Abstract
Veterinary pathologists working in diagnostic laboratories are sometimes presented with cases involving animal poisonings that become the object of criminal or civil litigation. Forensic veterinary toxicology cases can include cases involving animal cruelty (malicious poisoning), regulatory issues (eg, contamination of the food supply), insurance litigation, or poisoning of wildlife. An understanding of the appropriate approach to these types of cases, including proper sample collection, handling, and transport, is essential so that chain of custody rules are followed and proper samples are obtained for toxicological analysis. Consultation with veterinary toxicologists at the diagnostic laboratory that will be processing the samples before, during, and after the forensic necropsy can help to ensure that the analytical tests performed are appropriate for the circumstances and findings surrounding the individual case.
While the overall incidence of animal poisoning is not known, reports from animal and human poison control centers indicate that exposure of animals to potentially toxic agents is not an uncommon occurrence. 16 Of reported poisoning cases, the vast majority (>99%) are accidental exposures, with less than 1% reported to be intentional. Intentional poisonings include those in which a potentially toxic agent was administered to an animal without intent of causing harm (eg, administration of acetaminophen to a cat in an unwitting attempt to relieve pain), and those cases where the toxic agent was intended to cause harm to an animal (malicious poisoning). Malicious poisonings account for less than 0.5% of all poisoning cases reported to animal poison control centers. However, due to the clandestine habits of many animal poisoners and the potential for a malicious poisoning to be mistaken for accidental exposure or natural disease, the actual incidence of malicious poisonings is likely higher than what is reported. Dogs are the most common species involved in malicious poisonings, composing ∼75% of reported cases (with the majority of these being medium to large-sized dogs), while cats account for ∼15%, with the remaining 10% including cases of equine, food animal, exotic, and wildlife poisonings. 16
While there may be fewer incidents of poisonings involving livestock, individual livestock poisoning incidents have the potential to affect large numbers of animals, such as intensive housing operations or stockyard systems that can put tens, hundreds, or thousands of individual animals at risk when a malicious poisoning occurs. Similarly, malicious wildlife poisonings frequently result in multiple animal deaths due either to targeting of large groups of animals (eg, migratory birds) or to placement of poisoned bait that attracts and poisons not only the targeted species but also nontarget species. Media attention to the deaths of large numbers of animals (wild or domestic) may result in intense pressure by the public for action to be taken. Because of the potential financial and/or political ramifications of these types of large-scale poisoning incidents, they are oftentimes more likely to be actively investigated than incidents involving individual animals.
Forensic toxicology is defined as the application of toxicology for the purposes of the law. 20 The veterinary pathologist working in a diagnostic environment will inevitably be presented with forensic animal poisoning cases. In the United States, intentional poisoning of animals is considered animal cruelty under most jurisdictions and may be prosecuted as such. Intentional poisoning of food-producing animals that threatens public health through contamination or adulteration of the human food supply may be criminally prosecuted under chemical terrorism statutes. 27 However, prosecution of criminal cases involving animal poisonings is relatively uncommon, and most animal poisonings are adjudicated through the civil court system, with 1 party seeking damages from a second party whom they hold responsible for the poisoning. Such cases may involve an animal owner seeking restitution for veterinary fees or loss of animal use or life. Insurance investigations may be contested in civil court over losses from animal deaths, loss of use or production, adulteration of feedstuffs resulting in inability to market animal products in the food supply chain (eg, having to dump milk due to drug residues exceeding regulatory tolerances), or through adulteration or contamination of pet foods resulting in widespread illness and/or death of pets (eg, the 2007 melamine-cyanuric acid adulteration of wheat gluten used in pet foods). In general, animal poisoning cases that are elevated to the status of legal cases are not common, but these cases demand thorough and detailed investigation to fulfill the evidentiary requirements of the legal system.
Forensic Toxicology
Human forensic toxicology is structured into 3 subfields: postmortem forensic toxicology, performance toxicology, and forensic drug testing. Postmortem toxicology is designed to aid in the determination of the cause and manner of death through identification of substances within the body. Performance toxicology focuses on the identification and interpretation of the presence of substances that may impair or enhance an individual’s ability to perform a task (eg, alcohol and driving). Forensic drug testing entails screening of body tissue or fluids from individuals to determine the presence or absence of illicit substances, for instance workplace drug testing or court-ordered drug testing for parolees. The discipline of human forensic toxicology is large enough that human toxicologists are able to specialize in 1 or more of these fields.
In contrast to human forensic toxicology, the field of veterinary forensic toxicology is less well-defined, with most veterinary toxicologists performing a range of duties that may or may not include the occasional forensic case. Historically, the major focus of veterinary toxicology as it applies to law has been in dealing with the regulatory aspects of residues in food-producing animals or contaminants in animal feeds. Interestingly, in the United States, the field of veterinary forensic toxicology as it applies to criminal law is probably most advanced in the field of wildlife forensic toxicology, as the US Fish and Wildlife Service Forensics Laboratory in Ashland, Oregon, has been involved in investigating criminal wildlife cases, including poisoning cases, since its inception in 1989. 39 With the exception of regulatory and wildlife toxicology cases, veterinary forensic toxicology investigations are not commonly performed, and their relative infrequency when compared to human forensic toxicology may be due to factors unique to veterinary medicine. Suspicious human deaths are automatically investigated by local or state authorities, with the cost of the investigation borne by governmental agencies. While in some animal neglect or cruelty cases animal humane societies or law enforcement may intervene and provide funding or other resources (eg, necropsy service), in most cases suspicious animal deaths are investigated only if the animal owner is willing to cover the costs of the investigation. The cost of a forensic toxicology investigation, including necropsy (if the patient is deceased), hospitalization and clinical laboratory workup (if the patient is alive), field or site investigation, sample collection and shipping, and toxicological analysis, is often beyond the ability or willingness of an animal owner to pay. Physicians are mandated to report suspected poisonings, but there is no such mandate in veterinary medicine, although in some states veterinarians are mandated to report animal cruelty under which poisoning may fall depending on statute. The lack of mandated reporting and further lack of a centralized reporting structure that could aid in identifying poisoning clusters within a region further limit the effective identification and prosecution of malicious animal poisonings. Fortunately, in recent years law enforcement and mental health authorities have become more cognizant of the association between animal abuse and violence against humans. Associated with the increased acknowledgement of this association, more meaningful anticruelty laws have been legislated, and there appears to be an increased willingness to investigate and prosecute cases of animal cruelty, including animal poisonings. 1,24
Clinical signs caused by many poisons can mimic those caused by natural diseases, making definitive diagnosis based on clinical signs alone difficult, if not impossible. Some toxicants commonly used in malicious animal poisonings cause characteristic gross and/or histopathological lesions that can aid in diagnosis. For instance cantharidin from blister beetles produces intense reddening of the gastrointestinal and urinary mucosa, bromethalin produces characteristic spongiosis in the central nervous system, and ethylene glycol causes the deposition of calcium oxalate crystals associated with renal tubular degeneration and necrosis. However, most toxicants leave few gross or histologic lesions that point to only 1 potential cause, and even in cases where consistent pathological findings suggest a particular toxicant, further investigation may be required to establish a diagnosis that will stand up to the rigors of the legal arena. The ideal situation in a veterinary forensic toxicology case is one where (1) the clinical syndrome, including historical information, clinical signs, and response to antidotal or appropriate therapy, are consistent with the suspected toxicant; (2) pathological and/or clinical pathological findings are consistent with the suspected toxicant; and (3) results of analytical testing confirm the presence of the suspected toxicant in the tissues of the patient at a level consistent with poisoning. Obtaining this perfect trifecta of facts requires coordination between animal caretakers, veterinarians, veterinary pathologists, and veterinary toxicologists.
Anamnesis
Historical information is an important component of investigating any case of animal illness or death. Because most intentional animal poisonings are not witnessed other than, perhaps, by the actual poisoner, the exact circumstances surrounding the poisoning may not be known. However, even in these cases, careful and thoughtful questioning of animal caretakers may reveal some clues as to potential sources of poisonings. For the veterinary pathologist, there is often the expectation that these questions would have been dealt with by the primary care veterinarian in the case, but that is unfortunately not always the case, and it is especially disheartening to open a case file and see that the referring veterinarian has provided “found dead, suspect poisoning” as the only historical information. The good news is that in most veterinary forensic cases, by the time the victim presents to the veterinary pathologist, many essential questions have already been answered via interviews with the referring veterinarian and/or law enforcement—it’s sometimes just a matter of getting the involved parties to share that information! Having a list of appropriate questions to ask or send to the referring veterinarian can help pave the way to more efficient communication. A thorough forensic toxicology history will include information about the suspected exposure, the patient’s environment, and the patient.
The Exposure
Any information regarding exposure to the suspected toxicant should be obtained. Was there a witnessed exposure? If so, can the toxicant be identified? If not, a description of its physical features such as size, shape, color, and so on should be obtained. Where did the exposure occur? How long after exposure did signs begin?
The Environment
For agricultural or large scale animal environments (eg, zoos, animal shelters, etc), standard husbandry procedures including sources of feeds, water, medications, supplements, bedding, pasture quality, sanitation, and so on should be reviewed. Arrivals of new animals, shipments of feed, supplements, medications and the proximity of these arrivals to the onset of signs should be documented. Movement of people within the environment should be documented, including presence of authorized and unauthorized personnel, delivery persons, and others who may have had contact with the affected animals. A list of recently discharged personnel or people who may have a grudge against the establishment should be developed. Any recent machinery failures, especially those that impact feed or water delivery to animals should be documented. In some cases, large-scale suspected poisoning incidents will have had a field investigation performed by the referring veterinarian with thorough documentation using both written and imaging media (ie, photography, videography). In other cases, the veterinary pathologist may be requested to participate in a field investigation from the outset of the case. For wildlife field investigations, close work with wildlife officials is important due to the legalities entailed with handling wildlife; this is especially true for investigations related to protected species. Ideally, consultation with or participation of a veterinary toxicologist should be sought prior to the field investigation to obtain any suggestions on potential toxicants to search for or any special sample collection or handling procedures to follow. Field investigations should include interviews with on-site personnel, evaluation of both affected and unaffected animals, and a walk-through of animal housing areas, pastures, feed preparation areas, and water sources to identify potential sites of exposure as well as to rule out the presence of other potential causes of toxicosis (eg, toxic plants in pasture). Detailed information on performing field investigations for suspected animal poisoning cases has been previously published. 14,15
The environment of the affected animals will dictate the type of toxicants to which they may be exposed. Animals with access to indoor areas may be exposed to household products such as pet foods and treats, medications (human and veterinary), flea and tick control products, human foods, illicit drugs, garbage can contents, cleaning products, health and beauty aids, alkaline batteries, nicotine, houseplants, rodenticides, insecticides, and so on. Animals with access to outdoors may be confined or roaming. For confined animals, a listing of landscaping plants, lawn care products, compost piles, pool products, ice melts, antifreezes, grill products, mushrooms in the yard, rodenticides, insecticides, and so on can be compiled. The animal’s outdoor environment should be checked for the presence of unexplained food products, empty containers, foreign materials (granules, pellets, etc), open gates or doors to storage areas, changes in color or consistency of food, adulterated water. For roaming animals, the number of potential toxicants expands tremendously. Animals that roam in rural areas may be exposed to medicated feeds or growth promotants for livestock, various pesticides, roadkill, and buried euthanized animals, whereas suburban pets may be more at risk for exposure to outdoor pesticides.
The Patient
Pertinent questions to ask about the patient include basic signalment (species, breed, age, reproductive status), and pertinent health history (eg, vaccination status, prior health, current medications including supplements, husbandry practices, etc). For cases involving multiple animals, the number of animals at risk, number of animals affected, and number of deaths should be determined—note that as the case progresses these numbers may change and these changes should be documented. Information should be obtained on the time of onset of clinical signs (or when the patient was last noted to be normal), gradual or sudden onset of signs, duration of signs, types of signs (including any that resolved prior to presentation or death), and severity of signs. If the onset of signs is not known, when was the last time the patient was seen to be normal (ie, eating, drinking and acting normally)? Full documentation of treatments administered by the caretaker or veterinarian, and the response (or lack thereof) to administered treatments should be made. Any injections of medications should be documented and compared against injection sites found on the patient at necropsy. The results of any clinical pathology laboratory testing, diagnostic imaging, feed and/or water analysis, or any other ancillary testing should be provided as available.
A Brief Primer of Toxicology
To be comfortable with managing forensic toxicology, the veterinary pathologist should be familiar with some basic principles of veterinary toxicology. As with any discipline, veterinary toxicology has its own vocabulary. “Toxicology” is the study of the adverse effects of chemicals on the body. 11 “Poison” is a compound that can cause deleterious effects on a biological system. A “toxin” is a poison of biologic (plant, animal, microbial) origin, while a “toxicant” refers to any toxic agent, although some use toxicant to refer to compounds only of anthropogenic origin. “Xenobiotic” is any compound that is foreign to the body, but it is often used when describing compounds of medicinal purpose such as pharmaceuticals, herbs, and so on. “Toxicity” refers to the relative potency or amount of toxicant required to cause an adverse effect, whereas “toxicosis” and “toxidrome” are terms that encompass the clinical syndrome caused by exposure to a toxic agent. The disciplines of toxicology and pharmacology are both centered on the concept of dose response, that is, that for a given dose, a predictable effect will be seen. The paraphrased statement of Paracelsus, “The dose makes the poison,” is an essential concept for those dealing with toxicology cases, especially with our modern analytical equipment capable of detecting compounds at minutely small concentrations. 18 Even the most toxic compound known will not cause an adverse effect if exposure to a toxic dose does not occur. The dose-response concept enables distinction between toxic reactions and idiosyncratic reactions (unpredictable and excessive sensitivity or resistance to a compound) and allergic reactions (require prior sensitization, response may not be dose-dependent), both of which can clinically be mistaken for toxic reactions. 11
“Toxicokinetics” describes the movement of a toxicant into, around, and out of the body, encompassing the 4 stages: absorption, distribution, metabolism, and elimination. 7,11 Absorption encompasses the entry of the toxicant into the body, including site of exposure, route of entry, and mechanism of transport across biological barriers. The alimentary tract (ingestion) is the most common route of entry of toxicants, followed by lungs (inhalation) and skin (topical), with ocular, intramammary, and parenteral injection being less common routes of exposure. 19 Toxicants may pass through biological barriers by passive (eg, diffusion) or active (eg, active transport) mechanisms, and the relative amount of toxicants being absorbed will vary depending on their chemical and physical characteristics (eg, ionization, size, etc). Some toxicants, such as corrosives, may have minimal systemic absorption, but act locally to cause tissue injury. Once absorbed into the systemic circulation, toxicants are distributed to various body compartments based again on their physical and chemical characteristics. Some toxicants have low distribution and tend to stay in the plasma from where they are ultimately eliminated. Other toxicants widely distribute to various tissues with some toxicants demonstrating predilection for particular tissues (eg, the herbicide paraquat concentrates in the lungs). Although all tissues have some metabolic capacity, the primary sites of toxicant metabolism are liver and kidney with metabolites being eliminated in the urine and/or feces.
Considering the toxicokinetic properties of a known toxicant, then, one can deduce the best samples for analysis to take at a given time postexposure. For instance, in cases where the time frame from exposure to clinical syndrome was very short (eg, minutes to a few hours), the site of entry might contain relatively high concentrations of toxicant. As the toxicant is absorbed, blood concentrations increase, making blood a valuable sample for toxicological analysis. For toxicants that extensively distribute to specific tissues (eg, bromethalin distributes to body fat), blood concentrations may quickly fall below the level of detection, while measurable toxicant concentrations may remain in the target tissues for a much longer period of time. As biotransformation and elimination of parent compound and/or metabolites occurs, the toxicant may be detectable in elimination products (eg, urine, feces) for hours to weeks following the initial exposure, depending on the terminal half-life of that toxicant.
While toxicokinetics defines the movement of xenobiotics within a body during life, postmortem redistribution of xenobiotics (PMR) describes the changes in blood xenobiotics after death. 32 To date studied almost exclusively in human forensic medicine, PMR is the result of diffusion of compounds from antemortem “reservoirs” following death and can result in variable postmortem blood concentrations of xenobiotics. Diffusion of unabsorbed xenobiotics from the gastrointestinal tract to mediastinal vessels and cardiac tissue results in drug concentrations in heart blood that exceed the antemortem systemic blood concentrations. Stomach or rumen contents containing unabsorbed xenobiotics that are regurgitated and actively inhaled during the perimortem (agonal) stage or that are displaced through postmortem handling of the body may result in contamination of airways and lungs, with subsequent diffusion of xenobiotics from gastric or rumen contents into cardiac blood. In addition, the lungs may themselves act as reservoirs for xenobiotics that selectively distribute to pulmonary tissue (eg, macrolide antibiotics). Similarly xenobiotics sequestered in the liver may redistribute via hepatic veins or vena cava into the cardiac blood. Drugs such as digoxin and morphine concentrate in the myocardium in the live animal, and postmortem diffusion into cardiac blood can result in spuriously high concentrations. 32 Some lipophilic compounds may diffuse from the blood into body fat stores, resulting in decreased postmortem blood concentrations. Other factors contributing to PMR are loss of physiological and anatomical barriers due to cell death, blood coagulation and hypostasis, and postmortem putrefaction processes such as microbial production of ethanol and degradation of cyanide. 21 In human forensic toxicology PMR is of concern due to the need to distinguish between normal therapeutic concentrations of drugs and potentially toxic or lethal concentrations of drugs in the blood. In humans, the femoral vein is considered to be the least subject to PMR and is considered the site of choice for blood sampling, although algorithms exist that compare measurements from right and left cardiac chambers to estimate the extent of PMR. Whether the anatomical differences between humans and quadrupeds impacts PMR is not known. In veterinary medicine, quantitation of drug concentrations is usually not necessary since it is often the mere detection of an unexpected xenobiotic that is significant. However, PMR is an important phenomenon to understand in those cases where postmortem blood concentrations may be used as evidence.
Forensic Toxicology Specimen Collection, Handling, and Storage
Knowing the toxicokinetics characteristics of a particular toxicant can be helpful in determining which samples are likely to yield the most rewarding results in cases of animal poisoning. However, oftentimes the toxicant is not known or toxicosis may not be suspected at the time of the forensic necropsy, so a systematic approach to collection of samples must be undertaken by the veterinary pathologist to ensure adequate samples are available for toxicological analysis. In forensic toxicology cases, the proper collection, storage, handling, and analysis of samples are essential to providing admissible evidence needed to successfully adjudicate the case. 27 Prior to the forensic necropsy, consultation with a veterinary toxicologist at the diagnostic laboratory that will perform the analyses can aid the veterinary pathologist in formulating a list of samples to be collected. As with the forensic necropsy, it is often helpful to develop a forensic toxicology checklist of necessary samples to be collected in the case so that items are not overlooked.
Sample Containers
Specimens for toxicology can be collected at the same time that histopathological samples are being taken; appropriate sample sizes for toxicology are included in Table 1. Each sample container should be marked with the patient’s name, case number, date and time of collection, type of sample (eg, tissue, fluid type, and collection site when applicable; eg, heart blood) and a chain of custody log should be initiated for each collection of samples destined for a different department or laboratory (eg, histopathology, toxicology). 7 Each tissue sample should have its own container and the collector should work with 1 organ or tissue at a time to avoid cross-contamination of samples; knives and other sectioning equipment should be cleaned between tissues. Collection of duplicate samples is frequently recommended in case original samples are lost or damaged during shipping or opposing counsel requests their own samples to analyze. 17,24 Having a “clean” assistant available to prelabel containers and assist with sample collection (eg, opening, sealing containers) can aid in minimizing cross-contamination and expediting routing of samples to the appropriate destinations.
Sample Collection For Toxicology.
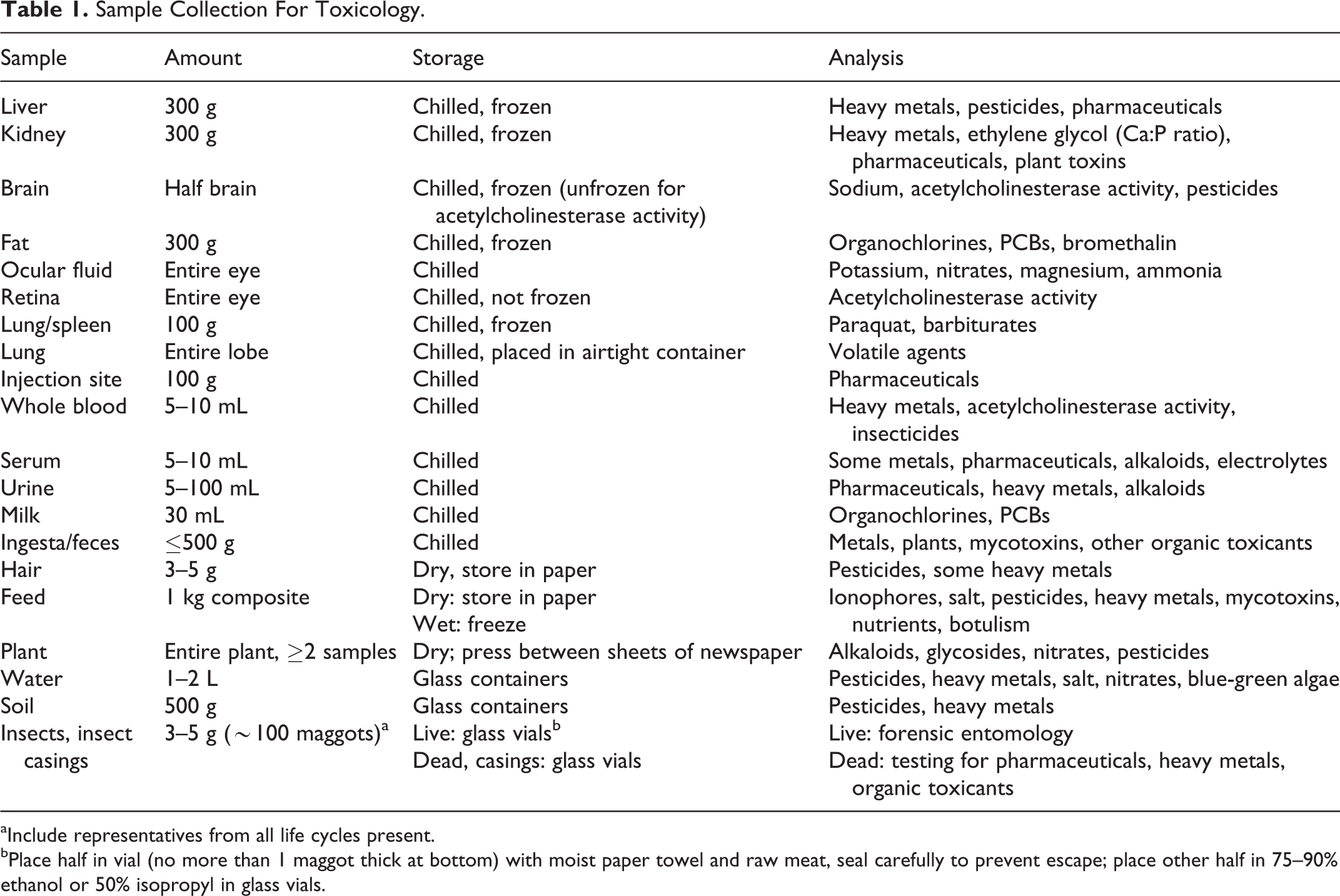
aInclude representatives from all life cycles present.
bPlace half in vial (no more than 1 maggot thick at bottom) with moist paper towel and raw meat, seal carefully to prevent escape; place other half in 75–90% ethanol or 50% isopropyl in glass vials.
As soft plastics may leach contaminants into samples, most samples should be placed in glass or hard plastic (polypropylene, polystyrene) containers with screw caps.
7,26
If samples are to be frozen, polystyrene containers should be avoided as they have a tendency to crack upon freezing. If glass or hard plastic containers are not readily available, samples may be wrapped in aluminum foil and placed in soft plastic sample bags (eg, Whirl-Pak® bags) with the caveat that the foil may interfere with some analyses (eg, fluoride). Samples that may contain volatile compounds should be placed in air-tight containers such as unused paint cans or glass vials or bottles with Teflon or metal-foil-lined lids; plastic containers should be avoided because some volatile agents will degrade plastic and unwanted leachates may contaminate the sample, complicating interpretation of analytical results. Biological fluids or other liquids may be collected via pipettes or disposable hypodermic syringe and needle, then transferred to a labeled, capped container; spillage on the outside of the container should be rinsed and decontaminated with 10% bleach solution after the container is capped. Fluid samples should
Sample Collection
During the forensic necropsy in a suspected poisoning case, all visible abnormalities should be documented verbally (audio recording or written record) and photographed, videoed, and/or sketched as appropriate. Standard forensic necropsy procedure should be followed and samples collected for histopathology, microbiology or other testing as deemed fit. The external condition of the patient should be recorded in regards to rigor mortis, livor mortis, insect activity, body temperature, and degree of decomposition. The veterinary pathologist should be alert to any abnormal odors that may be on or around the body. Odors such as rotten fish or rotten garlic may indicate the presence of phosphine gas (from ingestion of zinc or aluminum phosphide rodenticide), and almond-like odors may suggest that cyanide gas is present; inhalation of either of these gases poses significant health risks to nearby personnel. 5,20 Both of these compounds have been used to maliciously poison animals in the past, although cyanide is not as readily available as is zinc phosphide. If either of these odors are detected, appropriate measures should be taken to prevent inhalation of the fumes during the necropsy and minimize risk to other personnel. External examination of the body should include documentation of any foreign material on hair or coat (shave 3 × 3 inch square of hair and save), material around the mouth or anus (collect), injection sites (collect skin and underlying subcutis and muscle), or on or between the paw pads (collect). Collect any foreign material in the mouth or adherent to the teeth. Any loose plant material or insects and their casings should be collected. Examine eyes for lesions (petechiae, etc) and remove 1 eye for vitreous and/or retinal evaluation (for acetylcholinesterase activity in the retina, chill and send to the laboratory immediately). The brain should be removed with 1 hemisphere packaged for toxicological analysis and the remainder for histopathology and/or testing for infectious agents; brain for acetylcholinesterase activity should be chilled (not frozen) and submitted immediately.
Upon opening of body cavities, any excessive fluids should be collected. Gastrointestinal contents should be examined in a way that will minimize the risk of contamination of other viscera. 7 For monogastric animals, the stomach should be ligated proximal to the esophageal sphincter and at the pylorus, then removed. Gastric contents should be collected into a clean container or basin via an incision along the greater curvature and the volume recorded. 26 Any solid or foreign objects should be removed, photographed, and packaged separately, while liquid contents should be mixed thoroughly before being aliquoted into containers for submission for testing. Thorough mixing of gastric contents allows for estimation of the total amount of a xenobiotic, such as a drug, once quantitation of a representative sample is made. 7 Any unusual odors of the gastric contents should be noted. If no gastric contents are present, a portion of the gastric wall should be collected, as residues from some toxicants may be within the range of detection. 7,26 For ruminants, representative samples of the rumen contents should be collected along with any foreign material, and the abomasum should be managed as for stomach contents. Several centimeters of small intestine should be removed and contents collected, as should large intestinal contents and/or feces. In cases with suspected exposure to volatile agents, a sample of lung or lung lobe (the former for very small animals) may be obtained by tightly ligating the trachea or bronchi and resecting the tissue, which should be immediately placed in an airtight container and sealed to minimize loss of any volatile compounds. Multiple sections of liver and kidney should be collected, as these are major metabolic and excretory organs. Samples of subcutaneous or other adipose tissue should be collected for detection of highly lipophilic compounds such as bromethalin and organochlorines.
Blood may be obtained from cardiac or peripheral sites; if insufficient blood is available, samples of spleen may be taken. 7 Urine should be collected from the bladder, and milk should be collected from lactating animals for determination of toxicants that may be preferentially eliminated via the milk (eg, white snakeroot). 3
Toxicology Testing and Interpretation
With the forensic necropsy complete and samples for toxicology collected and labeled, it is time for the veterinary pathologist and veterinary toxicologist to discuss the necropsy findings, historical information, clinical findings, and any available test results to strategize a diagnostic plan for the case. In most cases, the summation of these findings can aid in developing a list of most likely toxicants for which testing would be recommended. Other differential diagnoses including infectious, inflammatory, and metabolic disorders should be considered, and additional testing may need to be performed to rule in or out these alternative diagnoses.
Unlike the forensic toxicology laboratories often depicted on television crime shows, real-life toxicology laboratories do not have a single “toxicology screen” that can analyze for all of the thousands of known toxicants, so individual assays have to be performed, and each test has a cost. Some laboratories offer specific screening tests based on clinical findings. For instance, several veterinary diagnostic laboratories offer convulsant screens that will analyze for toxicants frequently associated with seizures or convulsions including bromethalin, metaldehyde, organophosphate insecticides, carbamates, strychnine, and tremorgenic mycotoxins. However, it is important to realize that this type of screen is not a single test, but a bundle of individual tests. Each analysis performed destroys sample, so randomly running multiple tests without a real plan can exhaust the available samples and financial resources without increasing the likelihood of reaching a diagnosis. Approaching the analysis in a stepwise fashion can minimize expenditure to the client while maximizing the likelihood of a diagnosis, and this is where the services of a veterinary toxicologist will be most valuable.
Modern toxicology laboratory capabilities range from physical inspection to the most advanced chemical analytic techniques. 20 Many veterinary diagnostic laboratories are capable of performing analyses for some of the more common toxicants encountered in veterinary medicine including insecticides, herbicides, metals and rodenticides. However, due to budgetary constraints, many veterinary diagnostic laboratories have had to curtail many of their toxicology capabilities such that only a handful of laboratories offer full or nearly full toxicology services. When particular analyses need to be performed during a forensic toxicology investigation, it is best to work directly with the laboratory and toxicologist that will actually perform the analysis rather than submitting through a laboratory that is going to forward that submission to a different laboratory. This will not only minimize chain of custody issues with the sample passing through too many hands, but also facilitate more efficient communication with the laboratory’s toxicologist when it comes to interpretation of laboratory results. For North America, medicolegal veterinary cases should be directed to veterinary diagnostic laboratories accredited by the American Association of Veterinary Laboratory Diagnosticians (AAVLD), an organization with stringent requirements for competence and technical standards; a list of AAVLD-accredited laboratories can be found at http://www.aavld.org.
Types of Toxicology Analytical Methods
Analytical methods used in toxicology laboratories include visualization, bioassays, chemical reactions, spectroscopy or spectrometry, immunoassays, mass spectrometry, and chromatography.
20
Physical inspection includes visual and olfactory assessments of sample characteristics. Visualization requires nothing more than a sample, a pair of eyes and perhaps a magnifying glass or microscope. Visualization is used to identify toxic plants and mushrooms, toxic algae, and contaminants or adulterants in animal feeds or feces. Visualization requires considerable expertise, especially in the areas of algae identification and feed microscopy. Olfactory clues and evaluation of physical properties of the sample (eg, dissolution in solvents, density determination) are also components of physical inspection. Bioassays utilize living animals to aid in diagnosis of poisoning cases. Bioassays may be as simple as documenting a response to therapy (eg, reversal of muscarinic signs of organophosphate toxicosis upon the administration of antidotal doses of atropine), although for legal purposes this alone would probably be insufficient to satisfy a court of law. Other bioassays include exposing normal animals to the suspect compound and documenting the toxidrome; although this may show that the compound was toxic, the actual identity of the toxicant might still be in question. This type of bioassay is rarely performed anymore with the exception of mouse inoculation to detect the presence of botulinum toxin. Chemical reactions are sometimes used as qualitative tests to indicate the presence of certain compounds. For instance, the use of iron sulfate and a mineral acid will result in the formation of Prussian blue when cyanide is present. Spectroscopy and spectrophotometry use light or ultraviolet light emission or absorption characteristics to detect compounds in liquid samples via characteristic wavelength signatures. Immunoassays utilize antibodies to identify and measure quantities of chemical compounds with a color change indicating the presence or absence of a particular compound. Immunoassays are frequently used in screening tests, such as over-the-counter urine drug test kits or the Toxi-Lab® Drug Identification System used by many human hospital laboratories to screen for the most common compounds associated with human poisonings. Although generally very sensitive, these tests tend to have lower specificity, resulting in false positives due to cross-reaction with other chemicals. For this reason, these tests are most frequently used as screening tests, with positive results requiring confirmation using more specific techniques such as gas chromatography/mass spectrometry (GC/MS) Mass spectrometry (MS) is a technique that superheats (ionizes) a sample then separates the ions according to their mass-to-charge ratios. The resulting mass spectra output gives the mass and relative amounts of the different ions, allowing determination of the chemical formula of the compound (but not the chemical structure). MS is rapid and accurate and is commonly used to detect metals such as lead and zinc as well as combined with chromatography techniques to identify organic molecules. Tandem mass spectrometry (MS/MS) allows for more powerful elucidation of chemical structures. Chromatography is commonly used to detect drugs, pesticides and other organic toxicants. Chromatography separates compounds based on their chemical properties, and the separated compounds are then detected by analysis for chemical properties including UV light absorption, fluorescence, oxidation/reduction, electron transfer and mass weight. High-performance liquid chromatography (HPLC) separates chemicals in liquids, while thin-layer chromatography (TLC) separates compounds in a solid matrix and gas chromatography (GC) separates compounds in a gas matrix. Compared to spectroscopy, chromatography is more labor intensive and time-consuming due to more exacting sample preparation requirements. Detection of a suspicious specimen frequently requires additional analysis (eg, mass spectrometry) to identify and quantify the compound. Gas chromatography followed by mass spectrometry (GC/MS) is considered by many to be the “gold standard” of chemical analysis, although liquid chromatography-mass spectrometry (HPLC/MS) and tandem mass spectrometry (MS/MS) are gaining momentum in the field of analytical toxicology.
Interpretation of Toxicological Results
Just as important as collecting the proper samples for toxicological analysis and performing the appropriate test(s) is accurate interpretation of the results. Analytical equipment and methodology have become so efficient as to allow detection of many compounds at the parts per trillion (ppt) level, which can bring up huge questions when attempting to interpret these findings. In human forensic toxicology, nomograms have been developed for a wide variety of potential toxicants which indicate therapeutic (if a drug), toxic, and lethal concentrations of these compounds in tissues. Unfortunately, in veterinary toxicology access to similar data is generally limited to common toxicants in animals for which most veterinary diagnostic laboratories have established reference ranges (such as heavy metals and minerals, some rodenticides, some plant toxins, and some mycotoxins), and interpretation can be problematic for those toxicants for which reference values have not been developed. Interpretation of results of toxicological analysis is another area where consultation with a veterinary toxicologist can be of benefit.
Toxicants Used in Intentional Animal Poisonings
Agents used to intentionally poison animals can vary considerably from those toxicants associated with accidental animal poisonings. 16 In general, poisoners use what they know is toxic to the animal(s) they are trying to poison. It is not surprising then, that the most commonly reported malicious poisonings in animals involve compounds that are universally known as toxicants, such as rodenticides and insecticides. It takes a fairly sophisticated poisoner to understand that other compounds such as acetaminophen, caffeine, nicotine, and paraquat can be effective animal poisons. Intentional poisonings of companion animals commonly involve household products that are easily acquired such as rodenticides, insecticides, slug/snail killers, ethylene glycol, caffeine, nicotine, and human medications such as acetaminophen. Malicious livestock poisonings may involve agricultural pesticides, rodenticides, and feed additives (especially ionophores), as these products are generally readily accessible on a farm or ranch. Valuable animals may be intentionally poisoned with “natural” toxins, such as blister beetles or yew in an attempt to make the poisoning appear accidental to collect insurance payouts. 14,42 The types of poisons used tend to vary regionally throughout the country, depending on the availability of the toxicants in that particular area. For instance, strychnine is still commonly used as a rodenticide in the northwestern United States, whereas aldicarb is a commonly used insecticide in the Southeast, and patterns of malicious animal poisonings in these regions reflect the availability of these compounds. A full listing of all agents potentially used in intentional animal poisonings could fill an entire textbook. Tables 2, 3, 4, and 5 list major features of some of notable animal poisons, including toxicological effects and major lesions.
Rodenticides Associated With Intentional Animal Poisonings.

Pesticides Associated With Intentional Animal Poisonings.
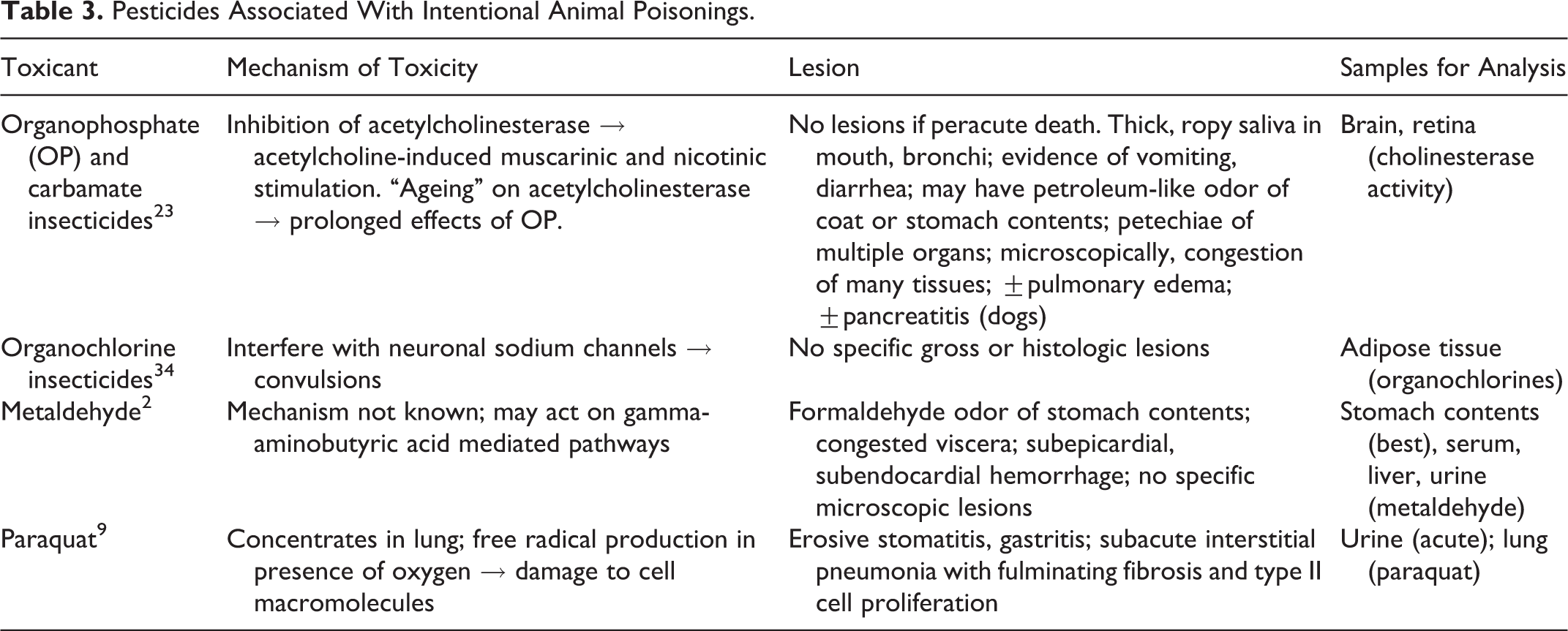
Miscellaneous Toxicants Associated With Intentional Animal Poisonings.

Plants Associated With Intentional Animal Poisonings.
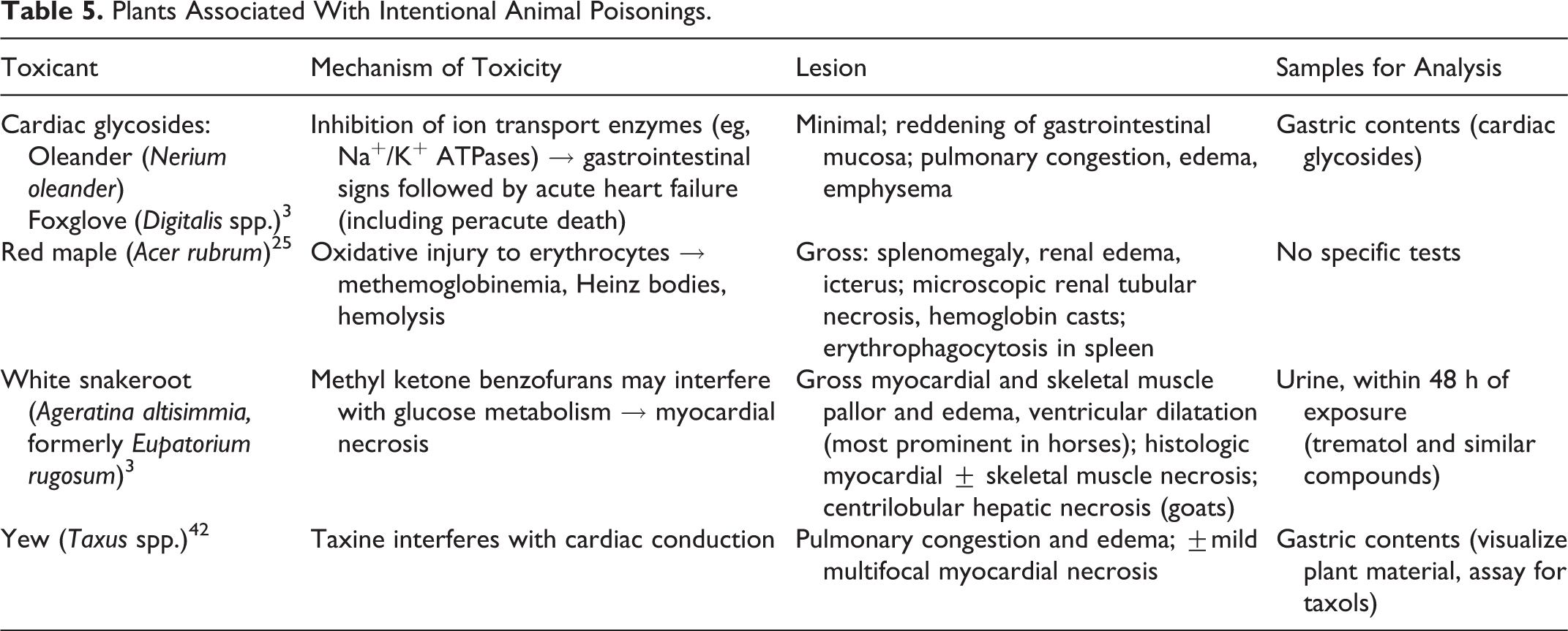
Conclusion
Intentional or accidental poisonings of animals of high financial value or of protected wildlife species have the greatest potential to trigger criminal and/or civil prosecutions of the suspected poisoners. As prosecutions for animal cruelty increase, the frequency of criminal prosecutions for individual cases of malicious animal poisonings will likely also increase. Veterinary pathologists who aid in the forensic investigation of animal poisonings will be expected to be able to identify and collect appropriate samples for toxicological analysis. Open and frequent consultation between animal caretakers, referring veterinarians, veterinary pathologists, and veterinary toxicologists can expedite the investigative process and maximize the likelihood of a diagnosis and, ultimately, successful prosecution of these cases.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
