Abstract
A coronary artery perforation is a rare, but potentially lethal, complication of percutaneous coronary intervention. We present a case of massive main vessel coronary perforation of the right coronary artery in a patient with acute ST segment elevation myocardial infarction, which was successfully treated with a second drug-eluting stent. This uncommon therapeutic approach was used to preserve flow to the large side branch. Early recognition, rapid balloon re-inflation at the perforation site and a “ping-pong” guiding technique allowed us to prepare the optimal strategy and to treat the perforation without developing cardiac tamponade.
Keywords
Introduction
A coronary artery perforation (CAP) is a rare, but potentially lethal, complication of percutaneous coronary intervention. CAP has an estimated incidence of 0.5% 1 and it is conventionally classified into three types on the basis of its severity (Ellis classification). 2 The treatment approach of CAP is different between main vessel perforation and distal vessel perforation. 1 We present a case of massive CAP (Ellis type III) in a patient with acute ST segment elevation myocardial infarction. CAP was successfully treated with the second drug-eluting stent (DES) strategy.
Case report
A woman in her late 50s without any relevant medical history was admitted to our department for acute inferior ST segment elevation myocardial infarction. Coronary angiography showed an acute thrombotic lesion of the right coronary artery (RCA) with positive artery remodeling and thrombolysis in myocardial infarction (TIMI) 2 flow (Figure 1).

Coronary angiography of the right coronary artery shows an acute thrombotic lesion at the border of the proximal and middle segments of the right coronary artery.
Direct implantation of the Synergy DES (4 × 32 mm; Boston Scientific Corporation, Marlborough, MA, USA) was performed, and the stent was post-dilatated with the non-compliant NC Sprinter balloon (5 × 15 mm; Medtronic, Minneapolis, MN, USA) at 16 atm. During post-dilatation, the patient complained of intense sharp chest pain. A control angiography showed contrast streaming in the post-dilatated segment of the RCA (Ellis type III CAP) (Figure 2). The balloon was immediately positioned at the perforation site and re-inflated. Bedside transthoracic echocardiography showed only a small separation of the pericardium without any signs of cardiac tamponade physiology. Prolonged balloon inflation was complicated by third degree atrioventricular block with hypotension and ST segment elevation. This situation was managed with a combination of intravenous fluid, atropine and low-dose norepinephrine, and was well tolerated. After 15 minutes of balloon inflation, angiography showed persistent contrast extravasation. Therefore, the balloon was re-inflated again, and we secured a second femoral access. The large dominant right ventricular branch in close proximity to the perforation site was at risk of closure if we decided to use a polytetrafluoroethylene (PTFE)-covered stent. Therefore, we decided to use a second DES instead. The RCA was intubated with another guiding catheter, which was introduced with the “ping-pong” technique 1 (Figure 3). This technique is used to facilitate the delivery of a PTFE-covered stent. In in our case, this technique was used to facilitate delivering a second DES, while minimizing the time that blood traveled from the perforation site to the pericardium, thus maintaining hemodynamic stability. A second Synergy Megatron DES (4 × 16 mm; Boston Scientific Corporation) (14 atm) was then implanted at the perforation site, and the balloon was re-inflated. After 5 minutes, control angiography showed that the extravasation had ceased (Figure 4) with TIMI 3 flow in all branches. The balloon deflation was then followed by prompt hemodynamic improvement, and the resolution of atrioventricular block and ST segment elevation. After extraction of all balloons, guidewires and one of the two guiding catheters, we reversed unfractionated heparin with protamine. Repeated transthoracic echocardiography was performed without any progression of pericardial effusion and with preserved systolic function of both ventricles.
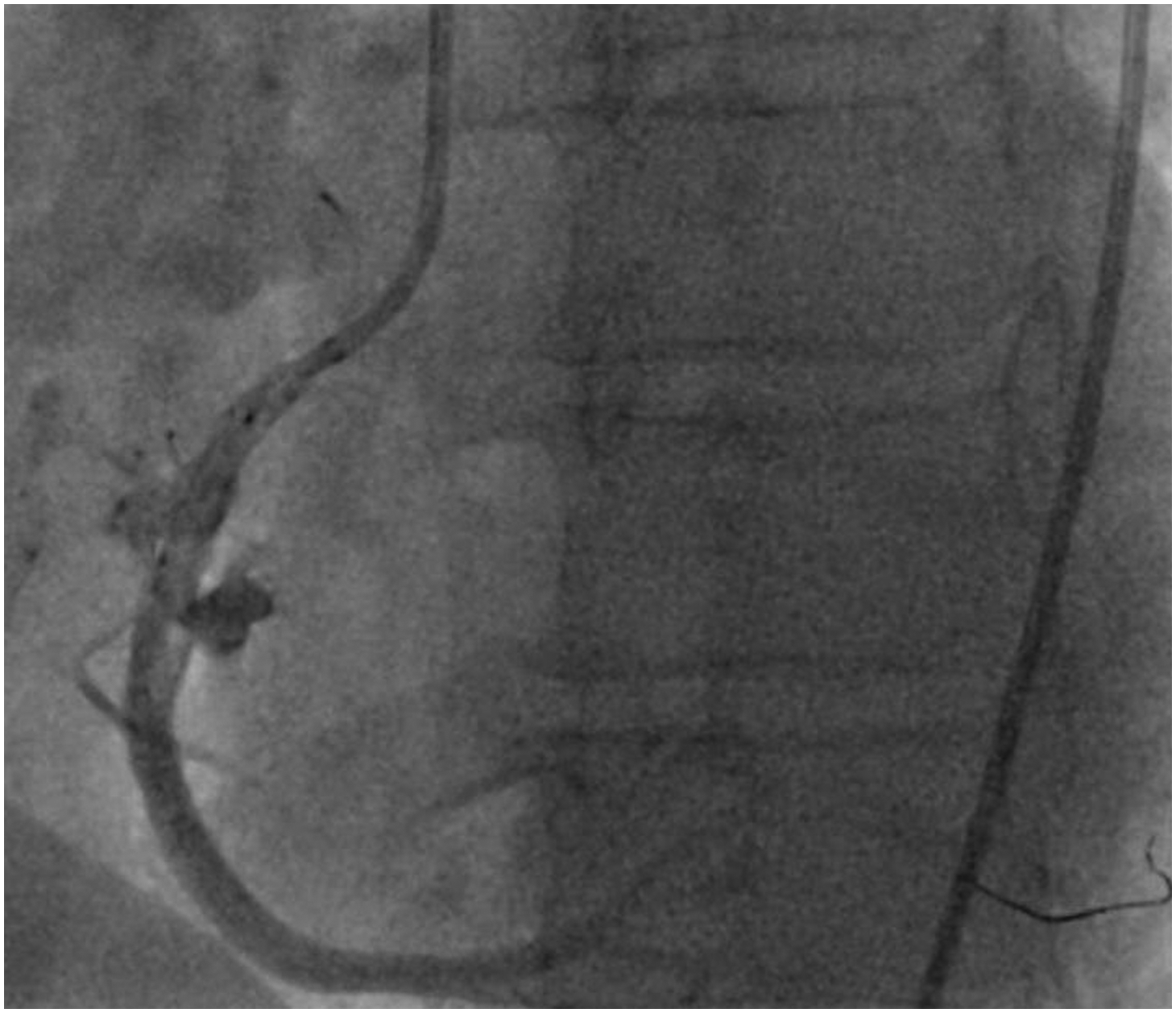
Coronary angiography of the right coronary artery shows contrast streaming in the post-dilatated segment (coronary artery perforation Ellis type III) with the balloon left in position.

Coronary angiography of the right coronary artery showing the ping-pong technique. This strategy involves intubation of an affected vessel with another guiding catheter with simultaneous slight dislocation of the original catheter. A guidewire from the second guide catheter is introduced into the coronary vessel, and the angioplasty balloon is temporarily deflated to allow distal passage. The polytetrafluoroethylene-covered stent/drug-eluting stent is then quickly advanced across the perforation and is deployed following the removal of the angioplasty balloon.
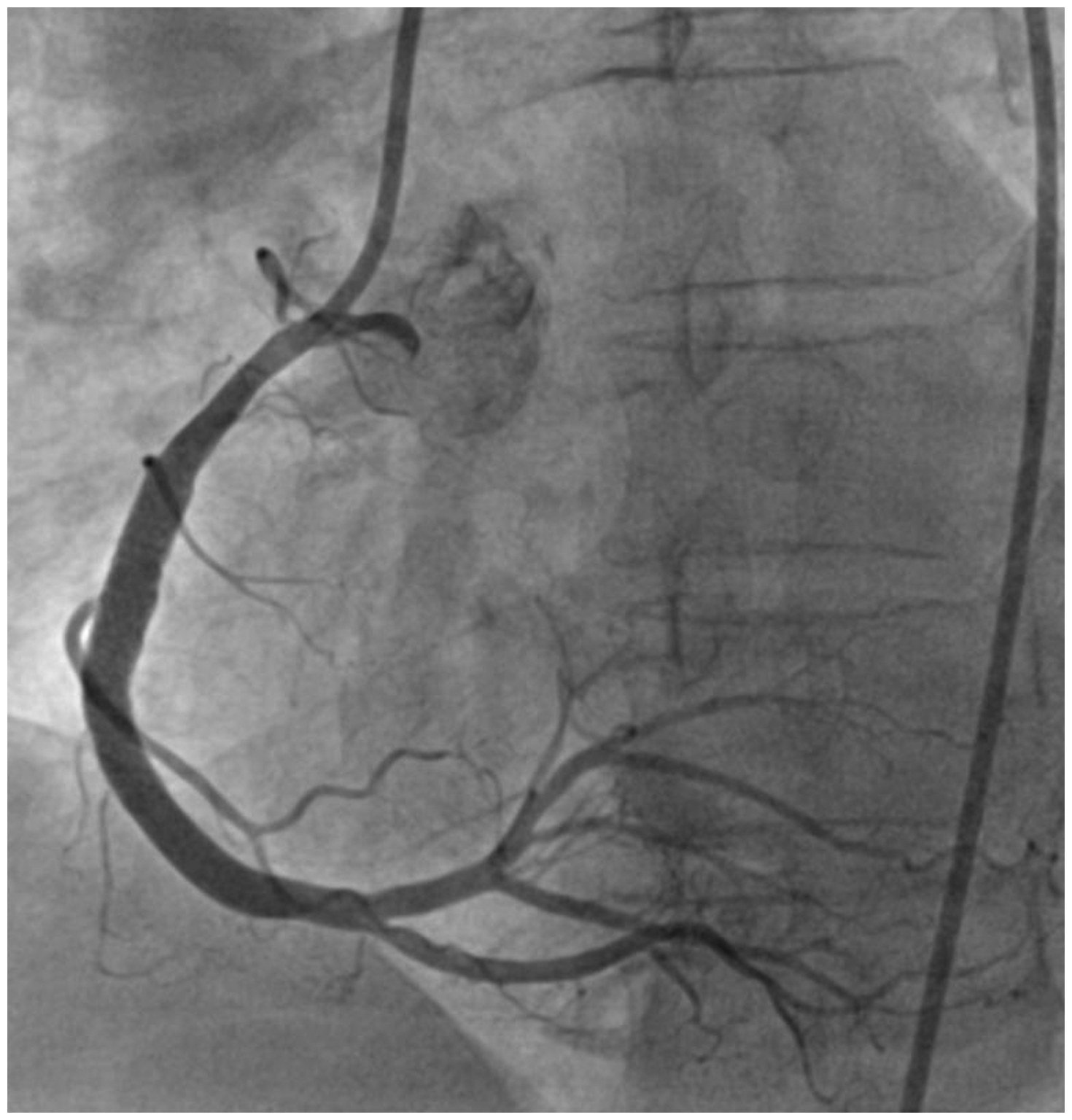
Coronary angiography of the right coronary artery shows that extravasation has ceased, and flow to the large dominant right ventricular branch is preserved after implantation of a second drug-eluting stent.
The patient was discharged home after 5 days. Early follow-up showed no progression on transthoracic echocardiography, and the patient was free of any symptoms. The reporting of this study conforms to the CARE guidelines. 3 All of the patient’s information was de-identified, and the patient signed informed consent for the procedure.
Discussion
A main vessel CAP is most commonly caused by balloon/stent oversizing or when high deployment/post-dilatation pressure is used. This is in contrast to distal vessel perforation where the most common cause of CAP is inadvertent coronary guidewire migration. These differences in the location and etiology of CAP determine the specific therapeutic approach. The most common strategies for CAP are the implantation of a PTFE-covered stent for proximal main vessel perforations and distal embolization for peripheral perforations. 1
The likely cause of CAP in our case was post-dilatation balloon oversizing (5 mm) in a mildly calcified RCA with positive remodeling. This situation could probably have been prevented by intravascular coronary imaging before stent deployment or before stent post-dilatation. CAP is often associated with sudden onset of acute intense sharp chest pain, 1 and this should always raise suspicion of CAP. Immediate balloon re-inflation and the ping-pong guiding technique played an important role in reducing the streaming time of blood to the pericardium and prevented the development of cardiac tamponade, which is associated with a higher mortality. 4 Even though prolonged balloon inflation was associated with new onset of third degree atrioventricular block and hypotension, it allowed us time to prepare our next strategy.
Perforations of the proximal main vessel can be effectively treated with PTFE-covered stents, but not at bifurcation sites. The implantation of a PTFE-covered stent (Papyrus, Biotronik, Lake Oswego, OR, USA) in our case would have been associated with a risk of right ventricle infarction and insufficient apposition of the PTFE stent (the largest Papyrus stent that we had was 4 mm in diameter with a maximum stent expansion diameter of 4.65 mm). PTFE-covered stents also have a higher risk of stent restenosis and thrombosis, and have a poor long-term outcome.4,5 Therefore, we decided to implant another DES. We chose the Synergy Megatron because it has the highest strut density among the stents available for our use, and it has optimized and uniform scaffolding at larger diameters, with the highest radial and axial strength (enabled by a 12-peak design). If the rescue “second DES strategy” had failed, we would have performed PTFE-covered stent implantation. If PTFE-covered stent implantation had also failed, we would have had to transfer the patient for acute surgery.
The second DES strategy for treating CAP of the main vessel is uncommon, mainly because of good immediate results of PTFE-covered stents. According to a recent Dr. Johnson’s Twitter survey, only less than 1% of physicians would use the second DES strategy to treat CAP of the proximal main vessel. 6 Our case indicates the feasibility of this strategy in a specific scenario, but another plan is required if this strategy fails.
Conclusion
The implantation of a second DES may lead to successful treatment of a massive CAP. The selection of a second DES based on its specific structure may play a role in the result of this strategy. This uncommon therapeutic approach was used to preserve flow to the side branch in our case. Early suspicion and recognition, rapid balloon re-inflation at the perforation site and the ping-pong guiding technique allowed us to prepare the best strategy and to treat the perforation without developing cardiac tamponade.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605231174998 - Supplemental material for Coronary artery perforation successfully treated with a second drug-eluting stent
Supplemental material, sj-pdf-1-imr-10.1177_03000605231174998 for Coronary artery perforation successfully treated with a second drug-eluting stent by Matej Strycek, Lukas Jaworski, Rostislav Polasek and Pavol Tomasov in Journal of International Medical Research
Footnotes
Author contributions
Writing (original draft, review & editing): Matej Strycek; visualization and conceptualization: Lukas Jaworski and Pavol Tomasov; supervision: Pavol Tomasov and Rostislav Polasek. All authors discussed the results and contributed to the final manuscript.
Data availability statement
No datasets were generated or analyzed during the current study.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics statement
This case report did not require approval by the ethics committee at our institution. Verbal informed consent for publication was obtained from the patient.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
