Abstract
Objective:
To investigate the surface topography and ultimate tensile strength of 3 types of nickel–titanium (NiTi) wires before and after 3 months of intraoral use and to assess the efficiency of the wires in cases requiring extensive alignment.
Methods:
NiTi wires of 0.016″ (0.40 mm) were divided into 3 groups—martensitic stabilized NiTi™ (group 1), austenitic active Copper NiTi™ 27°C (group 2), and martensitic active copper NiTi™ 35°C (group 3)—each further divided into 2 subgroups: (a) as-received wires; and (b) used wires. Each wire was subjected to scanning electron microscopy (SEM) analysis and tensile testing. Ultimate tensile strength data were analyzed using one-way analysis of variance (ANOVA) and Tukey testing at the .05 level of significance.
Results:
Martensitic stabilized archwires had a significantly lower ultimate tensile strength (93.99 ± 0.23 MPa) than martensitic active (116.96 ± 0.43 MPa) and austenitic active (106.94 ± 0.36 MPa) archwires. Among the used archwires, the martensitic stabilized ones showed the most and the martensitic active ones the least surface degradation.
Conclusion:
Ultimate tensile strength was the highest for martensitic active archwires with superior surface properties and the lowest for martensitic stabilized archwires with an increased amount of surface degradation.
Introduction
Malocclusion is a common problem across all age groups, with its prevalence estimated between 20% and 88%. 1 Tooth morphogenesis, development, and craniofacial growth are factors generally implicated in causation. 2 Crowding of the anterior teeth is a common and perplexing malocclusion with associated aesthetic and functional aberrations. 3 Maloccluded teeth require application of mechanical force for initial leveling and alignment. Prior to the introduction of nickel–titanium (NiTi) alloys into orthodontics, stainless steel (SS) was the material of choice. Degradation of the material on exposure to saliva and other natural bio-flora, with the release of degradation products, commonly termed “tribocorrosion,”4, 5 is associated with NiTi. Degradation of the material has clinical implications, such as low force exertion, stress-induced failure, and an undefined risk of tumorigenesis. 4 Investigators have also focused on adverse intraoral effects, such as pitting, crevice corrosion, and integument formation. 5 Initially, martensitic stabilized conventional NiTi alloys were introduced, followed by active generic NiTi alloys—austenitic active and martensitic active alloys. 6 These had properties of shape memory, greater elasticity, and the potential to simplify treatment.7-9 Studies analyzing the efficacy of heat-activated NiTi wires in the initial stages of treatment have shown inconclusive results.10, 11 A study evaluating the mechanical properties of heat-activated and superelastic archwires concluded that heat-activated wires had superior mechanical properties. 12 Data related to the efficacy of NiTi archwires in relieving crowding and failure rates on their use intraorally with unpredictable clinical responses occasionally and changes in material surface are scant. In vivo studies of orthodontic alloys have concluded that intraoral ageing of alloys affects their mechanical and surface properties.13, 14 The efficacy of heat-activated NiTi arch wires in relieving crowding, failure rates on use intra orally with unpredictable clinical responses occasionally and changes in material surface topography is minimal.15-17 A study evaluating the efficacy of conventional NiTi and copper NiTi wires in alleviating crowding showed no significant differences in the use of either wire type. 12 A recent systematic review was also inconclusive about the most effective archwire for leveling and aligning teeth. 18
The purpose of this in vivo comparative study was to test the hypothesis that complex conditions present in the oral cavity could alter the chemical and mechanical properties of NiTi archwires, leading to their possible failure. Extended alignment periods with NiTi wires cause degradation in their elastic properties, affecting their fracture resistance and ultimate tensile strength. Three types of NiTi wires were tested for their ultimate-tensile-strength and surface properties before and after 3 months of intraoral use to correlate the findings to clinical usage time.
Materials and Methods
Three types of 0.016-inch (0.40 mm) NiTi archwires from the same manufacturer (Ormco Corp, Glendora, CA)—martensitic stabilized NiTi™, non-superelastic (group 1), austenitic active copper NiTi™ 27°C, superelastic (group 2), and martensitic active copper NiTi™ 35°C, true shape memory (group 3)—were evaluated for ultimate tensile strength and surface topography alterations before and after 3 months of intraoral use. The study was reviewed and approved by the Institutional Ethics Committee (ACDS/IEC/09/Nov/2018). Forty lower archwires in each group further divided into 2 subgroups—as-received wires and used wires—were analyzed. The groups were: group 1—martensitic stabilized NiTi (1a: as-received wires, 1b: used wires); group 2—austenitic active NiTi (2a: as-received wires, 2b: used wires); and group 3—martensitic active NiTi (3a: as-received wires, 3b: used wires). Patients requiring fixed orthodontic therapy were included in this study. All patients received MBT (McLaughlin, Bennett, Trevisi) 0.22″ × 0.028″ prescription brackets (MiniTwin, Ormco, Glendora, CA).
Patients were randomly allocated to groups 1b, 2b, or 3b with the following inclusion criteria:
No medications; Little’s irregularity index greater than 4 mm, requiring non-extraction therapy; Male and female patients of age between 18 and 50 years; and No previous history of orthodontic treatment.
After placement of brackets, allocated archwires were engaged using elastomeric modules. The patients were given standard instructions. Only lower archwires were evaluated. The patients were followed up on at 4-week intervals for any breakages, and modules were changed every visit. After 3 months of intraoral use, the archwires were retrieved. All archwires were rinsed with distilled water to remove loosely bound deposits and were individually stored in sterilized pouches. Archwire placement and retrieval were done according to standard protocols. All samples were evaluated for: (a) ultimate tensile strength, using a specialized tabletop testing apparatus; and (b) surface morphology, analyzed using a scanning electron microscope.
Tensile Testing
The tensile properties of the archwires were measured using a testing apparatus, “TA.XTplusC, Stable Microsystems” (Figure 1). We followed a methodology similar to that described by Devaprasad et al, 19 who studied the fracture resistance of 0.016″ superelastic NiTi wires from 2 manufacturers and compared them in their as-received condition and after 3 and 6 months of intraoral use. The machine’s parameters were set to test a scale load of “1000 N,” and it was operated in the “tensile” mode at a crosshead speed of “5 mm/min” to enable analysis of the tensile strength of each wire, similar to a previously published article. 19 Each wire sample was cut at both ends for a standardized span of 20 mm and was placed between the jaws of the machine. The maximum tensile load of 1000 N at a rate of 5 mm/min, which the wire could withstand prior to its failure, was noted (Figure 2).
Apparatus for Testing Ultimate Tensile Strength of “TA.XTplusC, Stable Microsystems.”

Wire Section Tested for Ultimate Tensile Strength.

Surface Analysis
A scanning electron microscope (Thermo Scientific Apreo SEM) was used to study the surface topography of all the archwires at the magnification levels of 200×, 300×, 500×, and 1000×, sequentially, in the scanning mode. For scanning electron microscopy (SEM) analysis, 6 mm of archwire was cut from one end of all the used and unused archwires, mounted on metal studs, and evaluated. These metal studs were then placed in a vacuum-evacuated chamber and bombarded with electrons at 20 kV accelerating voltage whose reflection intensity was quantified and analyzed. The surfaces of all the archwires were analyzed on the attached computer, and representative secondary electron images were then obtained.
Statistical Analysis
The required sample size was estimated using G Power software Ver 3.1.9.2. The measured effect size (f) at 35%, study power at 80%, and error margin at 5% were considered, for which the total sample size required was 114, rounded to 120. Three wire groups of 40 wires, each subdivided into as-received wires and used wires (20 each), were analyzed. Quantitative analysis of tensile strength was done statistically using one-way analysis of variance (ANOVA), with the wire type serving as a predictor. Group differences were evaluated using Tukey’s HSD (honestly significant difference) test, with a P-value < .05 considered as the level of statistical significance.
Results
Table 1 shows the ultimate tensile strengths of the as-received and used archwires. The mean values and standard deviations reported are rounded to the nearest 0.01 MPa. The results show a statistically significant difference in the mean ultimate tensile strengths of all the 6 subgroups at P < .001.
Comparison of Mean Ultimate Tensile Strength (in MPa) of 6 Groups Using One-Way Analysis of Variance Test.
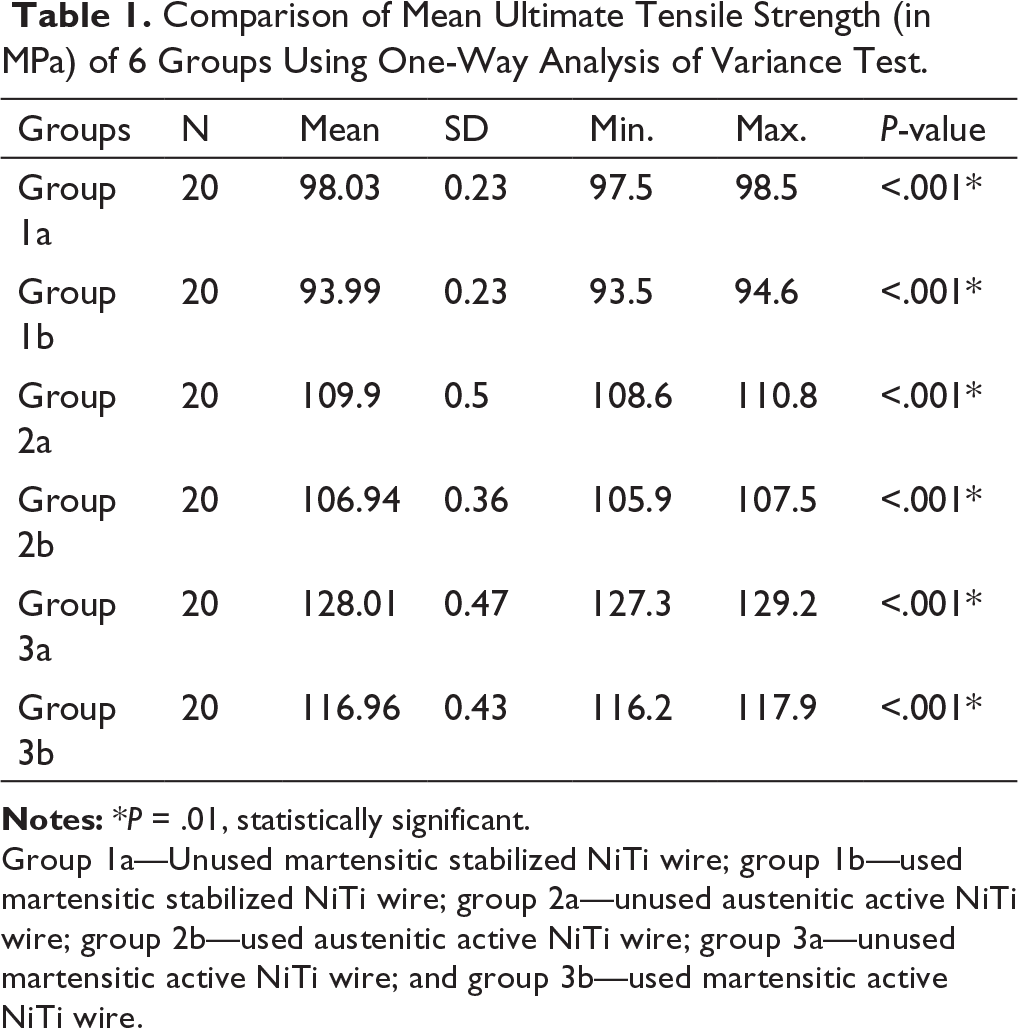
Group 1a—Unused martensitic stabilized NiTi wire; group 1b—used martensitic stabilized NiTi wire; group 2a—unused austenitic active NiTi wire; group 2b—used austenitic active NiTi wire; group 3a—unused martensitic active NiTi wire; and group 3b—used martensitic active NiTi wire.
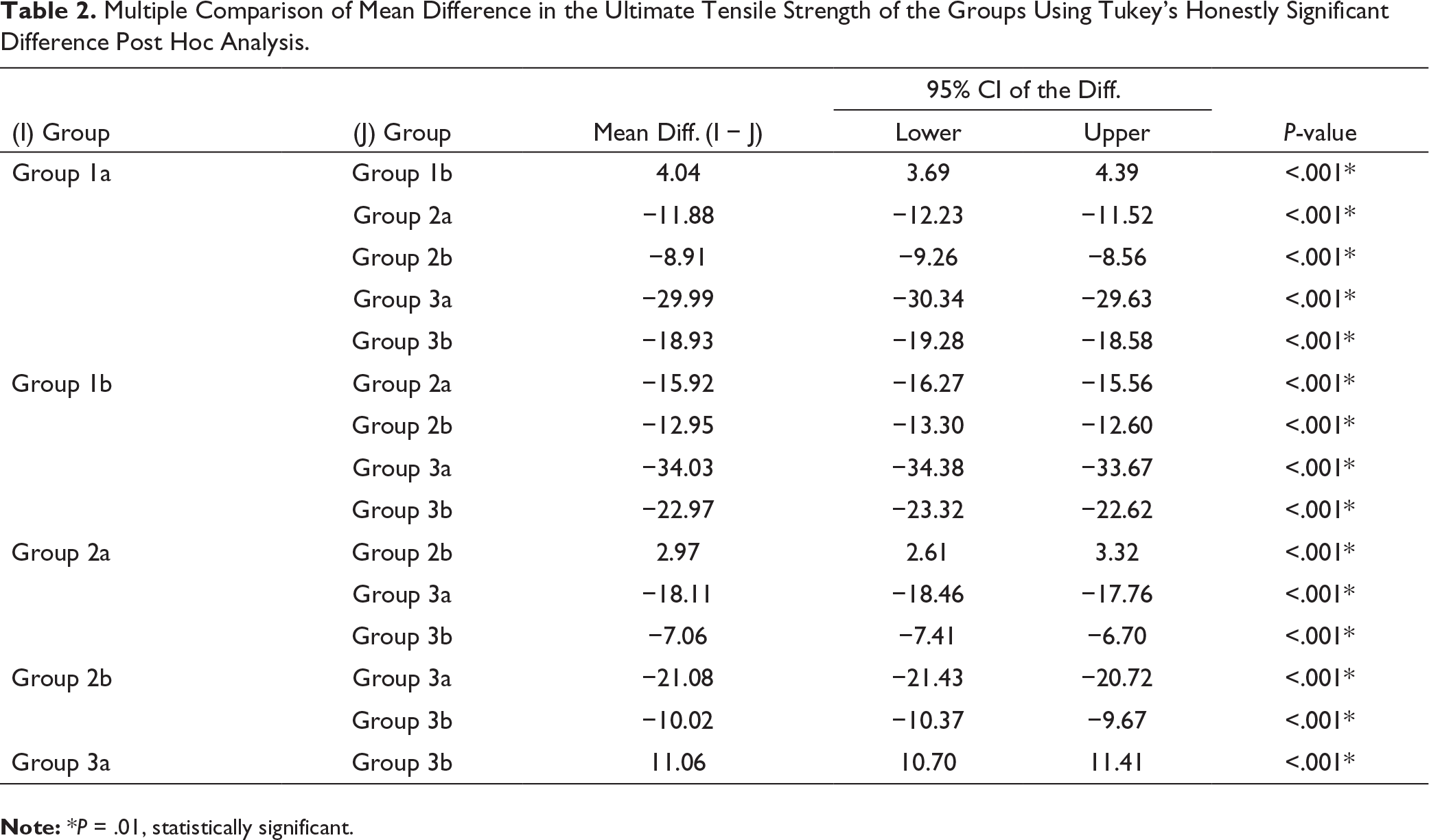
Multiple Comparison of Mean Difference in the Ultimate Tensile Strength of the Groups Using Tukey’s Honestly Significant Difference Post Hoc Analysis.
The topography of all the unused wires shows surface irregularities, with characteristic striations derived from the drawing process. Figure 3c depicts the surface of the unused martensitic active NiTi wires, which show reduced striations and surface irregularities as compared to the martensitic stabilized and austenitic active wires.
The used-wire topography was rough, with plaque deposits and surface abnormalities, assessed using the secondary-electron images for all the tested samples. The martensitic active NiTi wire surfaces showed reduced porosity and plaque deposits relative to the martensitic stabilized and austenitic active wires. Figure 4b depicts used martensitic stabilized NiTi wire surfaces revealing the maximum surface roughness, porosity, and plaque deposits.
Representative Scanning Electron Microscopy Images, at 1000× Magnification, of: (a) Unused Austenitic Active Nickel–Titanium; (b) Unused Martensitic Stabilized Nickel–Titanium; and (c) Unused Martensitic Active Nickel–Titanium.

Representative Scanning Electron Microscopy Images, at 1000× Magnification, of: (a) Used Austenitic Active Nickel–Titanium; (b) Used Martensitic Stabilized Nickel–Titanium; and (c) Used Martensitic Active Nickel–Titanium.

Discussion
Archwires form the backbone of modern orthodontic therapy. Wires made of NiTi are used extensively in the treatment of malocclusions. Scant information exists on the intraoral ageing pattern of NiTi archwires and their associated phenomena such as surface alterations, structural changes, and variations in mechanical properties with use. 20 Ideal archwire properties include a low load deflection rate, flexibility with high resistance to orthodontic forces, low elasticity, a low friction coefficient with high springiness, high resilience, corrosion resistance, and biocompatibility. The titanium in NiTi helps in the formation of a stable passive layer that increases the corrosion resistance of an archwire. 21 NiTi archwires are thus suitable for and yield good results in the treatment of most orthodontic problems. 2
In vitro and in vivo studies have shown conventional and heat-activated NiTi wires to have different structural and mechanical properties. 2 Most studies have used experimental approaches 10 and storage media, 13 which cannot simulate the in vivo environment accurately, bringing an element of uncertainty to the findings. Wires with a light mechanical force and low load deflection ratio are more efficient and hence preferred for the initial alignment phase. 22 The wires assessed in this study were grouped into either non-superelastic martensitic stabilized, superelastic or austenitic active copper NiTi™ 27°C and true shape memory or martensitic active copper NiTi™ 35°C, according to data published by Kusy et al. 6 Most manufacturers do not disclose structural data and manufacturing processes, which could enable an orthodontist to choose the right archwire for a given clinical situation.
Ultimate tensile strength (measured in MPa) is the greatest stress an archwire can bear and may vary due to composition and defects in the drawing process. The ultimate tensile strength of the wires used in the study was evaluated using a tabletop testing apparatus (TA.XTplusC, Stable Microsystems). The test revealed the highest degradation in martensitic stabilized NiTi and the lowest degradation in martensitic active NiTi among the wire types studied, similar to the findings of Fernandes et al. 12
In an in vivo evaluation, superelastic NiTi wires exhibited degradation in ultimate tensile strength after 6 months of use. 19 Superelastic NiTi wires retrieved after 6 months of intraoral use showed deep crevices and indentations resulting in reduced tensile strength, 19 in a study by Devaprasad et al. Our study revealed alterations in the surface texture and mechanical properties of all the retrieved archwires. The results were similar to those of Bavikati et al 23 and Eliades 20 et al.
A few studies have analyzed surface characteristics, elemental composition, and mechanical properties of conventional SS orthodontic wires. 4 Both SS and NiTi wires show deep surface pits due to complex manufacturing processes and surface treatment. 24 The intensity of drawing marks on the surface of a wire depends on its period of use, spinneret finishing, alloy composition, and thermodynamic properties. The effects include greater concentration of tension in the wires due to long-term use of the spinneret, reduced traction resistance, increased coefficient of attrition, and biofilm adhesions. Superelastic NiTi archwires manufactured by Masel show low wire-surface roughness. 25 An in vitro evaluation of NiTi archwires from Ormco (Ormco Corp, Glendora, CA) showed visible drawing marks under magnification, along with micro-cavities, which lead to higher coefficient of attrition. 25 NiTi wires manufactured by 3M Unitek (Unitek Corporation, Monrovia, USA) were found smoother than those manufactured by American Orthodontics (American Orthodontics, Sheboygan, WI). 19 A study evaluating the characteristics of SS Australian wires (A.J. Wilcock, Whittlesea, Victoria, Australia) showed them to possess irregular surfaces and excessive porosity, 26 more so among the higher grades. 26
Fischer-Brandies et al 27 demonstrated that copper NiTi wires had a significant percentage of copper in addition to nickel and titanium in their composition. Addition of copper to NiTi alloys increases their strength and reduces hysteresis as measured by the area between the first plateau (austenite transforms to martensite) and second plateau (martensite transforms to austenite). 6 Further, 0.5% and 0.2% chromium are added to reduce the phase transformation to 27°C and 35°C, respectively. 6 An in vitro study 25 comparing Ormco superelastic and heat-activated NiTi wires found increased pitting in heat-activated NiTi, attributed to particle pullout after tensile testing, which was not noted in this study where in vivo testing showed no such severe effects.
The ageing effects of NiTi wires after use include adsorption and calcification of biofilms with increased porosity and roughness leading to decreased tensile strength and fracture resistance. Surface texture is analyzed using a profilometer, 19 integrated scatter, diffuseness, angular scattering distributions, and SEM. In our study, surface morphology was evaluated using a scanning electron microscope, and the representative electron images obtained were assessed. It showed the unused wires as having surface abnormalities, as reported previously in the literature.
Our study showed an increase in the amount of degradation in the form of pitting, plaque formation, and increased porosity across all the retrieved archwires, in concordance with previous results. The tested NiTi wires had nickel and titanium as the main elements of the alloy, with minor differences in their composition. 25
In the present study, all the archwires exhibited pitting and plaque deposits. The martensitic stabilized archwires displayed a higher degree of surface roughness compared to the other 2 types of archwires, and hence they were the most susceptible to crevice corrosion. Alteration in surface texture can be attributed to various intraoral conditions and to the engagement of the archwire with the slot. 20 The surface alterations of the retrieved wires profoundly altered their mechanical properties, making them less fracture-resistant to orthodontic forces. The microstructure of martensitic active shape memory alloys is dominated by equiaxed grains rather than dendrites, as noted in conventional nitinol alloys, making them less susceptible to corrosion. 28 Superelastic NiTi wires are unbreakable in vitro, 20 but they do break more frequently when used intraorally. In moderate-crowding cases, which require extended use of an aligning archwire, fracture of the initial wire is one of the most common problems. 29 Any alteration in surface topography can initiate a fracture. 30 No wire breakage was noticed in any of the 3 groups during the study period. The martensitic stabilized archwires retrieved after 3 months of intraoral use, with maximum pitting and indentations, displayed a reduction in ultimate tensile strength. These wires were the most vulnerable to fracture. As the properties of NiTi are altered after intraoral use, it is not advisable to expose martensitic stabilized (non-superelastic) and austenitic active (super elastic) archwires to the intraoral environment for 3 months or longer. Martensitic active (true shape memory) archwires, with better structural and mechanical properties relative to the other 2 wire types, can be used efficiently in cases with extensive crowding requiring additional time for alignment.
The results in this study should not be considered as conclusive evidence, as the sample size was small and also the variations in different clinical situations and properties of the wires were not assessed. Intragroup variability was also not assessed but could be considered in future studies for additional information.
Conclusions
Martensitic active NiTi archwires after 3 months of intraoral use showed the least surface abnormalities and superficial plaque formation compared to the other 2 tested wires, which decrease their surface roughness, resistance to shear forces, and corrosion rate. Surface degradation was the highest in the martensitic stabilized NiTi wires.
Ultimate tensile strength (fracture resistance) was the highest in the martensitic active NiTi after 3 months of intraoral use, thus enabling it to be used in cases requiring extensive alignment for periods 3 months and longer.
Clinically, martensitic stabilized and austenitic active wires can be used in cases with mild crowding (Little’s irregularity index < 4 mm), but in cases with moderate to severe crowding (Little’s irregularity index >4 mm) where archwires have to remain for longer periods, the martensitic active wire is the material of choice.
Footnotes
Declaration of Conflicting Interests
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Research Ethics and Patient Consent
Prior to commencing this study, the protocol was approved by the Institutional Ethics Committee at Army College of Dental Sciences. (ACDS/IEC/09/Nov/2018).
