Abstract
Cerebral venous sinus thrombosis is a special cerebrovascular disease affecting young adult and middle-aged people. The clinical manifestations of cerebral venous sinus thrombosis are diverse and nonspecific; thus, imaging plays an important role in early diagnosis. Anticoagulation with heparin is the preferred treatment for cerebral venous sinus thrombosis. Endovascular treatment is also being increasingly used to achieve recanalization of the cerebral venous sinus. We herein describe a woman in her early 50s who was diagnosed with cerebral venous sinus thrombosis for which anticoagulation with heparin was ineffective. To improve her symptoms and prognosis, we selected balloon venoplasty to treat the right sigmoid sinus thrombosis. Her condition subsequently improved, and no recurrence was observed after several follow-ups.
Keywords
Introduction
Cerebral venous sinus thrombosis (CVST) is a relatively rare but potentially life-threatening cause of stroke, and it has variable and nonspecific clinical presentations. 1 CVST is caused by the blockage of cortical veins and dural venous sinuses, which ultimately leads to infarction of the draining zone in the brain parenchyma. 2 Depending on the extent of cerebral injury caused by venous infarction, cerebral edema, and increased intracranial pressure, the clinical presentations may vary from absence of symptoms, mild headaches, nausea, and vomiting to visual deficits, stupor, coma, and even death. 3 The most common risk factors for prothrombotic states include exogenous hormone therapy, pregnancy, and puerperium. 4 CVST is often misdiagnosed and inappropriately treated, resulting in a high rate of disability and mortality. 5 When CVST is highly suspected in clinical practice, definitive neuroimaging diagnosis is essential. 4 All major guidelines recommend anticoagulation with heparin as the standard treatment for CVST 6 ; however, endovascular treatment is considered for refractory cases. Endovascular treatment should be considered as an alternative therapeutic option for patients with worsening symptoms of CVST to reduce the risk of mortality. 7 We herein describe a woman in her early 50s with a neuroimaging diagnosis of CVST who underwent balloon venoplasty to treat right sigmoid sinus thrombosis.
Case presentation
The reporting of this study conforms to the CARE guidelines. 8 We have removed all patient-identifying details from the figures.
A woman in her early 50s was admitted to the hospital because of a 20-day history of headache, dizziness, nausea, vomiting, and blurred vision that had become aggravated during the last 3 days. She had received oral drugs containing estrogens because of vaginal bleeding. The patient’s intracranial pressure markedly increased to >300 mmH2O, and she gradually became blind. After admission, three-dimensional (3D) fast spin-echo (FSE) black blood imaging showed high signal intensity in the right sigmoid sinus (Figure 1(a)). The right sigmoid sinus was invisible on magnetic resonance venography (MRV) (Figure 1(b)). Fundus examination revealed bilateral papilledema (Figure 1(c), (d)). Digital subtraction angiography (DSA) showed that the proximal right sigmoid sinus was unclear and that collateral circulation had become established (Figure 1(e)). The patient continued to undergo routine therapy; however, she showed no improvement. Re-examination of the cerebrospinal fluid pressure showed that it had increased to >400 mmH2O. The patient was treated with balloon venoplasty to improve her symptoms and prognosis. After obtaining informed consent for treatment from the patient’s family, the following procedure was performed. The right femoral vein was punctured, and an 8-Fr introducer was placed. A 300-cm Command micro-guide wire (Abbott, Abbott Park, IL, USA) was carefully delivered to the distal superior sagittal sinus via a VTK catheter (Cook Medical, Bloomington, IN, USA) and fixed. A 6- × 30-mm Sterling balloon (Boston Scientific, Marlborough, MA, USA) was delivered along the micro-guide wire to the distal right sigmoid sinus. The balloon was filled to a pressure of 5 atm at the right sigmoid sinus and distal right internal jugular vein. After two balloon dilatations, intraoperative DSA showed dilatation of the narrow vascular lumen, and the balloon was evacuated. Tirofiban (10 mL) was slowly injected every 10 minutes, and DSA was repeated. After 20 minutes, the DSA findings were similar to those obtained postoperatively. After the operation, the patient’s symptoms improved significantly. Three-dimensional FSE black blood imaging showed that the abnormal signal in the right sigmoid sinus had almost disappeared (Figure 2(a)). MRV showed recanalization of the right sigmoid sinus (Figure 2(b)), and DSA showed partial recovery of the right sigmoid–jugular access (Figure 2(e)). The cerebrospinal fluid pressure dropped to 270 mmH2O, and fundus examination showed alleviation of the bilateral papilledema (Figure 2(c), (d)). The patient was discharged a few days later while continuing anticoagulant therapy, and she was followed up regularly thereafter. A few months later, she was readmitted for follow-up. Her symptoms had almost disappeared, and most follow-up test results were normal.
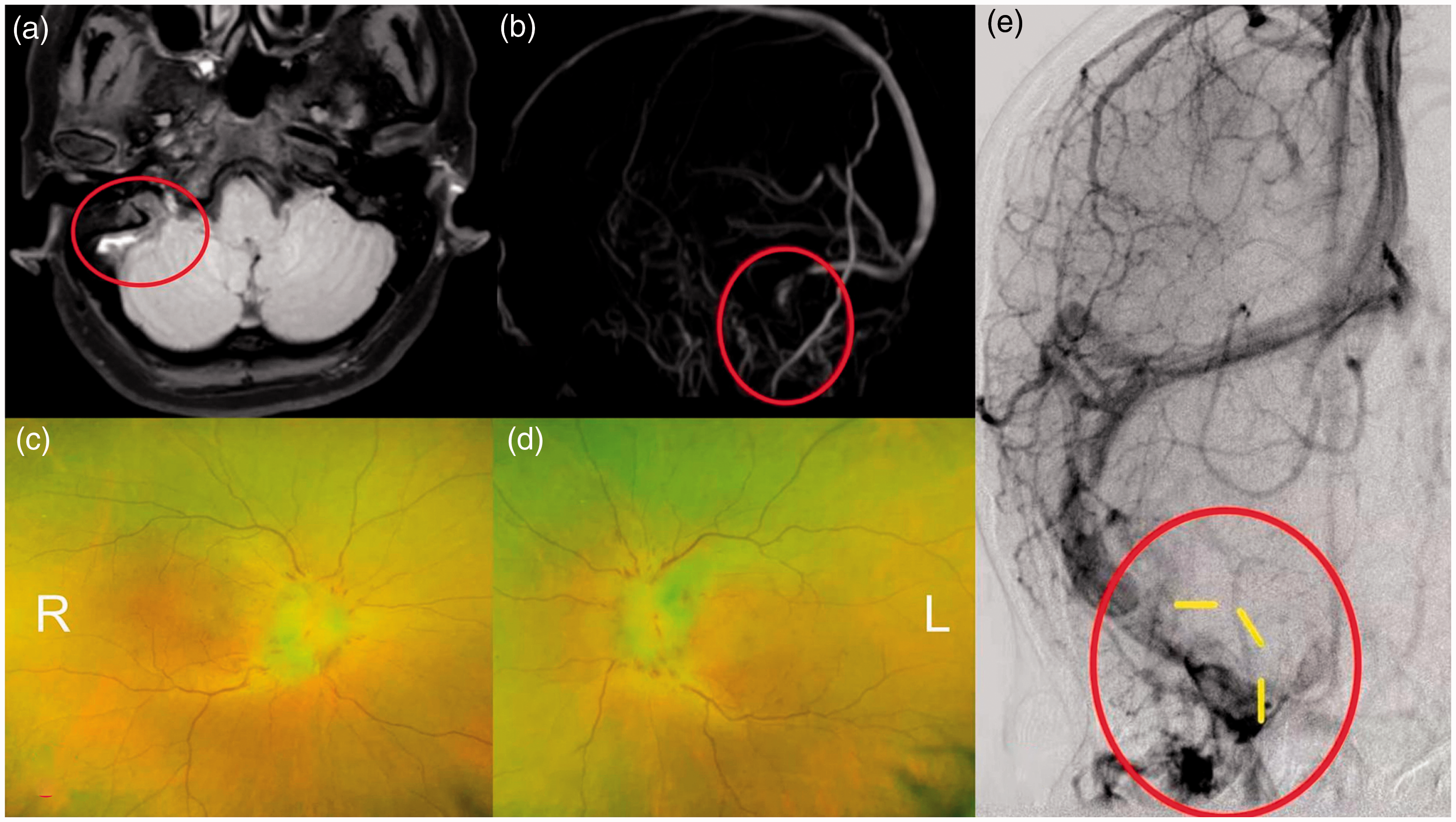
Preoperative imaging findings. (a) Preoperative axial three-dimensional fast spin-echo black blood sequence showed distinct hyperintensity in the right sigmoid sinus. (b) Preoperative magnetic resonance venography showed that the right sigmoid sinus was invisible. (c, d) Preoperative fundus examination showed obvious bilateral papilledema. (e) Preoperative digital subtraction angiography showed that the proximal right sigmoid sinus was unclear and that collateral circulation had become established (red circle) (the yellow curve indicates the normal shape of the right sigmoid sinus).
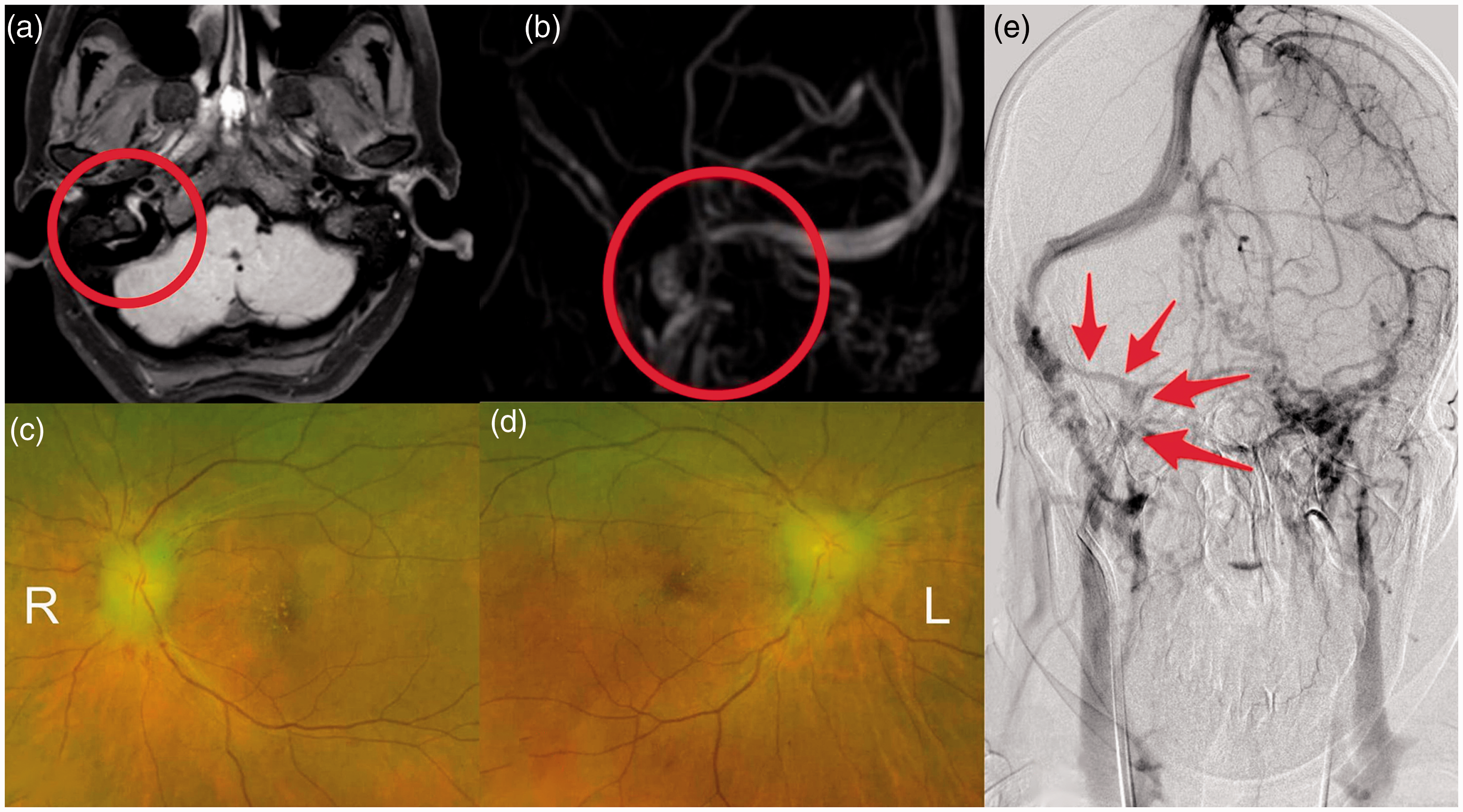
Postoperative imaging findings. (a) After the operation, axial three-dimensional fast spin-echo black blood sequence showed almost complete disappearance of the abnormal high signal intensity. (b) Preoperative magnetic resonance venography showed recanalization of the right sigmoid sinus. (c, d) Postoperative fundus examination showed alleviation of the bilateral papilledema. (e) Postoperative digital subtraction angiography showed partial recovery of the right sigmoid–jugular access (red arrow).
Discussion
CVST is a relatively uncommon cause of stroke, especially among women and younger individuals. 2 The chief associated pathophysiological changes include the hindrance of venous drainage, leading to increased venous and capillary pressure with resultant cerebral edema and increased intracranial pressure. In the present case, we inferred that the patient’s slender left internal jugular vein, sigmoid sinus, and transverse sinus had led to increased blood flow in the right venous sinus, which slowed blood flow. The patient had taken oral drugs containing estrogens, leaving the blood in a hypercoagulable state.
Magnetic resonance imaging of the brain combined with MRV is the most sensitive and effective modality for the diagnosis of CVST.
9
MRV shows low or absent flow in the venous sinuses, as shown in the present case. Given the variations in the venous anatomy and the phenomenon of flow gaps, it is sometimes impossible to completely rule out CVST on MRV.
10
Several 3D FSE black blood sequences have recently been used to evaluate cerebral vessels. One published study showed that a thrombus can be selectively visualized in 3D FSE black blood imaging as a hyperintensity with high accuracy.
10
The 3D FSE black blood sequences showed a thrombus with evident high signal intensity, allowing for identification of the intraluminal thrombus, which is consistent with our case. Anticoagulation is currently the first-line treatment for CVST, and systemic anticoagulation is effective in preventing falling of the thrombus and deep vein thrombosis and embolism.
11
The 2017 European Stroke Organization guidelines for the diagnosis and treatment of CVST, endorsed by the European Academy of Neurology, recommend the following for anticoagulation therapy in patients with CVST:
12
A therapeutic dosage of heparin for all patients with acute CVST, even in the presence of intracerebral hemorrhage. Low-molecular-weight heparin over unfractionated heparin except in patients who are allergic to low-molecular-weight heparin or if rapid anticoagulant effect reversal is required. The American Heart Association/American Stroke Association guidelines recommend anticoagulation for 3 to 6 months for provoked CVST, 6 to 12 months for unprovoked CVST, and potentially lifelong for recurrent CVST, venous thromboembolism following CVST, or CVST associated with severe thrombophilia with a target international normalized ratio of 2 to 3.
Based on these guidelines, our patient was administered subcutaneous enoxaparin at 40 mg once a day. Patients with CVST usually have a favorable clinical outcome with anticoagulant therapy; however, patients may either fail to improve or clinically deteriorate despite treatment. Endovascular interventions include mechanical thrombectomy, thromboaspiration, or balloon venoplasty as an alternative option for patients whose condition deteriorates after anticoagulation. 7 Thrombus dissolution takes a longer time because of the high thrombus load in the cerebral venous sinus. Thrombi may affect venous drainage, and intracranial hypertension may not be alleviated for a long time. We selected endovascular treatment for our patient to shorten the disease course and improve the prognosis. Endovascular thrombectomy may dislodge the thrombus, leading to serious complications. An endovascular stent can cause iatrogenic bleeding, increase the vascular load, and aggravate the disease. After consultation with the patient’s family, we finally used balloon dilatation to achieve venous sinus recanalization. A balloon is flexible and soft and can be easily guided to the lesion in curved blood vessels, such as the sigmoid sinus. Balloon dilatation has been reported for the treatment of CVST; however, few reports have described the treatment of CVST by balloon dilatation alone. Bishop et al. 13 reported a successful case of balloon dilatation to treat left transverse sinus and sigmoid sinus thrombosis. The patient’s intracranial pressure decreased after the operation, leading to a positive treatment outcome and favorable long-term prognosis. Similarly, our patient also had a favorable outcome; her clinical manifestations were significantly alleviated after the surgery, her intracranial pressure decreased to 270 mmH2O, and the vascular pathway partially recanalized. The success of balloon dilatation may be due to its ability to loosen the thrombus, which can allow anticoagulant drugs to act on the thrombosis. The improvement of venous drainage after partial recanalization of the occluded lumen can rapidly relieve intracranial hypertension. However, in cases of balloon dilatation for recanalization, postoperative venous sinus occlusion may occur after balloon dilation. We believe that balloon dilatation provides a certain space for subsequent endovascular treatment such as restenosis. Further study is essential because the clinical use of balloon angioplasty in the treatment of CVST is limited and clinical evidence is lacking.
Conclusion
For patients who have been clearly diagnosed with CVST, balloon venoplasty should be considered when the effect of anticoagulation is unsatisfactory.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605211063278 - Supplemental material for Successful treatment of cerebral venous sinus thrombosis by balloon venoplasty: a case report
Supplemental material, sj-pdf-1-imr-10.1177_03000605211063278 for Successful treatment of cerebral venous sinus thrombosis by balloon venoplasty: a case report by Wei Chen, Wen-Jing Gu, Ming-Chao Shi, De-Rui Kong, Ke-Xin Zhao and Hong-Wei Zhou in Journal of International Medical Research
Footnotes
Acknowledgements
We thank the Jilin Provincial Department of Science and Technology for its financial support. We also thank the patient and her family for their collaboration.
Authors’ contributions
CW and GWJ contributed to the concept, drafting, and reporting of the case. MCS provided the case and puted forward his own unique opinions on the revision of the manuscript. KDR and ZKX acquired the clinical data and analyzed all images. ZHW contributed to the revision of the manuscript. All authors have read and approved the final manuscript.
Research ethics and patient consent
Written informed consent was obtained from the patient to publish her case, and approval for this study was provided by the Research Ethics Committee of The First Hospital of Jilin University.
Data availability
All data related to this case report are documented within this manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and publication of this article: This study was supported by the Department of Science and Technology of Jilin Province (grant number: 3D5204408428). The funding body did not play a role in collection, analysis, and interpretation of data, or to the writing of this manuscript.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
