Abstract
Background:
We report our experiences of prosthetic fitting in quadruple amputees. Two patients underwent quadruple amputation after suffering from disseminated intravascular coagulation in conjunction with pneumococcemia with purpura fulminans.
Case Description and Methods:
The first patient, a 52-year-old man, underwent bilateral transradial, left transtibial, and right transfemoral amputation, and the second patient, a 62-year-old man, underwent bilateral transradial and bilateral transfemoral amputation, both for symmetrical peripheral gangrene subsequent to septic shock.
Findings and Outcomes:
The amputations were accompanied by skin damage due to ischemic tissue changes both on the stumps and on the nose and/or lips. The combination of the intensive prosthetic rehabilitation program and supportive medical care led to completely independent functioning, including driving a car, with the use of four prosthetic limbs and a wheelchair in both cases.
Conclusion:
Early initiation of a multidisciplinary approach can properly address impairments and minimize future disability.
Clinical relevance
We have reported our experience of limb fitting in two patients who had undergone quadruple amputation after suffering peripheral gangrene. Appropriate limb fitting that provides support in daily activities can address impairments and minimize disability.
Background
The major amputation of all four limbs (referred to as “quadruple amputation”) is a rare occurrence. According to the regional case registry in Hyogo prefecture, Japan, for the 30 years from 1968 through 1997, cases of quadruple amputation constituted only 0.02% of 5527 cases of lower extremity amputation. 1
Few studies have investigated prosthetic fitting for quadruple amputees. Serious damage requiring amputation of all four limbs has been reported in cases of electrical burns,2–5 complications of renal diseases, 6 and ischemic gangrene resulting from septic conditions.7,8 In this case report, we describe the management of prosthetic fitting in two patients with quadruple amputations, both of whom had suffered from pneumococcal purpura fulminans.
Case description and methods
Several problems associated with the use of prostheses by quadruple amputees became apparent during the rehabilitation program. The types of prostheses and improvements thereto were chosen for their abilities to enrich the patients’ activities of daily living and social participation. Quadruple amputees use their prostheses for special purposes not required by unilateral or bilateral amputees, such as standing up from the floor.
Case 1 history
The first patient was a 52-year-old male with bilateral transradial, left transtibial, and right transfemoral amputations. After the sudden development of septic shock, the patient’s general condition was stabilized over a period of 8 weeks. In addition to sequential amputations of four limbs, plastic surgery was performed on the nose and other facial areas.
The patient had no physical problems with the residual limbs. His only difficulty was the condition of the skin on the stumps, which was affected by livedo reticularis (a mottled reticulated vascular pattern that appears as a lace-like purplish discoloration). The skin was fairly vulnerable but was not ulcerated.
Findings and outcomes
The patient declined the use of myoelectric prostheses and an electric wheelchair, and his rehabilitation program relied on standard prostheses. Conventional bilateral body-powered transradial prostheses (figure-8 harness with a voluntary-opening hook device) were used for the upper limbs. The lower limb prostheses required silicone liners (Iceross®, Össur) in the sockets for skin protection. The goal of the program was the use of the prostheses in daily life, and the following special aspects were considered:
Upper limb prostheses: independent wheelchair handling
As the patient required a conventional wheelchair, several adjustments were made to improve the handling of the upper limb prostheses. The residual limbs were fixed using Northwestern-type sockets in order to prevent rotation of the prosthetic sockets during wheelchair propulsion and to maintain shock absorption and frictional force. This was achieved by attaching yellow rubber sponge pads covered with antiskid polyvinylchloride sheets to the medial sides of both sockets (Figure 1).
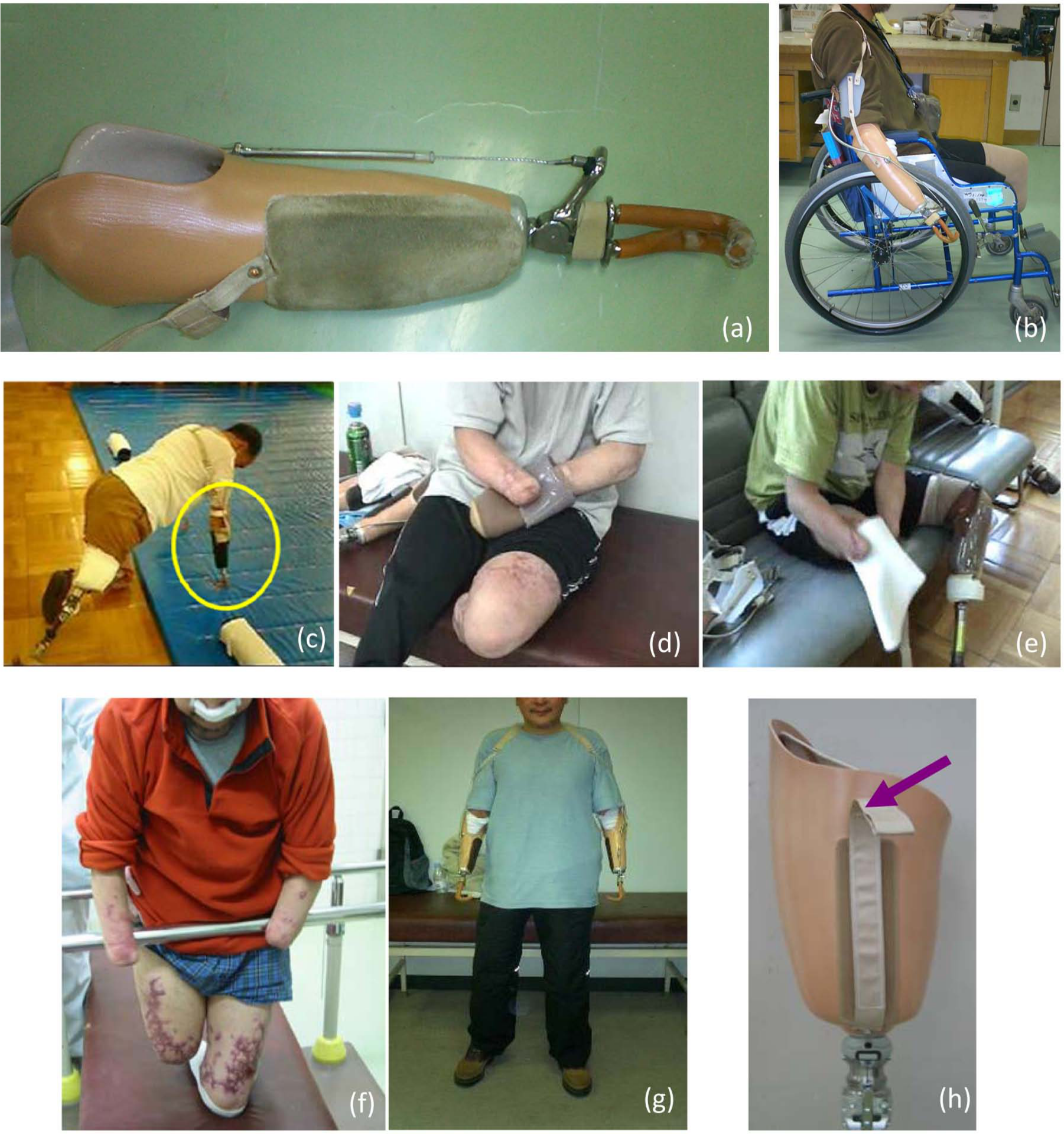
Case 1: (a and b) Upper limb prosthesis with pad for handling a wheelchair, (c) supporting body weight using the upper limb prostheses, (d and e) self-donning of silicone liners, subject (f) without and (g) with prostheses, and (h) socket suspension system with Velcro. Arrow shows the site of Velcro.
Upper limb prostheses: ability to support the body weight using the upper limbs
The patient had to be able to support his body weight using the upper limb prostheses when standing up from the floor or transferring to a wheelchair. Although the sockets were reinforced with carbon fiber–reinforced plastic, the strength of the prosthesis itself was unclear. Static strength testing using the Instron® universal testing machine (55R1125) showed that the prostheses could withstand 900 kg of mechanical vertical load (the maximum that the machine could produce). No breakage of the socket or damage to the devices was observed after 4 years of daily use. These results demonstrated that the durability of the prostheses was sufficient in case 1.
Lower limb prostheses: self-donning
Self-donning of the liners using the residual limbs without any other device required immense skill but was eventually accomplished. The upper limb prostheses were used for self-donning the lower limb prostheses. Donning a socket with a pin-lock liner generally requires setting the liner against the residual limb with the pin aligned correctly and winding the push button of the lock adapter.
A pin-lock system was not suitable for the patient in case 1 because the manipulations required were too complicated for him. However, it was not difficult to fasten the patellar-tendon-bearing cuff belt that suspended the left transtibial prosthesis using the upper limb prostheses. A Velcro suspension system 9 was used for the right transfemoral prosthesis. A Velcro strap at the end of the silicone liner was fed through a slot in the bottom front part of the socket. Pulling the strap with the upper limb prosthesis pulled the residual limb into the transfemoral socket. The strap was then attached with Velcro to the outside front part of the socket.
The patient achieved a successful prosthetic gait with the left transtibial and right transfemoral prostheses assembled with manually locked knee joints. In daily life, the patient predominantly used a wheelchair when outside of his home. He was able to use the prostheses to drive a car. The body-powered prosthesis on the right arm controlled the steering wheel, and the prosthesis on the left arm controlled the accelerator and the brake gear without the need for any adjustments. The steering wheel required a component to connect to the hook. In addition, the car was equipped with handling devices for the accelerator and brake systems on the driver’s left side.
Case 2 history
The second patient was a 62-year-old male with bilateral transradial and bilateral transfemoral amputations. Stabilization of his general condition and resolution of the dermatological problems on the stumps required more than 3 months. He also underwent plastic surgery on his upper lips. He had dermatological problems associated with his symptomatic diabetes, especially on the left forearm stump. Insulin treatment successfully improved the condition of the stump and made it possible to start prosthetic fitting.
In this case, the issues considered during early rehabilitation included dermatological problems on both residual upper limbs and the contracture of both shoulder joints (right shoulder flexion: 125°; left shoulder flexion: 100°). The left transradial residual limb in particular required wound care during the initial phase of hospitalization. Therefore, prosthetic fitting was initiated on the right arm (Figure 2).
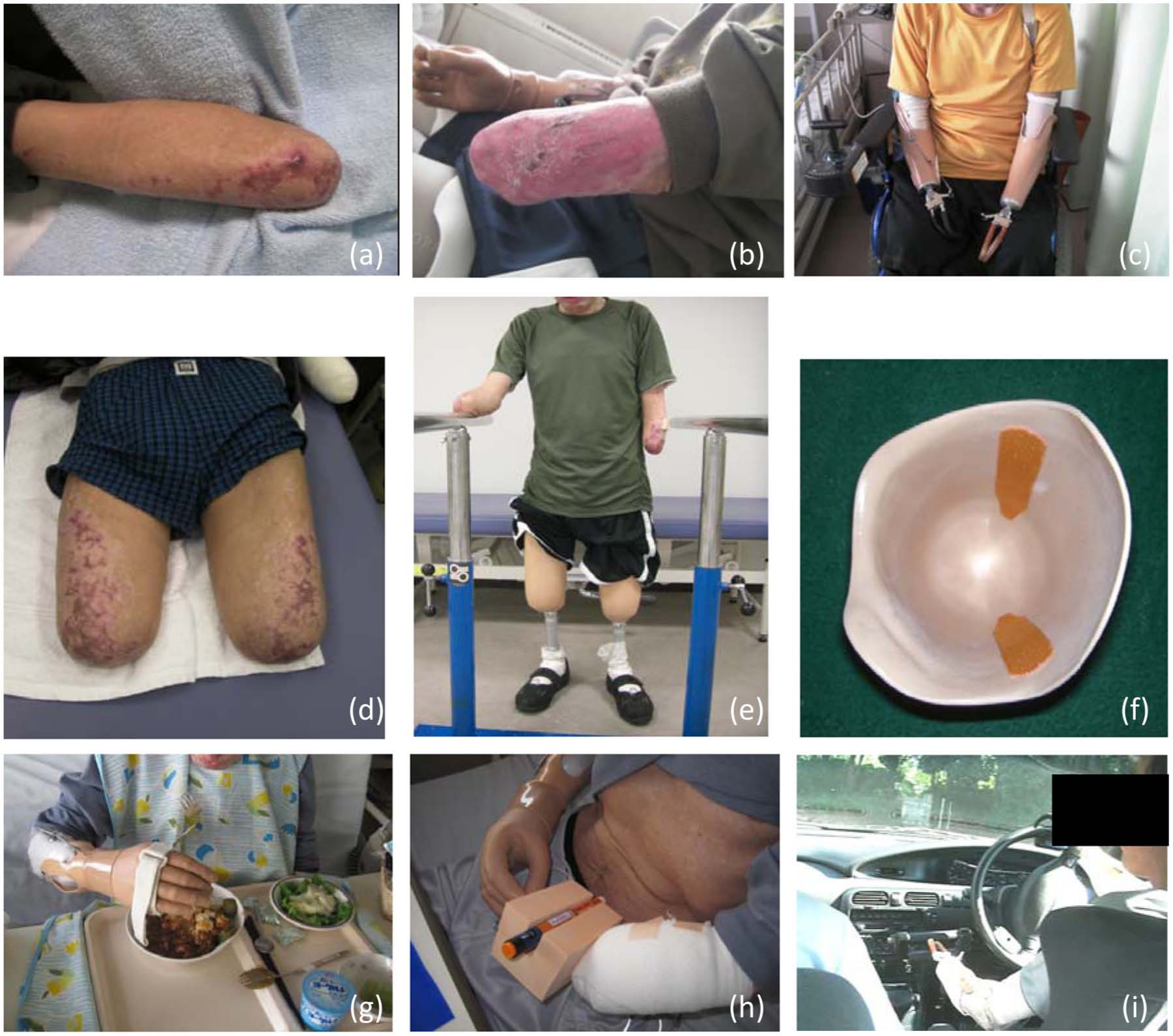
Case 2: (a) right and (b) left Residual upper limbs, (c) upper limb prostheses, (d) residual lower limbs and (e) with lower limb prostheses, (f) SAKAGE attached to the inside surface of the socket, (g) eating a meal using the upper limb prosthesis, (h) insulin injection using the upper limb prosthesis, and (i) driving a car using the upper limb prostheses.
Findings and outcomes
The rehabilitation program included not only the use of standard prostheses but also the use of a myoelectric prosthesis and an electric wheelchair. The goal of the program was to achieve the combined use of these tools in daily life, and the following special aspects were considered:
Upper limb prostheses
The patient found it difficult to wear a figure-8 harness due to the limited range of motion of both of his shoulders. Hence, a figure-9 harness was selected for ease of donning and doffing. The body-powered transradial prosthesis on the right residual limb included the Northwestern socket, a quick-disconnect wrist (Hosmer) for easy wrist rotation, and a voluntary-opening hook device (Hosmer).
After the completion of prosthetic training for the right arm, an attempt was made to fit a prosthetic arm on the left residual limb. However, no body-powered prosthesis could be provided for the left arm because the figure-8 harness is an essential component of bilateral body-powered prostheses.
A Northwestern socket and a friction wrist and hook (Hosmer) were selected for the left upper limb prosthesis to facilitate donning and doffing. Therefore, a combination of body-powered and non-body-powered prostheses was used. The body-powered prosthesis on the right arm was used mainly for performing fine work and the prosthesis on the left for arm-assisted activities.
Potential use of myoelectric prosthesis
A clinical evaluation of the patient’s potential for using a myoelectric prosthesis was carried out using the DMC plus® control system (Ottobock). Although the right residual limb (length, 15 cm) showed breakdown of the skin surface, a myoelectric signal could be acquired with good signal separation. The patient did not object to the weight of the myoelectric prosthesis. Moreover, he identified some advantages of the myoelectric prosthesis over the body-powered prostheses. For example, he was able to open and close the hand behind his back. He also found that he could lower his pants to use the bathroom faster and more easily with the myoelectric prosthesis than with the body-powered prosthesis. He also could manage his daily insulin injections without any assistance.
The left residual limb was shorter than the right (length: 11 cm). Although we could detect separated myoelectric signals, the dermatological problems precluded the use of a myoelectric prosthesis on the patient’s left arm. Fortunately, his activities of daily living were not limited despite the use of a myoelectric prosthesis only on the right.
Lower limb prosthesis: self-donning
The rehabilitation team set the goal of having the patient be able to walk a short distance in his house using his bilateral transfemoral prostheses. Silicone liners (Iceross transfemoral) were applied to both legs to protect the skin. The SAKAGE® (Lapoc), also called the Uni-Grip® (ST&G) in Western countries, was used to suspend the sockets. The SAKAGE was attached inside of the socket, where its directional texture facilitated donning and doffing the prostheses.
Stubbies were used for early gait training and were converted into SACH Feet (Ottobock) with pylons after a few weeks. These short knee-less prostheses were sufficient for household ambulation. The optimal length of the prostheses was determined to be 55 cm, as the patient’s top priorities were stability when walking and easy donning of the lower limb prostheses at bedside. After donning the silicone liners on the bed, the patient was able to slip his residual legs into each socket of the lower limb prostheses.
Unfortunately, a prosthetic knee joint could not be introduced because of the lack of space between the sockets and the feet and the requirement for light-weight prostheses. The patient successfully achieved household ambulation with the relatively short lower limb prostheses and generally used an electric wheelchair when out of his home. He was able to control the switches of the wheelchair using either the myoelectric prosthesis or the body-powered prosthesis in the right arm. There was no significant difference between the two prostheses for the purpose of controlling the electric wheelchair. The patient could also drive a car customized with driving devices for upper limb prostheses.
Discussion
Despite rapid and intensive intervention, purpura fulminans carries high rates of mortality and morbidity in survivors. A review of the literature concerning patients with symmetrical peripheral gangrene reported a mortality rate of 35%. 10
Lifesaving attempts are made in all cases managed in intensive care units. In addition to intensive supportive treatment, drug intervention, including administration of corticosteroids, anticoagulants, antiplatelet drugs, and activated protein C (drotrecogin alfa) to stabilize disseminated intravascular coagulation, is indicated.
So-called symmetrical peripheral gangrene often occurs due to ischemia in patients with purpura fulminans and requires amputation of the gangrenous area.11–14 An article by the Mayo Clinic described the various clinical manifestations of purpura fulminans observed in 12 cases. 15 Among these cases, three patients died within 1 week of the onset of disease, and eight of the nine surviving patients required amputation of at least one limb. Four patients required amputation of all four limbs. Silbart and Oppenheim 12 reported the details of 24 amputations in 12 pediatric patients as well as their medical and surgical treatment. Unfortunately, the details of the prosthetic management were not reported.
While our two patients experienced pneumococcal sepsis, some meningococcal infections also progress to purpura fulminans. Diabetes was not reported as a comorbidity in the Mayo Clinic series, and our patient had no history or hereditary background of diabetes. We considered it to be secondary symptomatic diabetes.
The limited number of previous case reports of quadruple amputations have included other causes, predominantly electrical burns and advanced renal failure. Garrison and Merritt reported in detail a large (1459 cases) series of patients with end-stage renal disease treated during a continuous 63-month period. In consideration of their general conditions, the three patients in whom all four limbs were amputated were fitted with adaptive equipment or below-the-elbow hook-type prostheses rather than with artificial limbs. 6
The goal of prosthetic rehabilitation in the present case report was self-donning of the limbs and restoration of locomotion. The prosthetic management of these quadruple amputees revealed some problems and limitations of the prostheses, which were overcome in each case. However, full ambulation in daily life should essentially not be expected of subjects who have undergone bilateral lower limb amputations. The combined use of prostheses and a wheelchair for locomotion should be considered. It is desirable for the patients to be able to put the prostheses on and take them off by themselves, and we achieved this goal in the present cases with the help of a roll-on liner.
Conclusion
We have reported our experience of limb fitting in two patients with quadruple amputation after pneumococcal purpura fulminans with disseminated intravascular coagulation. Appropriate limb fitting that supports the patient during daily activities can address the impairments and minimize future disability.
Footnotes
Ethical approval
Informed consent was obtained from both patients, and the contents of the present case study were reviewed and approved by the institutional review board of the National Rehabilitation Center for Persons with Disabilities.
Medical device statement
The devices in this article are approved for human use under the Japanese laws for medical devices.
Conflict of interest
The authors declare that there is no conflict of interest.
Funding
This work received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
