was fabricated using autopolymerizing acrylic resin material (DPI, cold cure). The fabricated nail shell was trimmed to conform to the nail bed that had been created on the silicone finger prosthesis. Once verified, it was smoothened and polished. Single-part silicone was dispensed onto the nail bed over which the finished nail shell was positioned and secured in place with cyanoacrylate.
Medical adhesive (Edge adhesive; Factor II) was applied to the base of the prosthesis for retention and to reduce the gap between skin and prosthesis. The patient was instructed regarding wearing of the prosthesis and its maintenance. This medical adhesive was found to provide retention for more than 8 h, after that it needs to be reapplied.
Findings and outcome
Final prosthesis was found with adequate retention. The patient was satisfied with the aesthetic of the prosthesis.
Discussion
The amputation of one or more fingers of the hand, as the consequence of trauma or congenital absence of one or more phalanges, carries a serious reduction in hand function and social dysfunction for the patient. 7 Many injuries and traumatic amputations of fingers can be rescued by microsurgery through re-implantation. However, it may not be advisable 8 or possible in some cases such as the patient’s unwillingness or factors such as cost. It is in this group of patients that prosthesis can be provided and may offer great psychological aid. 9
The level of amputation also affects the outcome of the result. Distal phalange amputation can usually be restored with normal functions. If at least 1 cm of mobile phalynx remains, some restoration of active grasp is feasible. The more the length of residual stump, the better the retention achieved.
Silicone finger restorations have proven to be effective in terms of flexibility, excellent colour matching, ease of fabrication and more life-like appearance. Silicone finger restorations may also have additional functional benefits. Silicones, unlike polyvinyl chloride prosthesis, allow copying of the natural hand in every detail; the material is supple and not subject to ordinary thermal damage or ink stains. As the finger was to be sleeved in thin thickness of silicone, these types of prosthesis should be constructed with materials with high strength where the degree of flexion over the existing joint is considerable. Thinness of the silicone prosthesis allows good sensibility.
Osseointegrated dental implants have been used to retain prostheses.10–12 Retention is better than the retention obtained by the medical grade adhesives. But implant treatment is more expensive and it requires a surgical procedure and good bone quality to be successful. In recent decades, much research effort has been focused on the development of more functional artificial hands. The most technologically advanced prostheses are myoelectric ones. Robotic knowledge has been applied to improve some of the basic components of prosthetic hands such as the overall dexterity, electromyographic (EMG) recording and the sensing ability of the device. 13 The main disadvantages of these prostheses are cost, aesthetic and weight of the prostheses. Prostheses, particularly for patients in developing countries, should exhibit functionality at a minimum cost, durability, simplicity of repair, adaptability to local materials and cultural acceptability. 14
Nowadays, bionic fingers are also used as a treatment modality; these are powered prosthetic digits for one or more fingers in patient with amputation at a transmetacarpal level or higher. Their action depends on the remaining muscle fibres at the level of amputation to allow fine movement control. They move independently and bend at joints, and work in conjunction with any other remaining fingers to increase functional capabilities.
This article describes the rehabilitation of a finger with prosthesis, which is simple to construct, aesthetic, retentive and easy to maintain. Since there was no residual stump, it was difficult to get vacuum suspension, so the prosthesis was extended to palmar aspect of hand to achieve adequate retention through adhesive. As it was adhesive, retained sweating was an issue, but was manageable. The prosthesis thus fabricated merged with the adjacent tissues providing desired aesthetics and psychological boost to the patient.
Conclusion
Fabrication of finger prosthesis has not been a means of physical fulfilment, but it also has imparted a deep sense of psychological upliftment for this patient who was otherwise undergoing a social stigma causing embarrassment and lack of social acceptance. For most patients, the aesthetic appearance of an amputated finger plays a more important role than function. With the advancement in skill, technology and materials available today, the rehabilitation of an amputated finger is no more aesthetically challenging. When fabricated with immense care, they can be made life-like. A well-fabricated aesthetic prosthesis can help in providing the patients with psychological support.
Footnotes
Conflict of interest
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
