Abstract
A ruptured infrarenal abdominal aortic aneurysm (rAAA) is associated with an in-hospital mortality rate of 40% and an overall mortality rate of 60–80%. Open surgical repair for rAAA remains the principal method of treatment when endovascular repair is not available. Graft infection occurs in 1–4% of patients at 5 years, with a high incidence following emergency treatment. Other graft-related complications include pseudoaneurysm, graft occlusion and aorto-enteric fistula. This case report describes a 66-year-old male patient that was admitted to hospital complaining of intense abdominal pain, low blood pressure and tachycardia. He was diagnosed with a rAAA and treated using segmental resection of the abdominal aorta followed by reconstruction with a synthetic Dacron prosthesis. A pedicle omental flap was wrapped around the prosthetic graft and it was also used to fill the retroperitoneal cavity in order to reduce the risk of graft-related complications. Computed tomography angiography after 6 months showed good integration of the aortic prosthetic graft and the viability of the omental flap. In our opinion, vascular surgeons should consider the pedicle omental flap when they perform open surgical repair for rAAA in order to reduce the incidence of graft-related complications.
Introduction
An abdominal aortic aneurysm (AAA) is defined as a focal increase in the diameter of the vessel that is > 1.5-times or > 3 cm. 1 The prevalence of AAA is 2–8%, with more males and those with increasing age being affected, especially men over 60 years of age. 1 Sixty-five percent of AAAs are located infrarenal and 15% are located juxtarenal. 1 , 2 In-hospital mortality associated with a ruptured infrarenal abdominal aortic aneurysm (rAAA) is 40% and the overall mortality is 60–80%.1,3
Open surgical repair (OSR) for the treatment of rAAA was first described by Cooley and DeBakey in 1954; 4 and it has remained the principal method of treatment when endovascular repair is not available. 5 Based on its unique proprieties, the great omentum has a wide application in many surgical specialities, including vascular surgery. 6
This current case report describes a patient with a rAAA that was treated by segmental resection of the abdominal aorta followed by reconstruction using a synthetic Dacron prosthesis that was covered with a pedicle omental flap. The flap was also used to fill the retroperitoneal cavity.
Case report
A 66-year-old male patient was admitted to the Emergency Department, Emergency District Hospital, Cluj-Napoca, Romania in December 2019 with intense abdominal pain, low blood pressure and tachycardia. Computed tomography angiography (CTA) showed a large infrarenal aortic aneurysm without contrast extravasation but with a periaortic haematoma extending to the left renal area (Figures 1a and 1b).
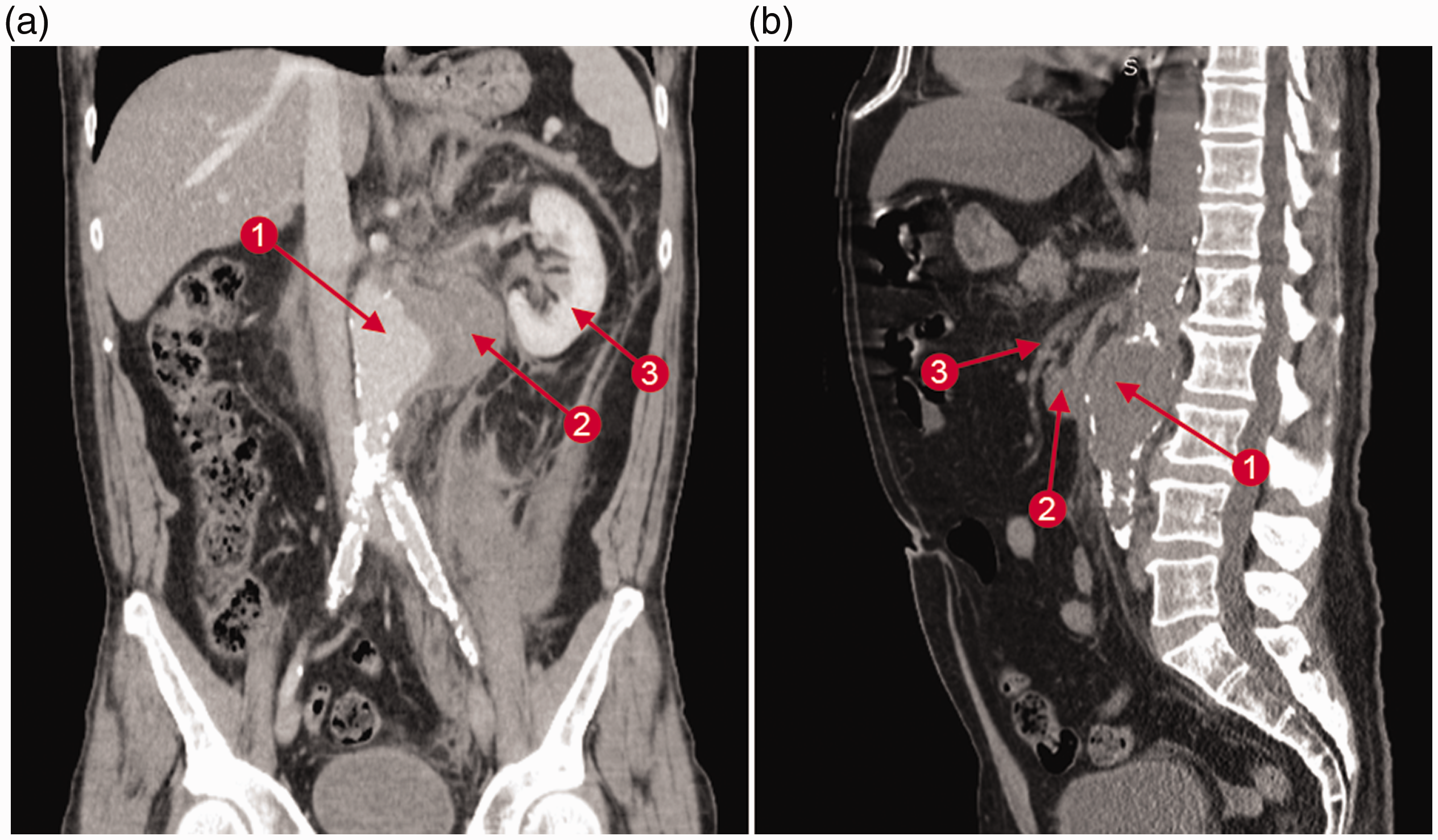
Preoperative computed tomography angiography of a 66-year-old male patient admitted to hospital with intense abdominal pain, low blood pressure and tachycardia: (a) coronal section showing a ruptured abdominal aortic aneurysm (rAAA, arrow 1), a left juxtarenal haematoma (arrow 2) and the left kidney (arrow 3); (b) sagittal section showing the rAAA (arrow 1), duodenum (arrow 2) and the superior mesenteric artery (arrow 3).
The patient was referred to the Department of Vascular Surgery, Emergency District Hospital, Cluj-Napoca, Romania and was operated on under emergency conditions. Under general anaesthesia, the infrarenal segmental aorta and the proximal segments of the common iliac arteries were identified. A partial resection of the infrarenal ruptured aneurysm was performed due to intensive arterial wall calcification (Figure 2a). The aortic reconstruction was performed with interposition of a collagen-coated Dacron bifurcated prosthesis (16/8 cm). The haematoma from the left renal area was removed. A pedicle omental flap was harvested, which was used for wrapping around the prosthetic graft and for filling the left retroperitoneal cavity resulting after haematoma evacuation (Figure 2b). The flap was based on the left gastroepiploic vessels.

Intraoperative images of a 66-year-old male patient admitted to hospital with intense abdominal pain, low blood pressure and tachycardia: (a) the ruptured abdominal aortic aneurysm (arrow); (b) the pedicle omental flap (arrow 1) and the prosthetic aortic graft (arrow 2). The colour version of this figure is available at: http://imr.sagepub.com.
The patient developed a postoperative reperfusion syndrome that was treated by temporary haemodiafiltration. The patient was discharged after 14 days with no other vascular complications. The follow-up was at 1, 3 and 6 months. CTA after 6 months showed good integration of the aortic prosthetic graft and the viability of the omental flap (Figures 3a and 3b). The reporting of this case conforms with the CARE guidelines. 7

Computed tomography angiography at 6 months postoperation in a 66-year-old male patient admitted to hospital with intense abdominal pain, low blood pressure and tachycardia: (a) transverse section showing the prosthetic aortic graft covered with the pedicle omental flap (arrow 1) and the duodenum (arrow 2); (b) sagittal section showing the prosthetic aortic graft (arrow 1) and the duodenum (arrow 2).
Discussion
Ruptured AAAs are associated with high mortality rates, causing 100 000 deaths/year in the US with an in-hospital mortality rate between 35.6% and 69%.8–10 Emergency intervention is mandatory as 12.5% of the patients die in the first 2 h. 5 Moreover, a systematic approach, using a protocol in the emergency setting, has been demonstrated to reduce the 30-day mortality from 32% to 18%. 11
The two treatment options for rAAA are OSR and endovascular aneurysm repair. OSR consists of the repair of the affected vessel segment by using a synthetic graft. To approach the abdominal aorta, a retroperitoneal or transperitoneal approach is used; the second one offering a more rapid and wider access. 12 There are no differences in mortality between these two approaches. 13 The mortality associated with OSR remains high (13–53%), 10 despite the evidence that, over the years, there has been a significant decrease in perioperative mortality. 14
Life-threatening adverse events are graft-related complications that can appear with a frequency of 3–10%.15–17 A previous study described the outcomes after treatment of an aortic graft infection: 17% mortality within 30 days postoperation and 21% mortality at the 1-year follow-up. 15 Graft infection appears in 1–4% of patients at 5 years, with a high incidence following emergency treatment. 18 Other graft-related complications include pseudoaneurysm, graft occlusion and aorto-enteric fistula. 3 Any of these complications is associated with high morbidity and mortality. 3
The omentum is an adipose tissue that covers the intra-peritoneal abdominal organs. It used to be called ‘the policeman of the abdomen’ and functions mainly like an organ system. It has wide application as a pedicle or free flap. 6 It offers a large amount of tissue with an excellent blood supply and lymphatic function. These proprieties permit a good delivery of antibiotics in association with efficient bacterial clearance, as well as an excellent absorptive capacity that reduces the dead space and, therefore, the risk of infection. 19 Also, the omentum promotes angiogenic activity in structures to which it is closely applied and releases pro- and anti-inflammatory cytokines that can play an important role in the omental defence mechanism supporting both ischaemic and inflamed tissues under pathological conditions. 20
All of the advantages of the omental flap described above (i.e. its availability, vascularity and lymphatic drainage) result in the superiority of the omentum in the preaortic position compared with other local retroperitoneal tissue in preventing aortic graft infection. 21 Moreover, covering the graft with the omentum tissue reduces the risk for adhesion formation between the graft and the intestinal wall, which is the mechanism for the development of aorto-enteric fistula. The omental flap is frequently used for the treatment of prosthetic graft infection.21,22
In this current case, the omental flap in preaortic position was used to protect against prosthetic graft infection because the omental flap blocks the translocation of intestinal bacteria to the prosthetic graft. Also, the omentum prevents formation of aorto-enteric fistulas (the omental flap separates the duodenum and prosthetic graft) and restricts the dead space from the left renal area after haematoma evacuation (the omental flap reduces the retroperitoneal seroma formation). The omental pedicled flap (based on the left gastroepiploic artery and vein) was wrapped around the prosthetic graft and filled the dead space from the left juxtarenal area. Wrapping prosthetic grafts with omentum to prevent postoperative graft infection has not yet been definitively proven to be effective in the long term.
After 6 months postoperation, CTA identified viability of the omental flap and good integration of the aortic prosthetic graft in this current case. The omental flap requires long-term monitoring, which can be undertaken using 18F-fluorodeoxyglucose positron emission tomography (PET)/CT or PET/CT scanning after complete local integration of the aortic prosthesis. 23
A search of the medical literature for the last 10 years (PubMed®, Embase®, Cochrane Library), in addition to Romanian journals and European Union data, was unable to identify any studies that had described the therapeutic use of an omentum flap for similar vascular patients. In our opinion, vascular surgeons should consider the pedicle omental flap when they perform OSR for rAAA in order to reduce the incidence of graft-related complications.
