Abstract
Objective
Femoral neck fractures are common. We evaluated the biomechanical performance of an internal fixation method based on traditional three cannulated screws (3CS) inserted from below the fracture in the direction of the calcar femorale in the treatment of Pauwels III femoral neck fracture.
Methods
We constructed and evaluated a three-dimensional model of a Pauwels III femoral neck fracture with four models of internal fixation (3CS, and 150°, 155°, and 160° nailing angles) for reconstruction of the calcar femorale, by finite element analysis (FEA).
Results
The peak stress values at the fracture ends in the 3CS, 150°, 155°, and 160° nailing angle models were 30.052 MPa, 33.382 MPa, 34.012 MPa, and 29.858 MPa; peak stress values for internal fixed stress were 315.121 MPa, 228.819 MPa, 198.173 MPa, and 208.798 MPa; and the maximum displacement of the femoral head was 13.190 mm, 13.183 mm, 12.443 mm, and 12.896 mm, respectively.
Conclusion
FEA showed that the new nailing methods and the 160° nailing angle for reconstruction of the calcar femorale showed better performance in resisting shearing force for Pauwels III femoral neck fracture, with better mechanical properties, than those with the other three models. These findings can provide a clinical reference.
Keywords
Introduction
Femoral neck fractures are a common fracture, accounting for 54% of all hip fractures. 1 With increased population aging, the incidence of femoral neck fractures is increasing annually.2–3 Femoral neck fractures are not common among young people. However, high numbers of people suffer high-energy injuries; therefore, the incidence of femoral neck fractures in young people is also increasing. 4
In Pauwels type I, II, or II femoral neck fractures, a small part of the calcar femorale at the femoral neck is damaged. 5 The calcar femorale is a supporting structure to the femoral neck that transfers stress from the trabecular bone of the femur and neck to the femoral shaft. 6 The calcar femorale plays an important role in the load distribution of the proximal femur as well as providing mechanical support. 7 Therefore, the mechanical restoration of this structure is of great importance in the treatment of femoral neck fractures. However, the reconstructive restoration of the calcar femorale is often overlooked in the treatment of femoral neck fractures, and the optimal surgical treatment option remains controversial. 8 In this study, we used finite element methods, which few investigators have used, to study the biomechanical properties of structural reconstruction of the calcar femorale in femoral neck fractures.
The three cannulated screws (3CS) nailing approach is a common clinical method of internal fixation for femoral neck fractures. 9 As part of the anatomical structure of the proximal end of the femoral neck, the calcar femorale is located at the junction of the femoral neck and the femoral shaft. On the posteromedial side of the junction, the calcar femorale extends from the posterior femoral neck to the posterior lesser trochanter, which is roughly located at an angle of 155° with the inner and distal femoral shaft axes. In this study, based on the position of the calcar femorale, three calcar femorale reconstruction nail angles, 150°, 155°, and 160°, were designed to simulate the femoral calcar structure. Based on the 3CS nailing approach, we designed three nailing approaches and models by placing the screws below the fracture using 150°, 155°, and 160° nailing angles for the reconstruction of the calcar femorale. To explore whether good biomechanical properties can be achieved with 3CS in calcar femorale reconstruction nailing, we analyzed the von Mises stress (VMS) and displacement with the three new nailing approaches in repairing Pauwels type III femoral neck fractures, by finite element analysis (FEA). Additionally, we set a control group using the 3CS method. Using the FEA results, we evaluated whether better biomechanical performance can be achieved with the placement of a structural reconstruction screw in the calcar femorale compared with 3CS, and we provide a theoretical basis and reference for the clinical treatment of femoral neck fractures.
Materials and methods
Establishment of the femoral fracture and internal fixation models
This study was approved by the Institutional Review Board (IRB) of Tianjin Hospital, and the volunteer provided written informed consent for the publication of the data derived from his images, and the clinical images. A healthy volunteer was selected for this study. The inclusion criteria were: no hip osteoarthritis, no diffuse hip pain, no cartilage damage on the femoral head, no ligament instability, and no history of lower limb fracture. The lower limbs were scanned using 64-row spiral computed tomography (CT). The scanning parameters were set as follows: voltage: 120 kV, current: 150 mA, and layer thickness: 0.625 mm. Digital imaging and communications in medicine (DICOM) data were obtained. The DICOM format data were imported into Mimics software, version 17.0 (Materialise, Leuven, Belgium) to extract the femoral image. We then optimized the quality of the femoral image to obtain the femur model and exported the STereoliLhography (STL) format file. The STL format file was imported into Geomagic Studio 2014 (SculptCAD, Dallas, TX, USA), and the model was repaired. We constructed surface patches and fit surfaces, fit the femur into the non-uniform rational basis spline (NURBS) surfaces, and saved the file in initial graphics exchange (IGS) format. We then imported the above-fitted surface into SolidWorks 2017 (Dassault Systemes SolidWorks Corp., Waltham, MA, USA), used the stitching function under the combination command to sew the model into a solid, and exported and saved the file in IGS format (Figure 1a).
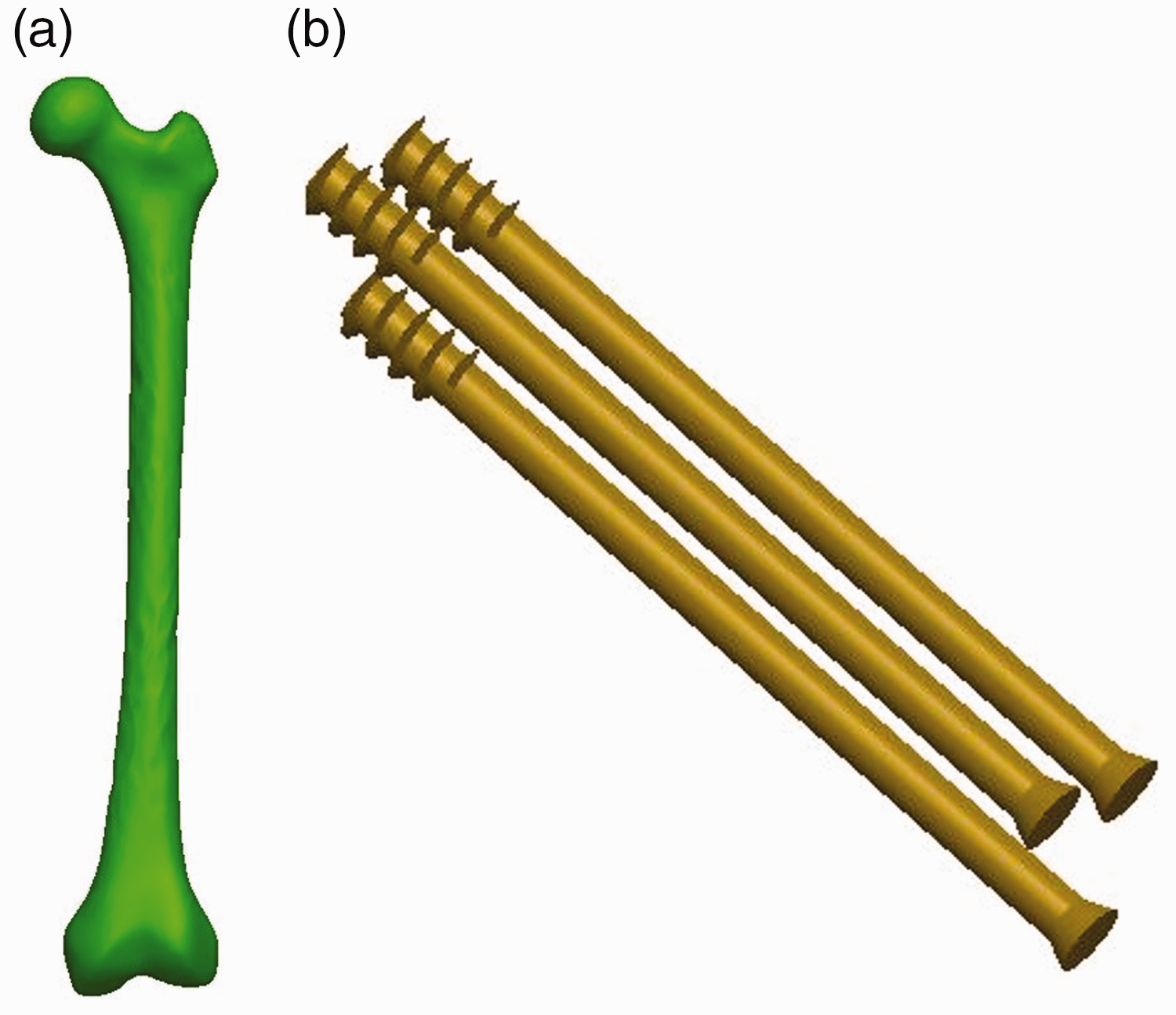
Constructing the finite element model: (a) three-dimensional model of the femur and (b) three-dimensional model of internal fixation.
SolidWorks three-dimensional software was used for modeling various types of internal fixation (3CS, and 150°, 155°, and 160° nailing angles) for reconstruction of the calcar femorale). In accordance with the cannulated screw parameters given by DePuy Synthes (West Chester, PA, USA), the diameter of the threaded part of the screws was 7.3 mm, the length was 16 mm, and the diameter of the non-threaded part was 4.8 mm (Figure 1b). The models were saved in SolidWorks part (SLDPRT) format.
Model assembly and fracture modeling
Based on the screw placement principle of an inverted triangle, 4 all screw tips should be placed within 5 mm of the femoral head subchondral bone, the inferior screw should be within 5 mm of the calcar subcortical bone, and the posterosuperior screw should be within 5 mm of the posterior subcortical bone. The different types of screws were placed in the bone model using SolidWorks software (Figure 2). Then, the internal fixation and femur images were saved in IGS format. Next, we imported the femur model into HyperMesh software, version 13.0 (Altair Engineering, Ltd., Troy, MI, USA) and drew the fracture line with a Pauwels angle of 70° to simulate a Pauwels type III fracture. The internal fixation files were also imported into the software. Finally, the bone model was meshed (Figure 3). To ensure that the calculation accuracy met the requirements of analysis, the mesh type and mesh size were controlled, with the mesh typeset as a hexahedral mesh, and the mesh size set as 2 mm (Table 1). The models were saved in input (INP) format.

Model of a femoral neck fracture treated with internal fixation for the reconstruction of the calcar femorale in each of the four models: (a) three cannulated screws (3CS); (b) 150° nailing angle; (c) 155° nailing angle and (d) 160° nailing angle.

Mesh generation in the finite element model.
The number of nodes and elements in the finite element model.

FE, finite element; 3CS: three cannulated screws.
Boundary conditions and loads
The meshed model was imported into Abaqus software, version 6.14 (Dassault Systèmes Simulia Corp., Providence, RI, USA), with the femur adopting the equivalent homogeneous material. The material properties for each component are shown in Table 2. Next, we set the interaction. In the fracture model, we simulated a complete fracture of the femoral neck, and the fracture surface remained in full contact after reduction. The contact condition of the two ends of the fracture was set as friction, with a friction coefficient of 0.2 and the contact relationship between the femur and the cannulated screw set as binding. 4 We then applied the load. In accordance with the results reported by Van Houcke et al., 10 when a person stood on one leg, the force on the hip joint was 3.3 times their body weight, and the applied force was 2100 N. We selected a certain range of nodes on the distal femur, and the degrees of freedom constraining its XYZ direction was 0, as shown in Figure 4. After selecting the settings, we submitted the operation for FEA.
Material properties used in the finite element models.


Finite element model setup: (a) interaction settings for the three-dimensional (3D) model and (b) constraint and load settings for the 3D model.
Evaluation Index
To evaluate the different methods of calcar femorale reconstruction for femoral neck fractures under mechanical loading conditions, we focused on the following variables: (1) VMS peak and distribution at the fracture ends; (2) VMS peak and distribution of the femur; (3) VMS peak and distribution of the internal fixation; and (4) displacement distribution and peak values of the femoral head and internal fixation.
Results
Volunteer characteristic
A male volunteer, aged 58 years, height: 172 cm, and weight: 64 kg, was selected in accordance with the inclusion criteria. The volunteer had normal femoral anatomy and could represent healthy adults. The femoral neck shaft angle was 125°, and the femoral neck angle was 13°.

Stress distribution cloud map of the fractured bone ends in the finite element model of the reconstruction of the calcar femorale: (a) three cannulated screws (3CS); (b) 150° nailing angle; (c) 155° nailing angle and (d) 160° nailing angle.
VMS distribution and peak stress at the fracture ends
Based on the stress cloud, we found that the stresses were mainly concentrated at the intersection of the internal fixation and the fracture surface, with the stress concentration below the femoral neck significantly higher than that above the femoral neck. The peak stress was 30.052 MPa in the 3CS model, and 33.382 MPa, 34.012 MPa, and 29.858 MPa in the 150°, 155°, and 160° nailing angle models, respectively, of the reconstruction of the calcar femorale (Figure 5).
VMS distribution and peak stress in the femur
Regarding the stress distribution cloud of the femur (Figure 6a–d), the stress was mainly distributed at the femoral neck and the femoral shaft. The stresses at the femoral neck were concentrated at the fracture point and near the lesser trochanter. The stress distribution was more concentrated below the fracture surface of the femoral neck than that above the fracture surface. In the femoral shaft, the stresses were mainly concentrated on the pressure and tension sides, with the stress distribution more intensive on the pressure side than that on the tension side.On the lateral cortex around the distal screw, the stress was mainly concentrated on the pressure side of the femoral shaft and at the junction between the screw tip and the femoral shaft cortex. The peak stress on the femur in the 3CS group was 106.605 MPa, and that of the 150°, 155°, and 160° nailing angles for the reconstruction of the calcar femorale were 87.317 MPa, 147.691 MPa, and 102.072 MPa, respectively. The peak stress with the 155° nailing angle was significantly higher than those for the other three methods.
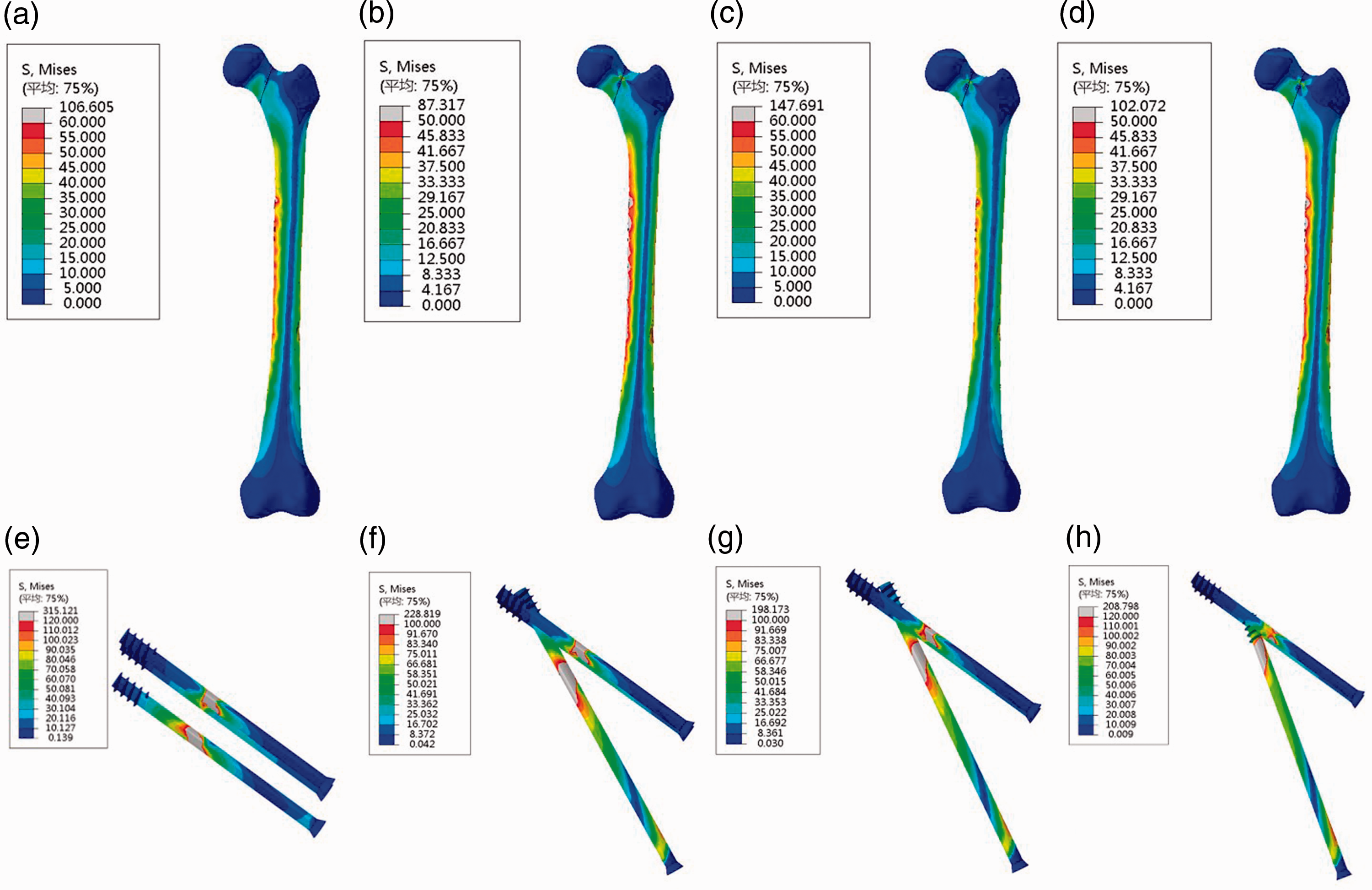
Finite element stress cloud map of the femur and internal fixation: (a–d) stress distribution cloud map of the femur and (e–h) stress distribution cloud map of the internal fixation.
VMS distribution and peak stress of the internal fixation
In the 3CS model, the stresses were mainly distributed at the intersection of the internal fixation and the fracture surface. In the other three models, the stresses were mainly distributed at three locations: the intersection of the internal fixation and the fracture surface, the threads of the screw in the reconstructed calcar femorale, and the intersection of the tip of the screw with the femur (Figure 6e–h). The peak internal fixed stresses for the four models were 315.121 MPa, 228.819 MPa, 198.173 MPa, and 208.798 MPa (3CS, 150°, 155°, 160° nailing angles, respectively).
Displacement distribution of the femur and internal fixation
Fixing the distal end of the femur and applying a downward concentrated force at the femoral head displaced the femoral head and the internal fixation downward. As seen in the displacement cloud map (Figure 6), the maximum displacement of the femur occurred at the tip of the femoral head and decreased gradually toward the distal femur (Figure 7a–d). Additionally, the maximum displacement of the internal fixation occurred at the screw threads and decreased gradually toward the tip of the screw (Figure 7e–h). The peak displacements of the femur in the four models were 13.190 mm, 13.183 mm, 12.443 mm, and 12.896 mm (3CS, 150°, 155°, 160° nailing angles, respectively). The peak displacements of the internal fixation in the four models were 12.646 mm, 12.625 mm, 11.932 mm, and 12.347 mm (3CS, 150°, 155°, 160° angles, respectively). The displacement peaks did not differ greatly between the models.

Finite element displacement distribution cloud map of the femur and internal fixation: (a–d) displacement distribution cloud map of the femur; (e–h) displacement distribution cloud map of the internal fixation.
Discussion
In this study, we used a computer simulation finite element method to investigate whether the use of a reconstructive nailing approach for the treatment of Pauwels III femoral neck fractures was superior to the commonly used traditional 3CS nailing approach. We also investigated which nailing angles could be used to achieve better biomechanical performance. The results of the displacement distributions of the four models showed that the new nailing methods provided better results and greater shear resistance than those with the traditional 3CS nailing method. The results of the analysis of the internal fixation stresses in the four models also showed that the three models with the new structure outperformed the results obtained with the traditional 3CS nailing approach, resulting in a more mechanically stable structure of the femur and a lower risk of internal fixation fracture.
As mentioned above, the optimal surgical treatment option for femoral neck fractures remains controversial. 8 Nakanishi et al 11 reported that the position of screw placement relative to the position of the femoral shaft had an effect on the outcome of femoral neck fracture treatment. Filipov et al. 12 described the use of a novel biplane double-supported screw fixation method comprising three cannulated screws that are bifurcated in the middle, two of which are fixed to the calcar femorale. By providing additional cortical support, this method improves the strength of femoral neck fracture fixation. A biomechanical study by Kauffman et al 13 on femoral neck fractures with calcar femorale disruption showed that femoral neck fractures fixed with four cannulated screws were mechanically stronger and more stable than those fixed with three screws. Khoo et al. 14 retrospectively analyzed 53 patients with femoral neck fractures fixed with cannulated screws and found that structural destruction of the calcar femorale significantly affected the incidence of femoral head necrosis. The treatment of femoral neck fractures with internal fixation is ideal to restore the function of the hip joint and provide good biomechanical properties and minimize complications, such as femoral neck shortening, femoral head necrosis, and non-union. However, to achieve these results, the structural design of the internal fixation and the nail placement must be reasonable, able to resist shear stress, maintain a certain compression force, and promote fracture healing. Additionally, the choice of internal fixation must consider the need to minimize soft tissue injuries and intraoperative bleeding, and be associated with a short operative time, which are currently difficult to achieve. According to Luttrell et al. 15 among the expert opinions of 272 physicians from the Orthopaedic Trauma Association, 43% recommended the use of a cannulated compression screw (CCS) for fixation because of its lower volume in situ, minimal tissue damage and intraoperative bleeding, and ease of surgical operation. In a biomechanical study by Tianye et al. 16 the maximum displacements of the femoral head for the “F”-shaped cannulated screw and the traditional cannulated screw were 1.53 mm and 1.73 mm, respectively, and the peak stresses in the calcar femorale were 115.2 MPa and 143.5 MPa, respectively. The “F”-shaped cannulated screw had better biomechanical properties that those of the cannulated screw. Zhang et al 17 compared screws fixed in the oblique triangle configuration with the traditional inverted equilateral triangle configuration by the finite element method. When the applied load was 2100 N, the peak stresses in the two models were 295.94 MPa and 344.41 MPa, (oblique triangle vs inverted equilateral triangle, respectively). The mechanical properties of the screws fixed in the oblique triangle configuration were better that those with the inverted equilateral triangle configuration. Comparing the results of previous studies 15 with those of our finite element analysis, there was consistency regarding the stress distribution and peak stress of the traditional inverted triangle model. Additionally, the optimized nailing method based on this structure had better mechanical performance than those of the other models, which proved the validity of this study.
Cannulated screws are currently the main surgical approach clinically; however, reoperation is necessary in ≥20% of cases. 18 Therefore, more effective internal fixation methods are worth exploring. Fractures of the femoral neck are often accompanied by disruption of the calcar femorale, which is an important weight-bearing structure in the proximal femur that transfers stress from the femoral head and neck to the femoral shaft.6,19 The destruction of the calcar femorale has a significant impact on the mechanics of the entire hip joint. The degree of displacement and comminution of the calcar femorale affects the outcome of femoral neck fractures, and satisfactory calcar femorale repositioning or reconstruction could reduce complications and improve hip function. The traditional inverted triangular nailing approach does not permit repositioning or reconstructing the damaged calcar femorale, thus failing to achieve excellent biomechanical properties. 4 The calcar femorale is attached to the medial femoral cortex at the junction of the femoral neck and the femoral shaft. In this study, we placed the lower cannulated screw at the calcar femorale position based on the inverted triangular nailing approach to reconstruct the calcar femorale and thus effectively restored the continuity of the medial femoral column.
The cannulated screw was able to transmit the compressive stress generated by body weight to the lateral femoral cortex, enhancing the axial compression resistance of the femoral neck. We used the finite element method to explore the biomechanical properties of the calcar femorale after reconstruction. The experimental results showed that the peak internal fixation stress, peak displacement of the femur, and stress distribution of the three angle models of the calcar femorale reconstruction were better than those of the traditional inverted triangle model (3CS). These results showed that the biomechanical performance of this new internal fixation method was better than that of the traditional inverted triangle method. The peak stress and stress distribution of the fracture ends, femur, and internal fixation were superior when the lower cannulated screw was placed at an angle of 160°, and this method provided superior biomechanical performance compared with the other approaches.
This study had some limitations. First, the effect of soft tissues, such as the muscles and skin around the femur, on the forces on the femur after internal fixation was not considered in this study. Second, the new screw placement method of a 160° nailing angle must be validated in clinical trials. Finally, despite using a finite element method in this study, the constructed model still had some variability compared with the actual femur.
Conclusion
In this study, compared with the conventional inverted triangular nailing approach (3CS) for Pauwels type III femoral neck fractures, in terms of stability, stress distribution, and prevention of hip inversion deformity and femoral neck shortening, the analysis showed that the nailing approach to reconstruction of the calcar femorale had superior biomechanical performance over the traditional 3CS method. Additionally, the mechanical properties were better when the lower cannulated screw was placed at an angle of 160° than those with either of the other two angles. These findings could provide a theoretical basis for the clinical treatment of femoral neck fractures.
Footnotes
Acknowledgements
The authors gratefully acknowledge the support of Professor Xinlong Ma, a member of Tianjin Hospital of Tianjin University.
Author contributions
Z.H.G. and J.X.M. conceived and designed the study, analyzed the data, and wrote the manuscript. Z.H.G. collected the data. Y.W., B.L., H.H.B., L.S., H.Z.J., and Z.J.Z. contributed to the data curation and preparation of the original draft of the manuscript. X.L.M. supervised the study, analyzed the data, and revised the manuscript. All authors read and approved the final manuscript.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Natural Science Foundation of China (11772226).
