Abstract
Canine malignant peripheral nerve sheath tumors (MPNSTs) occur not only in the peripheral nervous system (PNS) but also in soft tissue and various organs (non-PNS). The most important diagnostic criterion is proof of peripheral nerve sheath origin. This is difficult in non-PNS MPNSTs, and its differential diagnosis is challenging. Canine perivascular wall tumors (PWTs) also commonly arise in soft tissue. Their histopathological features are quite similar to those of canine MPNSTs, making their differential diagnosis challenging. To elucidate whether the morphological features are applicable to diagnose non-PNS MPNSTs and to demonstrate useful markers for distinction between canine MPNSTs and PWTs, the authors examined 30 canine MPNSTs and 31 PWTs immunohistochemically for S100, nestin, NGFR, Olig2, claudin-1, CD57, PRX, α-SMA, desmin, and calponin. Among canine MPNSTs, the PNS tumors displayed significantly higher S100 and Olig2 expression than the non-PNS tumors. The expression levels of the other markers did not differ significantly, suggesting that the same morphological diagnostic criteria are applicable regardless of their location. The PWT cells displayed significantly weaker immunoreactivity than MPNSTs to markers used except α-SMA and desmin. Cluster analysis sorted most canine MPNSTs and PWTs into 2 distinctly different clusters, whereas 3 MPNSTs and 6 PWTs were assigned to the opposing cluster. These 3 MPNSTs were negative for almost all markers, while these 6 PWTs were positive for only neuronal markers. In particular, NGFR and Olig2 were almost negative in the rest of PWT cases. These findings suggest that NGFR and Olig2 are useful to distinguish these 2 tumors.
Keywords
Peripheral nerve sheath tumors (PNSTs) occur not only in the peripheral nervous system (PNS) but also in soft tissue and various organs (non-PNS). PNSTs are histologically composed of pleomorphic spindle-shaped or polygonal neoplastic cells, which are derived from Schwann cells, perineurial cells, or both and are arranged in irregularly interwoven bundles, nuclear palisades, whorls, storiform patterns, or sheets. In addition, PNSTs contain various amounts of collagenous stroma. 12,13,19,20,31,45 Due to the poor prognosis of human malignant PNSTs (MPNSTs), their immunohistochemical features, pathogenesis, genetic basis, prognostic factors, and treatment strategies have been investigated extensively. 9,17,18,26,31,36,37,45 On the contrary, although there have been many reports on PNSTs, 2, 6, 11 –13, 19 –21, 28, 33, 34, 39, 41, 43, 44, 46 . their diagnostic criteria, histogenesis, subclassification, and immunohistochemical features are poorly understood in veterinary medicine. The most important diagnostic criterion for human PNSTs is proving that the neoplastic cells originate from peripheral nerve sheath components. 45 It is easy to detect the involvement of peripheral nerve sheath components in PNSTs in PNS tissue but not in non-PNS tissue. Without the proof of peripheral nerve sheath origin, the diagnosis of non-PNS MPNSTs should be made by morphological features. However, some spindle cell tumors have morphological features similar to those of MPNSTs, making the diagnosis of non-PNS MPNSTs challenging. Thus, immunohistochemical features should be confirmed based on those of PNS MPNSTs. In canine MPNSTs, it is not clear whether the morphological features are applicable to diagnose non-PNS MPNSTs without the proof of peripheral nerve sheath origin. Moreover, distinguishing MPNSTs from other spindle cell tumors that affect soft tissue such as fibrosarcomas or canine hemangiopericytomas (CHPs) 23,29 —recently suggested to be included in perivascular wall tumors (PWTs) 1,27 —is rather difficult. In such a case, it is very important to consider the morphological and immunohistochemical features based on those of PNS MPNSTs. Thus, it is important to determine useful diagnostic criteria and to clarify the effects of tumor location on morphological and immunohistochemical features to diagnose especially non-PNS MPNSTs.
Perivascular wall tumor is a novel classification for CHP suggested by a couple recent studies. 1,27 It is not included in the current World Health Organization international histological classification of tumors of domestic animals. 13 Canine PWTs also commonly arise in soft tissue. They are suggested to be a mixed group of tumors, including hemangiopericytoma, angioleiomyoma, angioleiomyosarcoma, myopericytoma, angiomyofibroblastoma, and angiofibroma. Their origin is considered to be the different cellular components of the vascular wall, such as undifferentiated stem cells, perivascular fibroblasts, pericytes, myopericytes, smooth muscle cells, myofibroblasts, or transitional cells with overlapping features. 1,27 The neoplastic cells are spindle shaped and arranged in interlacing bundles or in a myxoid, solid, storiform, or verocay-like pattern, and tumors have the following vascular growth pattern: perivascular whorls, staghorn, or placentoid vessels. 1,27 CHP has been considered a malignant unclassified soft tissue tumor, 13 and many PWTs are still diagnosed as CHPs based on histologic features, including perivascular whorls. Furthermore, the distinction from PNSTs is still under debate. 27
The histological features of PWTs resemble those of MPNSTs; therefore, distinguishing PWTs from MPNSTs arising in non-PNS tissue is difficult. There are several studies on the immunohistochemical or ultrastructural subclassification of PWTs 1,16,27 but very few studies on the comparison of immunohistochemical features for the differential diagnosis between canine MPNSTs and PWTs. 6,16 Furthermore, in companion animal practice, MPNSTs and CHPs have been treated as soft tissue sarcomas (STSs) together with other spindle cell tumors that arise in the soft tissue, such as fibrosarcomas, rhabdomyosarcomas, leiomyosarcomas, myxosarcomas, and malignant mesenchymomas, due to their similar histological features and biological behaviors. 22,38 However, Stefanello et al 38 recently suggested that PWTs (former CHPs) are a unique subgroup of STSs characterized by low to nonaggressive (ie, “benign”) behavior. Oversimplification sometimes prevents development of specific treatment. Research on the definite differentiation and prognostic factors for each STS is essential for the development of novel specific treatment strategies such as molecular targeted therapies.
In the present study, 30 canine MPNSTs and 31 PWTs were immunohistochemically investigated to determine useful diagnostic criteria and elucidate the effects of tumor location on the diagnostic criteria for canine MPNSTs and to demonstrate a useful immunohistochemical panel for the differential diagnosis between canine MPNSTs and PWTs.
Materials and Methods
Cases
Sixty-one canine spindle cell tumors were submitted to the Department of Veterinary Pathology, Graduate School of Agricultural and Life Sciences, the University of Tokyo, between 2008 and 2011. Histologically, 30 cases were diagnosed as canine MPNSTs and 31 cases were diagnosed as canine PWTs. The case histories and tumor locations of the MPNSTs and PWTs are listed in Tables 1 and 2, respectively. The data of the cases between 2008 and 2010 were obtained retrospectively, and the data of the cases between 2010 and 2011 were obtained prospectively. All tumors were obtained by excisional biopsy or complete surgical excision. Among the MPNSTs, 16 occurred in the PNS (Nos. 1–16), and 14 occurred in non-PNS tissue (Nos. 17–30), including the subcutaneous tissue (6/14; Nos. 17–22), visceral organs (4/14; Nos. 23–26), gingiva (2/14; Nos. 27 and 28), nasal cavity (1/14; No. 29), and external soft tissue around the right scapula (1/14; No. 30). Nos. 11, 18, 26, and 27 were recurrent tumors. Nos. 25 and 26 had metastatic lesions and were obtained by laparotomy. All 31 PWTs occurred in subcutaneous tissue. The tumor locations of the PWTs included the head and neck region (2/31; Nos. 31 and 32), the forelimbs or hindlimbs (22/31; Nos. 33– 43 and 51–61), and the body trunk (7/31; Nos. 44–50). The mean (SD) ages of the MPNST and PWT patients were 10.3 (2.0) years (range, 7 years to 13 years and 8 months) and 11.1 (2.2) years (range, 7 years and 5 months to 15 years and 1 month), respectively. Among the MPNST patients, 19 were males (including 10 castrated males), and 11 were females (including 6 spayed females). Among the PWT patients, 13 were males (including 4 castrated males), and 17 were females (including 6 spayed females). Age and sex data were not recorded for case No. 48.
MPNST Cases Examined.
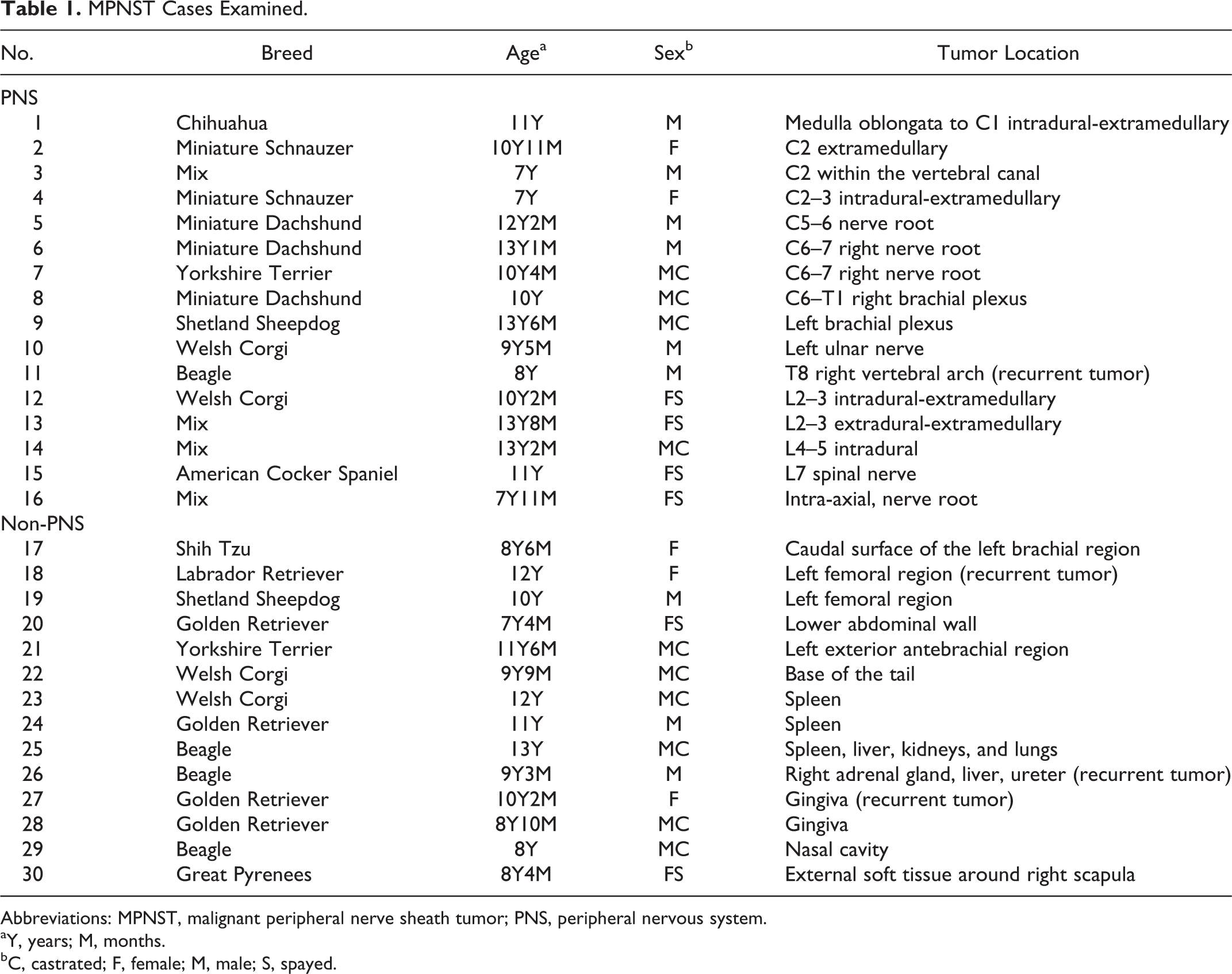
Abbreviations: MPNST, malignant peripheral nerve sheath tumor; PNS, peripheral nervous system.
aY, years; M, months.
bC, castrated; F, female; M, male; S, spayed.
CHP Cases Examined.
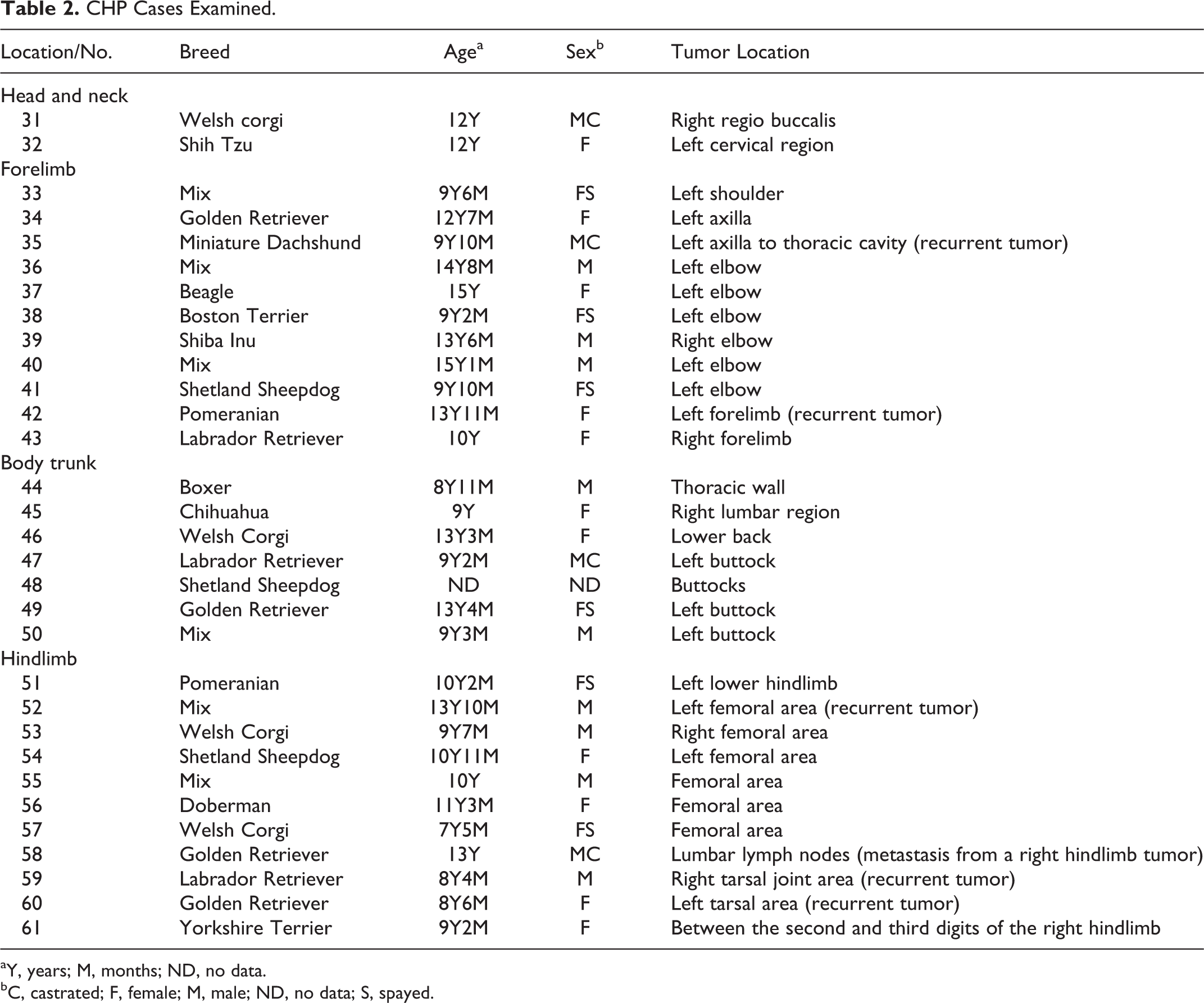
aY, years; M, months; ND, no data.
bC, castrated; F, female; M, male; ND, no data; S, spayed.
Histopathology
All tissue samples were fixed in a 10% phosphate-buffered formalin solution. Then, 2- to 4-μm-thick paraffin-embedded sections were cut and stained with hematoxylin and eosin (HE). MPNSTs were diagnosed based on the following modified histopathological criteria that were derived from the findings of previous studies 12,13,19,20,45 : (1) the tumor is composed of spindle-shaped or plump fusiform cells arranged in irregularly interwoven bundles, whorls, or sheets and/or displays nuclear palisades and contains various amounts of collagenous stroma; (2) peripheral nerve tributaries with neoplastic Schwann cells and/or perineurial cells can be observed, and the tumor appears to originate from them; and (3) the neoplastic cells display a certain degree of pleomorphism and invade the surrounding tissue, and the tumor also contains necrotic areas. PWTs were diagnosed using the histopathological criteria based on the current studies 1,27 : the tumor is composed of spindle-shaped cells arranged in interlacing bundles, or in a myxoid, solid, storiform, or verocay-like pattern, and has the following vascular growth pattern: perivascular whorls, staghorn, or placentoid vessels.
Immunohistochemistry
The primary antibodies used in the present study are listed in Table 3. To detect S100, claudin-1, CD57, PRX, desmin, and calponin, antigen retrieval was performed by autoclaving deparaffinized sections in citrate buffer (pH 6.0) at 121°C for 10 minutes, and for Olig2 detection, the sections were autoclaved in Target Retrieval Solution (DAKO Japan, Tokyo, Japan) (pH 9.0) at 121°C for 10 minutes. Antigen retrieval was not performed to detect nestin, NGFR, α-SMA, and neurofilament. The inactivation of endogenous peroxidase was performed by treating the sections with 3% hydrogen peroxide in methanol at room temperature (RT) for 5 minutes. To block nonspecific reactions, the sections were incubated in 8% skimmed milk in Tris-buffered saline (TBS) at 37°C for 30 minutes. Then, the sections were incubated with each primary antibody at 4°C overnight. After being washed 3 times with TBS, the sections were treated with Dako EnVision+ System horseradish peroxidase (HRP)–labeled polymer anti–mouse or anti–rabbit secondary antibodies (DAKO Japan) before being incubated at RT for 10 minutes, at 37°C for 40 minutes, and then at RT for a further 10 minutes. After being washed 3 times with TBS, 0.05% 3,3′-diaminobenzidine and 0.03% hydrogen peroxide in Tris-HCl buffer were used as the chromogen, and the sections were counterstained with Mayer’s hematoxylin. Tissue sections of the brachial plexus of a Pug dog (age 5 years and 4 months) without any neurological disorders were used as a positive control. Skeletal muscle and vascular wall were used as internal positive control for desmin and calponin, respectively. The primary antibodies were replaced with TBS to produce a negative control. The numbers of immunopositive neoplastic cells were counted within 10 randomly selected high-power (×400) fields, and the percentage of immunolabeled cells was calculated for each case.
Antibodies Used.
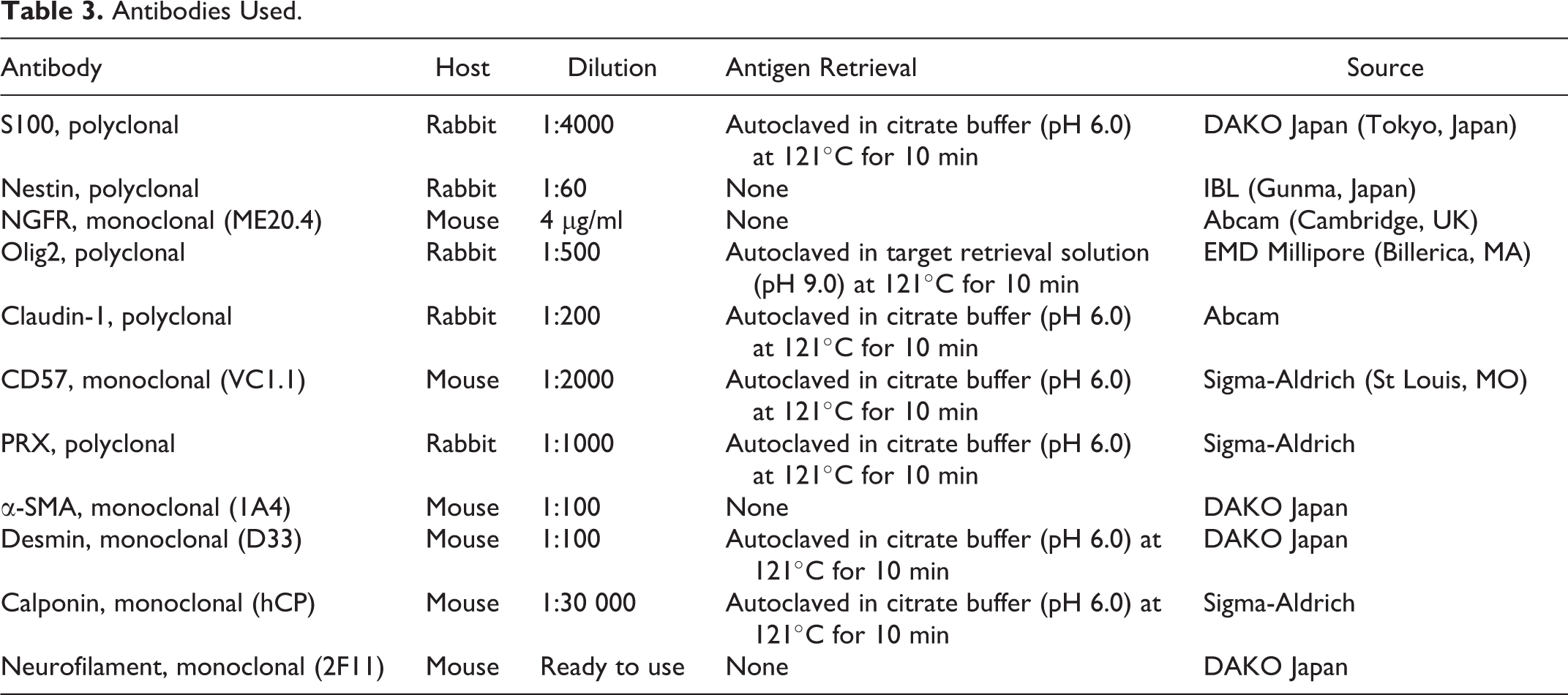
Statistical Analyses
Statistical analyses were performed using the SPSS 15.0 J software (SPSS Japan, Tokyo, Japan) with the percentage of immunolabeled cells. Pearson’s correlation coefficient analysis was performed within each tumor group to assess whether there was any correlation between the expressions of each marker. The Student’s t test was performed to examine whether there were significant differences in the mean percentage of immunopositive cells (1) between MPNSTs that arose in different locations (PNS and non-PNS) and (2) between MPNSTs and PWTs. P values of less than .05 were considered statistically significant.
Cluster Analyses
To examine the immunohistochemical differences (1) between PNS and non-PNS MPNSTs and (2) between MPNSTs and PWTs, the percentage of immunopositive cells of each case was assessed for each marker using a multivariate cluster analysis method, the Ward method, with the SPSS 15.0 J software. A dendrogram was constructed by assessing the squared Euclidian distances between the clusters.
Results
Histopathology
All tumors investigated were diagnosed as MPNST or PWT according to the diagnostic criteria described above. The histopathological features of the MPNST cases were quite similar regardless of the tumor location. They were composed of pleomorphic spindle cells. The neoplastic cells were mostly arranged in interwoven bundles, palisades, or whorls, and they occasionally had a wavy cytoplasm and nucleus. Tumors had necrotic areas within the lesion and invaded into the surrounding tissues. The involvement of peripheral nerve sheaths was not found in non-PNS MPNSTs. PWT cases had quite a similar morphology to MPNST cases. They were also composed of pleomorphic spindle cells and were arranged in interlacing bundles (3/31) or in a myxoid (14/31), solid (18/31), storiform (12/31), or verocay-like pattern (1/31), and the tumors had the following vascular growth pattern: perivascular whorls (14/31), staghorn (1/31), or placentoid vessels (4/31). Seventeen PWTs invaded into surrounding tissues, and 22 cases had necrotic areas within the lesion.
Immunohistochemistry
Cellular location of immunoreactivity to each antibody in the normal peripheral nerve sheaths, MPNSTs, and PWTs is summarized in Table 4. The immunoreactivity of normal peripheral nerve sheath components to each marker is shown in Figs. 1 to 10. The normal canine peripheral nerve sheaths displayed positivity for S100, NGFR, claudin-1, and CD57, as reported in previous reports. 3,5,6,14 On the other hand, the present study also found that the normal canine peripheral nerve sheaths expressed nestin, Olig2, and PRX, which has never been reported previously to our knowledge. S100 was expressed in the nuclei and cytoplasm of Schwann cells (Fig. 1), nestin was expressed in the cytoplasm of vascular endothelial cells and a few Schwann cells (Fig. 2), and NGFR was expressed in the perineurial cell membrane (Fig. 3). In addition, Olig2 was expressed in the cytoplasm of Schwann cells (Fig. 4), claudin-1 was expressed in the perineurial cell membrane (Fig. 5), and CD57 was expressed in myelin sheaths and the Schwann cell membrane (Fig. 6). Furthermore, PRX was expressed in myelin sheaths and the nuclei and membranes of Schwann cells (Fig. 7), α-SMA was expressed in the perineurium and vascular smooth muscle cells (Fig. 8), and neurofilament was expressed in axons (data not shown). Desmin and calponin were not expressed in peripheral nerve sheaths (Figs. 9 and 10, respectively).
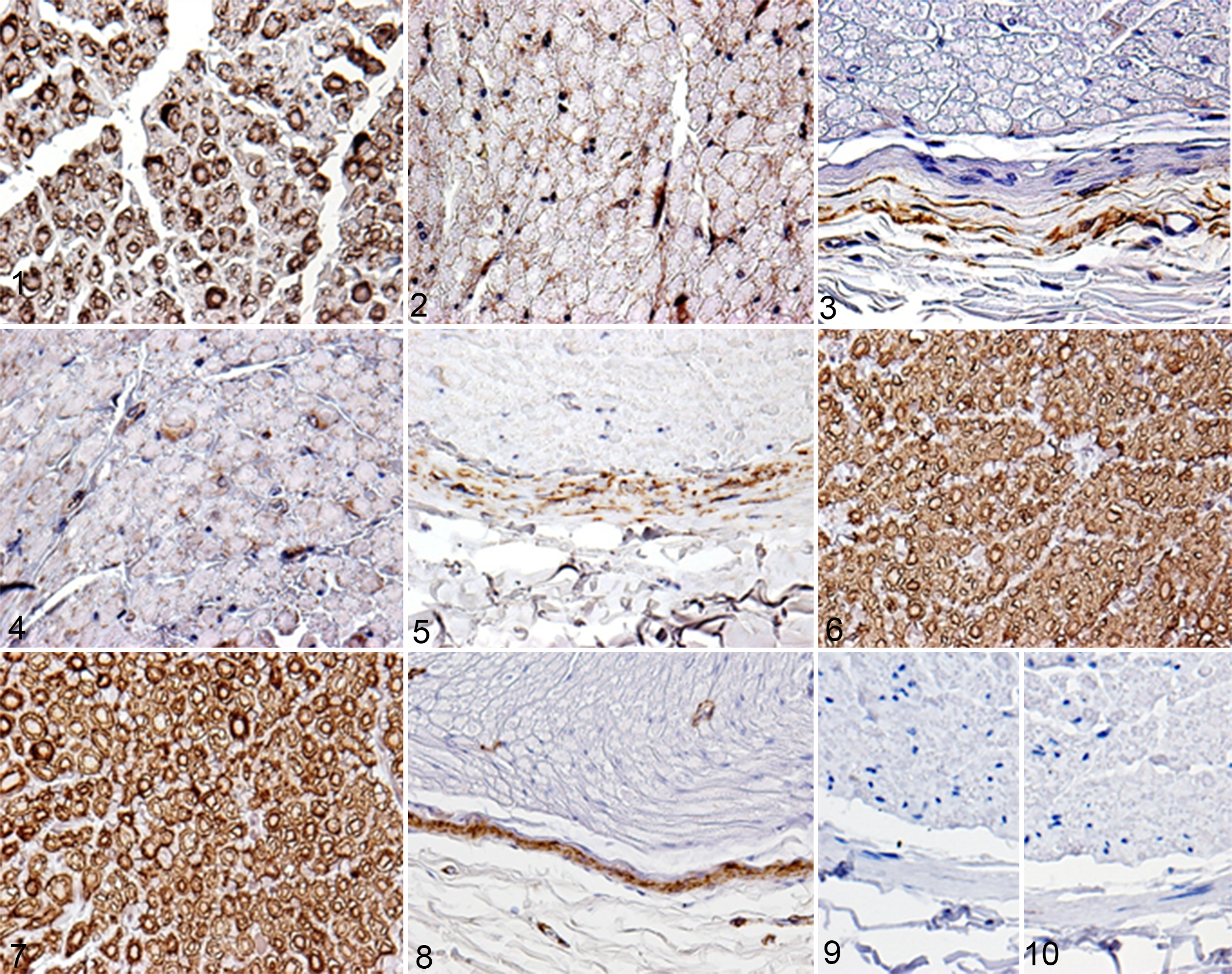
Brachial plexus; Pug. Many Schwann cells (myelin sheaths) in the normal peripheral nerve sheath are immunopositive for S100. Immunohistochemistry. Counterstain: Mayer’s hematoxylin.
Cellular Location of Immunoreactivity to each Antibody in the Normal Peripheral Nerve Sheaths, MPNSTs, and PWTs.
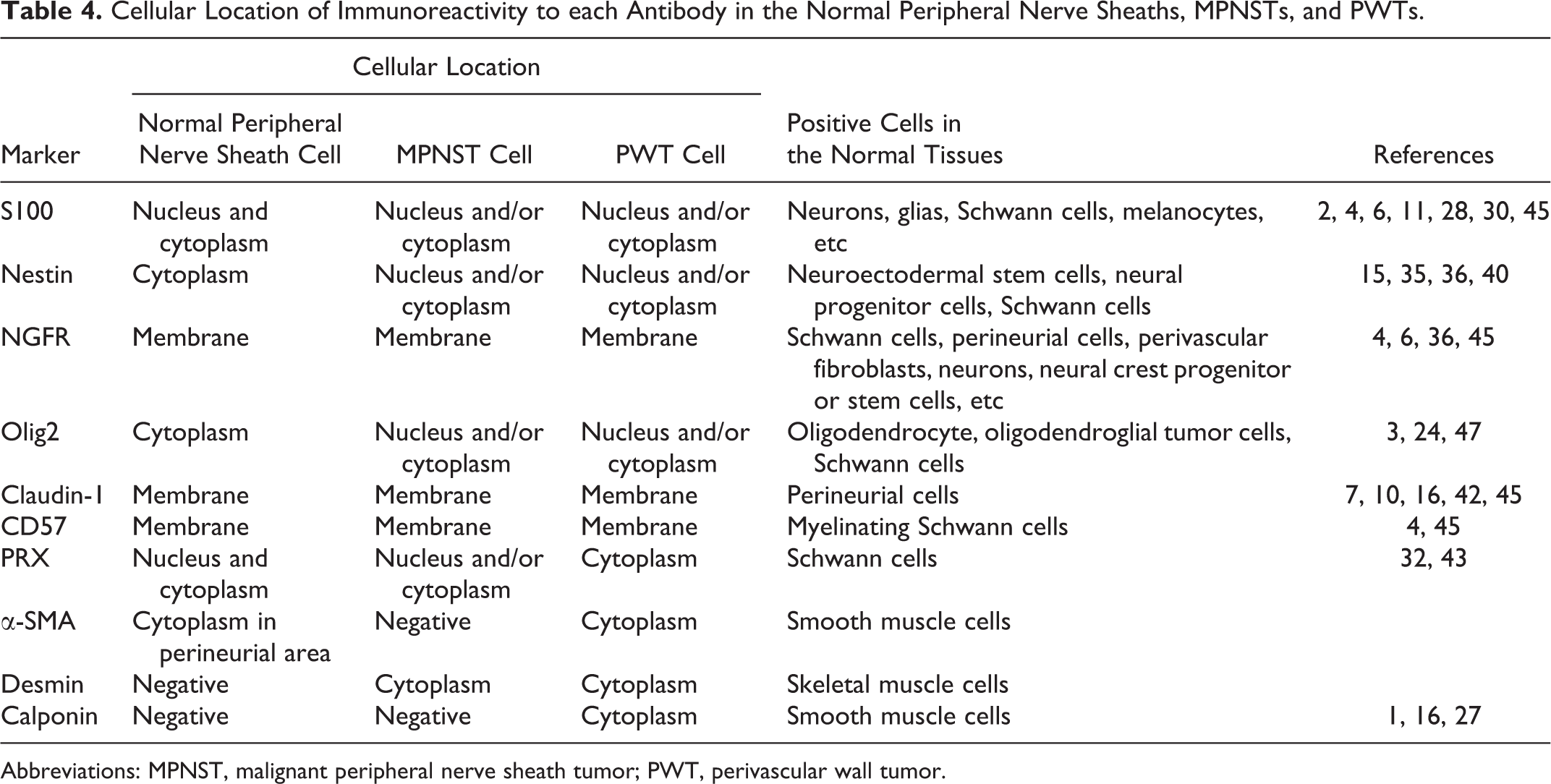
Abbreviations: MPNST, malignant peripheral nerve sheath tumor; PWT, perivascular wall tumor.
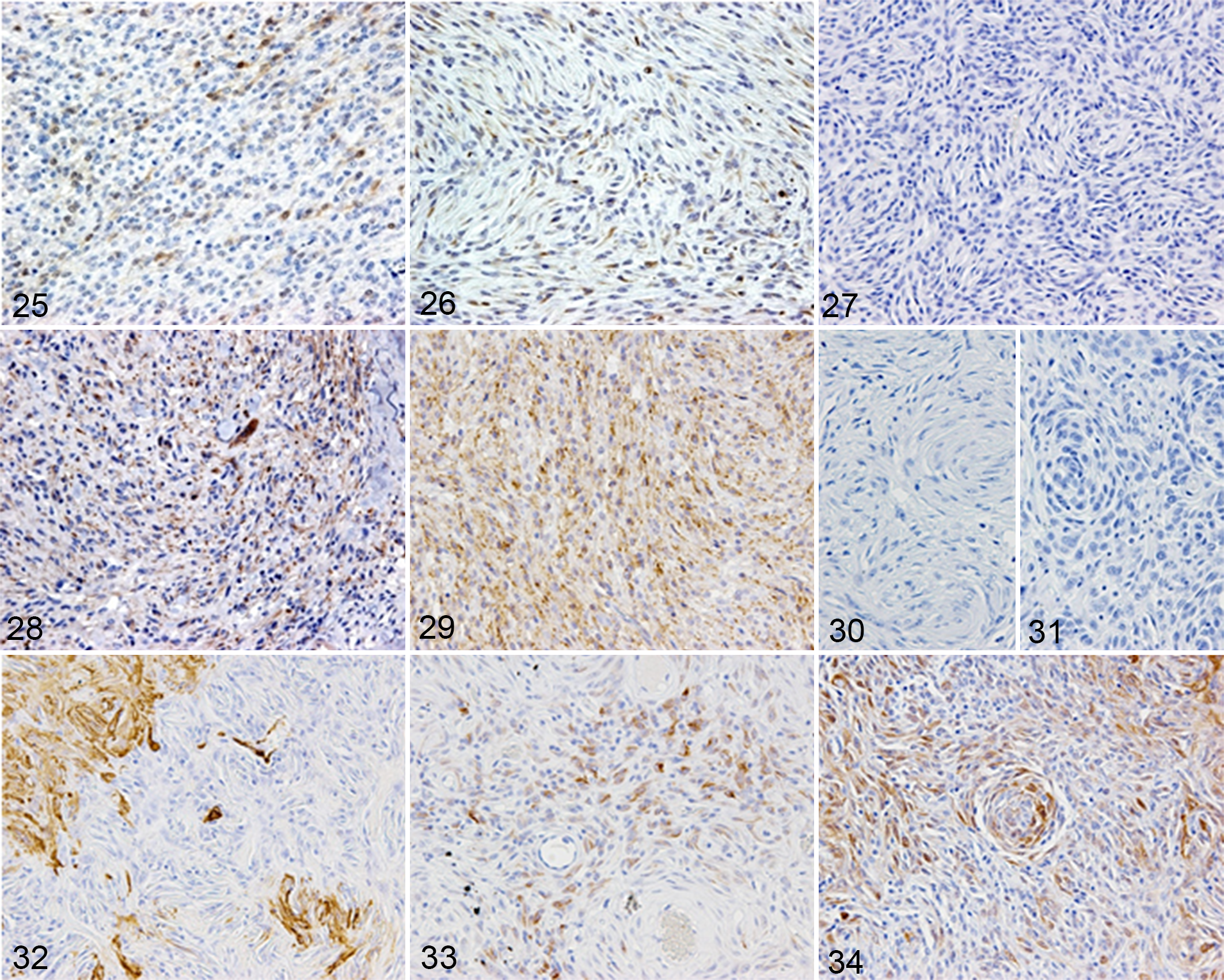
The staining patterns of each marker in MPNSTs and PWTs are shown in Figs. 11 to 34, and the percentages of MPNST and PWT cells that were positive for each marker are summarized in Tables 5 and 6, respectively. The staining intensities of the neoplastic cells were highly variable among the cases. In canine MPNSTs, S100 (29/30; 96.7%), nestin (28/30; 93.3%), Olig2 (27/30; 90.0%), and PRX (12/30; 40.0%) expression was observed in the nuclei and/or the cytoplasm of neoplastic cells, whereas NGFR (21/30; 70.0%), claudin-1 (21/30; 70.0%), and CD57 (18/30; 60.0%) expression was detected in the neoplastic cell membrane (Figs. 11–24). α-SMA, desmin, and calponin were not expressed in MPNSTs. Any peripheral neural axon was not detected in non-PNS MPNSTs with a neurofilament antibody. In PWTs, S100 (11/31; 35.5%), nestin (26/31; 83.8%), and Olig2 (6/31; 19.4%) expression was observed in the nuclei and/or the cytoplasm of the neoplastic cells, whereas NGFR (5/31; 16.1%), claudin-1 (17/31; 54.8%), and CD57 (1/31; 3.2%) expression was found in the neoplastic cell membrane. α-SMA (7/31; 22.6%), desmin (9/31; 29.0%), and calponin (7/31; 22.6%) expression was found in the cytoplasm of the neoplastic cells (Figs. 25–34). PRX was not expressed in PWTs.
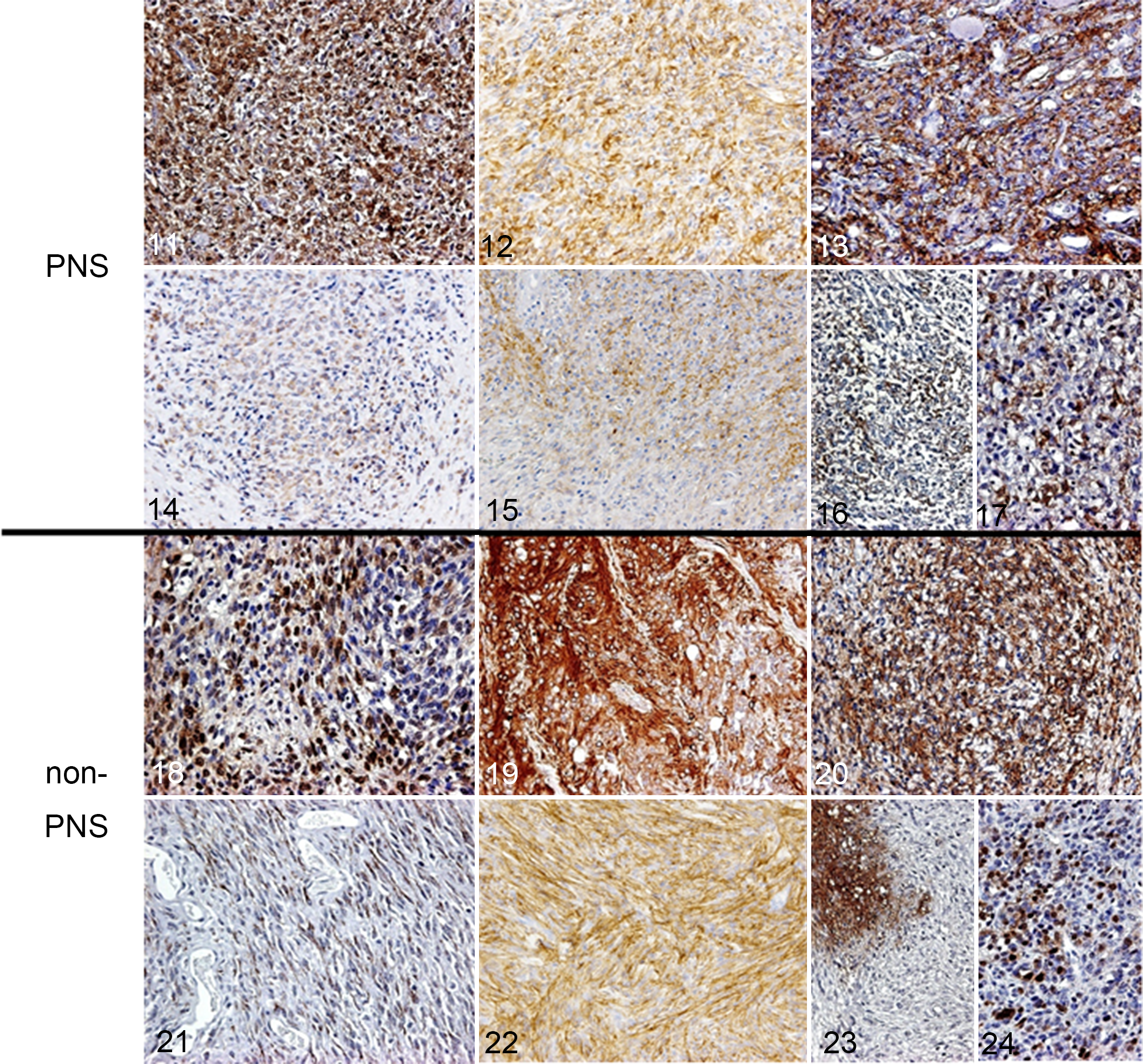
C2 extramedullary; Miniature Schnauzer, case No. 2. The malignant peripheral nerve sheath tumor (MPNST) cells are strongly immunopositive for S100 protein. Immunohistochemistry. Counterstain: Mayer’s hematoxylin.
Lumbar lymph nodes (metastasis from a right hindlimb tumor); Golden Retriever, case No. 58. The perivascular wall tumor (PWT) cells are weakly immunopositive for S100. Immunohistochemistry. Counterstain: Mayer’s hematoxylin.
Percentages of MPNST Cells Immunopositive for Each Marker.a
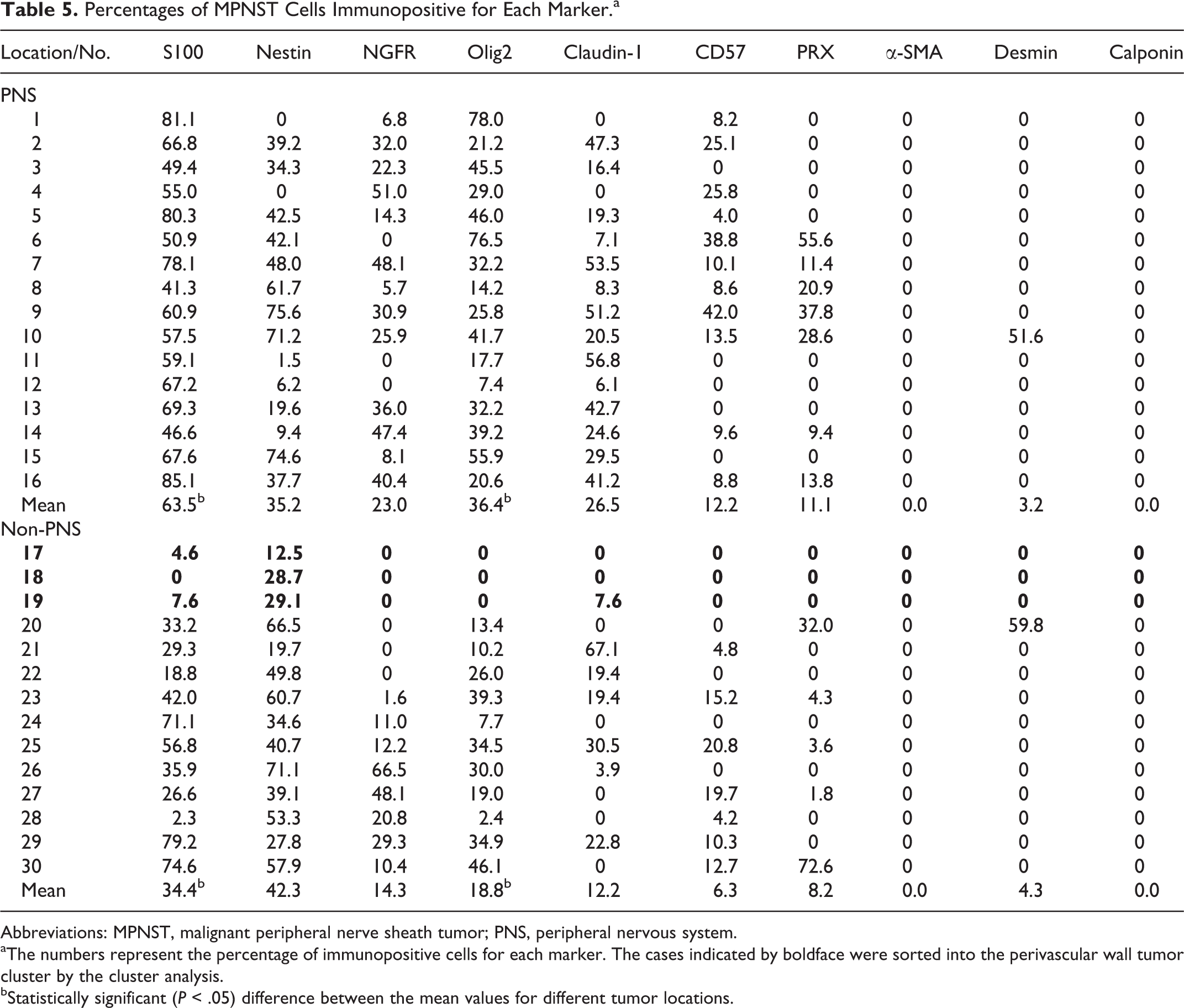
Abbreviations: MPNST, malignant peripheral nerve sheath tumor; PNS, peripheral nervous system.
aThe numbers represent the percentage of immunopositive cells for each marker. The cases indicated by boldface were sorted into the perivascular wall tumor cluster by the cluster analysis.
bStatistically significant (P < .05) difference between the mean values for different tumor locations.
Percentages of Perivascular Wall Tumor Cells Immunopositive for Each Marker.a
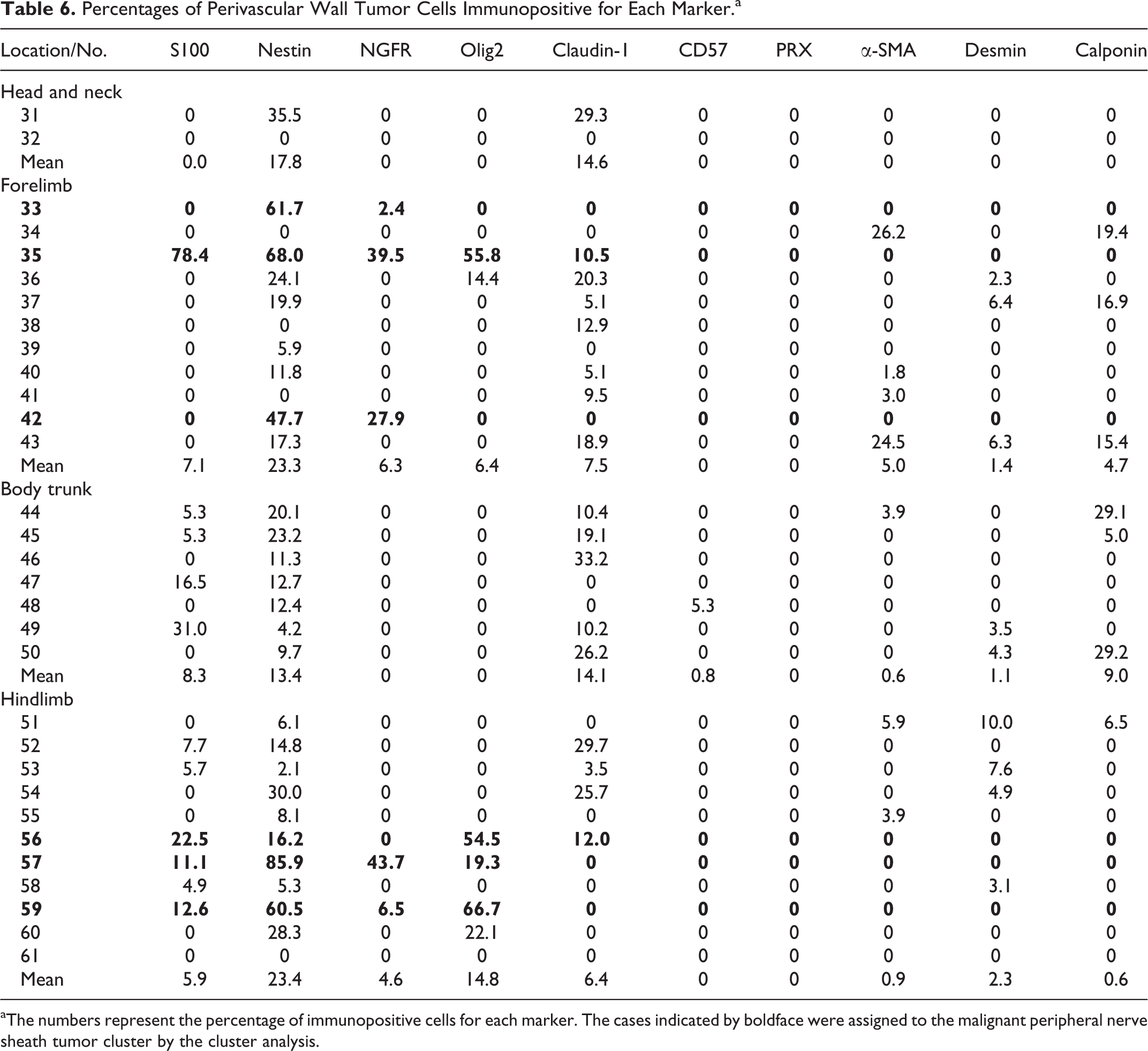
aThe numbers represent the percentage of immunopositive cells for each marker. The cases indicated by boldface were assigned to the malignant peripheral nerve sheath tumor cluster by the cluster analysis.
Statistical Analyses
The results of Pearson’s correlation coefficient analysis between each antibody within MPNST cases and within PWT cases are summarized in Tables 7 and 8. Within MPNST cases, moderate correlations were detected between S100 and Olig2, between nestin and PRX, and between CD57 and PRX. Within PWT cases, moderate correlations were detected between S100 and nestin, NGFR, and Olig2; between nestin and NGFR and Olig2; between NGFR and Olig2; and between α-SMA and calponin.
Pearson’s Correlation Coefficient Analysis Between Each Marker Within Perivascular Wall Tumor (PWT) Cases.a
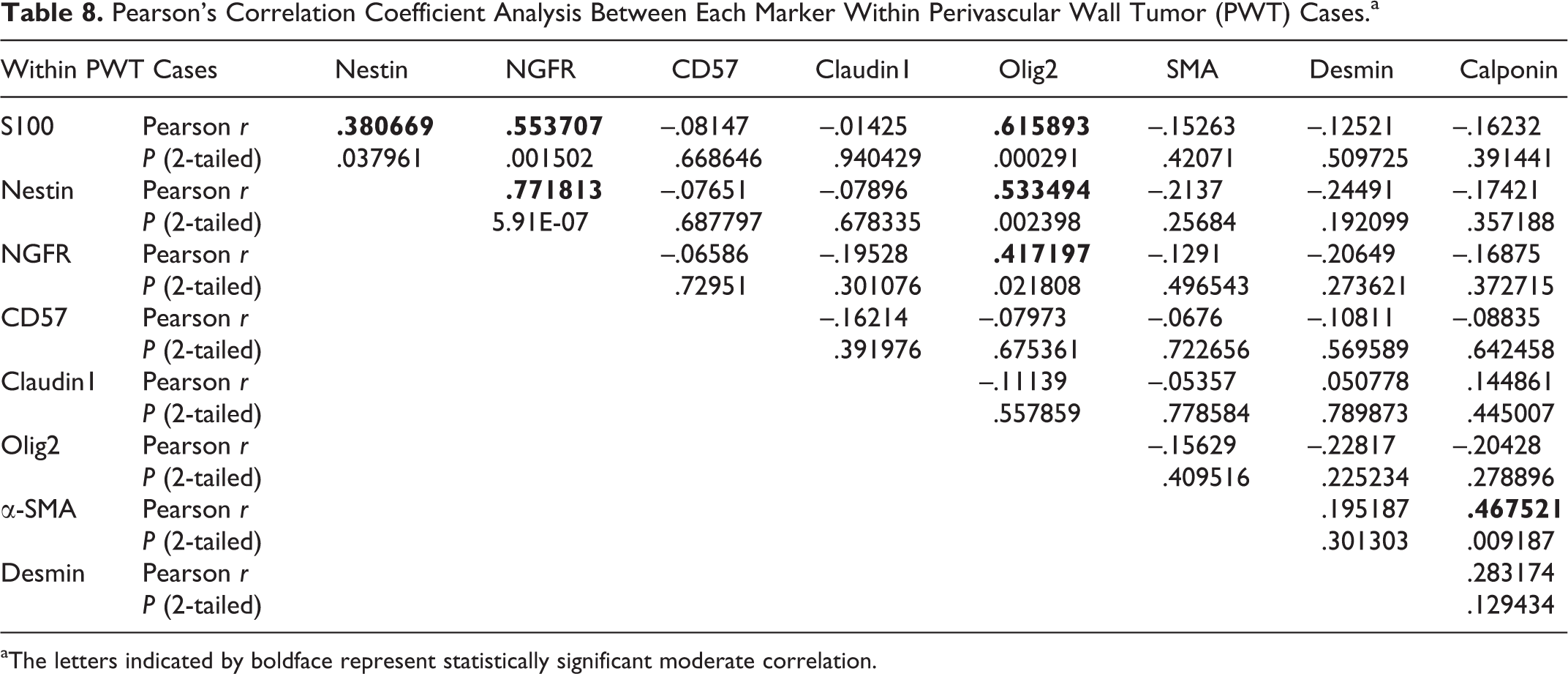
aThe letters indicated by boldface represent statistically significant moderate correlation.
Pearson’s Correlation Coefficient Analysis Between Each Marker Within Malignant Peripheral Nerve Sheath Tumor (MPNST) Cases.a
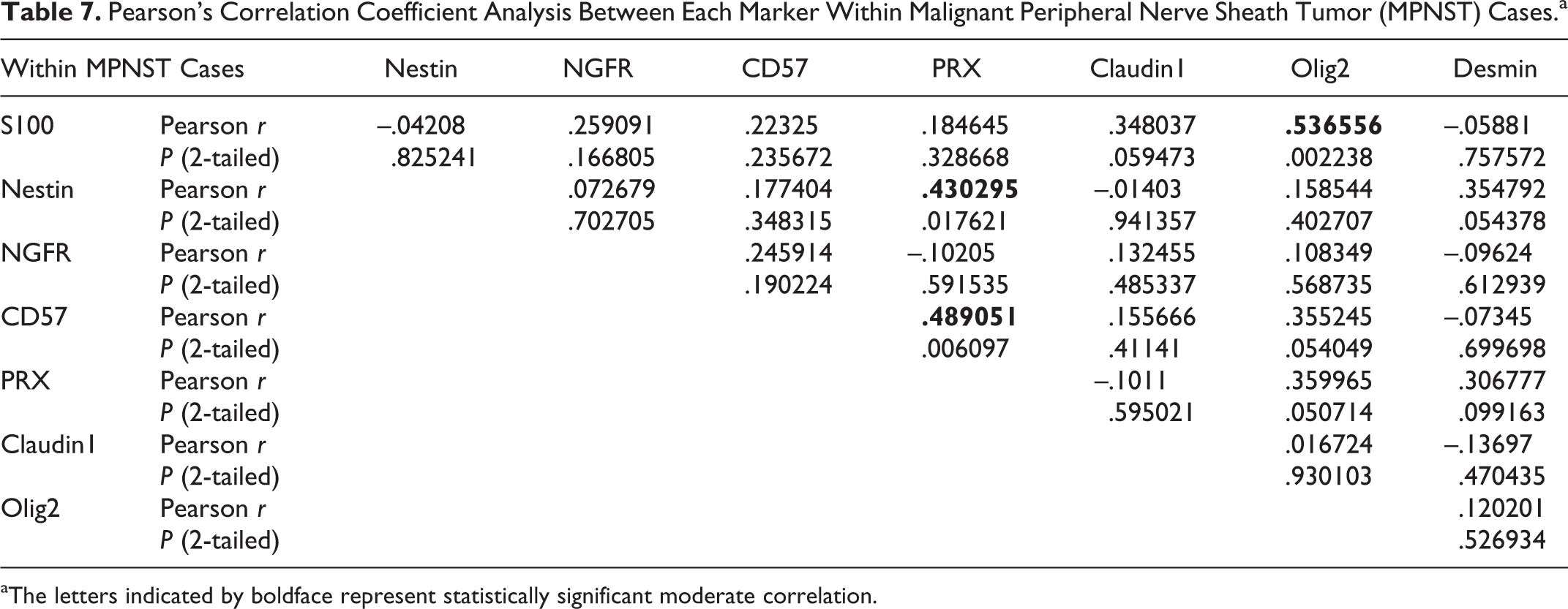
aThe letters indicated by boldface represent statistically significant moderate correlation.
Among MPNST cases, the mean percentages of neoplastic cells expressing S100 (63.5% in the PNS MPNSTs and 34.4% in the non-PNS MPNSTs) or Olig2 (36.4% in the PNS MPNSTs and 18.8% in the non-PNS MPNSTs) differed significantly between PNS and non-PNS (indicated in Table 5, Fig. 35). Between MPNSTs and PWTs, MPNSTs displayed significantly higher mean percentages of immunopositive neoplastic cells than did PWTs for all markers except α-SMA and desmin (Fig. 36).
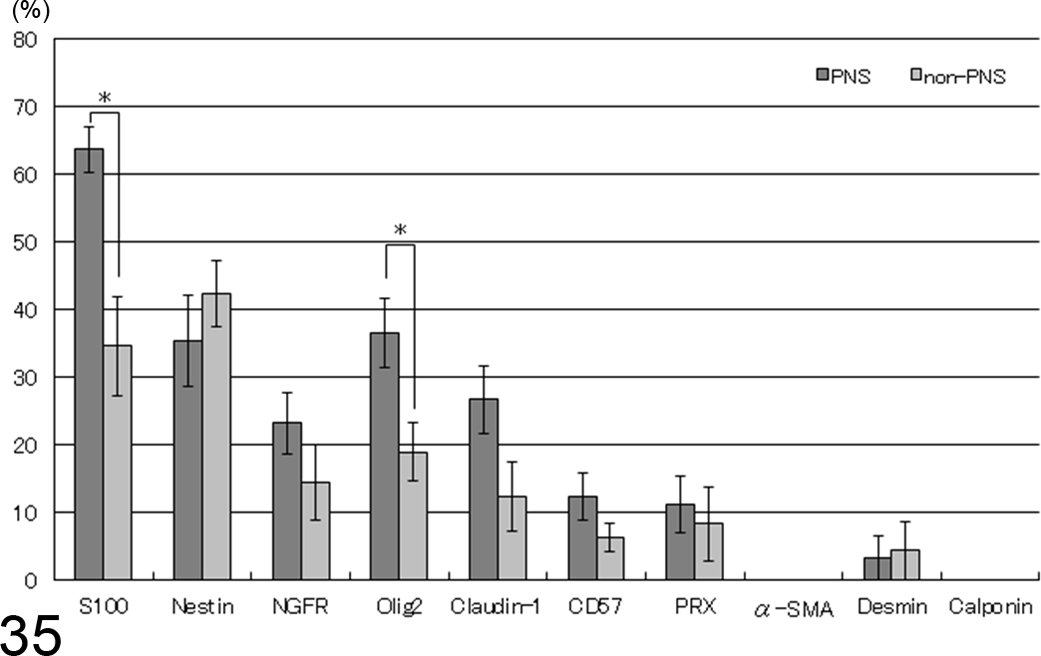
Mean percentages of immunopositive neoplastic cells in malignant peripheral nerve sheath tumors (MPNSTs). The peripheral nervous system (PNS) MPNSTs displayed significantly higher percentages of immunopositive cells than did non-PNS MPNSTs for S100 and Olig2 (mean ± SE). *Statistically significant (P < .05).
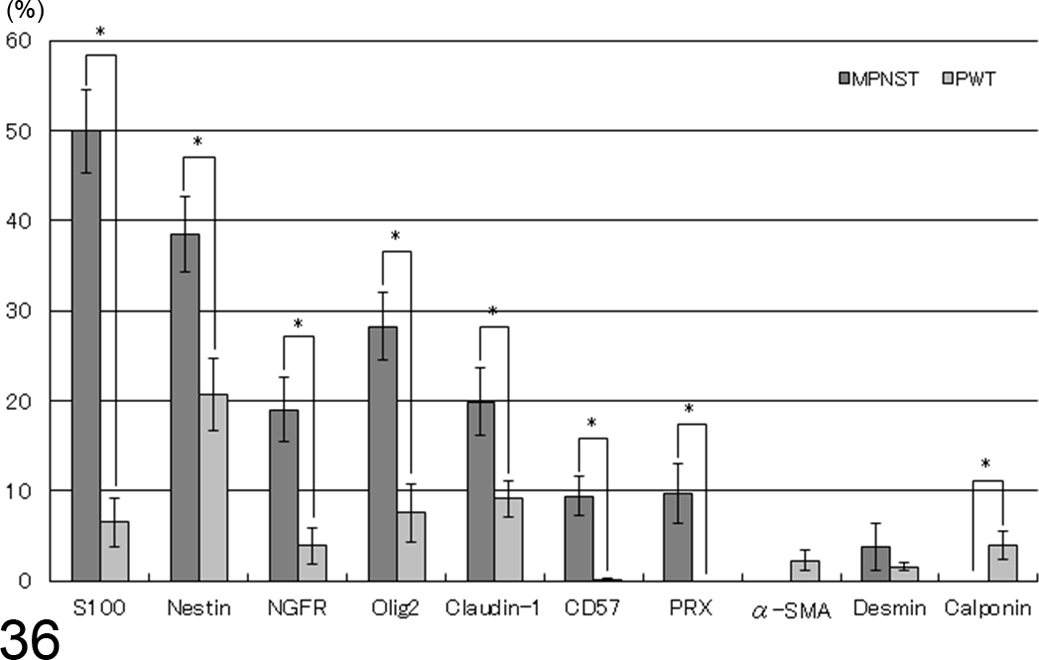
Mean percentages of immunopositive neoplastic cells in malignant peripheral nerve sheath tumors (MPNSTs) and perivascular wall tumors (PWTs). The MPNSTs displayed significantly higher percentages of immunopositive cells than did PWTs for almost all markers except α-SMA and desmin (mean ± SE). *Statistically significant (P < .05).
Cluster Analyses
In the cluster analysis, the PNS and non-PNS MPNSTs were not separated into 2 different clusters (Fig. 37). On the other hand, except for the 9 cases described below, the MPNSTs and PWTs were separated into 2 distinctly different clusters (Fig. 38). Three MPNST cases (Nos. 17–19) were sorted into the PWT cluster. These 3 MPNST cases occurred in the brachial or femoral region and were negative for almost all antibodies. No. 17 was weakly positive for S100 and moderately positive for nestin. No. 18 was moderately positive for nestin only. No. 19 was weakly positive for S100 and claudin-1 and moderately positive for nestin. Six PWT cases (Nos. 33, 35, 42, 56, 57, and 59) were assigned to the MPNST cluster. All of these tumors occurred in the forelimb or hindlimb, and all were positive for S100, nestin, NGFR, Olig2, and/or claudin-1 and negative for α-SMA, desmin, and calponin.

Cluster analysis between malignant peripheral nerve sheath tumor (MPNST) tumor locations. A dendrogram constructed using the Ward method demonstrates the relationship between MPNST tumor locations examined in the present study. Within MPNST tumor locations, cluster analysis did not sort them into 2 distinct groups.
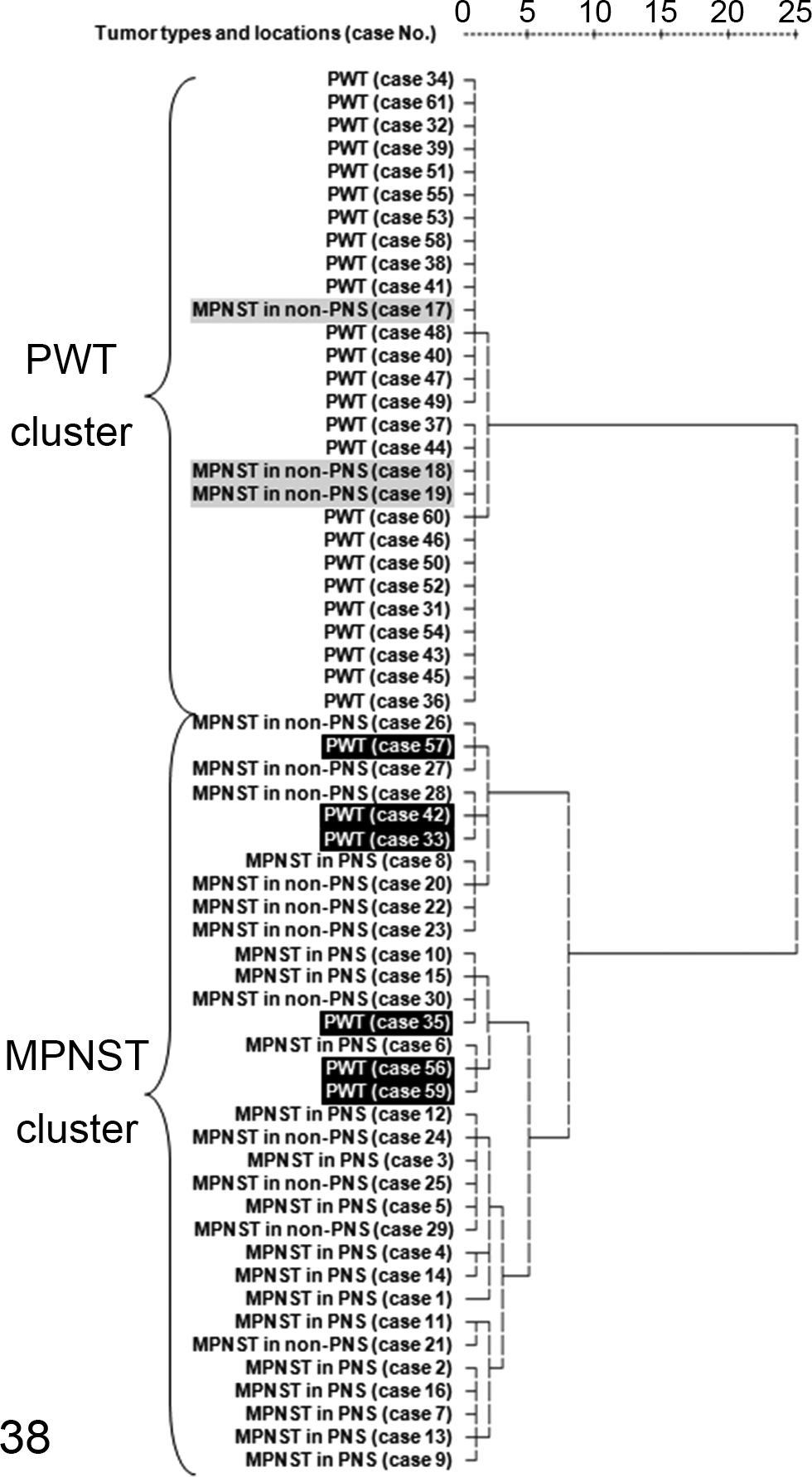
Cluster analysis between malignant peripheral nerve sheath tumors (MPNSTs) and perivascular wall tumors (PWTs). A dendrogram constructed using the Ward method demonstrates the relationship between MPNSTs and PWTs examined in the present study. MPNSTs and PWTs were sorted into 2 distinct groups. Three non-PNS MPNST cases (Nos. 17–19: gray shaded cases) were sorted into the PWT cluster, whereas 6 PWT cases (Nos. 33, 35, 42, 56, 57, and 59: black shaded cases) were assigned to the MPNST cluster.
Discussion
S100 and claudin-1 are markers of Schwann cells and perineurial cells, respectively. 10,35,42,45 Thus, the fact that we detected S100 and claudin-1 in canine MPNST cells indicates that neoplastic cells have a propensity to differentiate into Schwann cells and/or perineurial cells. Nestin has been used as a marker of neuroectodermal stem cells and cancer stem cells in human medicine. 35,36 Therefore, the detection of nestin expression in MPNST cells in the present study suggests that neural crest stem cells and/or cancer stem cell–like cells exist in canine MPNSTs. NGFR has been used as a Schwann cell differentiation marker 4,25 and a marker of neural crest progenitor cells or stem cells. 8,36 In 2 previous reports examining NGFR expression in MPNSTs, 6,14 10 of 10 human and 7 of 11 canine MPNSTs were NGFR positive. In the present study, 21 of 30 (70.0%) MPNSTs were NGFR positive, suggesting that undifferentiated Schwann cells and/or neural crest stem cells are present in canine MPNSTs as one of their components. Olig2 is a marker of the oligodendroglial lineage and some central nervous system progenitors. 3 Olig2 is expressed in normal human oligodendrocytes and oligodendroglial tumor cells but not in normal human Schwann cells and schwannoma cells. 47 On the other hand, to our knowledge, the expression of Olig2 has never been investigated in normal canine Schwann cells or MPNSTs. In the present study, most of the canine MPNSTs (27/30; 90.0%) and several PWTs (6/31; 19.4%) possessed Olig2-positive tumor cells. These results suggest that Olig2 is a relatively useful marker for distinguishing MPNSTs from PWTs. CD57 is a cell type–specific marker for human Schwann cells, 4,45 and PRX has been used as a diagnostic marker for devil facial tumor disease in the Tasmanian devil (Sarcophilus harrisii), 43 which has been confirmed to originate from the Schwann cell. Their expression has been observed in myelinating Schwann cells in previous studies with dogs and Sprague-Dawley rats. 4,32 However, their expression has not been investigated in canine MPNSTs. In this study, half of the MPNST cases expressed CD57 (18/30; 60.0%) and/or PRX (12/30; 40.0%). The intensity was low or moderate. These results suggest that the degree of differentiation of canine MPNST cells into myelinating Schwann cells is low. α-SMA and calponin are smooth muscle–specific antibodies. Desmin is a striated muscle–specific antibody. These antibodies have been used to subclassify PWTs in recent studies. 1,6,16 In the present study, no MPNST cells were positive for α-SMA and calponin, but only 2 cases (Nos. 10 and 20) were positive for desmin. These results suggest that MPNSTs do not differentiate to smooth muscle, but several MPNSTs differentiate to striated muscle as well as triton tumors in humans. 45 On the other hand, in the present study, only a few PWTs expressed these markers. With these results and the expression of claudin-1, it is suggested that these cases include hemangiopericytomas (Nos. 34 and 44), myopericytoma (No. 43), angioleiomyosarcoma (No. 51), and angiofibroma (Nos. 32, 39, 47, 48, 60, and 61). Fifteen cases should be classified as PWTs of uncertain or undifferentiated classification because Nos. 31, 38, 46, and 52 were positive for only claudin-1; Nos. 36, 49, 53, and 54 were positive for claudin-1 and desmin; Nos. 37 and 50 were positive for claudin-1, desmin, and calponin; No. 45 was positive for claudin-1 and calponin; Nos. 40 and 41 were positive for claudin-1 and α-SMA; No. 58 was positive for only desmin; and No. 55 was positive for only α-SMA.
The results of Pearson’s correlation coefficients between each antibody within MPNSTs are considered due to the Schwannian differentiation and the similarity of antigen (both CD57 and PRX recognize myelin), and the results within PWTs are considered due to the existence of MPNSTs misdiagnosed as PWTs.
Diagnosing canine non-PNS MPNST is challenging without the proof of peripheral nerve sheath origin due to not well-established diagnostic criteria. Thus, the immunohistochemical features of non-PNS MPNSTs should be confirmed based on those of PNS MPNSTs. In the present case, the canine MPNSTs that arose in the PNS displayed significantly higher expression levels of S100 and Olig2 than the non-PNS canine MPNSTs. The immunoreactivity levels of the other markers did not differ significantly between the PNS and non-PNS canine MPNSTs. Furthermore, cluster analysis revealed that the PNS and non-PNS MPNSTs were not sorted into 2 different clusters. These findings suggest that PNS and non-PNS canine MPNSTs display similar immunohistochemical and morphological features, and the same diagnostic criteria as for human MPNSTs are applicable regardless of their location. When it comes to distinguishing MPNSTs and other spindle cell tumors, especially PWTs, it is still difficult to do so with only morphological features. It is very important to consider the morphological and immunohistochemical features based on those of PNS MPNSTs. There are only few studies on the distinction between MPNSTs and PWTs. 6,16 In the present study, immunohistochemistry using neural and muscular markers demonstrated useful markers for distinction between MPNSTs and PWTs. The results revealed that the MPNSTs displayed significantly higher numbers of immunopositive cells than the PWTs for almost all markers except α-SMA and desmin. Furthermore, cluster analysis sorted the MPNSTs and PWTs into 2 distinct clusters. However, 3 non-PNS MPNSTs were sorted into the PWT cluster, and 6 PWT cases that expressed NGFR and/or Olig2 were assigned to the MPNST cluster. These 3 MPNST cases should be considered undifferentiated PWT, while the 6 PWT cases should be considered MPNSTs that arose in non-PNS tissue because of their immunohistochemical features. The above results suggest that diagnosing non-PNS MPNST and PWT with only HE-stained sections sometimes results in errors in diagnosis. Furthermore, the fact that PWT cases assigned into the MPNST cluster expressed NGFR and/or Olig2 and S100, nestin, and claudin-1 were positive in several or many PWT cases suggests that NGFR and Olig2 are the most useful markers to distinguish these 2 tumors immunohistochemically.
To develop novel strategies for the treatment of MPNSTs and PWTs such as molecular targeting therapies, it is very important to confirm the origins of these tumors and to study the cellular signaling pathways involved in their proliferation and invasion. 5,35 The expression levels of the neural crest stem cell markers nestin and NGFR observed in the present study suggest that canine MPNSTs contain neural crest stem cells or cancer stem–like cells, which might be useful treatment targets. Classifying MPNSTs and PWTs as “soft tissue sarcomas” together with other spindle cell tumors that arise in soft tissue will prevent treatments for MPNSTs and PWTs from being developed and, hence, their prognosis will never improve. Further studies are necessary to aid the development of novel treatment strategies for these tumors.
Footnotes
Acknowledgements
We thank Animal Clinic Kobayashi, Ishikawa Animal Hospital, Japan Animal Referral Medical Center, Kudo Animal Hospital, Ozawa Animal Hospital, Sanritsu Zelkova Veterinary Laboratory, Tajika Animal Hospital, Tamura Animal Hospital, Togasaki Animal Hospital, Umino-Nakamichi Animal Hospital, and the Veterinary Medical Center of the University of Tokyo for their cooperation with the sample collection.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
