Abstract
Objective
Unstable femoral neck fractures are typically high-angled shear fractures caused by high-energy trauma. Internal fixation of femoral neck fractures with placement of parallel cannulated screws in an inverted triangle configuration is commonly performed in the clinical setting. This study was performed to investigate the primary results of intramedullary nailing with cannulated screws for the treatment of unstable femoral neck fractures in young and middle-aged patients.
Methods
In total, 96 consecutive patients with no history of hip surgery using inverted triangular cannulated compression screws or construction nails with cannulated screws were reviewed. Their demographic and radiological data were retrospectively collected from our institutional database.
Results
Inverted cannulated screws had an excellent effect on decreasing the blood loss volume and incision size, but intramedullary nails exhibited superior advantages in decreasing screw exit and shortening the hospital stays. The Harris hip scores were comparable between the two groups.
Conclusions
Intramedullary fixation with cannulated screws has advantages in treating complicated femoral neck fractures. Besides cannulated screws, intramedullary fixation with cannulated screws might be another method to treat unstable femoral neck fractures in young and middle-aged patients.
The study was registered in ClinicalTrials.gov. Unique Protocol ID: 11156458. The ClinicalTrial number is NCT03550079.
Keywords
Introduction
Femoral neck fractures account for 3.6% of all fractures and are the most prevalent injuries among older people with high mortality and morbidity and among young, healthy people who sustain high-energy trauma.1,2 Nonunion and avascular necrosis are the most common complications of femoral neck fractures, especially vertical fractures, and result in loss of labor capacity and death. Treatment is difficult and challenging, and active prevention and appropriate treatment depending on the fracture pattern and patient characteristics must be implemented as early as possible to minimize poor outcomes. However, the currently available treatment options are a topic of great interest and controversy, and they vary substantially from one another depending on the extent of displacement, fracture configuration, physiological age of the patient, bone quality, and other factors. Nonoperative management is not considered in young patients with a high demand for a good prognosis.
Numerous surgical techniques have been reported for stabilization of femoral neck fractures in young patients. 3 Commonly used implants are the proximal femoral locking plate, dynamic condylar screw, dynamic hip screw (DHS), and cannulated screws. Only a few reports have described little change after management of femoral neck fractures with these four strategies.1,4 Most studies suggest that one implant is superior to another. Parker 5 reported that cannulated screws had a weak holding capability compared with other internal fixation devices and might lead to femoral neck shortening and compromised hip function, especially in patients with osteoporosis. The recently introduced method of biplane double-supported screw fixation exhibited improved cortical screw support and increased fixation strength. 6 However, in patients for whom arthroplasty is not the first-choice treatment especially young and middle-aged patients, placement of three parallel cannulated screws in an inverted triangle configuration is an appropriate and effective treatment option.7,8 Through compression of the fracture site, parallel screw fixation facilitates anatomic reduction, rigid internal fixation, and femoral neck fracture healing. The short time of the surgical procedure contributes to its minimal invasiveness, and the blood transfusion rate is low.9,10
A clear consensus that the inverted triangular configuration of cannulated screws helps to prevent complications such as nonunion or refracture has been reached. Because of its superior torsional stability and limited disturbance of the femoral head blood supply, placement of three parallel cannulated compression screws is the most widely used fixation technique for intracapsular femoral neck fractures in young and middle-aged patients. However, for young patients with vertical shear femoral neck fractures, three cannulated screws are not adequate to stabilize the fracture (failure rates range from 30% to 40%), and the essential factor in the treatment of these fractures is stability. 11 Röderer et al. 12 found that proximal femoral nailing antirotation achieves primary stability comparable to the DHS in an unstable medial femoral neck fracture model. However, few studies have revealed the outcomes of intramedullary fixation in treating femoral neck fractures. This study was performed to investigate the outcomes of unstable femoral neck fractures treated with intramedullary fixation with cannulated screws compared with traditional methods.
Materials and methods
Demographic data of patients
From 2016 to 2017, consecutive patients with no history of hip surgery treated with inverted triangular cannulated compression screws or intramedullary reconstruction nails with cannulated screws were reviewed, and their demographic and radiological data were retrospectively collected from our institutional database. All methods were performed in accordance with the relevant guidelines and regulations of the Third Hospital of Hebei Medical University. This retrospective study was conducted in 2018. Patients were contacted by telephone to ensure that they agreed to participate in the study, and informed consent was obtained from all participants or their legal guardians. The patients were classified into the inverted triangular (IT) group and reconstruction nails (RN) group according to the method of internal fixation. The inclusion criteria were a closed femoral neck fracture, no fractures at other sites, surgical treatment with cannulated compression screws or reconstruction nails, and a follow-up time of >1.5 years. The exclusion criteria were the absence of severe cognitive dysfunction, the presence of a pathological femoral neck fracture, a previous femoral neck fracture, treatment with other internal fixation techniques, and surgical treatment with open reduction. The mechanisms of injury were slips, trips, or falls and traffic accidents. This study was approved by the ethics committee of the Third Hospital of Hebei Medical University.
Patients in the IT group were treated with three inverted cannulated compression screws. The patients in the RN group were managed with reconstruction nails (Table 1). All operations were performed by senior orthopedic surgeons in our department. The average time between injury and surgical intervention was 4 days (3–8 days), which was mainly due to a delay in reporting to the hospital or the time taken to examine the patients’ biochemical indices.
General information of the patients with femoral neck fractures.
Data are presented as n or mean ± standard deviation
IT group, inverted triangular group; RN group, reconstruction nails group.
Surgical procedures
All patients were maintained on bed rest until the operation. For closed reduction, the operation was performed under general anesthesia or regional anesthesia. The choice of anesthetic method was decided by the anesthesiologist. The patient was placed in the supine position followed by percutaneous fixation with an inverted configuration of three cannulated screws or reconstruction nails using an image intensifier.
A guide pin was inserted with a lateral entry point located at the median line of the lateral cortex. In the anteroposterior view, the guide pin should be parallel to the neck shaft angle and as close as possible to femoral calcar. In the lateral view, the guide pin should be parallel to the anteversion angle and inserted directly in the center of the femoral neck and head. The head of the guide pin was located 5 mm beneath the surface of the femoral head. Another two or three guide pins were inserted parallel to the long axis of the femoral neck using the same method. The three guide pins formed an inverted triangle. Partial cancellous threaded cannulated compression screws (6.5-mm; Stryker, Kalamazoo, MI, USA) were then inserted along the direction of the guide pins. Each of these screws was placed with two supporting points (pivots) in the distal fragment: the medial supporting point was located on the distal femoral neck cortex, and the lateral supporting point was located at the screw entry point into the lateral diaphyseal cortex. Three were inserted in parallel with the inverted triangular configuration using guide pins, and the distal screw had an additional third medial supporting point on the posterior femoral neck cortex.
The reconstruction nail was inserted using the manufacturer’s aiming device. A 4- to 5-cm longitudinal skin incision was made over the surface of the proximal femur, and the entry was located at the greater trochanter with the help of a bone owl (a device used to open a pathway in bone tissue). Properly sized nails were used. Each nail was introduced with a handle using rotation movements of the wrist. Under image intensifier control, the nail was driven with rotatory movement or with a hammer to the fracture site, which was aligned to an anatomical or near-anatomical position, and the nail was advanced to the distal fragment. Fracture reduction was checked under the image intensifier, and one or two cannulated screws were inserted with the traditional method. The end of the nail was buried and the wound was closed.
The quality of reduction was ensured on the anteroposterior and lateral views, and all operations were conducted by senior surgeons. The sutures were routinely removed at approximately 2 weeks in most patients, and removal was delayed when preoperative gross swelling of the wound was present.
Perioperative management
Passive range-of-motion exercises were performed in the knee and hip after the operation. Deep vein thrombosis was prevented by administration of low-molecular-weight heparin for 1 week postoperatively. The patients were encouraged to sit on the bed and exercise the lower limb muscles for the first 24 hours postoperatively. From postoperative day 14, the patients were encouraged to perform partial weight-bearing ambulation with assistance for 0.2 hours daily. Full weight bearing for 1 hour daily starting from 20 kg with an incremental increase of 5 kg per week was allowed when radiographic union was evident.
Outcome measurement
The patients were followed up clinically and radiologically at regular intervals, and progress of union and possible complications were then assessed every 2 or 3 months for at least 1.5 years. Data regarding incision size, surgical blood loss, surgical time (from skin incision to skin closure), and hospital stay were extracted from the medical records. Complications such as femoral neck shortening, screw exit, cut-out, nonunion (defined as a fracture that did not heal within 1 year), and avascular necrosis were monitored. Femoral neck shortening measured in the vertical plane was categorized into four degrees (0, 1, 2, and 3).13,14 The Harris hip score (scale of 1–100) was used to evaluate hip function at the end of follow-up.15,16 The results were categorized as excellent (90–100), good (80–89), fair (70–79), and poor (<69). Nonunion was defined as radiographic lucency or a persistent fracture line that failed to exhibit progressive healing after 12 months. Initially, all radiographic evaluations and measurements were performed by the first author (all authors reviewed all radiographs), and if there was disagreement in the assessment of categorical data, the final decision was made by the corresponding author. The assessment was repeated after 2 weeks. The intraclass correlation coefficient was used for evaluation of the intraobserver and interobserver reliabilities, both of which were good (intraclass correlation coefficient of >0.9).
Statistical analysis
Continuous variables are described as mean and standard deviation, and categorical data are presented as frequency. The statistical analysis was performed with SPSS 21.0 (IBM Corp., Armonk, NY, USA). Pearson’s chi square test and the nonparametric Mann–Whitney U test were used to identify significant differences between two groups. If more than 20% of the cells had an expected frequency of less than 5, Fisher’s exact test was performed. A P value of <0.05 represented a statistically significant difference.
Results
Initially, 108 patients were included in the analysis; however, 12 were lost to follow-up. Of the remaining 96 patients, the IT group comprised 56 patients with a mean age of 52.0 ± 9.8 years, and the RN group comprised 40 patients with a mean age of 50.6 ± 12.8 years. The patients were injured after slips, trips, or falls (n = 36) or in traffic accidents (n = 60). There were no significant differences in the demographic data or classifications of the femoral neck fractures between the IT and RN groups (Table 1). There were also no significant differences in the baseline characteristics between the IT and RN groups (Table 1). All patients in the two groups had unstable fractures (Figure 1). The average follow-up duration was 17.5 months (range, 12–19 months).
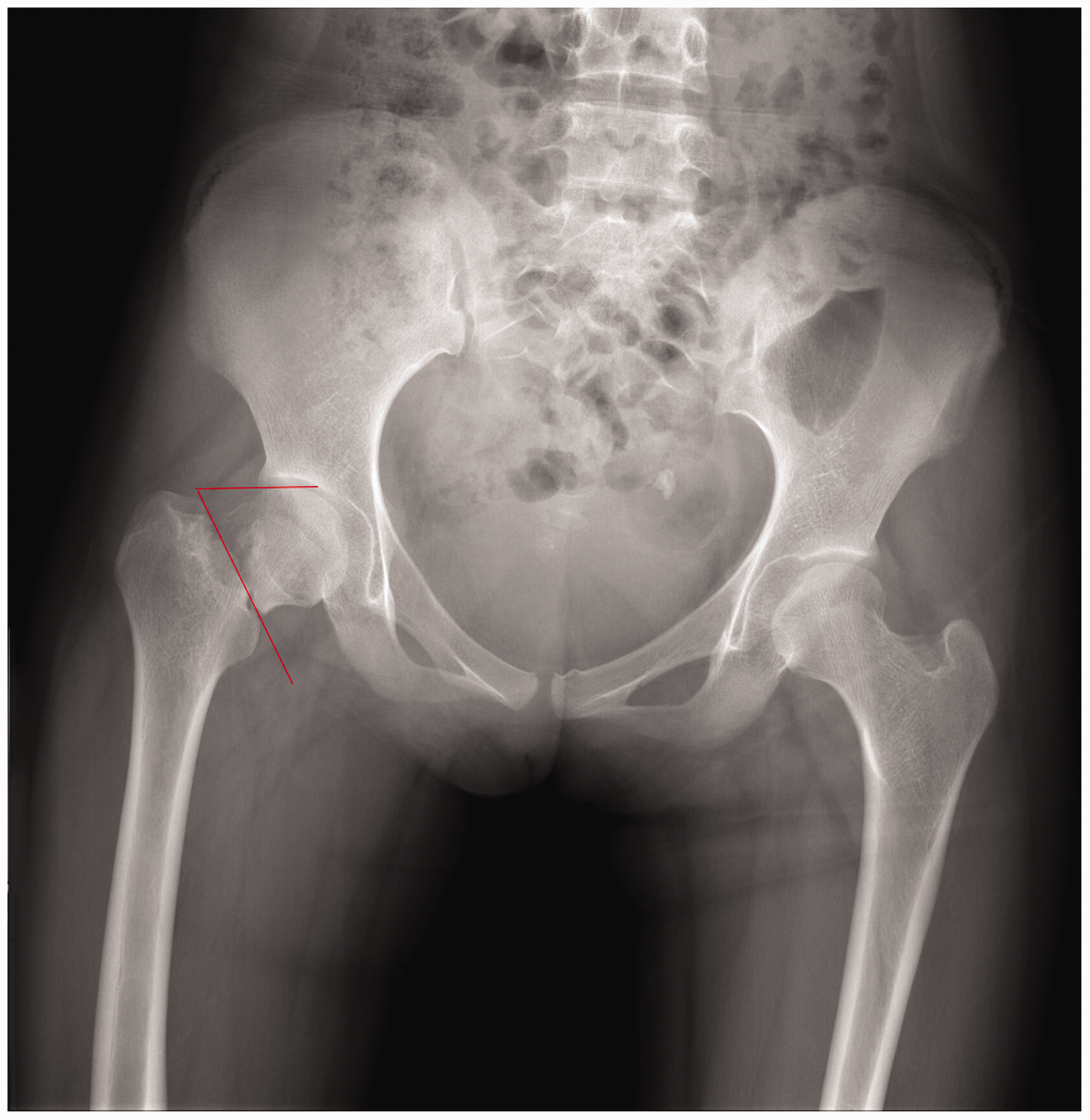
Radiograph of an unstable femoral neck fracture. Preoperative anteroposterior radiograph with a Garden IV, Pauwels III femoral neck fracture.
The clinical outcomes in the perioperative period are shown in Table 2. Images of femoral neck fractures fixed with inverted cannulated compression screws are shown in Figure 2. Significant differences were found in the incision size, surgical blood loss, and fluoroscopy time (P < 0.05) (Table 2). Patients in the RN group had a shorter hospital stay, which might have been due to more stable internal fixation (Figure 3). However, many variables may have affected this finding; thus, it cannot be taken as a true reflection of the impact of the implant type on the hospital stay. Notably, no patient in either group developed an infection after the operation.

Preoperative and postoperative radiograph of a 58-year-old man with a Garden III, Pauwels III femoral neck fracture treated with inverted triangular configurations. (a) Preoperative anteroposterior (AP) radiograph (b) Preoperative lateral radiograph (c) Postoperative AP radiograph (d) Postoperative lateral radiograph (e) On the AP radiograph at 13 months, the screws exhibited exit-out (f) Lateral radiograph at 13 months (g) AP radiograph showing revision arthroplasty after internal fixation failure (h) AP radiograph after arthroplasty (before follow-up).

Preoperative and postoperative radiographs of a 58-year-old woman with a Garden IV, Pauwels III femoral neck fracture treated with an intramedullary nail. (a) Preoperative anteroposterior (AP) radiograph (b) Postoperative AP radiograph (c) Postoperative lateral radiograph (d) AP radiograph before finishing follow-up (e) Lateral radiograph before finishing follow-up.
Clinical outcomes during the perioperative period.
Data are presented as mean ± standard deviation or n (%).
IT group, inverted triangular group; RN group, reconstruction nails group.
Complications after follow-up are shown in Table 3. The screw exit rate was significantly different between the IT and RN groups (21.43% vs. 0.00%, respectively; P = 0.034) (Table 3). Although no significant difference in shortening was observed, it was less severe in the RN group. Fracture healing was achieved in most patients in both groups. No significant differences were found in cut-out, nonunion, or avascular necrosis between the two groups. At the end of follow-up, no statistically significant difference in the Harris hip score was observed between the two groups (Table 3).
Clinical outcomes in the two study groups.
Data are presented as n (%) or mean ± standard deviation.
IT group, inverted triangular group; RN group, reconstruction nails group.
Discussion
Arthroplasty is the first-choice treatment for acute femoral neck fractures in patients aged >65 years. However, the optimal treatment is still internal fixation for patients aged <65 years. There is now sufficient evidence to support the use of cannulated compression screws for low-cost treatment of younger patients, who have higher functional demands. However, the biomechanical challenges and the vulnerability of the femoral head blood supply result in a high rate of nonunion and osteonecrosis after fixation. Additionally, whether the use of intramedullary nails is a suitable fixation method for treatment of unstable femoral neck fractures in young and middle-aged patients remains unclear. In this retrospective study of 96 patients, we compared patients treated with inverted cannulated screws and reconstructions nails. We found no significant difference in preventing cut-out or nonunion in the treatment of femoral neck fractures after follow-up. In contrast, the perioperative data illustrated significant differences in the incision size, blood loss, and fluoroscopy time between the two groups. To the best of our knowledge, no clinical studies have collected operative data to compare two fixation methods using three inverted parallel cannulated screws or intramedullary nails for unstable femoral neck fractures. The present results enrich our understanding about different methods in treating femoral neck fractures and suggest that intramedullary fixation is another treatment choice, especially for unstable fractures.
There is no “gold standard” method for the treatment of unstable femoral neck fractures. Many techniques other than inverted cannulated screws have been introduced to improve the treatment effect. Satish et al. 17 described a four-quadrant parallel peripheral screw fixation technique and concluded that a better prognosis was achieved. This four-quadrant parallel peripheral screw configuration was similar to the triangular screw configuration in that it had two distal screws; however, it also had an additional proximal screw. We do not believe that the mechanical characteristics of the four-quadrant parallel peripheral screw configuration are superior to those of the inverted screw configuration. Filipov and Gueorguiev 6 and Filipov et al. 18 introduced a method of biplane double-supported screw fixation and concluded that it improved cortical screw support and increased fixation strength through their mechanical and clinical studies. However, it is difficult to manage the screws under the level of a small trochanter, especially for less experienced orthopedic surgeons. The use of multiple compressive screws has been advocated for Garden types I and II fractures.19,20 Strictly speaking, cannulated screws are not appropriate for intramedullary fixation. More stable fixation using a DHS with or without antirotational screws has also been advocated. 21 However, larger skin incisions, extensive soft tissue dissection, a greater need for blood transfusion, and a longer hospital stay have limited its clinical use. 7 Swiontkowski et al. 22 also concluded that similar to the use of three parallel cannulated screws, the DHS did not resist torsional forces in unstable femoral neck fractures. The helical-shaped femoral neck blade that is applied in nailing systems to treat unstable femoral fractures is not suitable for young patients without osteoporosis. 23
Resistance of shear force, especially in unstable femoral neck fractures in the IT group, mainly depends on the head of the screws. Shear force may result in loss of reduction, screw exit, and coxa vara. Maintaining the stability of reduction and fixation during the process of fracture healing is the key to success. Placement of a medial buttress plate on the femoral calcar combined with the use of inverse cannulated screws has recently become a popular method. This technique provides adequate stabilization for femoral neck fractures. Kunapuli et al. 11 found that the strength of an augmented plate for stabilizing vertical shear in femoral neck fractures was superior to non-augmented fixation techniques through mechanical testing. Zhuang et al. 24 reported that an anteromedial femoral neck plate with cannulated screws could be used to treat irreducible displaced femoral neck fractures in young patients. On the basis of their retrospective study, Ye et al. 25 considered that a medial buttress plate improved the union rate of femoral neck fractures compared with a historical series using cannulated screws alone. However, the operation requires opening of the articular capsule and has a negative effect on the blood supply of the femoral head. Although the authors explained that the lateral circumflex femoral artery does not provide the primary blood supply to the femoral head, the operation method and complicated surgical technique have not yet been popularized, and more clinical studies should be conducted.
In young patients, arthroplasty leads to many problems such as fixation failure and revision, which result in poor function. Therefore, unstable fractures are always first treated by cannulated screws, and if avascular necrosis subsequently occurs, arthroplasty is performed as the ultimate treatment. As mentioned above, cannulated screws are a type of extramedullary fixation that have inherent deficiencies compared with intramedullary fixation. Röderer et al. 12 compared the use of a DHS with intramedullary nailing in an unstable medial femoral neck fracture model and concluded that proximal femoral nailing antirotation achieves primary stability comparable with that provided by the DHS. Although no clinical research has been published, intramedullary fixation might be better due to its biomechanically favorable characteristics (shorter lever arm and reduced bending moment on the implant) and is a minimally invasive technique compared with extramedullary fixation. The reconstruction nail is inserted using a minimally invasive technique to protect the soft tissues, and this is beneficial for quick recovery. Although the intraoperative indices in the RN group were not as good as those in the IT group, the rate of screw exit was significantly lower in the RN group. Additionally, although all patients in the RN group were young and middle-aged patients who could tolerate moderate blood loss and a long operative time, the negative effects of reconstruction nails in older patients should be noted.
Cannulated screw fixation for some types of vertical femoral neck fractures is not successful in the clinical setting. Construction nails should always be used to treat femoral shaft fractures combined with femoral neck fractures according to a previous study (Figure 4). These nails were used to treat femoral neck fractures in the present study because of their advantages with respect to intramedullary fixation. Nowotarski et al. 26 also found that femoral neck fractures with ipsilateral femoral shaft fractures treated with fixed-angle cephalomedullary intramedullary nails had satisfactory reduction and healed more reliably. However, screws inserted into the femoral head are not designed to act as compressive lag screws in construction nails. Additionally, when the femoral head and neck are anchored into strong cancellous bone, resorption of bone at the fracture site in the fracture healing stage may lead to a progressively increasing distance between the fracture edges. To minimize the negative effect and increase the strength of fixation, one or two cannulated screws were added to improve the sliding characteristics of internal fixation in the RN group. Extramedullary fixation and intramedullary fixation work together to make the fixation more reliable. Although three cannulated screws are widely used for femoral neck fractures, construction nails also have some advantages.7,8,11,12
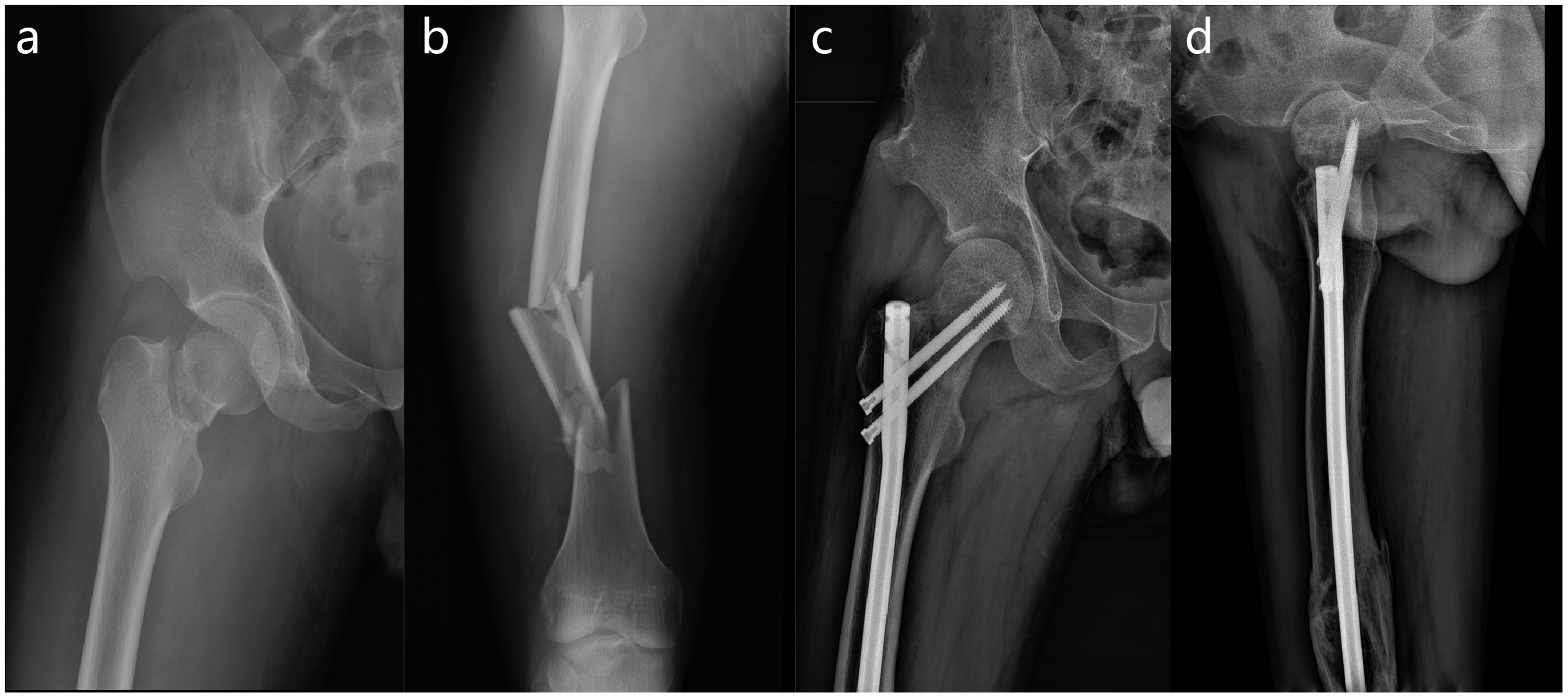
Preoperative and postoperative radiographs of a 42-year-old man with a femoral neck fracture combined with a femoral shaft fracture treated with an intramedullary nail. The femoral neck fracture was healed with no complications at 2 years postoperatively. (a) Preoperative anteroposterior (AP) radiograph (b) Postoperative AP radiograph (c) Postoperative lateral radiograph (d) AP radiograph at 2 years postoperatively.
The main limitations of this study are its retrospective nature and evaluation of the quality of reduction. Additionally, the patients’ follow-up time was limited. The femoral head is considered to be an minimal risk of developing avascular necrosis after a 5-year observation period in the clinical setting; this is a relatively short time and may be insufficient to register all cases of avascular necrosis. However, an average follow-up period of 18 months is still sufficient to demonstrate the occurrence of bone union or most complications after the operations. Finally, compression of the fracture site is considered one of the most important factors affecting the healing of femoral neck fractures. Nevertheless, this is difficult to achieve with reconstruction nails; intramedullary nails may be more suitable especially for Garden III/IV and Pauwels II/III fractures. However, this technique was popular in our hospital, and the number of patients treated with intramedullary nails was not large. Patients treated with intramedullary nails will be evaluated in future research.
In conclusion, intramedullary fixation with cannulated screws has advantages in treating unstable femoral neck fractures. Besides three cannulated screws, intramedullary fixation combined with cannulated screws might be another method to treat unstable femoral neck fractures in young and middle-aged patients.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
