Abstract
Osteochondrosis is defined as a focal disturbance in endochondral ossification. The cartilage superficial to an osteochondrosis lesion can fracture, giving rise to fragments in joints known as osteochondrosis dissecans (OCD). In pigs and horses, it has been confirmed that the disturbance in ossification is the result of failure of the blood supply to epiphyseal growth cartilage and associated ischemic chondronecrosis. The earliest lesion following vascular failure is an area of ischemic chondronecrosis at an intermediate depth of the growth cartilage (osteochondrosis latens) that is detectable ex vivo, indirectly using contrast-enhanced micro- and conventional computed tomography (CT) or directly using adiabatic T1ρ magnetic resonance imaging. More chronic lesions of ischemic chondronecrosis within the ossification front (osteochondrosis manifesta) are detectable by the same techniques and have also been followed longitudinally in pigs using plain CT. The results confirm that lesions sometimes undergo spontaneous resolution, and in combination, CT and histology observations indicate that this occurs by filling of radiolucent defects with bone from separate centers of endochondral ossification that form superficial to lesions and by phagocytosis and intramembranous ossification of granulation tissue that forms deep to lesions. Research is currently aimed at discovering the cause of the vascular failure in osteochondrosis, and studies of spontaneous lesions suggest that failure is associated with the process of incorporating blood vessels into the advancing ossification front during growth. Experimental studies also show that bacteremia can lead to vascular occlusion. Future challenges are to differentiate between causes of vascular failure and to discover the nature of the heritable predisposition for osteochondrosis.
Keywords
In 2007, a comprehensive review of the pathogenesis of osteochondrosis was published in Veterinary Pathology. 131 The current report is intended to provide an update on research into the pathogenesis of osteochondrosis since then and will focus particularly on the pathogenesis of articular osteochondrosis in pigs and horses.
What Was Known About the Pathogenesis of Osteochondrosis in 2007?
The term osteochondritis dissecans was introduced by König in 1887 to describe a condition that was associated with the formation of fragments in the joints of human patients. The term was later changed to osteochondrosis dissecans (OCD), in recognition of the fact that inflammation was not a characteristic of the primary lesions. 131 In horses, osteochondritis dissecans is still used when OCD and synovitis are diagnosed concurrently. 46 In humans, osteochondritis dissecans is used, and both juvenile and adult onset forms are recognized; the form that is most similar to OCD in animals is the juvenile form. 22,58,67
In an Acta Radiologica supplement published in 1978, it was concluded that OCD was a result of the underlying disease process “osteochondrosis.” 76 Osteochondrosis was characterized by a disturbance in the process of enchondral or endochondral ossification in the 6 animal species in which it had been described: pigs, 97 horses, 100 cattle, 99 dogs, 75 turkeys, 94 and chickens. 95 Endochondral ossification occurs within growth cartilage, which is a temporary tissue that is destined to be replaced by bone. 44 Growth cartilage is found at the metaphyseal growth plate or physis and in the epiphyseal growth cartilage that is found immediately deep to the articular cartilage of immature joints. 2,131 The current report focuses on disturbance at the epiphyseal growth cartilage that is associated with articular, rather than physeal, osteochondrosis. 131 Although there was agreement that osteochondrosis was characterized by a disturbance in endochondral ossification, 76 there was debate over whether it should be considered a focal 34 or generalized disease. 97 Continued research has revealed that lesions occur focally at specific predilection sites but that more than 1 joint is affected simultaneously in more than 50% of cases and that osteochondrosis therefore should be considered a disease that occurs multifocally at predilection sites. 51,68
From 1978 to 2007, research was aimed at discovering the pathogenesis of the focal disturbance in endochondral ossification. Kincaid et al, 52 Woodard et al, 127 and Carlson et al 14 independently discovered areas of necrotic growth cartilage at predilection sites for osteochondrosis in porcine joints. Growth cartilage has a blood supply that runs within cartilage canals that are present for a limited period of time during the early phases of development. 15,121 Areas of chondrocyte necrosis were associated with necrotic cartilage canal blood vessels. 14,52,127 Carlson et al 15 proceeded to experimentally transect vessels and compare surgically induced and spontaneous lesions in the femoral condyles of pigs. This and a subsequent (2004) experimental study 130 confirmed that osteochondrosis in pigs was a consequence of vascular failure and resultant ischemic chondronecrosis. Because ischemia is defined as deficient blood supply and growth cartilage has a blood supply, whereas articular cartilage does not, the phrase “ischemic chondronecrosis” specifically implies necrosis of growth cartilage. Following vascular transection, the most superficial and deepest layers of the growth cartilage remained viable, presumably due to diffusion from synovial fluid and from intact vessels in the subjacent bone, respectively. 15 The earliest lesion following vascular transection was therefore an area of ischemic chondrocyte necrosis located at intermediate depth of the epiphyseal growth cartilage, referred to as osteochondrosis latens. 130 When the ossification front advanced to surround an area of ischemic chondronecrosis, the area caused a focal disturbance in endochondral ossification and was then referred to as osteochondrosis manifesta. 130
The blood supply regressed by filling of canal lumina with cartilage, a process known as chondrification, and by incorporation of vessels into the advancing ossification front. 133 During incorporation, vessels in the midportion of the canal formed anastomoses with vessels in subchondral bone, and vessels in the distal portion shifted from their original perichondrial arterial source to a subchondral arterial source. 133 The location of the earliest osteochondrosis latens lesions suggested that vascular failure had occurred at the point where cartilage canal vessels were incorporated into the ossification front. 133 At the time, it was hypothesized that vascular failure was the result of microfracture of trabecular bone and associated trauma to vessels at this point. 129,133
In horses, the pathogenesis of osteochondrosis tended to be investigated in older animals and more chronic lesions than in pigs. As a consequence, there was no common understanding regarding the pathogenesis of the disease. The major hypotheses proposed before 2007 can be summarized chronologically as follows: Bridges et al
10
detected below-normal serum copper levels in 7 of 8 foals with osteochondrosis. Hurtig et al
45
subsequently demonstrated reduced collagen crosslinks, catalyzed by the cuproenzyme lysyl oxidase, in the cartilage of copper-deprived foals. The implication was that copper deficiency could lead to inferior collagen quality, biomechanically weak cartilage, and OCD.
45
Pool
93
considered that lesions in the lateral trochlear ridge of the distal femur were compatible with failure of vessels coursing from subchondral bone into growth cartilage due to shear forces acting along the junction between the 2 tissues. Carlson et al
12
later examined predilection sites in the hock and stifle and concluded that osteochondrosis was a result of ischemic chondronecrosis in horses as well as in pigs. Grøndahl et al
32
studied osteochondral fragments in the fetlock joint and suggested that they were representative of aberrant accessory centers of ossification. In 1997, Henson et al
42
and Shingleton et al
104
observed accumulations of small, undifferentiated chondrocytes deep to the ossification front (“retained cartilage cores”) and concluded that osteochondrosis was a result of inappropriate differentiation of chondrocytes, or “dyschondroplasia.” Hypotheses for the cause of the dyschondroplasia included primary nutritional or hormonal imbalances (insulin).
41,42,104
The study by Henson et al
42
included localization of type VI collagen. Collagens were subsequently studied as a group
113
and in terms of individual types, including type II,
61,62,103
type I,
103
and type X.
103
The studies did not result in a unified hypothesis for how disease of a particular type of collagen would lead to osteochondrosis but rather revolved around whether collagen changes were the cause of
62,103,113
or represented compensation for
42,103
inferior quality cartilage that would not withstand biomechanical load, thus resulting in lesions.
Summary
In 2007, it was known that the focal disturbance in endochondral ossification that is characteristic of osteochondrosis was the result of failure of the blood supply to epiphyseal growth cartilage and associated ischemic chondronecrosis in pigs.
There was no common understanding of the pathogenesis of osteochondrosis in horses.
What Is New in Osteochondrosis Research Since 2007?
Morphological Studies
Equine predilection site studies
After 2007, predilection sites for osteochondrosis were examined in the joints of young horses, guided by age windows for the presence of cartilage canal vessels. 12 This included foals submitted for postmortem examination, where parental osteochondrosis status was unknown, up to 5 months old for study of the distal tibia 85 and up to 11 months old for study of the distal femur. 84 It also included 9 Standardbred foals that had been bred from parents with radiographically diagnosed tarsal OCD for the purpose of conducting arterial perfusion studies (see below). These foals were from 0 to 7 weeks old, and examination included the hock, 88 stifle, 86 and fetlock 87 joints of one hindlimb from each foal. Areas of chondrocyte necrosis, centered on necrotic cartilage canal vessels, were observed at the examined cranial distal intermediate ridge of the tibia (Figs. 1–4), 85,88 distal lateral trochlear ridge of the talus and medial malleolus of the tibia predilection sites in the hock, 88 and the lateral trochlear ridge and medial condyle of the distal femur predilection sites in the stifle. 84 This work demonstrated that when sufficiently young horses are examined, the early lesions are highly consistent in appearance between different joints and predilection sites, as well as between horses and pigs. 14,52,127 Osteochondral fragments are frequently diagnosed at multiple sites in the fetlock joint of young horses, 16 but there is disagreement on whether the fragments are representative of osteochondrosis, and the studies that could answer this definitively are lacking. Importantly, an area of ischemic chondronecrosis was observed in 2 abaxial slabs from the plantaro-proximal border of the first phalanx in the 7-week-old purpose-bred Standardbred foal. 87 This corresponds to the location where un-united plantaro-proximal eminence is diagnosed clinically, 16 a lesion that may therefore also be the result of osteochondrosis.
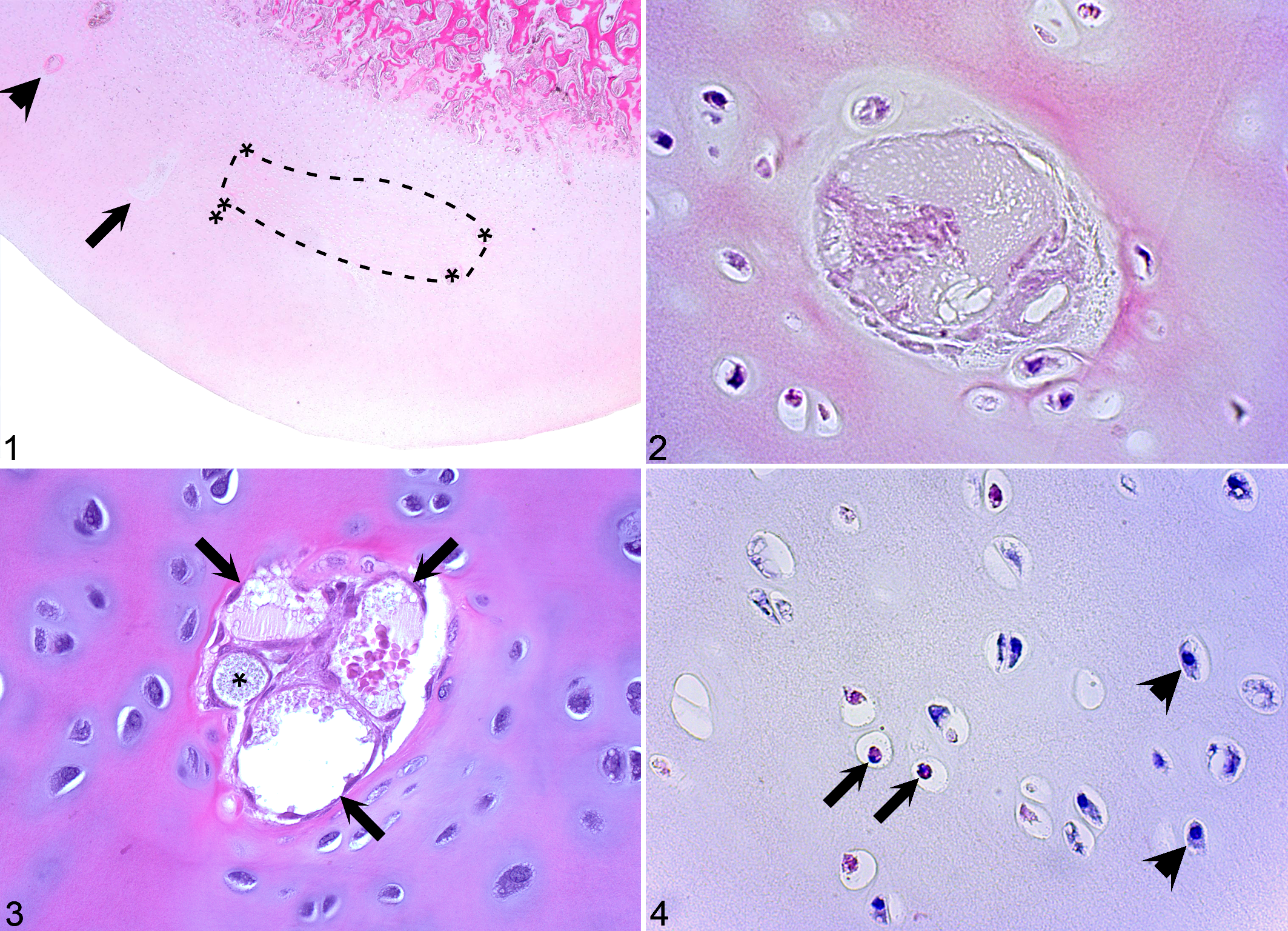
Osteochondrosis latens, distal tibia, cranial intermediate ridge, horse. Proximal is to the top and cranial is to the left of each image.
Equine arterial perfusion studies
The blood supply to the epiphyseal growth cartilage of the hock, 88 stifle, 86 and fetlock joints 87 was examined using an arterial barium perfusion technique adapted from earlier studies in pigs. 132 The studies were carried out in the above-mentioned group of Standardbred foals that had been purpose-bred to allow sampling at regular intervals from 0 to 7 weeks old. 88
The results revealed a minor species variation. Vessels in epiphyseal growth cartilage tended to course either predominantly parallel or perpendicular with respect to the underlying ossification front. 86 The latter configuration was particularly common after vessels had become incorporated into the ossification front, implying that configuration to some extent is related to maturation. Aside from this, it was observed that vessels that coursed parallel with respect to the ossification front across the articular aspect in pigs 132 were located on the abaxial aspect of the femoral condyles in horses. 86
The regression of vessels by chondrification and incorporation into bone, as well as the relative location of the earliest lesions of cartilage canal vessel and chondrocyte necrosis, was, however, identical between horses and pigs, suggesting that failure occurred at the point where vessels were incorporated into the ossification front in horses as well (Figs. 5, 6). 88,133 The blood supply regressed from distal limb joints such as the fetlock 87 and hock 88 at an earlier age than a proximal limb joint such as the stifle, 86 which agreed with previous longitudinal radiographic studies demonstrating that defects develop before the age of 5 months in the fetlock 16 and hock 16,20 and 8 months in the stifle. 20
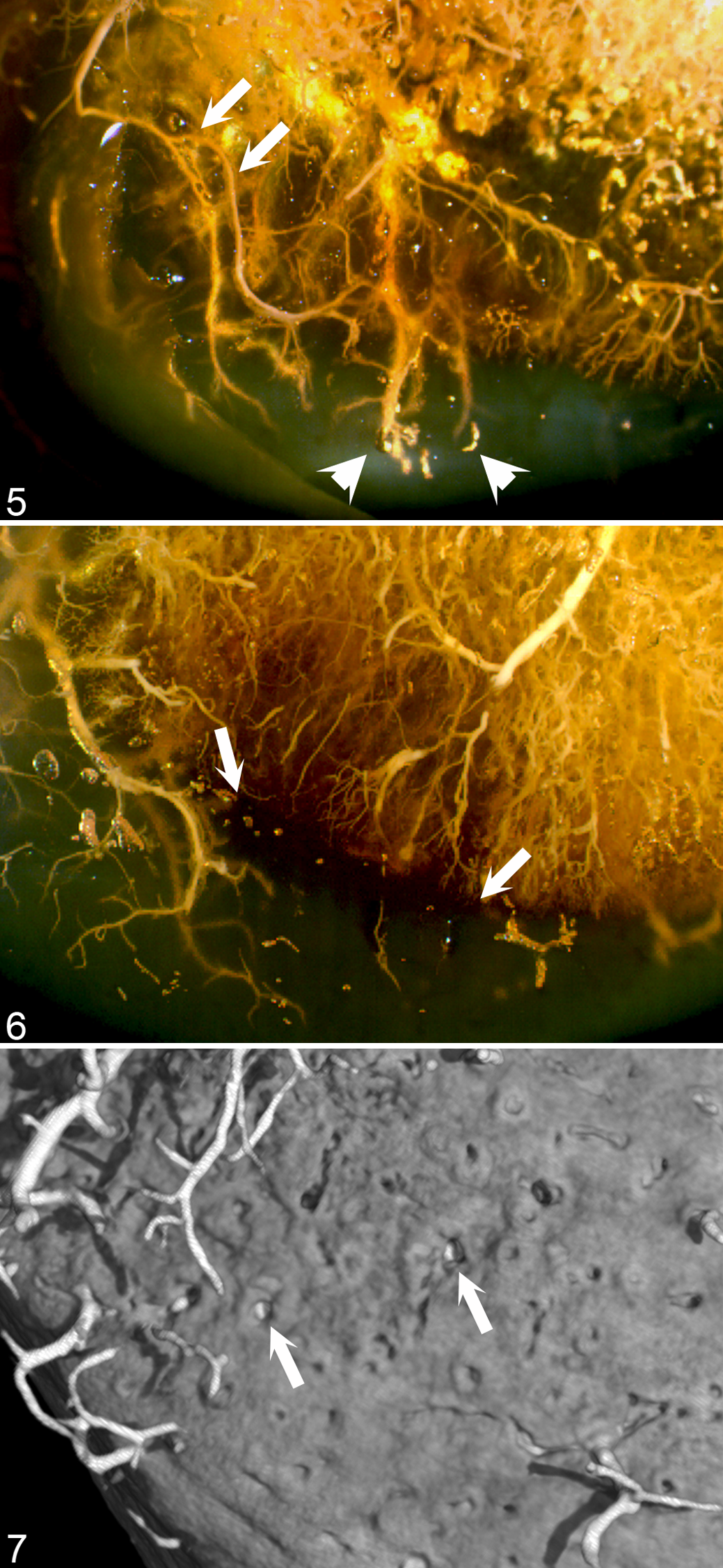
Vascular failure at the ossification front, distal tibia, cranial intermediate ridge, horse. Proximal is to the top and cranial is to the left of each image.
The prevalence of radiographically diagnosed osteochondrosis is high in large horse breeds such as the Dutch Warmblood 115 and Standardbred, 66 and low to negligible in small pony breeds such as the Norwegian Fjord Pony and the pony-sized Icelandic Horse. 9,106 The blood supply to the epiphyseal growth cartilage of the hock and hind fetlock joints was recently compared between the aforementioned purpose-bred Standardbred foals and a group of age-matched Fjord Pony foals. 40 Vessels regressed at the same age in both breeds, but during the age range when vessels were present, the Standardbred foals had more vessels (absolute counts) and thicker growth cartilage (absolute and relative thickness) in all examined regions. The difference was statistically significantly different at the distal lateral trochlear ridge of the talus predilection site (linear regression model; difference in mean number of vessels: 22; P = .003). 40 Accordingly, a greater number of vessels had to be incorporated into bone during the postnatal period in the Standardbred than in the Fjord Pony foals, and this can potentially explain the difference in prevalence between the 2 breeds.
Equine experimentally induced lesions
The prevalence of osteochondrosis is higher in pigs 33,98 than in horses, 66,115 and many of the pigs in which the blood supply was experimentally transected had concurrent spontaneous lesions of ischemic chondronecrosis. 15 In addition, although experimental transection resulted in cartilage canal vessel and chondrocyte necrosis in all operated pigs, 15,130 a focal delay in endochondral ossification was observed only in the single pig examined at the maximum time of 29 days after vessel transection. 130 Experimental transection was therefore repeated in a group of Fjord Pony foals, which were unlikely to have spontaneous lesions. 78 The observation interval was extended to 49 days after vessel transection, and foals were allowed gradually increasing opportunity for exercise once the arthroscopy portal sutures had been removed 7 days postoperatively. 78 As mentioned above, there was a species difference in the location of vessels that were oriented parallel to the ossification front. 86,132 Vascular transection was therefore carried out in the lateral trochlear ridge of the distal femur rather than the medial condyle. 78 In addition to confirming the results from the previous experimental studies in the medial femoral condyle of pigs 15,130 in a second species and site, areas of ischemic chondronecrosis were associated with a focal delay in endochondral ossification in 3 of the 5 foals examined 21 days or more after vessel transection. 78 One foal showed intermittent, grade 1 to 2 lameness on the operated hindlimb beginning 35 days after vessel transection; a dissecting OCD fissure through the area of experimentally induced ischemic chondronecrosis was identified when the foal was sacrificed 1 week later. 78 Thus, the experimental protocol succeeded in reproducing the entire hypothesized sequence of events from vascular failure via ischemic chondronecrosis to delayed ossification and pathological OCD fissure. The study also demonstrated that despite having thinner cartilage than Standardbred foals, 40 it was possible for Fjord Pony foals to develop ischemic chondronecrosis in regions where the cartilage was too thick to survive by diffusion. 15
Equine subchondral bone cysts
Osteochondrosis can progress to OCD, but it can also progress to the formation of a subchondral bone cyst, particularly in central, weightbearing regions of the joints of large animal species such as horses
100,107
and cattle.
50,99
In horses, it has been suggested that an osteochondrosis lesion can give way to infolding of the overlying cartilage when loaded
100,107
or that an OCD fissure can permit influx of pressurized fluid into subchondral bone, with either mechanism resulting in cyst formation.
91,102
The equine predilection site studies
12,84
provided access to material from young horses, and the experimental study
78
provided access to known early lesions. It was therefore possible to examine whether vascular failure could lead to cyst formation, in which case it would clarify the relationship between osteochondrosis and subchondral bone cysts.
83
A true cyst is usually defined as “an abnormal closed cavity in the body, lined by epithelium and containing a liquid or semisolid material.”
1,3
Epithelium is not a component of normal bone, and cysts in bone may therefore have to be defined differently from cysts in other tissues. In the report,
83
a true cyst was defined as a closed cavity with a distinct but not necessarily epithelial lining. Provided that an area of ischemic chondronecrosis could be characterized as “semisolid material,”
1
a pseudocyst was defined the same as a true cyst, with the exception that it was not separated from the surrounding tissue by a distinct lining.
83
The observed changes indicated that cyst formation could occur in 2 different ways: An area of ischemic chondronecrosis could become completely surrounded by bone on all margins, at which point it would be compatible with a diagnosis of “pseudocyst.”
83
A blood vessel within a failed cartilage canal or within lesion-associated granulation tissue could become dilated and then be compatible with a diagnosis of “true cyst.”
83
When early changes were examined in young horses, the results suggested that true cysts might predispose to the development of OCD, rather than vice versa. 83 If the true cyst is present for some time before the OCD/fissure forms, this would explain why many cyst cases present with a history of recent, acute onset lameness and large, chronic lesions. 49,69
Summary
Osteochondrosis was confirmed to be the result of vascular failure and ischemic chondronecrosis in horses.
Diagnostic Imaging Studies
Diagnostic imaging studies were pursued for a number of different reasons, including the fact that it is difficult to be certain of the significance of histological lesions unless they can be related to changes that are detectable clinically. It was also considered likely that combining histological examination with imaging would reveal new information about osteochondrosis and that developing an ability to study the disease by nondestructive techniques would facilitate translation of the results to species where histological examination, particularly of early lesions, is less feasible. The potential for research to improve the welfare of an individual or a population also increases once the results can be applied to diagnosis, treatment, and prevention in live animals.
Ex vivo contrast-enhanced micro–computed tomography of spontaneous lesions in horses
Sample blocks from the cranial distal intermediate ridge of the tibia and distal lateral trochlear ridge of the talus of the aforementioned hereditarily predisposed Standardbred foals were scanned using arterial contrast-enhanced micro–computed tomography (micro-CT). 77 Growth cartilage is radiolucent, and areas of ischemic chondronecrosis within it (osteochondrosis latens) did not alter attenuation but were nevertheless indirectly detectable as contrast-free foci outlined by contrast-filled arterioles on all peripheral margins in 3-dimensional volume-rendered models from the youngest foals with lesions (1 foal aged 1 week old and 2 foals aged 2 weeks old). 77 It was also possible to confirm that interrupted arterial contrast columns terminated at the ossification front (Fig. 7), as previously suspected from examination of histological sections. 88,133 Microfractures were, however, not present at the point where the arterial contrast columns terminated so could not have been the cause of the vascular failure in these foals. 77
The surface of the immature subchondral bone plate was generally irregular in the youngest foals. 77 In the tibia, there were conical indentations or “dimples,” and in the talus, there were circular protrusions or “tubes,” both of which were associated with patent or chondrifying cartilage canals and disappeared in a gradual and regular manner until the subchondral bone plate was relatively smooth in the 7-week-old foal. 77 Because of their generalized distribution and gradual disappearance, dimples and tubes were clearly distinguishable from the focal, uniformly radiolucent defects that corresponded to lesions of ischemic chondronecrosis within the ossification front (osteochondrosis manifesta) in histological sections. 77
Longitudinal radiographic studies 16,20 had documented that a proportion of osteochondrosis lesions undergo spontaneous resolution, but at the time, it was not known how this occurred. Ischemic chondronecrosis is associated with secondary repair responses in growth cartilage that include proliferation of adjacent viable chondrocytes and cartilage canal vessels (Fig. 8). 85,88,130 Chondrocyte proliferation was observed in response to both surgical incisions 80 and ischemic chondronecrosis 78 and is considered a response that is nonspecific with respect to the inciting insult. Vascular proliferation has, however, only been observed adjacent to lesions that include necrosis of vessels and may therefore be specific to ischemic insult. 78,80 Vascular proliferation was first noted in histological sections cut from decalcified tissue. 85,130 The micro-CT was carried out prior to decalcification of the tissue, and in scans, proliferating vessels were surrounded by focal mineral opacity and compatible with formation of separate centers of endochondral ossification (Fig. 9). 77 Secondary repair responses in bone included recruitment of chondroclasts and formation of granulation tissue that contained osteoblasts and was capable of intramembranous ossification. 77 The micro-CT study therefore indicated that spontaneous resolution of radiographically diagnosed osteochondrosis could occur by filling of the defect with bone from separate centers of endochondral ossification that form superficially adjacent to lesions and by phagocytosis of necrotic cartilage and intramembranous ossification of granulation tissue that forms deep to lesions of ischemic chondronecrosis. 77
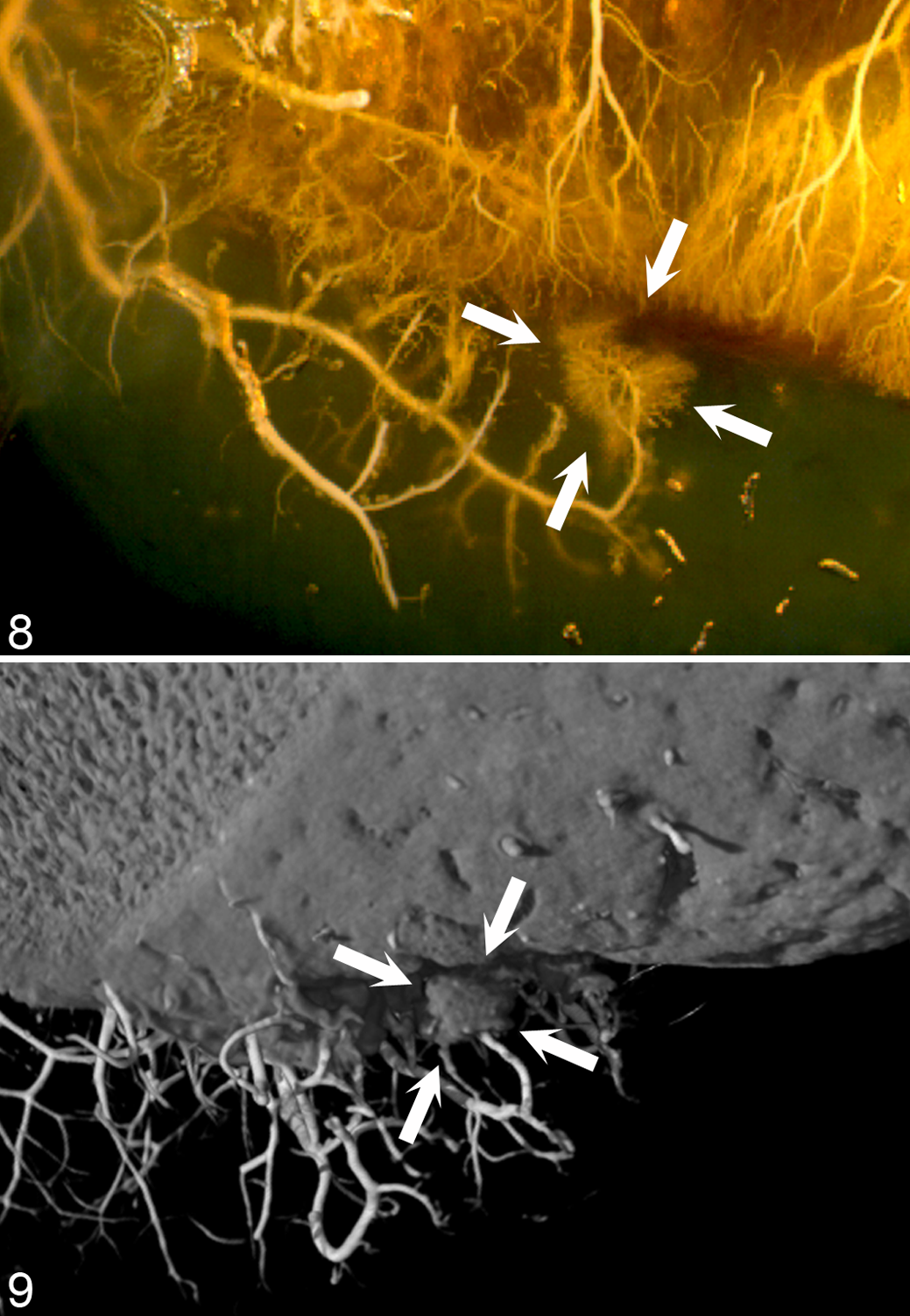
Lesion-adjacent vascular proliferation, distal tibia, cranial intermediate ridge, horse. Proximal is to the top and cranial is to the left of each image.
Ex vivo contrast-enhanced micro-CT and conventional CT of experimental lesions in horses
The equine experimentally induced lesions were examined ex vivo using plain (ie, noncontrast) radiography, arterial contrast-enhanced conventional CT, micro-CT, and histology. 79 Changes that were detectable in micro-CT scans were also detectable in conventional CT scans. 79 This included the fact that arterial contrast columns were observed to terminate abruptly at sites of vessel transection, as opposed to gradually tapering to a point, as was observed in control sites. 79 In plain radiographs, the hinged OCD flap in the foal examined 42 days after vessel transection 78 appeared as a thin body of mineral radiopacity, separated from the remainder of the lateral trochlear ridge by an undulating radiolucent line. 79 With contrast-enhanced CT, it was possible to determine that the mineral opaque body represented separate centers of endochondral ossification that had formed around intact vessels adjacent to the surgically transected vessels. 79
Histological validation of spontaneous lesions in CT scans of pigs
Selection of the boars that provide semen for artificial insemination in commercial pig production is based on extensive testing. In some countries, testing includes automated quantification of lean meat and fat percentage by CT scanning 29,92,101 of live, sedated boars. 55,119 It is therefore feasible to use CT to screen for lesions of osteochondrosis. To be useful in selection, quantification of lean tissue must be carried out at a standardized body weight, 6 usually 120 kg. Screening for osteochondrosis would therefore also be limited to scanning at a standardized body weight.
Computed tomography had been used to scan equine samples containing lesions of osteochondrosis, 77,79 but it was not known whether other disease processes could result in similar radiographic changes. It was therefore necessary to examine the spectrum of CT lesions that occurred in pigs within the weight range that is relevant to boar testing and provide a definitive histological diagnosis for each lesion. Any identified radiographic changes with a high specificity for osteochondrosis could then be identified and provide a basis for CT screening for the disease.
A total of 40 lesions detected by CT were registered and compared with definitive histological diagnoses in sections from the left distal femur of 18 hereditarily osteochondrosis-predisposed, male Landrace pigs from 82 to 180 days old and 33 to 128 kg body weight. 82 Thirty-six of the 40 CT lesions (90%) consisted of focal, uniformly radiolucent defects in the ossification front, and in histological sections, each lesion corresponded to 1 or more areas of ischemic chondronecrosis within the ossification front (osteochondrosis manifesta). 82 The remaining 4 of the 40 CT lesions had different radiographic characteristics and represented disease processes other than osteochondrosis (1 growth plate fracture and 3 mixed radiopacity defects at the origin of the long digital extensor tendon). 82 Focal, uniformly radiolucent defects in the ossification front of growing pigs were therefore highly specific for ischemic chondronecrosis and may be used in CT screening for osteochondrosis. 82
Thirty of the 36 lesions of osteochondrosis (83%) contained multiple, closely adjacent radiolucent defects or “lobes” (Fig. 10). 82 Epiphyseal growth cartilage consists of chondrocytes, extracellular matrix, and cartilage canals. The only component of epiphyseal growth cartilage that matched the distribution of the radiolucent lobes was the cartilage canals. Lesions have previously been observed to comprise multiple adjacent areas of ischemic chondronecrosis in histological sections and have then been referred to as “stair-step” lesions (Fig. 11). 15,84 If the midportion of a cartilage canal becomes incorporated into the ossification front at a point in time when the distal portion still has several branches, vascular failure can lead to necrosis around each branch, resulting in a lesion consisting of multiple adjacent areas of ischemic chondronecrosis (Fig. 12). Thus, in addition to the fact that focal, uniformly radiolucent defects in the ossification front were highly specific for osteochondrosis, multilobulated defects may be pathognomonic for primary disease of the cartilage canals (see “Causes of Vascular Failure,” below) and resultant ischemic chondronecrosis. 82
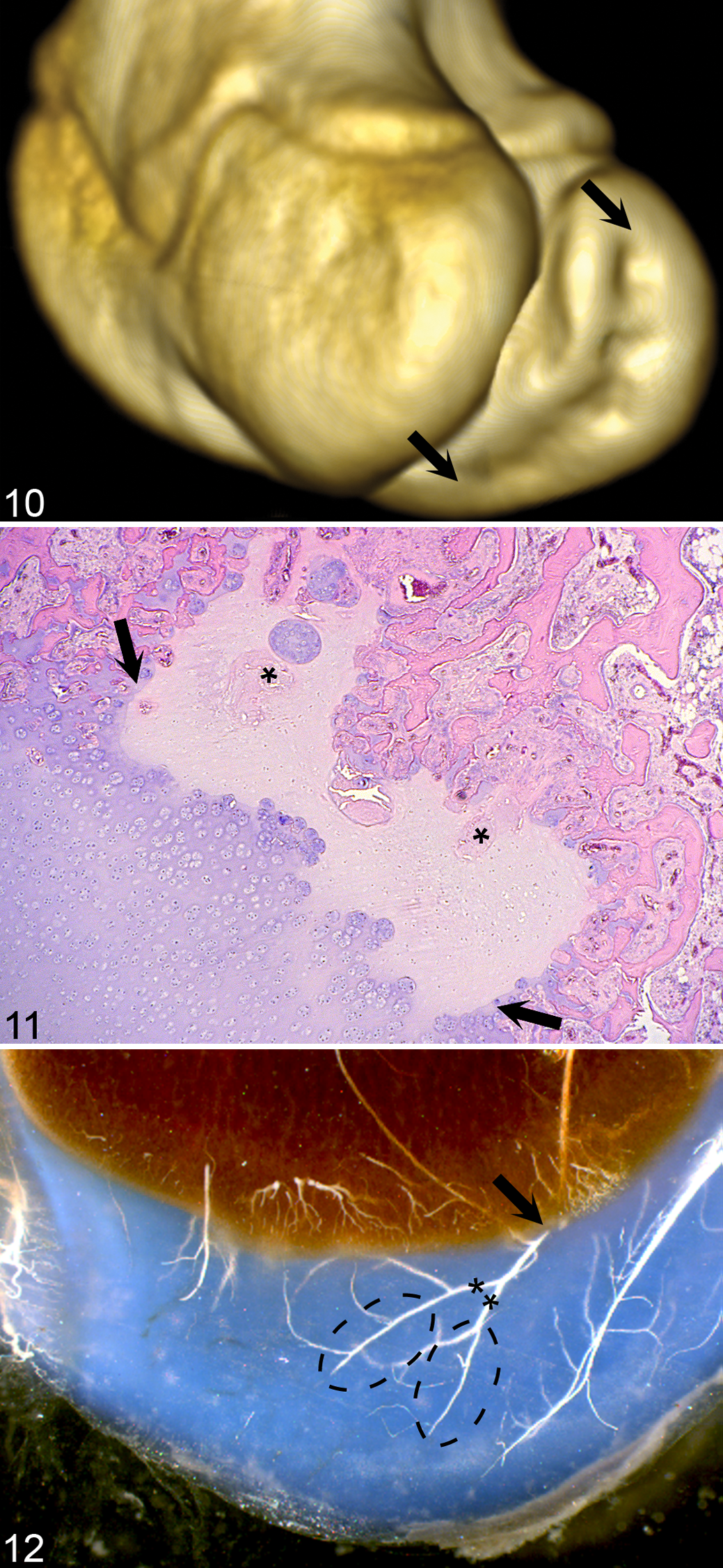
Multilobulated (“stair-step”) lesion, distal femur, medial condyle, pig. Proximal is to the top in all images. Cranial is to the left of Figure 10 and the left side of the animal is to the right side of Figures 11 and 12.
It should be noted that because they do not alter attenuation, the intracartilaginous areas of ischemic chondronecrosis (osteochondrosis latens) that were detectable in the equine arterial contrast-enhanced CT scans 77,79 were not detectable in the plain porcine CT scans. 82 However, all lesions detected in pigs that were ≥159 days old included at least 1 area of ischemic chondronecrosis that was surrounded by the ossification front (osteochondrosis manifesta) and therefore detectable in CT scans. 82
In vivo longitudinal monitoring of spontaneous lesions in pigs by serial CT examination
Horses have been screened radiographically for osteochondrosis, but selection has failed to reduce the prevalence of the disease. 114,115 This is most likely due to a high rate of false-negative diagnosis, which can occur if an animal is screened too early, before lesions have developed, or too late, after lesions have resolved. 16,20 To determine when lesions developed and resolved in 6 joints (the shoulder, elbow, carpus, hip, stifle, and tarsus), 17 of the above-mentioned pigs and 1 additional pig were serially CT-scanned from 2 to 8 times each at biweekly intervals from 70 to 180 days of age and 20 to 128 kg body weight, generating a total of 113 CT scans. 81
Within the hind- and forelimbs, the incidence of focal, uniformly radiolucent defects in the ossification front was highest in the stifle (n = 321) and the elbow (n = 110) joints, respectively. 81 Incidence decreased with increasing age, but the rate of decrease was different for different joints. 81 In each of the examined joints, there were 1 to 2 peaks in the incidence curves (Fig. 13), and these peaks are important because they indicate that several pigs developed ischemic chondronecrosis at the same examination interval, possibly for the same reason. 81 In experimentally induced lesions, there was a lag phase of 29 days from vascular failure to delayed ossification; 130 however, there was no external event that was common to all pigs and occurred 29 days before any incidence peak. 81 The principal alternative explanation was that the peaks reflected an internal event such as the incorporation of vessels into the ossification front (Fig. 14). If incorporation occurred at a similar age in most pigs, it could precipitate failure 88,133 in several pigs at the same time, resulting in peaks in the incidence curves. The incidence curves then potentially further implicate the process of incorporating vessels into the ossification front in the development of vascular failure. 81
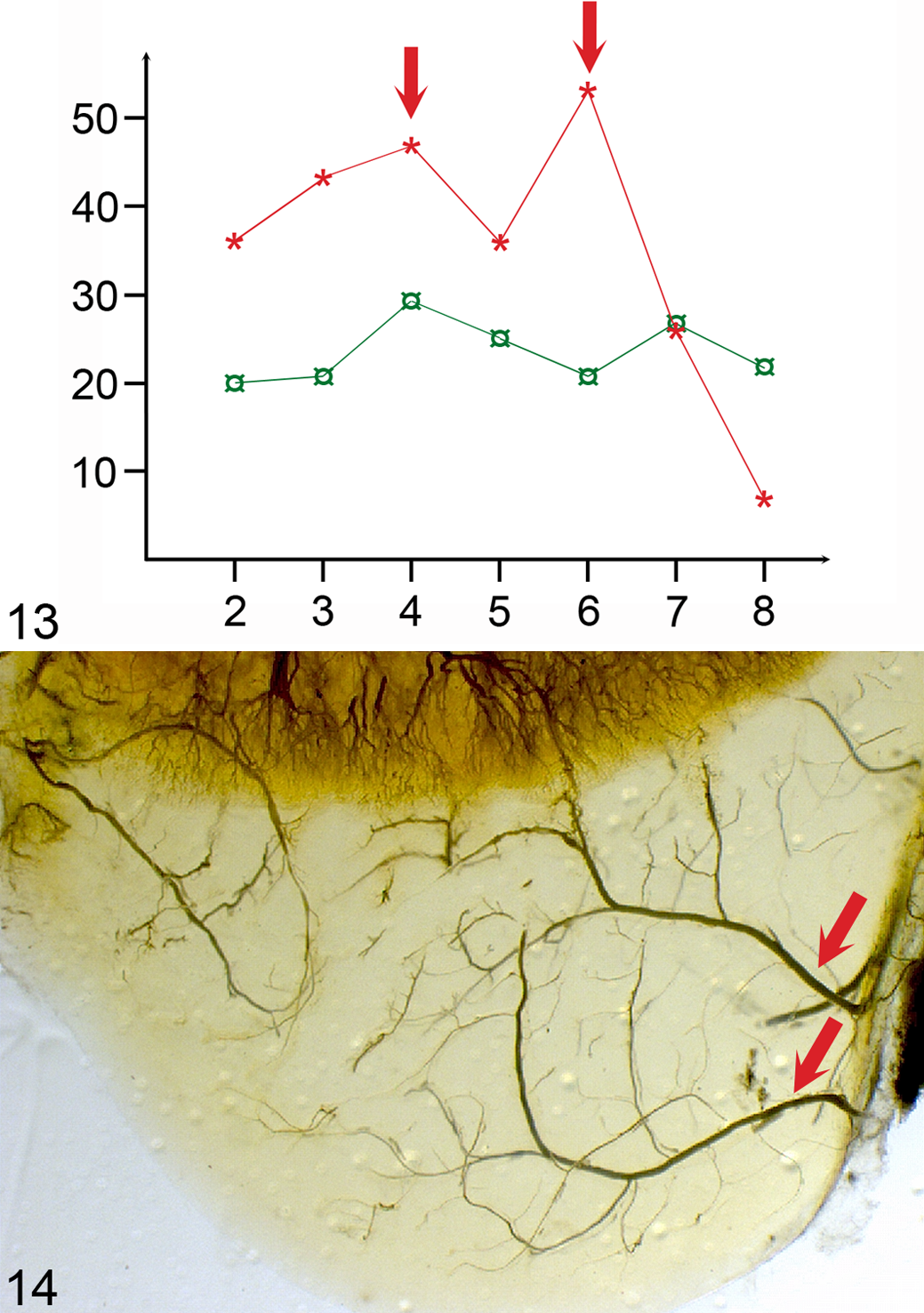
In the stifle and elbow joints, 98% of the defects that developed by the maximum age of 180 days had developed by mean age of 159 days and mean body weight of 98 kg. 81 The error of including pigs that are false negatives because defects had not developed yet in these joints would therefore be ≤2% for CT scanning at 120 kg body weight. 81
The proportion of defects that resolved during the observation interval ranged from 51% in the stifle to 69% in the elbow joint. 81 False-negative diagnosis due to defects resolving can only be eliminated through serial scanning, which is not feasible in practice. Erroneous inclusion of pigs that are false negatives because defects have resolved before scanning may result in selection of pigs that are disposed to healing. Optimally timed CT can therefore be a powerful tool and has already been implemented in screening for osteochondrosis. 4,81
The proportion of defects that resolved was higher in lateral compared with medial sites within the stifle joint, and the difference was statistically significant in the lateral compared with the medial trochlear ridge (P = .02). 81 This corresponds with the fact that the prevalence of histological lesions can be equal between the medial and lateral femoral condyles in young pigs, 15 whereas in older pigs, the prevalence of OCD is higher in the medial than in the lateral condyle. 34,97
Ex vivo contrast-enhanced and plain magnetic resonance image of cartilage canal vessels in pigs
Although ischemic chondronecrosis within the ossification front (osteochondrosis manifesta) could be monitored longitudinally by plain CT, 81 indirect detection of the earlier intracartilaginous osteochondrosis latens lesions relied on the use of a contrast agent. 77,79 An ability to detect osteochondrosis latens directly, without the use of a contrast agent or ionizing radiation, would facilitate comparative study and be particularly important for translation of the results of animal studies to the study of juvenile osteochondritis dissecans in children.
The possibility of detecting ischemic chondronecrosis by magnetic resonance imaging (MRI) was investigated in the distal femur of pigs. 111 Visualization of cartilage canal vessels by gadolinium contrast-enhanced MRI had previously been histologically validated in the distal femur of pigs. 48 Images of cartilage canal vessels were therefore generated using this technique (Fig. 15) and compared with an MRI sequence known as susceptibility-weighted imaging (SWI). 111 Susceptibility-weighted imaging relies on subtle, tissue-inherent differences in the susceptibility to magnetism and uses both magnitude and phase data to generate an image. 111 It is particularly sensitive to deoxygenated venous blood, and with SWI, it was possible to visualize cartilage canal vessels directly, without the use of a contrast medium (Fig. 16). The initial investigations were carried out in 9.4 T and 7 T research scanners, but feasibility of in vivo visualization was subsequently confirmed by examination of a live pig in a clinically available 3 T scanner. 73 Thus, because it was possible to visualize vessels, 73,111 it is probably also possible to detect osteochondrosis latens lesions indirectly as a focal absence of patent vessels in MRI scans.
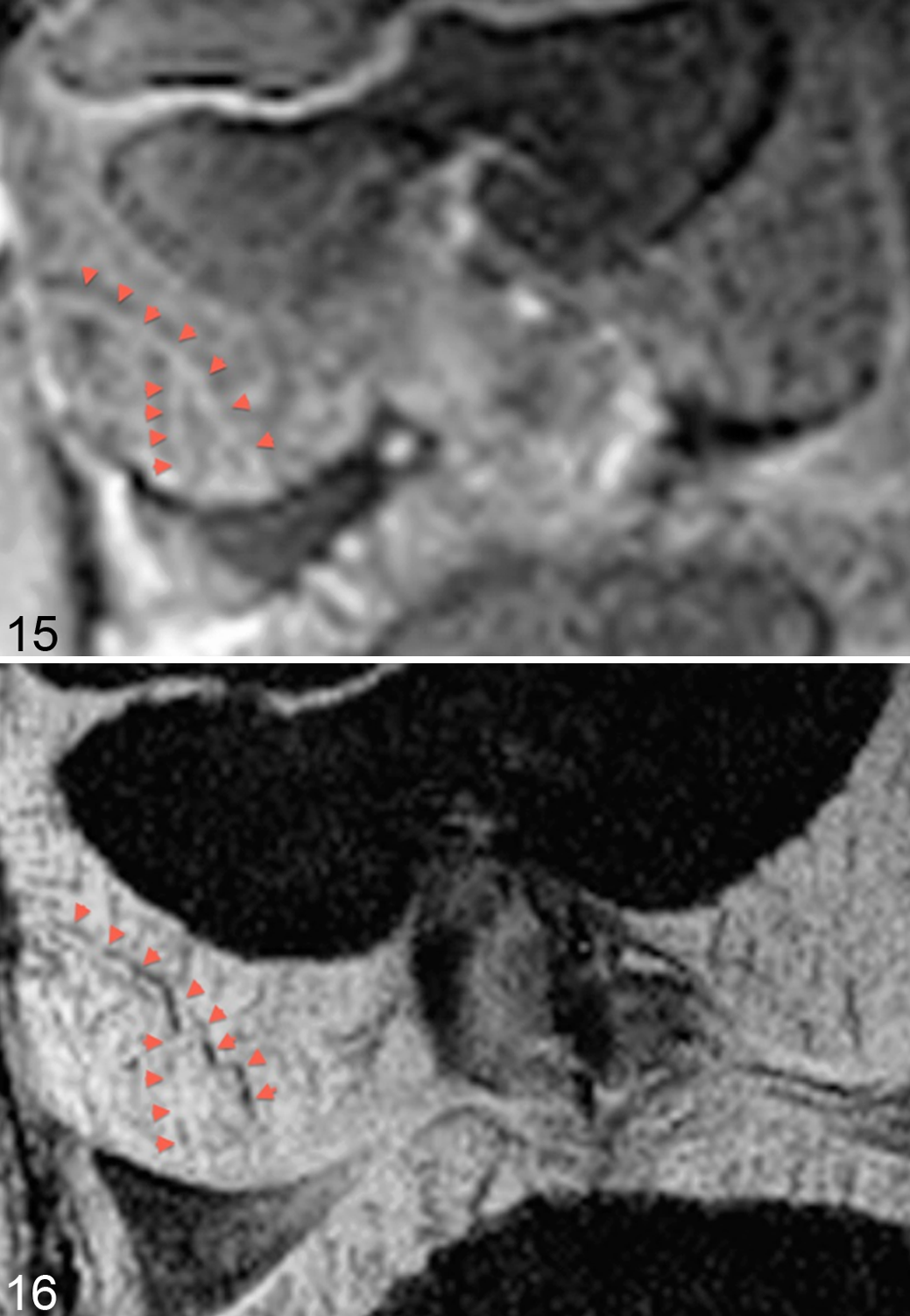
Distal femur, cartilage canal vessels, live pig. Magnetic resonance imaging (MRI) scanning (7 T). Proximal is to the top and the left side of the animal is to the right side of each image.
Ex vivo plain MRI of experimental lesions in goats
The possibility of detecting intracartilaginous areas of ischemic chondronecrosis (osteochondrosis latens) directly was further explored by experimental induction of lesions through surgical transection of the blood supply to epiphyseal growth cartilage followed by ex vivo MRI of the distal femur in goats. 110 Goats were chosen because they have not been reported to develop spontaneous osteochondrosis. Femurs were first imaged using a 3-dimensional gradient recalled echo sequence to identify the site of vessel transection. 110 A single, 1 mm-thick slice was then selected from the site and the so-called adiabatic T1ρ relaxation time was measured. The sequence was used because it has a known sensitivity for detection of changes in proteoglycan content. 110 In 3 of 4 goats with osteochondrosis latens, focal areas with increased relaxation time in adiabatic T1ρ maps (Fig. 17) corresponded to areas of necrosis-associated matrix change in safranin-O–stained histological sections (Fig. 18). 110 It is therefore highly likely that it will be possible to detect osteochondrosis latens lesions by in vivo MRI and adiabatic T1ρ mapping, and the technique is currently being evaluated using clinically available scanners.
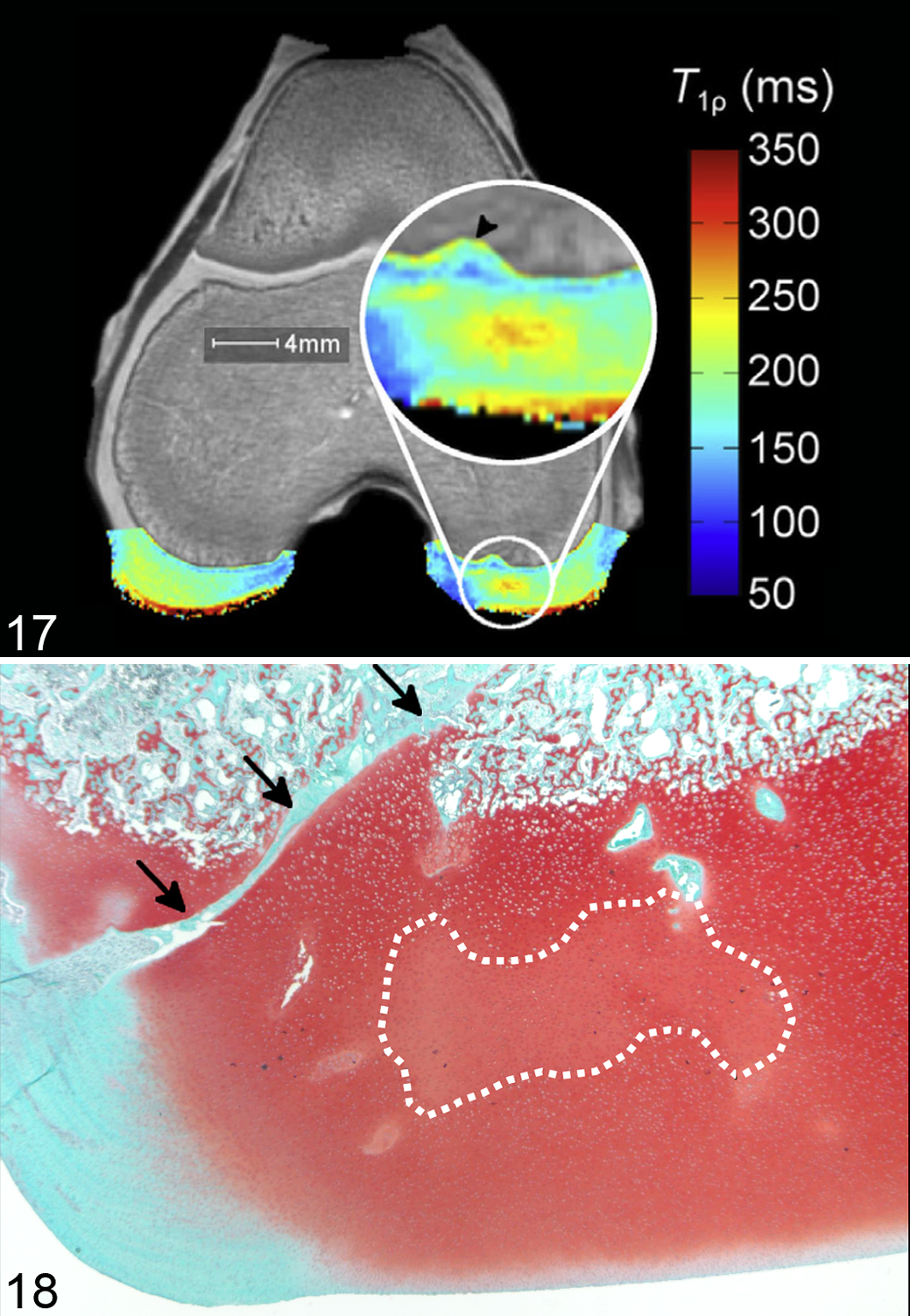
Distal femur, experimental osteochondrosis latens, goat. Magnetic resonance imaging (MRI) scan (9.4 T, ex vivo). Cranial is to the top and left side of the animal is to the right side of each image.
Summary
The earliest lesion following vascular failure is an area of ischemic chondronecrosis at intermediate depth of the growth cartilage (osteochondrosis latens) that is detectable ex vivo, indirectly using contrast-enhanced micro- and conventional CT or directly using adiabatic T1ρ MRI.
More chronic lesions of ischemic chondronecrosis within the ossification front (osteochondrosis manifesta) are detectable by the same techniques and have also been followed longitudinally in pigs using plain CT.
The results confirm that lesions sometimes undergo spontaneous resolution and in combination, CT and histology observations indicate that this occurs by filling of radiolucent defects with bone from separate centers of endochondral ossification that form superficial to lesions, as well as by phagocytosis and intramembranous ossification of granulation tissue that forms deep to lesions.
What Is the Relationship Between the Studies of Ischemic Chondronecrosis and Previous Studies of the Pathogenesis of Osteochondrosis in Horses?
The studies by Bridges et al 10 and Hurtig et al 45 indicated that osteochondrosis could be the result of copper deficiency–induced reduced collagen crosslinking, but in later studies, it has been difficult to influence prevalence 30,31 and impossible to eradicate osteochondrosis through copper supplementation alone. 17,89 There is some evidence to suggest that a high copper status at birth is associated with an increased proportion of lesions undergoing spontaneous resolution, 54,118 but the conclusion of the most recently published study was that the role of copper in the pathogenesis of osteochondrosis remains poorly understood. 30
Independent of copper, Lecocq et al 64 detected changes in collagen structure, and studies reviewed by Laverty and Girard 60 indicate that the biomarker change that is most frequently detected in young horses is an increase in type II collagen synthesis. Both author groups suggest that collagen changes could be involved in the initiation of lesions. 60,64 Chondrocytes that have undergone necrosis are unable to perform their role in matrix homeostasis, and reduced number and thickness of collagen fibrils were observed in areas of ischemic chondronecrosis in pigs. 13,25 Whether changes in collagen structure 64 or synthesis 60 are capable of causing vascular failure remains to be determined (see “Causes of Vascular Failure,” below).
The imaging 77,79 and experimental 78 studies agree that separate centers of endochondral ossification form in association with lesions of osteochondrosis 32 but confirm that these are a consequence rather than a cause of the disease.
The suggestion that osteochondrosis was the result of dyschondroplasia was based on observation of small, round chondrocytes deep to the ossification front. 42,104 Further studies have confirmed that the ossification front is generally irregular in young animals. 64,77,82,85 The irregularities that are associated with osteochondrosis contain chondrocytes that are necrotic, and it is possible to distinguish between such lesions and general irregularities in histological sections 85 and CT scans. 77,79,82
What Is the Relationship Between Ischemic Chondronecrosis and the Pathogenesis of Osteochondrosis in Species Other Than Pigs and Horses?
In 1978, it was determined that OCD was a result of the underlying disease process osteochondrosis in the 6 animal species in which it had been described. 76 The conclusion that osteochondrosis is a consequence of vascular failure and ischemic chondronecrosis in pigs and horses was based on histological examination of material collected from predilection sites during the age windows when lesions are known to develop 12,14,52,84,85,127 and experimental studies where lesions were induced by transecting cartilage canal vessels. 15,78,130 The most relevant histological and experimental studies that we have been able to find in cattle, dogs, and humans are summarized in Table 1. Histological studies confirm that areas of cartilage canal and chondrocyte necrosis occur at predilection sites in cattle, 122 and thus there is sufficient evidence to conclude that osteochondrosis is a result of vascular failure in this species. 72 While it seems likely that osteochondrosis is a result of vascular failure and ischemic chondronecrosis in dogs and humans also, 24,67,76 further studies are needed to reach a conclusion in these species.
Histological, Experimental, and Arterial Perfusion Studies That Are Relevant to the Pathogenesis of Articular Osteochondrosis in Cattle, Dogs, and Humans.
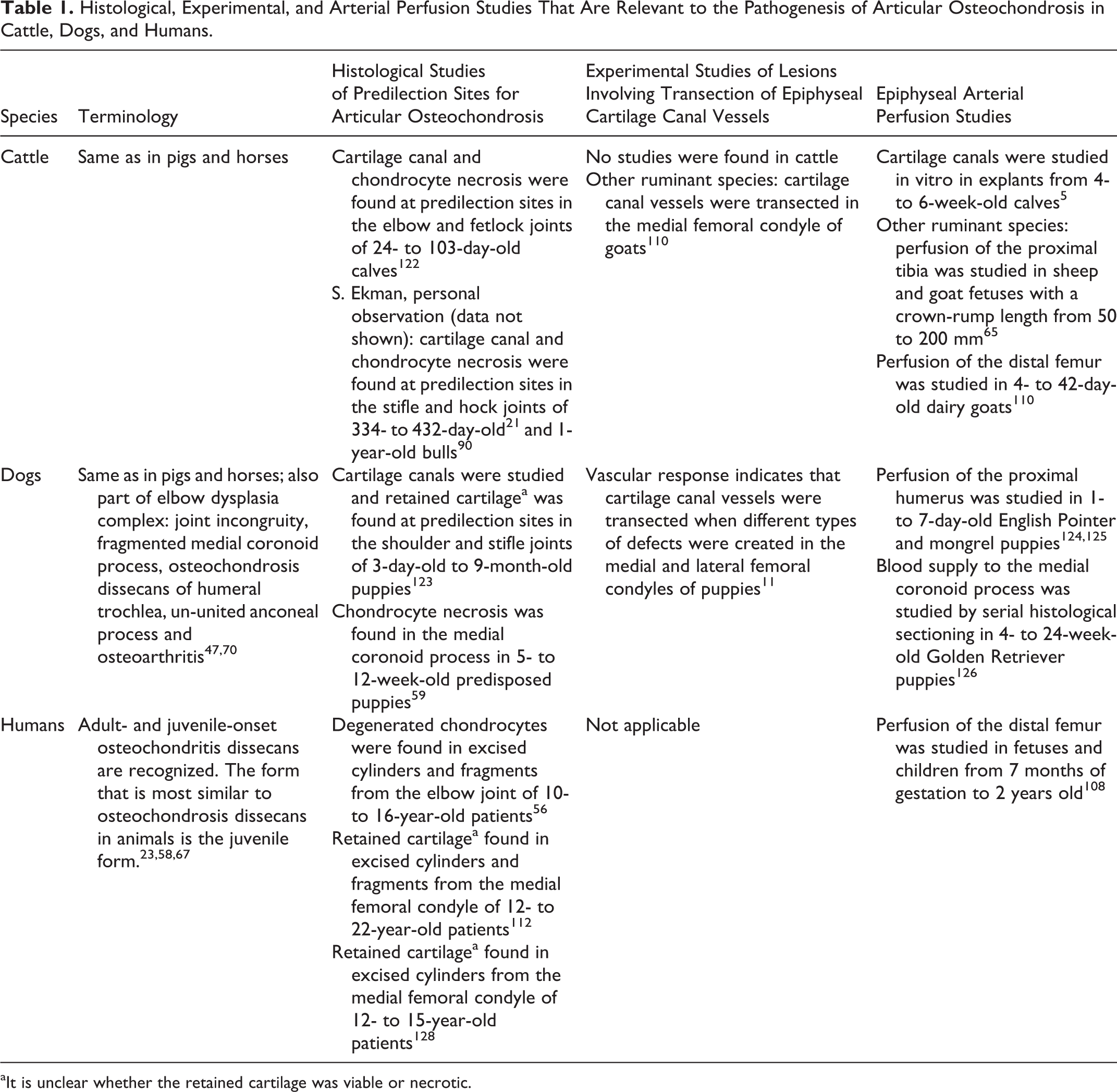

aIt is unclear whether the retained cartilage was viable or necrotic.
In pigs and horses, the process of incorporating cartilage canal vessels into the ossification front has been implicated in the initiation of the vascular failure in osteochondrosis. 88,133 The fact that vessels are incorporated into the ossification front was discovered during arterial perfusion studies, 15,86 –88,132 and the link between early lesions and incorporation was discovered because the perfusion studies were carried out in animals that were disposed to develop osteochondrosis. 88,133 Some of the arterial perfusion studies that are currently available in cattle, dogs, and humans are listed in Table 1.
What Is the Relationship Between the Studies of Ischemic Chondronecrosis and Studies Into Other Aspects of Osteochondrosis in Pigs and Horses?
The current report is intended to provide an update on research into the pathogenesis of osteochondrosis from 2007 to 2015, and studies focusing on pathogenesis are cited within the report. However, studies focusing on aspects of osteochondrosis other than pathogenesis have been published in the same time period. A PubMed search using the term osteochondrosis returned 22 such studies in pigs and 92 studies in horses. The 114 studies are listed in Supplemental Table S1.
In 87 of 114 studies (76%; Suppl. Table S1), osteochondrosis was identified using imaging and arthroscopic, macroscopic, and/or histological evaluation. Criteria for macroscopic diagnosis often included cartilage thickening or retained cartilage cores, meaning that studied lesions most likely represented osteochondrosis manifesta. In other cases, diagnostic criteria included fissures and cartilage loss, and the lesions that were studied represented OCD. Histological evaluation, the current reference standard for the diagnosis of osteochondrosis latens, was used in only 14 of 87 studies (16%), and the studies referred to 7 different sets of diagnostic criteria (Suppl. Table S1). Cartilage canal necrosis was included as a diagnostic feature in only 2 sets of criteria, 7,57 referred to in 3 of the studies listed in Supplemental Table S1. Thus, it would be possible to discuss the relationship between other studies and osteochondrosis manifesta or OCD, but this would reveal limited information about pathogenesis and would be more appropriate in a clinically oriented paper than in the current review. Discussion of the relationship between other studies and osteochondrosis latens would be confined to the 2 cases where cartilage canal necrosis was included as a diagnostic feature. 7,57 The 3 studies in question focus on genetics, and genetic studies were the most common among studies into aspects of osteochondrosis other than pathogenesis, representing 8 of 22 of the studies in pigs (36%) and 26 of 92 of the studies in horses (28%; Suppl. Table S1). The aim of the genetic studies was to discover the nature of the heritable predisposition for osteochondrosis, a topic that is considered beyond the scope of the current report. It is difficult to compare the results of different studies when different sets of diagnostic criteria are used. In Table 2, we have summarized the progression of lesions following experimental vascular transection because the fact that progression was so similar suggests that it may be valid to use a single set of diagnostic criteria in several species 15,78,110,130 The experimental studies strongly indicate what the histological criteria could be, and there are also studies available that indicate how the histological criteria listed in Table 2 correlate with changes in diagnostic imaging modalities that can be used in live animals such as radiography, 79 CT, 82 and MRI. 110
Progression of Lesions Following Experimental Vascular Transection in Pigs, Horses, and Goats.
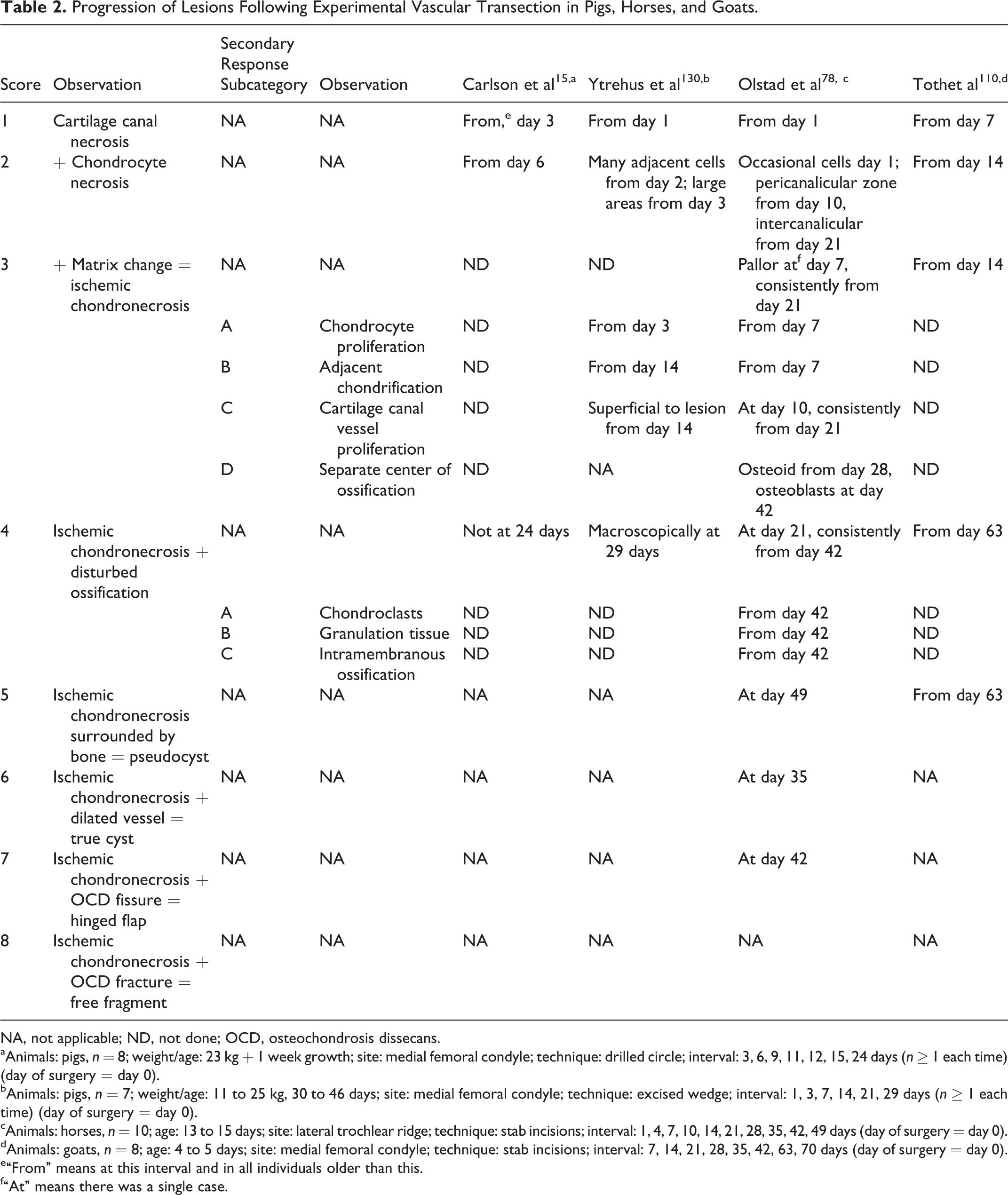
NA, not applicable; ND, not done; OCD, osteochondrosis dissecans.
aAnimals: pigs, n = 8; weight/age: 23 kg + 1 week growth; site: medial femoral condyle; technique: drilled circle; interval: 3, 6, 9, 11, 12, 15, 24 days (n ≥ 1 each time) (day of surgery = day 0).
bAnimals: pigs, n = 7; weight/age: 11 to 25 kg, 30 to 46 days; site: medial femoral condyle; technique: excised wedge; interval: 1, 3, 7, 14, 21, 29 days (n ≥ 1 each time) (day of surgery = day 0).
cAnimals: horses, n = 10; age: 13 to 15 days; site: lateral trochlear ridge; technique: stab incisions; interval: 1, 4, 7, 10, 14, 21, 28, 35, 42, 49 days (day of surgery = day 0).
dAnimals: goats, n = 8; age: 4 to 5 days; site: medial femoral condyle; technique: stab incisions; interval: 7, 14, 21, 28, 35, 42, 63, 70 days (day of surgery = day 0).
e“From” means at this interval and in all individuals older than this.
f“At” means there was a single case.
Causes of Vascular Failure
Several causal factors have been proposed and were discussed under subheadings of “Rapid Growth,” “Heredity,” “Anatomical Characteristics,” “Trauma,” and “Dietary Factors” in the 2007 review of osteochondrosis by Ytrehus et al. 131 As discussed above, osteochondrosis in pigs and horses occurs as a consequence of vascular failure and ischemic chondronecrosis.* The cause of the vascular failure is therefore also the indirect cause of the subsequent osteochondrosis. Vascular failure can only be studied during the age windows when the blood supply to epiphyseal growth cartilage is still present. In the equine fetlock and hock joints, vascular failure must be studied in animals that are less than 10 weeks old. 12,87,88 Most of the previously proposed causal factors emanated from studies of animals that were older than this (ie, where the epiphyseal growth cartilage was avascular). It may therefore be necessary to study each factor again in animals where the blood supply is still present, to determine whether the factor is capable of causing vascular failure or, alternatively, merely represents a factor that is capable of modifying the outcome of the disease.
Causes of vascular failure in ischemic chondronecrosis and osteochondrosis have been proposed, especially in pigs, from as early as 1987, 127 and some are summarized in Table 3. It was originally considered that vascular failure could develop due to potentially trauma-induced premature 127 or exacerbated 14,120 chondrification, but in later studies, no association was found. 132
Proposed Causes of Failure of the Blood Supply to Growth Cartilage.
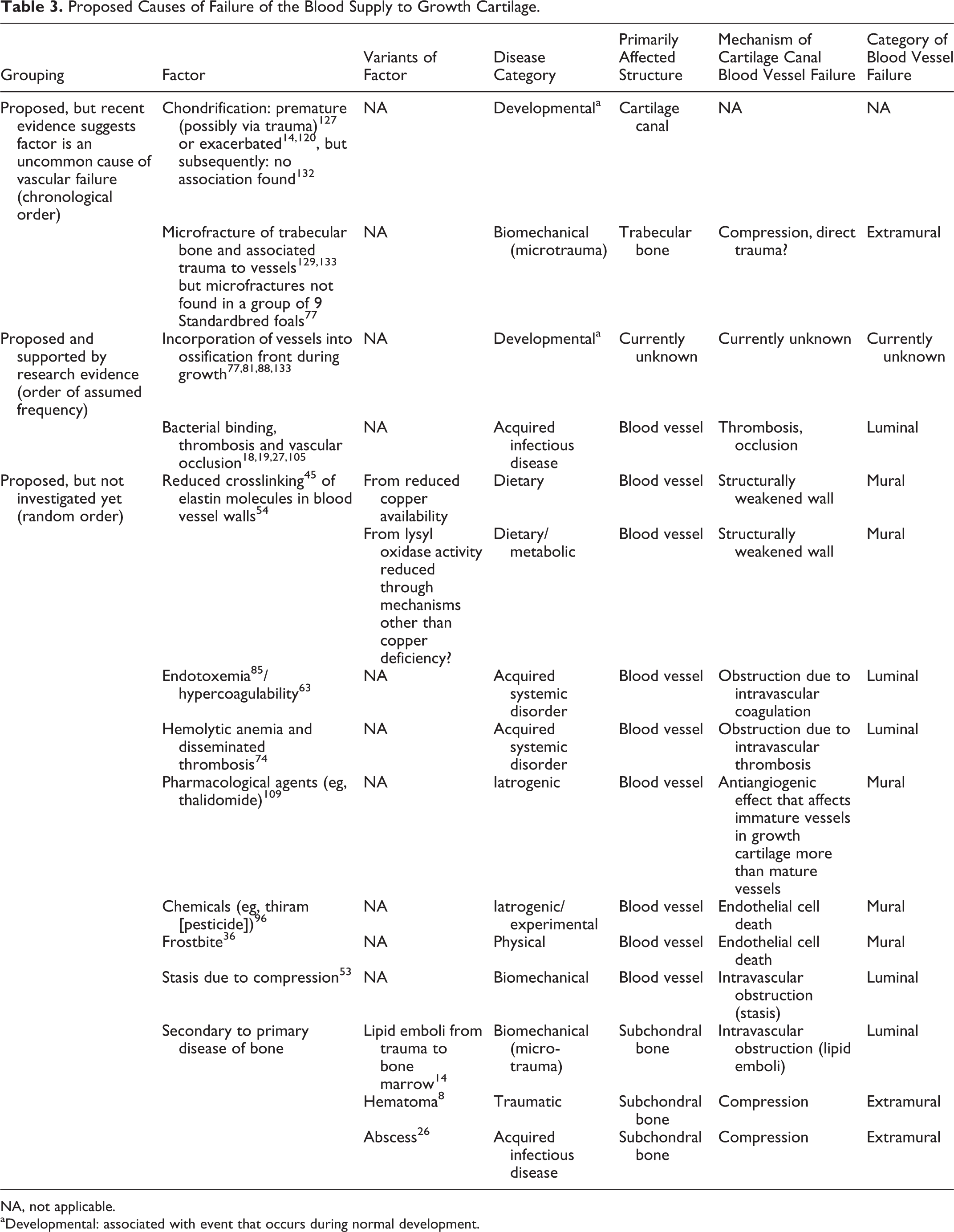
NA, not applicable.
aDevelopmental: associated with event that occurs during normal development.
When early lesions were studied by micro-CT with sufficient resolution to detect trabecular bone micro-fractures, the results indicated that micro-fracture was not the cause of the studied lesions (Table 3). 77 There is evidence to support, and little reason to doubt, that physiological 28,117 or traumatic 71 biomechanical force can influence the progression of osteochondrosis to OCD. For biomechanical force to be a valid cause of the vascular failure in osteochondrosis, the force must be capable of causing failure of vessels within a single cartilage canal while leaving vessels in immediately adjacent canals intact. 77,88 The force must also leave no sign of previous or ongoing physical disruption of bone 77 or cartilage (confocal microscopy; K. Olstad, unpublished data). Having said this, biomechanical force nevertheless remains a plausible cause of the vascular failure in osteochondrosis because studies have indicated that failure occurs at the ossification front, 88,133 which advances rapidly and therefore has the potential to obscure structural changes soon after they occur.
The cause that is supported by the most research evidence to date is that vascular failure is associated with the process of incorporating cartilage canal vessels into the advancing ossification front during growth. 77,81,88,133 Further studies are required to determine exactly which step of the process it is that fails in osteochondrosis. 116
In the equine predilection site studies, cause of death or euthanasia and concurrent disease were carefully recorded. 84,85 As was to be expected, a high proportion of the foals died or had been diagnosed with conditions involving septicemia. 84,85 A literature search revealed that, in addition to being a plausible cause of vascular failure in horses, 35,37 bacterial occlusion was an experimentally documented cause of vascular failure in pigs 18,19 and chickens. 27,105 It should be noted that although Erysipelothrix rhusiopathiae was used in some of the experimental studies, 18,19 this organism was not isolated when spontaneous lesions were examined in a larger number of pigs. 38 The prevalence of radiographically diagnosed lesions was higher in a group of Standardbred horses treated for infection prior to 6 months of age (68% prevalence) compared with a control group consisting of Standardbreds with unknown infection status as foals (51% prevalence). 39 Bacterial occlusion can therefore potentially account for a subset but not all lesions of osteochondrosis.
From 1997 to 2007, it was considered that osteochondrosis in horses could be the result of primary disease of collagen.
42,61,62,103,113
From 2008 onward, there was a shift from looking at collagen as the direct cause of osteochondrosis
42,61,62,103,113
to considering whether collagen disease is capable of causing vascular failure.
60,64
With reference to what has been discussed for biomechanical force and primary disease of collagen above, it may be pertinent to investigate the following questions: Collagen was organized differently around, compared with between, cartilage canals,
43,64
but is there any evidence to suggest that collagen is organized differently between adjacent individual canals, which could then explain why vessels within one canal fail at the same time as vessels in neighboring canals remain intact? Copper deprivation was associated with reduced crosslinking of collagen,
45
but is there any evidence that crosslinking of elastin in blood vessel walls is affected also,
45,54
resulting in weakening and vascular failure?
The above and other proposed causes of failure of cartilage canal blood vessels are listed in Table 3.
It is relatively easy to envisage that the process of incorporating vessels into the ossification front may be associated with a heritable predisposition. Conversely, bacterial occlusion represents an acquired cause of vascular failure. The fact that the 2 best-documented causes include 1 potentially heritable and 1 acquired cause indicates that it may become necessary to develop methods for distinguishing between different causes of vascular failure in the future. Failure of vessel incorporation and bacterial occlusion are likely to have different molecular biological signatures, and it would be a reasonable approach to investigate the extent to which these signatures are reflected in synovial fluid.
Summary
Research is currently aimed at discovering the cause of the vascular failure in osteochondrosis, and studies of spontaneous lesions suggest that failure is associated with the process of incorporating blood vessels into the ossification front during growth.
Experimental studies also show that bacteremia can lead to vascular occlusion.
Conclusions and Future Challenges
In 1978, it was concluded that OCD was a result of the underlying disease process osteochondrosis, characterized by a disturbance in endochondral ossification. 76
Observational and experimental studies have documented that osteochondrosis in pigs and horses occurs as a consequence of vascular failure and ischemic chondronecrosis. † The cause of the vascular failure is therefore also the indirect cause of the subsequent osteochondrosis.
The cause that is supported by the most research evidence to date is that vascular failure is associated with incorporation of vessels into the ossification front. 77,81,88,133 Bacterial occlusion is an experimentally documented cause of vascular failure in pigs 18,19 and chickens, 27,105 and observational studies indicate that this probably also occurs in horses. 35,37,39
The 3 most important challenges for the future are as follows: To determine which step of the vessel incorporation process it is that fails in osteochondrosis To develop methods for distinguishing between heritable and acquired causes of vascular failure To determine the nature of the heritable predisposition for vascular failure in osteochondrosis
Summary
Future challenges are to differentiate between causes of vascular failure and to discover the nature of the heritable predisposition for osteochondrosis.
Footnotes
Acknowledgements
We thank Bjørnar Ytrehus, Norwegian Institute for Nature Research, for contributions to this review through countless inspiring discussions on the pathogenesis of osteochondrosis over the years and for assistance with Figs. 12 and 14. We also thank Ferenc Toth, University of Minnesota, for assistance with Figs. 15 to ![]() .
.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Notes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
