Abstract
From 2016 to 2019, Southeastern Brazil faced an outbreak of yellow fever (YF) affecting both humans and New World primates (NWP). The outbreak was associated with a marked increase in traumatic lesions in NWP in the affected regions. Non-thrombotic pulmonary embolization (NTPE) can be a consequence of massive traumatic events, and it is rarely reported in human and veterinary medicine. Here, we describe NTPE of the brain, liver, and bone marrow in free-ranging NWP, highlighting the epidemiological aspects of these findings and the lesions associated with this condition, including data on traumatic injuries in wild NWP populations during the course of a recent YF outbreak. A total of 1078 NWP were necropsied from January 2017 to July 2019. Gross traumatic injuries were observed in 444 marmosets (44.3%), 10 howler monkeys (23.2%), 9 capuchins (31.0%), 1 titi-monkey (50.0%), and 1 golden lion tamarin (33.3%). NTPE was observed in 10 animals, including 9 marmosets (2.0%) and 1 howler monkey (10.0%). NTPE was identified in the lung and comprised hepatic tissue in 1 case, brain tissue in 1 case, and bone marrow tissue in 8 cases. Although uncommon, it is important to consider NTPE with pulmonary vascular occlusion during the critical care of traumatized NWP. In addition, this study highlights the importance of conservational strategies and environmental education focusing on One Health, not only to protect these free-ranging NWP populations but also to maintain the efficacy of epidemiological surveillance programs.
Traumatic injuries are well characterized in veterinary medicine, with a particular focus on forensic pathology.8,23,25,30 In free-ranging New World (neotropical) primates (NWP), traumatic injuries are important and prevalent, usually associated with periurban NWP populations and anthropogenic factors, and often have a negative impact on NWP conservation strategies.6,15,22,27
Non-thrombotic pulmonary embolism (NTPE) may be a consequence of trauma, but it is less common than pulmonary thromboembolism. NTPE is defined as the occlusion of pulmonary arteries and capillaries by non-thrombotic material, including adipose tissue, bone marrow, foreign material, gas, neoplastic cells, or infectious agents. 18 Both in humans and in animals, NTPE caused by brain, liver, or bone marrow tissues is uncommon and is usually associated with massive traumatic injuries.1,11,17,20,29
From 2016 to 2019, an outbreak of yellow fever (YF) took place in Southeastern Brazil affecting humans and NWP. This outbreak resulted in high lethality rates in NWP populations, especially howler monkeys, due to their high susceptibility to this disease.5,16,24 This YF outbreak was associated with a marked increase in trauma affecting free-ranging NWP from the regions affected by the YF outbreak. Due to misinformation and fear among the human population, and the misconception that NWP were responsible for transmitting YF, hundreds of NWP were brutally killed.15,27
Here, we describe a series of cases of NTPE caused by fragments of brain, liver, and bone marrow tissues in traumatized free-ranging NWP, highlighting the epidemiological aspects of these findings and the lesions associated with this condition, including additional data on traumatic injuries affecting these wild NWP populations. The diagnosis of embolic lesions as described in this study may allow identification of traumatized animals even when examining an incomplete set of tissue samples in the absence of a comprehensive gross report. Importantly, although previously recognized in humans, with the exception of bone marrow and fat embolism in experimental cynomolgus macaques, 9 these embolic lesions have not been reported in free-ranging nonhuman primates.
Materials and Methods
Animals
This study included NWP necropsied between January 2017 and July 2019 at the Instituto Municipal de Medicina Veterinária Jorge Vaitsman (IJV, Rio de Janeiro, Brazil), including wild NWP that were found dead from all regions in the State of Rio de Janeiro. Data about geographic origin, sex, age, and gross findings were provided by the IJV. All animals were tested for YF virus infection by quantitative reverse transcription polymerase chain reaction (RT-qPCR) by the official diagnostic service. This study was authorized by the government environmental agency (ICMBio, Brazil) under the SISBIO license number 67014. All procedures strictly adhered to humane care of animals and all applicable laws and regulations. This was a retrospective study based on diagnostic samples submitted for laboratory analysis.
Necropsy and Histopathology
Necropsies of NWP were performed by a veterinary pathologist at the IJV. Samples of lung, liver, heart, kidney, spleen, and brain were fixed in 10% buffered formalin and processed for paraffin embedding. Additional organ samples were collected in cases with gross changes in any organ or tissue. Paraffin-embedded tissue sections (3–4 µm thick) were stained with hematoxylin and eosin (HE) and analyzed under light microcopy.
Immunohistochemistry
Anti-hepatocyte-specific antigen (Hep Par 1) monoclonal antibody was used in cases of NTPE suspected to be composed of liver tissue; anti–glial fibrillary acidic protein (GFAP) and anti–neurofilament protein were used for NTPE suspected to be composed of brain tissue; and anti-myeloperoxidase (MPO) was used for NTPE suspected to be composed of bone marrow tissue. Antigen retrieval protocols and information about primary antibodies are detailed in Table 1. Negative controls included sections incubated with phosphate-buffered saline instead of the primary antibody.
Primary antibodies and protocols used for immunohistochemistry in this study.

Briefly, lung samples with tissue embolism were selected based on evaluation of HE-stained slides. Lung sections (3–4 µm thick) were mounted on silanized slides, deparaffinized in xylene, and hydrated in decreasing ethanol concentrations. Endogenous peroxidase activity and nonspecific protein antibody binding were blocked using a blocking solution provided with a commercially available kit (Envision®; Dako). After incubation with the primary antibodies, slides were rinsed and incubated with a secondary anti-mouse/anti-rabbit antibody conjugated with a polymer for 30 minutes at room temperature (Envision®; Dako). Reaction was revealed with a 3,3′-diaminobenzidine (DAB) solution, and sections were then counterstained with Mayer’s hematoxylin. Between all steps mentioned before, slides were washed with Wash Buffer® (1×) provided by a commercially available kit (Envision®; Dako).
Statistical Analysis
Data were analyzed using the GraphPad Prism software (version 9.0). Descriptive statistics and Fisher’s exact test for nonparametric data were performed.
Results
Epidemiologic Data on Traumatic Cases
A total of 1078 NWP were necropsied from January 2017 to July 2019, including 1001 marmosets (Callithrix sp.), 43 howler monkeys (Alouatta sp.), 29 capuchins (Sapajus sp.), 3 lion tamarins (Leontopithecus sp.), and 2 titi-monkeys (Callicebus sp.). Grossly identifiable traumatic injuries were observed in 444 marmosets (44.3%; 444/1001), 10 howler monkeys (23.2%; 10/43), 9 capuchins (31.0%; 9/29), 1 titi-monkey (50.0%; 1/2), and 1 golden lion tamarin (33.3%; 1/3).
Gross traumatic lesions were grouped into blunt or sharp trauma (contusions, lacerations, perforations, organ ruptures, and fractures) or thermal injuries (burns) (Table 2). There were no lesions attributable to gun shots, and no firearm projectiles were detected in any of the animals. Considering all genera included in this study, more than 90% of traumatic lesions were due to blunt or sharp trauma, affecting the head, thorax, abdomen, arms, legs, and tail. In addition, there were cases with a single traumatic injury and cases characterized as polytraumatized (multiple affected sites) (Table 2). In marmosets, gross traumatic injuries were observed more often in the head (P < .01) and less frequently in the limbs and tail (P < .01). Howler monkeys and capuchins did not have statistically significant differences in the frequency of affected sites. The titi-monkey had a fissure in the occipital bone with focal subcutaneous hematoma and a submeningeal blood clot, whereas the lion tamarin had severe head trauma with multiple fractures of the skull, severe loss of brain tissue, fractures of several ribs with laceration of intercostal muscles, and rupture of the diaphragm and the liver.
Types and distribution of gross traumatic lesions identified in the period January 2017 to July 2019 in 5 different genera of free-ranging New World primates.

Different letters in the same column indicate statistically significant differences (Fisher’s exact test P < .01).
Abbreviation: n, number of animals.
Gross traumatic lesions were observed more frequently in marmosets than in howler monkeys (P < .01). Traumatized juvenile marmosets were more frequent than adults (P < .01), with no statistically significant difference between males and females. Among howler monkeys, traumatized males were more frequent than females (P < .001). Traumatic lesions were not associated with YF virus infection in marmosets (P = .2559), howler monkeys (P = .2661), or capuchin (P = .2917). Additional details about these cases are provided in Table 3.
Epidemiological data from the cases with gross traumatic lesions identified in the period January 2017 to July 2019 in 5 genera of free-ranging New World primates.

Different uppercase letters in the first row indicate statistically significant differences among genera, whereas different lowercase letters indicate statistically significant differences between T and NT animals in each genus according to yellow fever diagnosis, sex, age, and geographic distribution (Fisher’s exact test; P < .01).
Abbreviations: n, total number of primates; T, traumatized; NT, non-traumatized.
NTPE Cases
NTPE was observed in 10 animals (cases 1–10; Supplemental Table S1), including 9 marmosets (2.0%, 9/444) and 1 howler monkey (10.0%, 1/10), with no statistically significant difference in the frequency of NTPE between these 2 genera. NTPE was only observed in the lung. In marmosets, the NTPE was composed of liver, brain, or bone marrow tissues, whereas the only case affecting a howler monkey involved bone marrow embolism.
NTPE of hepatic tissue was observed in only 1 animal (case 1), an adult female marmoset, polytraumatized, with multiple sites of rupture of the liver, lungs, and spleen. Microscopically, there were multiple emboli measuring 200 to 800 µm in diameter, occluding arteries in the pulmonary parenchyma. The emboli were characterized by cords of epithelial cells with morphology compatible with hepatocytes delimiting vascular spaces similar to hepatic sinusoids (Fig. 1A). All emboli in this case had a strong and diffusely positive cytoplasmic immunolabeling for Hep Par 1, confirming the hepatic origin of the emboli (Fig. 1B). There was moderate multifocal alveolar edema and hemorrhage, but these changes were not restricted to areas affected by embolism.
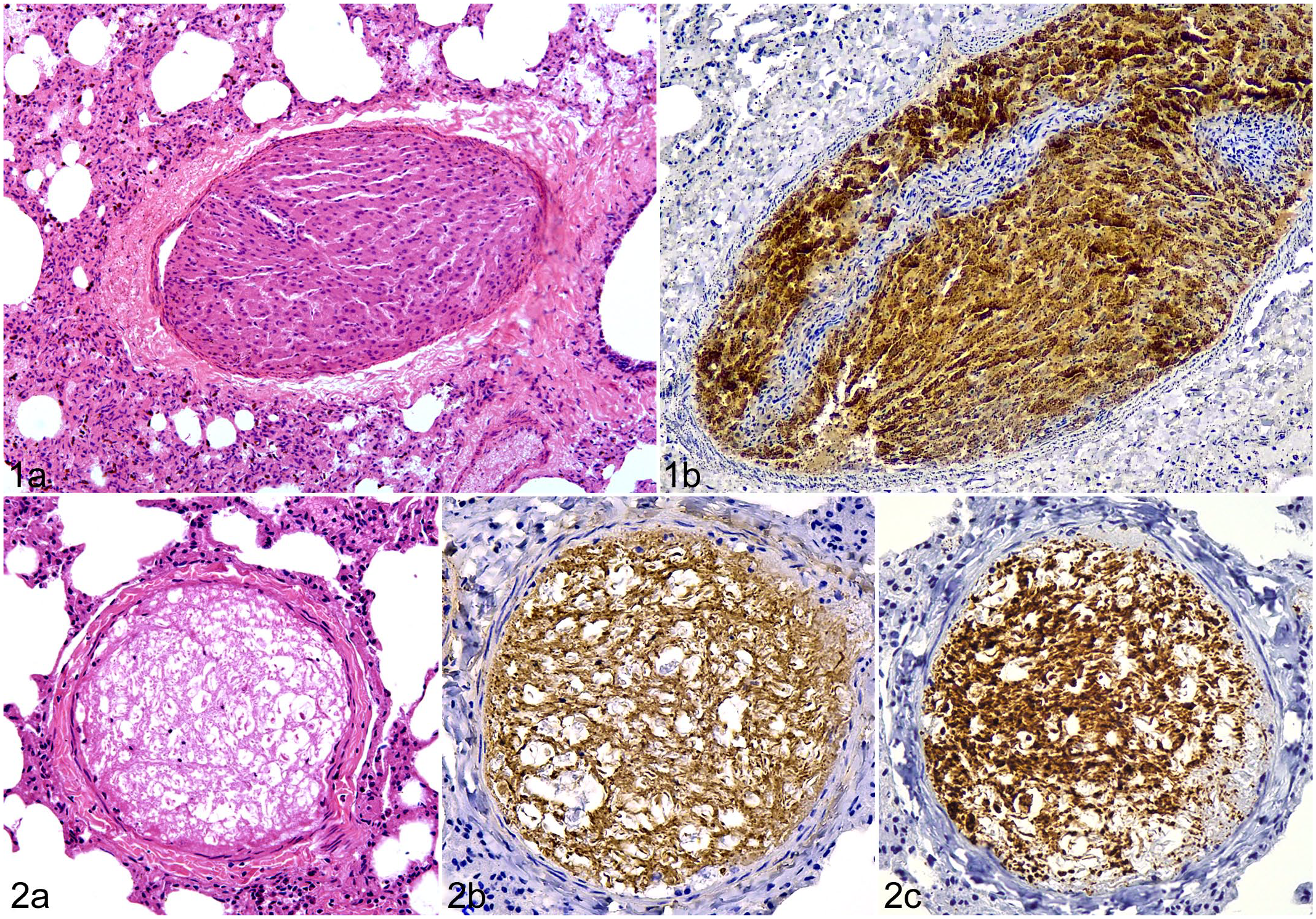
Non-thrombotic pulmonary embolism composed of hepatic tissue, lung, marmoset.
NTPE of brain tissue (case 2) was observed in only 1 animal, an adult female marmoset, also polytraumatized, with multiple fractures of the skull, jaw, and ribs, as well as brain evisceration and laceration, with severe meningeal hemorrhage. Microscopically, emboli occluded 2 pulmonary arteries, measuring 250 to 300 µm in diameter. Emboli in this case were characterized by a hypocellular tissue with a web pattern and rare cells with small nuclei, morphologically compatible with oligodendrocytes, suggestive of white matter (Fig. 2A). The emboli had a strong and diffusely positive immunolabeling for both GFAP and neurofilament protein (Fig. 2B, C). There was marked congestion particularly affecting larger arterioles, which was probably due to vascular occlusion by the emboli. In addition, there was a mild multifocal interstitial pneumonia, which was not associated with embolism.
Eight of the NTPE cases diagnosed in this study were composed of bone marrow tissue (cases 3–10). Seven of these cases affected marmosets and 1 case was observed in a howler monkey. All were associated with blunt trauma. Bone fractures were observed in all marmosets with this kind of embolism, but not in the affected howler monkey (Supplemental Table S1). Histopathology from these cases revealed a few to several small pulmonary arteries filled with a tissue composed of a heterogeneous population of myeloid cells interspersed with adipose tissue, ranging from 50 to 200 µm in diameter (Fig. 3A). By immunohistochemistry, the embolic tissues had positive heterogeneous immunolabeling for MPO, compatible with a polymorphic population of myeloid cell lineage, supporting the morphologic identification of the emboli as bone marrow tissue (Fig. 3B). Pulmonary alveolar hemorrhage and edema was observed in all cases with embolism, but it was not restricted to sites of embolism. In addition, the howler monkey with NTPE was also positive for YF virus, presenting the typical massive necrotizing hepatitis with Councilman-Rocha Lima bodies. Gross and histopathological findings from these 10 cases are detailed in Supplemental Table S1.
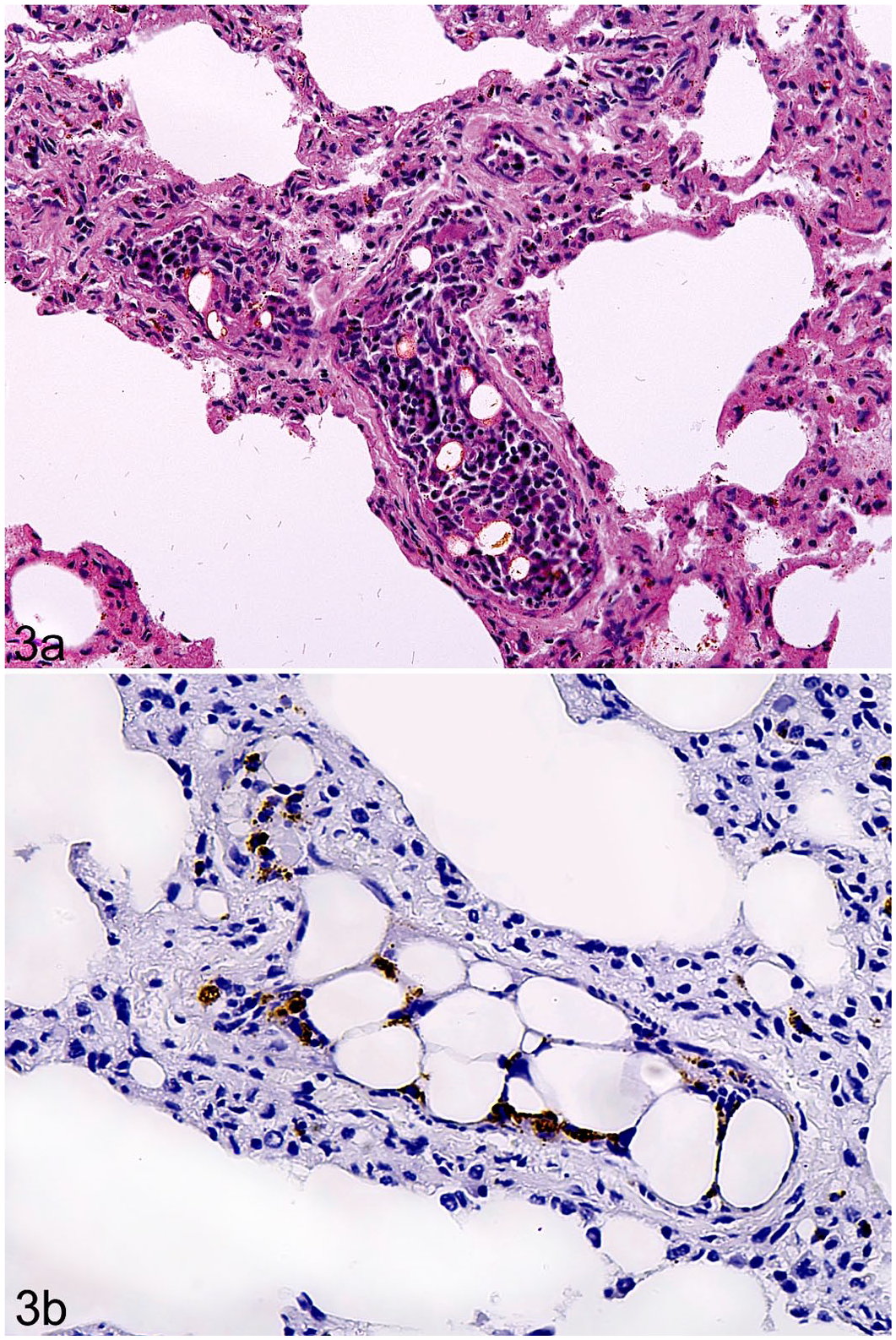
Non-thrombotic pulmonary embolism composed of bone marrow tissue, lung, marmoset. (A) Pulmonary artery occluded with bone marrow and fat tissue. Hematoxylin eosin. (B) Heterogeneous immunolabeling. Immunohistochemistry for myeloperoxidase.
Discussion
NWP belonging to the Callitrichidae family, especially Callithrix spp., have a high ability to survive in urbanized fragmented habitats, adapting well to anthropogenic changes. 10 However, this also makes them more exposed to anthropogenic trauma, such as electrocution, roadkill, dog attack, and direct human aggression.6,15,22,27 Importantly, in our study, Callithrix spp. (marmosets) were the main genus affected by traumatic events, and although it was not possible to precisely identify the cause of the trauma, blunt and sharp trauma represented more than 90% of the cases, and the head was the most commonly affected site in marmosets. The higher frequency of traumatic lesions in marmosets than in howler monkeys is likely explained by their social behavior as marmosets are highly susceptible to anthropogenic influence when compared with howler monkeys, which rarely get in close proximity to humans. Under these conditions, juvenile marmosets are supposedly less experienced and/or less agile, and therefore tend to be more susceptible to human-induced trauma.
There was no correlation between trauma and YF infection, indicating that many NWP deaths reported during the course of the YF outbreak were not associated with YF infection itself. Therefore, although the YF outbreak resulted in a great impact on wild NWP populations,3,16,26 especially among highly susceptible hosts such as howler monkeys,4,24 the indirect impact caused by high numbers of traumatic events during the same period is also very concerning and highlights the urgent need for environmental education and better strategies for wild NWP conservation. Furthermore, preservation of free-ranging NWP populations is not only an environmental conservation need, but it also has a significant public health relevance, as their phylogenetic proximity with humans makes nonhuman primates sentinels for certain zoonotic diseases such as YF.14,19 Thus, impairment of their natural habitat may lead to impairment of epidemiological surveillance programs.
In forensic pathology, NTPE composed of hepatic tissue is rare; it has been reported in humans involved in motor vehicle accidents, with multiple lacerations of the liver, symptoms related to acute pulmonary occlusion and rapid progressing to death.17,28 The one marmoset with NTPE composed of liver tissue in this study also had multiple lacerations of the liver with severe hemoperitoneum, rupture of the lungs and spleen, as well as multiple fractures in the ribs. Cases of pulmonary embolism caused by brain tissue are also uncommon, and they are usually associated with massive skull damage and cerebral laceration, with an incidence ranging from 1.9% to 10.0% in human cases of death by head trauma.2,21,29 In animals, cases of NTPE composed of brain tissue are reported in cattle subjected to slaughter using captive bolt guns, 1 and rarely in dogs and birds with severe head trauma.13,20 Therefore, head injury with a severe brain tissue involvement is the cause of this type of NTPE as observed in a marmoset in this study.
In contrast, bone marrow embolism of the lung is more commonly reported. In addition to traumatic injuries, this kind of embolism is also associated with other causes of bone marrow disruption, such as bone infarction secondary to sickle cell anemia or bone marrow neoplasia.11,12 There is only 1 previous report of NTPE in nonhuman primates caused by bone marrow and fat tissues, which included 5 cases affecting cynomolgus macaques (Macaca fascicularis) with clinical and histological evidence of pulmonary embolism that were thought to result from multiple bone marrow biopsies. 9 In our cases, all marmosets with bone marrow embolism had bone fractures. In contrast, the one affected howler monkey had lesions of blunt trauma, including inguinal hematoma, ruptured liver, and hemoperitoneum. Therefore, we hypothesize that this howler monkey may have had incomplete fractures or microfractures, which were not grossly detectable but sufficient to cause bone marrow embolism. Importantly, this howler monkey was also positive for YF virus, with massive necrotizing hepatitis, as the probable cause of death. Thrombotic pulmonary embolism or NTPE is not reported as a characteristic lesion in YF-infected NWP,4,7,24 and no correlation between the infection and traumatic lesions was observed.
In our study, there were 444 traumatized marmosets and 10 traumatized howler monkeys. However, pulmonary embolism was observed in only 9 marmosets (2.0%; 9/444) and in 1 howler monkey (10.0%; 1/10), which may suggest that pulmonary embolism is less frequent in traumatized NWP than in traumatized human patients.11,12 One required condition for pulmonary tissue embolism is that the heart must remain functional after the traumatic tissue laceration, allowing the tissue emboli to reach pulmonary vessels. 20 In cases of severe trauma to the brain or liver, the patient may die before pulmonary embolism is established. Therefore, emboli of nervous or hepatic tissues are more rarely observed. In contrast, trauma that leads to bone marrow injury is less likely to be lethal, and therefore embolism of marrow to pulmonary vessels is more frequently observed.
This study reports cases of NTPE composed of liver, brain, or bone marrow tissue in free-ranging NWP that were associated with traumatic lesions, often anthropogenic, occurring during a YF outbreak. Although uncommon, it is important to consider NTPE with pulmonary occlusion in the critical care of traumatized NWP. In addition, this study highlights the importance of conservational strategies and environmental education focusing on One Health, not only to protect free-ranging NWP populations but also to maintain the efficiency of epidemiological surveillance programs.
Supplemental Material
sj-pdf-1-vet-10.1177_03009858221075595 – Supplemental material for Non-thrombotic pulmonary embolism of brain, liver, or bone marrow tissues associated with traumatic injuries in free-ranging neotropical primates
Supplemental material, sj-pdf-1-vet-10.1177_03009858221075595 for Non-thrombotic pulmonary embolism of brain, liver, or bone marrow tissues associated with traumatic injuries in free-ranging neotropical primates by Ayisa Rodrigues Oliveira, Daniel Oliveira dos Santos, Fabiana Pizzolato de Lucena, Sara Aquino de Mattos, Thaynara Parente de Carvalho, Fabíola Barroso Costa, Larissa Giannini Alves Moreira, Izabela Magalhães Arthuso Vasconcelos, Tatiane Alves da Paixão and Renato Lima Santos1 in Veterinary Pathology
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Work in RLS lab is supported by CNPq (Conselho Nacional de Desenvolvimento Científico e Tecnológico, Brazil), FAPEMIG (Fundação de Amparo à Pesquisa do Estado de Minas Gerais, Brazil), and CAPES (Coordenação de Aperfeiçoamento de Pessoal de Nível Superior, Brazil). T.A.P. and R.L.S. have fellowships from CNPq (Brazil).
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
